In Canada, insufficient research has been undertaken on the practice environments of registered practical nurses (RPNs) and registered nurses (RNs) with regards to effects on retention1. Overall, 18% of the Canadian population live in rural and remote areas served by 17.5% RPNs. Furthermore, there are two registered nurses working for every one RPN in rural Canada2. In the province of Ontario, with large metropolitan centers in the south, Northern Ontario contains 90% of Ontario's land mass and has only 6% of the province's population3-5. Given concerns about the decreasing numbers of RPNs working in rural Canada2 and how this challenges health organizations, decision-makers, and health human resources investigators6, this area of research is in demand. The issue is recognized as complex and multifaceted and affects every sector of health care and the healthcare environment.
Recruiting nurses in environments where there are staff shortages and high turnover not only affects healthcare workers but also directly influences the safety of health care and outcomes generally. With many RPNs approaching retirement and fewer individuals entering the profession, nursing is experiencing a serious workforce shortage7,8. It is understood that nursing is an especially stressful occupation with unique physical and psychosocial stressors in rural and northern nursing settings. Moreover, northern Ontario residents have higher rates of chronic disease than the average provincial rate and have a higher proportion of the population that are overweight or obese5. Moreover, a higher proportion of the population are heavy drinkers and smokers9.
In 2013, 33 855 RPNs were employed in nursing in Ontario10. Growing fiscal constraints coupled with a persistent shortage of health human resources warrants a greater understanding of the work environment of RPNs including retention factors11-13. Much of the research on nursing retention has focused on the registered nurse as opposed to RPNs, particularly in northern and rural contexts. Examining and understanding this workforce, their work environments, and nurses' responses to their environments is an important antecedent to formulating retention strategies and bolstering health services that promote improved patient, nurse, and organizational outcomes1.
The objective of this article was to investigate the barriers and facilitators to sustaining the nursing workforce in north-eastern Ontario (NEO), Canada. In particular, factors reported to influence RPNs' intent to stay in a nursing position within the next 5 years, based on data from a survey of RPNs working in all nursing sectors of NEO, were explored.
Differences between RNs and RPNs in Ontario
In Ontario, nursing is a profession with two discrete categories: the RN and the RPN. Both categories have a legislated scope of practice, and important practice differences exist between both occupations. RNs in Ontario graduate with a baccalaureate degree in nursing (4 years), while RPNs graduate with a 2-year practical nursing diploma14. In their educational preparation, disparities between the two groups exist in three main areas: depth and breadth of knowledge, competencies required, and expectations for clinical performance. All nursing students learn from the same body of nursing knowledge; RNs study for a longer period of time, thus allowing for greater depth and breadth of foundational knowledge. RPNs study for a shorter period of time, resulting in a more focused body of foundational knowledge15.
Participants
Participants in this cross-sectional study were RPNs working in direct and indirect patient care settings in all specialties across NEO. The home addresses of nurses working in NEO who consented to participate in the study were obtained from the College of Nurses of Ontario; using a simple random sampling strategy and a modified Dillman approach16, including two mail-outs, survey packages were sent to all RPNs (N=1337) working in NEO. The Dillman approach was modified by increasing the time frame between mailings, and recorded delivery/registered mail was not used. The Northeastern Local Health Integration Network (LHIN) defined the geographic boundaries of NEO. A LHIN is a not-for-profit corporation that works with local health providers and community members to determine health service priorities of their regions in Ontario17.
Data collection
The survey package, comprising a cover letter, consent form, business reply envelope and questionnaire, was sent in two separate mailings approximately 4 weeks apart. Questionnaires were tracked and the second mailing was sent to nurses who had not returned a questionnaire prior to the start of the second mailing. Data collection began in March 2011 and continued until July 2011. A lottery prize was offered to one participant and this procedure was in compliance with Laurentian University Research Ethics Board guidelines and protocols.
Measures
The questionnaire was adapted by the authors that focused retention and recruitment issues from an earlier study of RNs in NEO18. The RPN questionnaire comprised 32 questions that inquired about demographics, nursing education, employment, factors influencing recruitment and retention, knowledge of workplace recruitment and retention policies, and awareness of community engagement in the recruitment of nurses. The instrument took approximately 15-20 minutes. This study was part of a larger project evaluating the retention and recruitment factors of RPNs, RNs and Bachelor of Science in Nursing students.
Data analysis
Prior to performing inferential statistical procedures, potential correlates of job satisfaction for rural acute care RPNs were identified based on the literature specific to nurses in rural and northern practice areas11,19,20. Variables included those relating to individual RPNs (sociodemographic, health, and professional), the workplace (organization), the community context, and satisfaction with the workplace and the community where the RPN lived and worked. Variables for analysis were selected based on their putative association with the intent to stay in their current position for the next 5 years11,21,22. Data analysis was performed using STATA v11.0 (StataCorp; http://www.stata.com).
Dependent variable-Intent to stay in your current position for the next 5 years: The following item was an indicator of the dependent (outcome) variable of intention to leave nursing position: 'Do you intend to stay in your current position for the next five years?' The respondent was offered two choices: 'yes' or 'no'. Because the average age of working nurses is increasing, nurses who chose that they were leaving their current position may have been indicating an anticipated retirement or a decision to leave the profession. As the average age of RPNs working is increasing, nurses leaving their current position may act as a reliable proxy of them retiring or leaving the profession.
Inter-rater agreement: Inter-rater agreement was evaluated using Cohen's kappa. All of the paper questionnaires were entered and coded by the primary rater in an electronic database. A second rater was provided a random sample of 25% of the RPN questionnaires. The second rater coded the answers independently of the first rater for six randomly selected questions for each questionnaire. Inter-observer agreement was achieved for RPN (n=506) questionnaires. Cohen's kappa was situated between 0.92 and 1.00, indicating a close agreement between observers for both groups.
Descriptive statistics (eg frequencies, percentages, cross-tabulations, and multivariate odds ratio estimates) were computed using STATA v11.0. Logistic regression models were fitted to provide estimates of multivariable odds ratios and corresponding 95% confidence intervals. Backward stepwise logistic regression analysis was performed using STATA v11.0 using a cut-off of p<0.05 for inclusion. Binary logistic regression was also performed, and intention to stay ('yes', 'no') was the dependent dichotomous variable. Six variables were included as independent predictor variables in the demographics and related factors model: gender, marital status, age, years living in NEO, and whether respondents and their spouses were born and/or raised in NEO. Similarly, eight variables were included as the occupation and career satisfaction factors: child care, workload allocation, internal staff development, the lifestyle of NEO, years of nursing experience, number of hours worked per week, number of overtime hours worked per week, education level, and employment status. Both unadjusted and adjusted logistic regression models were reported.
Ethics approval
The study received ethics approval from the Research Ethics Board at Laurentian University (REB #2011-04-13).
Table 1 shows the demographics of the 506 RPN (37.8% response rate) respondents who participated in this study. The mean age of RN respondents was 48.0 years (SD=10.5) and the mean age for RPN was 47.4 years (SD=10.6). The sample was mainly female (93.3%) and a diploma level of education was the highest education level attained by the majority of RPN respondents. The RPNs had, on average, 19.6 years (SD=11.8) of experience in the workplace. In terms of the participants' current workplace, 35% of the RPNs indicated working in a general hospital. With respect to their intent to stay in their practice, 70.5% of the RPNs reported that they planned to leave their present nursing position within the next 60 months.
Table 1: Characteristics of registered practical nurse respondents
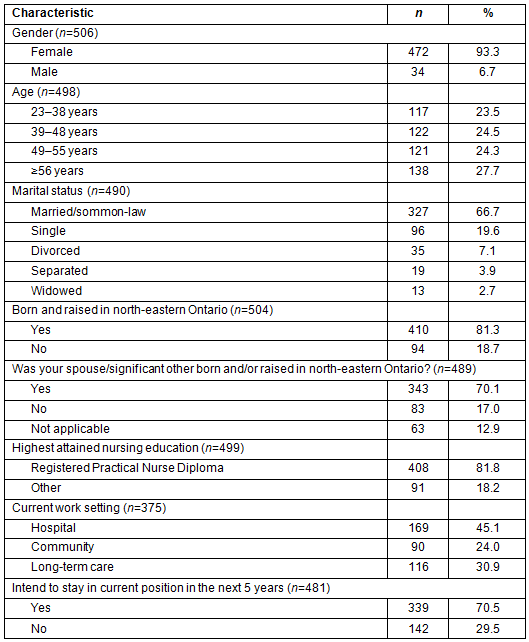
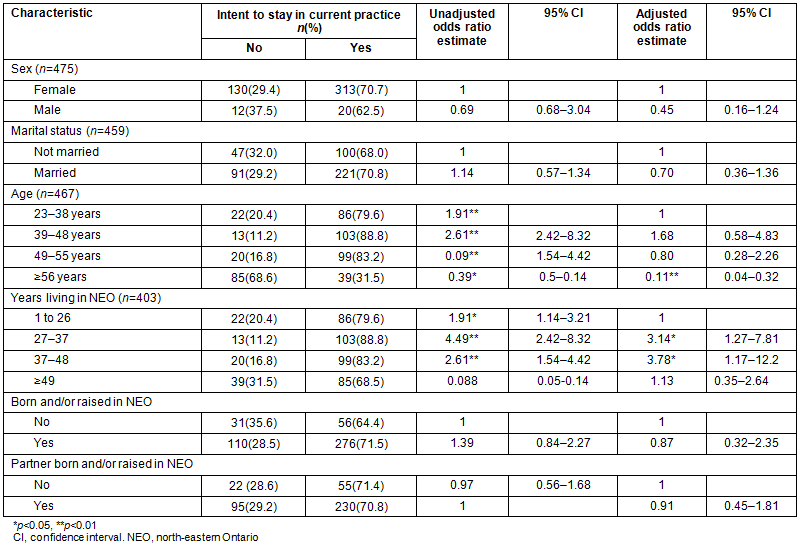
Table 2: Multivariable adjusted odds ratio estimates and approximate 95% confidence intervals
of demographic and related factors associated with intent to stay of registered practical nurses
Multivariable factors associated with ITS among RPNs
Demographic and career satisfaction factors: In the unadjusted model, statistically significant variables are shown in Table 2. The adjusted odds logistic regression analysis of RPNs who intended to remain in their current position for the next 5 years suggested that age equal to or greater than 56 years of age (odds ratio (OR): 0.11; 95% confidence interval (CI): 0.04-0.32) was a statistically significant factor of ITS. Similarly, those respondents who had lived for between 27 and 37 years (OR: 3.14, 95% CI: 1.27-7.81) in NEO were also more likely to stay. Similarly, a statistically significant association was shown for those who lived in NEO between 37 and 48 (OR: 3.78, 95% CI: 1.17-12.2). No other variables were determined to be statistically significant with ITS (Table 2).
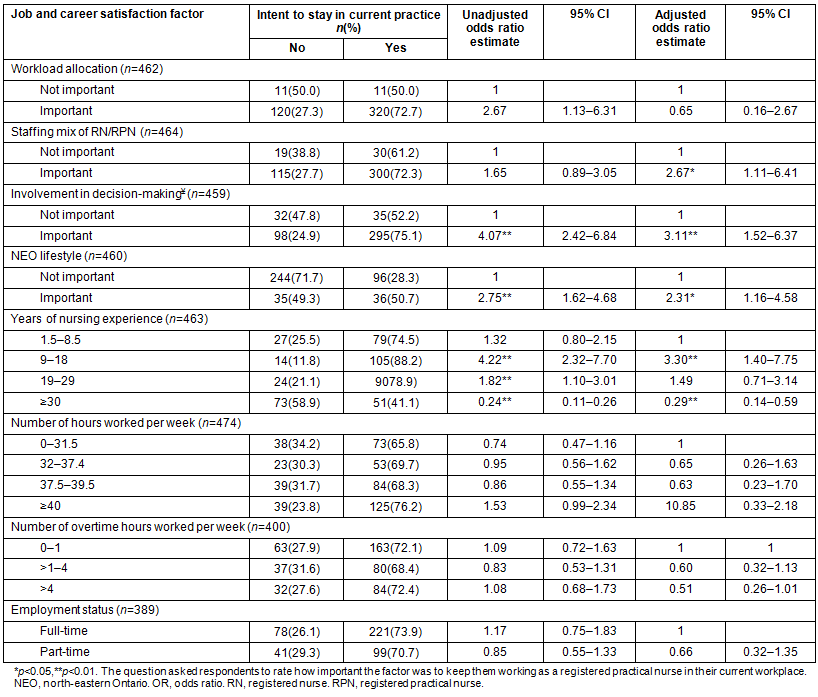
Occupation and career satisfaction factors: The unadjusted model findings are presented in Table 3. In the adjusted model, staffing ratios between RN and RPNs (OR: 2.61, 95% CI: 1.17-12.2), involvement in decision-making processes (OR: 3.11, 95% CI: 1.52-6.37), and the NEO lifestyle (OR: 2.31, 95% CI: 1.16-4.58) were statistically significant factors related to ITS. Furthermore, RPNs with between 9 and 18 years of work experience (OR: 3.30, 95% CI: 1.40-7.75) were more likely to stay while those with greater than 30 years (OR: 0.29, 95% CI: 0.14-0.59) were likely to leave their current position.
Table 3: Multivariable adjusted odds ratio estimates and approximate 95% confidence intervals
of job and career satisfaction factors associated with intent to stay of registered practical nurses
Discussion
What is already known about this topic
- In northern and rural settings such as northern Ontario, Canada, positive work environments are essential to the recruitment and retention of healthcare professionals.
- There is a global shortage of healthcare practitioners including registered practical nurses (RPNs) and the health human resources crisis will be exacerbated with an ageing workforce, rising rates of chronic diseases, and an increased demand on health services.
What this article adds
- The likeliness of RPNs' intent to stay (ITS) in their current position for the next 5 years was greater in the 46-56-years age group than among RPNs in the other age groups.
- The lifestyle of north-eastern Ontario, Canada, internal staff development, working in nursing for 14-22.5 years, and working less than 1 hour of overtime per week were factors associated with ITS.
- This provides preliminary evidence regarding retention factors related to ITS among RPNs in rural and northern regions.
The purpose of the present study was to examine factors related to retention of RPNs in NEO. Based on the nurses' demographics and the related factors model, the adjusted odds logistic regression analyses revealed that RPNs who had 9-18 years of work experience were more likely to stay in their present work settings than other nurses. Research indicates that, as age and years of experience increase, the desire to leave a position decreases23. The RPNs with greater than 30 years of work experience were more likely to leave current positions for various reasons including retirement24 and increasing workloads25,26. The findings of this study are, therefore, consistent with the existing literature.
The study also revealed that staffing proportions between RNs and RPNs, involvement in decision-making processes, and the NEO lifestyle were statistically significant factors related to ITS and retention rates of RPNs. Other studies have shown that staff allocation and increased decision-making capacity among rural nurses27,28 lead to higher job satisfaction29 and lower levels of work stress30.
The utilization of RPNs has moved from community and teaching hospitals into institutions such as nursing homes, retirement homes, and rehabilitation settings31. A more recent development is the employment of RPNs in home-based nursing services, including those administered through public health departments and visiting nursing organizations2,32.
There are several limitations to this study. The representativeness of participants is of potential concern. Although a simple random sampling strategy was used, the sample population was confined to NEO and cooperation by the participants is rarely perfect, which means that random sampling seldom results in random samples33. Therefore, the results may not be generalizable to other RPNs in other areas of Ontario. Nurses who had left the nursing profession were not reflected in the sample and may provide a different view of the relationship between retention and ITS than generated in the study. Selection bias may also have influenced the results. Size of the organization, size and location of the community, continuing education opportunities, organizational structure, and leadership are factors meriting investigation for their possible impact on the quality of work life and stress among nurses and, in return, the retention of nurses. Inherently, with every instrument, its psychometric properties need to be rigorously evaluated and this is a drawback of this study. However, retention is not consistently measured, making it difficult to interpret and compare. Therefore, empirical evidence demonstrating validity and reliability of existing indices, including the one used in this study, is warranted.
Research gaps continue to exist regarding the retention of nurses, and there is a need for large-scale and methodologically rigorous quantitative and qualitative investigations that examine the factors that influence rural nursing practice and retention. In NEO, the Northern Ontario School of Medicine, a rurally focused, community-based medical school that actively recruits students from Northern Ontario and other northern, rural, remote, Aboriginal, and Francophone backgrounds, has an important role to play in addressing these gaps34. This approach may be adopted by the schools of nursing in NEO in order to provide a workforce that is more inclined to live and work in the region. Addressing the challenges of health human resources in rural and northern communities requires examination of not only health professionals but also their spouses, access to leisure activities and the proximity of family and friends. The influence of rural background on personal and professional relationships and questions of work-life balance likewise require investigation. Through understanding what constitutes positive quality of work life as well as personal life, retention of RPNs in NEO and similar geographic regions may lead to enhanced retention of these important health professionals. Collaboration between academic health research centers, governments, and communities is recommended to achieve this goal.
References
1. Tourangeau AE, Coghlan AL, Shamian J, Evans S. Registered nurse and registered practical nurse evaluations of their hospital practice environments and their responses to these environments. Nursing Leadership 2005; 18(4): 54.
2. MacLeod MLP, Pitblado JR, Koren I, Stewart NJ, Kulig JC. Planning for the regulated nursing workforce in rural and small town Canada. Vancouver, BC: Annual CAHSPR Conference, 2013.
3. Canadian Institute for Health Information. Regulated nurses: Canadian trends, 2007 to 2011. Canadian Institute for Health Information, 2013.
4. Ministry of Finance - Ontario. Ontario population projections update. Toronto, ON: Queen's Printer for Ontario, 2012.
5. Ministry of Health and Long Term Care. Rural and northern health care framework. Toronto, ON: Ministry of Health and Long Term Care, Government of Ontario, Canada, 2011.
6. Hayes LJ, O'Brien-Pallas L, Duffield C, Shamian J, Buchan J, Hughes F, et al. Nurse turnover: a literature review - an update. International Journal of Nursing Studies 2012; 49(7): 887-905.
7. Vandewater D. Retirement and retention of late career nurses. Halifax, NS: College of Registered Nurses of Nova Scotia, 2005.
8. Murphy GT, MacKenzie A. Using evidence to meet population healthcare needs: successes and challenges. Healthcare Papers 2013; 13(2): 9-21.
9. North West Local Health Integration Network. Integrated health services plan. Thunder Bay, ON: North West Local Health Integration Network, 2013.
10. College of Nurses of Ontario. Membership statistics report. Toronto, ON: College of Nurses of Ontario, 2013.
11. Stewart NJ, D'Arcy C, Kosteniuk J, Andrews ME, Morgan D, Forbes D, et al. Moving on? Predictors of intent to leave among rural and remote RNs in Canada. Journal of Rural Health 2011; 27(1): 103-113.
12. Lea J, Cruickshank M. Factors that influence the recruitment and retention of graduate nurses in rural health care facilities. Collegian 2005; 12(2): 22-27.
13. Seago JA, Spetz J, Chapman S, Dyer W. POLICY perspectives: can the use of LPNs alleviate the nursing shortage?: Yes, the authors say, but the issues - involving recruitment, education, and scope of practice - are complex. American Journal of Nursing 2006; 106(7): 40-49.
14. College of Nurses of Ontario. Practice guidelines: utilization of RNs and RPNs. Toronto, ON: College of Nurses of Ontario, 2004.
15. Dillman DA. The design and administration of mail surveys. Annual Review of Sociology 1991; 17: 225-249.
16. Health Force Ontario. Nursing roles Toronto. ON: Queen's Printer For Ontario, 2014.
17. Ministry of Health and Long-Term Care. Local Health System Integration Act 2006. Frequently asked questions about LHINs. (Online) 2012. Available: http://www.health.gov.on.ca/english/public/legislation/lhins/lhins_faq.html#1 (Accessed 5 June 2012).
18. Rukholm E. Northeastern Ontario nursing recruitment and retention study. Sudbury, ON: Ministry of Health and Long-Term Care, 2005.
19. Andrews ME, Stewart NJ, Pitblado JR, Morgan DG, Forbes D, D'Arcy C. Registered nurses working alone in rural and remote Canada. Canadian Journal of Nursing Research 2005; 37(1): 14-33.
20. Stewart NJ, D'Arcy C, Pitblado JR, Morgan DG, Forbes D, Remus G, et al. A profile of registered nurses in rural and remote Canada. Canadian Journal of Nursing Research 2005; 37(1): 122-145.
21. Golubic R, Milosevic M, Knezevic B, Mustajbegovic J. Work-related stress, education and work ability among hospital nurses. Journal of Advanced Nursing 2009; 65: 2056-2066.
22. Gunnarsdottir S, Clarke SP, Rafferty AM, Nutbeam D. Front-line management, staffing and nurse-doctor relationships as predictors of nurse and patient outcomes. A survey of Icelandic hospital nurses. International Journal of Nursing Studies 2009; 46(7): 920-927.
23. O'Brien-Pallas L, Murphy GT, Shamian J, Li X, Hayes LJ. Impact and determinants of nurse turnover: a pan?Canadian study. Journal of Nursing Management 2010; 18(8): 1073-1086.
24. Wieck KL, Dols J, Landrum P (Eds). Retention priorities for the intergenerational nurse workforce. Nursing Forum; 2010: 45(1): 7-17.
25. Al-Kandari F, Thomas D. Adverse nurse outcomes: correlation to nurses' workload, staffing, and shift rotation in Kuwaiti hospitals. Applied Nursing Research 2008; 21(3): 139-146.
26. Sveinsdottir H, Biering P, Ramel A. Occupational stress, job satisfaction, and working environment among Icelandic nurses: a cross-sectional questionnaire survey. International Journal of Nursing Studies 2006; 43(7): 875-889.
27. Pinikahana J, Happell B. Stress, burnout and job satisfaction in rural psychiatric nurses: a Victorian study. Australian Journal of Rural Health 2004; 12(3): 120-125.
28. Albion MJ, Fogarty GJ, Machin MA. Benchmarking occupational stressors and strain levels for rural nurses and other health sector workers. Journal of Nursing Management 2005; 13(5): 411-418.
29. Hayes B, Douglas C, Bonner A. Work environment, job satisfaction, stress and burnout in haemodialysis nurses. Journal of Nursing Management 2013, doi: 10.1111/JONM.12184.
30. Lu H, Barriball KL, Zhang X, While AE. Job satisfaction among hospital nurses revisited: a systematic review. International journal of Nursing Studies 2012; 49(8): 1017-1038.
31. McGilton KS, Boscart VM, Brown M, Bowers B. Making tradeoffs between the reasons to leave and reasons to stay employed in long-term care homes: perspectives of licensed nursing staff. International Journal of Nursing Studies 2014; 51(6): 917-926.
32. Alameddine M, Laporte A, Baumann A, O'Brien-Pallas L, Croxford R, Mildon B, et al. Where are nurses working? Employment patterns by sub-sector in Ontario, Canada. Healthcare Policy 2006; 1(3): 65.
33. Polit DF, Beck CT. Generalization in quantitative and qualitative research: myths and strategies. International journal of Nursing Studies 2010; 47(11): 1451-1458.
34. Strasser R, Neusy AJ. Context counts: training health workers in and for rural and remote areas. Bulletin of the World Health Organization 2010; 88(10): 777-782.






