The burden of chronic diseases is rapidly increasing worldwide1. In Australia rural populations have a greater burden of disease2. Chronic diseases are largely preventable with diet as a key risk factor. With respect to diet-related chronic disease, dietary risk may be due to poor food access, namely, poor availability and/or the high cost of healthy food. It is likely that poor food access is an issue in rural areas. ________________
The most recent and comprehensive study of rural food access in Australia was conducted in the state of Queensland in 20033. This found the price of food was directly related to remoteness, as measured by the Accessibility Remoteness Index of Australia (ARIA)4. In this report the majority of the towns surveyed were remote or very remote, that is, there was a highly restricted accessibility of goods, services and little opportunity for social interaction (ARIA)4. However for many rural Australians there is only relatively limited restrictions to access to goods and services, that is, they have good road access to regional service centres and opportunities for social interaction. There have been no food access studies in these rural communities. The current study was undertaken to determine access to a healthy food basket (HFAB) in south-western (SW) Victoria, Australia (Figure 1). The majority of the towns in this area have been classified as highly accessible or accessible (ARIA). The area is characterised by a high prevalence of coronary heart disease (CHD)2. Our hypothesis was that food cost and availability in rural areas that are accessible not remote would be determined by proximity to a town serviced by a major food retail chain.
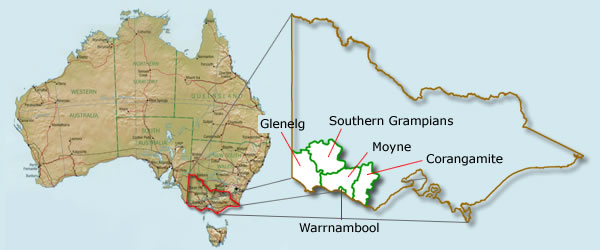
Figure 1: Map of the study area in south-western Victoria, Australia.
Methods
A cross-sectional survey was conducted of the costs and availability of a standard selection of a basket of healthy food choices. Also surveyed were the availability and cost of certain popular family food purchases and tobacco and take-away food items. The survey was conducted in stores that sold food at locations across five shires in SW Victoria: Glenelg, Warrnambool, Corangamite, Southern Grampians and Moyne.
Selection of stores
All supermarkets and grocery stores across the five shires were located via the Yellow Pages® telephone directory and their managers were invited to participate in the survey. All towns surveyed were classified as highly accessible or accessible according to ARIA. This indicates minor or relatively unrestricted access to goods, services and opportunities for social interaction in a regional service centre4.
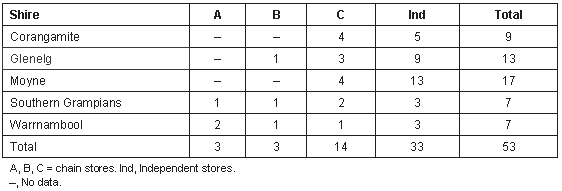
All food-related premises in towns with a population in excess of 100 persons were considered eligible. There is no complete database of stores across SW Victoria. In the absence of a list, the Yellow Pages® was searched electronically under the following headings: supermarkets, grocery stores and food/general stores. This list was cross-checked with local government area (LGA) records that list those stores serving cooked or chilled foods. All of these food stores must be registered under the Food Act 1984 with the LGA. Seventy-two percent of the eligible supermarkets and grocery stores in SW Victoria participated in the survey. The final survey sample was 53 shops in 42 towns across the five shires. The type of store was recorded as one of three major supermarket chains (A, B, C), or independent. The distribution of store types with respect to shire is given (Table 1). The towns surveyed were recorded as having one or more grocery stores. In addition, data have been collected separately using the same methodology to measure access and cost of HFAB from 11 supermarkets in the Municipality of Banyule in urban Melbourne (C Burns, unpubl. data, 2002). These data are presented as a comparison to the rural data.
Table 1: Distribution of store type across the shires
Foods in the Healthy Food Access Basket
The range and types of food included in the HFAB used in the present study were selected to represent commonly available and popular foods, rather than the nutritional ideal. The current study used the same list of foods that had been used in the 2000 Queensland HFAB Study3. The HFAB is made up of 44 foods (Appendix I). Model B of the Core Food Groups was used as the nutrient/dietary basis for the HFAB5. The total amount of food in the HFAB meets the nutritional requirements of a family of six people for 2 weeks and provides 70% of dietary requirements for all nutrients except energy. Energy rich, 'non-core foods (margarine, oil and sugar) were added to bring the energy content to 95% of the requirements. The basket contains choices consistent with a healthy heart diet3. The family consists of: an adult male (over 19 years), an adult female (over 19 years), an older woman (over 61 years), a teenage boy (aged 14 years), a girl (aged 8 years) and a boy (aged 8 years). It must be noted that though Model B of the Core Food Groups was used as the nutrient base for the HFAB, the HFAB was product-specific, meaning no generic brands were used. Generic brands were excluded because many small independent stores do not have the advantage of purchasing these brands and equal comparisons were sought across SW Victoria.
Takeaway and tobacco
In addition to the HFAB foods, access to the following items was measured: two commonly eaten takeaway foods (a meat pie and a can of Coke?)6 and two tobacco items (a packet of tobacco and a packet of cigarettes).
Popular supermarket food purchases
Ten foods (Appendix I) that fell in the list of top 100 items purchased in supermarkets in Australia within 2000 were also surveyed6. While many of these items were not healthy, these foods represented the most common retail food purchases in Australia. Access to and cost of these unhealthy but popular foods offered a comparison to access to the basket of healthy foods (HFAB) and an indicator of food security (ie, access to any food in rural communities).
Survey
The survey was carried out by eight final-year Masters of Nutrition and Dietetics students. Data were collected from March to April 2002. Data were collected according to a previously reported protocol3.
Ethical issues
The information collected in this survey was considered in the public domain. No towns or stores were directly named. All data were coded to protect the names of individual stores and stored in secure facilities at Deakin University, Victoria, Australia.
Analysis
The sample included all stores from which a minimum of 88% of the basket was available; that is, no more than five items were missing (n = 27). In these stores, the availability of the HFAB was determined relative to shire, store type and number of stores in a town. Statistical significance for these calculations was determined using c2 tests using SPSS (SPSS Inc, Chicago, IL, USA).
For the calculation of the total cost of the HFAB for missing items, we inserted mean cost of that item for the total sample. The total cost for the HFAB in each store for which 88% of the items were available was calculated by multiplying the cost per g for each item with the quantity required to match the HFAB content specified by the current study. Statistical differences between shires were determined by ANOVA, using SPSS.
Results
Store distribution
The distribution of store types by shire is given (Table 1). With the exception of one store in Glenelg, all major chain (A, B) stores were located in Southern Grampian and Warrnambool. The minor chain C and the independent stores were concentrated in Corongamite, Glenelg and Moyne. In 20 of the 42 towns surveyed, there was only one grocery store or supermarket. Only five of these 20 lone grocery stores were chain stores. The majority of stores (15 of 20) in one-store towns were independent.
Availability
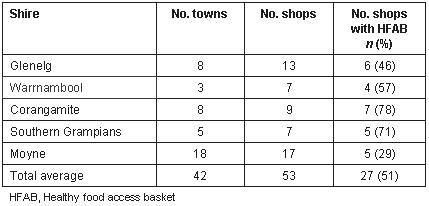
Fifty-one percent (27 of 53) of the surveyed shops in SW Victoria could supply the majority (>88%) of the HFAB (ie, have no more than five of the 44 items missing). In the shire of Corangamite, 78% of stores could supply the HFAB, while in Moyne, only 29% could supply the HFAB (Table 2). The HFAB was statistically more likely to be available in one of the three chain stores (c2 30.93, p<0.000). The HFAB contents were significantly less likely to be available in an independent store in a one-store town (c2 = 10.00, p = 0.002).
In contrast to these figures, a meat pie, a can of Coke, a block of chocolate, a packet of spaghetti and a packet of cigarettes were all available in over 90% of the shops surveyed.
Table 2: Availability of Healthy Food Access Basket in surveyed supermarkets and general stores
Cost
The average cost across SW Victoria for the HFAB was $380.30 ± $25.14 (mean ± SD). The lowest individual price was $335.77 (large chain supermarket in a service centre) and the highest individual price was $444.50 (independent store). While there was a mean cost range of $36.91 across the shires of SW Victoria, there was no statistical difference between the shires for mean costs of the HFAB. While there was no difference in the average mean cost of the HFAB between SW Victoria and urban Melbourne ($380.80 ± 30.40).
When the cost of the HFAB is determined relative to store type, the price for the HFAB ranged from chain A ($353.05 ± 16.94) to chain C ($389.41 ± 26.86). Differences in cost on basis of store type showed a trend for cheaper prices being provided by large chain stores but were not statistically significant.
Discussion
In SW Victoria, the rural consumer can purchase basic foods within his or her local community; however, a complete healthy diet is more likely to be available if the consumer has easy access to a large food retail chain store. This is more likely to be in a regional centre or large town. This finding is hardly surprising. However, it indicates both a possible cause for dietary risk in rural communities as a result of food access being centralised away from smaller rural communities to regional centres.
Fifteen towns (36%) were found where there was only one independent store in town and poor access to a basket of basic healthy foods. This is particularly an issue in these communities for those without transport, money for transport and/or the physical ability to go to large service centres to shop. It should be noted that in these towns, the availability of both healthy and a range of common but not necessarily healthy foods purchases was compromised. This was indicative of the general poor access to food in small rural communities. The poor access to healthy food shown may explain some of the high burden of disease suffered in rural Australia. The universal availability of soft drink and some takeaway food may further compound this diet-related ill health.
The cost of a range of healthy foods in SW Victoria was comparable with the average cost of the same food in the urban centre of Melbourne. The price ranges across shires were not as great as those observed in remote and very remote areas3. Variation in the cost of fruits and vegetables accounted for a significant amount of the observed regional differences. Variation in the price of fruits and vegetables may be due to variation in growing conditions and transportation costs7. It is known that taste and cost are the primary determinants of food purchase8. The relationship between price variability of fruits and vegetables and consumption in these rural communities has yet to be determined.
The average weekly cost of the HFAB in SW Victoria for a family of six was $190. This was consistent with the average Australian household food expenditure ($190.32) for a family of six given a weekly income of $1115.80 and 1.7 persons in a household working9. It should be noted though that the average weekly food expenditure in rural Australia is $123.47 with an average weekly household income for rural Australia of $761.95 with 1.4 persons working in a household9. It would appear likely that many rural families would be at an economic disadvantage in accessing sufficient healthy food if the cost of a healthy food basket in SW Victoria is indicative of rural costs in general.
The HFAB methodology was developed for use in the Northern Territory and Far North Queensland. The current HFAB reflects the poor access to fresh food in these areas. We choose to use the HFAB in its current form to facilitate comparison with data from studies using this method in remote Australia. It could be advantageous for the method to be adapted for use in areas where fresh food is readily available and there is not as great a reliance on canned and frozen food. Future studies should also take into account the difficulty in producing statistically significant differences when the groups of interest are unavoidably small.
Conclusion and implications
The implications of this study are that families living in small rural towns serviced by only one shop may be at a disadvantage in their ability to access a healthy diet. Maintaining the sustainability of a local food supply; that is, local markets and stores may be important not only for health but also to safeguard local employment, minimise food transportation and strengthen community cohesion in smaller rural communities10. Centralising food supply in regional centres with large supermarkets does provide economies of scale but may have adverse social and economic consequences for rural communities.
This study highlights the need for an increased understanding of food acquisition in rural areas (i.e. shopping habits). Researchers need to study the social implications of food supply and purchase in rural communities. It could be that the distances travelled for food in rural areas are not seen as prohibitive if the trip entails social contact. It is also important that the sources of local food supply (local vs non-local) are studied. Studies in the UK have begun to calculate food miles; that is, the number of miles covered (and fuel expended) by produce from producer to shop11. Given that SW Victoria is a rich beef and dairy producing area, it may be possible to reduce food miles and thus reduce the price for consumers by increasing use of local foods. Interventions to increase local consumption of local food could make better sense in both economic and health terms while saving on fossil fuels.
Acknowledgements
The authors would like to thank Emily Chambers, Kerri Gordon, Belinda Hodgson, Robyn Hunter, Hazreen Abdul Majid, Anna O'Brien, Anna Rizzuto and Tanya Wigg for their tireless effort in collecting the data. Thanks also to Professor Damien Jolley, Dr Said Aden and Geoffrey Der for help with presentation of the data, and Amanda Lee and Steven Cummins for helpful comments on the draft paper.
References
1. WHO. Diet, nutrition and the prevention of chronic diseases. Report of a Joint WHO/FAO Expert Consultation. WHO Technical Report Series 916. Geneva: WHO, 2003.
2. Victorian Department of Human Services. The Victorian burden of disease study: morbidity. Melbourne: Victorian Government, Public Health Division, 1999.
3. Lee AJ, Darcy AM, Leonard D et al. Food availability, cost disparity and improvement in relation to accessibility and remoteness in Queensland. Australian and New Zealand Journal of Public Health 2002; 26: 266-272.
4. Australian Department of Health and Aging. Accessibility/Remoteness Index of Australia (ARIA) 2001. (Online) 2001. Accessible: http://www.health.gov.au/ari/aria.htm (Accessed 27th May 2004 ).
5. Cashel K, Jeffreson S. The core food groups. Canberra: NHMRC, 1994.
6. Kerslakw D. 'AC Nielson top-100 brands 2000 - get bug or else...' AC Nielson Grocery Report. (Online) 2001. Available: http://www.acnielsen.com.au (Accessed 27th May 2004).
7. Australian Bureau of Statistics. Consumer Price Index. Table 6A. CPI: Food, contribution to change in all groups. Cat. No 6401.0. Canberra: Australian Bureau of Statistics, 2004.
8. Australian Bureau of Statistics. 1998-99 Household expenditure survey - companion data. Table 5. Household expenditure by Broad Geographic Area. Table 7 by Household Composition. Cat. No. 6530.0. Canberra: Australian Bureau of Statistics, 2000.
9. Tansey G, Worsley A. The Food System. London: Earthscan, 1995
10. Clunies-Ross T, Hildyard N. The politics of industrial agriculture. London, Earthscan, 1992.
11. Jones A. An environmental assessment of food supply chains: A case study on dessert apples. Environmental Management 2002; 30: 560-576.

Abstract
Introduction: The burden of chronic diseases is rapidly increasing worldwide. In Australia rural populations have a greater burden of disease. Chronic diseases are largely preventable with diet as a key risk factor. With respect to diet-related chronic disease, dietary risk may be due to poor food access, namely, poor availability and/or the high cost of healthy food. It is likely that poor food access is an issue in rural areas. Objective: To assess food access in rural south-west (SW) Victoria, Australia.
Methods: A total of 53 supermarkets and grocery stores in 42 towns participated in a survey of food cost and availability in the rural area of SW Victoria. The survey assessed availability and cost of a Healthy Food Access Basket (HFAB) which was designed to meet the nutritional needs of a family of 6 for 2 weeks.
Results: Seventy-two percent of the eligible shops in SW Victoria were surveyed. The study found that the complete HFAB was significantly more likely to be available in a town with a chain-owned store (p <0.00). The complete HFAB was less likely to be available from an independently owned store in a town with only one grocery shop (p <0.004). The average cost of the HFAB across SW Victoria was AU$380.30 ± $25.10 (mean ± SD). There was a mean range in difference of cost of the HFAB of $36.92. In particular, high variability was found in the cost of fruits and vegetables.
Conclusions: Cost and availability of healthy food may be compromised in rural areas. Implications: Improvements in food access in rural areas could reduce the high burden of disease suffered by rural communities.
Key words: food access, nutrition.
You might also be interested in:
2022 - Rural–urban differences in physical activity and TV-viewing in Brazil
2019 - Social and community networks influence dietary attitudes in regional New South Wales, Australia
2006 - Postgraduate medical placements in rural areas: their impact on the rural medical workforce


