Low-trauma, osteoporotic fractures among older men are associated with a two-fold increase in mortality; in particular, hip fractures are associated with a 1-year mortality of 30%1-3. Low-trauma fractures are also associated with decreased mobility, increased pain and functional limitations, increased risk of institutionalization, as well as an increased risk for subsequent fractures4-10. Treatment for osteoporosis has been shown to greatly reduce the risk of subsequent fractures and significantly reduce the risk in mortality11-13.
Despite effective therapies for osteoporosis, several studies have demonstrated that management and treatment after a low-trauma fracture remain inadequate, especially among men14-17. In 2010, the Veterans Affairs Office of the Inspector General reviewed osteoporosis care among veterans with low-trauma fracture and found that only 24% received appropriate care18. System-wide quality improvement interventions were advocated including provider education, patient education, and improved surveillance components.
While fracture liaison services have been shown to significantly improve osteoporosis treatment19-21, they frequently rely on local availability of a specialty team with expertise in metabolic bone disease. Such a service may be less feasible for medical centers, such as the Veterans Affairs Health Administration, which cares for a large number of patients living in rural areas. Substantial disparities in the availability and quality of medical care have been described for rural patients, who are on average 5 years older than urban patients and therefore have a higher burden of age-related chronic diseases such as osteoporosis22,23. Therefore, comparing the reach and impact of models such as fracture liaison services in rural patients is an important goal.
The post-fracture electronic consult (e-consult) program at a single, centralized Veterans Administration Medical Center (VAMC), and the program's effects on osteoporosis screening and treatment rates, has been previously described24. In the present study, the authors sought to determine the geographic scope of the e-consult program and its impact on rural patients in this region, wherein over 43% of the veterans live in rural or highly rural areas.
The Osteoporosis E-consult program has been described previously24,25. Patients with recent fracture were identified by a central data warehouse report using fracture-related International Classification of Disease (ICD9) codes (733.93-733.95; 767.3; 800-829; V54.13). The program coordinating staff then completed an electronic medical record screening at the central coordinating VAMC. Eligibility for the e-consult program including patients aged more than 50 years, who had sustained a low-trauma fracture within the previous 12 months, and who had a primary care provider within the VAMC. Patients were excluded for fractures not considered osteoporotic (eg facial, skull, or digital fracture) and for fractures that occurred more than 10 years prior. Patients with an active prescription for a bisphosphonate, a recent bone mineral density (BMD) test, or an estimated life expectancy of 1 year or less were also excluded. Patients with medical record documentation noting that the patient had been offered but had declined osteoporosis screening or therapy were not included. Patients who had died after the index fracture but prior to medical record screening by the e-consult coordinating staff were not included.
After screening by the e-consult coordinating staff, patients were referred to a metabolic bone specialist , a physician with training in endocrinology and/or geriatric medicine, for chart review. Medical chart review included identification of other clinical risk factors for osteoporosis, for example low body mass index, hyperparathyroidism, and rheumatoid arthritis. The physician also review prior laboratory results, such as serum chemistries and vitamin D levels, and prior medical treatments, such as corticosteroid use and androgen-deprivation therapy. The physician then provided a consult note with recommendations regarding osteoporosis screening (eg bone density assessment) and possible osteoporosis treatment based on current clinical practice guidelines from the National Osteoporosis Foundation and the VA18,26. The consult note was then sent to the patient's primary care provider (PCP) via the electronic medical record for review.
Starting in October 2013, a bone health nurse liaison, located at the central VAMC, coordinated the evaluation and management plans for PCP-reviewed recommendations, including ordering and follow-up of laboratory and bone density assessment, osteoporosis education (eg medication administration and side effects, calcium and vitamin D supplementation, falls prevention, and exercise), and adherence follow-up via telephone. Initially, the nurse liaison only served clinics associated with the central VAMC, and then in January 2014 expanded to include the additional two nearest VAMCs, while the remaining two VAMCs did not receive nurse services. Thus, the effect of the nurse liaison service could be assessed. Nurse liaison services were provided to both urban and rural patients at the associated VAMCs.
Statistical analysis
Patients were identified as living in a rural area if their ZIP code was not in a US Census Bureau-defined urban area, population density greater than approximately 386 persons per square kilometer (1000 persons per square mile). Baseline characteristics for the patients are described using frequencies and percentages for categorical variables and means with standard deviations for continuous variables. To compare rural and urban subjects, student's t-test was used for continuous variables and χ2 or Fisher's exact tests for categorical variables. Expected numbers were based on VA regional enrollment data from the 2013 financial year and the relative proportion of rural/highly rural enrollees. Statistical significance was assessed for p<0.05. Maps were based on the ZIP code tabulation areas obtained from the US Census Bureau. Total travel distance saved was based on distance from veteran's home address to the nearest VA primary care clinic. Analyses were performed using Statistical Analysis Software v9.3 (SAS; http://www.sas.com). This study was approved by the Institutional Review Board at the Durham VAMC (#01653).
Study population
From October 2013 to September 2014, there were 2775 fractures identified by a fracture-related ICD9 code (Fig1). Of these, 1381 individuals were automatically excluded from e-consult due to ineligibility. The most common reason was because the veteran was younger than 50 years. An additional 1073 individuals were excluded during the chart extraction phase. The most common reason for exclusion during chart extraction was because the fracture occurred due to high trauma. Therefore, 321 unique individuals with fractures were subsequently reviewed by a metabolic bone specialist, of which 171 occurred in rural veterans.
Baseline patient characteristics are presented in Table 1. Veterans were predominantly male (94.7%) with a mean age of 70.5±10.6 years. Common medical comorbidities included diabetes mellitus and chronic lung disease. The most common fracture sites were of the lower leg (24.7%) and of the hip/pelvis (21.9%). Demographics, medical comorbidities, or fracture site were not significantly different between the rural and urban veterans.
Figure 2 shows the geographic distribution of e-consults during the study period. The total travel distance saved for rural veterans who were managed with e-consult, assuming that one visit to the healthcare center was avoided for each veteran, was 19 178 km (11 917 miles), or 112.2 km (69.7 miles) per person. Based on enrollment demographics within the VAMC, there was a trend toward more rural patients receiving e-consults (171 completed vs 149 expected). However, this was not statistically significant (p=0.52). Within the rural cohort, bisphosphonates were recommended 51 times, with 33 (64.7%) ordered, compared to 50 recommended and 25 (50.0%) ordered within the urban cohort (p=0.13). Within the rural cohort BMD was recommended 109 times with 79 (72.5%) ordered, compared to 88 recommended and 64 (72.3%) ordered within the urban cohort. For both rural and urban cohorts, an in-person endocrine-bone consultation was recommended for 6.4% and 6.0%, respectively, due to medical complexity.
The bone health nurse liaison services began in October 2013 at the central VAMC and then expanded to two additional facilities starting in January 2014. During the study period, 118 individuals were followed by the bone health nurse liaison, of which 71 resided in a rural area (Table 2). In these patients, bisphosphonates were ordered in 75.8% of patients for whom treatment was recommended, compared to 39.7% of patients without nurse liaison involvement (p<0.01). With regards to BMD assessment, testing was completed in 63.0% of patients followed by the nurse liaison, compared to 37.1% of those not followed by the nurse liaison (p<0.01). There was no significant difference in the effect of the nurse liaison between rural and urban veterans (p=0.57 for bisphosphonate prescriptions, p=0.20 for BMD testing).
Table 1: Baseline characteristics of veterans with an e-consult
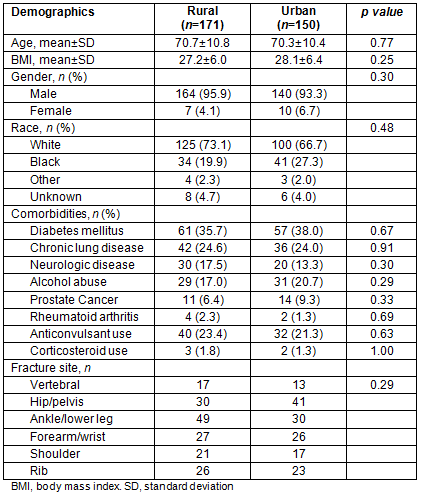
Table 2: Characteristics of veterans with an e-consult by involvement of bone health nurse liaison
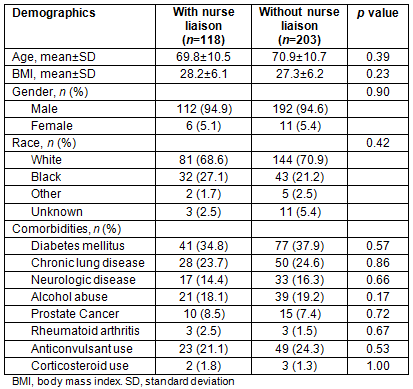
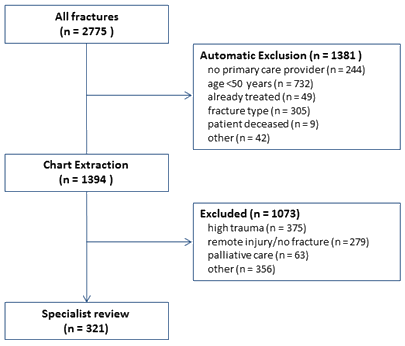
Figure 1: The e-consult referral process.
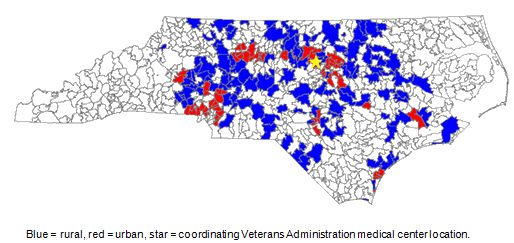
Figure 2: Geographic distribution of veterans with e-consults by ZIP code tabulation area.
Discussion
Prior to the program start, testing and treatment rates in the participating VAMCs were <20%24. The authors had previously shown the effectiveness of an E-consult program on osteoporosis management. However, inclusion of a bone health nurse liaison to coordinate care and provide patient education significantly improved the rate of osteoporosis evaluation and treatment among Veterans with a recent low-trauma fracture, beyond the E-consult program to the primary care provider alone. The program was able to save a substantial number of travel miles for rural patients. Despite differences in local access to BMD testing, which was available exclusively within the urban VAMC during the study period, there were no differences in rates of BMD testing or bisphosphonate prescriptions between rural and urban patients.
Fracture liaison services have been demonstrated to significantly improve osteoporosis screening and treatment rates and are also cost-effective, sometimes cost-saving, programs21,27-29. However, such programs may be inefficient or relatively more costly for small medical centers with lower fracture volumes. Moreover, osteoporosis testing and treatment decisions may be more complex in men or patients with multiple comorbidities, requiring subspecialty physician input, which may not be available in rural locales1,30. The current e-consult service, a centralized fracture liaison service, with surveillance of regional medical centers and affiliated outpatient clinics, may be an effective strategy for healthcare systems where there are multiple centers with variable fracture volumes and complex patient characteristics. The service can also increase access in areas with more limited availability to subspecialty physician consultation and nurse education.
The limitations of the e-consult service should be considered. The surveillance and patient identification process depends on accurate and consistent coding of fractures by clinicians. Although fracture identification using administrative databases has been validated31,32, it has not been in the VA setting. Moreover, rural patients may be more likely to seek care for fractures in non-VA local emergency departments and therefore not be identified through VA clinical data. While the authors likely missed some fracture patients who received care outside the VA system, it is reassuring that this e-consult service had a greater-than-expected proportion of fracture patients who were rural. The VA Health Administration has a well-established network of community-based outpatient clinics affiliated with regional medical centers, along with its integrated electronic health record. Thus, aspects of the current e-consult program may be unique to the VA system. However, given the increasing integration of health systems in the US and increasing use of electronic health records, the current e-consult program may serve as a model for a feasible, centralized service to increase access to specialized medical care.
A centralized e-consult program with a bone health nurse liaison can efficiently provide specialty bone health services to patients residing in both rural and urban areas and substantially increase the assessment and management of veterans with previously untreated osteoporosis. Further program improvements will include an assessment of the impact on long-term medication adherence and the development and integration of a falls prevention program delivered via bone health nurse liaison.
Acknowledgements
This work was supported by Project Award #N06-FY14Q1-S1-P01167 from the United States Department of Veterans Affairs, Office of Rural Health. RHL, KWL and CCE acknowledge support from the Duke Claude D. Pepper OAIC (P30AG028716-08). RHL acknowledges support from the NIH/NIA GEMSSTAR (R03AG048119-02).
References
1. Bass E, French DD, Bradham DD, Rubenstein LZ. Risk-adjusted mortality rates of elderly veterans with hip fractures. Annals of Epidemiology 2007; 17(7): 514-519.
2. Bliuc D, Nguyen ND, Milch VE, Nguyen TV, Eisman JA, Center JR. Mortality risk associated with low-trauma osteoporotic fracture and subsequent fracture in men and women. Journal of the American Medical Association 2009; 301(5): 513-521.
3. Trombetti A, Herrmann F, Hoffmeyer P, Schurch MA, Bonjour JP, Rizzoli R. Survival and potential years of life lost after hip fracture in men and age-matched women. Osteoporosis International 2002; 13(9): 731-737.
4. Cree M, Soskolne CL, Belseck E, Hornig J, McElhaney JE, Bryant R, et al. Mortality and institutionalization following hip fracture. Journal of the American Geriatrics Society 2000; 48(3): 283-288.
5. Scane AC, Francis RM, Sutcliffe AM, Francis MJ, Rawlings DJ, Chapple CL. Case-control study of the pathogenesis and sequelae of symptomatic vertebral fractures in men. Osteoporosis International 1999; 9(1): 91-97.
6. Burger H, Van Daele PL, Grashuis K, Hofman A, Grobbee DE, Schütte HE, et al. Vertebral deformities and functional impairment in men and women. Journal of Bone and Mineral Research 1997; 12(1): 152-157.
7. Matthis C, Weber U, O'Neill TW, Raspe H. Health impact associated with vertebral deformities: results from the European Vertebral Osteoporosis Study (EVOS). Osteoporosis International 1998; 8(4): 364-372.
8. Sanders KM, Nicholson GC, Ugoni AM, Pasco JA, Seeman E, Kotowicz MA. Health burden of hip and other fractures in Australia beyond 2000. Projections based on the Geelong Osteoporosis Study. Medical Journal of Australia 1999; 170(10): 467-470.
9. Colon-Emeric C, Kuchibhatla M, Pieper C, Hawkes W, Fredman L, Magaziner J, et al. The contribution of hip fracture to risk of subsequent fractures: data from two longitudinal studies. Osteoporosis International 2003; 14(11): 879-883.
10. Klotzbuecher CM, Ross PD, Landsman PB, Abbott TA, 3rd, Berger M. Patients with prior fractures have an increased risk of future fractures: a summary of the literature and statistical synthesis. Journal of Bone and Mineral Research 2000; 15(4): 721-739.
11. Lyles KW, Colon-Emeric CS, Magaziner JS, Adachi JD, Pieper CF, Mautalen C, et al. Zoledronic acid and clinical fractures and mortality after hip fracture. New England Journal of Medicine 2007; 357(18): 1799-1809.
12. Beaupre LA, Morrish DW, Hanley DA, Maksymowych WP, Bell NR, Juby AG, et al. Oral bisphosphonates are associated with reduced mortality after hip fracture. Osteoporosis International 2011; 22(3): 983-991.
13. Center JR, Bliuc D, Nguyen ND, Nguyen TV, Eisman JA. Osteoporosis medication and reduced mortality risk in elderly women and men. Journal of Clinical Endocrinology and Metabolism 2011; 96(4): 1006-1014.
14. Ganda K, Puech M, Chen JS, Speerin R, Bleasel J, Center JR, et al. Models of care for the secondary prevention of osteoporotic fractures: a systematic review and meta-analysis. Osteoporosis International 2013; 24(2): 393-406.
15. Giangregorio L, Papaioannou A, Cranney A, Zytaruk N, Adachi JD. Fragility fractures and the osteoporosis care gap: an international phenomenon. Seminars in Arthritis and Rheumatism 2006; 35(5): 293-305.
16. Elliot-Gibson V, Bogoch ER, Jamal SA, Beaton DE. Practice patterns in the diagnosis and treatment of osteoporosis after a fragility fracture: a systematic review. Osteoporosis International 2004; 15(10): 767-778.
17. Feldstein AC, Nichols G, Orwoll E, Elmer PJ, Smith DH, Herson M, et al. The near absence of osteoporosis treatment in older men with fractures. Osteoporosis International 2005; 16(8): 953-962.
18. Department of Veterans Affairs, Office of the Inspector General. Management of osteoporosis in veterans with fractures. Washington, DC: VA Office of the Inspector General, 2010.
19. McLellan AR, Gallacher SJ, Fraser M, McQuillian C. The fracture liaison service: success of a program for the evaluation and management of patients with osteoporotic fracture. Osteoporosis International 2003; 14(12): 1028-1034.
20. Dell R, Greene D, Schelkun SR, Williams K. Osteoporosis disease management: the role of the orthopaedic surgeon. The Journal of Bone and Joint Surgery, American volume. 2008; 90 Suppl 4: 188-194.
21. Eisman JA, Bogoch ER, Dell R, Harrington JT, McKinney RE, Jr, McLellan A, et al. Making the first fracture the last fracture: ASBMR task force report on secondary fracture prevention. Journal of Bone and Mineral Research 2012; 27(10): 2039-2046.
22. Gamm L, Hutchison L, Bellamy G, Dabney BJ. Rural healthy people 2010: identifying rural health priorities and models for practice. Journal of Rural Health 2002; 18(1): 9-14.
23. Larson SL, Fleishman JA. Rural-urban differences in usual source of care and ambulatory service use: analyses of national data using Urban Influence Codes. Medical Care 2003; 41(7 Suppl): III65-III74.
24. Lee RH, Lyles KW, Pearson M, Barnard K, Colon-Emeric C. Osteoporosis screening and treatment among veterans with recent fracture after implementation of an electronic consult service. Calcified Tissue International 2014; 94(6): 659-664.
25. Colon-Emeric C, Lee R, Barnard K, Pearson M, Lyles KW. Use of regional clinical data to identify veterans for a multi-center osteoporosis electronic consult quality improvement intervention. Journal of Hospital Administration 2013; 2(1): 8-14.
26. National Osteoporosis Foundation. Clinician's guide to prevention and treatment of osteoporosis. Washington, DC: National Osteoporosis Foundation, 2014.
27. Marsh D, Akesson K, Beaton DE, Bogoch ER, Boonen S, Brandi ML, et al. Coordinator-based systems for secondary prevention in fragility fracture patients. Osteoporosis International 2011; 22(7): 2051-2065.
28. Akesson K, Marsh D, Mitchell PJ, McLellan AR, Stenmark J, Pierroz DD, et al. Capture the fracture: a best practice framework and global campaign to break the fragility fracture cycle. Osteoporosis International 2013; 24(8): 2135-2152.
29. McLellan AR, Wolowacz SE, Zimovetz EA, Beard SM, Lock S, McCrink L, et al. Fracture liaison services for the evaluation and management of patients with osteoporotic fracture: a cost-effectiveness evaluation based on data collected over 8 years of service provision. Osteoporosis International 2011; 22(7): 2083-2098.
30. Khosla S, Amin S, Orwoll E. Osteoporosis in men. Endocrine Reviews 2008; 29(4): 441-464.
31. Lix LM, Azimaee M, Osman BA, Caetano P, Morin S, Metge C, et al. Osteoporosis-related fracture case definitions for population-based administrative data. BMC Public Health 2012; 12: 301.
32. Ray WA, Griffin MR, Fought RL, Adams ML. Identification of fractures from computerized Medicare files. Journal of Clinical Epidemiology 1992; 45(7): 703-714.
