Numerous reports across North America reveal that early childhood caries (ECC) is a common occurrence in many vulnerable communities and cultural groups. Indigenous children in Canada have a higher prevalence of ECC and increased rates of primary tooth decay than the general population1-4. The term 'Indigenous' encompasses First Nations (Status and non-status), Métis, and Inuit persons. The challenge facing communities, policy-makers, and dental and other professional groups is finding effective and sustainable approaches to promote infant and early childhood oral health (ECOH), reduce the severity of caries among children, and ultimately curb the incidence of ECC1,2,4.
Long waiting lists for pediatric dental surgery under general anesthesia (GA) to treat a severe manifestation of ECC, called severe early childhood caries (S-ECC) have unfortunately become the norm in some regions of Canada5,6. Further, the province of Manitoba reports high rates of dental surgery for preschool children under GA5,7,8. Many of these children are from disadvantaged communities in urban centres and rural and Northern communities5,7-9 (R Schroth et al. unpubl. data, 2015). Conservative estimates of the cost of treating one child with S-ECC under GA in Manitoba is $32008. In some First Nations communities, the prevalence of ECC may affect more than 90% of 3-5 year olds, with mean deft (decayed, extracted, and filled teeth) scores of 13.7±3.2, some of the highest recorded rates of decay in the North American literature9.
Community-developed oral health promotion initiatives have the potential to increase community engagement and therefore knowledge and awareness of ECC and preschool oral health. The challenge is to evoke sustainable, long-term behavioural change among parents, caregivers, and the community-at-large10. Community-development initiatives that extend beyond the participation of health service providers to actively involve residents and community agencies may help in ultimately improving the oral health of young children from high-risk groups11-14. Such a multidisciplinary, comprehensive approach has proven to be a valid vehicle to engage American Indian communities in sustainable ECC prevention that can influence caries rates15,16. Carrying out such programming may be an important step in preventing and reducing the severity of ECC in Manitoba, Canada.
The purpose of this study was to evaluate the impact of a project based on community-development principles with the goal of improving community and caregiver knowledge and awareness, and improving ECOH in four distinct Manitoba communities.
In response to the high rates and wait times for dental surgery under GA to treat S-ECC, a multi-agency collaborative formed. Partners included the Winnipeg Regional Health Authority, Health Canada - First Nations and Inuit Health Branch, the University of Manitoba, Manitoba Health, Healthy Living and Seniors, and a northern health region. The partnership developed the Healthy Smile Happy Child (HSHC) project based upon the pillars of community identification and relationship building, oral health education and promotion, and research and evaluation17. A logic model for the project was developed (Fig1).
Four Manitoba communities participated: an anonymous rural First Nation in southern Manitoba, an anonymous remote northern First Nation, and two urban centres - the Point Douglas community in Winnipeg, and Thompson18. Results from a baseline survey before the start of the HSHC project have previously been published18,19.
A community-development approach was adopted for the HSHC project to foster community solutions to address ECC. It focused on developing contact with community members and identifying potential 'leaders', both residents and service providers able to provide guidance on prevention activities that would engage their community and how best to implement such strategies. Embedding ECOH promotion within existing programs, services and community activities was one focal objective. This would engage the community and make efficient use of community resources, thus ensuring that prevention strategies were integrated with ongoing community-based chronic disease prevention and healthy living strategies.
HSHC goals included: (1) promoting the initiative in these communities; (2) using existing early childhood and family-focused community-based programs, services and activities to deliver the oral health promotion and ECC prevention activities; and (3) recruiting and training natural leaders to assist in program development and to deliver the ECC prevention program on an ongoing basis. Further goals were to (4) build capacity within existing programs and communities to assist in the sustainability of the promotional and educational program; and (5) to determine the impact this would have on preschool oral health and parental knowledge and attitudes regarding ECC.
The HSHC coordinator worked with community leaders, service providers, and residents to develop a comprehensive list of potential strategies to address ECC. The coordinator met with community residents and leadership to share results and transfer knowledge gained from the baseline epidemiological study in the four communities18,19. This knowledge exchange informed community programs and the community-at-large of the scope of ECC in their community and led to targeted prevention activities and actions18,19.
Numerous activities occurred in each community that engaged members and increased their knowledge of ECOH and ultimately led to the adoption of preventive oral health practices (eg recommending early first dental visits, improving oral hygiene practices, lifting the lip to look for signs of caries, and limiting snacks and sugary beverages)20. The HSHC coordinator also facilitated many other community-development initiatives at the local service level or 'organizational capacity building'.
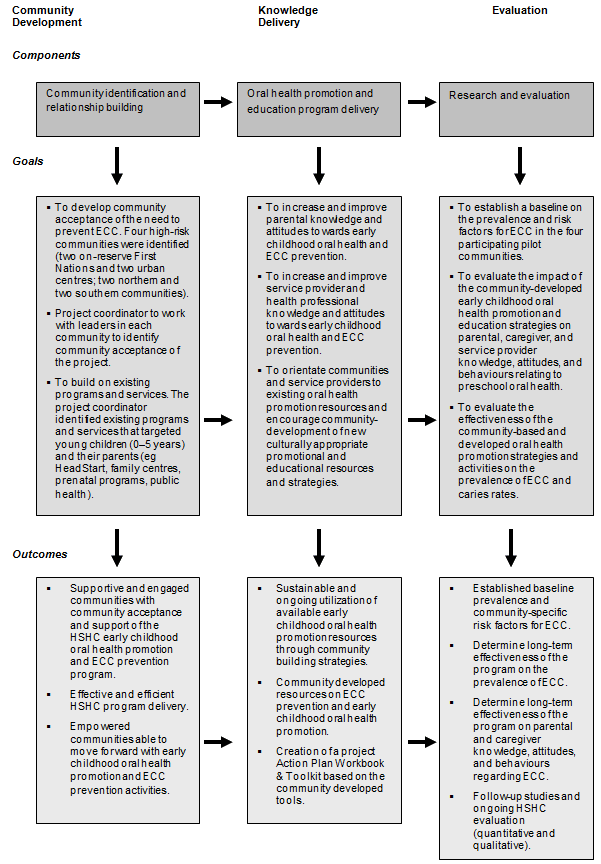
Figure 1: Healthy Smile Happy Child Project Logic Model.
Locality development
Health fairs were used to increase awareness of ECC in all four communities. The HSHC coordinator partnered with family centres, community nutritionists, and public health staff, including local dental professionals. These events provided excellent opportunities to discuss ECC prevention and alert primary caregivers of the dental services and resources available in their community.
The HSHC coordinator met with community program workers, community leaders, health providers, teachers, and others to share baseline study results, increase awareness of the issue within their own community, and build capacity in the area of ECC prevention and oral health promotion. Sharing baseline data sparked interest in ECOH and led to the generation of initiatives within the communities.
Teaching tools and resources promoting ECOH were developed in partnership with members of the four communities for use by service providers, program workers, and community members. Examples of these community-developed resources included a True/False game, Dental Bingo game, So Sweet Bottles table display demonstrating the sugar content of beverages commonly given to infants and young children, the 'Think about your Baby's Teeth' poster, and age-specific fact sheets for parents and caregivers21. Resources were developed in such a manner that community members and workers with very little or no knowledge of ECC could use them.
Organizational capacity building
Train-the-trainer activities were undertaken in each community with service providers from programs such as pre- and post-natal programs, Aboriginal Head Start, parenting groups, community health centres, and daycare centres. This method was selected as the primary way for disseminating information about the causes and consequences of ECC and prevention because it recognized that trusted relationships were already formed within the community. All necessary information was included with the resources to increase community worker comfort in addressing a new subject in front of a group and to encourage use of the various teaching tools.
Key meetings with provincial and regional Medical Officers of Health and other senior health decision-makers provided opportunities to inform them of the burden ECC has on children, families, and the healthcare system, to help shape health policy, and raise awareness of the importance of ECOH. It also permitted the sharing of baseline study information and community-development initiatives at work.
To encourage use of these resources, all information on ECC was provided within each teaching tool itself, allowing program workers to learn while teaching. At the request of one community, dental 'anticipatory guidance bags' were developed to correspond with children's immunization schedules to provide parents with timely advice for caring for baby teeth. This idea engaged public health nurses in ECC education and was introduced into all communities.
Early dental visits and infant oral health screenings were promoted in each community. Program staff was also instructed to encourage parents and caregivers to regularly check their children's teeth for early signs of ECC, by 'lifting the lip'. 'Lift the lip' was also shared with primary health care nurses and physicians, which encouraged incorporation of this practice into their daily routines, and to conduct oral health and caries-risk assessments on their young patients.
Partnerships
Key partnerships were developed between a home visiting program, school, and dental therapist in the northern First Nation community. Family support home visitors were educated on the importance of discussing ECC prevention with parents during their visits. Numerous project resources were shared with home visitors. In the other First Nation community, the dental therapist, who primarily provided clinical treatment, became involved in preventive activities, offering fluoride varnish to young children at risk for ECC. In Thompson, the project coordinator facilitated a partnership between caregiver programs to encourage them to partner in train-the-trainer workshop activities.
Numerous other partnerships were formed during the tenure of this project with agencies, professional organizations, including the Manitoba Dental Association, but more importantly with community members and groups and community centres.
Study design
A serial cross-sectional study design was selected to assess changes in community knowledge and attitudes towards ECOH and preschool oral health status five years after the HSHC project started. Parents and caregivers with children <71 months who resided in each of the four communities were eligible to participate. Participation was unrestricted. Following informed consent, face-to-face interviews with the parent or primary caregivers assessed knowledge and attitudes towards ECOH and behaviours impacting on oral health. This serial cross-sectional approach was selected as it was felt to be the only design to properly assess changes as a result of adopting a community-development framework to foster change.
Pediatric dental examinations were conducted according to WHO guidelines by one of two experienced and calibrated licensed dentists22. Criteria governing the dental examinations were the same as used for the previously published baseline study18. Both ECC and S-ECC were defined according to established criteria23,24. Dental radiographs were not utilized. Caries experience was assessed via the total deft scores. Mean and standard deviations (SD) for deft scores for each community and the overall cohort were determined. Gingival health and the presence of debris and plaque were also assessed.
The survey tool used for the baseline survey was modified for this follow-up study18,19. The standardized survey tool collected demographic information, caregiver attitudes, knowledge and behaviours, and their awareness of the HSHC project and the resources that were developed. The survey tool was originally based upon a tool developed by Lawrence and her research partners to evaluate risk factors for ECC in the Sioux Lookout Zone, Ontario25. The survey tool was administered by interview and addressed the child's general and dental health, feeding history, oral hygiene practices, and family demographics. Parental interviews were completed at the same visit as the dental examinations.
Each child's dental findings were matched with the responses to the caregiver interview. Data were analyzed using Statistical Analysis Software v9.1 (SAS Institute Inc, Cary, NC) and NCSS 2007 (Kaysville, Utah). Descriptive analyses included frequencies and means, along with SD. Bivariate analyses included χ2 analysis, t-tests, and analysis of variance (ANOVA). Results from this follow-up study were contrasted with those from the baseline study18,19. Poisson regression and multiple logistic regression analyses were also performed. A p-value of ≤0.05 was statistically significant.
Ethics approval
The study was approved by the University of Manitoba's Health Research Ethics Board (No. H2001:182) and the two First Nations.
A total of 319 children and their parents or caregivers participated in this follow-up study. Table 1 provides characteristics of participants by community. Children in this follow-up study were significantly older than those participating in the baseline study (34.0±20.5 baseline vs 38.2±18.6 follow-up, p=0.0042). Among parents and caregivers (mean age 29.7±8.0 years), 273 were mothers, 21 were fathers and 18 were either a legal guardian or a grandparent.
Parental and caregiver knowledge and attitudes of ECOH and ECC were contrasted with baseline study findings (Table 2)19. Of all the questions posed to parents and caregivers, 15 of 17 showed statistically significant improvements post-HSHC project activities. Overall, respondents in this follow-up study were significantly more likely to report that baby teeth are important (98.8% follow-up vs 91.0% baseline (7.8% improvement), p<0.0001), that problems with baby teeth will affect adult teeth (74.6% vs 59.3% [15.3% improvement], p<0.0001), and that decay in the primary dentition can impact on childhood health (94.3% vs 87.5% [6.8% improvement], p=0.0023). Caregivers also appeared to have acquired more knowledge about the importance of beginning infant oral hygiene before primary teeth begin to erupt following the HSHC project (Table 2).
Significantly more parents and caregivers reported that bottle-feeding after one year of age can harm a child's teeth (78.1% vs 62.0% [16.1% improvement], p<0.0001) and that breastfeeding is important for a child's teeth (88.4% vs 74.8% [13.6% improvement], p<0.0001). A significantly greater proportion of parents and caregivers correctly responded that bedtime bottle use was not a safe practice (79.0% vs 70.3% [8.7% improvement], p=0.0073). However, there was still a considerable proportion of respondents who were unsure of the relationship between prenatal diet and infant oral health (48.6% vs 39.3%, p=0.022). The majority of respondents were aware of the importance for a child to visit the dentist by their first birthday (82.4% follow-up vs 74.3% baseline [8.1% improvement], p=0.023).
Compared with baseline study findings, there was no significant difference in the proportion of caregivers who believed their child had caries after the HSHC project (37.6% follow-up vs 38.9% baseline, p=0.73). Similarly, there was no significant difference in caregivers' assessments of their child's oral health as being good or very good between the follow-up and baseline periods (71.2% vs 63.8%, p=0.056). Fortunately, significantly more respondents in this HSHC follow-up investigation reported that their child had already visited a dentist (50.2% vs 35.7%, p=0.0005). There also appeared to be progress in actual behaviours related to ECOH after the HSHC project. Significantly more children's teeth were being cleaned or brushed at home (87.7% vs 68.2%, p<0.0001) and more caregivers reported that they were brushing their child's teeth (86.7% vs 53.3%, p<0.0001). The frequency of brushing also increased, with 49.3% reporting that their child's teeth were being brushed more than once per day compared to 37.6% in the baseline study (p=0.001). Respondents in this follow-up investigation also indicated that children were significantly younger when brushing was initiated; 43.7% indicating to brush their child's teeth before 12 months in this follow-up study compared with only 26.8% at baseline (p<0.0001).
Breastfeeding rates (60.2% follow-up vs 59.3% baseline, p=0.80) and bottle-feeding rates (87.3% vs 89.7%, p=0.36) remained similar across the study periods. However, among children who had been weaned from the breast, children in this follow-up study were breastfed to a significantly greater age than those in the baseline study (10.2±9.9 months vs 7.7±8.0, p=0.0099). The proportion of children using sippy cups significantly increased over the HSHC project period (93.0% vs 77.8%, p=0.0001).
This follow-up study also provided an opportunity to see whether caregivers had seen the HSHC ECOH promotional resources developed by communities during the intervention period (Table 3). The southern First Nation helped develop the 'Think about your Baby's Teeth' poster while members of the Northern First Nation suggested anticipatory guidance dental goody bags corresponding with key developmental milestones in the life of the child, beginning prenatally and corresponding with immunization schedules. Collectively, the HSHC coordinator worked with all communities to develop pamphlets, games, and the So Sweet Bottle resource that were then provided to all four communities. These resources were made available online21 and compiled into an HSHC ActionPlan Workbook and Toolkit. Some resources were more recognized by follow-up study participants than others (eg 'Think about your Baby's Teeth' poster (64.5%), So Sweet Bottle resource (56.0%), HSHC pamphlets (52.2%), and 'anticipatory guidance bags' (36.0%)). There were some differences in the awareness of various resources between communities (Table 3).
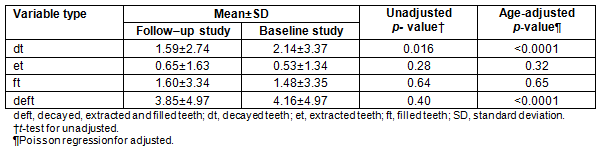
Overall, 166 children (52.0%) in this follow-up study had ECC (Table 4). Statistically significant differences in ECC prevalence were observed between children from the four participating communities (p=0.0012) (Table 4). Logistic regression analysis for ECC, adjusted for childhood age and including the various communities, revealed that there were significant associations. The prevalence of ECC significantly differed between the southern First Nation and Thompson (p=0.00075) and the northern First Nation and Thompson (p=0.00010), but not between the two urban centres (p=0.13).
Overall, 38.6% of children had S-ECC (Table 4). Logistic regression for S-ECC adjusted for childhood age and including each participating community revealed a significant association with age. Significant differences in S-ECC again were observed between the southern First Nation and Thompson (p=0.00081), the northern First Nation and Thompson (p=0.044), but not between Winnipeg and Thompson (p=0.97).
Chi-square analysis revealed that there was no significant change in ECC prevalence between the baseline and follow-up investigations (p=0.68) (Table 4). Further, unadjusted analyses revealed that the reduction in the prevalence of S-ECC from baseline to follow-up stages was not statistically significant, but did approach the threshold of significance (45.0% baseline vs 38.6% follow-up, p=0.08). However, after adjusting for age, logistic regression analysis for S-ECC did reveal a significant difference in prevalence between study periods following the years of community-development activity; the occurrence of S-ECC was significantly lower in the follow-up sample (p=0.026, adjusted odds ratio 0.71).
The mean deft score for all children in this study was 3.85±4.97 (range 0-20). ANOVA revealed that there was a significant difference in deft rates among the communities (p=0.0068), with those from the anonymous Northern First Nation having significantly higher overall scores than children from Thompson (5.11 vs 2.76). Overall, equal proportions of teeth were either filled (41.5%) or decayed and untreated (41.5%).
t-test analysis revealed that Thompson was the only community that had significant reductions in both dt (number of primary teeth with untreated decay) and deft caries scores following the HSHC project periods (Table 5). However, age-adjusted Poisson regression analysis for decayed teeth (dt), extracted teeth (et), filled teeth (ft), and deft scores for each community did not reveal statistically significant difference from baseline to follow-up (data not shown). Therefore, data for communities were combined and analyzed together.
There was a statistically significant reduction in the dt score from the baseline study to follow-up evaluation (2.14±3.37 vs 1.59±2.74, p=0.016) (Table 6). After adjusting for childhood age, since children in the follow-up study were significantly older than those at baseline, Poisson regression for the entire cohort revealed that children in the follow-up study group had significantly lower dt caries rates than those in the baseline study (p<0.0001). Likewise, age-adjusted Poisson regression also revealed that the overall deft score among children in the follow-up study was significantly less than what was reported at baseline (p<0.0001).
Table 1: Distribution of participants in this follow-up study by community
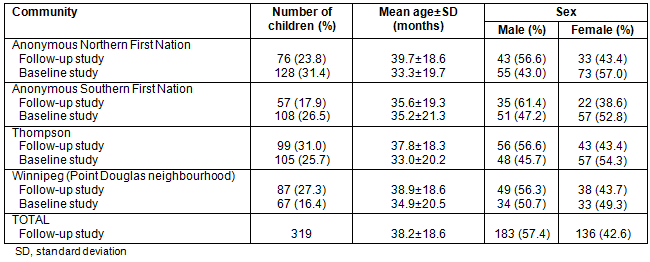
Table 2: Parental and caregiver knowledge and attitudes towards early childhood oral health
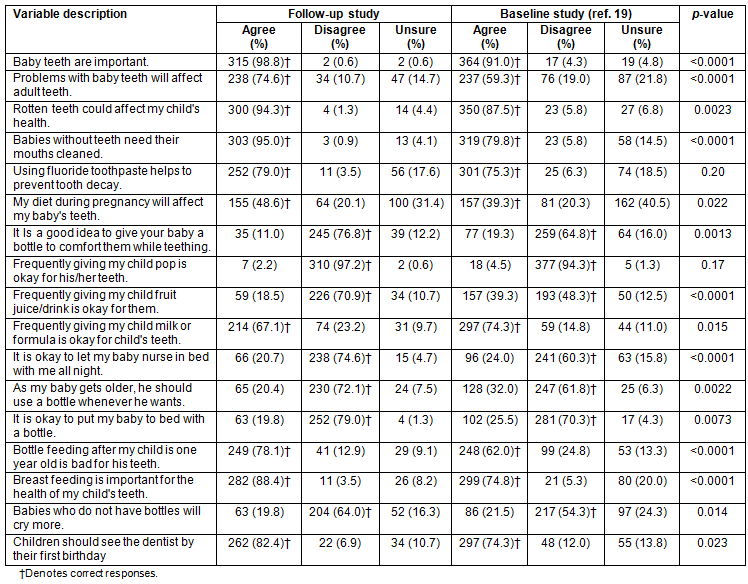
Table 3: Follow-up study participant awareness of HSHC community developed resources
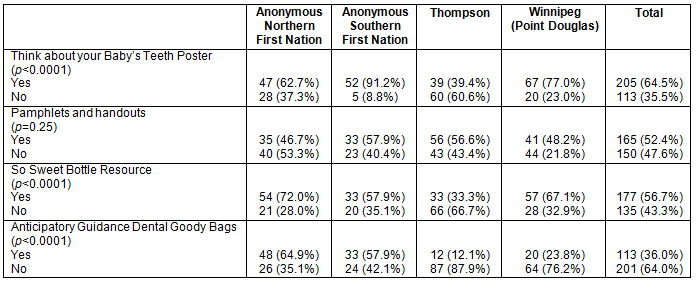
Table 4: Prevalence of early childhood caries and severe early childhood caries in follow-up study children by community
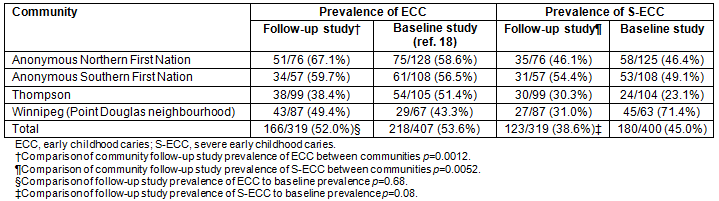
Table 5: Changes in decayed, extracted and filled teeth caries rates by participating communities
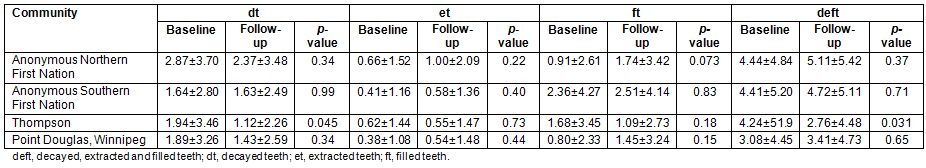
Table 6: Changes in decayed, extracted and filled teeth caries rates for entire population
Discussion
This study assessed the impact of the HSHC initiative in four Manitoba communities, including two First Nations. The HSHC partnership believed that an evaluation of the community-development approach was necessary and was part of the project's original health promotion logic model. It was fortunate that all four communities participated in both the baseline and this follow-up study. HSHC community-engagement over the five years fostered creative approaches to prevent ECC. Goals of the initiative, mentioned in the Methods section, were generally satisfied. Each community was actively engaged in the project and worked collaboratively with the project coordinator, and individual, community and organizational capacity was nurtured to support ECOH. Further, the strategy to embed ECOH promotion into existing programs was key to ensure that these activities would be sustained.
HSHC ECOH promotion activities appeared to have had a positive influence on communities and families. Respondents in this follow-up study had a significantly better understanding of oral health than reported at baseline19. Participants placed a greater value on primary teeth and were more knowledgeable of behaviours placing young children at risk for decay; and more knew that caries can affect health and well-being. This is important progress considering that ECC negatively affects wellbeing3. It appeared that more caregivers reported that their child was using a sippy cup, perhaps in an attempt to wean children from bottles. Unfortunately, sippy cups used incorrectly also carry significant risk for the development of decay. Follow-up results of a community-based intervention with a First Nations community in British Columbia reported similar improvements in community awareness of preschool oral health and ECC and also identified a reduction in harmful bottle feeding behaviours13,26.
Raising the profile of oral health in these communities appeared to result in some important shifts in behaviours relating to infant oral health. Significantly more caregivers in this study initiated brushing before their child's first birthday than before the initiative began. The frequency of brushing was also significantly improved over this time period. These findings are encouraging and the adoption of these practices certainly contributes to the reduction of a child's risk of developing ECC, as plaque levels are minimized and primary teeth are exposed to topical fluoride through the use of toothpaste. Initiating proper oral hygiene routines at crucial early stages of child development can be challenging for many families, particularly single parents or large families where there may be greater demands on family time than simply looking after oral hygiene. It has been reported that children whose families face problems in brushing their teeth are more likely to experience caries27,28.
Another observed improvement was the increased number of children in this follow-up survey who had already had a prior dental visit. Children with delayed dental experiences are at increased risk for ECC29. The fact that many children in this study had already been to the dentist is a good indicator that dental practitioners are seeing young children and that families are valuing the importance of good ECOH.
While it was originally hypothesized that it was not likely that any significant improvements in oral health status among preschool children following the five years of community-development activity would be seen, early results are very encouraging. The overall dt and deft scores at follow-up significantly differed from baseline. While it is not possible to pinpoint whether this was due to a specific activity or a synergy of activities resulting from the HSHC project, it was not due to differing ages of participating children in the baseline and follow-up assessment periods. It might be argued that the greater proportion of children from Thompson in this follow-up study might have skewed the findings as children from this urban centre may be perceived as having better access to dental care. However, the limited number of dentists and dental offices in this city in northern Manitoba means that access to dental care is still a concern. In fact, a recent evaluation of the Manitoba Dental Association's Free First Visit program reveals that few children from this area of Manitoba benefitted from an early first dental visit30. Few oral health-promotion initiatives have relied upon the use of community-development to prevent ECC. A former study involving American Indian communities, relying upon similar community-development strategies, reported a significant reduction in the prevalence of ECC at the time of follow-up16. This earlier project with American Indians involved a community-wide campaign including one-on-one counselling with parents and oral health promotion messages delivered via the media15,16. There are similarities between the methods they used and what was selected for the HSHC project here. Their study involved trained parent volunteers, health professionals and tribal employees who then counselled caretakers of young children and made group presentations. This study relied upon a similar approach of training the trainer, in order to build capacity and sustainability for ECOH promotion and ECC prevention activities among community members.
While reducing the prevalence of ECC is a laudable long-term goal, a more appropriate population marker to measure the success of prevention interventions involving high-risk populations is probably S-ECC31 (R Schroth et al. unpubl. data, 2015). Preventing any decay may be impossible. However, preventing severe cases of caries undoubtedly will reduce the need for complex rehabilitative surgery under GA. This may reduce some of the stress experienced by families and may lessen the strain on an otherwise overwhelmed healthcare system. Results from this study revealed that the age-adjusted prevalence of S-ECC was lower when compared to the baseline study (38.6% vs 45.0%), which is likely a better indication that the severity of the disease has declined over time. This might indicate that a community-engagement approach regarding the issue of preschool oral health may have had some measurable benefit on oral health status itself.
A recent randomized controlled trial providing anticipatory guidance in the form of printed material suggests that the prenatal period is an opportune time to engage mothers that can have positive impacts on toddler oral health, thereby reducing the incidence of S-ECC32. Two randomized controlled trials (RCTs) involving Canadian Aboriginal children have also examined the impact of different interventions, namely fluoride varnish and motivational interviewing33,34. Applying fluoride varnish at least twice a year resulted in a reduction in the caries rate in the range of 18-25% in the Sioux Lookout Zone34. These benefits of varnish are especially heightened when combined with education and counselling34-36. However, it is likely naïve to believe that fluoride varnish alone will adequately address the problem of S-ECC. The other RCT of motivational interviewing among the James Bay Cree of Quebec did not demonstrate a reduction in the prevalence of caries; it did provide evidence that motivational interviewing was associated with a reduction in the relative risk for severe caries lesions extending into dentin and pulp tissues37. Similarly, while a RCT of 10% chlorhexidine varnish failed to demonstrate a reduction in the prevalence of ECC in an American Indian community it did lead to a reduction in the number of children developing severe ECC38.
Community members were inspired to develop unique teaching tools to raise awareness of ECOH and prevent ECC. Since the community members were involved in the development of resources, they had meaningful input as to what information they wanted in them and what they thought would be suitable for their community. Similar educational resources have arisen from other caries prevention initiatives that engaged communities in developing solutions like educational materials, counseling booklets, posters, and bumper stickers16,39.
The HSHC project recently evaluated the effectiveness of its capacity-building train-the-trainer workshops. Results of these HSHC workshop evaluations reveal that there were significant improvements in awareness and knowledge of preschool oral health, which also lead to an increase in self-reported behaviours17. That study concluded that non-dental professionals can successfully promote ECOH and increase participant knowledge of the subject and impact their future behaviours17, providing additional rationale for partnering with non-dental service providers to promote oral health. Results from this follow-up study and ongoing evaluation by the HSHC partnership could assist in designing and implementing future S-ECC prevention programs in other high-risk populations and communities in Manitoba.
Previous oral health promotion and ECC preventive initiatives have been hampered by a lack of knowledge of local risk factors. This study strategically used baseline prevalence and risk factor data specific to each community to help engage, inform, and guide communities in the HSHC community-development process. Many lessons were learned throughout this initiative. One important realization was that ECOH must be considered a part of overall health. Further, the partnership identified that it is advantageous to incorporate oral health education and promotion into programs that have existing relationships with parents and other community members rather than establishing new services. Another important lesson was that knowledge exchange of baseline survey information specific to communities is a powerful tool to engage the community-at-large in ECC prevention. Further, it is very important to act upon requests and suggestions made by communities to ensure continued support for the HSHC project and community-engagement. Finally, to create sustainability and ensure effective and efficient use of resources, it is important to integrate health education about ECC into current programming, services and activities where trusted relationships have already been established as opposed to creating new services. For change to occur, it is important to raise awareness, equip health professionals and community health workers with a basic understanding of ECOH and risk factors for ECC, discuss the need for policy change, identify the need for ongoing organizational capacity-building, and address the related determinants of suboptimal oral health.
Successful oral health promotion strategies should empower communities and individuals, be holistic, collaborative, equitable, evidence based, sustainable, incorporate multiple approaches, and should be measurable in order to evaluate them40. The HSHC initiative satisfied many of these criteria and is now recognized as a leading practice in Manitoba. The project strived to empower communities and individuals by introducing several initiatives that increased knowledge on topics such as early first dental visits, improving oral hygiene practice and limiting sugary snacks and beverages, all while encouraging the community to adopt these practices. The HSHC partnership was a true collaborative of stakeholders and agencies. The initiative also promoted oral health as part of total childhood health and wellbeing, essentially adopting a holistic view of oral health. The HSHC initiative incorporated existing programs, services and resources in strategies while continuing to integrate healthy living strategies and prevention of chronic disease.
While results from this follow-up study are encouraging, caution is exercised about what they imply. The fact that questions posed to caregivers were retrospective in nature might have resulted in recall bias as caregivers may not have remembered early events in their child's life. Further, as several different strategies were implemented in each of the four communities, it was not possible to pinpoint the specific community-developed activities that might have been the most successful in evoking change and improvements. Rather, the overall benefit of all these combined initiatives was assessed. Apart from assessing awareness of project resources in this follow-up study, the extent of community buy-in was not formally evaluated. However, the HSHC team has undertaken focus group evaluations of service providers and community members to determine the impact of the project in the province41.
Concurrent screening in one of the First Nations community as part of Health Canada's Children's Oral Health Initiative just prior to this follow-up study and springtime flooding in the community may have resulted in a lower participation rate for that community. Despite this, it was fortunate that all four communities that took part in the baseline study participated in this evaluation. While the two dental examiners for this study were calibrated, Kappa scores were not calculated. Another consideration is the fact that control communities where there were no HSHC community-development activities occurring were not included. Since the serial cross-sectional design sampled populations at two different time periods, there may have been some other temporal changes within these communities during that time, which may have also influenced oral health. Finally, no economic evaluation was undertaken. The largest expenses related to the salary of the full-time HSHC project coordinator, travel, and the production and distribution of teaching resources.
Improvements in parental and caregiver knowledge and attitudes towards ECOH were observed following the HSHC project. Further, modest yet statistically significant reductions in caries scores and the prevalence of S-ECC were observed.
Acknowledgements
At the time of this study Dr Schroth was a CIHR Strategic Training Fellow in the Canadian Child Health Clinician Scientist Program. Operating funds for this follow-up study were obtained from the Children's Hospital Research Institute of Manitoba (formerly the Manitoba Institute of Child Health) and Manitoba Departments of Health and Healthy Living. Thank you to Dr H Lawrence and her research partners for kindly allowing us to adapt their caregiver interview tool to our study. Thank you to Drs Valerie Dorward and Olva Odlum for serving as dental examiners and to the study team including Carol Yakiwchuk, Mary Bertone, Lynn Giesbrecht, Eleonore Kliewer, Mohammad Haque, and Tara Monkman. A special note of appreciation is extended to the four communities that participated in the HSHC pilot project. HSHC activities were made possible by grant funding from the Winnipeg Foundation, the Children's Hospital Foundation of Manitoba, and contributions from First Nations and Inuit Health (Health Canada) and the Winnipeg Regional Health Authority.
References
1. Early childhood caries in indigenous communities. Pediatrics 2011; 127(6): 1190-1198.
2. Schroth, Harrison R, Lawrence H, Peressini S. Oral health and the Aboriginal child: a forum for community members, researchers and policy-makers. Journal of the Canadian Dental Association 2008; 74(5): 429-432.
3. Schroth RJ, Harrison RL, Moffatt ME. Oral health of indigenous children and the influence of early childhood caries on childhood health and well-being. Pediatric Clinics of North America 2009; 56(6): 1481-1499.
4. Irvine J, Holve S, Krol D, Schroth R. Policy statement - Early childhood caries in indigenous communities. Paediatrics and Child Health 2011; 16(6): 351-357.
5. Schroth RJ, Pang JL, Levi JA, Martens PJ, Brownell MD. Trends in pediatric dental surgery for severe early childhood caries in manitoba, Canada. Journal of the Canadian Dental Association 2014; 80: e65.
6. Canadian Institute for Health Information. Treatment of preventable dental cavities in preschoolers: a focus on day surgery under general anesthesia. Ottawa, ON: CIHI; 2013.
7. Brownell M, DeCoster C, Penfold R, Derksen S, Au W, Schultz J, et al. Manitoba child health atlas update. Winnipeg, MB: Manitoba Centre for Health Policy; 2008.
8. Schroth RJ, Morey B. Providing timely dental treatment for young children under general anesthesia in a government priority. Journal of the Canadian Dental Association 2007; 73(3): 241-243.
9. Schroth RJ, Smith PJ, Whalen JC, Lekic C, Moffatt ME. Prevalence of caries among preschool-aged children in a northern Manitoba community. Journal of the Canadian Dental Association 2005; 71(1): 27.
10. Weinstein P. Research recommendations: pleas for enhanced research efforts to impact the epidemic of dental disease in infants. Journal of Public Health Dentistry 1996; 56(1): 55-60.
11. Weinstein P. Public health issues in early childhood caries. Community Dentistry Oral Epidemiology 1998; 26(1 Suppl): 84-90.
12. Ismail AI. Prevention of early childhood caries. Community Dentistry Oral Epidemiology 1998; 26(1 Suppl): 49-61.
13. Harrison R. Oral health promotion for high-risk children: case studies from British Columbia. Journal of Canadian Dental Association 2003; 69(5): 292-296.
14. Harrison RL, Wong T. An oral health promotion program for an urban minority population of preschool children. Community Dentistry Oral Epidemiology 2003; 31(5): 392-399.
15. Bruerd B, Kinney MB, Bothwell E. Preventing baby bottle tooth decay in American Indian and Alaska native communities: a model for planning. Public Health Reports 1989; 104(6): 631-640.
16. Bruerd B, Jones C. Preventing baby bottle tooth decay: eight-year results. Public Health Reports 1996; 111(1): 63-65.
17. Macintosh AC, Schroth RJ, Edwards J, Harms L, Mellon B, Moffatt M. The impact of community workshops on improving early childhood oral health knowledge. Pediatric Dentistry 2010; 32(2): 110-117.
18. Schroth RJ, Moore P, Brothwell DJ. Prevalence of early childhood caries in 4 Manitoba communities. Journal of the Canadian Dental Association 2005; 71(8): 567.
19. Schroth RJ, Brothwell DJ, Moffatt ME. Caregiver knowledge and attitudes of preschool oral health and early childhood caries (ECC). International Journal of Circumpolar Health 2007; 66(2): 153-167.
20. Schroth R, Edwards J, Moffatt M, Mellon B, Ellis M, Harms L et al. Healthy Smile Happy Child: evaluation of a capacity-building early childhood oral health promotion initiative. Circumpolar Health Supplements 2010; 7: 60-66.
21. Winnipeg Regional Health Authority. WinnipegHealthRegion.ca. News and Information from Winnipeg Regional Health Authority. (Online) 2015. Available: www.wrha.mb.ca/healthinfo/preventill/oral_child.php (Accessed 13 April 2015).
22. WHO. Oral health surveys: basic methods. 4th edn. Geneva: WHO; 1997.
23. Drury TF, Horowitz AM, Ismail AI, Maertens MP, Rozier RG, Selwitz RH. Diagnosing and reporting early childhood caries for research purposes. A report of a workshop sponsored by the National Institute of Dental and Craniofacial Research, the Health Resources and Services Administration, and the Health Care Financing Administration. Journal of Public Health Dentistry 1999; 59(3): 192-197.
24. American Academy of Pediatric Dentistry. Definition of early childhood caries (ECC). Pediatric Dentistry 2008; 30(7): 13.
25. Lawrence HP, Romanetz, Rutherford L, Cappel L, Binguis D, Rogers JB. Effects of a community-based prenatal nutrition program on the oral health of Aboriginal preschool children in northern Ontario. Probe 2004; 38(4): 172-190.
26. Harrison R, White L. A community-based approach to infant and child oral health promotion in a British Columbia First Nations community. Canadian Journal of Community Dentistry 1997; 12: 7-14.
27. Tiberia MJ, Milnes AR, Feigal RJ, Morley KR, Richardson DS, Croft WG, et al. Risk factors for early childhood caries in Canadian preschool children seeking care. Pediatric Dentistry 2007; 29(3): 201-208.
28. Watson MR, Horowitz AM, Garcia I, Canto MT. Caries conditions among 2-5-year-old immigrant Latino children related to parents' oral health knowledge, opinions and practices. Community Dentistry and Oral Epidemiology 1999; 27(1): 8-15.
29. Schroth RJ, Cheba V. Determining the prevalence and risk factors for early childhood caries in a community dental health clinic. Pediatric Dentistry 2007; 29(5): 387-396.
30. Schroth RJ, Boparai G, Boparai M, Zhang L, Svitlica M, Jacob L et al. Tracking early visits to the dentist: a look at the first 3 years of the Manitoba Dental Association's free first visit program. Journal of the Canadian Dental Association 2015; 81: f8.
31. Schroth RJ, Halchuk S, Star L. Prevalence and risk factors of caregiver reported severe early childhood caries in Manitoba First Nations children: results from the RHS Phase 2 (2008-2010). International Journal of Circumpolar Health 2013; 72: 1
32. Plutzer K, Spencer AJ. Efficacy of an oral health promotion intervention in the prevention of early childhood caries. Community Dentistry and Oral Epidemiology 2008; 36(4): 335-346.
33. Harrison R, Veronneau J, Leroux B. Design and implementation of a dental caries prevention trial in remote Canadian Aboriginal communities. Trials 2010; 11: 54.
34. Lawrence HP, Binguis D, Douglas J, McKeown L, Switzer B, Figueiredo R et al. A 2-year community-randomized controlled trial of fluoride varnish to prevent early childhood caries in Aboriginal children. Community Dentistry and Oral Epidemiology 2008; 36(6): 503-516.
35. Weintraub JA, Ramos-Gomez F, Jue B, Shain S, Hoover CI, Featherstone JD, et al. Fluoride varnish efficacy in preventing early childhood caries. Journal of Dental Research 2006; 85(2): 172-176.
36. Azarpazhooh A, Main PA. Fluoride varnish in the prevention of dental caries in children and adolescents: a systematic review. Journal of the Canadian Dental Association 2008; 74(1): 73-79.
37. Harrison RL, Veronneau J, Leroux B. Effectiveness of maternal counseling in reducing caries in Cree children. Journal of Dental Research 2012; 91(11): 1032.
38. Robertson LD, Phipps KR, Oh J, Loesche WJ, Kaciroti N, Symington JM. Using chlorhexidine varnish to prevent early childhood caries in American Indian children. Journal of Public Health Dentistry 2013; 73(1): 24-31.
39. Kelly M, Bruerd B. The prevalence of baby bottle tooth decay among two native American populations. Journal of Public Health Dentistry 1987; 47(2): 94-97.
40. Watt RG. Strategies and approaches in oral disease prevention and health promotion. Bulletin of the World Health Organization 2005; 83(9): 711-718.
41. Schroth RJ, Wilson A, Prowse S, Edwards JM, Gojda J, Sarson J et al. Looking back to move forward: understanding service provider, parent, and caregiver views on early childhood oral health promotion in Manitoba, Canada. Canadian Journal of Dental Hygiene 2014; 48(3): 99-108.



