Introduction
Suicide rates in Australia have decreased over the past 40 years against a backdrop of an increasing global suicide rate1,2. Suicide rates in Indigenous communities and rural and remote communities are greater in number than in urban communities, and tend to be increasing3. Poorer mental health outcomes in rural areas4,5 have been partly attributed to the general inaccessibility of general practitioners (GPs) and health services due to distance and low population thresholds, socioeconomic adversity, natural disasters6,7, social and educational disadvantage, and social and cultural isolation8,9. In terms of suicide specifically, males aged 15-24 years have proven to be most at risk of suicide in rural areas7. A deepening understanding of factors that protect against suicide is emerging10 such as access to GP services, social networks and personal self-esteem and coping strategies. Because rural communities are all different7, suicide prevention strategies need to address the context of each community as a necessary step in tailoring processes aiming to respond to their associated health outcomes.
The latest Australian National Suicide Prevention strategy promotes holistic suicide prevention strategies acting at the levels of individuals, families and communities and aims to decrease the numbers of people at high risk of suicide, while also decreasing the mean risk of suicide across the whole population. The most successful prevention strategies include decreasing access to the means to suicide, programs that educate healthcare practitioners, and gatekeeper suicide prevention education programs11. Gatekeeper programs aim to improve the knowledge, skills and attitudes of individuals who are well positioned in communities to recognise and refer someone at risk of suicide (eg teachers, pharmacists, sports coaches, police officers)12-14. Although strong communities are considered protective of suicide, little is known about suicide prevention models that involve community-based approaches. However, there is growing evidence of the effectiveness of gatekeeper programs in community settings13,15-17. The CORES (Community Response to Eliminating Suicide) program aims to build and support communities as well as provide both broad and targeted support to people at risk of suicide.
In this paper we report the history, philosophy and development of the CORES community-based gate keeper suicide intervention program, a description of the program and its implementation, and provide evidence for the effectiveness of the program in Australian rural communities.
CORES program philosophy and design
The CORES suicide awareness and intervention program was developed in Sheffield, Tasmania in response to concern about the rising suicide rates in the rural regions of the state. The local region has few social and community services and suffers significant social disadvantage, with high unemployment, high youth unemployment, a high incidence of diabetes, obesity, smoking and the lowest life expectancy in the state18. The program was conceived as a holistic approach to suicide awareness that involved building local leadership and social networks to find solutions to improve the general health and wellbeing of the whole community. The aims of the program were to (i) gather local people in the community to examine and understand their community, (ii) foster an understanding of suicide, (iii) develop the skills of local people to identify and respond to suicide at an early stage, (iv) engage local people in the delivery of the program, (v) identify and link people to community and professional support services and (vi) empower the local community to own and manage the program. The explicit adoption of a community-based approach19 for CORES infused the rationale, development and delivery of the overall program.
Implementing CORES with a community
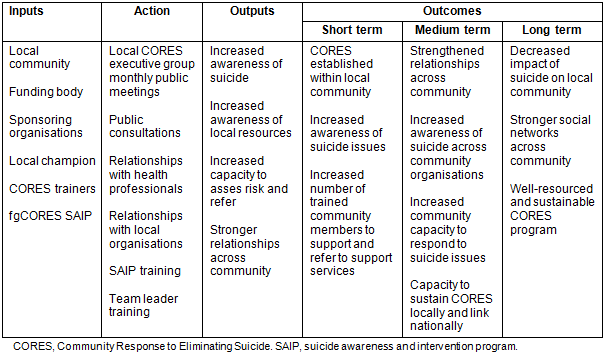
Community engagement is essential in establishing a new CORES program and for its ongoing success. The program comprises a comprehensive package to build community engagement with the goals of the project (Table 1), and training for a local team to lead the program to deliver suicide awareness and intervention programs (SAIP) for local residents. A local community CORES leadership group is established to link with health and human services in the region and to review available statistical data and health service reports as part of a needs analysis and review. It aims to uncover local health issues and concerns, factors associated with suicide, barriers to accessing help, knowledge of help-seeking behaviours and service mapping within the community. This information is used to inform the local training and mentoring for six team leaders and the delivery of SAIP training program to residents. The CORES team also facilitates communication with the public through social media and supports networking amongst team leaders from communities around Australia.
Table 1: Overview of the CORES program inputs, outputs and outcomes over
short, medium and longer term (This report does not evaluate long-term outcomes.)
One-day SAIP
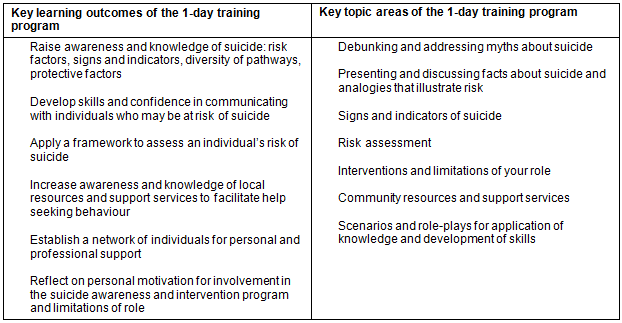
The aim of the 1-day SAIP is to increase the ability of local community members to identify people at risk of suicide, assess the immediate risk of suicide through structured conversation and facilitate help-seeking behaviour through identification of support services. The outcomes and content of the 1-day SAIP (Table 2) is consistent with best practice guidelines19 and those espoused in the Australian LIFE (Living is for Everyone) framework20. The SAIP is delivered by two team leaders to a small group of 10-15 participants in a manner that draws upon lived experiences and promotes active participation.
The SAIP commences with ice-breaker activities and discussion about ground rules and the importance of personal safety and confidentiality, particularly in small rural communities. The body of the SAIP focuses on three elements: (i) suicide myths and realities, (ii) understanding of a suicide journey and (iii) an intervention/suicide discussion role-play. A significant amount of time is spent discussing suicide myths and statistics and answering questions. The suicide myths and realities question-and-answer period covers many issues associated with rural suicide5 and provides a neutral zone for conversation before an open invitation for participants to offer a broader self-introduction. This is followed by a refreshment break to promote a positive dynamic within the group and provide a time-out for any individuals who may feel distress after suicide-related personal disclosures.
The concept of a journey towards suicide is shown through the use of a visual image of life as a river with many tributaries, which represent the stresses and struggles experienced by most people, held back by a dam wall. This image is a central element of the program. It is used by trainers to illustrate the processes that may lead an individual to contemplate suicide and later as a tool for discussion and risk assessment. Understanding of the journey is developed further through the 'funnel vision' experience. Participants look through a funnel to experience the narrowed perspective of someone who can only focus on ending their life and see how this view prevents someone from seeing the positive aspects of their life. The participants are asked to look again through the funnel from the narrow end as an illustration of how the course will enable them to help 'turn the funnel around' and show the person at risk that there are other options than suicide. This assists greatly in the understanding of what it is like for an individual contemplating suicide and offers a visual representation of the goal of the intervention.
The third element is the ABCD intervention where all parts of the training are brought together through use of intervention scenarios. Participants learn how to ask the person at risk if they are considering suicide (A); assess for past behaviours or experience, thereby gauging the level of risk (B); assess if the person at risk has a current plan for suicide (C) and understand what it is that is keeping them alive and how they have managed to cope with their stresses and struggles in the past (D, the dam). The team leaders demonstrate how to recognise a person at risk, how to assess risk, and how to assist the person by referral. Assessment follows a strengths-based approach21, including an assessment of 'hopelessness'22. Participants apply their learning and new skills using examples, scenarios and role-plays of 'interventions'. During the final role-play, participants playing the person at risk and the support person work through coping skills that may have once been in place, but have been forgotten. Identifying these skills helps the participant in the role of the support person 'turn the funnel around' for the individual at risk. Community members work in pairs through the role-play, supported by the trainers. The small group environment ensures that there is sufficient quality interaction between participants to build professional relationships amongst the team. The training regularly emphasises the limits and possible outcomes of any intervention.
The day concludes with a circle activity designed to illustrate how the SAIP can operate in a rural community. Passing a ball of wool amongst the trainees (which forms a web), the team leader reflects that this experience links them as a network that will support their community.
The SAIP places an emphasis on knowledge about suicide and safety for community members. Given the nature of rural communities, the importance of privacy and confidentiality is stressed. In the absence of other risk factors for suicide, current evidence suggests that such thinking by itself is not a risk factor10. However, for a small group of individuals, such suicidal thinking can become uncontrollable and persistent, and when associated with other mental health problems, may indicate a serious risk of suicide or suicide attempt17. CORES emphases for trainees that not all individuals at risk of suicide can be identified, and that not all suicides can be prevented23. CORES facilitates and supports counselling for those who have used their SAIP training in practice in their community.
Table 2: Key learning outcomes and topic areas of the SAIP 1-day program
Team leader training program
The success of CORES depends significantly on the team that manages the program, delivers SAIP training to community members and works to ensure its ongoing presence in the community. Team leaders must have leadership potential and significant time, motivation and profile within the community to support the governance and management of the program in the community. They must understand the community in which they are working, and have an informed understanding of the health and support services in their community. In addition, they require a capacity to learn about suicide and to develop interpersonal communication skills for the successful delivery of the SAIP. CORES works with the local community to select the best group of team leaders with a balance of skills suited to the successful embedding of the program within the new community.
The team leader training program (TLTP) is a 4-day program for a maximum of six people, based upon adult learning principles of reflection, application and role-play. This program consists of the successful completion of the 1-day SAIP program, followed by 3 days of learning how to deliver that program. The TLTP unpacks the program philosophy and rationale, delivers specific content about mental health and suicide, and develops the micro teaching and communication skills necessary to deliver the program in a safe and supportive environment. The final requirement of the TLTP is for the trainees to deliver two 1-day SAIP courses under the supervision of the team leader trainer. Team leaders are supported as a community within CORES. Quarterly face-to-face team leader meetings are held, usually centred on a guest speaker (eg StandBy, men's health) or professional development activity. Networking, information-sharing and updating of resources by team leaders is facilitated by these meeting and the use of a 'secure zone' on the CORES website (http://www.cores.org.au).
Approach to evaluation
Over the past decade CORES has been evaluated through ongoing informal feedback, internal review and external evaluations24,25. Internal evaluations involved written feedback gathered after SAIP training sessions and team leader training. Recent SAIP training evaluations used pre- and post- training surveys and follow-up questionnaires using questions relating to previous knowledge/training in regard to suicide awareness and intervention; the level of comfort in talking about suicide to people who may be at risk; and the confidence of the participant's ability to provide appropriate assistance to family members, friends, colleagues or strangers. Follow-up email questionnaires, interviews and focus groups, and the CORES website, have sought feedback from participants on their use of knowledge and skills developed through CORES. Research was approved by the Tasmanian Research Ethics Network.
Evaluations have demonstrated the importance of providing a safe learning environment (eg double trainer model), managing communication and processed for managing confidentiality for participants and CORES-trained individuals working in communities.
Reach of CORES into rural communities
Since its inception in 2003, the CORES program has been adopted by Tasmanian communities and by rural communities in three other Australian states. CORES has delivered 408 of the 1-day SAIP courses to 4242 individuals, with 43 TLTP programs for 157 team leaders of whom 87 remain active in their community (Table 3). The focus of the first 5 years was to refine the program, while the last 5 years have seen a significant expansion into other rural communities concerned about mental health and suicide rates (Table 4).
Table 3: Scale of CORES program uptake across Australia. (Total for community sites not included as sites entered and left program.)
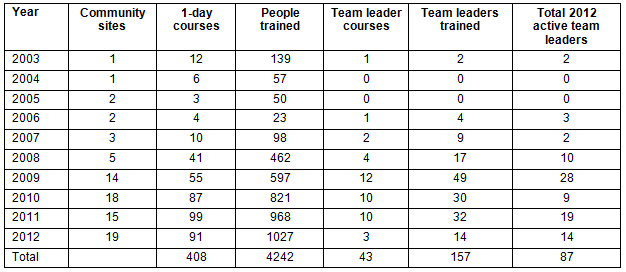
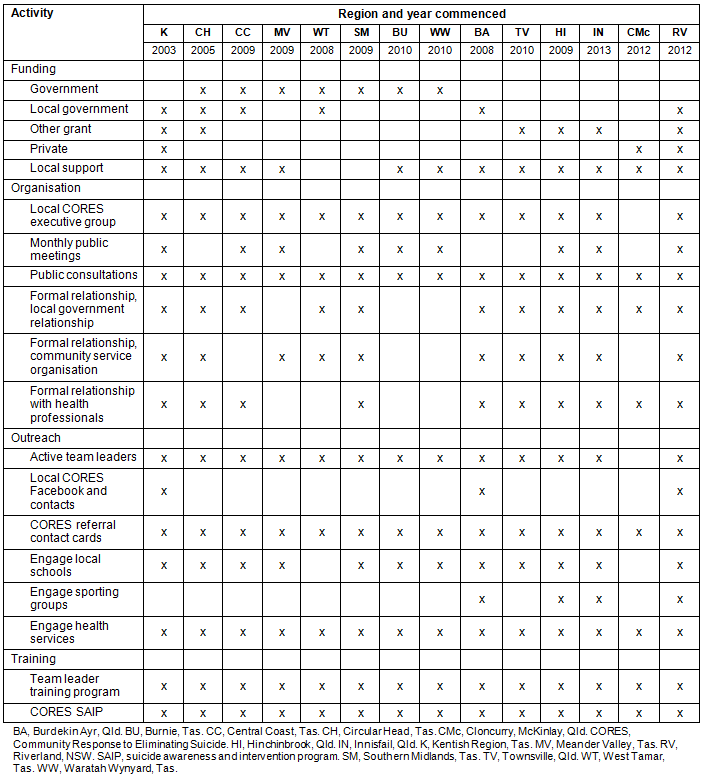
Table 4: Range of community engagement strategies employed in the active CORES programs operating in regional Australia
SAIP experience, knowledge and confidence
Participant experiences with the SAIP have been positive. The scaffolding of understanding of a suicide journey by the river analogy and funnel vision exercise consistently received strong positive feedback and participants reported grasping concepts more fully through the reiteration of these strategies. The use of a team teaching approach was introduced after some participants needed 'time out' after disclosure of emotional events related to suicide experiences. The approach enables one trainer to step out and support any individual who may have an emotional response to the training, thus maintaining a supportive and safe environment. The funnel vision experience was very challenging for some participants, although the majority reported that the exercise provided them with a sense of how individuals contemplating suicide may view their world. Analysis of the SAIP surveys revealed a greater awareness of the signs and symptoms of an individual at risk, which resulted in a positive shift in attitude towards those individuals and improved knowledge and practical skills. Participants also reported higher levels of comfort and confidence (Table 5) in discussing suicide with those who may be considering it.
Table 5: Participant-reported levels of comfort and levels of confidence
discussing suicide with an individual who may be 'at risk', before and after SAIP training

Intervention and social isolation
The intervention element of CORES aims to decrease the social isolation felt by those contemplating suicide through dialogue, consideration of their suicide risk and referral for assistance. CORES seeks to normalise help-seeking behaviour. A sensitive intervention can decrease social isolation as individuals share their circumstances. Six months after completing the 1-day SAIP training in 2011, 10 trainees across two sites reported that they had applied their skills in their community. Since 2010, more than 900 interventions have been reported in which a trained individual engaged with another person at risk of suicide, specifically using their CORES-based skills. Focus groups and interviews with trainees24 revealed that many trainees believe that their conversations about CORES and suicide are creating change within their community.
Community engagement
Community engagement and ownership of CORES is critical for its long-term success when newly adopted. Internal evaluations and a review of Australian suicide prevention strategies16 have informed the ongoing development of community engagement processes. The CORES team visits the prospective community to conduct an analysis to assess (i) a sense of community, (ii) a desire for the program, (iii) the capacity to manage and develop the program, (iv) a clear focus on goals and outcomes and (v) the dedication to undertake the work to achieve those goals. A strong and well-established community-based organisation with sufficient financial, management and organisational capacity is an ideal sponsor.
The effect of CORES on local communities can be evaluated through the strategies used to build social capital. The range of activities that engage the community is broad, though CORES aims to use a common set of strategies to engage communities (Table 4). CORES has been continually operating for nearly a decade in Sheffield, supported by local government funding, regular fundraising events in the town and external grants. Monthly meetings and annual meetings have been held since its inception, with strong attendances at annual meetings. The program has a high profile in the township, supported by a committed executive team of people, refreshed every few years. By linking with local government, health and human services organisations to support health and social needs analyses, CORES has advocated for social and infrastructure development and improvements in health care in the region18. CORES has trained five team leaders in Sheffield, all of whom are still active, and more than 300 people have attended 1-day SAIPs. The CORES program generates a high profile through the relationships it has built between service organisations, businesses, schools, and religious and sporting groups, resulting in links between individuals and families across social and geographical boundaries. Feedback gained from the community18 shows consistently strong support for a program seen as beneficial for the community. This same pattern of community engagement is seen with CORES' presence in other regions across Australia. In terms of successful programs, the establishment of a local CORES executive to lead the local program and gain financial support is a key step in the process.
Discussion
The value and success of the CORES program is discussed here against two broad domains: evidence-based design and development, and success in terms of its uptake and impact.
SAIP design, development and outcomes
Philosophy: The community-based approach was adopted by CORES in 2003. There is increasing evidence that community engagement is an essential step in the development of new health services in communities26,27. The approach used by CORES, linking with existing health and service organisations whilst developing ownership and skills within the community to maintain the program (for example through the TLTP), has been identified16 as good practice for successful and sustainable community health programs.
Learning outcomes: The implementation of CORES is consistent and aligns with the LIFE framework20 by delivering on the four key areas identified by LIFE: building individual resilience, improving community strength using a coordinated approach, providing targeted activities, and implementing proven remedial standards. Gould and Kramer15 suggest that the purpose of training is to help to 'identify people at risk, assess levels of risk and manage the situation and refer when necessary'. The outcomes that CORES achieves align with the goals of the most effective gatekeeper suicide programs13 and recent Australian mental health training initiatives16 including those utilised in drought- and disaster-affected rural areas28,29. Comparisons between trainees' pre- and post-SAIP surveys show significant improvements (Table 5) in awareness and knowledge of suicide, confidence in raising discussion around suicide and recognition of when and how to refer someone at risk of suicide.
Content and activities in SAIP: The structure and key activities used within the 1-day SAIP developed by CORES reflect present public guidelines and research on effective gatekeeper suicide prevention programs. These programs13,30 are also organised on a five-part structure: preparing, connecting, understanding, assisting and networking. Guidelines for the public on assisting individuals contemplating suicide were developed through consensus with health professionals and people who have been suicidal19. The SAIP specifically addresses key issues for assisting individuals contemplating suicide: recognising the signs of distress, interpreting those signs and taking action by including them in role-play scenarios. The ABCD intervention used by CORES is lay-focused, and analogous to that of ALGEE (Approach/Assess/Assist, Listen, Give, Encourage help seeking, Encourage self-help) used in Mental Health First Aid31 and the LINK framework (Look for possible concerns, Inquire about concerns, Note level of risk, and Know referral resources) used by the US Airforce program13. Participants have responded positively to the repeated use of the river analogy in teaching, explaining and in intervention role-plays. The novel use of the funnel vision experience illustrates the sense of entrapment, impaired perspective and the inability to see a positive future felt by those at risk of suicide5,32. The program materials were rated highly, with particular comments made about their accessibility for a lay audience. This reflects CORES' decade-long efforts to write materials in a straightforward manner to accommodate the range of health literacy levels in rural areas.
CORES uptake and sustainability
The unique element of the CORES program, compared to models used by Lifeline and Beyondblue, is the focus on community engagement. CORES aims to strengthen communities through its network of activities that link individuals and groups across service organisations, schools and sporting teams. CORES promotes inter-community networking across the country and amongst training teams so that communities can learn and support each other. This growing community strength frees capacity within CORES so that it can continue work with new communities. CORES has been specifically engaged in some communities after drought or natural disasters because of its focus on community engagement and leadership rather than service delivery. The presence of active community leaders and active community organisations is the key to CORES' ability to work with communities. Not all communities are able to engage and sustain CORES, and attempts to build CORES within 12 other communities have stalled or failed. In several communities suffering a combination of drought, industry restructuring or downturn, business closures and increasing unemployment, service organisations and key community leaders have been overwhelmed and unable to take on further work to sustain leadership or funding to embed CORES.
Another indicator of CORES' success is its longevity and continuing interaction with community members. CORES has provided SAIP training to more than 4000 people in 24 communities around Australia, making it one of the largest and long-running programs of its type in Australia. Other rural mental health initiatives launched in response to drought and natural disasters in Australia have been service-focused and short term28,29. CORES leverages off existing community networks and organisations to form new relationships between them (eg linking service clubs with sporting clubs and school groups) to achieve its broader goals. In addition to creating new networks, CORES connects individuals in pursuit of a common goal (eg via the 1-day SAIP), and links people with services. This level of networking takes years to build. In 2012 more than half of CORES-trained team leaders over the past decade were still active in their communities, providing support and further SAIP training, even though CORES has moved from active community development to a support phase in many of those regions. Their longevity is due to the positive outcomes of CORES' community development philosophy.
Limitations to researching community-based approaches to mental health
Whilst evaluations have demonstrated the value of CORES, assessing its value to the community and impact on rural mental health is the next challenge. The use of community-based approaches for mental health promotion challenges program managers to select carefully between measures that are valued by health professionals, but that also reflect community level concerns as well as individual clinical and social outcomes. Evaluative models need to not only align with program goals, but also address community outcomes33. The complexity of the suicide phenomenon and nature of community gatekeeper suicide prevention programs challenges effective evaluation and research5,12. Suicide data, whilst available, is aggregated at the regional level and interpretation of data subject to many caveats. Thus even long-term impact evaluations of such programs is difficult. Whilst gatekeeper programs increase comfort and confidence in raising the issue of suicide with a person at risk, the retention of skills and effectiveness of translation into practice is unknown and an area for further work. CORES has a significant base of engaged communities, trainees and team leaders from which evidence can be obtained to address gaps in knowledge of community-based gatekeeper programs.
Conclusion
This study provides support for CORES as a community-based gatekeeper program. CORES builds community capital through establishing training teams, creating new connections across communities and linking people with services. The SAIP provides demonstrated increases in knowledge and confidence in the issues surrounding the prevention of suicide. Reports from community members confirm increased competence to recognise individuals at risk and respond appropriately with dialogue and referral.
Acknowledgement
CORES was developed with financial support of the Australian Government Department of Health and Ageing and the Tasmanian Community Fund. CORES received the 2007 Tasmanian Life Award, which recognises the role of individuals and organisations in promoting life and preventing suicide in Tasmania.
References
1. Martin G, Page A. National suicide prevention strategies. A comparison. Brisbane: University of Queensland, 2010.
2. Australian Bureau of Statistics. Causes of death, Australia, 2010. Canberra: ABS, 2012.
3. Judd F, Cooper AM, Fraser C. Rural suicide-people or place effects? Australian and New Zealand Journal of Psychiatry 2006; 40: 208-216.
4. Phillips A. Health status differentials across rural and remote Australia. Australian Journal of Rural Health 2009; 17(1): 2-9.
5. Stark CR, Riordan V, O'Connor R. Conceptual model for suicide in rural areas. Rural and Remote Health 11: 1622. (Online) 2011. Available: www.rrh.org.au (Accessed 25 March 2015).
6. Tonna AM, Kelly B, Crockett J. Improving the mental health of drought-affected communities: an Australian model. Rural Society 2009; 19: 296-305.
7. Kolves K, Milner A, McKay K, De Leo D. Suicide in rural and remote areas of Australia. Brisbane: Australian Institute for Suicide Research & Prevention, 2012.
8. Hirsch JK. A review of the literature on rural suicide: risk and protective factors, incidence, and prevention. Crisis 2006; 27: 189-199.
9. Crawford MJ, Kuforiji B, Ghosh P. The impact of social context on socio-demographic risk factors for suicide: a synthesis of data from case-control studies. Journal of Epidemiology and Community Health 2010; 64: 530-534.
10. Beautrais AL. Risk factors for suicide and attempted suicide among young people. Australian and New Zealand Journal of Psychiatry 2000; 34: 420-436.
11. World Health Organization. Towards evidence based suicide prevention programs. Manila: WHO (Western Pacific), 2010.
12. Mann JJ, Apter A, Bertolote J, Beautrais A, Currier D, Haas A, et al. Suicide prevention strategies: a systematic review. Journal of the American Medical Association 2005; 294(16): 2064-2074.
13. Isaac M, Elias B, Katz LY, Belik S, Deane FP, Enns MW, et al. Gatekeeper training as a preventative intervention for suicide: a systematic review. Canadian Journal of Psychiatry 2009; 54(4): 260-268.
14. Jorm AF, Kitchener BA, Sawyer MG, Scales H, Cvetkovski S. Mental health first aid training for high school teachers: a cluster randomized trial. BMC Psychiatry 2010; 10: 51.
15. Gould MS, Kramer RA. Youth suicide prevention. Suicide and Life-Threatening Behavior 2001; 31: 6-31.
16. Headey A, Pirkis J, Merner B, Huevel AV, Mitchell P, Robinson J, et al. A review of 156 local projects funded under Australia's National Suicide Prevention Strategy: overview and lessons learned. Australian e-Journal for the Advancement of Mental Health 2006; 5: 1-15.
17. Beautrais AL, Fergusson D, Coggan C. Effective strategies for suicide prevention in New Zealand: a review of the evidence. New Zealand Medical Journal 2007; 120: U2459.
18. Snashell R, Reusanna A. Health survey of the Kentish local government area of Tasmania. Hobart: ERS Consultancies, 2005.
19. Kelly CM, Jorm AF, Kitchener BA, Langlands RL. Development of mental health first aid guidelines for suicidal ideation and behaviour: a Delphi study. BMC Psychiatry 2008; 8: 17.
20. Department of Health and Ageing. Living Is For Everyone (LIFE): a framework for prevention of suicide in Australia. Canberra: Department of Health and Ageing, Commonwealth of Australia, 2007.
21. Rapp CA, Goscha RJ. The strengths model. A recovery oriented approach to mental health services. New York: Oxford University Press, 2012.
22. Davidson CL, Wingate LR, Rasmussen KA, Slish ML. Hope as a predictor of interpersonal suicide risk. Suicide and Life-Threatening Behavior 2009; 39(5): 499-507.
23. Walter G, Pridmore S. Suicide is preventable, sometimes. Australasian Psychiatry 2012; 20: 271-273.
24. SuccessWorks. CORES. Community Response to Eliminate Suicide. Evaluation review. Melbourne: SuccessWorks, 2011.
25. SuccessWorks. CORES. Community Response to Eliminate Suicide. Independent evaluation. Sheffield: Kentish Regional Clinic, 2009.
26. Seebohm P, Gilchrist A. Connect and include: an exploratory study of community development and mental health. London: National Social Inclusion Programme, 2008.
27. Taylor J, Wilkinson D, Cheers B. Working with communities in health and human service. Melbourne: Oxford University Press, 2008.
28. Wade D, Varker T, Coates S, Fitzpatrick T, Shann C, Creamer M. A mental health training program for community members following a natural disaster. Disaster Health 2013; 1: 1-4.
29. Hart CR, Berry HL, Tonna AM. Improving the mental health of rural New South Wales communities facing drought and other adversities. Australian Journal of Rural Health 2011; 19: 231-238.
30. Pisani AR, Cross WF, Gould MS. The assessment and management of suicide risk: state of workshop education. Suicide and Life-Threatening Behavior 2011; 41(3): 255-276.
31. Kitchener BA, Jorm AF. Mental Health First Aid: an international programme for early intervention. Early Intervention in Psychiatry 2007; 2: 55-61.
32. Ni Laoire C. Masculinity, responsibility and staying on the land in contemporary Ireland. Irish Journal of Sociology 2005; 14: 94-114.
33. Sainsbury P. The problems of evaluating a community psychiatric service. Community Development Journal 1976; 11(3): 215-229.




