Between 1971 and 2000, the incidence of type II diabetes in India has increased by 11%, affecting over 61 million individuals1,2. As per an estimate of the International Diabetes Federation, there are 66.8 million individuals living with diabetes in India as of 2014, of whom 33.4 million are women. This amounts to a national prevalence of 8.6%3. According to the same source, by 2035, more than 10% of India's population, equivalent to 109 million patients, is expected to be diabetic3. Unlike many parts of the world, in the South-East Asia region, including India, around half of those estimated to have diabetes have not been diagnosed. This poses a higher socio-economic burden in the time to come4. A total of 25% of females living with diabetes die of the disease, much greater than the 15% of males who die of diabetes5.
Though initially diabetes was considered primarily an urban phenomenon in India, 47% of Indians with diabetes now live in rural areas, where the prevalence has risen from 2% in 1994 to 6% in 20094,5. While not much is known about the prevalence of diabetes among rural women, there is evidence of a prevalence as high as 12% in Mandur, Goa6,7. The growing burden of the non-communicable disease has been attributed to Westernization and the increased consumption of high-calorie foods in rural areas, in addition to an increasingly sedentary lifestyle8. The problem is further intensified because most rural women have poor access to quality diagnosis and treatment, in addition to a markedly low knowledge about the disease itself6. In addition, in some areas of South Asia, 50% of rural women living with type II diabetes are illiterate, which further exacerbates the inherent comprehension barrier that prevents them from making informed, healthy choices about diabetes care6. For instance, in Phase I of the Indian Council of Medical Research India Diabetes Study, 47% of men reported knowledge about diabetes, as compared to 39% of women9.
Knowledge about various aspects of illness is also an important part of being confident about managing the illness. This level of perceived confidence to complete a task, such as manage a disease, is known as self-efficacy. According to Albert Bandura's Self-Efficacy Theory, if individuals gain a sense of self-efficacy and feel they have control over their own behavior, they will be more likely to practise positive health behaviors and care for their own wellbeing10,11. In modern India, however, many women lack this sense of self-efficacy, specifically with regard to diabetes. According to a survey of patients with type II diabetes attending Guru Tegh Bahadur hospital in Delhi, India, only 32% of women felt confident in controlling their diabetes, compared to 54% of men12.
As a result, the lack of self-efficacy largely impedes women from seeking care. Particularly, they feel their duty to the household as wives and mothers surpasses their own personal health, leading them to constantly prioritize the health of their family over their own2,5,10. In a study conducted in the Anand District of Gujarat, 45% of women living with diabetes were housewives and had an overall lower mean performance score in most self-care practices than men2,13.
Recent health education interventions in India have touched upon knowledge and self-efficacy in the general population by applying the Health Belief Model, which is a psychosocial model that focuses on the attitudes and beliefs of individuals to explain and predict health behaviors14 (Fig1). Employing insights from the Health Belief Model in practical studies has been shown to inspire at-risk populations to practise positive health-seeking behaviors. Such studies address the primary constructs of the model (perceived susceptibility, perceived severity, perceived benefits, perceived barriers, cues to action, and self-efficacy) to promote better health outcomes in a given population15,16. Only recently, the model was adapted to include self-efficacy, suggesting that knowledge helps increase self-efficacy, which in turn promotes better health practices and health-seeking behaviors14,17. However, after an in-depth data search, no studies were found that have explored the specific relationship between diabetes knowledge and self-efficacy among rural, Indian women, suggesting a potential gap in the literature.
Indian Institute of Public Health Gandhinagar (IIPHG), in partnership with All India Institute of Diabetes Research, has implemented the Conquer Diabetes Project (CDP). CDP is a three-pronged model to generate awareness among communities and to provide care to poor diabetic patients in different settings. The five major activities are: (a) capacity building of public health professionals; (b) use of technology-handholding of public health professionals; (c) development and dissemination of information, education and communication material; (d) monitoring and supportive supervision; and (e) research activities.
While the major focus of the project was on training physicians and other facility-based as well as grass-root healthcare providers, patients visiting these facilities were also provided with information about disease and its prevention. Little effort was made to specifically reach out to female patients in rural areas as it was expected that information would percolate over a period of time in the community18,19. Given the growing threat of diabetes among women in rural India, knowledge regarding the disease's prevention, complications and treatment is invaluable. The Health Belief Model could help facilitate improved awareness and decision-making among women who lack adequate knowledge about diabetes. This study assesses the diabetes knowledge and self-efficacy in rural women by applying the Health Belief Model in villages of the Mehsana District in Gujarat.
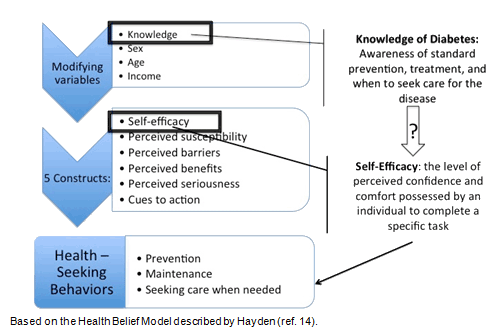
Figure 1: Health Belief Model - a theoretical framework that suggests a relationship between the four modifying variables and the five constructs and demonstrates how these affect health-seeking behaviors. The modifying variable and construct of interest in this study were knowledge and self-efficacy, respectively.
Study design
The sample was collected by quantitative cross-sectional, descriptive survey using a pre-tested tool.
Selection and description of participants: Women aged more than 18 years from the villages of Rajpur and Valam in Mehsana District of Gujarat with a random blood sugar (RBS) level of greater than 140 mg/dL (which is the minimum RBS level characteristic of diabetes) as per the records being maintained at the laboratory of the government primary health centers (PHCs) were included in the study. These records were compiled through tests performed by primary healthcare staff from November 2012 to March 2014. During this period, 264 women had been tested for their RBS levels. Of these 264 women, the survey was distributed to 126 women, and thus 77% of those tested were included in the study.
Technical information: All information in this study is reported based on the STROBE Guidelines for observational studies in epidemiology20.
Data collection
A purposive snowball sampling technique was utilized. The entire registry of patients who had been tested for diabetes at Valam and Rajpur PHCs was used to identify all women who still lived in their respective villages and fit the inclusion criteria. These respondents were then asked to suggest other women they knew who fit the specific inclusion criteria and the survey was also administered to these women. Though the use of purposive sampling may limit the generalizability of this study, random sampling was not feasible in this population where many women had limited freedom of movement. The most practical method of saturating the sample of all females with diabetes was to take participants' inputs into account during recruitment.
A local female investigator verbally administered all surveys to participants in the vernacular language. Verbal consent was obtained before the interview as many of the participants were illiterate or had low literacy levels. Participants were also assured that their identity would remain anonymous. All responses were recorded on a Samsung tablet using Open Data Kit Software v2.0 (ODK; http://opendatakit.org). Open Data Kit Software also mapped and recorded the GPS location of survey administration to ensure each survey was completed in the appropriate household. Following survey completion, participants were given an informational booklet about diabetes designed as a part of the CDP.
Survey items
The survey was adapted from both the Diabetes Knowledge Attitude and Health-Seeking Practices (KAP) Survey (Indian Institute of Public Health Gandhinagar) utilized as a part of situation analysis in the CDP, and the Diabetes Empowerment Scale - Short Form (DES-SF) (Michigan Diabetes Research and Training Center)17,19. The KAP component of the survey had already been translated into Gujarati when it was administered to 10 individuals with diabetes in each of 52 villages in Gujarat in 2013. The DES-SF reliability had already been tested in an initial sample of n=229 patients with a Cronbach-a of 0.8521. The DES-SF was translated and back-translated into Gujarati and adapted for proper comprehension by the rural study population.
The survey began with a section about the family and household demographics, which allowed quantification of the employment status, marital status, level of education, household income, caste, religion and age of patient. The 23-item Diabetic Patient Details section assessed the daily lifestyle of the patient, including her level of physical exertion, genetic predisposition to diabetes, and health habits. It also recorded quantitative measures such as the height, weight, waist circumference, and hip circumference of the patient. The 19-item KAP portion measured the diabetes prevention, treatment and management knowledge possessed by participants. The DES-SF component of the final apparatus measured the psychosocial self-efficacy of people with diabetes. This 11-item component of the survey represented two conceptual dimensions: both assessing the need for change and supporting oneself to make appropriate diabetes care choices.
Data analysis
The data were imported to Statistical Analysis Software v9.3 (SAS; http://www.sas.com). Each participant was given an individual score for both KAP and DES-SF. The score for KAP was out of a possible 24 points, and the score for DES-SF was out of 11 points.
A linear regression was used for the unadjusted analysis to evaluate the relationship between the primary covariate, knowledge (KAP) score, and the primary outcome, the self-efficacy (DES-SF) score. To determine the final model for the adjusted analysis, a bivariate analysis was run between each of the covariates of age, marital status, education, employment and monthly income, and the primary outcome of self-efficacy. A backwards selection Generalized Linear Model (GLM) was used to confirm the final correlations predicted by the bivariate analyses. Covariates with a p<0.05 were included in the final model, while those with p>0.05 were excluded. Secondary regressions were run between knowledge and the frequency of glucose monitoring of the participants. Descriptive values for body mass index (BMI) were also calculated.
All mean values for data are presented with mean±standard deviation. Both beta-coefficients and the p-values were used in the final results. A p-value of <0.05 was considered significant.
Ethics approval
The Yale University Institutional Review Board for the Protection of Human Subjects (approval #1404013815) and the Institutional Ethical Committee at IIPHG granted ethical clearance for the study.
Sociodemographic characteristics of sample
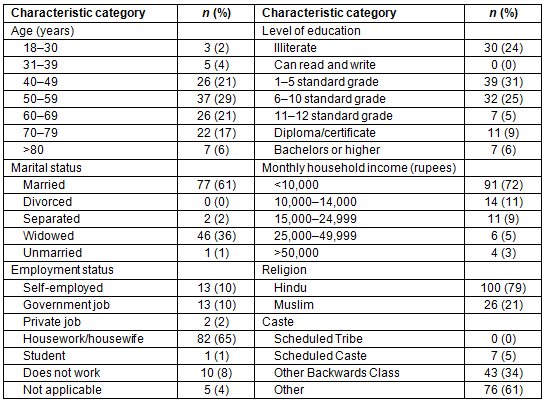
The study sample consisted of 126 women who met the inclusion criteria from two PHCs in the villages of Rajpur and Valam (Table 1). Of the 126 women in the study, 111 (88%) were between the ages of 40 and 79. Seventy-seven (61%) women were married, and 46 (37%) were widowed. The primary form of employment for most women was housework, as 82 (65%) of the women classified themselves as housewives. Most women had little education, as 30 were illiterate (24%), 39 (31%) had only completed between first and fifth standard grades in school. Ninety-one women (72%) belonged to households with an income of less than 10,000 rupees per month. Forty-three participants (34%) classified as belonging to the Other Backwards Class. The mean BMI of the study participants was 25.31±4.81 with no outliers, indicating that, on average, participants were slightly overweight.
Table 1: Descriptive statistics for women (n=126) who met the inclusion criteria from two primary health centers in Rajpur and Valam
Knowledge and self-efficacy scores
Mean knowledge score (KAP) of the participants at interview time was significantly low, at 10.77±2.86 out of a possible 24 points, for a mean percentage correct of 45%, median of 11 and interquartile range of 4 (Table 2). In particular, individual questions assessing participants' knowledge of several key causes, complications and treatment methods of diabetes was assessed in the KAP section of the survey. Only 17 (13%) of participants recognized heredity and genetic factors as key causes of diabetes. Nineteen women (24%) reported that occasionally consuming sweets caused diabetes. Another perceived cause of diabetes was stress, more commonly known as 'tension', which 54 (43%) women mentioned as a crucial contributor to diabetes.
Knowledge of most of the complications that arise from diabetes was also low. Only three (2%) participants recognized the kidneys as being afflicted by diabetes, and four (3%) women recognized heart problems as characteristic of the disease. Thirty-two women (25%) connected vision problems with diabetes. Physically painful and easily recognizable complications from diabetes, such as swollen feet due to peripheral neuropathy, were more commonly recognized as a diabetic complication (n=99 women, 79%). Finally, the notion of eating only sweets one day of the week to compensate for a week of healthy meals suggests a lack of understanding about the importance of maintaining a balanced diet.
Although only five women (4%) used smokeless tobacco, when asked about the impact of tobacco use on diabetes, 57 (45%) women responded that tobacco could potentially be used to help manage their diabetes. A common treatment mentioned for diabetes was the direct consumption of uncooked 'methi', or fenugreek. Many women also reported use of religious bands to help control their blood pressure as a diabetes treatment. Most noticeably, women typically related their diagnosis of diabetes with a hardship in life, such as the passing of a family member or their husband losing a job. Of the 126 women surveyed, only three women (2%) believed that diabetes could be prevented in future generations of their family by proper care and education. Sixty-eight women (54%) reported having adopted any change in their lifestyle after being diagnosed with diabetes.
The median self-efficacy score was 7 with an interquartile range of 3, leading to a median score of 70%. Because the distribution of self-efficacy scores was skewed to the right, a mean and standard deviation were less appropriate (7.72±2.81 out of 11) (Table 2). Forty-five percent of women did not feel confident in their ability to manage their diabetes. However, of the 63 women (50%) who believed they possessed adequate knowledge about how to manage diabetes, 57 (89%) felt confident in their ability to manage diabetes. Thirty-three percent of married women felt that their husband played a role in their decision to seek health care; most married women felt that their health-seeking behavior was a joint decision with their husbands, rather than an individual one.
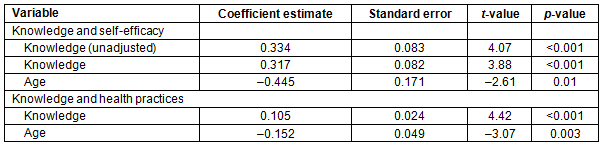
Knowledge scores were compared with self-efficacy scores. The age-adjusted multiple regression analysis demonstrated a significant correlation between knowledge and self-efficacy (p<0.001). It was found that every 1 unit increase in knowledge score was associated with a 0.32 unit increase in self-efficacy (Table 3). Age was the only significant confounder, as knowledge was typically higher among younger women. This was confirmed by both the bivariate analyses of each potential cofounder and the backwards selection GLM multivariate regression run in SAS (p=0.010).
Table 3 shows a secondary analysis that was conducted, which demonstrated that an increase in knowledge was correlated with more consistent glucose monitoring. Such consistent glucose monitoring was used as an indicator of better health practices. After adjusting for age, increased KAP score was associated with more regular glucose monitoring (p<0.001).
Table 2: Descriptive statistics for Diabetes Knowledge Attitude and Health-Seeking Practices Survey and standard deviation scores?
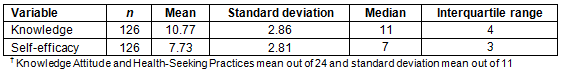
Table 3: Unadjusted bivariate analysis and age-adjusted multiple regression analysis. Knowledge was associated significantly with self-efficacy, as shown by both the unadjusted and age-adjusted analyses. Knowledge was also significantly associated with more consistent glucose monitoring, an indicator of better health practices
Discussion
Knowledge, self-efficacy and health practices
The study indicates that increase in type II diabetes knowledge is associated with an increase in women's self-efficacy and potentially leads to more consistent monitoring and maintaining desirable blood glucose levels, an indicator of better health practices. Though previous studies have not been explored self-efficacy and diabetes knowledge in rural Indian women, researchers have obtained similar findings. Previous studies suggest that knowledge of HbA1c testing leads to better glycemic control in patients with type II diabetes22. Additionally, increased knowledge of diabetes retinopathy among rural Indian populations has been shown to positively affect patients' attitude and practice17.
The average KAP score of 45% also demonstrates an alarming diabetes knowledge deficit in the rural women in Rajpur and Valam villages. Though women are aware of their diabetic status and know the term 'diabetes', they have common misconceptions about its causes, complications and treatment procedures. These misconceptions likely arise from discussion among village members about the disease. The use of methi, plants, and religious bracelets as treatment procedures for diabetes suggests the reliance on homemade or Ayurvedic medications to address the growing burden of disease. The perception that living a more sedentary lifestyle alleviates the symptoms of diabetes demonstrates an inherent misunderstanding of the nature of diabetes and its complications. Though genetics were not recognized as a key factor in diabetic status, women still felt they could not protect their children or family members from the disease by education or lifestyle changes, further indicating the general lack of awareness in the population. Though overall women possessed little knowledge about the various health complications that arise from diabetes, most did recognize the swelling of the feet (peripheral neuropathy) as a key manifestation of the disease. Though this is a neurological symptom of the disease, neuropathy's physical pain and apparent visual characteristics made women more likely to recognize it as a cause of diabetes. Women did not commonly attribute heart and kidney problems to diabetes, perhaps because these symptoms do not necessarily have physically visible manifestations.
Notably, during the survey administration, many women openly admitted that they had no idea of the correct answer to many of the questions. For instance, when asked about tobacco's influence on diabetes, women responded uncertainly that because chewing tobacco helped them relax and de-stress, it could be used to treat diabetes. This suggests that the one misconception, that diabetes can be a direct result of 'tension' and worrying, perpetuates other misconceptions.
In addition to the lack of adequate knowledge, women possessed a self-efficacy level that was only slightly above average, and half of the respondents reported they did not feel confident in managing their diabetes. Interestingly, most women who felt they had sufficient knowledge about diabetes also reported that they felt confident in their ability to manage their diabetes every day. Results also demonstrate that knowledge has a small, yet significant, impact on self-efficacy, further validating previous studies that suggest knowledge helps empower patients to maintain a healthier lifestyle2,16. Just as the Health Belief Model suggests, addressing women's diabetes knowledge likely affects their confidence in being able to manage the disease.
Results of this study also show that women with better diabetes knowledge monitor their blood glucose levels more frequently, demonstrating better health practices. This is supported by the Health Belief Model, which suggests knowledge leads to favorable health behaviors.
Strengths and limitations
Though the study design explores the relationships between knowledge and self-efficacy, and knowledge and health practices, it does not address the relationship between self-efficacy and health-seeking behaviors, which is also supported by the Health Belief Model. Because the study population was obtained by approaching health clinics, health-seeking behaviors were expected to be slightly skewed. This was because most participants had already visited the clinic, suggesting they already possessed some health-seeking behaviors. Additionally, the time since diagnosis with diabetes was not known for the women; this may have been a possible confounder, as women who know about their diabetic status for a longer period of time may possess more knowledge about the disease. Future studies across a wider range of villages in India should therefore not only explore this relationship between self-efficacy and health-seeking behaviors, but also address possible confounders in knowledge levels. Conducting a similar study in men could also be beneficial to make more direct comparisons between the two genders and their knowledge levels.
The use of non-probability sampling was another inherent limitation of the study, and resulted from the 'hidden' nature of the female diabetic study population that was restricted to the Mehsana District in Gujarat due to feasibility. However, the study successfully conducted a census of all the known females with diabetes in the two villages with the highest reported cases of diabetes at PHC level in the district.
Because this is the first analysis that addresses knowledge and self-efficacy in rural Indian women, the DES-SF measure had to be adapted from the Michigan Research Training Program's initial scale and tailored to the specific population. For this reason, this self-efficacy scale was used for the first time in Gujarat.
While the CDP has initiated efforts of strengthening rural response to diabetes through public healthcare services, its impact on awareness generation is yet to be evaluated. The findings from the present study indicate that women are not fully aware of its specific causes, complications and treatments, which have perpetuated certain misconceptions. This is especially an issue in a population where diabetes rates are increasing. For this reason, large-scale diabetes educational interventions targeted specifically to women should be undertaken in villages. Since the CDP previously addressed physicians and healthcare professionals, future educational interventions should utilize a more grassroots approach by following up and providing supportive supervision to grassroots health workers, such as Accredited Social Health Activist workers, who directly work in the villages each day with the women. Future studies should also explore the determinants of higher levels of self-efficacy exhibited by some of the study participants.
Lastly, in addition to the study findings, personal interactions with the women research subjects also led the authors to believe that female-centric diabetes interventions could have immense impacts on women's knowledge, self-efficacy and, eventually, health practices.
Acknowledgements
The authors would like to acknowledge Dr Kristina Talbert-Slagle of the Yale University Global Health Leadership Institute for her review of and incredible support of the research proposal from its inception, Dr Elizabeth Bradley of the Yale University Global Health Leadership Institute for her critical expertise and content review of the manuscript, the Yale University Center for International and Professional Experience and Yale South Asian Studies Council for their financial and material support, and Archana Shrimali for all survey administration to study participants.
References
1. Wild S, Roglic G. Global prevalence of diabetes estimates for the year 2000 and projection for 2030. Diabetes Care 2004; 27: 1047-1053.
2. Bajaj S, Jawad, F, Islam N, Mahtab H, Bhattarai J, Shrestha D et al. South Asian women with diabetes: psychosocial challenges and management: consensus statement. Indian Journal of Endocrinology Metabolism 2013; 17(4): 548-562.
3. International Diabetes Federation. IDF Diabetes Atlas update 2014. 6th edn, Brussels: International Diabetes Federation, 2014.
4. International Diabetes Federation. IDF Diabetes Atlas. 6th edn, Brussels: International Diabetes Federation, 2013.
5. Misra P, Upadhyay RP, Misra A, Anand K. A review of the epidemiology of diabetes in rural India. Diabetes Research and Clinical Practice 2011; 92(3): 303-311.
6. Balagopal P, Kamalamma N, Patel TG, Misra R. A community-based diabetes prevention and management education program in a rural village in India. Diabetes Care 2008; 31(6): 1097-1104.
7. Vaz NC, Ferreira AM, Kulkarni MS, Vaz FS. Prevalence of diabetes mellitus in a rural population of Goa, India. National Medical Journal of India 2011; 24(1): 16-18.
8. Ramachandran A, Snehalatha C, Latha E, Manoharan M, Vijay V. Impacts of urbanisation on the lifestyle and on the prevalence of diabetes in native Asian Indian population. Diabetes Research and Clinical Practice 1999; 44(3): 207-213.
9. Deepa M, Bhansali A, Anjana RM, Pradeepa R, Joshi SR, Joshi PP et al. Knowledge and awareness of diabetes in urban and rural India: The Indian Council of Medical Research India Diabetes Study (Phase I): Indian Council of Medical Research India Diabetes 4. Indian Journal of Endocrinology Metabolism 2014; 18(3): 379.
10. Bandura A. Self-efficacy: toward a unifying theory of behavioral change. Psychological Review 1977; 84(2): 191.
11. Joshi A, Mehta S, Grover A, Talati K, Malhotra B, Puricelli Perin DM. Knowledge, attitude, and practices of individuals to prevent and manage metabolic syndrome in an Indian setting. Diabetes Technology and Therapeutics 2013; 15(8): 644-653.
12. Venkataraman K, Kannan AT, Kalra OP, Gambhir JK, Sharma AK, Sundaram KR et al. Diabetes self-efficacy strongly influences actual control of diabetes in patients attending a tertiary hospital in India. Journal of Community Health 2012; 37(3): 653-662.
13. Raithatha SJ, Shankar SU, Dinesh K. Self-care practices among diabetic patients in Anand District of Gujarat. ISRN Family Medicine 2014; 2014: 743791.
14. Hayden JA, Health Belief Model. In: Introduction to health behavior theory. Burlington, MA: Jones & Bartlett Learning, 2013.
15. Shamsi M, Sharifirad G, Kachoyee A, Hassanzadeh A. The effect of educational program walking based on health belief model on control sugar in woman by type 2 diabetics. Iranian Journal of Endocrinology and Metabolism 2009; 11(5): 490-499, 597.
16. Hermanns N, Kulzer B, Ehrmann D, Bergis-Jurgan N, Haak T. The effect of a diabetes education programme (PRIMAS) for people with type 1 diabetes: results of a randomized trial. Diabetes Research and Clinical Practice 2013; 102(3): 149-157.
17. Rani PK, Raman S, Subramani S, Perumal G, Kumaramanickavel G, Sharma T. Knowledge of diabetes and diabetic retinopathy among rural populations in India, and the influence of knowledge of diabetic retinopathy on attitude and practice. Rural and Remote Health (Internet) 2008; 8: 838. Available: www.rrh.org.au (Accessed 23 August 2015).
18. IIPHG. Conquer Diabetes Project: status report. Gandhinagar, Ahmedabad: Indian Institute of Public Health, 2015.
19. Trivedi M, Kumar G, Saxena D. Diabetic care through public private partnership in rural setup: a case study of Primary Health Centre Valam. Gandhinagar, Ahmedabad: Indian Institute of Public Health, 2015.
20. ISPM - University of Bern. STROBE Statement (Internet). 2009. Available: http://www.strobe-statement.org (Accessed 22 November 2014).
21. Anderson RM, Funnell MM, Fitzgerald JT, Marrero DG. The Diabetes Empowerment Scale: a measure of psychosocial self-efficacy. Diabetes Care 2000; 23(6): 739-743.
22. Kumpatla S, Medempudi S, Manoharan D, Viswanathan V. Knowledge and outcome measure of HbA1c testing in Asian Indian patients with type 2 diabetes from a tertiary care center. Indian Journal of Community Medicine 2010; 35(2): 290-293.
