WHO recommends the practice of exclusive breastfeeding as an essential component of infant nourishment, which is defined as giving no food or liquid other than mother's breast milk during the first 6 months after birth1. However, after many years of continuous efforts by various government and non-government agencies across the world, approximately 1.3 million lives are lost annually because of inadequate exclusive breastfeeding2. In India, only 46.4% of children are exclusively breastfed and the country still struggles to achieve a reasonable level of optimal infant and child-feeding practices3.
Odisha state of India has recorded a high infant mortality rate (59 per 1000 live births)4,5. This figure is especially higher in rural Odisha (62) than in urban areas (41). Rural children in Odisha are also more likely to be undernourished than urban children with a total of around 41% of 0-5 year children being underweight3. Regardless of the universal breastfeeding norm, in Odisha incorrect and suboptimal breastfeeding practices are widespread. In the state, only 27% of infants receive exclusive breastfeeding for 6 months4,5. Further, pre-lacteal feeding after birth is a common practice in rural Odisha with about 42% of children being fed a liquid other than breast milk after birth3. The breastfeeding practices are further influenced by various cultural and community beliefs in rural regions6. Thus, it is essential to understand the factors underlying rural women's breastfeeding behaviour.
Previous researchers have identified maternal intention as an important determinant of breastfeeding behavior7-9. Further, prenatal intention has been emphasised by many authors as one of the strongest factors for breastfeeding intensity and duration10-13. In addition, a woman's clear vision about breastfeeding before pregnancy or during the early stage of pregnancy increases her likelihood of optimal breastfeeding14,15.
The framework of theory of planned behaviour has given insights into the effect of breastfeeding intention on the actual behaviour and related determinants10,16-18. The key factor in this theory is the intention of the individual to execute a behaviour that is determined by its three constructs - the individual's attitude towards that behaviour, subjective norms (perception of social pressure from significant others to perform a particular behaviour) in the society about that behaviour and the perceived control (perception of the ease or difficulty of performing a particular behaviour) to be able to practice that behaviour16,17. This theory has been used by numerous researchers on breastfeeding intention, who have found that the three constructs, attitude, subjective norm and perceived behavioural control, have significant effect on breastfeeding intention19-24.
Most researches on maternal breastfeeding intention have been conducted in developed countries11,13 with limited existing data from India and none from Odisha state. Moreover, only a few studies have specifically focused on prenatal intention for exclusive breastfeeding6,25,26 and rural women's breastfeeding intention has been much less examined. Thus, the aim of this study was to assess the exclusive breastfeeding intention of rural pregnant mothers in Odisha state of India and its relationship with their knowledge, attitude, subjective norm and perceived control for exclusive breastfeeding.
Study area
A cross-sectional survey was conducted between March and June 2012 in rural areas of Angul district of Odisha. This district was chosen because it had one of the lowest exclusive breastfeeding rates in the state. This selection was done with the aim of identifying possible predictors of low exclusive breastfeeding in Odisha. Only 11.1% children were exclusively breastfed for 6 months in Angul district, which is less than other rural areas (10.6%)27.
Odisha state has a majority of rural areas with an overall population density of 269 per square kilometre4,5 as compared to the defined limit for rural areas in India of 400 per square kilometre28. Angul district has an even lower population density of 200 per square kilometre27 with an estimated total population of 1.27 million, 84% of whom live in rural areas29. All four subdistricts in Angul district are denoted as rural except for two small urban municipalities Angul town and Talcher30. The average literacy rate is 77.5%29 while 52% live below the poverty line30. About 0.29 million women are within the age group of 15-49 years. Agriculture is the main occupation along with jobs in mining and other industries30.
Sampling
The sample for this study was selected from pregnant women living only in rural areas of Angul district, using a multi-stage sampling method. First, one subdistrict among a total of four subdistricts in Angul district was randomly chosen. In that subdistrict, there were three community health centres (CHCs) and under each CHC, there were more than one subcentre. Of those, one subcentre was randomly selected under each CHC. Then, a total of 283 registered pregnant women at these three selected subcentres were included in the study. Finally, data were collected from 218 pregnant women through face-to-face interviews. Sixty-five women could not be reached.
Data collection
A structured interview schedule was developed and field-tested for accuracy. This was used as the data collection tool. All questions were prepared in English, then translated to the local Odia language and pretested in a similar area. The content validity of the interview schedule was ensured through prior review by two medical doctors and two nurses working in the area as well as two public health specialists at Tata Institute of Social Sciences (TISS), Mumbai.
Measures
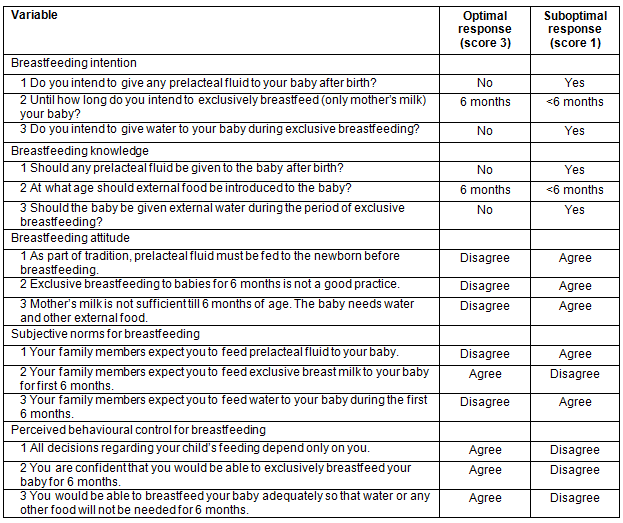
Data were collected about the respondent's intention, knowledge, attitude, subjective norm and perceived control about exclusive breastfeeding, together with details about their demographic and socio-economic status and questions about the breastfeeding education received from health personnel. Exclusive breastfeeding intention, knowledge, attitude, subjective norm and perceived control were measured using three questions each on a scale of 1-3. The highest score of 3 was given to optimal responses while the lowest score 1 was given to suboptimal responses. A middle score of 2 was assigned for responses as 'not sure' (Table 1).
Reliability analysis of the scales measurements were computed using Cronbach's alpha statistic, which was greater than 0.7 (intention 0.78, knowledge 0.83, attitude 0.71, subjective norm 0.73, perceive control 0.71). The overall index score for each of these variables was calculated by adding the scores of all questions for that variable. These variables (range 3-9) were further categorised into two groups. A total score of 9 was denoted as 'high', whereas any score from 3 to 8 was denoted as 'low'. This grouping criteria was used with a view of the importance of all three optimal responses (no pre-lacteal feeding, exclusive breastfeeding for 6 months and no feeding of water during exclusive breastfeeding) so as to ensure optimal exclusive breastfeeding.
Data analysis
Data were analyzed using Statistical Package for Social Sciences v18 (SPSS Inc; www.spss.com). Descriptive statistics included computation of means, frequencies and standard deviations (SD) for all variables. Sociodemographic factors affecting knowledge, attitude, subjective norm and perceived control for exclusive breastfeeding were examined through logistic regression tests. For this, respondent's age, education, caste category and receipt of breastfeeding education from health personnel were included as potential confounders in categorical form. All dependent variables were used as dichotomous variables with high (score of 9) and low (score of less than 9) categories.
In addition, logistic regression analysis was used to assess the associations between the respondent's knowledge, attitude, subjective norm and perceived control with their intention for exclusive breastfeeding. All variables were included dichotomous variables with high (score of 9) and low (score of less than 9) categories. Computation of odds ratios (ORs) and confidence intervals (CIs) were done and p<0.05 denoted statistical significance.
Table 1: Variable assessment scales, their optimal and suboptimal responses and assigned scores
Ethics approval
The study was approved by the Board of Research Studies, School of Health System Studies, Tata Institute of Social Sciences (TISS), Mumbai. Written informed consent prepared in Odia language was taken from all respondents for maintenance of anonymity and the confidentiality.
The mean age of sampled pregnant women was 23.6 years (SD 3.4; range 18-35 years). About 56% of women had previously given birth and 79% were in their second or third trimester of pregnancy. The respondents had a mean of 6.14 years of education with about 24.3% being illiterate. One-third of the women had a per-capita monthly income of less than US$15 (median US$20). The average family size was 5.8 (SD 2.62). A majority of interviewed women belonged to other backward castes (OBCs) followed by scheduled castes (SCs) and scheduled tribes (STs). Breastfeeding education was reported to be received by 67% of respondents from the health personnel working in that area (Table 2).
There were 65 (29.8%) women who reported having high intention for exclusive breastfeeding, which includes a combination of intention for no prelacteal fluid, only mother's milk without any water or other food for first 6 months. Older women (48.1%) had higher exclusive breastfeeding intention than younger women (21.7%; p<0.05) and literate women (32.2%) had higher intention than illiterate women (22.4%; p<0.05). Respondents belonging to backward castes (OBCs 41.4%, SCs 27.3%, STs 25.8%) reported stronger intention than general caste women (8.8%; p<0.05). Those women (18.1%) who had received breastfeeding education from health personnel possessed higher intention than those who had not (35.6%; p<0.05) (Table 2).
The mean score for breastfeeding knowledge was 6.7 (SD 1.6), mean attitude score was 7.0 (SD 1.8), mean subjective norm score was 7.2 (SD 1.5) and mean perceived control score was 7.1 (SD 1.7). Age of respondents had a positive association with knowledge, subjective norm and perceived control but not with attitude. Literacy status was positively associated with only knowledge whereas OBC women had significantly higher breastfeeding knowledge and more supportive subjective norm for exclusive breastfeeding than general caste women. Breastfeeding education had a significant positive relationship with knowledge, attitude, subjective norm and perceived control. Furthermore, higher age, being literate, lower caste category and receipt of breastfeeding education from health personnel had a significant relationship with exclusive breastfeeding intention (Table 3).
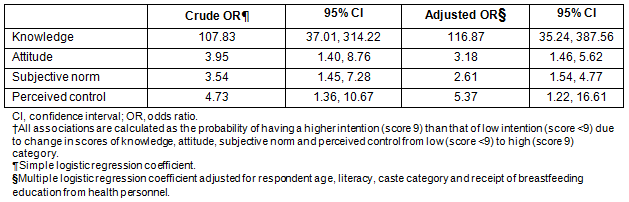
Higher breastfeeding knowledge was found to be significantly associated (OR 5.84; 95% CI 3.62, 9.42) with stronger exclusive breastfeeding intention. Similarly, positive attitude towards exclusive breastfeeding (OR 2.99; 95% CI 1.53, 6.17), supportive subjective norm (OR 1.45; 95% CI 1.09, 3.94) and greater perceived control (OR 1.39; 95% CI 1.03, 2.89) had a significant effect on the respondent's higher intention for exclusive breastfeeding. These associations appeared to be unaffected after adjusting for respondent age, literacy, caste category and receipt of breastfeeding education from health personnel (Table 4).
Table 2: Sociodemographic information about study respondents, by their exclusive breastfeeding intention
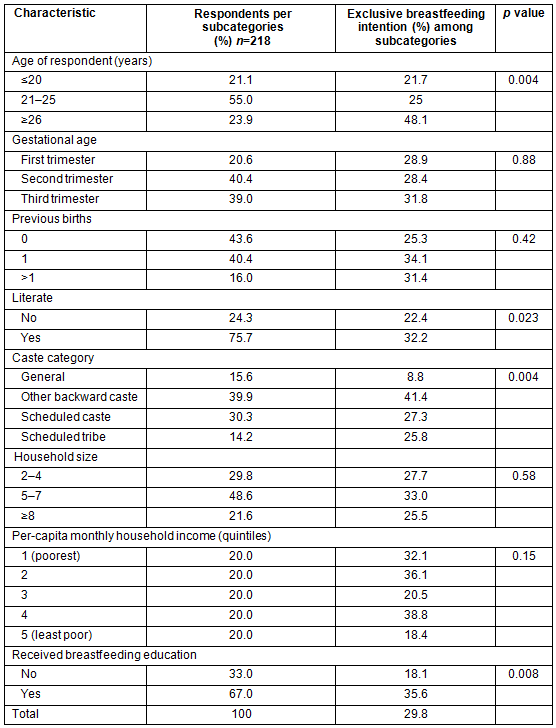
Table 3: Sociodemographic predictors of exclusive breastfeeding knowledge, attitude,
subjective norm, perceived control and intention of 218 pregnant women in Angul district of Odisha, India
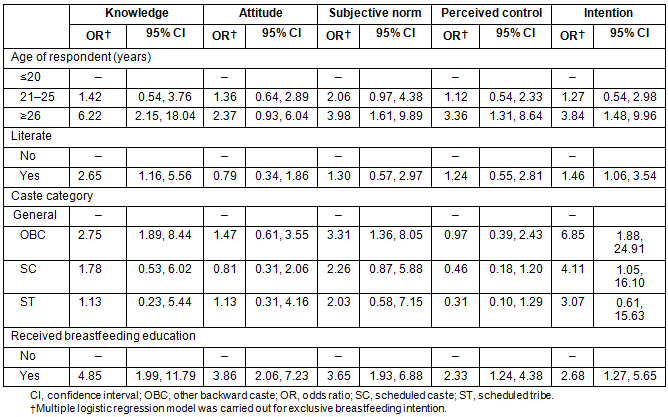
Table 4: Associations between exclusive breastfeeding intention of respondents and their knowledge, attitude,
subjective norm and perceived control.?
Discussion
Despite continuous efforts to address the pressing challenge of malnutrition and premature deaths among rural Indian children in the form of various health and nutrition programs, optimal exclusive breastfeeding rates have not been achieved yet3. With a high level of infant mortality and under-nutrition status in rural Odisha3, a persisting low exclusive breastfeeding rate further exacerbates the situation. The present study found that only a small percentage (29.8%) of pregnant women in rural Odisha possessed a strong intention for exclusive breastfeeding for 6 months. Further, it also indicated that feeding prelacteal fluid at birth and water or other liquid and solid diet during the first 6 months is commonly intended in Odisha, which is consistent with the previously identified norm among rural Odia society3. In addition, most previous studies conducted on exclusive breastfeeding intention were carried out in developed countries; not many studies have been made in rural India. Thus, the findings of this study would result in better understanding about rural Indian women's breastfeeding intention so that appropriate intervention strategies can be designed to achieve optimal exclusive breastfeeding rates.
This study demonstrated that older women had a stronger intention for exclusive breastfeeding possibly because of better knowledge and higher perceived control. Similarly, women belonging to lower castes had a higher breastfeeding intention, which is similar to the findings of other studies in India31,32. Higher receipt of breastfeeding education from health personnel could be a possible reason for this. Odisha's Village Health and Nutrition Days (VHND) participation statistics suggested that higher percentages of OBC, SC and ST than general caste women attend the VHND sessions, which are organised every month to spread awareness about health and nutrition, including optimal breastfeeding guidelines33.
Moreover, these research findings supported the interrelationships between the constructs of theory of planned behavior, which hypothesises that exclusive breastfeeding intention is affected by the attitude, subjective norm and perceived behavioural control for exclusive breastfeeding. The positive association of breastfeeding knowledge and attitude with exclusive breastfeeding intention in the current study is consistent with the findings of other studies20,34-36. Further, this study identified that support extended by significant others as well as perceived control among mothers had a huge influence on breastfeeding intention20,21,24,35. Therefore, efforts must be made to create a supportive environment in the family and community to enhance exclusive breastfeeding behaviour among rural mothers.
The effectiveness of structured counselling sessions on exclusive breastfeeding practice is well known37,38. The findings of the current study also supported this point, which revealed that breastfeeding education from health personnel such as medical staff and community health workers potentially contributed to a higher exclusive breastfeeding intention, as well as respondent's knowledge, attitude and subjective norm towards breastfeeding. This argues that more rigorous educational mechanisms on optimal breastfeeding benefits during prenatal stages can be useful to promote knowledge and intention of pregnant women towards exclusive breastfeeding.
However, the study respondents who received breastfeeding education demonstrated a lower level of perceived control. Incorporating motivational elements into breastfeeding education sessions could be used to boost the ability and confidence of women to take correct decisions about feeding their baby and practising them. Previously, motivational interviewing techniques have been successfully used to produce higher breastfeeding self-efficacy21,39. Therefore, instead of imparting only information about correct breastfeeding practice, trained health workers may be engaged to persuade women for optimal exclusive breastfeeding behaviour.
This study implies that inadequate knowledge, restrictive attitude, faulty norms and weak perceived control are the major predictors of a low intention for exclusive breastfeeding among pregnant women in rural Odisha. Educational interventions focusing on the importance of exclusive breastfeeding could be stressed by all levels of health personnel in order to attain universal exclusive breastfeeding intention and practice in rural areas. Considering greater bonding and dependence in rural societies, inclusion of husbands and important family members of pregnant women during educational sessions could be crucial to eradicate restrictive societal attitudes and faulty norms related to exclusive breastfeeding.
Limitations
This study's results may have overestimated the level of breastfeeding intention due to potential social desirability bias as the data were collected from the respondents through face-to-face interviews. However, the data collection tool was designed with a mix of direct and reverse questions so as to reveal accurate information.
Acknowledgements
The authors thank the Chief District Medical Officer of Angul district and the community health workers of the study area for their kind cooperation and support during the data collection process. The authors also gratefully acknowledge the contribution of all the participating pregnant women in this study.
References
1. WHO. Exclusive breastfeeding for six months best for babies everywhere. (Online) 2011. Available: http://www.who.int/mediacentre/news/statements/2011/breastfeeding_20110115/en/ (Accessed 5 December 2014).
2. 2. UNICEF. Nutrition - what are the challenges? (Online) 2003. Available: http://www.unicef.org/nutrition/index_challenges.html (Accessed 5 December 2014).
3. International Institute for Population Sciences and Macro International. National Family Health Survey (NFHS-3), 2005-06: Orissa, Mumbai: IIPS, 2007.
4. Registrar General and Census Commissioner of India. Annual health survey 2011-12. (Online) Available: http://www.censusindia.gov.in/vital_statistics/AHSBulletins/AHS_Factsheets_2011_12/OdishaFactsheet_2011-12.pdf (Accessed 5 December 2014).
5. Registrar General and Census Commissioner of India. Orissa population census data 2011. Census 2011. (Online) 2011. Available: http://www.census2011.co.in/census/state/orissa.html (Accessed 2 February 2015).
6. Bandyopadhyay M. Impact of ritual pollution on lactation and breastfeeding practices in rural West Bengal, India. International Breastfeeding Journal 2009; 4(2): 1-8.
7. Bai Y, Middlestadt SE, Peng CY, Fly AD. Predictors of continuation of exclusive breastfeeding for the first six months of life. Journal of Human Lactation 2010; 26(1): 26-34.
8. Forster DA, McLachlan HL, Lumley J. Factors associated with breastfeeding at six months postpartum in a group of Australian women. International Breastfeeding Journal 2006; 1(18): 1-12.
9. Shi L, Zhang J, Wang Y, Guyer B. Breastfeeding in rural China: association between knowledge, attitudes, and practices. Journal of Human Lactation 2008; 24(4): 377-385.
10. Dodgson JE, Henly SJ, Duckett L, Tarrant M. Theory of planned behaviour-based models for breastfeeding duration among Hong Kong mothers. Nursing Research 2003; 52(3): 148-158.
11. DiGirolamo A, Thompson N, Martorell R, Fein S, Grummer-Strawn L. Intention or experience? Predictors of continued breastfeeding. Health Education and Behaviour 2005; 32: 208-226.
12. Scott JA, Binns CW, Oddy WH, Graham KI. Predictors of breastfeeding duration: evidence from a cohort study. Paediatrics 2006; 117(4): e646-655
13. Swanson V, Power KG. Initiation and continuation of breastfeeding: theory of planned behaviour. Journal of Advanced Nursing 2005; 50(3): 272-282.
14. Buxton KE, Gielen AC, Faden RR, Brown CH, Paige DM, Chwalow AJ. Women intending to breastfeed: predictors of early infant feeding experiences. American Journal of Preventive Medicine 1991; 7(2): 101-106.
15. Hood LJ, Faed JA, Silva PA, Buckfield PM. Breast feeding and some reasons for electing to wean the infant: a report from the Dunedin multidisciplinary child development study. New Zealand Medical Journal 1978; 88(621): 273-276.
16. Ajzen I. The theory of planned behavior. Organizational Behavior and Human Decision Processes 1991; 50: 179-211.
17. Ajzen I and Fishbein M. Understanding attitudes and predicting social behaviour. Englewood Cliffs NJ: Prentice-Hall, 1980.
18. Wambach KA. Breastfeeding intention and outcome: A test of the theory of planned behaviour. Research in Nursing & Health 1997; 20(1): 51-59.
19. Al-Akour NA, Khassawneh MY, Khader YS, Ababneh AA, Haddad AM. Factors affecting intention to breastfeed among Syrian and Jordanian mothers: a comparative cross-sectional study. International Breastfeeding Journal 2010; 5(6): doi: 10.1186/1746-4358-5-6
20. Kools EJ, Thijs C, de Vries H. The behavioral determinants of breast-feeding in the Netherlands: predictors for the initiation of breast-feeding. Health Education and Behaviour 2005; 32(6): 809-824.
21. Meedya S, Fahy K, Kable A. Factors that positively influence breastfeeding duration to 6 months: a literature review. Women and Birth 2010; 23(4): 135-145.
22. Persad MD, Mensinger JL. Maternal breastfeeding attitudes: association with breastfeeding intent and socio-demographics among urban primiparas. Journal of Community Health 2008; 33(2): 53-60.
23. Rempel LA. Factors influencing the breastfeeding decisions of long-term breastfeeders. Journal of Human Lactation 2004; 20(3): 306-318.
24. Swanson V, Power KG. Initiation and continuation of breastfeeding: theory of planned behaviour. Journal of Advanced Nursing 2005; 50(3): 272-282.
25. Nommsen-Rivers LA, Chantry CJ, Cohen RJ, Dewey KG. Comfort with the idea of formula feeding helps explain ethnic disparity in breastfeeding intentions among expectant first-time mothers. Breastfeeding Medicine 2010; 5(1): 25-33.
26. Stuebe AM, Bonuck K. What predicts intent to breastfeed exclusively? Breastfeeding knowledge, attitudes and beliefs in a diverse urban population. Breastfeeding Medicine 2011; 6(6): 413-420.
27. Registrar General and Census Commissioner of India. Anugul (Angul) district: census 2011 data. Census 2011. (Online) 2011. Available: http://www.census2011.co.in/census/district/408-anugul.html (Accessed 05 March 2015).
28. Registrar General and Census Commissioner of India. Rural urban distribution of population (provisional population totals). Census 2011 (Online) 2011. Available: http://censusindia.gov.in/2011-prov-results/paper2/data_files/india/Rural_Urban_2011.pdf (Accessed 2 February 2015).
29. Registrar General and Census Commissioner of India. Annual health survey 2010-11. (Online) 2011. Available: http://www.censusindia.gov.in/vital_statistics/AHSBulletins/AHS_Baseline_Factsheets/Odisha1.pdf (Accessed 5 December 2014).
30. District Administration, Angul. District background and profile. In: Comprehensive district Plan 2011-12. (Online). Available: http://angul.nic.in/distplan.htm (Accessed 5 December 2014).
31. Meshram II, Laxmaiah A, Venkaiah K, Brahmam GNV. Impact of feeding and breastfeeding practices on the nutritional status of infants in a district of Andhra Pradesh, India. National Medical Journal of India 2012; 25(4): 201-206.
32. Singh R, Bedi S, Mishra RN, Mishra CP, Singh A. Caste still a determinant of MCH care in India. Indian Journal of Preventive and Social Medicine 2013; 44(1-2): 75-81.
33. Department of Health & Family Welfare and Department of Women & Child Development, Government of Orissa. VHND assessment conducted in six districts, quality indicators developed and discussed with DoH&FW & DWCD. (Online) 2011. Available: http://www.nrhmorissa.gov.in/writereaddata/Upload/Documents/VHND%20Assessment%20Conducted%20In%20Six%20Districts,%20Quality.pdf (Accessed 28 May 2015).
34. Cernadas JM, Noceda G, Barreara L, Martinez AM, Garsd A. Maternal and perinatal factors influencing the duration of exclusive breastfeeding during the first 6 months of life. Journal of Human Lactation 2003; 19(2): 136-144.
35. Lundberg PC, Ngoc Thu TT. Breast-feeding attitudes and practices among Vietnamese mothers in Ho Chi Minh City. Midwifery 2012; 28(2): 252-257.
36. O'Brien M, Buikstra E, Fallon T, Hegney D. Exploring the influence of psychological factors on breastfeeding duration, phase 1: perceptions of mothers and clinicians. Journal of Human Lactation 2009; 25(1): 55-63.
37. Anderson AK, Damio G, Young S, Chapman DJ, Pérez-Escamilla R. A randomized trial assessing the efficacy of peer counselling on exclusive breastfeeding in a predominantly Latina low-income community. Archives of Paediatrics and Adolescent Medicine 2005; 159(9): 836-841.
38. Haider R, Ashworth A, Kabir I, Huttly SR. Effect of community-based peer counsellors on exclusive breastfeeding practices in Dhaka, Bangladesh: a randomised controlled trial. The Lancet 2000; 356(9242): 1643-1647.
39. Wilhelm SL, Stepans MB, Hertzog M, Rodehorst TK, Gardner P. Motivational interviewing to promote sustained breastfeeding. Journal of Obstetric, Gynecologic, and Neonatal Nursing 2006; 35(3): 340-348.
