Background
In Norway, hospitals and specialist healthcare services are organized at the state level, while the municipalities are responsible for primary healthcare services. In a nationwide patient list system general practitioners (GPs) are mainly appointed as mixed public-private practitioners and more seldom as employees with a fixed salary. The latter option is mainly used in rural areas like Senja. Senja is the second largest island in Norway with an area of 1586 km2, located in the northern part of the country (Fig1). The island encompasses four municipalities, three small (Berg, Torsken and Tranøy) with populations of 880-1500, and one larger municipality (Lenvik), which is partly located on the mainland and has a population of about 11 300. Driving distance to the nearest hospital, the university hospital of Tromsø, is 160-230 km. Driving time is 2-3 hours. Fishing, fish farming and fishing industry are essential to employment in the three small municipalities.
Norwegian studies in the 1990s showed that doctors in rural and remote municipalities experienced heavier workloads and more professional isolation than peers elsewhere1,2. Short temporary employment of locums and high turnover of doctors were common. This situation was certainly true for Senja, where people living in the small rural communities experienced deteriorating continuity and quality of health care due to the problems with recruiting and retaining of GPs. The main response among the municipal authorities had been to turn to commercial recruitment agencies for help, and most often this resulted in rather expensive short-term locums. Specific offers such as extra wages, low household costs and reduced workload had been tried without improving the situation. A report from a previous mayor documenting that around 100 different GPs had been appointed during a period of 11 years may well illustrate the difficult situation. This raised great concerns in the public, among politicians and municipal healthcare authorities. It also concerned state healthcare authorities represented by the county medical officer of Troms, who proposed a collaborative system intervention in order to improve the situation.
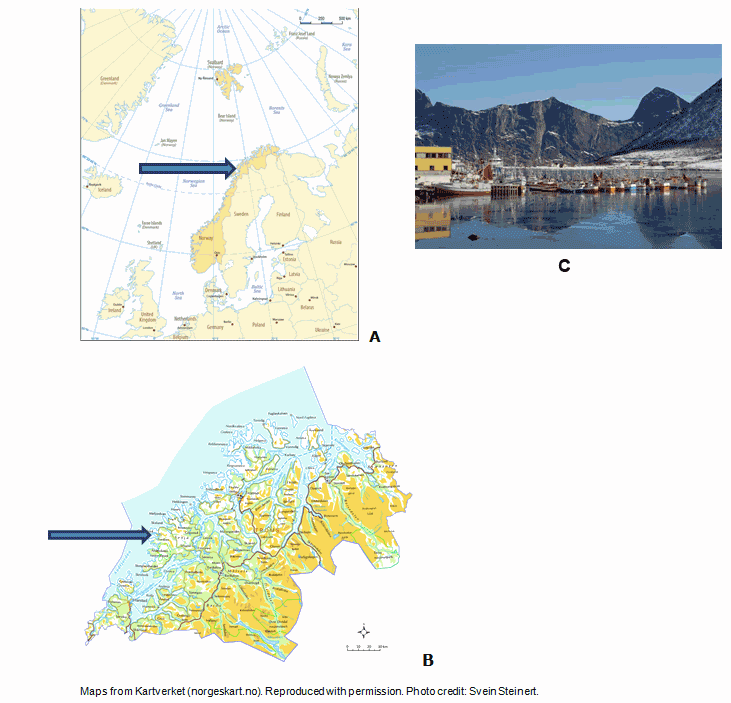
Figure 1: Maps of (A) Norway and neighboring countries and (B) Senja and adjacent mainland. Arrows show location of Senja. (C) The fishing village of Senja.
2001: First intervention attempt
In 2001 the proposal from the county medical officer (regional representative for the national health authorities) was published in a report, The Senja Doctor, with recommendations for improvements3. This report outlined several models for a joint municipal GP service involving all four municipalities. One common objective for all models was to create stronger professional teams to prevent the isolation that rural doctors face. The report was discussed in the four municipal councils and rejected by all of them. Even though the situation was in no way acceptable, with GP service driven by short-term locums, the municipalities were resistant to changes that could imply losing control over their own GP services.
2007: Second intervention attempt
In 2007, when problems were still unresolved and escalating, the mayor of one small municipality (Torsken) eventually turned to the larger municipality (Lenvik) for collaboration. Key professionals in the two municipalities used the now obvious lack of sustainability to start a collaborative process, focusing on the shared perception of a need for change and mutual trust between the stakeholders. This was the turning point that facilitated the process of restarting and realizing the Senja Doctor project. The process has included core elements as listed in chronological order below:
- A joint application was sent to an external body for economic support of the project. Support was granted as applied.
- A steering committee including local politicians and administrators was established. Academic resources in the form of a key professional from the National Centre of Rural Medicine (NCRM) University of Tromsø joined the committee as external advisor.
- A local inter-professional working party was formed for the purpose of developing models for partnership and cooperation, and to secure adequate professional information and adjustments in the process.
- A series of minor preparatory meetings preceded a major introductory seminar, where representatives from all four municipalities in the Senja region and key representatives from the national and regional authorities and NCRM were present.
- During the introductory seminar the two remaining and until then reluctant municipalities finally declared their interest to join the Senja Doctor project.
- From early 2008 the steering committee and working group were completed with members from all four municipalities in a joint team building process.
The joint GP service is today named in Norwegian Senjalegen ('the Senja Doctor')
Terms of recruitment to Senjalegen
The aim of the project was to establish working conditions that would attract young doctors to stay in the region for longer periods of time.
The members of the local working party realized that the main obstacles for young doctors when considering moving to and staying in the region for a longer period of time were not only the workload but also the professional isolation and the lack of guidance from more experienced colleagues. It was also realized that it would not be possible to establish a sustainable system for guidance and support for young doctors without more extended inter-municipal cooperation.
According to this, the following terms were suggested, and accepted by the steering committee.
- Linking service of four remote surgeries together by a newly built main surgery at a strategic location.
- Four GPs and two interns will work in the main surgery most of the time.
- Remote surgeries will be served 1-2 days per week by a GP accompanied by an intern/junior doctor.
- Fair payment according to own preferences: fixed salary or fee for service.
- Reasonable workload, patient lists somewhat below official recommendations.
- Restricted on-call duties and out of hours work: an agreement among six neighboring communities about mutual emergency services will ensure a fairly moderate out-of-hours work load for individual doctors.
- Funds and opportunities for research as an integrated part of work.
- Participation in professional networks.
- Participation in specialist education programs for GPs.
- Driving included in working time.
The terms listed above gave rise to the final model of Senjalegen with an average workload of 37-40 hours per week for each GP. Out-of-hours service (1530-0800) is usually twice a month for week days and one weekend day every month. One day every week is allocated for team building objectives, with all doctors gathered in the main office for meetings, guidance and professional support.
Outcomes
Turnover of GPs
As previously mentioned approximately 100 different doctors had come and gone during a period of 11 years, in the time period from 1998 and 2009. After the introduction of Senjalegen nine GPs have since been employed as doctors on an ordinary contract. This represents a significant reduction in turnover rate. Although there is still a need for locums, this is quite moderate and mainly due to working rights of those already employed, such as maternity leave and for educational purposes. By the end of 2013 all positions in Senjalegen were held by doctors who have expressed their intentions to stay.
Doctors' views
In a group discussion the young doctors presently employed in Senjalegen unanimously stated that they would not have sought positions in this rural area if it had not been for the working conditions given. Working alone in a small municipality was not an option for any of them. The two comments below may well exemplify the experiences and attitudes revealed in this group discussion.
Senjalegen gives you the possibility to live more centrally which increases the possibility for spouses to get a job.
It is a great value to be part of a professional network, where you can seek guidance and discuss difficult cases
Views of politicians and administrators
In a recent interview, the former mayor of Torsken municipality, the person who first took the initiative to establish Senjalegen, emphasized the unacceptable situation prior to the establishment, with inferior quality of GP services. He was satisfied with the start and the outcome of the Senjalegen process. His only concern is that the surgeries of the remote municipalities are attended to fewer days than he had expected.
In another interview the mayor and the municipal director from the municipality of Tranøy stated that Senjalegen has contributed to the improvement and continuity of GP services to the inhabitants of Tranøy (municipality). The organization model with four collaborating municipalities was challenging, but nevertheless successful.
Since Senjalegen was launched in full scale in 2009 the steering committee has consisted of the municipal directors from the four collaborating municipalities. The feedback from the directors has been that of consistent satisfaction concerning the service provided by Senjalegen.
Discussion
The final structure and function of Senjalegen was very similar to that previously suggested by the county medical officer 10 years ago. There may be many different reasons as to why it was possible to implement a structural change in 2009, whilst the same proposal was turned down in 2001. We think the main reasons are related to history and tradition, a shared acknowledgement of the need for change and how the process of change was accomplished.
History and tradition
Norway has a long history of extensive autonomy for the municipalities, including responsibility for primary healthcare and social services. The belief that every municipality should have its own GP is profound and well established. That is probably one reason for the resistance towards organizing an inter-municipal GP service, and why the attempt from the medical officer in Troms county did not succeed in 2001.
Need for change
Local leaders and healthcare professionals recognized that the rapid turnover of short-term locums was expensive and did not provide an acceptable quality of care for the inhabitants. It was acknowledged that good wages, reasonable workload and subsidized housing were not sufficient to ensure a continuous and sustainable GP service. In the past all three small municipalities had experienced periods of stable GP coverage, and thus knew the importance of continuity in the GP service. The demand for a more continuous GP service, and the inability to achieve this within the present framework of the small municipalities, favored the development of an inter-municipal service. The terms for recruitment proposed in the project, including the elements especially appreciated by the young doctors working at Senjalegen (as described in their interview), are well in accordance with international research and recommendations4. To be included in a collegial group promoting professional development has been shown to prevent isolation and foster retention in Finnmark, a Norwegian rural county north of Senja5.
Process of change
As mentioned, the municipal autonomy has traditionally given both politicians and the population a sense of control over the level of service in the community. The prospect of losing control was probably an important part of the resistance against the change suggested in 2001. In 2007, on the other hand, there was a greater feeling of ownership over and participation in the process, because the politicians and administrators themselves were in charge of the progress and the decisions. Being able to take part in the project from the beginning and establishing a new primary healthcare service from scratch created an atmosphere of confidence between politicians, administrators and healthcare professionals. This contributed to a process where political, administrative and professional aspects were ensured. In a recently published book, Senjalegen has been scientifically recognized as an example of an innovative inter-municipal process6.This process has contributed to stabilizing doctors and to securing safe and predictable health care for the rural and remote communities of Senja. The expectations are that this will also lead to improved continuity of GP care, which in turn has been shown in other studies shown to increase patient satisfaction and reduce the use of specialist services7,8.
Conclusions
A general conclusion from Senjalegen is that the processes of changing healthcare services should be based on local involvement and control. Models for inter-municipal healthcare services should be developed in an environment of mutual participation and cooperation between politicians, administrators and the healthcare workforce. Senjalegen also shows evidence that young doctors prioritize professional support and teamwork over income level, as motivation for long-term commitment in rural areas.
Acknowledgement
The authors thank Elisabeth Swensen and Kristina Shanley for reading and commenting on a draft of this article.
References
1. Andersen F, Forsdahl A, Herder O, Aaraas IJ. Lack of doctors in rural districts - the situation in Northern Norway. (English summary) Tidsskr Nor Lægeforen 2001; 121: 2732-2735.
2. Andersen F, Herder O, Forsdahl A. Kommunelegetjenesten i Nord-Norge 1995-97. [Municipality medical service in Northern Norway 1995-97] (English summary). Tidsskr Nor Lægeforen 1999; 119: 1296-1298.
3. Fylkeslegen i Troms. Senjalegen - en utredning om interkommunal legetjeneste i Troms. [The Senja Doctor - a report about inter-municipal medical services in Troms County]. (In Norwegian). (Online) 2001. Available: http://www.nsdm.no/filarkiv/File/Eksterne_rapporter/SENJALEGEN_QmfHP.pdf (Accessed 7 August 2015).
4. World Health Organization. Global policy recommendations 2010: increasing access to health workers in remote and rural areas through improved retention. Available: http://whqlibdoc.who.int/publications/2010/9789241564014_eng.pdf (Accessed 7 August 2015).
5. Straume K, Søndenå MS, Prydz P. Postgraduate training at the ends of the Earth - a way to retain physicians? Rural and Remote Health 10: 1356. (Online) 2010. Available: www.rrh.org.au (Accessed 7 August 2015).
6. Ringholm T, Teigen H, Aarsæther N (eds). Innovative municipalities. (In Norwegian). Oslo: Cappelen Academic Press, 2013.
7. Hansen AH, Halvorsen PA, Aaraas IJ, Førde OH. Continuity of GP care is related to reduced specialist health care use: a cross-sectional survey. British Journal of General Practice 2013; 63(612): 482-489.
8. Hjortdahl P, Laerum E. Continuity of care in general practice: effect on patient satisfaction. British Medical Journal 1992; 304: 1287.

