The general practice setting is characterised by a broad spectrum of reasons for encounter1,2 and a limited access to diagnostic resources including laboratory testing. There is increasing evidence that point-of-care (POC) testing is an acceptable alternative to conventional testing in the clinical laboratory3-5. The application of POC testing in general practice settings has been increasing in Europe and worldwide6,7. Although most POC testing devices require specific training and follow-up to ensure internal quality control as well as a correct interpretation of the test results, the available methods and equipment enable persons not specially trained in laboratory medicine to perform high-quality laboratory POC testing under certain conditions within a short time6. This also enables operators to use specimens like saliva and urine, as well as full blood specimens. The potential for POC testing is obvious and, since it is based on rapid tests providing results faster than conventional laboratory analyses, POC testing may facilitate quicker clinical decisions8.
The number of parameters that can be assessed by POC testing is extensive. However, in many cases, POC testing requires complex sample preparation and additional technical devices, limiting mobile availability. This study focused on POC tests that are easily applicable in a general practice setting, for example during a home visit.
A number of studies on single POC tests have been performed and published during the last few years. Most of them compared the quality of POC tests to routine laboratory methods4,5. Some investigated the influence of a POC test result concerning the decision-making of physicians9. A few studies assessed the physicians' attitude towards POC tests in a general practice setting, for example Butler et al in 2008 and Pulcini et al in 201210,11. Cals et al. reported the present use of POC testing and needs for the future of Dutch general practitioners (GPs)12. No investigation has yet been performed to find out which POC tests are used by GPs in Germany in a daily setting.
Therefore, this investigation was conducted to determine which POC tests are known and used by GPs in Saxony, Germany. Furthermore, the usefulness GPs attribute to specific POC tests was investigated and possible differences in the use of POC tests between GPs and university-associated GPs who teach undergraduates (GPTUs) as well as between urban and rural GPs were elucidated.
Identification of POC tests
Available POC tests were identified by searches in PubMed and using the search engine at http://www.web.de. The search was performed by a doctoral candidate of the authors' department and supervised by a general practice trainee. Fifty-one possible applicable POC tests were found. Each test was reviewed for the specimen needed, the necessary time to get a test result and the equipment needed to perform the test. The criteria to include a POC test in the investigation were that the specimen was easily accessible under general practice conditions, that the test could be performed within a patient's consultation in a reasonably short time, that little accessory equipment was necessary and that the test could be performed during a home visit. At the end, a list of 27 POC tests resulted. All 27 POC tests included in the survey are easily available to GPs in Saxony.
Design of the questionnaire
The questionnaire used was self-designed with the assistance of a male GP, a psychologist and a general practice trainee. Three GPs participated in pilot tests to check comprehensibility and face validity. It was a three-sided questionnaire that also contained sociodemographic data of the GP. With regard to all 27 POC tests, four items had to be marked if the answer was yes: 'I know the tested parameter', 'I know how to interpret the parameter', 'I know that there is a point-of-care test for this parameter' and 'I use this point-of-care test'. The last question focused on the estimated usefulness of the respective test: 'I think the test is ...' (1, 'not useful'; 2, 'rather not useful'; 3, 'rather useful'; 4, 'very useful'). The answers to this question were dichotomously summarised as 'not useful' and 'useful'. In a free-text section, the GPs were asked about the demand for further information concerning single POC tests. The questionnaire contained a short introductory letter and some short explanations about how to complete the form.
Sample and survey
The GPs were randomly selected from the register of members of the Kassenärztliche Vereinigung Sachsen (Saxon Association of Statutory Health Insurance Physicians KVS, http://www.kvs-sachsen.de). This is the most valid and up-to-date register of physicians in Saxony. Their list of members contained a total of 1808 GPs in 2009. The GPTUs who were also members of the KVS (n=96 in 2009) had to be excluded during the selection process in order to prevent them from being selected for both groups. The resulting list of 1712 GPs was sorted alphabetically and numbered consecutively. Then, 244 numbers in the range of 1-1712 (one in seven GPs) were randomly selected using the Statistical Package for Social Sciences v18.0 (SPSS; IBM Deutschland GmbH, http://www-01.ibm.com/software/de/analytics/spss). These 244 GPs were contacted by mail in the first half of December 2009. The list of GPTUs was sorted alphabetically and numbered consecutively. For the mail survey, 48 numbers (one in two GPTUs) were randomly selected from the range of 1-96 using SPSS. Each potential participant was contacted once. There was no pre-warning or reminder. The participants received no incentives for participating in the survey.
Statistical analysis and graphical presentation of data
The coding of the data and the statistical analysis were performed with SPSS. Depending on the presence of normal distribution (Kolmogorov-Smirnov test), either Mann-Whitney U-test or the independent sample t-test was used to compare means. For the comparison of frequencies, the χ² test or Fisher's exact test was used. Differences were assumed as statistically significant for p<0.05. The graphical presentation of the results was created with GraphPadPrism v5.0 (GraphPad Software, http://www.graphpad.com/scientific-software/prism/). Data in the text are given as mean ± standard deviation (SD).
Ethics approval
The study was conducted in accordance with the ethics committee of the Medical Faculty of Leipzig University. It acts according to the Declaration of Helsinki and the Professional Code for Physicians in Germany. No patients, patient data or human body materials were involved. This led to the conclusion that no ethical vote was necessary in this case.
Sample description
A total of 292 randomly selected GPs (48 GPTUs and 244 other GPs) were notified by mail. Due to incorrect address data, six letters were returned. Of the 286 GPs who were finally notified, 31 GPTUs and 63 other GPs responded.
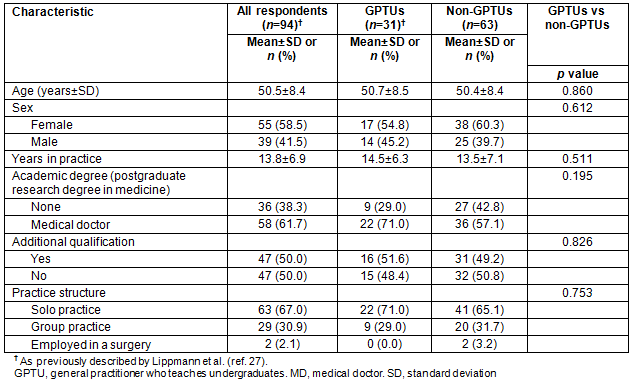
The response rates for GPTUs and GPs were 64.6% and 26.5%, respectively. The sociodemographic characteristics of the sample are presented in Table 1. In summary, no statistically significant differences between the responding GPs and GPTUs were found.
Table 1: Sociodemographic description of the responding general practitioners and the responding general practitioners who teach undergraduates.
Knowledge and utilisation of the POC tests
The GPs knew 22.5±4.5 of the laboratory parameters, the GPTUs knew 22.9±4.3 (p=0.427). The amount of known POC tests was 11.6±4.9 vs 12.4±5.5 (GPs vs GPTUs; p=0.441). The amount of used POC tests was 5.5±2.3 vs 6.0±2.5 (GPs vs GPTUs; p=0.431). Comparing the knowledge and utilisation of the single POC tests between GPs and GPTUs revealed no relevant or statistically significant differences except for the knowledge of the M2 pyruvate kinase POC test. This test was known to 27.0% of the GPs and 48.4% of the GPTUs (p=0.040). The knowledge and utilisation of the POC tests is presented in Figure 1.
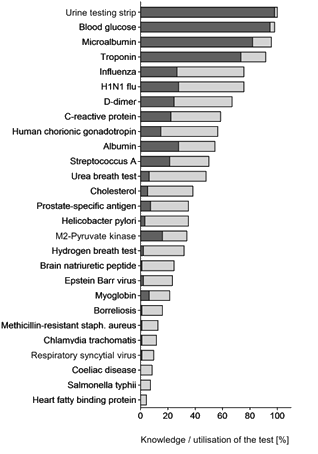
Figure 1: Knowledge (grey) and utilisation (black) of point-of-care tests among general practitioners (n=94).
Estimated usefulness of the POC tests
Twelve of the 27 POC tests were estimated as 'rather useful' or 'very useful' by more than 50% of GPs who felt able to answer this item. Figure 2 summarises these results. There were no significant differences between GPs and GPTUs concerning the perception of the usefulness of the examined POC tests. Furthermore, no significant differences were found with regard to the perceived usefulness of the examined tests between GPs practising in rural and urban regions.
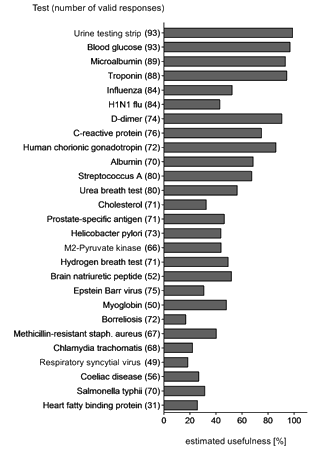
Figure 2: Estimated usefulness (percentage of general practitioners who stated the rapid test is rather useful or very useful from all GPs who gave information about the estimated usefulness of the test) regarding specific point-of-care tests. The number of valid responses for the respective test is given in brackets.
Rural versus urban general practitioners
The total amount of known laboratory parameters was not different between rural (n=43) and urban (n=57) general practitioners (rural vs urban: 22.8±4.5 vs 22.5±4.4; p=0.479). A statistically significant difference in respect of the knowledge of heart fatty acid binding protein (rural vs urban: 25.6% vs 9.8%; p=0.043) was detected. This was contrary to the findings regarding chlamydia (rural vs urban: 76.7% vs 92.2%; p=0.037). Rural GPs were aware of more POC tests than their urban colleagues (mean number of tests (rural vs urban): 13.3±5.5 vs 10.6±4.4; p=0.011). This difference was abundantly clear for the following tests: heart fatty acid binding protein (percentage of GPs aware (rural vs urban): 9.3% vs 0.0%; p=0.040), C-reactive protein (72.1% vs 47.1%; p=0.014), prostate specific antigen (46.5% vs 25.5%; p=0.033), Helicobacter pylori (51.2% vs 21.6%; p=0.003), brain natriuretic protein test (34.9 vs 15.7%; p=0.031), and the H2-exhalation test (44.2% vs 21.6%; p=0.019). Despite these differences, there was no significant difference in the amount of used POC tests between rural and urban GPs (mean number of tests 5.9±2.7 vs 5.5±2.2; p=0.875).
The two statements ('I perform POC tests that are not mentioned in the questionnaire' and 'For the following parameters I would like to have a POC test') at the end of the questionnaire brought only single answers.
Discussion
This study investigated the use of POC tests among German GPs. Each GP knew on average 22.6±4.4 laboratory parameters and 11.8±5.1 POC tests and used 5.7±2.4 of the selected tests. Twelve of the 27 POC tests were estimated as useful by the majority of GPs. In this investigation, the rural GPs were aware of more POC tests than their urban colleagues.
As found in this study, POC tests that are commonly known and utilised allow monitoring diabetes or hypertension and its complications, diagnosing infections and testing for pregnancy (Fig1)6,10,13,14. Undoubtedly, the application of tests depends on the regional epidemiology. For example, and as supported by comparing the present study's findings to those from India or South Africa, testing for infection-related parameters or causative organisms is more relevant in developing than in industrial countries15,16. As pointed out earlier, these problem fields reflect a large proportion of all reasons for encounter in a general practice setting1,2,17.
A factor other than consultation frequency that may influence the knowledge, use and attributed importance of diagnostic testing is therapeutic consequence (eg relating to use of antimicrobial agents). This was the case for infection-related parameters in the present survey and is consistent with the findings of Butler et al, who reported that general practitioners in the UK were excited about the concept of distinguishing bacterial from viral infection by a POC test10, as was also shown by others18. This may be considered to be one of the reasons for the development of new tests for infectious agents such as Mycoplasma pneumoniae19.
In comparison with a Danish investigation that was focused on the C-reactive protein POC test20, much lower test utilisation (76.6% vs 22.3%) was found. This difference may be attributed to the different study design or other factors, for example rules for compensation of POC testing costs to GPs that differ among countries.
Furthermore, a fact that might determine the knowledge and the utilisation as well as the attributed importance of different ready-for-use POC tests is the possibility of an underlying dangerous course of the problem that has to be managed. This and the reimbursement that covers the costs of performing these tests21 may explain the relatively broad use and high importance of troponin and D-dimer POC tests (Figs1, 2). Acute myocardial infarction and pulmonary embolism are rare conditions in the GP's consultation hours22,23 and, as described by Sodi et al24, the results of almost all measurements of troponin ordered by GPs are negative. They also state that patients with clinical suspicion of myocardial infarction should be referred to emergency departments to avoid harm due to delayed commencement of therapy. From this perspective, the usefulness of these tests in daily routine seems to be overestimated by GPs. Nevertheless, the benefit of the troponin POC test for ruling out dangerous courses in unclear cases of chest pain25 and thereby reducing diagnostic uncertainty might explain the high importance the GPs attributed to this test. Combined testing of troponin and heart fatty acid binding protein, as suggested by others26, is not performed in general practice since the determination of heart fatty acid binding protein is not even part of the current recommendation for myocardial infarction diagnosis. This in turn may explain why GPs are not acquainted with this test (Fig1).
Both the estimated usefulness (Fig2) and the ratio of utilisation to knowledge indicate the importance GPs see in a POC test. The tests with a low attributed importance and a low ratio of utilisation to knowledge have the following in common:
- Quantitative methods can be assumed to be superior to a (semi-)quantitative ready-to-use POC test.
- Cases to apply the test in general practice (with a satisfactory pretest probability) are rare.
- Alternative diagnostic methods are available to confirm the diagnosis.
No difference was found in the utilisation of POC tests between rural- and urban-working GPs. This might reflect the well-developed infrastructure in Saxony where it is possible to send patient samples to a conventional laboratory every day. This is also in accordance with the conclusions drawn by Davids et al that existing centralised laboratory services, poor quality assurance of POC tests and lack of staff capacity deter the use of more rapid tests at POC16.
Strengths of the study
Only a few surveys have investigated the perception of the general practitioners and consider several tests. The present investigation was not limited to a single POC test. In addition, the authors examined differences between rural and urban GPs and checked if the involvement in academic training of undergraduate medical students influences knowledge and utilisation behaviour in respect of POC tests.
Limitations of the study
This investigation was performed during the influenza season and H1N1 pandemic in December 2009, which may have led to a bias in the results for the influenza POC test data. The respondents were not a representative sample of all Saxon GPs and the response rate was low27. However, the responding GPTUs were representative of all responding GPs regarding all assessed sociodemographic variables, as described earlier27. In particular, the low response rate is a known problem in general practice research28-30 and similar response rates are considered as high by other authors31. Despite low response rates, resulting samples are not necessarily biased32,33. Nevertheless, reminders, pre-warnings or incentives might have raised the response rate.
As a further possible limitation it can be argued that this study examined only a few potential influence factors regarding the GPs' perceptions of usefulness of POC tests by using univariable comparisons (GPs vs GPTUs, rural vs urban practice environment). Future studies with substantially larger sample sizes might reveal other influences, for example an association with a specific treatment focus of the GPs or different characteristics of the patient populations to which the service was provided.
Another limitation is that the literature search in the run-up to the study was not performed systematically.
GPs commonly use POC tests. The amount of different POC tests used and the number of POC tests that appear useful to GPs is small. Further research should elucidate the effectiveness of the different tests in a general practice setting regarding costs and quality of care. It should also be examined whether POC tests are used correctly by GPs and which barriers to the use of POC tests exist in general practice.
Acknowledgements
The authors would like to thank all the GPs who responded to the survey and thereby contributed to the work. Further, the authors thank Mrs Anja Heuser for proofreading the manuscript.
Author contributions
Thomas Frese and Kathleen Steger contributed equally to the present work.
References
1. Frese T, Klauss S, Herrmann K, Sandholzer H. Children and adolescents as patients in general practice - the reasons for encounter. Journal of Clinical Medicine Research 2011; 3(4): 177-182.
2. Moth G, Olesen F, Vedsted P. Reasons for encounter and disease patterns in Danish primary care: changes over 16 years. Scandinavian Journal of Primary Health Care 2012; 30(2): 70-75.
3. Cals J, van Weert H. Point-of-care tests in general practice: hope or hype? The European Journal of General Practice 2013; 19(4): 251-256.
4. Gialamas A, Laurence CO, Yelland LN, Tideman P, Worley P, Shephard MD, et al. Assessing agreement between point of care and laboratory results for lipid testing from a clinical perspective. Clinical Biochemistry 2010; 43(4-5): 515-518.
5. Yelland LN, Gialamas A, Laurence CO, Willson KJ, Ryan P, Beilby JJ. Assessing agreement between point of care and pathology laboratory results for INR: experiences from the Point of Care Testing in General Practice Trial. Pathology 2010; 42(2): 155-159.
6. Junker R, Schlebusch H, Luppa PB. Point-of-care testing in hospitals and primary care. Deutsches Ärzteblatt International 2010; 107(33): 561-567.
7. Shephard M, Shephard A, Watkinson L, Mazzachi B, Worley P. Design, implementation and results of the quality control program for the Australian government's point of care testing in general practice trial. Annals of Clinical Biochemistry 2009; 46(Pt 5): 413-419.
8. Weatherall C, Paoloni R, Gottlieb T. Point-of-care urinary pneumococcal antigen test in the emergency department for community acquired pneumonia. Emergency Medicine Journal 2008; 25(3): 144-148.
9. Cohen R, Romain O, Levy C, Perreaux F, Decobert M, Hau I, et al. Impact of CRP rapid test in management of febrile children in paediatric emergency units of Ile-de-France [in French]. Archives de Pédiatrie 2006; 13(12): 1566-1571.
10. Butler CC, Simpson S, Wood F. General practitioners' perceptions of introducing near-patient testing for common infections into routine primary care: a qualitative study. Scandinavian Journal of Primary Health Care 2008; 26(1): 17-21.
11. Pulcini C, Pauvif L, Paraponaris A, Verger P, Ventelou B. Perceptions and attitudes of French general practitioners towards rapid antigen diagnostic tests in acute pharyngitis using a randomized case vignette study. The Journal of Antimicrobial Chemotherapy 2012; 67(6): 1540-1546.
12. Cals J, Schols A, van Weert H, Stevens F, Zeijen C, Holtman G, et al. [Point-of-care testing in family practices: present use and need for tests in the future]. [In Dutch] Nederlands Tijdschrift voor Geneeskunde 2014; 158: A8210.
13. Gialamas A, St John A, Laurence CO, Bubner TK. Point-of-care testing for patients with diabetes, hyperlipidaemia or coagulation disorders in the general practice setting: a systematic review. Family Practice 2010; 27(1): 17-24.
14. Stürenburg E, Junker R. Point-of-care testing in microbiology: the advantages and disadvantages of immunochromatographic test strips. Deutsches Ärzteblatt International 2009; 106(4): 48-54.
15. Satyanarayana S, Sagili K, Chadha SS, Pai M. Use of rapid point-of-care tests by primary health care providers in India: findings from a community-based survey. Public Health Action 2014; 4(4): 249-251.
16. Davids M, Dheda K, Pant Pai N, Cogill D, Pai M, Engel N. A survey on use of rapid tests and tuberculosis diagnostic practices by primary health care providers in South Africa: implications for the development of new point-of-care tests. PloS One 2015; 10(10): e0141453.
17. Laux G, Kühlein T, Gutscher A, Szecsenyi J. Versorgungsforschung in der Hausarztpraxis. Ergebnisse aus dem CONTENT-Projekt 2006-2009. München: Springer Medizin, Urban & Vogel, 2010.
18. Lubell Y, Blacksell SD, Dunachie S, Tanganuchitcharnchai A, Althaus T, Watthanaworawit W, et al. Performance of C-reactive protein and procalcitonin to distinguish viral from bacterial and malarial causes of fever in Southeast Asia. BMC Infectious Diseases 2015; 15(1): 511.
19. Li W, Liu Y, Zhao Y, Tao R, Li Y, Shang S. Rapid diagnosis of Mycoplasma pneumoniae in children with pneumonia by an immuno-chromatographic antigen assay. Scientific Reports 2015; 5: 15539.
20. Bjerrum L, Gahrn-Hansen B, Munck AP. C-reactive protein measurement in general practice may lead to lower antibiotic prescribing for sinusitis. British Journal of General Practice 2004; 54(506): 659-662.
21. Kassenärztliche Bundesvereinigung. Einheitlicher Bewertungsmaßstab. Stand: 2. Quartal 2015. (Online) 2015 Available: http://www.kbv.de/media/sp/EBM_Gesamt___Stand_2._Quartal_2015.pdf (Accessed 30 March 2015).
22. Frese T, Sobeck C, Herrmann K, Sandholzer H. Dyspnea as the reason for encounter in general practice. Journal of Clinical Medicine Research 2011; 3(5): 239-246.
23. Verdon F, Herzig L, Burnand B, Bischoff T, Pécoud A, Junod M, et al. Chest pain in daily practice: occurrence, causes and management. Swiss Medical Weekly 2008; 138(23-24): 340-347.
24. Sodi R, Hine T, Shenkin A. General practitioner (GP) cardiac troponin test requesting: findings from a clinical laboratory audit. Annals of Clinical Biochemistry 2007; 44(Pt 3): 290-293.
25. Blank WA, Schmidt R, Schneider A. [Use of troponin T testing in family practice] [In German]. Zeitschrift für Allgemeinmedizin 2009: 418-422.
26. Li C, Li J, Liang X, Li X, Cui J, Yang Z, et al. Point-of-care test of heart-type fatty acid-binding protein for the diagnosis of early acute myocardial infarction. Acta Pharmacologica Sinica 2010; 31(3): 307-312.
27. Lippmann S, Frese T, Herrmann K, Scheller K, Sandholzer H. Primary care research - trade-off between representativeness and response rate of GP teachers for undergraduates. Swiss Medical Weekly 2012; 142: w13537.
28. Barclay S, Todd C, Finlay I, Grande G, Wyatt P. Not another questionnaire! Maximizing the response rate, predicting non-response and assessing non-response bias in postal questionnaire studies of GPs. Family Practice 2002; 19(1): 105-111.
29. Creavin ST, Creavin AL, Mallen CD. Do GPs respond to postal questionnaire surveys? A comprehensive review of primary care literature. Family Practice 2011; 28(4): 461-467.
30. Crouch S, Robinson P, Pitts M. A comparison of general practitioner response rates to electronic and postal surveys in the setting of the National STI Prevention Program. Australian and New Zealand Journal of Public Health 2011; 35(2): 187-189.
31. Behmann M, Schmiemann G, Lingner H, Kühne F, Hummers-Pradier E, Schneider N. Job satisfaction among primary care physicians: results of a survey. Deutsches Ärzteblatt International 2012; 109(11): 193-200.
32. Cockburn J, Campbell E, Gordon JJ, Sanson-Fisher RW. Response bias in a study of general practice. Family Practice 1988; 5(1): 18-23.
33. Templeton L, Deehan A, Taylor C, Drummond C, Strang J. Surveying general practitioners: does a low response rate matter? British Journal of General Practice 1997; 47(415): 91-94.
