Rural Australians continue to regard the GP as the preferred provider of medical care and the gateway to many additional health and medical services1. In carrying out their professional duties, GPs have traditionally maintained and operated their general practice essentially as a small business. Currently in rural and remote areas of Australia 84% of all practising GPs depend on fee-for-service or private practice salary for their primary source of income2.
Australia's free-market economy relies on the adequate distribution of private practitioner services across geographical regions to provide choice and ensure equity in provision of health services to small and isolated communities. Today, however, private practices in rural and remote communities seem to be increasingly unattractive to existing and prospective GPs. Despite a raft of recruitment and retention initiatives, medical workforce shortages continue in rural areas, exacerbated by an ageing workforce3,4. Due to the shortage of doctors willing to take up rural practice many of these communities now depend on salaried practice arrangements, or overseas-trained doctors practising on restricted provider numbers, to meet their primary care needs5,6. (Several sources detailing Commonwealth government arrangements determining rural general practice in Australia are available on-line3,6.)
The loss of GPs as private practitioners in rural areas may exacerbate the already generally poorer health outcomes of rural residents. It can mean loss of choice and procedural skills in the local community, and reduce the availability of after-hours activity and flexibility in the way services are delivered. Much rural health services research has focussed on education, recruitment and retention issues, with workforce initiatives emerging to address these areas7-11. To date, the workforce implications of the operation of rural practices as small businesses have received relatively little attention in large scale studies. One way to enhance both rural workforce recruitment and retention initiatives is through systemic measures which support and sustain practice viability. Implementation of such measures necessitates an understanding of what factors GPs, as business operators, see as contributing to and threatening practice viability, and whether the importance of these factors varies significantly according to geographical context.
The present study addresses three questions from the perspectives of private GPs currently practising in non-metropolitan communities:
- What are the key factors that contribute to practice viability in rural areas?
- What factors threaten practice viability in rural areas?
- Do viability factors vary according to the degree of rurality or geographical remoteness?
Rural general practice can be considered a business opportunity, the viability of which may depend on prevailing conditions affecting market demand, workforce supply, potential income and other returns and legislative and compliance requirements. The focus of this article is on the systemic problems that may impact on rural and remote practice, rather than on issues that may be relevant only to particular doctors or communities.
Methods
Based on an extensive review of the literature and a Delphi-type exercise, the following definition of a viable rural general practice was adopted:
A viable rural general practice is defined as one which meets the particular medical needs of the community by providing appropriate services in a way that takes account of the financial and personal costs to both the practitioner and the community at large12.
Data
The data were collected as part of a national study into the viability of rural general practice undertaken jointly by the Rural Doctors Association of Australia and Monash University School of Rural Health Bendigo12. Using an address list provided by the Health Insurance Commission all general practitioners providing non-referred services on average one day per week or more in RRMA 3 - 7 communities (Table 1) were surveyed. Two open-ended questions relating specifically to practice viability were included in the national questionnaire, namely:
- What are the key factors contributing to the viability of your practice?
- What factors would put the viability of your practice at risk?
Because this analysis focuses specifically on issues relating to practice viability, only the responses of practitioners with some financial interest in the practice, beyond that from a salary or contract earnings, are included - specifically practice principals, partners or associates.
Rurality indicator
The Rural Remote and Metropolitan Area (RRMA) classification was used as the indicator of rurality13 (Table 1). This taxonomy is the basis for considerable government funding to general practice, differentiated by level of rurality or remoteness, as for example with the Practice Incentives Program14.
Table 1: Rural, Remote and Metropolitan Areas classification for communities: population sizes for rural and remote categories

Analysis
Survey responses were analysed using qualitative content analysis. Coding categories generated from the data were continuously modified during the coding cycle, as required to accommodate new responses15. These categories of similar and related responses formed the basis for aggregation into broader viability factors or dimensions. This data reduction step maintained the integrity of the original responses while allowing them to be analysed under headings generated from the original data and consistent with the practice viability factors discussed in the literature.
Statistical analysis included comparisons across rural categories (RRMA 3 to 5), across the two remote categories (RRMA 6 & 7), and between all combined rural categories and the combined remote categories. The c2 tests for linear association across the RRMA categories and the Fisher exact tests were conducted using SPSS vers. 11 software (SPSS Inc; Chicago, IL, USA).
Results
A response rate of 35% of practitioners, representing 53% of practices, was obtained from the national survey. In general, the responses were broadly representative of the distribution of doctors across RRMA categories12. A total of 1050 respondents from the national survey of rural and remote GPs nominated themselves as a principal, partner or associate in their practice. The characteristics of these respondents who formed the basis for this study are shown (Table 2).
Table 2: Characteristics of respondents with a financial interest in their practices

What were the key factors contributing to practice viability in rural areas?
The 944 respondents to this question generated 2325 responses which were coded into 78 separate categories. These categories in turn were aggregated into seven major factors contributing to practice viability (Table 3).
Table 3: 'What are the key factors contributing to the viability of your practice?', by RRMA. Percentage of responding doctors mentioning each factor. Factors aggregated from free text responses
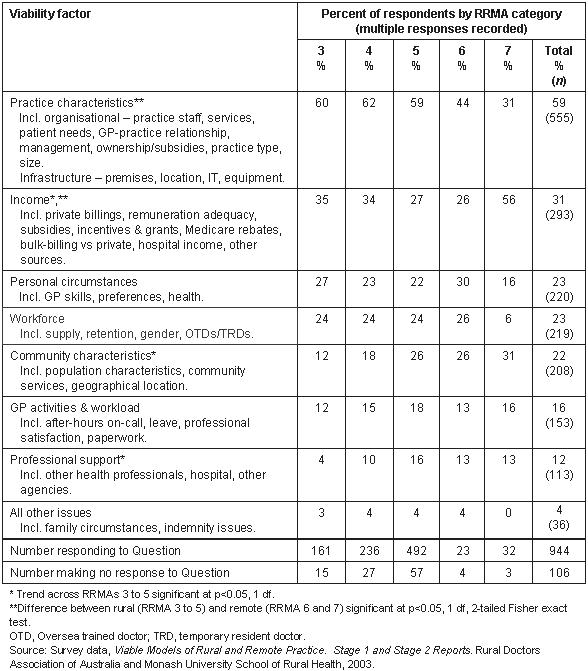
More than half of all GPs (59%) who responded to this question regarded at least one aspect of practice characteristics as important in contributing to the viability of the practice. This factor includes items relating to practice premises, facilities and infrastructure, organisation and management and patient services. The most common items included reference to the characteristics of practice staff (14% of respondents), having a sufficient number of patients (11% of respondents), good practice management and efficiencies (9% of respondents) and good working relationships between partners (7% of respondents).
Income (including Medicare rebates, hospital income, bulk-billing and private billing practices and incentive payments) was nominated as a key factor of practice viability by 31% of respondents. The most frequent items here referred to private billings or realistic fees (11% of respondents), with 10% referring to adequate remuneration.
Personal circumstances, workforce issues and community characteristics were each nominated by about 23% of respondents, with GP activities and workload, and issues of professional support, identified by fewer GPs as contributing to practice viability.
What factors threaten practice viability in rural areas?
The 939 respondents provided a total of 2242 responses which were initially coded into 87 categories. These were aggregated to eight factors which GPs identified as putting the viability of their practice at risk (Table 4).
Table 4: 'What factors would put the viability of your practice at risk?', by RRMA. Percentage of responding doctors mentioning each factor. Factors aggregated from free text responses
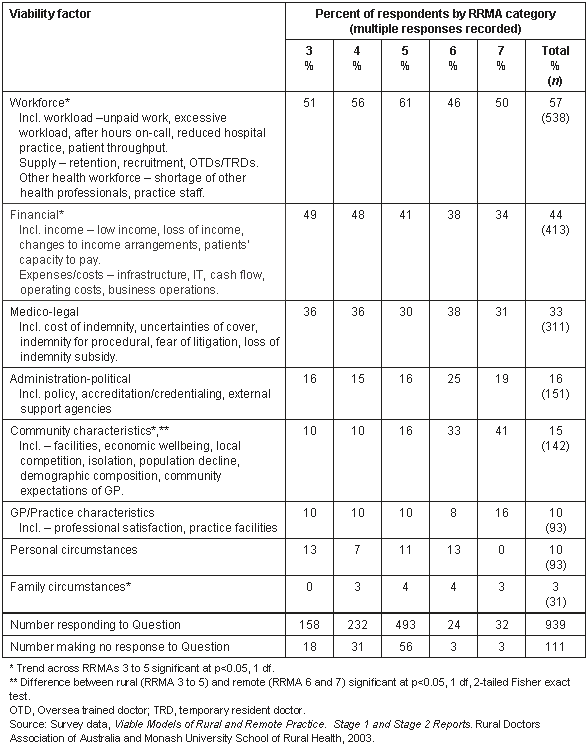
Workforce was clearly the most important factor considered to threaten practice viability, nominated by 57% of practitioners. Workforce supply items of doctor retention (21%) and recruitment difficulties (9%) were the most frequently mentioned. Workload issues included unpaid paperwork (8%) and loss of hospital work due to downgrades or closure (5%).
Many respondents (44%) identified financial issues that threaten practice viability, with both income and expenses or costs mentioned. Inadequate Medicare rebate was cited by 16% of respondents, inadequate remuneration by 11%, and increases in practice costs by 14%.
Medico-legal issues were raised by one-third of respondents. These issues concerned the cost of indemnity cover (18%) and concerns over the uncertainty of cover and collapse of insurers (13%).
Fewer respondents nominated administration-political issues, community characteristics, GP/practice characteristics and personal and family circumstances.
Do viability factors vary according to the degree of rurality or geographical remoteness?
Rural community comparisons, RRMA 3 - 5: Regardless of the size of the population centre within rural areas (as measured by RRMA 3 - 5), there was a high degree of agreement in the order of the percentages of respondents nominating each of the factors identified as contributing to the ongoing viability of the practice. The magnitude of the percentages differed significantly by the size of the population centre for the following factors: income (which was lower in smaller communities), community characteristics (which was higher in smaller communities), and professional support (which was higher in smaller communities).
In relation to threats to viability, GPs in rural (RRMA 3 - 5) areas agreed that workforce issues presented the greatest risks, with many identifying financial and medico-legal issues regardless of community size. The magnitude of the percentages was statistically significantly higher for the smaller population centres for community characteristics, workforce and family circumstances. The percentages nominating financial issues were statistically significantly higher in the larger population centres.
Remote community comparisons, RRMA 6 & 7: Unfortunately, the low number of respondents from remote (RRMA 6 & 7) areas precludes even moderate differences being statistically significant.
Although there were relatively few respondents from remote (RRMA 6 & 7) areas, doctors in these communities appear to share similar perceptions to doctors in rural areas about which factors contribute to or threaten the viability of their practices. Compared with rural GPs, a smaller percentage of doctors in remote areas identify practice characteristics as contributing to practice viability and a higher percentage identify community characteristics as threatening practice viability. Compared with rural GPs, those in remote areas were more likely to identify income as a key factor contributing to practice viability. As Table 3 shows, this difference is accounted for by RRMA 7 doctors alone. The difference between RRMA 6 and 7 in the proportion of doctors nominating workforce as a contributing factor, while large, is not statistically significant.
Discussion
The results of this study provide valuable insight into the importance of distinguishing between factors that contribute to and threaten practice viability. Doctors clearly identify appropriate organisation and management of their practices as the major factor influencing their ongoing practice viability, particularly given their need to maintain income levels and ensure personal wellbeing in the presence of workforce supply difficulties that often lead to onerous and unreasonable workloads.
The greatest threat to practice viability perceived by doctors across all degrees of rurality relates to workforce and workload issues, including the need for recruitment and retention of appropriately trained medical staff in adequate numbers to allow reasonable workloads, time off and professional support. It is important to note that rural workforce undersupply not only affects communities without the services of a GP, but also threatens the viability of existing rural practices, especially those where GPs work unsustainable hours due to a lack of professional relief.
Following workforce and workload issues, financial factors emerge as the biggest threat to rural practice viability. This finding indicates that economic considerations are critical components of the quest to ensure the viability of rural practices. Merely obtaining more doctors to practise in communities whose population cannot afford to make substantial co-payments may help to reduce working hours per doctor to manageable levels but may simultaneously result in insufficient income to support existing doctors, in turn threatening practice viability. Aside from the argument that non-metropolitan GPs undertake more complex activities and thus warrant differential remuneration16,17, the issue of the adequacy of existing rebate levels against constantly rising practice costs in rural areas clearly requires further investigation.
The findings suggest a broad consensus across rural and remote communities in the relative importance of factors perceived by doctors to affect the viability of their practices. Some differences in the magnitude of the percentage of respondents nominating the various viability factors were observed across communities of differing degrees of rurality or remoteness.
The greater relevance of professional support to doctors in smaller rather than larger rural communities may be a response to recent trends to downgrade or close small rural hospitals. The lesser significance to doctors of income as a contributor and financial issues as threats to practice viability, as rural town size decreases, may indicate the presence of greater competitive pressures in larger towns. It may also indicate the need for and importance of current financial support initiatives, differentiated by a rurality and remoteness loading, which shift the focus from financial to other factors. In small isolated RRMA 7 communities, where GP services are often heavily subsidised, income is seen as of major significance as a contributor to viability and may in fact be the only incentive which attracts doctors to the location. In this case, as was observed, financial issues such as the net return from GP services and the patients' capacity to pay are less likely to be identified as threats to viability.
The increased percentages nominating community characteristics as both contributing to and threatening viability as community size decreases is unsurprising, given that smaller communities are likely to have fewer community services and facilities, fewer doctors and an ageing population with greater healthcare needs. Populations may also be in danger of declining below the critical minimum for supporting a single doctor.
The increasing percentage of GPs across RRMA 3 to 5 nominating workforce as a risk factor, confirms the difficulties with workforce recruitment faced by small communities and the consequent increased workload for existing practitioners.
Limitations
The response rate for the national survey was 35% of individual GPs, but respondents represented 53% of all Australian rural and remote general practices. While GPs within a practice may differ in their opinions as to the factors relevant to viability, all respondents had some proprietorial interest in the practice. The results reported here, therefore, represent the GP perspective on a majority of Australia's rural and remote practices.
The results reflect the views of GPs in rural and remote communities as to the factors affecting the viability of their practices. Other experts might identify different priorities. The findings are relevant because these are the factors which GPs will consider when assessing the current or future viability of a practice, whether their own or one they may consider joining.
Conclusion
Practice viability in rural and remote communities is a critical aspect of ensuring the access of residents to primary medical and health care. Given the importance of equitable access to health care as the basis for improving health outcomes, the need to implement measures to improve and maintain the viability of rural practices is paramount. While a primary component of practice viability is clearly economic, specifically income from consultations, the strong inter-relationships between viability factors should not be overlooked.
Only through the adoption of a systems solution, in which the drivers of change and the inter-relationships between factors are clearly recognised, will the provision of adequate and effective primary medical care provided through viable practices to rural and remote communities be assured. Systemically based initiatives which take account of differences in the nature and complexity of activities according to degree of remoteness or rurality will improve the net return from rural practices, something which in turn will increase the attractiveness of rural practice and make it feasible for extra doctors to share the workload without significantly reducing the net income of existing doctors. In conjunction with other initiatives which will ensure a sufficient workforce supply, benefits will flow in the form of increased retention and reduced burnout of existing and future rural GPs. Other related initiatives which address practice organisation and management issues will also contribute to continuing practice viability, but only once the threats to practice viability have been addressed.
Acknowledgements
The study on which this analysis is based was funded by a grant from the Australian Government Department of Health and Ageing, under the auspices of the Rural Doctors Association of Australia (RDAA) in association with Monash University School of Rural Health Bendigo. The authors gratefully acknowledge the input and assistance of the following: Dr David Mildenhall, Dr Paul Mara, Dr Bruce Chater, Dr Nola Maxfield, Dr David Rosenthal, Mr Brian Curren and Ms Anna Boots of the Viable Models Project Committee of the RDAA, Health Connections and technical assistance from Ms Vanessa Prince of Monash University.
References
1. Smith K, Humphreys J, Lenard Y, Jones J, Prince V, Han G. Still the doctor - by a country mile! Preferences for health services in two country towns in north-west New South Wales. Medical Journal of Australia 2004; 181: (in press).
2. Australian Rural and Remote Workforce Agencies Group, Reality Bites: Rural and remote GP workforce information. Deakin, ACT: National Centre for Epidemiology and Population Health, ANU, 2003.
3. Department of Health & Aged Care. General Practice in Australia 2000. Canberra: Department of Health & Aged Care, 2000. Available: http://www.health.gov.au/pcd/publications/gpinoz2000/ (accessed 16 June 2004).
4. Australian Medical Workforce Advisory Committee. The General Practice Workforce in Australia. AMWAC Report 2000.2. Sydney, NSW: AMWAC, 2000.
5. Australian Medical Workforce Advisory Committee. Temporary Resident Doctors in Australia. AMWAC Report 1999.3. Sydney, NSW: AMWAC, 1999.
6. Commonwealth Department of Health and Aged Care. The Australian Medical Workforce. Occasional Papers: New Series No. 12, 2001. Canberra: Department of Health and Aged Care, 2001. Available: http://www.health.gov.au/pubs/hfsocc/ocpanew12a.htm (accessed 16 June 2004).
7. Durham G, Durham J. Building the Australian Rural Health Workforce. Rural health in New Zealand and Australia Part 2. Healthcare Review 4(1). (Online) 1999. Available: http://www.enigma.co.nz/hcro/website/index.cfm?fuseaction=articledisplay&featureid=96 (accessed 31 March 2004).
8. Humphreys J, Jones J, Jones M, Hugo G, Bamford E, Taylor D. A critical review of rural medical workforce retention in Australia. Australian Health Review, 2001; 24: 91-102.
9. Humphreys J, Jones M, Jones J, Mara P. Workforce retention in rural and remote Australia: determining the factors that influence length of practice. Medical Journal of Australia 2002; 176: 472-476.
10. Rabinowitz HK, Diamond JJ, Hojat M, Hazelwood CE. Demographic, educational and economic factors related to recruitment and retention of physicians in rural Pennsylvania. Journal of Rural Health 1999; 15: 212-218.
11. Wilson D, Woodhead-Lyons S, Moores D. Alberta's rural physician action plan: an integrated approach to education, recruitment and retention. Canadian Medical Association Journal 1998; 158: 351-355.
12. Rural Doctors Association of Australia and Monash University School of Rural Health. Viable Models of Rural and Remote Practice. Stage 1 and Stage 2 Reports. Canberra, ACT: Rural Doctors Association of Australia, 2003.
13. Department of Primary Industries and Energy and Department of Human Services and Health. Rural, Remote and Metropolitan Areas Classification 1991 Census Edition. Canberra, ACT: Australian Government Publishing Service, 1994.
14. Commonwealth Department of Health and Aged Care. An Outline of the Practice Incentives Program July 2001. Canberra: DHAC, 2001. Available: http://www.hic.gov.au/providers/incentives_allowances/pip.htm (accessed 29 April 2004).
15. Sandelowski M. Whatever happened to qualitative description? Research in Nursing & Health 2000; 23: 334-340.
16. PriceWaterhouseCoopers. Medicare Schedule Review Board A resource-based model of private medical practice in Australia - final report. PWC: 2000.
17. Humphreys J, Jones J, Jones M, et al, The influence of geographical location on the complexity of rural general practice activities. Medical Journal of Australia 2003; 179: 416-420.


