There has been much recent investment to improve the recruitment and retention of medical graduates in rural Australia, as maintaining an adequate medical workforce in rural and remote Australia is challenging1. Evidence-based strategies used to improve rural career intentions of Australian medical graduates include the targeted selection of students with a rural background, bonding schemes for medical school places, government scholarships to financially support selected students (especially those with a rural background), and providing students with significant, positive rural experiences during undergraduate training2,3. More recent initiatives have also included extended rural clinical placements4,5 and establishing rural clinical schools6 and regionally based medical schools7.
James Cook University (JCU) was the first Australian medical school to be established in a regional area (northern Queensland, Australia), and enrolled its first Bachelor of Medicine, Bachelor of Surgery (MBBS) cohort in 2000 with a mission to address the region's health needs. This six-year undergraduate program has oriented its selection processes to attract applicants from rural, remote and Indigenous Australian backgrounds via targeted recruitment of local high-school students. All students undertake a minimum of 20 weeks of rural community placements throughout the course.
The JCU program is decentralised across the northern Australian region in years 4-6, with the majority of students moving away from the early years base in Townsville to rural clinical school sites in Cairns (approximately 34%), Mackay (approximately 17%) and Darwin (approximately 8%). JCU adopted this decentralised education model primarily to ensure medical students have adequate clinical supervision and exposure to clinical experiences, as the steady yearly growth in enrolments has led to a current cohort size of more than 200 medical students, up from 60 in the first cohort, which commenced in 2000. Students are attached to two clinical schools in year 4 (Townsville and Cairns), and four sites in years 5 and 6 (Cairns, Townsville, Mackay and Darwin). Students undertake the majority of their clinical training in their site of allocation, with additional rotations to undertake eight-week rural terms in years 4 and 6, and the possibility of a rural elective in year 6.
The JCU program also has over one-third of its students enrolled under the Bonded Medical Placement (BMP) and rurally orientated scholarship schemes, which also aim to increase the number of doctors practising in non-metropolitan communities across Australia. Nationally, the BMP scheme provides over 700 additional Commonwealth Supported Places (CSPs) each year to first-year Australian medical students8. At the time, BMP participants entered a legal contract to work in a 'District of Workforce Shortage' following specialty training for a period equal to the length of their medical degree (although half of the return-of-service obligation can be completed during prevocational and vocational training). It has recently been estimated that over 25% of all first-year students entering medical school with a CSP are allocated to BMP or rurally bonded scholarship schemes9.
The Medical Rural Bonded Scholarship (MRBS) was designed to address doctor shortages outside metropolitan areas by providing 100 CSPs each year to first-year Australian medical students along with scholarships worth over $25,000 (in 2012)10. Students accepting the MRBS are obliged to complete their medical studies, gain Fellowship as a specialist, and then work for six continuous years in a rural or remote area of Australia (less any credit obtained through scaling), and then commencing work in an RA2-5 area within 12 months of attaining Fellowship.
First-year Queensland students enrolled in an applicable health-related program could also previously receive financial assistance from the Queensland Health Rural Scholarship Scheme (QHRSS); while recently discontinued, this was available to graduates in this study. Following graduation, QHRSS holders are employed contractually in predominantly rural positions within hospital and health services across Queensland, with a return-of-service period equalling the number of years that financial assistance was provided. In contrast, the Rural Australia Medical Undergraduate Scholarship (RAMUS) scheme assists about 130 rural background students with a $10,000 grant to study medicine at university each year, but does not require them to work in a rural area after they graduate. However, applicants must state a positive rural intention and scholarship holders must be mentored by a rural doctor and be members of their university's student rural health club.
While very little is known about the effectiveness of BMP and rurally orientated scholarship schemes in increasing the number of doctors practising in Australian communities outside of metropolitan areas11, there is some evidence that rural clinical schools11,12 and decentralised medical programs have additional benefits in addressing geographic mal-distribution of medical doctors13.
This paper describes the different outcomes of the strategies used at JCU to bolster the recruitment and retention of medical graduates in four northern Australian towns: the decentralised model of four rural clinical schools; selecting students with a rural home town; enrolling students under the BMP scheme; and providing rurally orientated scholarships. Two of these towns - Darwin in the Northern Territory (NT) and the Mackay region of north Queensland - are experiencing significant challenges in recruiting resident doctors, GPs and specialists, and are classed as 'areas of workforce shortage'14.
Design
This analysis of practice location data is part of an ongoing longitudinal cohort study to provide information about JCU MBBS graduate outcomes. Annual practice location data have been obtained for graduates in the first nine cohorts who entered the workforce as interns or postgraduate year (PGY) 1 doctors from 2006 to 2014, PGY2 from 2007 to 2014 etc.
Data collection
Practice location data for the Townsville, Cairns, Darwin and Mackay areas were obtained from several sources. Consent to join an alumni contact list and permission for subsequent contact by the medical school via email, telephone and FacebookTM were obtained from an annual exit survey of graduating medical students, conducted since 2005 as part of the JCU longitudinal tracking project on graduate outcomes15. Contact has been made by email and telephone communication on a biannual basis, and via a JCU School of Medicine FacebookTM page, which was initiated on student advice in 2005 and has been continued since for all graduating cohorts.
Additional data on practice location were sourced from the Australian Health Practitioner Regulation Authority (AHPRA), the validity of which was checked by a comparison of 20 practice locations obtained via direct contact, showing agreement for 18/20 (90%) of cases. An Australian study that correlated data from this website with data from personal contact also estimated using the AHPRA website to be 90% accurate16. In combining these strategies, practice locations could be identified for 742 out of a total of 768 graduates from 2005 to 2013, representing 97% of all graduates.
Administrative databases held by the medical school provided the following data for the 632 JCU MBBS graduates from 2005 to 2012: whether they were accepted under the BMP scheme or were awarded a rurally bonded scholarship (RAMUS, QHRSS or MRBS); their home town at application to medical school; and their rural clinical school location. Data were available on BMP for 622 graduates (98% of the total); on rurally bonded scholarships for 622 (98% of total); on home town for 605 (96% of total); and on rural clinical school location for 585 (93% of total).
The 'home town at application to medical school' data were dichotomously categorised into 'home town within 40 kilometres of Townsville/Cairns/Mackay/Darwin' and 'home town within Townsville/Cairns/Mackay/Darwin health service districts'. Similarly, internship and current practice location was categorised into the associated town or Hospital and Health Services District (HSD). HSDs were based on the boundaries map obtained from the Queensland Health website17.
Data analysis
Multivariate logistic regression analysis was used to identify independent predictors of intern practice location (Table 1) and current (2014) practice location for PGY4-9 graduates (Table 2) at each of the four rural clinical school sites of Townsville, Cairns, Darwin and Mackay.
Predictors of intern practice location in each particular town were calculated using the variables of BMP scheme (yes/no), rurally bonded scholarship (no/MRBS/RAMUS/QHRSS), had a home town within 40 km of that rural clinical school site (yes/no), and attended the clinical school in that particular town (yes/no). Predictors of current (2014) practice location in the HSD were calculated using the variables of BMP scheme (yes/no), rurally bonded scholarship (no/MRBS/RAMUS/QHRSS), had a home town within the HSD of that rural clinical school site (yes/no), and attended the clinical school in that particular town (yes/no). Results of the multivariate logistic regression analysis are presented as prevalence odds ratios (POR) together with 95% confidence intervals (95% CI). Throughout the study, a statistical test was considered significant with a p-value <0.05.
Any JCU medical graduate from 2006 to 2013 who had spent time practising in the NT and Mackay regions, had attended the Mackay or NT clinical schools, or had a home town at application in either the NT or Mackay regions was displayed in three-set Venn diagrams (Fig1), which depicts all possible logical relations between a finite collection of sets.
Table 1: Results of multiple logistic regression analysis identifying the predictive effect of home town and decentralised medical education on James Cook University (JCU) Bachelor of Medicine, Bachelor of Surgery graduates (n=620) undertaking their internship in a northern Australian teaching hospital having a JCU clinical school (Townsville, Cairns, Mackay and Darwin) from 2006 to 2013
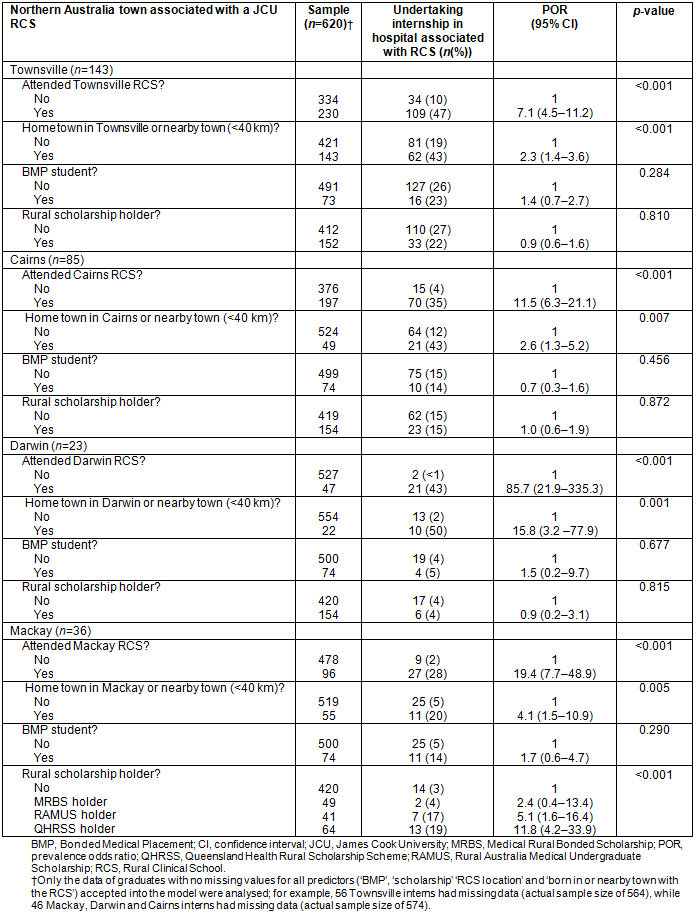
Table 2: Results of multiple logistic regression analysis identifying the predictive effect of home town and decentralised medical education on James Cook University Bachelor of Medicine, Bachelor of Surgery graduates from postgraduate years 4-9 (n=406) currently practising (2014) in a northern Australian Health Services Districts surrounding Townsville, Cairns, Mackay and Darwin
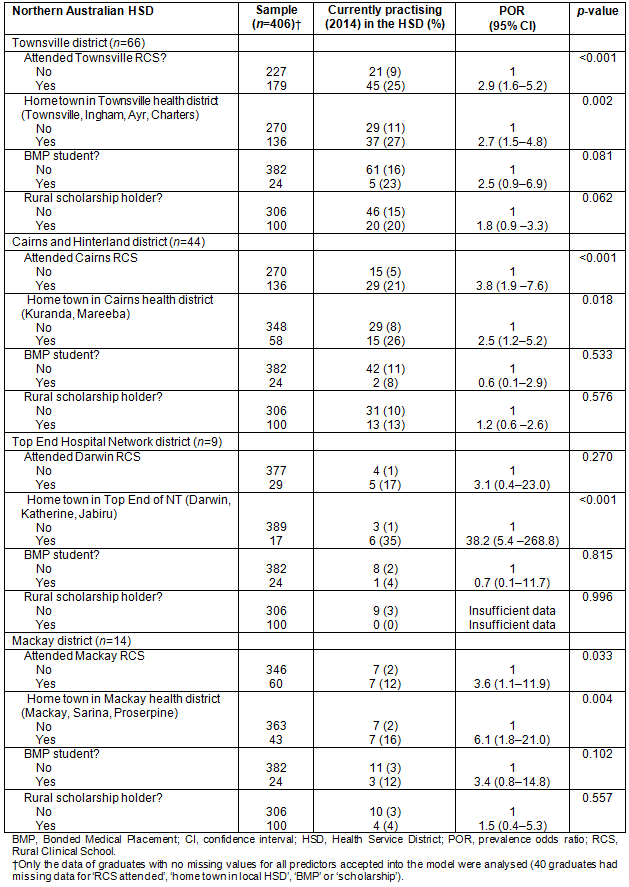
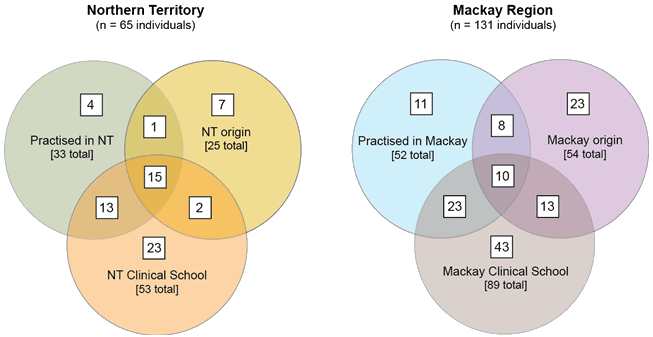
Figure 1: James Cook University Bachelor of Medicine, Bachelor of Surgery graduates' previous practice, training and/or home town at application to the JCU medical school in the Northern Territory and Mackay regions, 2006-2013. (Courtesy Maria Bellei, JCU Medical School)
Ethics approval
Ethical approval for the study was obtained from the JCU Human Research Ethics Committee (#H1804).
Description
In the years 2006-2013, of the 742 JCU MBBS graduates with known data, 199 (27%) undertook their internship in Townsville, 103 (14%) in Cairns, 43 (6%) in Mackay, and 29 (4%) in Darwin. Of PGY4-9 graduates, 77 (17%) of the known 441 graduates (17%) from the first six cohorts were currently (in 2014) practising in the Townsville HSD, while 47 (11%) were practising in Cairns HSD, 16 (4%) were practising in Mackay HSD, and 9 (2%) were practising in the Top End Hospital Network district surrounding Darwin (Fig2). Overall, 25% of the PGY4-9 MBBS graduates from JCU were awarded a rural scholarship, and 16% were accepted under the BMP scheme (with some overlap).
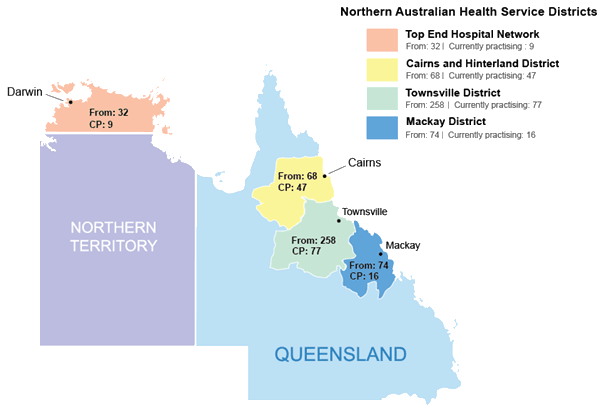
Figure 2: James Cook University Bachelor of Medicine, Bachelor of Surgery graduate numbers in northern Australia from Townsville, Cairns, Mackay and Darwin (home town at application to medical school, internship and current practice in 2014). (Courtesy Maria Bellei, JCU Medical School)
Multivariate analysis
Multivariate logistic regression demonstrates that the strongest predictor of JCU MBBS graduates undertaking their internship in Townsville, Cairns, Mackay or Darwin was attending the JCU clinical school in that location (p<0.001, POR=7.1; p<0.001, POR=11.5; p<0.001, POR=19.4; p<0.001, POR=85.7; respectively) (Table 1). Similarly, attending the JCU clinical school in the main town was a strong predictor of JCU MBBS graduates currently practising (2014) in the Townsville, Cairns and Mackay HSD (although not in the Top End Hospital Network district surrounding Darwin) (p<0.001, POR=2.9; p<0.001, POR=3.8; p<0.001, POR=3.6; respectively) (Table 2).
Having a home town at application to medical school in or nearby Townsville, Cairns, Mackay or Darwin was also a consistently strong predictor of JCU MBBS graduates undertaking internship in that town (p<0.001, POR=2.3; p=0.007, POR=2.6; p=0.005, POR=4.1; p=0.001, POR=15.8; respectively), (Table 1). Similarly, having a home town at application to medical school in the Townsville, Cairns, Mackay or Darwin HSDs was also a consistently strong predictor of JCU MBBS graduates currently practising (2014) in those respective districts (p=0.001, POR=2.7; p<0.018, POR=2.5; p=0.004, POR=6.1; p<0.001, POR=38.2, respectively) (Table 2).
Having been awarded a rural scholarship was a significant predictor (p<0.001) of internship at the Mackay Base Hospital, where being a QHRSS or RAMUS holder predicted undertaking internship in that town (POR=11.8 and POR=5.1, respectively) (Table 1).
Discussion
These findings show that a decentralised medical model with distributed rural clinical schools can assist recruiting and retaining medical doctors to those particular rural and regional locations. This study supports evidence from other studies11-13 that attending a rural or regionally based clinical school can promote rural workforce. Indeed, the association of the decentralised medical education on later practice in the present study was stronger than that of home town in all sites for internship and in half the sites for current practice, and far stronger than being accepted as a BMP student or being awarded a rurally bonded scholarship.
The JCU medical program has an undergraduate intake predominantly of high-school leavers; thus, at graduation these students are mostly 23-24 years of age. While further qualitative studies are needed to understand the reasons for graduates' choice of locations, it is possible the familiarity of the clinical school and the associated location would make graduates view that training hospital much more positively as a supportive, quality learning environment for internship training and an appropriate place to live. In addition, life decisions, including partnering, can take precedence over career intentions, and at least some graduates who may never had undertaken internship at hospitals in these towns except for the influence of their clinical school and social experiences may end up staying permanently in these towns, or return later after specialty training obligations.
However, it can be seen that the retention aspects of the decentralised training model are not as strong as recruitment. One likely reason is that specialty training programs and lack of later specialist positions are playing a role in graduates moving away from these northern HSDs to practise in more metropolitan centres. In response, JCU has established the Northern Clinical Training Network18, which aims to develop career and training pathways to postgraduate practice in a range of specialties across the region. In addition, JCU has recently been contracted to provide postgraduate education and training for doctors specialising in general practice under the Australian General Practice Training Program. Commencing from January 2016, JCU's Generalist Medical Training (GMT) Unit19 is delivering GP training for North Western Queensland (all of regional Queensland except greater Brisbane, the Gold Coast and the Darling Downs). Through GMT, the School is seeking to better connect the training pipeline from medical school to a career in general practice, with a special emphasis on remote and underserved communities. Analysis of the School's tracking database shows a number of graduates are already moving away from the larger HSDs to practise/train as rural generalists in remote northern Australian locations, including Thursday Island, Weipa, Cooktown, Broome, Katherine, Arnhem Land and Mount Isa. The vertically integrated GMT program should further enhance this promising pattern of JCU medical graduates undertaking remote practice.
Rural scholarship predicted internship practice in Mackay (both QHRSS and RAMUS). QHRSS holders are obligated to return service after graduation in predominantly rural positions. Mackay fulfils the requirements of the QHRSS for an intern practice location for at least 1 year of return service. While medical graduates holding a RAMUS are not rurally bonded, the RAMUS scheme is often linked to the Rural Generalist specialty - for which the Mackay Base and Townsville Hospitals have training pathways available. However, it is not clear whether accepting a rural scholarship results in JCU graduates undertaking their internship or later practice in Mackay and Cairns, or is adopted by graduates who would practise there anyway.
There are likely to be complex interactions that impact on recruitment and retention between the variables of home town, training location and rural scholarship. Figure 1 presents a summary of the data on 196 graduates from 2006 to 2013 who had a home town in the Mackay and Northern Territory regions, attended the Mackay or NT Clinical School, or later practised for at least 12 months in Mackay or the NT after graduation. The Venn diagrams show that nearly all graduates who later chose to practise in Mackay or the NT regions either had a home town in the region or attended the clinical school in the town (79% and 88%, respectively), while a significant percentage (19% and 45%, respectively) had a home town in the region and also attended the clinical school. While these data are interesting and illustrate the PORs described previously, more qualitative research needs to be undertaken to better understand the interactions between these and other lifestyle, family and postgraduate training variables on rural recruitment and retention decisions.
While the proportions of JCU medical graduates returning to the four major population centres in northern Australia are significant, it is also important to note that it is the absolute numbers of JCU graduates in northern Australia that will really make a difference to workforce. In 2014, the JCU graduating cohort undertaking internship numbered 136 doctors, with 62 (46%) undertaking internship in a northern Australian town. In addition, 320 of the total 762 JCU MBBS graduates (42%) are known to be currently practising in northern Australia. Therefore, JCU MBBS graduates are now providing a significant proportion of the northern Australian medical workforce, not only in areas of medical workforce shortage surrounding and including Darwin and Mackay, but also in areas surrounding the other major population centres of Cairns and Townsville.
Limitations
The nature of the JCU MBBS program - an undergraduate course that selects students with a rural background and has a decentralised training model - means this study is not representative of all Australian medical graduates. In addition, data were missing for some graduates on their home town at application, internship practice location, what JCU clinical school attended, if a BMP scheme student, and if a scholarship holder. Together, these missing data meant the multivariate analysis was missing 12% of cases for analyses around internship predictors and 5% of cases around current practice predictors, which may distort PORs.
The BMP and RAMUS scholarship schemes have also only been introduced relatively recently, so only 5 years of postgraduate location data are available for these variables. More later-career practice location data from JCU MBBS graduates is also needed before firm conclusions can be drawn about the retention aspects of the decentralised training model, and the interactions between the many variables can be better understood. However, the school's tracking database shows that many JCU graduates practising during 2013 in the Townsville, Cairns, Mackay and Darwin HSDs moved in 2014 to practise in northern Australian towns located in different HSDs, including remote towns such as Cooktown, Weipa, Thursday Island, Broome and Mount Isa, which suggests that limiting the current practice area to the four HSDs undervalues the real impact of JCU MBBS graduates on the overall northern Australian medical workforce.
This study supports the effectiveness of improving the rural medical workforce via the targeted selection of students with a rural background, rurally bonding scholarships and bonding schemes for medical school places. However, a decentralised medical education program appears to have one of the strongest influences of all strategies for promoting rural recruitment and retention, including in districts of workforce shortage and/or geographically remote locations. It is likely that the familiarity with the training hospital and local area, established habits and life choices that occur during the 2 years of clinical school training create the strongest bonds for JCU MBBS graduates to undertake internship and either stay or return for current practice in the four major northern Australian towns, areas where it has traditionally been challenging to maintain an adequate medical workforce.
Understanding the factors that influence medical graduates' choice of location of practice is the first step in taking a more targeted approached to recruiting and retaining a rural medical workforce. These results support other evidence for a decentralised medical model assisting recruitment and retention to rural and/or underserved regions, and are important for other jurisdictions looking to invest in a decentralised medical training model, and for future workforce planning and funding.
References
1. Ricketts TC. The changing nature of rural health care. Annual Reviews of Public Health 2000; 21: 639-657.
2. Rabinowitz H, Paynter N. The role of the medical school in rural graduate medical education: pipeline or control valve. Journal of Rural Health 2000; 16(3): 249-253.
3. Barrett F, Lipsky M, Lutifyya M. The impact of rural training experiences on medical students: a critical review. Academic Medicine 2011; 86(2): 259-263.
4. Rolfe IE, Pearson SA, O'Connell DL, Dickinson JA. Finding solutions to the rural doctor shortage: the roles of selection versus undergraduate medical education at Newcastle. Australian and New Zealand Journal of Medicine 1995; 25: 512-517.
5. Henry JA, Edwards BJ, Crotty B. Why do medical graduates choose rural careers? Rural and Remote Health (Internet) 2009; 9: 1083. Available: www.rrh.org.au (Accessed 17 July 2014).
6. Australian Government Department of Health and Ageing. Rural Clinical Training and Support (RCTS) 2011-2014 (Internet). Canberra, ACT: Department of Health and Ageing. Available: http://www.health.gov.au/clinicalschools (Accessed 17 July 2014).
7. Sen Gupta T, Murray R, Hays R, Woolley T. James Cook University MBBS graduate intentions and intern destinations: a comparative study with other Queensland and Australian medical schools. Rural and Remote Health (Internet) 2013; 13: 2313. Available: www.rrh.org.au (Accessed 27 April 2015).
8. Department of Health and Ageing. Bonded Medical Places Scheme - Information Booklet for 2012. Canberra, ACT: Australian Government, 2011.
9. Australian Medical Students Association (AMSA). Bonded Medical Places Scheme Policy. Canberra, ACT: AMSA, 2011.
10. Department of Health and Ageing. Medical Rural Bonded Scholarship Scheme. Canberra, ACT: Australian Government, 2011.
11. Grobler L, Marais BJ, Mabunda SA, Marindi PN, Reuter H, Volmink J. Interventions for increasing the proportion of health professionals practising in rural and other underserved areas. Cochrane Database Systematic Reviews 2009; 1. Available: http://onlinelibrary.wiley.com/doi/10.1002/14651858.CD005314.pub2/abstract (Accessed 27 April 2015).
12. Forster L, Assareh H, Watts LD, McLachlan CS. Additional years of Australian rural clinical school undergraduate training is associated with rural practice. BMC Medical Education 2013; 13: 37 Available: http://www.biomedcentral.com/1472-6920/13/37 (Accessed 27 April 2015).
13. Fryer GE, Stine C, Krugman RD, Miyoshi TJ. Geographic benefit from decentralized medical education: student and preceptor practice patterns. Journal of Rural Health 1994, 10(3): 193-198.
14. Australian Government Department of Health. DoctorConnect (Internet). Available: www.doctorconnect.gov.au (Accessed 17 July 2014).
15. Woolley T, Hays R, Barnwell S, Sen Gupta T, McCloskey T. A successful longitudinal tracking system for monitoring Australian Rural Clinical School graduate outcomes. Rural and Remote Health (Internet) 2015; 15: 3542. Available: www.rrh.org.au (Accessed 21 October 2015).
16. Playford D, Power P, Boothroyd A, Manickavasagar U, Ng WQ, Riley G. Is the National Registration website (Australian Health Practitioner Regulation Agency) effective in tracking Australian medical graduates' rural work? Australian Journal of Rural Health 2013; 21(5): 249-253.
17. Queensland Health. Queensland Hospital and Health Services Maps (Internet). 2015. Available: http://www.health.qld.gov.au/maps (Accessed 11 August 2015).
18. James Cook University. Northern Clinical Training Network (Internet). 2015. Available: http://www.nctn.net.au (Accessed 18 May 2015).
19. James Cook University. Generalist Medical Training (Internet) 2015. Available: http://www.gmt.edu.au (Accessed 21 October 2015).



