The distribution of physicians in Indonesia is unequal: services are concentrated in metropolitan areas, such as Jakarta. This condition leads to poor health services in rural areas, mainly in primary care services. Data from 2013 showed that primary care physician (PCP) ratio was 38.1 per 100 000 population nationally. Jakarta as the capital city had the biggest ratio, which was 155.5 for 100 000 population. In contrast, rural areas such as East Nusa Tenggara and West Sulawesi had no more than 10.5 PCPs per 100 000 people1. Considering the interrelated factors in the current health system in Indonesia (ie referral system and continuity of care), lack of PCP may negatively affect the provision of health services in Indonesia2.
The Indonesian government acknowledged this situation as a problem in the current national health status. Hence a breakthrough to fulfill the need for PCPs across the area of Indonesia in a relatively brief period was needed. Some programs have been implemented to attract young PCPs to work in rural areas, including pegawai tidak tetap (PTT; which means 'temporary employment'). This program aims to distribute PCPs, mainly fresh graduates of medical schools, to areas of national need. Graduates are required to dedicate several years to a career in a location determined by the government, usually rural and remote areas3. Graduates who join this program may get priority to be employed as a civil servant after completion. Those intending to serve in remote areas will receive financial incentives. The PTT contract duration is shorter for those who serve in remote or disaster areas4. Unfortunately, the program has not been mandatory since 2007.
Medical students may have their own plans for their future careers as PCPs5. A prior study by Silvestri et al. that was conducted in eight countries to investigate nursing and medical students' work plan found that only 18% of the students had a high likelihood of choosing rural careers6. Various factors (lifestyle7, incentives7, or previous rural training8) were considered influential for students in choosing careers in rural areas. Such studies, however, are rare in the Indonesian setting.
Factors affecting medical students' career choices in rural areas could be a guide to develop some interventions by government or medical schools to better organize medical doctors' distribution in Indonesia. The aim of this study was to explore Indonesian medical students' choices, particularly students in the Faculty of Medicine at Universitas Indonesia (FMUI), regarding their interest in future practice location for either a long-term or short-term period with PTT. Another aim was to identify intrinsic factors perceived by students to be important.
The study design was cross-sectional, using a total sampling method. The subjects were medical students of year 4 and 5 from FMUI who had already been exposed to clinical practice rotations. The medical curriculum uses a competency-based approach and consists of 3 years of pre-clinical modules and 2 years of clinical clerkship. Most clinical clerkship activities have been conducted at Cipto Mangunkusumo Hospital, a tertiary referral hospital and the main teaching hospital in Indonesia.
There are two types of enrollment in the FMUI undergraduate medical program: the regular and international classes. International class enrollment differs from the regular class: it uses English as the formal language and it requires the students to have a 1-year international placement between pre-clinical and clerkship phases. The recruitment of regular class students are conducted in several ways: national selection for universities and local selection within universities. Since 2011, the policy for national selection states that student intake through invitation will increase the variety of regions where the students come from. This policy is implemented by FMUI by considering potential students coming from regions with low health profiles, in the hopes that the students become agents of health development in their regions upon graduation.
Data were collected in August 2014 when all year 4 and 5 students gathered for their academic result announcement. Before completing the questionnaire, respondents were given written information so that they could provide their consents where appropriate. A validated questionnaire adapted from the study of Gill et al was used to identify subjects' demographic profiles, their workplace preference, their desire to enroll in PTT, and factors affecting their choice9. This questionnaire was selected based on the accordance of its content to the aim of the current study. It was translated into Indonesian and back-translated into English to assess the content validity. The translation was completed by the authors with feedback from a member of academic staff proficient in English and with necessary knowledge background. The questionnaire was piloted to 30 third-year medical students prior to the data collection. The result of the pilot study showed a good realiability with Cronbach's alpha value of 0.749 and good feedback on the clarity of the questionnaire items.
In this study, 'metropolitan' was defined as an area with >200 000 population, mostly capital cities in Indonesia. 'Urban' was defined as an area with 25 000-200 000 population and rural as an area with <25 000 population. Examples of areas within these three groups were listed in the questionnaire to help the students to complete the questionnaire9. Students were asked to mention if they had previous background in a rural area. Their reported areas were cross-checked with national data to see which had populations less than 25 0008. Students who chose an urban or metropolitan area were asked if they were interested (using a Likert scale ranging from 1 ('very unsure') to 5 ('very sure')) to enroll in PTT. Twenty one factors influencing the workplace preference were scored using a Likert scale ranging from 1 ('very unimportant') to 5 ('very important'). As well as comparing mean Likert scales among the three groups of selected practice location (metropolitan, urban, and rural) the scoring with simplified, with 1-3 as 'unimportant' and 4-5 as 'important', as per the study by Gill et al9.
Independent t-test and one-way ANOVA were used to compare numerical data with normal distribution between two groups (eg 'want' and 'do not want to enroll in PTT program' groups) and more than two groups (eg 'rural', 'urban', and 'metropolitan' groups), respectively. Post-hoc analysis was completed to further assess which pair of groups had significant association with a given factor. Pearson χ2 analysis was used to compare categorical data between groups. Also performed was logistic regression analysis to determine the association of both demographic and perception factors regarding medical students' choices of practice location and enrollment in PTT. Factors with initial p values of <0.25 were included in the analysis using a backward stepwise method. Odds ratios (OR) were then calculated. Statistically significant results were defined as p<0.05. Statistical Package for the Social Sciences v16.0 for Windows (SPSS; http://www.spss.com) was used.
Ethics approval
This study was approved by the ethical committee of the Faculty of Medicine, Universitas Indonesia (No.14/UN2.F1/ETIK/2014).
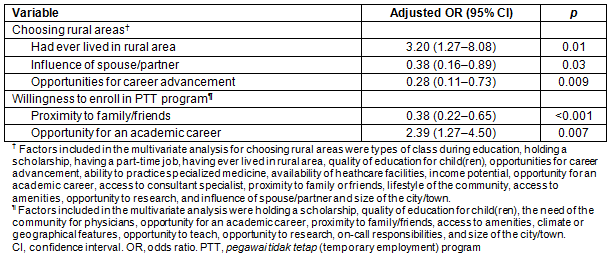
A total of 310 subjects from 372 year 4 and 5 medical students participated in this study (83.3% response rate). The remaining 62 subjects failed to participate as they either did not come to take the questionnaire or did not submit the completed questionnaire. Furthermore, they did not respond to the authors' request to participate in the study at a time after the initial questionnaire administration. A total of 152 (49%) subjects were male with a mean age of 22.2 years (standard deviation (SD) 1.1 year). Most subjects (159, 51.4%) opted for later practice in metropolitan locations, while 123 subjects (39.8%) chose urban locations and the rest (27, 8.7%) chose rural locations. Of some demographic characteristics, the types of student enrollment (regular class, p=0.006), sources of funding (scholarships, p=0.03; part-time job, p=0.002), and previous experience of living in rural areas (p=0.008) were significantly and positively associated with future practice locations of the students (Table 1).
Among those respondents who chose rural areas as their future practice, 22.7% (5/27 students) were considered to become PCPs. The trend was lower among those who chose urban (4.2%, 5/118 students) and metropolitan areas (0.6%, 1/158 students, p<0.001).
Twenty one factors were analyzed to identify those that influenced medical students' preferred location of practice. These factors were divided into three groups based on the mean value of the Likert scale (most important factors, moderately important factors, and least important factors). None of the factors had a mean value <3, so only two groups were included: most and moderately important factors. 'The need of the community for physicians', 'quality of education for the child(ren)' and 'opportunities for career advancement' were factors considered most important by students, with mean Likert scales of 4.2 (SD 0.6), 4.2 (SD 0.7), and 4.2 (SD 0.7), respectively.
A further analysis was performed by comparing the mean value of the Likert scale of these factors, and grouping them into two categories: important factors (mean of Likert scale ≥4) and moderately important factors (mean of Likert scale <4) to the students who chose to work either in metropolitan, urban and rural areas. Four factors had a statistically significant comparison in both numerical and categorical analyses (t-test and χ² analysis, respectively). In the most important factors category, the 'opportunity for career advancement' was considered important by 93.6% of students in the metropolitan group versus 87.0% in urban and 70.4% in rural group (p=0.001). In the moderately important factors category, three factors were statistically significant: 'access to specialist consultants' (79.7% metropolitan vs 65.9% rural vs 63.0% urban, p=0.02), 'proximity with friends/family' (metropolitan vs urban vs rural: 69.6% vs 58.5% vs 40.7%, p=0.008), and 'access to public amenities (shopping, sports centers, etc.)' (69.0% metropolitan vs 50.4% urban vs 48.1% rural, p=0.003). These three factors were associated with students' choice for a career not in rural areas (Table 2).
Factors associated with the interest to practice in rural areas with PTT enrollment were also analyzed. This further investigation was conducted to identify students' interests in practicing in rural areas in the short term. Among those who did not choose a career in rural areas (n=264), 48.5% (128) wished to participate in the PTT program. 'Community need for physicians' (96.1% PTT vs 85.9% not PTT, p=0.004) and 'proximity to friends/ family' (55.5% PTT vs 74.1% not PTT, p=0.002, Table 3) were factors with significant statistical results in both numerical and categorical analyses.
On multivariate logistic regression analysis, there were different factors attributed to choosing rural area and willingness to enroll in the PTT program. 'Had ever lived in a rural area' was the only demographic characteristic associated with rural choice (adjusted OR 3.20, 95%CI 1.27-8.08). Among perception factors, 'influence of spouse/partner' (adjusted OR 0.38, 95%CI 0.16-0.89) and 'opportunities for career advancement' (adjusted OR 0.28, 95%CI 0.11-0.73) made the students less likely to choose a rural area. 'Opportunity for an academic career' (adjusted OR 2.39, 95%CI 1.27-4.50) and 'proximity to family/friends' (adjusted OR 0.38, 95%CI 0.22-0.65) were associated with willingness to enroll in the PTT program (Table 4).
Table 1: Characteristics of questionnaire respondents
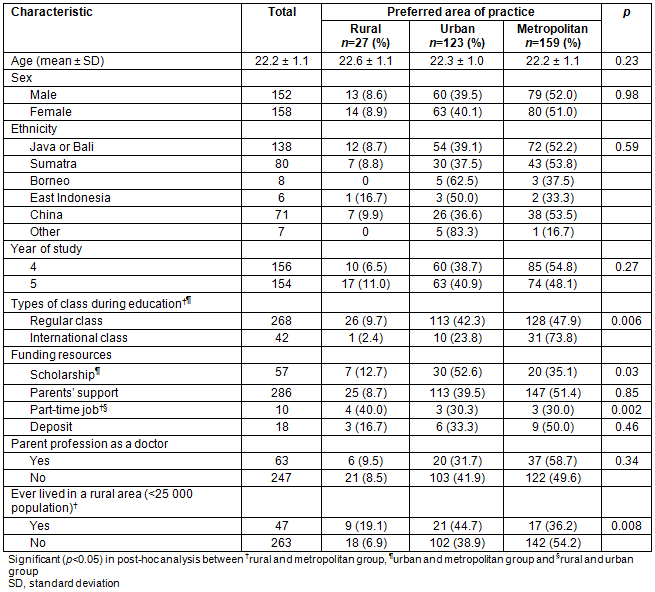
Table 2: Factors influencing preference of practice area
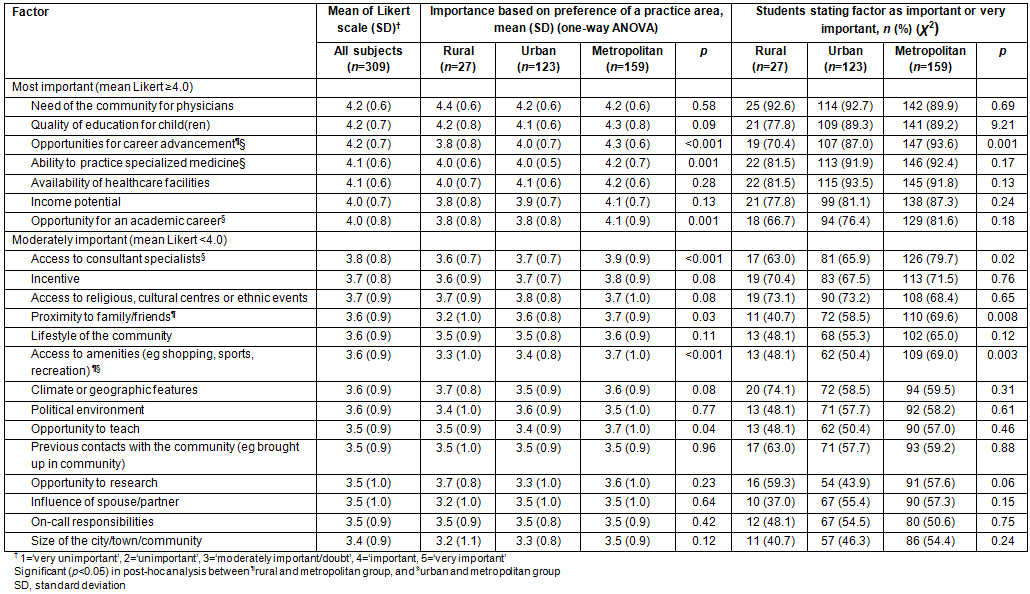
Table 3: Factors influencing preference to be involved in temporary employment program for those who want to practice in locations other than rural areas
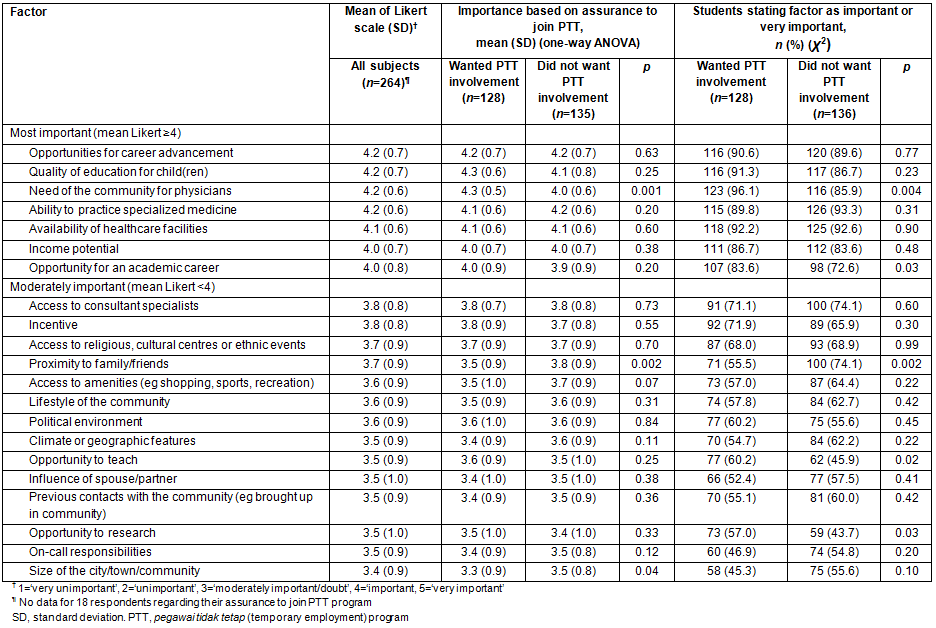
Table 4: Choosing rural areas and willingness to enroll in temporary employment program: multivariate analysis
Discussion
Distribution of PCPs in Indonesia is unequal: most physicians work in metropolitan or urban areas1. A holistic approach is required to overcome the issue; one of them is determining characteristics of medical students that make them suitable for work in rural areas. Meeting the need for physicians in every area of Indonesia is reliant on individual interest, as PCPs in Indonesia are free to choose their preferred practice location5. Therefore, the mapping of career choices of medical students and factors affecting their preferences becomes important as well. The main finding of this study was that the majority of medical students wanted to have their future practice in metropolitan areas (51.5%), while only 27 of 309 students (8.7%) wanted to practice in rural areas. Of those students who did not want to practice in rural areas for a long period, 48.5% still wanted to devote themselves to rural areas in the short term through the PTT program organized by the government.
A number of factors influenced preferences of students' future career locations. The experience of living in rural areas affected the interest of the students for a career in rural areas; thus, an increase in the supply of physicians in rural areas might be improved by increasing the number of medical students from rural regions. This is similar to previous findings that the experience of living in rural areas was a strong factor related to a rural choice9,10. A retrospective study among medical graduates in South Africa also showed that students with rural background would return to rural areas as their practice location11.
Based on the categorical and numerical comparison analyses, several factors were perceived to affect medical students' preferences of practice location in this study: 'opportunities for career advancement', 'access to specialist consultants', 'proximity to family/friends', and 'access to amenities (eg shopping, sports, recreation)' (Table 2). In the multivariate analysis, 'had ever lived in rural area', 'influence of spouse/partner' and 'opportunity for career advancement' were considered to have significant association with practicing in rural areas (Table 4). This study's results reflect that the development of facilities and infrastructures was still concentrated in urban/metropolitan areas, which become the main interest for physicians and also their partners. This study also supported that rural background, spouse influence, readiness for a rural lifestyle, and a pathway for better career advancement were factors to be considered by students12,13.
Indonesia's PTT program is held by the government to meet the needs of PCPs in the community of rural areas, but the program is not mandatory for physicians. This program applies only to physicians who are interested, based on the agreed terms. At the end of 2013, there were only 3153 PCPs as active PTT doctors, placed in provinces with an insufficient number of doctors1. In this study, among respondents who did not choose a career in rural areas (n=264), 128 respondents (48, 5%) were interested in the PTT program. Related to their background, where most of the students come from metropolitan/urban areas, 'proximity to family/friends' appeared to be a barrier to enrolling in the PTT program. Previously reported14, having family in rural areas might increase the likelihood to enter rural areas for future practice. Interestingly, the present study showed that medical students who perceived 'opportunity for an academic career' were interested to enroll in the PTT program. Graduates who served in remote areas are generally prioritised to be employed as a civil servant4 or to be accepted in a specialist program. However, the perception about 'opportunity for career advancement' was attributed to their desire to not choose a rural area as their long-term practice area. Long-term urban area selection was indeed associated with professional career and postgraduate education15. In addition, the multivariate analysis showed that perception about 'community need of physicians' was not a strong factor driving the students to practice in rural areas nor to enroll in the PTT program. Thus, their desire to serve community requires relevant actions during medical training16.
To the authors' knowledge, this is the first study evaluating Indonesian medical students' preference toward their future practice area. The study suggests that a holistic approach is needed to attract more medical graduates to practice in rural areas. Rural exposure, therefore, should be addressed accordingly and adequately in medical education. A current review suggested that, in addition to rural background, rural exposure in medical curricula would attract more students to rural practice13,17. Moreover, it is rewarding for students to learn medicine in a rural setting. Students could have a positive experience to overcome rural health problems and get accustomed to facility limitations18.
This study was not without limitations. First, this study was conducted in a single center in Indonesia. Currently there are 75 medical schools in Indonesia and a further multicenter study needs to be conducted to gain more representative results. However, the current results will be valuable to show the value of rural exposure within the medical curricula and that rural background of the medical student candidates should be considered in the selection. Second, this study used a cross-sectional design, hence it did not reflect changes over time. Third, the questionnaire only measured students' current preferences, not their actual choices. Fourth, despite the authors' awareness that 18.5% of the students had scholarship support, the rules tied to the scholarship which require students to return to their hometown after graduation do not yet seem to be implemented consistently. Therefore, this was not analyzed further as it is a confounding factor for interest in a rural career. Future studies in need to consider this scholarship factor accordingly.
Only 8.7% of students participating in this study were interested to work in rural areas after graduating from medical school. Multiple factors were associated with the selection of a rural area as a future practice location for either a long- or short-term period with the PTT program. Based on this study's results, the authors would like to encourage medical schools interested to increase the proportion of medical students choosing a future career in rural locations, to adjust their student enrollment policies and learning processes to enable more rural practice exposures in medical education. The findings would also be beneficial for the Indonesian government to further direct strategies to increase medical students' interest to fulfill the need for physicians in rural areas of Indonesia.
References
1. Kementerian Kesehatan Republik Indonesia. Profil Kesehatan Indonesia tahun 2013. (Internet) 2014. Available: http://www.depkes.go.id/resources/download/pusdatin/profil-kesehatan-indonesia/profil-kesehatan-indonesia-2013.pdf (Accessed 16 June 2015).
2. Starfield B, Shi L, Macinko J. Contribution of primary care to health systems and health. Milbank Quarterly 2005; 83(3): 457-502.
3. Biro Kepegawaian Setjen Departemen Kesehatan. Kebijakan Departemen Kesehatan tentang Pengadaan Dokter PTT. (Internet) 2008. Available: http://www.cdc.fk.ui.ac.id/_UPLOAD_/_ARTICLE_/Pemaparan%20tentang%20Program%20Dokter%20PTT.pdf (Accessed 16 June 2015).
4. Efendi F. Health worker recruitment and deployment in remote areas of Indonesia. Rural Remote Health (Internet) 2012; 12: 2008. Available: www.rrh.org.au (Accessed 16 June 2015).
5. Ministry of Health of Indonesia. Peraturan Menteri Kesehatan Nomor 512 tentang Izin Praktik dan Pelaksanaan Praktik Kedokteran. (Internet) 2007. Available: http://dinkes.surabaya.go.id/portal/files/permenkes/PermenkesRI-No.512.pdf (Accessed 1 February 2015).
6. Silvestri DM, Blevins M, Afzal AR, Andrews B, Derbew M, Kaur S, et al. Medical and nursing student's intention to work abroad or in rural areas: a cross-sectional survey in Asia and Africa. Bulletin of the World Health Organization 2014; 92: 750-759.
7. Jutzi L, Vogt K, Drever E, Nisker J. Recruiting medical students to rural practice: perspectives of medical students and rural recruiters. Canadian Family Physician 2009; 55(1): 73e1-4.
8. Daniels ZM, Vanleit BJ, Skipper BJ, Sanders ML, Rhyne RL. Factors in recruiting and retaining health professionals for rural practice. Journal of Rural Health 2007; 23(1): 63-71.
9. Gill H, McLeod S, Duerksen K, Szafran O. Factors influencing medical students' choice of family medicine effects of rural versus urban background. Canadian Family Physician 2012; 58: e649-657.
10. Walker JH, Dewitt DE, Pallant JF, Cunningham CE. Rural origin plus a rural clinical school placement is a significant predictor of medical students' intentions to practice rurally: a multi-university study. Rural and Remote Health (Internet) 2012; 12: 1908. Available: www.rrh.org.au (Accessed 16 June 2015).
11. de Vries E, Reid S. Do South African medical students of rural origin return to rural practice? South African Medical Journal 2003; 93(10): 789-793.
12. Royston PJ, Mathieson K, Leafman J, Ojan-Sheehan O. Medical student characteristics predictive of intent for rural practice. Rural and Remote Health (Internet) 2012; 12: 2107. Available: www.rrh.org.au (Accessed 16 June 2015).
13. Henry JA, Edwards BJ, Crotty B. Why do medical graduates choose rural careers? Rural and Remote Health (Internet) 2009; 9(1): 1083. Available: www.rrh.org.au (Accessed 16 June 2015).
14. Chan BT, Degani N, Crichton T, Pong R, Rourke J, Goertzen J, et al. Factors influencing family physicians to enter rural practice: does rural or urban background make a difference? Canadian Family Physician 2005; 51: 1246-1247.
15. Reid SJ, Couper ID, Volmink J. Educational factors that influence the urban-rural distribution of health professionals in South Africa: a case-control study. South African Medical Journal 2011; 101(1): 29-33.
16. Agyei-Baffour P, Kotha SR, Johnson JC, Gyakobo M, Asabir K, Kwansah J, et al. Willingness to work in rural areas and the role of intrinsic versus extrinsic professional motivations - a survey of medical students in Ghana. BMC Medical Education 2011; 11: 56.
17. Viscomi M, Larkins S, Gupta TS. Recruitment and retention of general practitioners in rural Canada and Australia: a review of the literature. Canadian Journal of Rural Medicine 2013; 18(1): 13-23.
18. Diab P, McNeill PD, Ross AJ. Review of final-year medical students' rural attachment at district hospitals in KwaZulu-Natal: student perspectives. South African Family Practice 2014; 56(1): 57-62.
