Introduction
Problems associated with recruiting and retaining doctors in non-metropolitan areas have been acknowledged by governments in Australia, the US, Canada and elsewhere as a continuing concern1,2. Since the early 1990s, the Australian government has introduced a range of initiatives designed to improve the supply of, and access to, doctors in rural areas3-6.
These initiatives, however, have not resulted from any comprehensive or system-wide analysis of the problem of medical workforce supply and distribution. Rather, they have largely been a response to numerous reports into particular aspects of the overall problem7,8, or responding to various lobby groups (such as local government, Rural Doctors Association)9 or the opposition parties. Indeed, many of the most recent initiatives have arguably been directed to placating the demands of parliamentarians whose marginal electorates include communities designated as under-supplied with doctors or classified as 'areas of need'10.
Considerable resources from both Commonwealth and State governments, as well as local communities, have been invested in these rural medical workforce initiatives and programs. For example, the Regional Health Strategy announced by the Minister for Health and Aged Care in 2000 was budgeted at AU$562 million5. The Rural Retention Program alone, which makes payments to GPs based on their length of service and the remoteness of the area in which they practice, has a budget of AU$81.6 million for the period 2003-200711.
In view of the plethora of recruitment and retention initiatives and their not insignificant cost, it is important and timely to ascertain which of the many factors that might be addressed by these initiatives are likely to have the most impact on recruitment or retention. In addition, given that the relevance and significance of such initiatives may differ according to geographical location, it is appropriate to gauge whether doctors' perceptions of the initiatives' importance vary according to the size and degree of rurality or remoteness of communities.
The objective of the present study was to examine the effectiveness of different recruitment and retention incentives from the perspective of the rural GP, who is well placed to make judgements about their relative merits. Doctors practising in rural and remote communities were, therefore, asked to indicate their perceptions of the relative importance of several possible interventions, in terms of their impact on recruitment to and retention of GPs in their communities.

Figure 1: Australia's Medicare.
Methods
The questions
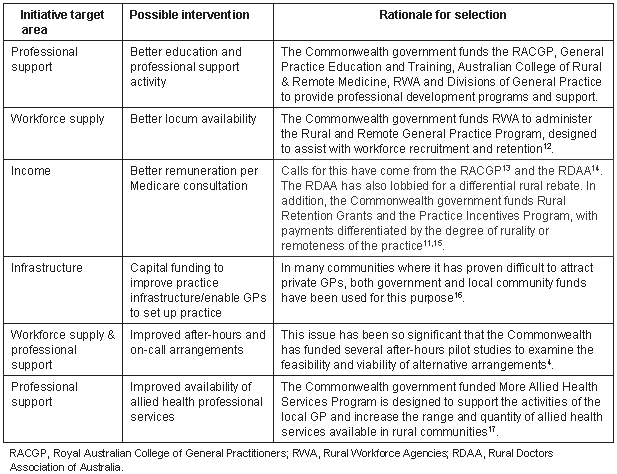
Six possible interventions which cover the major objectives underpinning rural workforce initiatives most relevant to doctors currently in rural practice were selected. Their selection was guided by the recruitment and retention literature and the recommended and actual initiatives emerging from that body of knowledge. The number of interventions was limited to six to minimise fatigue from the ranking task. These interventions, together with the respective initiative target areas are listed in the order of presentation (Table 1).
Respondents were asked to assign a rank from 1 to 6 to indicate the relative importance of each item ('1'= 'most important' to '6' = 'least important') with respect to the question "What would help most to attract more GPs to this community?". The task was then repeated with the question "What would help most to retain GPs in this community?"
Table 1: Initiative areas, possible interventions and rationale for selection for ranking task
GP selection
The data were collected as part of a national study into the viability of rural general practice undertaken jointly by the Rural Doctors Association of Australia and Monash University School of Rural Health Bendigo18,19. Using contact details provided by the Australian Health Insurance Commission, all general practitioners providing non-referred services for an average of one day per week or more in RRMA 3 to RRMA 7 communities were surveyed during winter 2002. Because this analysis was concerned with the perceptions of those doctors with potentially some proprietorial interest in and responsibility for their practices, only the responses of practitioners nominating themselves as practice principals, partners or associates (termed 'owners' from here on) are included.
Rurality indicator
The Rural Remote and Metropolitan Area (RRMA) classification was used as the indicator of rurality20. This classification is used for determining the levels of assistance available through a number of Commonwealth initiatives, such as the Practice Incentives Program15.
Analysis
Responses that had validly ranked all items per question were included in the analysis. Tied ranks were excluded (<0.7% of respondents). Mean ranks were calculated for each item. These item means were then ranked to indicate the most through to least important items for respondent GPs in total and within each RRMA category, as well as for the control variables of practice size and GP sex.
The SPSS program procedure 'Explore' (SPSS Inc; Chicago, IL, USA) was used to calculate item means and to determine the 95% Confidence Intervals. Figures 2 and 3 were prepared using Microsoft Excel.
Ethics approval
The study was approved by the Monash University Standing Committee on Ethics in Research Involving Humans.
Results
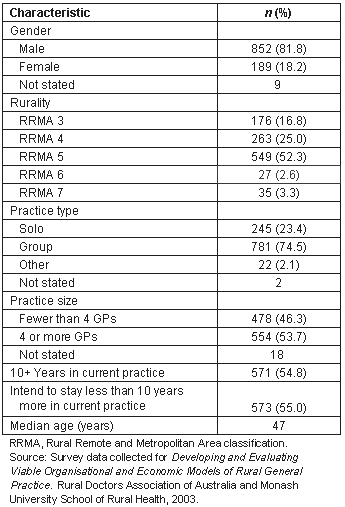
Thirty-five percent of all GPs practising in rural and remote Australia responded to the national survey, representing 53 percent of practices in those areas18,19. A total of 1050 respondents nominated themselves as owners of their practice. Table 2 shows the characteristics of these respondents. The majority have been in their practice for more than 10 years and thus have had the opportunity to see the effects of recruitment and retention initiatives.
Table 2: Characteristics of practice owner GPs
Eighty-three percent of the eligible respondents provided valid responses to the question on what would help to attract GPs and 85% to the question on retention. The results, including their statistical significance are shown (Table 3). (Note that lower item mean equates to higher rank.)
Table 3: Means, ranks and confidence intervals for the importance of 6 intervention items to recruitment and retention, as perceived by owner GPs
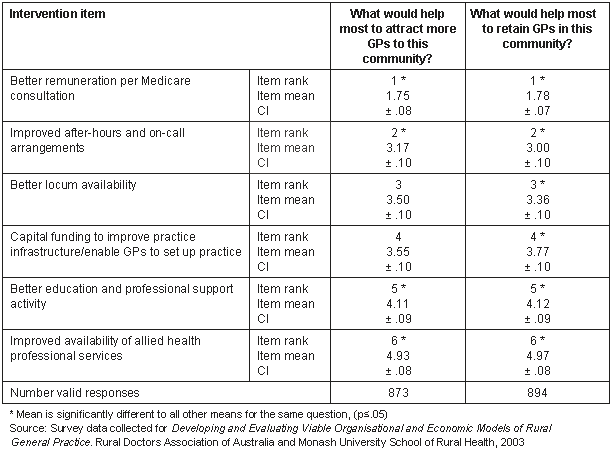
The most notable finding is the high degree of agreement in the responses to the two questions, with the possible interventions being ranked in the same overall order for both. 'Better remuneration for Medicare consultations' and 'Improved after-hours and on-call arrangements' were ranked as the most important interventions for both attracting and retaining GPs, whereas 'Better education and professional support activity' and 'Improved availability of allied health professional services' were ranked as least important of the options presented.
Results of the analysis by degree of rurality and remoteness are displayed (Figs 2,3).
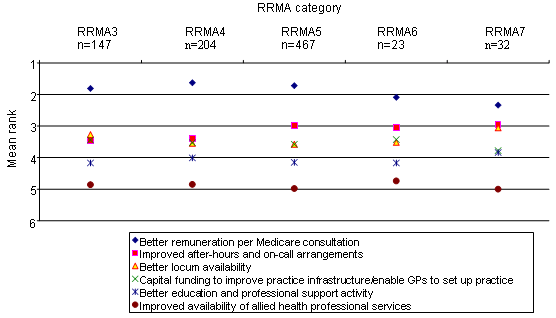
Figure 2: Mean ranks for the importance of intervention items to recruitment by RRMA category, as perceived by owner GPs. Source: Survey data collected for Developing and Evaluating Viable Organisational and Economic Models of Rural General Practice. Rural Doctors Association of Australia and Monash University School of Rural Health, 2003.
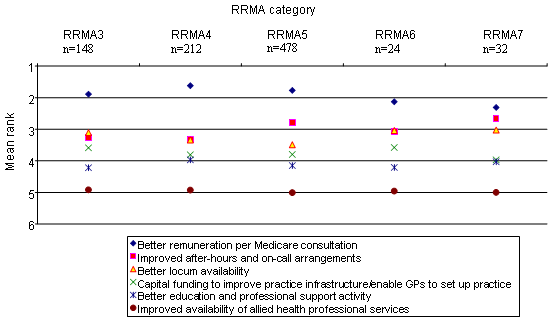
Figure 3: Mean ranks for the importance of intervention items to retention, by RRMA category, as perceived by owner GPs. Source: Survey data collected for Developing and Evaluating Viable Organisational and Economic Models of Rural General Practice. Rural Doctors Association of Australia and Monash University School of Rural Health, 2003.
Analysis by degree of rurality (RRMA 3 to RRMA 5) also found strong agreement on the most important item, 'Remuneration per Medicare consultation', and on the two least important items, 'Availability of allied health services' and (excluding RRMA 4, retention question) 'Education and professional support', on both questions. For the three remaining items, differences between the means were not significant for RRMA 3 and RRMA 4, suggesting owner GPs regarded them as of similar importance. In the RRMA 5 communities, the items 'Better locum availability' and 'Capital funding to improve practice infrastructure' tied for third place on the recruitment question; while, on the retention question the six items were ranked without any overlap between them.
Despite small respondent numbers for the remote RRMA 6 and RRMA 7 communities, it is noteworthy that 'Better remuneration per Medicare consultation' and 'Improved after-hours and on-call arrangements' significantly outranked 'Improved availability of allied health services' for both questions.
Male and female doctors gave identical rankings on both the recruitment and retention questions. The only significant difference when controlling for practice size was that locum availability was rated more important for both recruitment and retention (second compared with fourth) by GPs working in practices with fewer than four doctors.
Discussion
Limitations
Although it was not high, the response rate for this study related to a population, not a sample, and is comparable with response rates for other GP surveys without monetary or other incentives21,22. Because the population of non-metropolitan owner GPs, as defined, is not known, it was not possible to test directly for representativeness of this sub-group, which makes up 70% of all respondents. Comparison of the total respondent characteristics with those of the population revealed a high degree of congruence, with respondent and total population groups within one year of each other on mean and median age, within 2% on sex distribution, within 5% on proportions who were Australian trained, within 7% on proportions within each RRMA category, and with identical proportions of solo practitioners. The one-third of the population who responded were, therefore, representative of the population on these indicators. A lack of evidence of non-response bias in any of the independent variables of interest, coupled with the large proportion of the population who responded, increased confidence in the extent to which findings may be generalised to the population. Caution has been exercised in interpreting results from RRMA 6 and RRMA 7 GPs because the total population of GPs in these locations is only 135 and 178, respectively.
The limited number of possible interventions might also be considered a shortcoming of this study. However, although only six interventions were presented for consideration by GPs, they represent sentinel initiatives selected on the basis of their representativeness of, and centrality to, the major programs directed towards solving the rural medical workforce problem.
Interpretation of results
In general, the initiatives identified by rural and remote owner GPs as being of most value in the recruitment and retention of doctors were those targeting income and medical workforce supply, with income being well ahead of all other items. Initiatives targeting infrastructure funding and professional support were ranked lower. This finding does not indicate that lower-ranked items were regarded by respondents as unimportant. All six items were selected because of the considerable body of evidence indicating their significance in ensuring the recruitment and retention of GPs to rural and remote areas.
Improved income, particularly remuneration from Medicare consultations, has long been an objective of organisations representing doctors in rural and remote regions of Australia. Throughout these regions, many communities are characterised by high medical care needs and generally low incomes23. In such areas, many doctors feel obliged to bulk-bill a large proportion of their patients, thereby limiting their consultation income to the Health Insurance Commission's maximum payment of AU$24.45 per standard consultation at the time of the survey. The recently announced MedicarePlus scheme will provide a higher rebate than that paid to metropolitan GPs to doctors practising in RRMA 3 to RRMA 7 and in Tasmania, who bulk-bill for services to children under 16 years and concession card holders24. It remains to be seen what the actual effect will be on GP recruitment and retention in non-metropolitan areas.
After-hours and on-call arrangements were identified as a major issue for rural and remote GPs, even those working in sizeable group practices. Both excessive after-hours on-call and the difficulty in obtaining locums contribute significantly to GP overwork and burnout, so it is not surprising that initiatives designed to address these issues are ranked highly in importance for recruiting and retaining the medical workforce in rural and remote areas.
The lowest ranked item, 'improved availability of allied health professional services', encompasses the objective of the More Allied Health Services program17. This program was established to increase allied health services in rural and remote areas (RRMA 4 to RRMA 7) and in so doing increase opportunities for GPs to access Enhanced Primary Care items on the Medicare Benefits Schedule. (These items require GPs to develop care plans and to case conference with other members of a health care team.) Regardless of the success of this program in meeting its primary objective, it is clear that further improvements in income and the medical workforce supply represent a greater priority for recruitment and retention for owner GPs than further improvements in the allied workforce supply.
Conclusions
Ensuring professional support, workforce supply, income and infrastructure support are all relevant to the recruitment and retention of GPs in rural and remote areas. The present study clearly demonstrates, however, that from the perspective of current owner GPs practising in such areas, specific initiatives that increase the core income of rural practices and which address those medical workforce supply issues which impact most on workload are considered those which are most likely to assist in the recruitment and retention of GPs to Australia's rural and remote communities.
Acknowledgements
The study on which this analysis was based was funded by a grant from the Australian Government Department of Health and Ageing, under the auspices of the Rural Doctors Association of Australia (RDAA) in association with Monash University School of Rural Health Bendigo. The authors gratefully acknowledge the input and assistance of the following: Dr David Mildenhall, Dr Paul Mara, Dr Bruce Chater, Dr Nola Maxfield, Dr David Rosenthal, Mr Brian Curren and Ms Anna Boots of the Viable Models Project Committee of the RDAA, Health Connections, and technical assistance from Ms Vanessa Prince of Monash University.
References
1. Commonwealth Department of Health and Aged Care. The Australian medical workforce. Occasional papers: New Series No. 12. Canberra: Department of Health and Aged Care, 2001.
2. Australian Medical Workforce Advisory Committee and Commonwealth Department of Health and Aged Care. 5th International Medical Workforce Conference 2000: Papers. Sydney: Australian Medical Workforce Advisory Committee; 2001.
3. Dugdale P. The Better Practice Program funding formula: a neo-liberal approach to funding general practice. Australian Journal of Public Administration 1997; 56: 65-76.
4. Australian Government Department of Health and Aged Care. People Care Quality Budget 2001-2002 Health Fact Sheet 3. Canberra: AGPS, 2001. Available: http://www.health.gov.au/budget2001/index.htm (Accessed 27 May 2004).
5. Australian Government Department of Health and Aged Care. More Doctors, Better Services. Regional Health Strategy. Canberra: AGPS; 2000 Available: http://www.health.gov.au/budget2000/rural.pdf (Accessed 27 May 2004).
6. Australian Department of Health and Ageing. Health Budget 2003-2004 - Fact Sheet 6. 13 May 2003.Canberra: Australian Department of Health and Ageing, 2003.
7. Shehadie N. Report of the Committee of Enquiry into Services Provided by General Medical Practitioners to Country Public Hospitals. Sydney: New South Wales Department of Health, 1987.
8. Western Australian Health Department. Report of the Ministerial Inquiry into the Recruitment and Retention of Country Doctors in Western Australia. Perth: Western Australian Health Department, 1987.
9. Rural Doctors Association of Australia. RDAA Responses to Regional Australia Summit Theme 3 Health. Canberra: RDAA, 1999.
10. Anastasopoulos C. Tasmanian boost leaves other GPs in the cold. Australian Doctor, 26 March 2004; 2.
11. Australian Government Department of Health and Ageing. Rural Retention Program - Funding arrangements for 2003-07. Canberra: DHAC; 2004. Available: http://www.health.gov.au/pcd/programs/ruralgp/rurret/funding.htm (Accessed 25 May 2004).
12. Australian Department of Health and Ageing. Rural Workforce Agencies. Canberra: ADHA, 2003. Available: http://www.ruralhealth.gov.au/workers/rwa.htm (Accessed 22 June 2004).
13. Hemming P. College calls for rebate increase for all GPs. RACGP (Online) 2001. Available: http://www.racgp.org.au/document.asp?id=4118 (Accessed 27 May 2004).
14. The Rural Doctors Association of Australia, Australian Local Government Association, Country Women's Association of Australia, Health Consumers of Rural & Remote Australia, National Farmers Federation. Good health to rural communities. A collaborative policy document. Canberra: The Rural Doctors Association of Australia, Australian Local Government Association, Country Women's Association of Australia, Health Consumers of Rural & Remote Australia, & National Farmers Federation, 2004.
15. Commonwealth Department of Health and Aged Care. An Outline of the Practice Incentives Program July 2001. Canberra: DHAC, 2001. Available: http://www.hic.gov.au/providers/incentives_allowances/pip.htm (Accessed 29 April 2004).
16. NSW Rural Doctors Network. Easy Entry, Gracious Exit. Newcastle: NSW Rural Doctors Network, 2003.
17. Commonwealth Department of Health and Ageing. Guidelines for the More Allied Health Services Program. May 2002 edn. Canberra: CDHA; 2002 Available: http://www.ruralhealth.gov.au/services/mahs.htm (Accessed 12 May 2004).
18. Rural Doctors Association of Australia, Monash University School of Rural Health. Viable Models of Rural and Remote Practice. Stage 1 and Stage 2 Reports. Canberra: Rural Doctors Association of Australia, 2003.
19. Jones JA, Humphreys JS, Adena MA. Doctors' perspectives on the viability of rural practice: 305. (Online) 2004. Available: http://rrh.org.au/journal/article/305 (Accessed 20 August 2004).
20. Department of Primary Industries and Energy, Department of Human Services and Health. Rural, Remote and Metropolitan Areas Classification 1991 Census Edition. Canberra: Australian Government Publishing Service, 1994.
21. Kellerman SE, Herold J. Physician response to surveys. A review of the literature. American Journal of Preventive Medicine 2001; 20: 61-67.
22. McAvoy BR, Kaner EF. General practice postal surveys: a questionnaire too far? BMJ 1996; 313(7059): 732-733.
23. Haberkorn G, Hugo G, Fisher M, Aylward R. Country matters Social Atlas of Rural and regional Australia. Canberra: Bureau of Rural Sciences, 1999.
24. Australian Government Department of Health and Ageing. MedicarePlus Factsheets (update). Canberra: AGPS, 2004. Available: http://www.health.gov.au/medicareplus/update_march_04/glance04.htm (Accessed 12 May 2004).


