In Japan, the shortage of physicians is well documented. There have been absolute and relative deficiencies in the number of physicians, and Japan is in the lowest group as ranked by the Organization for Economic Cooperation and Development (OECD)1. In addition, the gap in distribution of physicians between rural and non-rural areas has constantly been increasing since 19802, and there is maldistribution in the different specialties because few doctors choose specialties that cover a broad domain (eg general medicine/family medicine, internal medicine, pediatrics, surgery, and emergency medicine), which are needed especially in rural areas3.
The Japanese government has recently implemented a form of rural quota at medical schools in all 47 prefectures. If the programs work successfully, the impact on the geographic distribution of physicians will be substantial4. In times of physician shortage, it is important for those seeking a career in medicine to know the expectations for future generation of physicians. In many other countries a lot of studies have been done to explore career choices of medical students5-16. In Japan, few studies have focused specifically on exploring characteristics and identifiers of medical students that will predict their intention to practise rurally4,17-19. Thus, identification of these relationships between various characteristics and intent for rural practice will assist Japanese medical schools to effectively recruit future rural physicians.
The purpose of this study was two-fold: to understand what career preferences medical students have at medical school and to determine the characteristics of medical students who intend to practice in a rural area.
Participants
This study was designed as a cross-sectional survey. Students from one Japanese regional university school of medicine were surveyed. From April 2009 to 2013 (in Japan, the academic year begins in April), a five-page entry questionnaire was administered within the first 4 weeks of the first semester of each medical school year.
Questionnaires
A self-administered questionnaire developed by Takeda et al20 was used, enquiring about background factors and specialty preference. Sociodemographic questions regarding gender, age, academic year, type of high school, work experience before admission, relatives in the medical field, presence of a role model, scholarship, admission by school recommendation, admission by a special policy directly aimed to increase rural physicians as one main purpose (chiiki-waku in Japanese), and the area of living until the age of 18 years were included. Participants were asked to specify which of 14 medical specialties they intended to pursue: general medicine/family medicine, internal medicine subspecialty, surgery, pediatrics, obstetrics/gynecology, psychiatry, anesthesiology, emergency medicine, dermatology, orthopedics, ophthalmology, otolaryngology, urology and radiology, or 'other'. They were instructed to choose one as the most preferable specialty and other specialties 'under consideration', as many as applied. When 'other' was chosen for a non-listed specialty, the respondent was asked to specify which discipline they were choosing. They then indicated the degree to which their choice was influenced by 30 items (Table 1). The subscales of 'characteristics of the specialty' (10 items), 'personal experience' (3 items), 'experience at a medical school or during postgraduate training' (5 items), 'advice from others' (4 items), 'considering future work conditions' (8 items), and 'others'(1 item) cover reasons for choosing a specialty. The subscales of 'how important is the decision on where to practice in the future?' (20 items) describe the individual aspects. Influence of the responses to the subscales was rated on a four-point Likert scale (1='not at all'; 2='not particularly'; 3='fairly well'; 4='extremely well'). The authors defined 'no' as Likert scale from 1 to 2 and 'yes' from 3 to 4. The participants were asked whether they are willing to practice in a rural area (1='positively motivated'; 2='willing to work for a certain period of time'; 3='would rather avoid it'; 4='never').
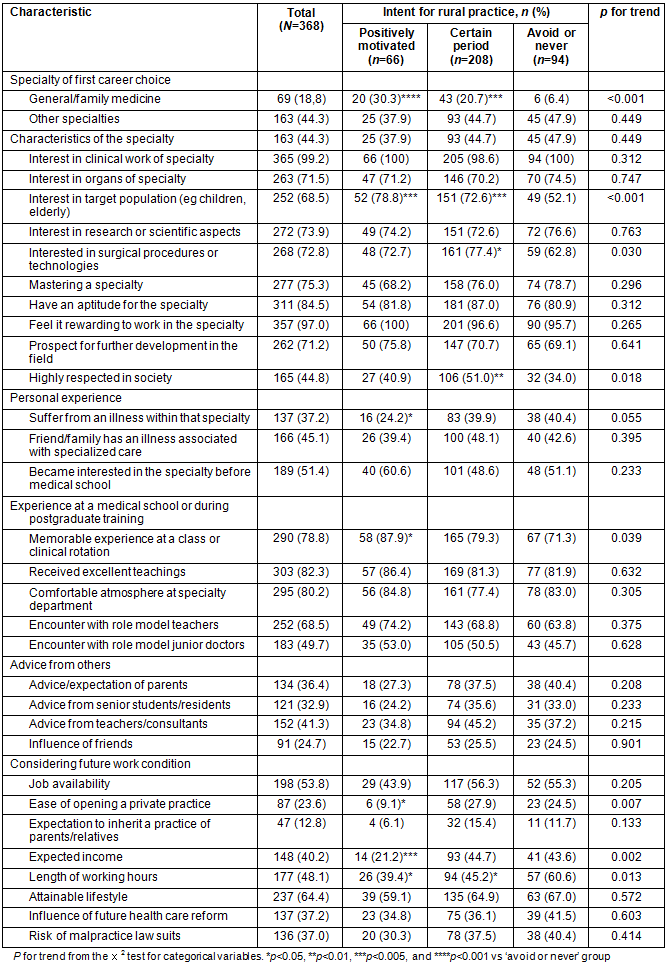
Table 1: Reasons for choosing future career of participants by intent for rural practice
Data analysis
Data are presented as the mean ± standard deviation (SD) unless otherwise specified. Statistical analysis was performed using IBM SPSS Statistics v21 (Statistical Package for the Social Sciences; http://www.spss.com). Differences were analyzed by one-way ANOVA test for continuing variables and the χ2 test for categorical variables. Logistic regression analysis (backward elimination method) was used to evaluate the contribution of each confounding factor for the participants' intent to practice in a rural area (eg 'positively motivated' or 'willing to work for a certain period' vs 'avoid' or 'never' groups). A value of p<0.05 was considered significant.
Ethics approval
The study was approved by the ethics committee of the Ehime University Graduate School of Medicine (2450960), and informed consent was obtained from all subjects.
A total of 417 students completed the survey giving an 88.2% response rate (368 students). Characteristics of respondents and comparisons by practice intent are summarized (Table 2). Age of students opting for rural practice was significantly younger (p=0.004). Most students were in the first or second academic year (p=0.005) and had a higher rate for work experience before admission (p=0.021), relatives in the medical field (p=0.015), admission by school recommendation (p=0.001), admission by a special policy (p=0.049), and grew up in a rural area (p=0.009). There was no significant difference in intention for rural practice by gender, high school type, presence of a role model, or scholarship.
Reasons for the choice of specialty by the participants are summarized according to their intention for rural practice (Table 1). There were significant differences between students with and without the intention for rural practice. In particular, students with intent for rural practice had higher rates for selecting general medicine/family medicine as the first career choice (p<0.001), having interest in the target population (eg children, the elderly) (p<0.001) and surgical procedures or technologies (p=0.030), being highly respected in society (p=0.018), and having a memorable experience at a class or clinical rotation (p<0.001). However, fewer students with intention for rural practice were likely to be interested in ease of opening a private practice (p=0.007), expected income (p=0.018), and working hours (p=0.013).
Medical school students' opinions are summarized in relation to influences on their choice of practice and their opinion of physicians practising in a rural area (Table 3). Students intending rural practice were more likely to consider location of medical school (p=0.002) and availability of support from other doctors (p<0.001) as important, and less likely to consider educational environment for children (p=0.003), teaching opportunities (p=0.011), and income (p<0.001) as important.
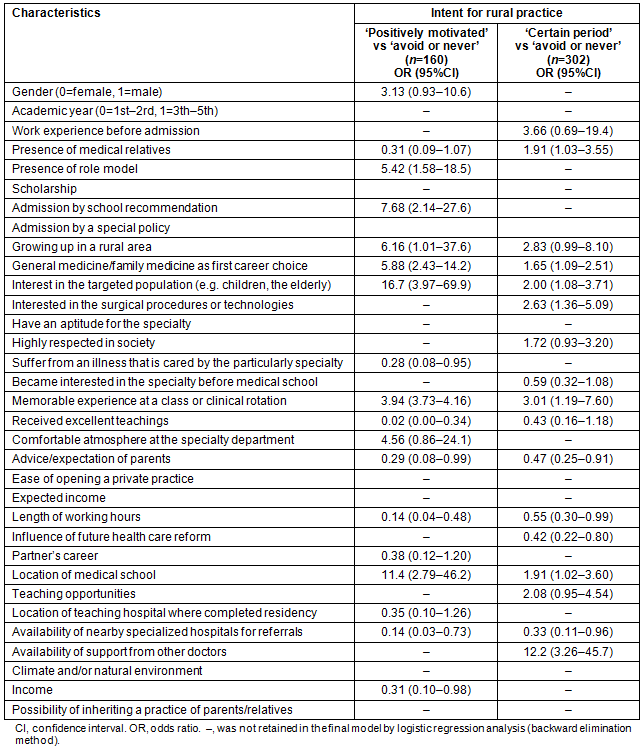
Table 4 shows the odds ratios for each of the confounding variables by multivariate logistic regression analysis. Significant variables associated with positively motivated intent for rural practice are 'presence of a role model' (odds ratio (OR), 5.42; 95% confidence interval (CI), 1.58-18.5), 'admission by school recommendation' (OR, 7.68; 95%CI, 2.14-27.6), 'growing up in a rural area' (OR, 6.16; 95%CI, 1.01-37.6), 'general medicine/family medicine as a first career choice' (OR, 5.88; 95%CI, 2.43-14.2), 'interest in the targeted population' (OR, 16.7; 95%CI, 3.97-69.9), 'memorable experience at a class or clinical rotation' (OR, 3.94; 95%CI, 3.73-4.16), and 'location of their medical school' (OR, 11.4; 95%CI, 2.79-46.2). Significant variables associated with negative intent for rural practice were 'I suffer(ed) from an illness of the specialty' (OR, 0.28; 95%CI, 0.08-0.95), 'received excellent teachings' (OR, 0.02; 95%CI, 0.00-0.34), 'advice/expectation of parents' (OR, 0.29; 95%CI, 0.08-0.99), 'working hours' (OR, 0.14; 95%CI, 0.04-0.48), 'availability of nearby specialized hospitals for referrals' (OR, 0.14; 95%CI, 0.03-0.73), and 'income' (OR, 0.31; 95%CI, 0.10-0.98).
Table 2: Characteristics of participants by intent for rural practice
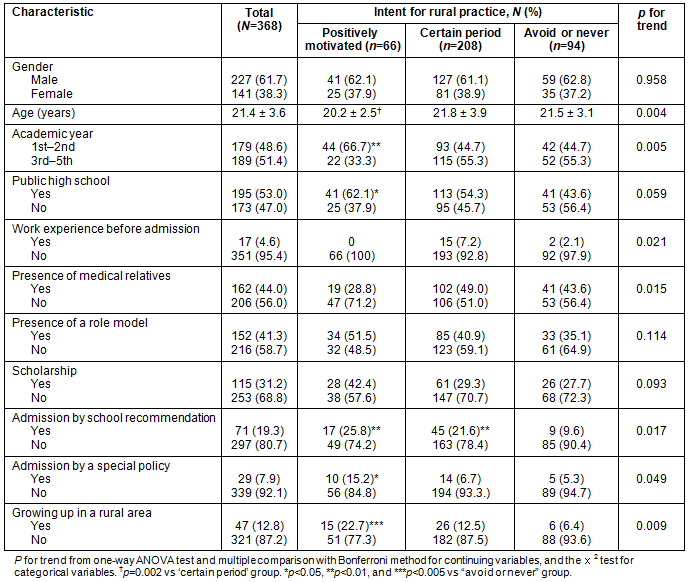
Table 3: Reasons for participants' choice of a practice location by intent for rural practice
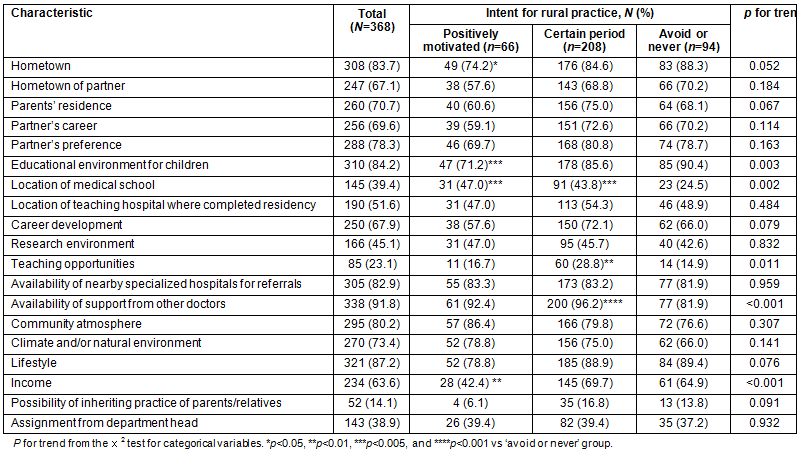
Table 4: Multiple logistic regression models of confounding factors for intent for rural practice
Discussion
The purpose of this study was to determine the characteristics associated with medical students who opt for rural practice. Some factors found to be important for recruiting in a rural area in previous studies5,6 were also found to be important in this study. Medical students with 'presence of a role model', 'growing up in a rural area', 'admission by school recommendation', 'general medicine/family medicine as first career choice', 'interest in the targeted population (eg children, the elderly)', 'memorable experience at a class or clinical rotation', and 'location of the medical school' are more likely to opt for rural practice. These suggest that students' characteristics may be strongly correlated with opting for rural practice and it is imperative that Japanese medical schools promote admission by school recommendation of such students in order to solve the shortage of physicians in rural areas.
With the continuing need for rural physicians, conditions associated with medical students' intention for rural practice need to be identified and addressed. The factor most often found to influence rural practice preference is having a rural background such as a 'rural origin'7, 'growing up in a rural area'8-10, and 'graduating from a rural high school'10. The present study supports these researches and most of these predictive factors can be identified at the time of admission to medical school. Thus, medical schools should actively recruit students who have lived in a rural area. However, recruitment of students with rural backgrounds may be difficult because there are a limited number of students from rural areas who are interested in becoming physicians8.
The study data show that 'general/family medicine as the first career choice' is also important in opting for rural practice. Medical students understand that career choice of family/general medicine is necessary for rural practice, which is expected to cover a broad range of conditions. Rabinowitz demonstrated that students with an interest in family medicine who enter medical school are more likely than their peers to become family physicians or to practice in a rural area11. Moreover, in the choice of specialties, although many medical students frequently change their minds about the specialty they select, most students usually consider themselves as either generalists or specialists and their career choice of generalist is more consistent than that of other specialties12,13. In addition, medical students tend not to switch into family medicine if this choice had not been considered from the outset12. Thus, the percentage of students interested in family medicine as the first career choice reflect a preference for a career in family medicine at graduation14.
'Presence of a role model' and 'memorable experience at a class or clinical rotation' were also strongly correlated with opting for rural practice. It is important for medical students to meet rural family physicians as role models. Exposure to rural practice in undergraduate medical education has been demonstrated as an encouraging factor for future rural practice7,15,19. The present study's results showed that opportunities for rural exposure in medical schools may be effective for recruitment. However, programs with short rural exposure are ineffective in shaping students' career choices and decisions on internship location16. Rural exposure at the undergraduate and graduate levels performed recently in Japanese medical schools is a short rotation (1 to 2 weeks), and the experience may be daunting.
'Admission by school recommendation' may increase interest in rural practice. This is a system in which students can enter a medical school on the assumption that they remain and work in a local prefecture after graduation, although this system is not binding. However, medical students' thoughts may be related to their intent for rural practice. In the present study, scholarship was not important for intent for rural practice because the duty after graduation is not necessarily followed by a scholarship system. On the other hand, programs such as debt cancellation of student loans may be useful in recruiting students to rural practice8. In Japan, Jichi Medical University (JMU) was established in 1972 to supply graduates to rural areas and has several unique characteristics aimed at motivating graduates to opt for rural practice, and has achieved its aim of supplying doctors to rural areas4,21. Therefore, the government has recently implemented a JMU-like contractual program as a form of rural quota at other medical schools in all 47 prefectures4.
'I suffer(ed) from an illness of the specialty', 'received excellent teachings', 'advice/expectation of parents', 'working hours', 'availability of nearby specialized hospitals for referrals', and 'income' are characteristic backgrounds that were negatively associated with medical students' intention for rural practice. Medical students who opt for rural practice demonstrate flexibility, self-reliance, and internal motivation.
Some limitations of this study must be considered. First, the cross-sectional study design does not eliminate potential causal relationships between characteristics of medical students and intention for rural practice. Second, the OR associated with rural upbringing was higher than has been reported in studies examining factors related to rural practice choice. This is possibly due to the fact that the characteristics evaluated in this study were based on intent rather than actual practice; rural upbringing may have a greater effect on intent than on final choice of practice8. Third, this study was on a limited number of students who belong to one regional university. Therefore, the students were more likely to choose rural practice than students from other schools. Fourth, this study measured students' intent for rural practice but not their actual choice of practice because students' intent was measured prior to residency. Fifth, as the authors used a self-administered questionnaire developed for fourth and sixth-year medical students20, some of the characteristics examined appeared to be suitable for upper grade students (eg specialty choice) but not for undergraduate students. Sixth, the authors defined 'no' as the Likert scale from 1 to 2 and 'yes' from 3 to 4, and this may affect the interpretation of the results of this study. Future research using longitudinal data collection will enable the authors to monitor the relationship between early stated intentions, medical educational experiences, and actual behavior.
The present study showed that in order to provide rural areas with physicians, Japanese medical schools might promote admission by school recommendation of students who display the characteristics that are associated with their intention for rural practice and give such students a memorable experience in their educational training.
Acknowledgements
This work was supported in part by a Grant-in-Aid for Scientific Research (KAKENHI) (2012-2014).
References
1. Organization for Economic Cooperation and Development. OECD health data 2013 (report). OECD. (2013-06). Doctors consultations, number per capita. (Online) 2014. Available: http://www.oecd.org/health/healthdata (Accessed 20 March 2014).
2. Kobayashi Y, Takaki H. Geographic distribution of physicians in Japan. Lancet 1992; 340: 1391-1393.
3. Koike S, Ide H, Yasunaga H, Kodama T, Matsumoto S, Imamura T. Postgraduate training and career choices: an analysis of the National Physicians Survey in Japan. Medical Education 2010; 44: 289-297.
4. Matsumoto M, Inoue K, Kajii E, Takeuchi K. Retention of physicians in rural Japan: concerted efforts of the government, prefectures, municipalities and medical schools. Rural and Remote Health 10: 1432. (Online) 2010. Available: www.rrh.org.au (Accessed 20 March 2014).
5. Curran V, Rourke J. The role of medical education in the recruitment and retention of rural physicians. Medical Teacher 2004; 26: 265-272.
6. Hart LG, Salsberg E, Phillips DM, Lishner DM. Rural health care providers in the United States. Journal of Rural Health 2002; 18: 211-232.
7. Easterbrook M, Godwin M, Wilson R, Hodgetts G, Brown G, Pong R, Najgebauer E. Rural background and clinical rural rotations during medical training: effect on practice location. Canadian Medical Association Journal 1999; 160: 1159-1163.
8. Royston PJ, Mathieson K, Leafman J, Ojan-Sheehan O. Medical student characteristics predictive of intent for rural practice. Rural and Remote Health 12: 2107. (Online) 2012. Available: www.rrh.org.au (Accessed 20 March 2014).
9. Rabinowitz H, Diamond J, Veloski J, Gayle J. The impact of multiple predictors on generalist physicians' care of underserved populations. American Journal of Public Health 2000; 90: 1225-1228.
10. Feldman K, Woloschuk W, Gowans M, Delva D, Brenneis F, Wright B, Scott I. The difference between medical students interested in rural family medicine versus urban family or specialty medicine. Canadian Journal of Rural Medicine 2008; 13: 73-79.
11. Rabinowitz HK. Recruitment, retention, and follow-up of graduates of a program to increase the number of family physicians in rural and underserved areas. New England Journal of Medicine 1993; 328: 934-939.
12. Colwill JM. Where have all the primary care applications gone? New England Journal of Medicine 1992; 326: 387-393.
13. Rabinowitz HK. The change in specialty preference by medical students over time: an analysis of students who prefer family medicine. Family Medicine 1990; 22: 62-63.
14. Wright B, Scott I, Woloschuk W, Brenneis F. Career choice of new medical students at three Canadian universities: family medicine versus specialty medicine. Canadian Medical Association Journal 2004; 22: 1920-1924.
15. Wilkinson D, Laven G, Pratt N, Beilby J. Impact of undergraduate and postgraduate rural training, and medical school entry criterion on rural practice among Australian general practitioners: national study of 2414 doctors. Medical Education 2003; 37: 809-814.
16. Denz-Penhey H, Shannon S, Murdoch CJ, Newbury JW. Do benefits accrue from longer rotations for students in rural clinical schools? Rural and Remote Health 5: 414. (Online) 2005. Available: www.rrh.org.au (Accessed 20 March 2014).
17. Matsumoto M, Inoue K, Kajii E. Characteristics of medical students with rural origin: implications for selective admission policies. Health Policy 2008; 87: 194-202.
18. Matsumoto M, Kajii E. Medical education program with obligatory rural service: analysis of factors associated with obligation compliance. Health Policy 2009; 90: 125-132.
19. Inoue K, Matsumoto M, Toyokawa S, Kobayashi Y. Transition of physician distribution (1980-2002) in Japan and factors predicting future rural practice. Rural and Remote Health 9: 1070. (Online) 2009. Available: www.rrh.org.au (Accessed 20 March 2014).
20. Takeda Y, Morio K, Snell L, Otaki J, Takahashi M, Kai I. Characteristic profiles among students and junior doctors with specific career preferences. BMC Medical Education 2013; 13: 125.
21. Inoue K, Hirayama Y, Igarashi M. A medical school for rural areas. Medical Education 1997; 31: 430-434.

