Lead exposure in children aged less than 6 years remains a public health issue throughout the world. Some researchers indicate a greater rural prevalence in certain regions of the USA1-3 (perhaps due to agricultural pesticide use) while other researchers report a greater prevalence in urban areas4,5. Lead research peaked in the 1980s and 1990s; therefore, the current patterns of prevalence in highly rural areas of the USA need further study.
Lead has many effects. It disrupts enzymes and the sodium-potassium-adenosine triphosphate pump; it interferes with the nervous system, hemoglobin synthesis, bone formation, and kidney function6. IQ deficits, attention-related disorders and poor academic achievement are associated with blood lead levels at 5 μg/dL7,8. The neurotoxic effect on the developing brain is described as a 'silent pandemic'8. For children, there is no safe blood lead level9. Researchers at the Centers for Disease Control and Prevention (CDC) use 5 μg/dL as a reference blood lead level and 45 μg/dL as the level at or above which chelation therapy is recommended10.
Non-remediated lead-based painted houses are the major source of lead exposure to US children. Lead-based paints were banned in 1978; however, many homes and buildings still occupied by children aged less than 6 years were built before 1978. Children living in non-remediated housing are at particular risk because they are more sensitive to the effects of lead and they have habits that predispose them to exposure (such as placing items into their mouths)6,10,11.
Other sources of lead in non-occupational exposure are water, soil, and food12. Well water in rural areas is not federally regulated and may have naturally occurring lead12 or have corroding lead service water lines. The use of lead-free solder and black, high-density polyethylene plastic water lines has helped to reduce the risk of lead exposure from water.
Some soils and the food grown in them have very high lead concentrations. The contamination may be due to lead-containing pesticides; soils near metalliferous mines; tailings sites; industrial emissions; shooting ranges; burned garbage; demolished structures; outside structures with lead-based paint degraded by weather, busy streets/highways; and wood chips from recycled, lead-based painted wood, for example. In the USA in 1996, 18 million homes had soil lead levels greater than 400 mg/kg (400 ppm), 2.5 million homes had soil lead levels greater than 2000 mg/kg, and 2.5 million had levels greater than 5000 mg/kg13. Researchers collecting 3045 soil samples from across the USA in 1993 found a median lead level of 11.0 mg/kg14. Other researchers reported a US median of 16.5 mg/kg15 from data collected between 1960 and 1975, and from National Geochemical Survey data the median was 19.75 mg/kg14. The background lead concentration in naturally occurring rural agricultural soils in the USA is 10.6 mg/kg (standard deviation 1.74 mg/kg) or 10.6 ppm16.
The Environmental Protection Agency's lead limits are 400 mg/kg in soil where children play and 1200 mg/kg for the remainder of the yard17. Lead absorption from the soil into food varies with plant species/varieties. Each has specific lead uptake, accumulation, detoxification, and excretion mechanisms18. There is a gradient of lead levels in plants grown in contaminated soil, with lead highest in the root, less in the shoot, and lower in the edible fruits19. Soils with 100 mg/kg lead or less are considered safe for gardening to grow food for children; soils with 300 mg/kg lead or less are considered safe for gardening for food for adults20.
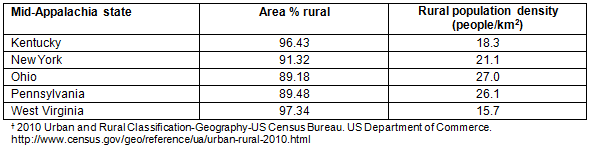
A band of high lead levels occurs in agricultural soils along the Mississippi, Ohio and Missouri rivers16. The Mid-Appalachia area (Kentucky, New York, Ohio, Pennsylvania, and West Virginia), which is 89-91% rural with a population density from 16-21 people/km2 (41-54 people/mi2) (Table 1), has a high agricultural footprint and urban areas are highly industrialized. Mid-Appalachia was a part of the old Lead Belt16 in which contamination from coal mining included aluminum, arsenic, barium, cadmium, manganese, mercury, iron, zinc, and lead21. Socioeconomic disparities are greater in mining versus non-mining regions of Mid-Appalachia22. The mining regions continue to have higher poverty rates, higher unemployment rates, and lower educational levels than the non-mining regions of Mid-Appalachia21.
The Mid-Appalachia region may pose a risk of greater lead exposure to children due to mining, industry, agriculture, and existing housing. Thus, the purpose of this study is to compare the reported blood lead levels of screened children, aged 0-72 months, to the children in the USA in general. The null hypothesis is that there is no difference in the blood lead levels of screened children in Mid-Appalachia and the blood lead levels of screened children in the rest of the USA. The research hypothesis is that there will be a greater percentage of children with a blood lead level greater than 5 μg/dL in Mid-Appalachia than in the rest of the USA. The rationale for this study is that there is a need to know about existing disparities so that policies and plans can be implemented to improve health and wellbeing.
Table 1: Mid-Appalachia states' rural status, 2010 Census Urban and Rural Classification and Urban Area Criteria, United States Census?
The data used for this study were from the CDC National Surveillance Data on Tested and Confirmed Elevated Blood Lead Levels by State, Year, and Blood Lead Level Group for Children <72 months, and the US Bureau of the Census, Decennial Census: SF3, Tables H34, H35, and American FactFinder. The surveillance year for the blood lead level data was 2011. The CDC surveillance website (http://www.cdc.gov/nceh/lead/data/national.htm) has summary data supplied by researchers from the reporting states who decide upon collection and reporting techniques23. Due to the variability in the collection and reporting methodologies, and selection of the children to be screened, the study design for this current study was semi-ecological.
The blood lead level reference number used in the present study as the variable of interest was 5 μg/dL. In the reporting states, the blood draw had been analyzed by a laboratory with Clinical Laboratory Improvement Amendments certification or an approved portable device. A confirmed blood lead level of 5 μg/dL or greater was determined using one venous blood specimen of 5 μg/dL or by taking two capillary blood specimens of 5 μg/dL or greater within 12 weeks.
The states that represented Mid-Appalachia were Kentucky, New York, Ohio, Pennsylvania, and West Virginia. The other states in this study were Alabama, Arizona, California, Connecticut, Delaware, Florida, Georgia, Illinois, Indiana, Iowa, Kansas, Louisiana, Maryland, Michigan, Minnesota, Missouri, Mississippi, New Hampshire, Oklahoma, Oregon, Rhode Island, Vermont, Wisconsin, and also included was Washington, DC. The baseline population for this study included live children born between 2005 and 2011. Individual-level data regarding family housing type, highest level of education, race/ethnicity, or income were not available.
Prevalence ratios, Fisher's χ2 exact test, and unadjusted logistic regression were analyzed with the Statistical Package for the Social Sciences v21 (SPSS; http://www.spss.com). The a priori significance level was set to 0.05.
Ethics approval
This study received West Virginia University Institutional Review Board acknowledgement (ethics approval number: 1409442143) and the research was conducted in accordance with prevailing ethical principles. The strengthening of reporting of observational studies in epidemiology (STROBE) statement checklist was followed in this study.
Table 2 has the descriptive characteristics of the Mid-Appalachia states and national summary. Nationally, 3 697 798 children aged 0-72 months received blood lead level testing reported to the CDC for 2011. Tests for 214 275 children were confirmed to have lead levels of at least 5 μg/dL (weighted percentage: 5.79%; SE, 1.34). Within the Mid-Appalachia region, there were 556 398 children tested and 43 122 children were confirmed for at least 5 μg/dL of lead (weighted percentage: 7.75%; standard error (SE), 0.68). The Mid-Appalachia state with the most children with confirmed lead levels at or above 5 μg/dL was Pennsylvania: 16 085 children of the 150 110 children tested (weighted percentage, 10.72%). The Mid-Appalachia state with the least number of children with confirmed lead levels at or greater than 5 μg/dL was Kentucky: 1180 children of the 22 185 children tested (weighted percentage, 5.32%). Census data for children aged 0-72 months is also presented in Table 2 to compare statewide lead testing practices.
Table 3 has the descriptive characteristics of the housing in the Mid-Appalachia states and nationally. Nationally, 25 815 821 housing units (weighted percentage, 22.3%; SE, 2.2) had pre-1950 construction. There were 17 380 053 housing units (weighted percentage, 15.0%; SE, 1.8) with pre-1940 construction. In the Mid-Appalachia states, 7 504 476 housing units (weighted percentage, 36.9%; SE, 13.8) had pre-1950 construction. There were 5 445 509 housing units (weighted percentage, 26.8%; SE, 3.96) with pre-1940 construction. The Mid-Appalachia state with the highest number of pre-1940 housing units was New York (2 398 237 housing units; weighted percentage, 31.2%). The Mid-Appalachia state with the least number of pre-1940 housing units was Kentucky (217 673 housing units; weighted percentage, 12.4%).
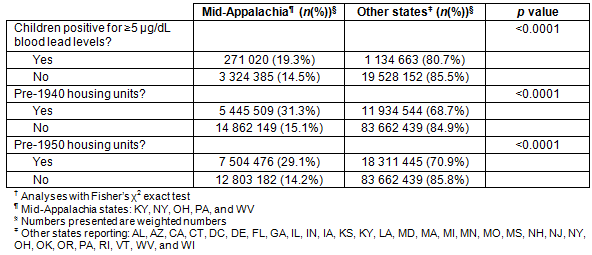
Table 4 presents the χ2 relationships comparing Mid-Appalachia with the rest of the USA in relation to blood lead level and older housing. There were significant differences, with the Mid-Appalachia region having more children with confirmed lead levels at or greater than 5 μg/dL, and Mid-Appalachia having a greater number of older housing units. The numbers presented in Table 4 for children with confirmed lead levels at or or greater than 5 μg/dL are weighted to the respective populations.
The children in the Mid-Appalachia region were more likely to have confirmed lead levels at or above 5 μg/dL (odds ratio, 1.40; confidence interval (CI), 1.397-1.41).
Table 2: Mid-Appalachia states' confirmed elevated lead levels in children aged 0-72 months23
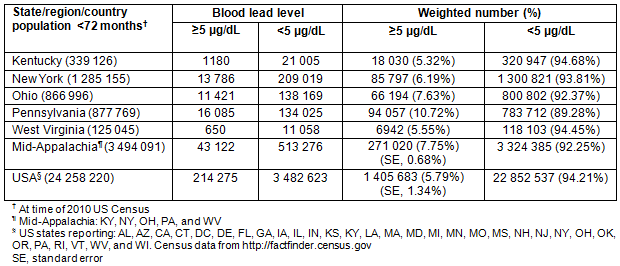
Table 3: Mid-Appalachia states' 1940-1949 and pre-1940 housing units
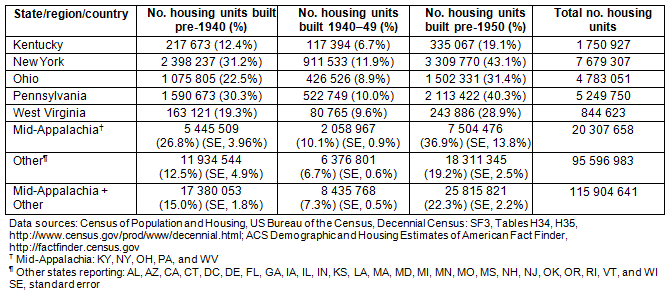
Table 4: Chi-squared analyses? comparing blood lead levels in Mid-Appalachia and other states for older housing
Discussion
Mid-Appalachia is a region with significant health disparities. The results of this study are that the region's children, aged 0-72 months, are 40% more likely to have an elevated blood lead level than children of the same age in the rest of the nation. Although the prevalence of high blood lead levels has decreased substantially over the decades, the exposure has not been eliminated11. The prevalence of 10 μg/dL or greater blood lead levels for non-Hispanic white children aged 12-60 months in 1976-1980 was 85%, and for non-Hispanic black children the prevalence was 97.7%24. By 1988-1991, the prevalence was 5.5% for non-Hispanic white children and 20.6% for non-Hispanic black children24. In 2012, the CDC proposed changes in its surveillance of lead exposure, and 5 μg/dL was identified as the reference level. The reference was based on the 97.5th percentile of the 2007-2010 National Health and Nutrition Examination Survey's (NHANES) blood lead levels in children and will be updated every 4 years10.
Progress in lowering blood lead levels in children in the USA has occurred through the elimination of lead from petrol, lead solder from soft-drink cans, and housing remediation of lead (removal of lead-based paint). In 1973, there were 0.53-0.79 g lead/L of petrol (181 437 metric tonnes/year)25. By 1995, 99.4% of petrol was unleaded25. In 1980, the beverage and food industries used lead solder in 47% of cans; by 1990, 99.15% cans were lead-free24.
The major source of lead exposure currently is lead-based paint dust. Non-remediated homes pose a health risk nationwide and particularly for the Mid-Appalachia region's children. Mid-Appalachia has a significantly higher number of older homes than the rest of the nation, both in the rural areas of Mid-Appalachia and in the industrialized urban areas. Lead-based paint deteriorates into dust. Pre-1950 lead-based paint was up to 50% lead by weight26. If a lead-based paint with a lead content of 1 mg lead/cm2 (the lowest level covered by US regulation) is completely sanded from 1 ft2 (929 cm2) of a painted wall, and dust is spread over 100 ft2 (9.29 m2), the leaded dust contains 9300 μg/ft2 (10 µg/cm2) of lead27. The dust has more than 200 times the amount permitted by the US Department of Housing and Urban Development (40 μg/ft2; 0.043 µg/cm2)27.
Blood lead level screenings for higher risk children nationally is a Grade I (insufficient evidence) recommendation by the US Preventive Services Task Force7. Nevertheless, the housing in Mid-Appalachia is older than nationally, and the percentage of children testing positive is higher than nationally. Most children with a blood lead level of 5 μg/dL or greater do not report symptoms; however, neurological and behavioral changes occur, hence the term 'silent pandemic'8. The estimated annual cost of lead exposure is $43 billion for medical care and productivity losses7. Much progress has been made; however, much more is needed. The results of this study indicate that Mid-Appalachia children have a greater burden of lead exposure than children in the rest of the nation.
This study does have limitations. The data concerning blood lead levels was summary data supplied by researchers from the reporting states, who decided upon the collection and reporting technique. There was variability in the collection and reporting methods and selection of the children to be screened. Not all children at high risk were screened. Not all states provided data. Individual-level data regarding family housing type, highest level of education, race/ethnicity, or income were not available.
As a semi-ecologic study, this study does have strengths. It supports the research that suggests there is an overall reduction in lead exposure in children; and this is a large study, with many children screened for lead exposure in each of the reporting states.
To the authors' knowledge, this is the first study to examine the disparities of lead exposure for children in the Mid-Appalachia region. The study adds to the literature the current status of lead exposure in children aged 0-72 months in the Mid-Appalachia region. It also includes the number of older homes within the region as compared with the rest of the nation and demonstrates the disparities that exist for Mid-Appalachia.
Acknowledgement
Research reported in this publication was supported by the National Institute of General Medical Sciences of the National Institutes of Health under Award Number U54GM104942. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
References
1. Brink LL, Talbott EO, Sharma RK, Marsh GM, Wu WC, Rager JR, et al. Do US ambient air lead levels have a significant impact on childhood blood lead levels: results of a national study. Journal of Environmental Public Health 2013; 2013: 278042.
2. Norman EH, Bordley C, Hertz-Picciotto I, Newton DA. Rural-urban blood lead differences in North Carolina Children. Pediatrics 1994; 94: 59-64.
3. Lizardi PS, O'Rourke MK, Morris RJ. The effects of organophosphate pesticide exposure on Hispanic children's cognitive and behavioral functioning. Journal of Pediatric Psychology 2008; 33: 91-101.
4. Rifai N, Cohen G, Wolf M, Cohen L, Faser C, Savory J, et al. Incidence of lead poisoning in children from inner-city, suburban, and rural communities. Therapeutic Drug Monitoring 1993; 15: 71-74.
5. Tong S, von Schirnding YE, Prapamontol T. Environmental lead exposure: a public health problem of global dimensions. Bulletin of the World Health Organization 2000; 78(9): 1068-1077.
6. Shaik AP, Sultana SA, Alsaeed AH. Lead exposure: a summary of global studies and the need for new studies from Saudi Arabia. Disease Markers 2014; 2014: 415160.
7. Raymond J, Wheeler W, Brown MJ. Lead screening and prevalence of blood lead levels in children aged 1-2 years - child blood lead surveillance system, United States, 2002-2010 and national health and nutrition examination survey, United States, 1999-2010. Morbidity and Mortality Weekly Report 2014; 63: 36-42.
8. Grandjean P, Herz KT. Trace elements as paradigms of developmental neurotoxicants: lead, methylmercury and arsenic. Journal of Trace Elements in Medicine and Biology 2015; 31: 130-134.
9. Wheeler W, Brown MJ. Blood lead levels in children aged 1-5 years - United States, 1999-2010. Morbidity and Mortality Weekly Report 2013; 62: 245-248.
10. Centers for Disease Control and Prevention. Lead prevention tips. (Internet) 2014. Available: http://www.cdc.gov/nceh/lead/tips.htm and http://www.cdc.gov/nceh/lead/acclpp/blood_lead_levels.htm (Accessed 11 March 2016).
11. Roberts JR, Hulsey TC, Curtis GB, Reigart JR. Using geographic information systems to assess risk for elevated blood lead levels in children. Public Health Reports 2003; 118(3): 221-229.
12. Sanders AP, Desrosiers TA, Warren JL, Herring AH, Enright D, Olshan AF, et al. Association between arsenic, cadmium, manganese, and lead levels in private wells and birth defects prevalence in North Carolina: a semi-ecologic study. BioMedical Central Public Health 2014; 14: 955.
13. US Environmental Protection Agency. Distribution of soil lead in the nation's housing stock. (Internet) 1996. Available: http://www2.epa.gov/lead/distribution-soil-lead-nations-housing-stock-may-1996 (Accessed 11 March 2016).
14. Markus J, McBratney AB. A review of the contamination of soil with lead: II. Spatial distribution and risk assessment of soil lead. Environment International 2001; 27: 399-411.
15. Gustavsson N, Bolviken B, Smith D, Severson R. Geochemical landscapes of the conterminous United States - new map presentations for 22 elements. Denver, CO: US Department of the Interior, USGS, 2001.
16. Holmgren GGS, Meyer MW, Chaney RL, Daniels RB. Cadmium, lead, zinc, copper, and nickel in agricultural soils of the United States of America. Journal of Environmental Quality 1993; 22: 335-348.
17. US Environmental Protection Agency. Hazard standards for lead in paint, dust and soil (TSCA Section 403). (Internet) 2001. Available: http://www2.epa.gov/lead/hazard-standards-lead-paint-dust-and-soil-tsca-section-403 (Accessed 11 March 2016).
18. Jiang W, Liu D. Pb-induced cellular defense system in the root meristematic cells of Allium sativum-L. BMC Plant Biology 2010; 10: 40.
19. Finster ME, Gray KA, Binns HJ. Lead levels of edibles grown in contaminated residential soils: a field survey. Science of the Total Environment 2004; 320: 245-257.
20. Rosen CJ. Garden: lead in the home and urban soil environment. (Internet) 2010. Available: http://www.extension.umn.edu/garden/yard-garden/soils/lead-in-home-garden (Accessed 11 March 2016).
21. Hendryx M, Ducatman AM, Zullig KJ, Ahern MM, Crout R. Adult tooth loss for residents of US coal mining and Appalachian counties. Community Dentistry and Oral Epidemiology 2012; 40(6): 488-497.
22. Hendryx M, Ahern MM. Mortality in Appalachian coal mining regions: the value of statistical life lost. Public Health Reports 2009; 124: 541-550.
23. Centers for Disease Control and Prevention. CDC national surveillance data 1997-2012. (Internet). Available: http://www.cdc.gov/nceh/lead/data/national.htm (Accessed 11 March 2016).
24. Pirkle JL, Brody DJ, Gunter EW, Kramer RA, Paschal DC, Flegal KM, et al. The decline in blood lead levels in the United States. The National Health and Nutrition Examination Surveys (NHANES). Journal of the American Medical Association 1994; 272: 284-291.
25. United States Environmental Protection Agency. EPA takes final step in phaseout of leaded gasoline. (Internet) 1996. Available: http://www2.epa.gov/aboutepa/epa-takes-final-step-phaseout-leaded-gasoline (Accessed 11 March 2016).
26. Curtis GB, Braggio JT, Fokum F, Roberts JR, Scott R, Staley F, et al. Using GIS to assess and direct childhood lead poising prevention. (Internet) 2004. Available: http://www.cdc.gov/nceh/lead/publications/UsingGIS.pdf (Accessed 11 March 2016).
27. Jacobs DE, Clark S, Cox D, Dewalt G, Farfel M, Farr WG, et al. Guidelines for the evaluation and control of lead-based paint hazards in housing. (Internet) 2012. Available: http://portal.hud.gov/hudportal/HUD?src=/program_offices/healthy_homes/lbp/hudguidelines (Accessed 11 March 2016).
