Oral diseases are still a major public health issue due to the high prevalence and high treatment cost they represent1. Dental caries, periodontal disease, tooth loss and mucosal lesions affect daily life's crucial functions, such as eating, chewing and swallowing. Moreover, they interfere with the important social functions of smiling and communication, affecting quality of life2. Among all the oral conditions, dental caries and periodontal disease are the major causes of dental disease worldwide3. Dental caries, for example, affects 60-90% of school-age children worldwide and, in most countries, 100% of adults. In Latin America, most of the countries report DMFT (decayed, missing, filled teeth) scores between 2.7 and 4.4 in 12-year-old children and the majority of children present signs of gingivitis3.
In addition to the canonical biological determinants of dental caries and periodontal disease, other factors such as personal and family experience, health behaviors and beliefs and the socioeconomic status have been shown to be health determinants and should be included in assessing dental risk4. Importantly, these non-biological factors also explain the majority of health inequalities5. In the same context, living in rural areas is associated with a lack of access to dental health services, low levels of education, specific lifestyle patterns and lack of fluoride-containing drinking water. Frequently found in rural areas, lower access to care and lack of basic services seem to condition differential prevalence of oral disease6. Interestingly, data coming from countries with very different realities, such as Australia7, Mexico8, Poland9 and Pakistan10, agree on the fact that oral status of rural people is worse than that of their urban counterparts.
Despite the vast amount of information on the oral health of rural and remote compared to urban populations, in Chile no information on this matter is available. Since disparities and other social and biological problems may result from this type of difference, comprehensively understanding the oral health situation of a population allows planning effective strategies for their resolution. In that context, the oral health status of Chileans has only been outlined in terms of global estimations, with little information arising from representative studies at the regional level. At the national level, a high prevalence of oral diseases has been reported in 6-year-old children. Dental caries have been found to occur in 70.36% of children in this age group, with a deft of 3.71 and a DMFT of 0.15. Furthermore, gingival disease affecting 55.09% of children of this age have been found. Of particular relevance to the current study, 6-year-old children have been defined as a priority group in Chile. There has been a gradual increase in dental coverage in terms of plans and programs designed specifically for this age group11.
Although Chile exhibits the highest human development index (HDI) in the context of the Latin American region, the Maule region has almost the lowest levels in Chile12. This region has the highest percentage of people living in rural areas in Chile with 37.4%, versus the national mean of 13.4%. Moreover, the Maule region has the lowest schooling level in the country, with an average of just 5.9 and 9.3 years for the rural and urban populations, respectively13. It is reasonable, therefore, that the oral health status in this region may be poorer than the rest of the country. Unfortunately, almost no information with regional representation on caries and gingival status is available for the Maule region. Furthermore, little information is available in Chile on how rurality affects oral health status. Given the lack of specific information regarding the oral health condition of the Maule region and the high rurality rate that it has, the aim of this study was to characterize oral health conditions of 6-year-old children living in a highly rural region of central Chile, regarding dental caries prevalence and some indicators of gingival health. An association between rurality and the prevalence of oral diseases was also investigated.
This cross-sectional study was part of a larger International Association for Dental Research (IADR) project Regional Development Program for Training in Research Methods and Oral Health Surveys and the Assessment of Oral Health in the Chilean Division of the IADR, the EpiMaule study. The aim of the project was to analyze the oral health status and treatment needs of the residents of the Maule region of Chile of varying ages according to the criteria set by WHO: 6, 12, 15, 35-44 and 65-74 years14. This study reports only the information gathered from 6-year-old children.
Subjects
The sample was selected from population projection data for the Maule region for 201013 from the last official census in 2002. A total number of 13 428 6-year-old children was projected for the region by 2011. The sampling process was stratified by age to estimate proportions, considering caries prevalence reported in Chile (deft) at 6 years of age11 and the presence or absence of fluoride in the drinking water to define rurality15 with 95% confidence level and 3% estimation error, which is customary in this type of study. Using a cluster analysis, the 30 districts of the region were divided into four groups according to rurality and population size. In each group, a proportional number of districts, according to the population size, were weighted and randomly chosen until completion of 19 districts. Sample selection was carried out by randomly selecting schools from the official register of the Ministry of Education. Children in each school were randomly selected using a random numbers table. Participants were excluded from the study if they did not provide consent to participate, they misbehaved during examination, were sick on the day of their exam, or had a systemic disease that prevented them from having a periodontal examination. Hence, a final sample of 485 children would be needed.
Examination methodology
Sociodemographic variables such as age, sex, residential area and type of school, and the participant's medical history, were collected through a survey. A clinical exam, which evaluated the oral health status of each participant, was administered according to the criteria outlined by the WHO for oral health studies14 by four calibrated examiners. Exams were carried out without radiographs, using a community periodontal index (WHO) probe, mirrors and LED front lamps, following standard infection-control procedures. To access rural locations, schools were invited to participate by the coordinator of the study who reached the responsible person at each school. In both settings, rural and urban, examinations were performed following an identical protocol. To evaluate dental caries, the DMFT and deft indexes were used. The gingival exam included the oral hygiene index (OHI) of Silness and Löe and the gingival index (GI) of Löe and Silness14. Calibration of the examiners was performed for both the DMFT and GI, obtaining in both cases a linear kappa index of above 0.85. Data collection and archiving of the hard copies of the surveys and exams was carried out by the principal investigator.
Data management
The identity of the participants was concealed from researchers during the analysis of the data and throughout the study. Statistical comparisons of the variables with proportions were carried out using a Z-test to compare proportions. Statistical comparisons for variables presented as means were measured by student t-test for independent samples. In both cases, the statistical significance was set at p<0.05. Statistical Package for the Social Sciences software v15 (SPSS; http://www.spss.com) was used to analyze the data.
Ethics approval
The study protocol was approved by the Bioethics Committee of the University of Talca (number 00038). A specially designed informed consent was given to the legal guardian of each participant. Only those subjects who returned a signed informed consent were included in the study.
Gender distribution of the participants was 47.6% and 52.4% for males and females, respectively. Concerning rurality, 41.9% of the sample population lived in urban areas, while 58.1% in rural areas.
Caries prevalence at 6 years was 80.62% (n=391) for the total population of the Maule region. Children from urban districts had lower (p<0.0001) caries prevalence (69.95%), when compared to those living in rural districts (88.30%), which represents 18.35% higher prevalence than that of the urban districts. In deciduous teeth, the deft was 4.63 (±3.96) for the region, with 5.74 (±4.00) for rural and 3.09 (±3.34) for urban districts. Regional defs (decayed, extracted, filled surfaces) was 10.34 (±11.37), with 13.30 (±12.38) for rural areas and 6.24 (±8.20) for the urban areas (Table 1). The significance index of dental caries (SiC) was 9.30 (±2.31) for the Maule region, with 10.23 (±2.17) in the rural and 7.13 (±2.42) in the urban districts. The deft, defs and SiC scores in rural children were higher when compared to those living in urban areas (p<0.001) (Table 1). Thus, rural indexes for deft, defs and SiC were higher than those of the urban districts by 86.07%, 113.35% and 43.46%, respectively. With regard to permanent teeth, the region's DMFT was 0.24 (±0.74), and DMFS was 0.32 (±1.10). No difference was observed in either permanent teeth index (p>0.05). While SiC for permanent teeth was 0.74 (±1.14) for the entire region, an SiC of 0.78 (±1.23) for rural and 0.66 (±1.00) for urban 6-year-olds was obtained. Rural children showed 19.18% higher SiC than their urban counterpart (p<0.001) (Table 1).
Mean OHI was 1.44 (±0.37) for the Maule region, but urban and rural areas showed a significant difference (p<0.0001) in the indexes with an average of 1.37 (±0.39) and 1.49 (±0.35), respectively (Table 2), which is 9% higher in rural districts. The OHI was classified according to severity as 'healthy', 'low', 'moderate' and 'high'. While 82.47% of the population was in the moderate range, 12.16% and 5.36% were in the low and high ranges, respectively (Table 3). When compared by location, rural districts showed poorer hygiene (p<0.0001). Indeed, urban areas had more children in the low range than rural areas, with 17.24% and 8.51%, respectively. Likewise, OHI in children from rural communities exceeded that of those in urban districts by 7.13% in the moderate range and by 1.6% in the high category. Mean GI for 6-year-old children from the Maule region was 1.37 (±0.28). This score is considered as a moderate level of inflammation. No differences were detected between urban and rural children (p>0.05) in this index, with GI 1.39 (±0.30) and 1.36 (±0.27), respectively (Table 2). Most of the participants (90.52%) had a moderate GI severity, without significant differences by rurality (Table 4).
Table 1: defs, deft, DMFS, DMFT and SiC indexes and their components in 6-year-olds from the Maule region, Chile
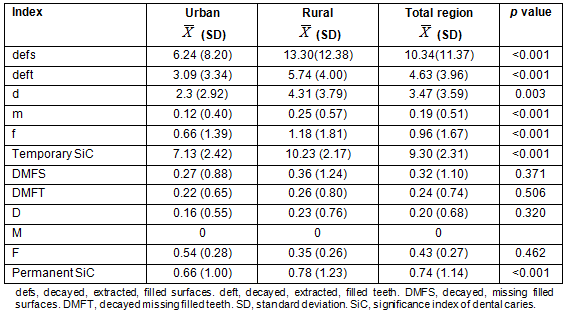
Table 2: Oral health index and gingival index of 6-year-olds of the Maule region, Chile, by rurality
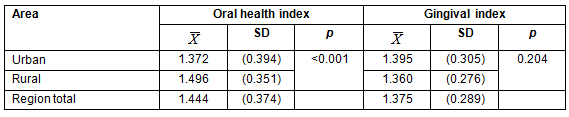
Table 3: Distribution of 6-year-olds of the Maule region, Chile, by severity of oral hygiene index and rurality
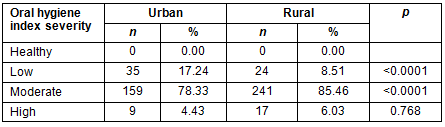
Table 4: Distribution of 6-year-olds of the Maule region, Chile, by severity of gingival index and rurality
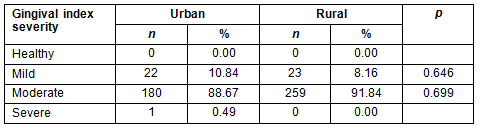
Discussion
This study reports the oral health status of the 6-year-old population of a region of central Chile. Caries experience in the region was 80.63%. This prevalence is higher than the national mean of 70.36%, reported by the Chilean Ministry of Health11. In the same report, the Maule region had lower caries prevalence than in the present investigation, with 76.10%. Data from previous studies had suggested a decrease in the prevalence of dental caries in 6-year-old children from Chile. However, the results of the present study do not seem to follow this national trend. When compared with international studies, the high caries prevalence of 6-year-old children in the Maule region is similar to that reported in several countries including Jordania16, Georgia17 and Russia18. In Latin America, caries prevalence at 6 years old is also very high. Interestingly, prevalence reported in countries with a similar level of development than Chile, like Argentina19 and Brazil20, also exhibit very high caries prevalence at this age. Conversely, other countries, including France21, India22 and Mexico23, have reported much lower caries prevalence at this age.
When considering caries experience, the deft index was higher than that reported for the Maule region by the national study. In fact, the mean deft score of 4.6 found here (Table 1) is higher than the national mean of 3.71. Importantly, the Maule region also had the highest deft in the national study11. The decayed (d) component of the deft index was the highest contributor to the index, while the filled component (f) is low, suggesting a low level of dental coverage for this age group in this predominantly rural region of central Chile (Table 1). The extracted tooth (e) component of the present EpiMaule study was higher than that reported in the national study, with 0.96 and 0.22, respectively. The latter suggests that when reached, dental therapy is rather radical, involving tooth extraction. Given that the sample from the Maule region in the national survey was representative of the country, but not of the region, a selection bias could have explained the difference between the studies. Consistent with the deft index, the DMFT index was higher at this age, when compared with previous national data11 (Table 1).
After many years of interventions with preventive and therapeutic approaches in this population, it could be reasonable to expect a decrease in caries experience. Reality, however, shows that caries prevalence has been steady over time, as described here. Despite the efforts in providing dental care in the community, a study carried out in a rural community in Chile reported little variations in caries prevalence in a timeframe of 10 years24.
Caries prevalence in rural areas (88.3%) was significantly higher than that for urban 6-year-olds (69.95%). Asymmetry in caries prevalence observed in urban and rural areas is consistent with the existing data in Chile11. The same trend was verified for the deft and the DMFT indexes (Table 1). Likewise, when the SiC index was analyzed for permanent teeth, urban population showed lower values (p<0.05), with 0.66, whereas the rural counterpart exhibited 0.78 (Table 1). A similar situation occurred with the temporary teeth, with 7.13 for urban and 10.23 for rural children (p<0.05). These findings give support to the idea that rural populations accrue considerably more oral damage due to caries than the population living in urban areas.
Given the different distribution of caries in the population, a specific analysis of the most affected group appears necessary. In that context, the SiC index focuses attention on those individuals with the highest caries scores in each population25. Interestingly, DMFT score did not show differences between urban and rural population. SiC index, however, for permanent teeth was significantly different between these two populations (Table 1). Additionally, the SiC index for temporary teeth was higher (9.3) in the EpiMaule Study than the same index found in the Bío-Bío region, a Chilean region that is not supplied with fluoridated water, unlike the Maule region26. Hence, it is possible to conclude that rurality may play a role in dental caries, beyond water fluoridation. This is currently a matter of debate among scholars and health authorities in the country to decide whether or not to continue with the program.
Inequalities in access to care or other unidentified variables associated with life in rural areas may also be involved as explanatory factors for the differences in caries prevalence. Hence, rurality might be considered as a risk factor for caries or oral conditions. Consistent with these observations, a recent study found an association between geographical factors and oral health. People with low access to piped potable water had worse DMFT scores8. Indeed, a lower socioeconomic status in rural populations may strongly influence the prevalence of oral diseases27. A recent study in Russia showed similar caries experience between rural and urban 6-year-old children, but the number of decayed teeth in rural areas was higher than in urban areas, with fewer missing and filled teeth18. The same EpiMaule study, but in adults and older adults, showed similar results to the Russian study, highlighting that rural populations usually have less access to dental care28.
Regarding the gingival situation, national studies available for 6-year-old children are based on the actual diagnosis of periodontal disease. The present study, however, used gingival health indicators, including OHI, GI (Table 2) and the severity of them. Given that previous studies in Chile did not report on those indexes, it is difficult to establish accurate comparisons. Despite this limitation, it is possible to carry out some analyses. In the present study, no children were found to be gingivally healthy, that is, without signs of gingivitis (Table 4). Data at the country level showed quite different results. Of the 6-year-olds included in the national survey, 55.09% were considered gingivally healthy29. It is unclear, however, whether those results can be directly compared. In a similar study to the present one, but in the Valparaiso region, 39.10% of children between the ages of 6 and 8 years were healthy while 79.50% experienced bleeding. Furthermore and similar to the EpiMaule study, 96% of the children in the same group were reported to have dental plaque30. Of note, the Valparaiso study also included children of 7 and 8 years of age.
Multiple risk factors have been associated with the onset and progression of periodontal disease and dental caries, including oral hygiene practices, diet, and plaque accumulation. Furthermore, the importance of fluoride, in its various forms, in decreasing the burden of dental caries has been clearly demonstrated31. Despite the role of the aforementioned biological factors, social, cultural and economic factors have been added to the list of risk factors for these common oral conditions. These factors have been shown to have even a greater association with the disease than canonical biological factors4. Future studies should incorporate data on the participant's socioeconomic background, education level and sociodemographic information of their parents or guardians. This more holistic approach to oral health may enhance the understanding of all the factors involved and at the same time facilitate more efficient preventive strategies.
The WHO and FDI World Dental Federation have established clear goals for oral health of the population for the year 202032. It has been proposed that children under the age of 12 years have a maximum of three teeth with caries. Furthermore, a goal of 50% caries-free 5-6-year-old children for 2020 has been set32. According to the data of the EpiMaule study, the objective seems ambitious and difficult to achieve, particularly for rural communities. With the data obtained and analyzed in this study and despite the improvements in lowering prevalence and severity of dental caries, children from the Maule region had an average of 4.8 affected teeth, when deft (4.63) and DMFT (0.24) are added (Table 1). The latter reveals a great gap between the goals set by international health organizations and the current dental health status of the Chilean population, at least in the Maule region. The situation is a little more encouraging in the case of urban communities, which had an average of 3.3 affected teeth, closer to the proposed limit. Rural population, however, shows a much worse situation with almost six teeth affected with caries (Table 1). Based on these data, rural communities should be given priority in oral health policies, including better preventive plans and more access to oral health care. Thus, data obtained from this study will be of importance for public health in Chile and in many other places with highly rural communities. Moreover, these data will serve as a baseline for further studies intended to evaluate the effectiveness of public health policies.
Children of the Maule region in central Chile show high caries prevalence and GIs, largely exceeding those previously reported at the national level. Rural children were more affected than those living in urban areas. Rurality could act as a risk factor for dental caries and to a lesser extent for an altered gingival condition. Specifically designed oral health strategies for the rural population seem reasonable and are highly recommended.
Acknowledgements
The authors thank the students from the Dental School of the University of Talca who participated in registering the data during the field stage of the project. This study was partially funded by a research development program of the IADR awarded by the Australian and Chilean divisions of the IADR and by an internal grant awarded by the University of Talca.
References
1. Marcenes W, Kassebaum NJ, Bernabé E, Flaxman A, Naghavi M, Lopez A, et al. Global burden of oral conditions in 1990-2010: a systematic analysis. Journal of Dental Research 2013; 92(7): 592-597.
2. Martins-Júnior PA, Vieira-Andrade RG, Corrêa-Faria P, Oliveira-Ferreira F, Marques LS, Ramos-Jorge ML. Impact of early childhood caries on the oral health-related quality of life of preschool children and their parents. Caries Research 2013; 47(3): 211-218.
3. Petersen PE, Bourgeois D, Ogawa H, Estupinan-Day S, Ndiaye C. The global burden of oral diseases and risks to oral health. Bulletin of the World Health Organization 2005; 83(9): 661-669.
4. Fontana M, Jackson R, Eckert G, Swigonski N, Chin J, Zandona AF, et al. Identification of caries risk factors in toddlers. Journal of Dental Research 2011; 90(2): 209-214.
5. World Health Organization. Social determinants of Health. Progress on the implementation of the Rio political declaration. (Online) 2013. Available: http://www.who.int/social_determinants/thecommission/finalreport/en/ (Accessed 13 November 2013).
6. Rwenyonyi CM, Muwazi LM, Buwembo W. Assessment of factors associated with dental caries in rural communities in Rakai District, Uganda. Clinical Oral Investigations 2011; 15(1): 75-80.
7. Zander A, Sivaneswaran S, Skinner J, Byun R, Jalaludin B. Risk factors for dental caries in small rural and regional Australian communities. Rural and Remote Health 13(3): 2492. (Online) 2013. Available: www.rrh.org.au (Accessed 15 June 2015).
8. Maupome G, Martínez-Mier EA, Holt A, Medina-Solís CE, Mantilla-Rodríguez A, Carlton B. The association between geographical factors and dental caries in a rural area in Mexico. Cadernos de Saúde Pública 2013; 29(7): 1407-1414.
9. Rodakowska E, Wilczy?ska-Borawska M, Bagi?ska J, Stokowska E. Epidemiological analysis of dental caries in 12-year-old children residing in urban and rural settings in the Podlaskie region of north-eastern Poland. Annals of Agricultural and Environmental Medicine 2013; 20(2): 325-328.
10. Sufia S, Chaudhry S, Izhar F, Syed A, Mirza BA, Khan AA. Dental caries experience in preschool children: is it related to a child's place of residence and family income? Oral Health & Preventive Dentistry 2011; 9(4): 375-379.
11. Soto L, Tapia R, Jara G, Rodríguez G, Urbina T, Venegas C. National assessment of the oral health of 6 year-old children. Santiago, Chile: Health Ministry (MINSAL). 2007.
12. United Nations. Desarrollo Humano en Chile. (Online) 2008. Available: http://desarrollohumano.cl/idh/download/pnud_rural.pdf (Accessed 29 September 2014).
13. National Institute of Statistics. Population projections. (Online) 2010. Available: http://www.ine.cl/canales/chile_estadistico/familias/demograficas_vitales.php (Accessed 13 September 2013).
14. World Health Organization. Oral health surveys: basic methods, 4th edn. Geneva: WHO, 1997.
15. SEREMI7. Localidades con Fluoración en agua potable Región del Maule. Talca, Chile: Nuevo Sur SA, 2010.
16. Rajab LD, Petersen PE, Baqain Z, Bakaeen G. Oral health status among 6- and 12-year-old Jordanian schoolchildren. Oral Health & Preventive Dentistry 2014; 12(2): 99-107.
17. Sgan-Cohen HD, Margvelashvili V, Bilder L, Kalandadze M, Gordon M, Margvelashvili M, et al. Dental caries among children in Georgia by age, gender, residence location and ethnic group. Community Dental Health 2014; 31(3): 163-166.
18. Gorbatova MA, Gorbatova LN, Pastbin MU, Grjibovski AM. Urban-rural differences in dental caries experience among 6-year-old children in the Russian north. Rural and Remote Health 2012; 12: 1999.
19. Llompart G, Marin GH, Silberman M, Merlo I, Zurriaga O, GIS (Grupo Interdisciplinario para la Salud). Oral health in 6-year-old schoolchildren from Berisso, Argentina: falling far short of WHO goals. Medicina Oral, Patología Oral y Cirugía Bucal 2010; 15(1): e101-105.
20. de Souza AL, Leal SC, Bronkhorst EM, Frencken JE. Assessing caries status according to the CAST instrument and WHO criterion in epidemiological studies. BioMed Central Oral Health 2014; 14: 119.
21. Joseph C, Velley AM, Pierre A, Bourgeois D, Muller-Bolla M. Dental health of 6-year-old children in Alpes Maritimes, France. European Archives of Paediatric Dentistry 2011; 12(5): 256-263.
22. Basha S, Swamy HS. Dental caries experience, tooth surface distribution and associated factors in 6- and 13- year- old school children from Davangere, India. Journal of Clinical and Experimental Dentistry 2012; 4(4): e210-216.
23. Irigoyen ME, Mejía-González A, Zepeda-Zepeda MA, Betancourt-Linares A, Lezana-Fernández M, Álvarez-Lucas CH. Dental caries in Mexican schoolchildren: a comparison of 1988-1989 and 1998-2001 surveys. Medicina Oral, Patología Oral y Cirugía Bucal. 2012; 17(5): e825-e832.
24. Cárdenas C, Saavedra M, Giacaman RA. Caries and gingivitis changes among 6 and 12 year-old children of Peralillo, Chile, between 2000 and 2010. Revista Clinica de Periodoncia, Implantología y Rehabilitación Oral 2011; 4(3): 102-105.
25. Bratthall D. Introducing the Significant Caries Index together with a proposal for a new global oral health goal for 12-year-olds. International Dental Journal 2000; 50(6): 378-384.
26. Rodriguez G, Cabello R, Urzua I, Faleiros S. Inequalities in dental caries distribution between fluoridated and non-fluoridated regions in Chile in 2008. 58th Annual ORCA Congress (Abstracts). Caries Research 2011; 45: 205.
27. Piovesan C, Mendes FM, Antunes JL, Ardenghi TM. Inequalities in the distribution of dental caries among 12-year-old Brazilian schoolchildren. Brazilian Oral Research 2011; 25(1): 69-75.
28. Quinteros ME, Cáceres DD, Soto A, Mariño RJ, Giacaman RA. Caries experience and use of dental services in rural and urban adults and older adults from central Chile. International Dental Journal 2014; 64(5): 260-268.
29. MINSAL. Resumen Ejecutivo Estudios de Difusión e Implementación de la Garantía Explícita: Salud Oral Integral para niños de 6 años. Santiago, Chile: Ministry of Health (MINSAL), 2008.
30. Badenier O, Moya R, Cueto A. Prevalencia de las enfermedades Buco dentales y necesidades de tratamiento de la V Región. Valparaíso, Chile: Proyecto FONIS, 2007.
31. Yeung CA. A systematic review of the efficacy and safety of fluoridation. Evidence-Based Dentistry 2008; 9(2): 39-43.
32. Hobdell M, Petersen PE, Clarkson J, Johnson N. Global goals for oral health 2020. International Dental Journal 2003; 53(5): 285-288.


