Introduction
The epilepsy rate in Kilifi, Kenya, where the present study was conducted, is estimated to be 9% - one of the highest on the African continent1,2. The high prevalence of epilepsy in the developing world may be related to more prevalent alcoholism and childhood trauma3, as well as poor sanitation that includes parasitic contamination4. Other research suggests that the high rates of epilepsy in developing countries may reflect marriage practices in which individuals with epilepsy are the only suitable partners for others with the disorder, or may result from perinatal head trauma associated with the birthing practices of some cultures5. Striking gaps in Kilifi between the prevalence of epilepsy and the number of individuals receiving effective biomedical treatment make these statistics even more dramatic6.
In this article, the public health issues of access to care are addressed with an intervention design from an anthropological perspective that focuses on treatment providers. Previous studies have documented the epilepsy treatment gap (TG) and identified demographic and resource-related barriers to treatment-seeking7-10. Ethnographic studies have concentrated on the treatment decision-makers, examining motives beyond material resource factors including cultural models, past experiences and assessment of results11-20. However, few studies have examined the social and procedural factors that shape and constrain choices, such as the roles of providers in the community, and structural differences between biomedical and alternative treatments21. Furthermore, explanations by decision-makers given for past treatment-seeking events may be attempts to establish meaning and continuity for choices already made and may not capture the actual decision-making process22,23.
To address these shortcomings, this study focused explicitly on treatment providers as a source of data and the ways in which treatment-seeking may be facilitated or deterred by the availability of treatment options and characteristics of service providers, rather than by characteristics of the persons in need of treatment (a study by Finkler15 is a notable example of this approach). Therefore the following analysis does not represent a comprehensive decision model about how families seek care for children with chronic epilepsy. Instead it documents factors related to treatment providers in these decision-making processes. Furthermore, the comparison between provider characteristics represents an important tool in intervention research and serves as a means of identifying and assessing structural barriers to treatment-seeking and adherence.
A comparative ethnographic approach was employed to explore the distinguishing characteristics of services for childhood epilepsy in Kilifi. To our knowledge, this is the first study to contrast the characteristics of service providers as potential determinants of treatment choice for children with epilepsy. A review of data from our sample of providers revealed important differences between the two options that inform future efforts to develop a more effective healthcare delivery system.
Study area and religious beliefs
Kilifi town, the administrative center of the Kilifi District, is approximately 64 km north of Mombasa, Kenya's second largest city, and 64 km south of the city of Malindi. The majority of people who live in this coastal district reside in rural areas. Traditionally, Arab traders and the Islamic religion have had a strong presence on the coast. However since the time of British colonization, Christianity has become more prominent. The majority of the traditionally up-country tribes and some members of the coastal tribes practice various forms of Christianity24. Forty-seven per cent of individuals in the study area identify as Christian, 13% Muslim, 24% Traditionalists, 12% 'other', and 4% unknown25. Some tribes, such as the Giriama, have managed to retain elements of their unique religious beliefs and practices that form the basis of traditional healing and local epilepsy beliefs24.
Treatment in Kilifi
Traditional: While Parkin has provided invaluable background on the Mijikenda culture24,26-29, treatment-seeking in this area remains largely unstudied from an anthropological perspective. The most notable exception is the work of Susan Beckerleg in a Swahili settlement in Watamu located in Malindi District, to the north of Kilifi District11. While her findings are illuminative of health beliefs and healing related to fever, or homa, in this Swahili cultural pocket, treatment and treatment-seeking in Kilifi District vary dramatically from what is described in her study. Differences include the underlying model used to explain illness and treatment, and the actual treatment techniques employed30. For example, individuals in the Beckerleg study attributed illness to imbalances in hot and cold states, while for the Mijikenda, ill health is less frequently about these humoral balances and more often perceived as the physical manifestation of events occurring in the spiritual realm. Thus, while many of the treatments Beckerleg describes are designed to improve balance, Mijikenda treatments focus on communicating with spirits and addressing the needs and desires of these spirits. These differences are likely due to the fact that Beckerleg studied a Swahili population, while the present study focused on traditional Mijikenda beliefs and practices.
In the system of Mijikenda traditional healing, illnesses, as well as social problems more generally, are caused by a system of spirits. This system can be divided into four general categories. Healers deal with each of these categories by employing a different general treatment ideology.
In cases where traditional treatment is sought, the healer must divine which type of spirit is causing a particular problem, determine the best way to deal with the spirit responsible, administer the treatment, and finally follow up to assess the necessity of on-going intervention. The perception of which spirit is causing a problem is key to determining which specific treatment will be used and, because certain healers are specialists in dealing with specific spirits, who the most qualified healer is to administer such treatment.
Biomedical: Biomedical treatment in Kilifi is provided by a government hospital, government health centers, and private clinics. Kilifi District Hospital (KDH), the only hospital in Kilifi District, is located in Kilifi town. Thirty-four government health centers and dispensaries are dispersed throughout the district, staffed by doctors, nurses, and health workers with various degrees of training in biomedicine, ranging from limited course work and experience, to medical degrees and extensive experience in practice. In addition, approximately 25 private clinics operate in the district, which vary widely in staff training and medication supplies.
The KDH, in conjunction with Kenya Medical Research Institute-Coast, operates a special clinical program for children with epilepsy. It provides free assessment and clinical services and anti-epileptic drugs (AEDs) at subsidized prices and is staffed by three clinicians with experience in the management of epilepsy. Government health centers do not offer this level of service. The latter facilities are only permitted to prescribe the AED phenobarbitone, and consistently lack supplies of even this medication. The staff members at these health facilities and at private clinics frequently have little training in epilepsy diagnosis and management. Research with families of children with epilepsy in Kilifi30 revealed that neither government nor private clinics are seen as viable options for epilepsy treatment, and that KDH is perceived as the only option for biomedical treatment of the disorder.
Methods
Sample and procedures
Treatment provider data was collected from approximately 200 hours of person-centered interviews31 and observations over 9 months with a group of traditional healers. Data consisted of both audiotaped interviews and field notes from informal participant observation sessions. Researchers observed a total of 52 healing sessions with these healers. The traditional healer sample was selected using a combination of convenience and snowball sampling. Researchers located the families of children with epilepsy in four different sub-locations of Kilifi District. Families were asked to identify traditional healers who were known to provide treatment for epilepsy. Healers identified by members of multiple families were located and asked if they would be willing to participate in the study. One healer was selected from each sub-location. Each of these healers was then asked to identify a colleague who also treated epilepsy. This procedure resulted in final sample of eight traditional healers from approximately 35 to 60 years of age. The sample of traditional healers also represented a range of treatment specializations or specific 'types of spirits' that the individual was known to be proficient in treating.
To understand the types and delivery of treatment provided in KDH, area clinics, and drug dispensaries, interview and observation data was gathered between the years 2005 and 2007 from 12 biomedical health workers, including doctors, neurological technicians, research staff, nurses and general health aids. This sample was also assembled using convenience and snowball sampling. Several medical professionals working in the epilepsy clinic at the district hospital were approached. These individuals referred the researcher to other health workers involved in epilepsy treatment. Efforts were made to select a sample that represented the range of biomedical services and professional specialization and training in Kilifi. However, the sample was purposefully selected to over-represent health workers at the district hospital. This choice was made after preliminary research revealed problems relating to the supply of drugs and training of staff at local clinics and dispensaries. The research suggested that the district hospital was the primary, if not the only, practical place for families to seek biomedical care for their children.
Following transcription and translation, NVivo qualitative analysis software (QSR; Melbourne, Vic, Australia; http://www.qsrinternational.com/) was used to analyze both transcripts and field notes to generate themes and code materials. To assure informant anonymity, each participant was given a pseudonym that was used in all research and publication materials; only two researchers had access to data during the project.
Ethics
All participants in the study were given an oral description of the study design, purpose, and consent procedures. Participants were also given a page of written description of these procedures and the local contact information of the lead researcher. Each participant signed written consent to participate in the research. Human subjects approval was obtained from the Kenya Medical Research Institute and the University of California, Los Angeles.
Results
Epilepsy in the spirit system of traditional healing
Within the four-category framework of the Mijikenda system of traditional healing, there are three causes of epilepsy, or Kifafa as it is traditionally called.
Natural spirits (mapepo ya pori): Natural spirits are believed to cause a variety of diseases and conditions, including dizziness, and loss of appetite. Individuals may be infected by one of these spirits if they have passed the residence of a natural spirit, or if the spirit is attracted to the 'sweetness' of the person's blood. Mzee Haro, one of the healers in the sample, explained:
This woman here [healer points to the patient] she is having stomach problems because she now has Mapepo ya Bahari [spirit of the beach]. She said that she passed by a large cave at the beach the other day in the evening. This is when the spirit came to her. Now it will not leave.
Nyagu is the natural spirit most commonly considered to cause seizures in the traditional system. Mzee Makanju, another healer in the sample, explained, 'These are spirits that live in the environment, they come as signs of animals. When a child sees the vision of a hawk in his mind Nyagu has come to him'. Seizures occur when the spirit comes to a child and subside when the spirit leaves. Tremors and convulsions experienced during seizures are perceived as attempts to break free of the Nyagu. Nyagu is attracted by the smell or taste of certain children's blood. The spirit's preference for specific types of blood is used to explain why the spirit comes to some children and not others, as well as variation in the persistence of childhood seizures. If the Nyagu continues to visit the child, the spirit matures and reaches full maturity when the child is between the ages of five and ten, at which point the condition transforms from Nyagu to Kifafa.
Kifafa caused by Nyagu is thought to be heritable to some degree. Once a member of a family has a Nyagu spirit, it may develop a proclivity to the person's blood and be drawn to other members due to familial similarities in blood. Mama Mzingo, a healer, explained, 'Nyagu can come from the mother to the child but then if it is not treated by a healer it can move to another child in the family'. There is also the belief that Nyagu may be transmitted from mother to child while breast-feeding. For this reason a mother with epilepsy is not to breast feed her children.
There are two essential components of treating a natural spirit: removal and deflection. A healer must remove the spirit and assure that it does not return. As natural spirits inhabit an individual they develop an affinity for the person's blood. Treatment becomes more difficult and the prognosis less promising if the person has been living with the spirit for an extended period. An immature Nyagu is weak, can be easily pulled from the child, and prevented from re-entering. As the spirit matures, treatment becomes more difficult. For this reason, in the traditional system, early treatment of this condition is paramount.
The methods healers use to remove natural spirits fall into two general groups. First, a healer can drive the spirit out using herbal baths, root concoctions, or dung that the spirit is known to dislike. Mzee Makanju explained, 'It [a specific herbal mixture] drives the Nyagu out. It does not like the smell of my medicines'. Another healer explained his treatment for immature Nyagu:
You must look for the Mtasalafu, Mrori, and Mrashapungu. You must bring these leaves and tear them up and mix them in a container [bucket] of water. You may have to go far to find these, but for me they are not far. The child must come and be washed in the water [with the leaves]. It is very important to wash the head of that child. If you are able it is good to get elephant dung and burn this near the child to smoke him [the child]. The spirit does not like these two things and will go from the child...Also, if you are a Muslim and know how to read from the Koran you can read 'The Resurrection' verse. The Nyagu does not like the verse and it is very powerful for treating Nyagu. Doing these two things will make the child unattractive to the Nyagu.
Healers also explained a process of waving a cloth or basket in front of the patient to 'blow out' the spirit. Mzee Haro explained:
First I go to select those herbs. I put them in a container and fill it with water. When it has been mixed very well I grab the child and dip his head into the water. Then I put the child on the ground and wave a basket over him 7 times. I do this thing in three different places where I know the Nyagu likes to stay [the doorway, the rubbish area, and under a tree]. This is an easy treatment and is not long.
The second method of healing a natural spirit is to entice it out of the person through offerings. Objects offered included incense, herbs, rose water, honey, and animal blood. Once drawn out, the healer calls on his own spirits to battle the natural spirit. Involving other spirits in the cure is thought to be a stronger but more difficult procedure and is used to treat the more mature Nyagu. Mzee Kahindi described this procedure:
You must get a red chicken and a black chicken [the healer later explained that red chickens are for attracting/appeasing spirits from the land and white chickens are for attracting/appeasing spirits that come from the beach/coast]. First I say the part of the Koran that makes the spirit weak because it is now strong...I kill the black chicken and put its blood on the ground. This attracts the Nyagu, which leaves the person to drink the blood. Then I kill the red chicken and put its blood on the ground also. This pulls the Marahani spirit [a very powerful Muslim spirit that Hassan uses in his healing practice]... I then tell the Marahani to kill the Nyagu who is weak from the words of the Koran. If the Marahani is able to defeat the Nyagu, the epilepsy will be cured. It is difficult if the Nyagu is very strong... I must work hard to make the Marahani happy so that he helps me.
Once removed, healers employed techniques to deflect future re-entry of the natural spirit. The two most common practices were to periodically repeat the bathing technique mentioned above and to construct an amulet. The amulet is a pouch the individual wears on a string around their neck, arm, or leg, which contains materials the spirit dislikes. These materials included herbs, roots, or parts of particular animals. Mzee Ruwa, another healer explained:
I make this. [Healer holds up a small leather pouch attached to a string]. I give it to the child and he/she wears it around the neck...I put many things inside. Inside there is hair of the child, leaves, and the claws of a bird. The claws are to make the Nyagu know it will be defeated. It will not come to the child if they wear it.
Majini: Majini are malevolent spirits controlled by witches and are blamed for a host of problems ranging from insomnia to social and economic troubles. Witches are contracted by jealous parties to send Majini to specific individuals or families. Majini are sent in two ways. A witch can draw a special picture in the sand. Once the targeted individual walks over the drawing, the curse is cast. A witch may also send Majini directly to a person by verbally casting a spell. Seizures caused by witchcraft are considered easier to treat than the Nyagu type because Majini are not as strong or persistent as Nyagu.
Healers employed methods of reversal to treat these problems. The healer typically guides the patient back across the symbol believed to have caused the illness, and in this way reverses the curse. This procedure is called mihambo. Mama Mzingo, a female healer explained, 'Passing over the drawing that I have said words to breaks the curse'. Mzee Haro explained, 'This is how witchcraft comes and also the way it goes. They [the witch] did this and to heal this it is necessary that I also do this. But my medicine is much stronger'. Majini are also thought to have a fondness for blood or certain foods including coconuts and eggs. For this reason some healers used animal blood in the drawing or placed broken coconuts or eggs beside the drawing. Mama Mzingo said, 'If it [Majini] is happy, it will leave more times than if it is mad. You can't just kick it out. You have to give it something to make it happy'.
The following is an excerpt from an interview with Mzee Ruwa describing the treatment used for epilepsy caused by Majini.
brought that boy to this sacred place here. He sat right there where you are sitting now. I made him sit there while I made the drawing in the dirt. Then I sent Katana to get me the leaves that I use for this problem. I made the boy cross the drawing seven times and each time he crossed I threw some of the herbs on him. I was saying words to the spirits so that they would come and help me change these Majini so that this boy would not be bothered by them anymore.
Ancestral spirits (mapepo ya kiasili): Ancestral spirits are the descendants of original Mijikenda ancestors. The Mijikenda believe that their first traditional healer was Mepoho, the mother of two sisters, Matsezi and Mbodze. These daughters were also powerful healers and had 12 children of their own who became renowned healers. The spirits of these 12 children are the primary Mijikenda ancestral spirits, and can cause various problems from bad luck in farming to headaches and infertility. Other secondary ancestral spirits may also cause these problems, and anyone who has died has the possibility of becoming a spirit of this type and affecting the world of the living.
Ancestral spirits are believed to cause problems because of unfulfilled desires. Mzee Kangwangu, another healer from the sample, said, 'Those spirits [ancestral spirits] are always wanting things. They want a chicken or goat or even a piece of cloth...They are like living people, they just want things to have them, because they are hungry'. An ancestral spirit may also demand a sacrifice due to improper behavior.
Healers employed an appeasement ideology to treat illnesses caused by ancestral spirits. The healer communicates with the spirit, or through a proxy spirit, to learn what items or actions are desired. As a temporary appeasement, the healer may offer the spirit an herbal or root concoction. However, to cure the affliction, the desired items must be offered. Commonly desired items included goats, chickens, or swatches of colored cloth.
Epilepsy may be transferred between family members if specific rituals are not performed following the death of a member with epilepsy. When someone with Kifafa has died, a special set of rituals must replace normal funeral procedures. The family is not to remain in the village for the normal mourning period, and they are not to perform the normal funeral anniversary ceremony. The family is to bury the individual and must have a traditional healer present to prepare a special herbal mixture that each family member must wash with. The concoction is believed to repel the spirit of the deceased. Several months after the burial, the family must again enlist the help of a healer to prepare a second herbal bath to ensure the spirit does not return. If these rituals are not performed, the spirit of the dead relative may return and the next child born may have the condition. As Mzee Kahindi said, 'If the funeral is handled correctly there will be no infection'. Mzee Kahindi elaborated on the treatment used for epilepsy inherited from a relative:
[This type of epilepsy] can be treated. The people who have celebrated the funeral and have done all of the normal things ask for forgiveness from the spirit of the person who is causing the illness in the child. They must make offerings to this spirit. It might be a goat or even a cow if they have one. They must tell the spirit that they are sorry for having made a mistake and they should try to make the spirit happy. This is why they must make a sacrifice. If the spirit is not made happy the child will continue having seizures. This is an easy kind of epilepsy to treat because all you must do is make the spirit forgive you and then it will go.
Islamic spirits (mapepo ya Kiislamu): Islamic spirits are not believed to cause epilepsy. They are the spirits of important Muslim teachers and religions figures and are believed to be more powerful than their Mijikenda counterparts. This power is attributed to two factors. First, they gain strength from the spiritually powerful places they inhabit. Second, they are associated with the Koran, which is a powerful spiritual symbol in the coastal region. Because of the tremendous spiritual power required to manipulate one of these spirits, they are rarely sent. Islamic spirits, like the Mijikenda variety, come to living individuals because of specific desires.
Distinguishing features of the biomedical and traditional treatment options
Interviews with and observations of traditional healers and biomedical personnel revealed several characteristics that distinguished these two treatment options (Table 1).
Table 1: Summary of the comparison of traditional healers' and biomedical treatments
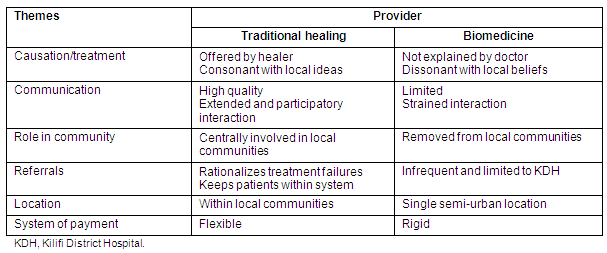
Explanations of causation: Biomedical explanations of causes, symptoms, and treatment were dramatically different from those employed in traditional healing. Traditional healers referred to spirits to explain the occurrence and intermittent presentation of seizures. The spirit comes to an individual and causes a seizure, and the individual regains consciousness with the spirit's departure. Symptoms are sporadic because of Nyagu's attraction to multiple children concurrently. Similar explanations were offered for symptoms of epilepsy caused by Majini. Healers accounted for the tremors and shaking associated with seizures as the struggle between the affected individual and the spirit grabbing them. The common looks of surprise or screams prior to seizure onset were rationalized as the individual's reactions to the spirit's sudden appearance. The traditional system offered treatments that directly addressed the assumed causes of the patient's symptoms. Biomedical practitioners and treatments did not address the connection between causation, treatment, and seizure symptoms.
Communication style: Communication during treatment also differed substantially between the two treatments. One patient summed it up:
When I am at this place [the traditional healer] I can sit and talk and explain things for many hours. Sitting here is important for healing. It is necessary to do this if you want to be cured...I walk here and then return [over the diagram the healer has drawn]. I turn this way and follow his instructions...when I go to Kilifi [hospital], the doctor does not talk to me. He just asks me some few questions and then gives me a paper [prescription]. That is it!
The traditional process of diagnosis and treatment involved constant communication between healer and patient over a one- to four-hour period. To establish a diagnosis, patients were asked numerous questions and encouraged to communicate with the spirit via healer-facilitated 'channeling'. Conversations during treatments covered subjects directly related to the illness as well as general community topics, and the patient was a physically active participant in the healing process.
In contrast, appointments at clinics and hospitals were brief, and doctor/patient interaction limited. Patients were not acquainted with their doctors and the average length of visit was less than 20 min. Communication was frequently strained and patients were guarded in sharing personal information. Biomedical patients were also passive rather than active participants in their care. Typically, they sat in a chair in an office, answered a few questions, sometimes without having the doctor even facing them, and were handed a prescription.
Traditional healers also reported strained relationships with doctors and expressed animosity towards them. One of the healers in the sample explained, '...they [biomedical doctors] do not care about us here in the community. They do not talk to healers or even know what we do, but they think we are all quacks!' The general community perceived this dynamic, and several patients reported social pressure not to seek care from biomedical facilities.
Social roles of providers: Most of the biomedical practitioners interviewed were wealthy and well educated by community standards. Many of those who practiced at KDH were Kenyans from other areas of the country who trained at national universities. Some expatriate doctors working at the Kenya Medical Research Institute also saw patients at the hospital. Doctors at KDH were generally not members of the communities they treated and were unaware of the daily activities and lives of their patients, nor did they hold much power in community social or political dynamics. Unlike traditional healers who lived in the same communities as their patients, biomedical health workers were largely unaware of other treatments received by their patients.
However, patients and traditional healers were often members of the same community, shared acquaintances, and were aware of important events in each others' lives. Such familiarity created an open dynamic in which patients freely asked questions and sought further information about the causes of illness and the specific detail of treatments. Healers were well-respected community members, and their ability to communicate with spirits contributed to their elevated status. One healer received up to 15 patients a day, and all had clear advisory roles in a wide range of social issues.
Referral practices: A further distinguishing feature was the manner in which traditional healers referred patients for additional treatment. When treatments failed to reduce or eliminate symptoms, healers claimed that the offending spirit was too powerful or that they were not proficient at handling the specific spirit responsible for the child's disorder. A community member described this referral system:
[Traditional healers] say that they can treat you but when they fail they say 'this spirit was too strong' and they send you to another healer and then to another. You can go to many healers before you get cured because each healer has his own medicines.
Seven of the eight healers in the sample described cases in which their treatments had failed to cure Kifafa (epilepsy). In each case the child was treated a second time. If this second attempt failed, the healer referred the patient to another healer believed to provide more powerful or specialized treatments, maintaining hope in an eventual cure within the traditional system.
In contrast, no explanation was available for the families of children treated at KDH who continued to have seizures. Although these children may have had their AED regimens modified, there were no further biomedical treatment options.
Location of care: The accessibility of care was another distinguishing characteristic. While traditional healers were located within local communities, the only location for viable biomedical epilepsy treatment was in Kilifi Town. Kilifi District is large and many individuals live in rural areas a long way from Kilifi Town and KDH. Because of the lack of effective epilepsy treatment at rural health facilities, individuals had to choose between traveling long distances to KDH or walking minutes to a local traditional healer.
Systems of payment: Finally, the two treatment modalities differed according to models of payment. The traditional healers interviewed used a flexible payment system. Treatment was provided regardless of the individual's ability to pay and payment was not discussed until after treatment. If the individual was unable to pay, they were expected to return and pay at a later date. In 49 of the 52 traditional treatment interactions observed, individuals paid less than 25% of the payment asked by the healer. The balances were carried for several months, or even years, and healers and patients reported that in many cases such debts are never settled. The traditional model of payment was also flexible in terms of the type of payment accepted. Each healer in the sample accepted livestock, grain, palm wine, cloth, clothing, and labor in lieu of monetary payment.
In comparison, individuals were required to pay 40 Ksh (approximately US$0.75) to receive AEDs at KDH. While this treatment was less expensive than that provided by traditional healers, there was no alternative form of payment, and deferrals or loans were not granted.
Discussion
Consistent with previous research in other areas of Africa32-38, this study documented the importance of traditional healers as an option for treatment of childhood epilepsy. However, investigators have rarely compared interview and observation data collected from traditional healers with data from biomedical practitioners as a means of understanding the gap between treatment needs and healthcare utilization, and identifying potential barriers to treatment access and adherence. This research shows this comparative ethnographic method to be particularly useful in identifying targets and questions for further qualitative and quantitative research on decision-making and intervention design.
The extent to which a family's beliefs about epilepsy causation correspond to this traditional system of spirits is important to understanding why some families seek traditional treatments while others choose biomedicine; this is discussed in greater detail elsewhere30. The comparative provider focus used in this study is effective due to the implicitness of cultural models and their role in decision-making39.
Individuals seeking treatment may be limited in explicitly identifying the factors that shape their treatment decisions, such as payment methods, explanations of causation, social roles of providers, and systems of referral. Service providers have a unique perspective on treatment. Their opinions and structural aspects of the services they provide are critical to understanding the determinants of health decisions.
Previous research on families of children with epilepsy has demonstrated that distance-to-facility was an important factor in treatment-seeking30. However, cases in which families were willing to travel significant distances for either treatment option suggests that other factors, such as consonance between a family's beliefs of causation and that employed in treatment, appear to be important considerations in modeling treatment decisions30. In the present study the observed ability of traditional healers to generate convincing explanations for the mysterious, intermittent, and dramatic symptom presentation and to offer logical justifications for treatment helped explain the popularity of traditional epilepsy treatments in Kilifi. In contrast, there were no explanations for failed biomedical treatments for children treated at KDH who continued to have seizures. The traditional system's method of explaining treatment failures and referring patients to other healers plays a role in keeping patients in the traditional system and away from the hospital.
Biomedical practitioners would benefit from instruction in effective and appropriate communication styles. Training in culturally accessible ways of framing epilepsy, symptoms, causation, and treatment in doctor-patient interaction is vital. This component would increase patient satisfaction with biomedical services and improve treatment adherence.
Further, observations of traditional treatment encounters suggested the difference in type and flexibility of payment appears to be a significant factor in families deciding where to seek treatment for their child's epilepsy.
Our results suggest several promising strategies for improving access to biomedical care in Kilifi District. First, because traditional healers are generally well accepted in local communities, and traditional treatments for epilepsy in Kilifi were found to be culturally meaningful, the expansion of biomedical care should involve the cooperation and involvement of traditional practitioners. This could be generalized to other settings where healers assume a major role in treatment.
However, before any traditional healer inclusion program can be implemented, the quality of biomedical care must be addressed. The low quality of epilepsy treatment at health centers throughout the district and the limited accessibility of KDH to those living in remote areas suggest the need to improve services at rural health facilities. Such improvements could be accomplished through a diagnostic and treatment training program instituted and supervised by KDH. Increasing the supply of AEDs to these facilities, and implementing a more flexible payment plan should also be components of such interventions.
Limitations
The primary limitation of this study is the lack of data from individual decision-makers. To address this, research was also conducted with the families of children with epilepsy30. This research obtained information on the perceived relevance of provider characteristics to family members' treatment-seeking. The results corroborate the significance to treatment decisions of factors identified in the present study, such as payment methods, systems of referral, and explanations of causation.
Implications of the study
The findings of this study have implications for future research on treatment-seeking. Comparing treatment providers is a tool for and initial step in building more comprehensive models of treatment decision-making that include factors that facilitate or deter treatment-seeking. These findings are relevant to programs aimed at improving access to health care.
The strategies discussed could be applied in intervention research designed to improve healthcare utilization for children with epilepsy. Outcomes could be assessed by evaluating program effectiveness in decreasing the epilepsy TG and improving the quality of life of children and their families. Treatment studies could also examine the specific intervention components most responsible for improved outcomes, which could be tested in a randomized cluster trial. This would be the ultimate test of the benefits of ethnographic comparisons of service providers.
An intervention program informed by the present findings as well as additional research conducted with families of children with epilepsy is currently being designed in Kilifi. It is hoped that the effectiveness of this program will provide improved healthcare access and reduce the morbidity of childhood epilepsy in the developing world.
Conclusions
The article identified the following six key differences between biomedical and traditional treatments (explanations of causation, communication styles, social roles, referral practices, location and systems of payment) that may help to explain the existence of the biomedical TG in Kilifi. This study suggests that comparing data on treatment providers reveals barriers to obtaining biomedical care, thereby offering an important tool in intervention design research.
Acknowledgements
The authors acknowledge support from the Kenya Medical Research Institute/Welcome Trust, the National Science Foundation, and the Institute of International Education. The authors also acknowledge Thomas Weisner for his guidance on research design, data analysis, and his comments on drafts of the paper. Finally, the authors acknowledge Carolina Izquierdo for her comments on drafts and her guidance on the theoretical underpinnings of the research. Charles Newton is funded by the Wellcome Trust, United Kingdom.
References
1. El Sharkawy G, Newton C, Hartley S. Attitudes and practices of families and health care personnel toward children with epilepsy in Kilifi, Kenya. Epilepsy Behavior2006; 8(1): 201-212.
2. Mung'ala-Odera V, White S, Meehan R, Otieno G, Njuguna P, Mturi N et al. Prevalence, incidence and risk factors for epilepsy in older children in rural Kenya. Seizure 2008; 17(5): 396-404.
3. Shorvon SD. Epidemiology, classification, natural history, and genetics of epilepsy. Lancet 1990; 336(8707): 93-96.
4. Diop AG, de Boer HM, Mandlhate C, Prilipko L, Meinardi H. The global campaign against epilepsy in Africa. Acta Tropica 2003; 87(1): 149-159.
5. Jilek-Aall L, Jilek WG. The Influence of culture on epilepsy in East Africa. Curare 1993; 16(3): 141-144.
6. Carter J. Epilepsy and developmental impairments following severe malaria in Kenyan Children: a study of their prevalence, relationships, clues to pathogenesis and service requirements. PhD dissertation. University of London, 2002.
7. Mansour ME, Lanphear BP, DeWitt TG. Barriers to asthma care in urban children: parent perspectives. Pediatrics 2000; 106(3): 512-519.
8. Coleman R, Loppy L, Walraven G. The treatment gap and primary health care for people with epilepsy in rural Gambia. Bulletin of the World Health Organization 2002; 80(5): 378-383.
9. Weisner C, Matzger H. A prospective study of the factors influencing entry to alcohol and drug treatment. Journal of Behavioral Health Services and Research 2002; 29(2): 126-137.
10. Reilley B, Abeyasinghe R, Pakianathar MV. Barriers to prompt and effective treatment of malaria in northern Sri Lanka. Tropical Medicine and International Health 2002; 7(9): 744-749.
11. Beckerleg S. Medical pluralism and Islam in Swahili communities in Kenya. Medical Anthropology Quarterly 1994; 8: 299-313.
12. Sussman LK. Unity in Diversity in a polyethnic society: the maintenance of medical pluralism on Mauritius. Social Sciences and Medicine 1981; 15B: 247-260.
13. Young JC, Garro L. Medical choice in a Mexican village. New Brunswick, NJ: Rutgers University; 1994.
14. Fabrega H Jr. Disease and social behavior. Cambridge: MIT Press; 1974.
15. Finkler K. Sacred healing and biomedicine compared. Medical Anthropology Quarterly 1994; 8: 178-197.
16. Good B, Delvecchio M. The meaning of symptoms: A cultural hermeneutic model of clinical practice. In: L Esienberg, A Kleinman (Eds). The relevance of social science for medicine. Hingham, MA: Kluwer Boston; 1981.
17. Kleinman A. Patients and healers in the context of culture: an exploration of the borderland between anthropology, medicine, and psychiatry. Berkeley, CA: University of California Press; 1980.
18. Mathews H, Hill CE. Applying cognitive decision theory to the study of regional patterns of illness treatment choice. American Anthropologist 1990; 92: 155-169.
19. Quinn N. Do mfantse fish sellers estimate probabilities in their heads. American Ethnologist 1978; 5: 206-226.
20. McGrath BB. Swimming from island to island: healing practice in Tonga. Medical Anthropology Quarterly 1999; 13(4): 483-505.
21. Good B. Explanatory models and care-seeking: a critical account. In: S Mchugh, TM Vallis (Eds). Illness behavior: a multidisciplinary model. New York, NY: Plenum; 1986.
22. Boster J. Inferring decision making from preferences and behavior: an analysis of Aguaruna Jivaro manioc selection. Human Ecology 1984; 12) 343-358.
23. Bibeau G. At work in the fields of public health: the abuse of rationality. Medical Anthropology Quarterly 1997; 11: 246-252.
24. Parkin DJ. Sacred void: spatial images of work and ritual among the Giriama of Kenya. Cambridge: Cambridge University Press; 1991.
25. Centre for Geographical Medicine (Coast) KMRI, Kilifi, Kenya, Census Division. Religious identification. Kilifi: Kenya Medical Research Institute; 2005.
26. Parkin DJ. Medicines and men of influence. Man 1968; 3(3): 424-439.
27. Parkin DJ. Politics of ritual syncretism: Islam among the Non-Muslim Giriama of Kenya. Africa: Journal of the International African Institute 1970; 40(3): 217-233.
28. Parkin DJ. Palms, wine, and witnesses: public spirit and private gain in an African farming community. San Francisco, CA: Chandler; 1972.
29. Parkin DJ. Swahili Mijikenda: facing both ways in Kenya. Africa: Journal of the International African Institute 1989; 59(2): 161-175.
30. Kendall-Taylor N. Treatment seeking for a chronic disorder: how families in Coastal Kenya make epilepsy treatment decisions. Human Organization 2009; 68(2): 141-153.
31. Levy R, Hollan D. Person-centered interviewing and observation in Anthropology. In: HR Bernard (Ed.). Handbook of methods in cultural anthropology. Walnut Creek, MD: Alta Mira Press; 1998.
32. Birbeck GL. Traditional African medicines complicate the management of febrile seizures. European Neurology 1999; 42(3): 184.
33. Chavunduka GL. Traditional healers and the Shona patient. Gwelo: Mambo; 1978.
34. Feierman EK. Alternative medical services in rural Tanzania: a physician's view. Social Sciences and Medicine 1981; 15(3): 399-404.
35. Gessler MC, Msuya DE, Nkunya MH, Schar A, Heinrich M, Tanner M. Traditional healers in Tanzania: sociocultural profile and three short portraits. Journal of Ethnopharmacology 1995; 48(3): 145-160.
36. McMillen H. The adapting healer: pioneering through shifting epidemiological and sociocultural landscapes. Social Sciences and Medicine 2004; 59(5): 889-902.
37. Millogo A, Ratsimbazafy V, Nubukpo P, Barro S, Zongo I, Preux PM. Epilepsy and traditional medicine in Bobo-Dioulasso (Burkina Faso). Acta Neurologica Scandinavica 2004; 109(4): 250-254.
38. Oppong AC. Healers in transition. Social Sciences and Medicine 1989; 28(6): 605-612.
39. Quinn N, Holland D. Culture and cognition. In: D Holland D, N Quinn N (Eds). Cultural models in language and thought. Cambridge: Cambridge University Press, 1987, 3-40.



