Historically, access to health services, particularly for the rural population and low income groups, has posed a major challenge for healthcare systems worldwide1-4. Globally, healthcare systems distinguish health inequalities as their top priority and continually aim at ensuring an equitable distribution of health services5. While it is practically impossible to provide similar access to services for everyone, the aim of such measures is to ensure a fair and just distribution of resources based on population needs6,7. Despite these efforts, disparities in accessing health and oral health services continue to be experienced by rural communities worldwide, including in Canada3,4,8-10. Therefore, due to inadequate access and underutilization of oral health services, rural communities experience poorer oral health than the general population9,11,12.
Rural communities are highly dependent upon neighboring larger rural cities and urban centers for obtaining health services, particularly specialist care13. It is observed that factors such as excessive travel time and long distances significantly hamper accessibility to services14-16, especially for older adults. In addition, various factors such as geographical isolation, socioeconomic deprivation, underprovided public structures, shortage of workforce and limited availability of oral health services negatively affect access to care in rural areas9,10,17.
In Canada, the magnitude of the challenge faced can be appreciated by the fact that one out of every five Canadians lives in rural areas, representing almost a quarter (18.9%) of the country's population18. Moreover, the Canadian rural population is spread over 95% of the country's expansive landmass, making accessibility particularly cumbersome18. Providing oral health services and equitable access to dental care evolves into a bigger challenge for the health authorities as the rural population ages, making prevention and treatment of oral diseases even more complicated19,20.
To address rural and urban oral health disparities and ensure equitable distribution of services it is crucial to address the factors that constitute spatial and non-spatial dimensions of access21,22. The average number of practitioners per head of the population and their geographical distribution can provide an appropriate measure for reliable prediction of accessible services23. The objective of this study was to examine and map the distribution pattern of dental workforce (dentists, denturists and dental technicians) in the province of Quebec, Canada using a geographical information system (GIS), open-source global positioning system (GPS) visualizer (Schneider A; http://www.gpsvisualizer.com).
For the purpose of this study, GIS techniques were used to map Quebec's dental workforce. A Census Metropolitan area (CMA) or a Census Agglomeration (CA) is formed by one or more adjacent municipalities around a population center. A CMA has a population of 100 000 or more, with a core population of at least 50 000, whereas the core population of a CA is at least 10 00024. Urban zones were considered to be CA in the present study.
Areas defined as rural and small towns are not part of a CMA or CA24. These areas are defined by Statistics Canada as Census Metropolitan and Census Agglomerated Influenced Zones (MIZ) based upon population density, distance and commuting flow; from rural areas to large centers, and from residences to workplaces25. This index illustrates the degree of influence that urban areas had over rural areas in the 2001 and 2006 censuses. In this study, zones are categorized into five subsets: urban zones, strongly influenced zones, moderately influenced zones, weakly influenced zones, and not influenced zones. A zone is categorized as 'strong MIZ' if 30% or more of its workforce has a place of work in the CMA or CA. A zone where less than 5% of the workforce has a place of work in the CMA or CA is categorized as weak MIZ24,25. The term MIZ is used interchangeably with 'metropolitan-influenced zone' for the purpose of this study.
Utilizing the most updated database available at the time of the study, personal information for all active members of the Quebec dental workforce (dentists, denturists and dental technicians), such as data on gender, practice locations, type of practice and license issue date, were obtained from the membership directory of Quebec Professional Order (2009-2010). Geographical attributes of divisions and census subdivisions in Quebec such as professional localization and regional context were obtained from Statistics Canada. Reverse geocoding of Quebec dental workforce ZIP codes provided by Quebec Professional Orders was used to find textual location from geographic coordinates by means of an open source GPS visualizer. The forward sortation area, corresponding to only the first three characters of postal codes, was used to determine their location26. Using this spatial location of the dental workforce the 'theoretical served area' by each dental professional in each census division was determined in order to represent the relationship between territory and concentration of dental workforce. This was presented as km2/dental professional.
Analysis
The Statistical Package for the Social Sciences v17 for Windows (SPSS; http://www.spss.com.au) was used to perform descriptive statistics. Normality of data distribution was assessed with the Shapiro-Wilk test. A two-sample t-test was used to compare dentist-to-population ratios between urban zones and others. The Mann-Whitney U-test was used to compare license issue year between urban zones and others. Fisher's exact test was used to compare gender of health professionals and distribution of general dentist and specialist between urban zones and others. ArcGIS v9.3 (ESRI; http://www.arcgis.com/features) was used for analyzing MIZ data available from the Community Information Database, an interactive mapping tool offered by the Government of Canada. Cartography layers were extracted from a geospatial database, Géogratis, provided by Canada Natural Resources.
Ethics approval
This research was exempt from institutional review board review at l'Université de Montréal's Ethic Research Office according to the article 2.2 of the Tri-council policy statement: ethical conduct for research involving humans-2014 (http://www.pre.ethics.gc.ca/eng/policy-politique/initiatives/tcps2-eptc2/chapter2-chapitre2), because the information was publicly accessible and there was no reasonable expectation of privacy.
The superimposition of geographic MIZ typology and geographic distribution of the dental workforce revealed statistically significant differences in the distribution of the dental workforce in rural and urban areas.
Figure 1 is a map of the availability of dental workforce by 5000 inhabitants in Quebec's census divisions. The index average for each census division was used and rounded off to obtain values from 1 to 6. This map illustrates a dental workforce-to-population ratio of 1:3300 in rural areas, compared to a ratio of 1:2283 in urban areas in 2009. Urban zones such as Montreal, Quebec and Sherbrooke had a higher workforce availability (4-6 dentists for every 5000 people). Figure 2 depicts the geographic distribution of the Quebec dental workforce according to MIZ in census subdivisions. The difference in the distribution of dental workforce in urban and rural areas was statistically significant (urban 59.4±19.4/100 000 vs rural 39.9±17.6/100 000; p<0.001). Most of the workforce was located in either one of the three urban cities Montreal, Quebec and Sherbrooke.
The distribution of the dental workforce by MIZ is shown according to sex in Table 1, and according to license issue dates in Figure 3 and Table 2. While the workforce comprised a higher proportion of men (61.8%), the distribution of the dental workforce was not influenced by sex (p=0.15) or license issue date (p=0.11). Figures 1 and 2 also shows that the dental workforce for 5000 residents is higher in weak MIZ than that in strong MIZ (Le-Haut-Saint-François and Vallée-de-la-Gatineau with less than 1 dentist/5000 residents, and Nord-du-Québec, Manicouagan and Le Fjord-du-Saguenay with 2-4 dentists/5000 residents).
Table 3 shows the distribution of general dentists and specialists by MIZ. Approximately 90.3% of the dental workforce (general dentists and specialists) was located in urban census subdivisions, 1.3% in the zones strongly influenced by metropolitan area, and 4.9% in the moderately influenced zones. Only 0.3% of the combined general dentists and specialists was located in non-metropolitan-influenced zones. Even though there was a higher distribution of general dentists in urban zones (89.3%), a small number were present in all MIZ. In contrast, 98.9% of specialists were located only in urban areas (p<0.001). Out of a total of 447 dental specialists in Quebec, only five were located in rural areas.
Figure 4 presents the theoretical served area by the dental workforce in Quebec's census divisions. The surface areas covered by a dental professional in rural areas was 1000-25 000 km2 in contrast to 1-10 km2 in urban regions. Note that the served area is based on theoretical estimation and a dental professional did not physically cover these zones.
Table 1: Distribution of dental workforce by metropolitan-influenced zones according to sex
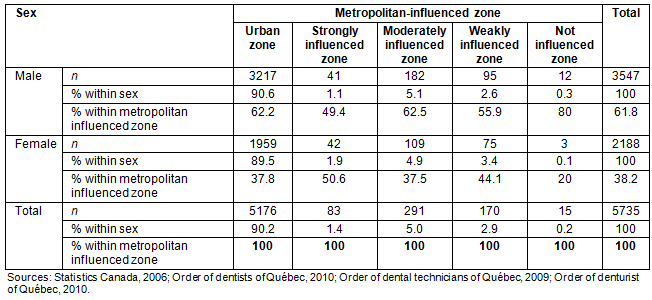
Table 2: Distribution of general dentists and specialists by metropolitan-influenced zones according to license issue date
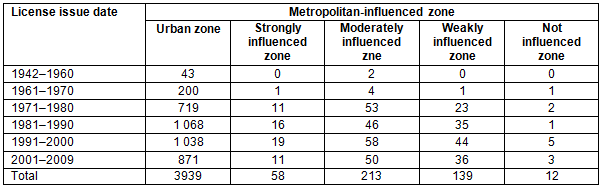
Table 3: Distribution of general dentists and specialists by metropolitan-influenced zones
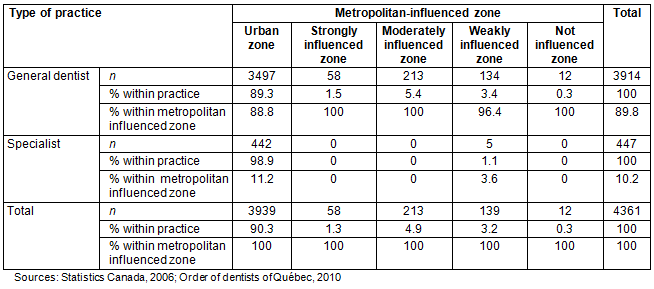
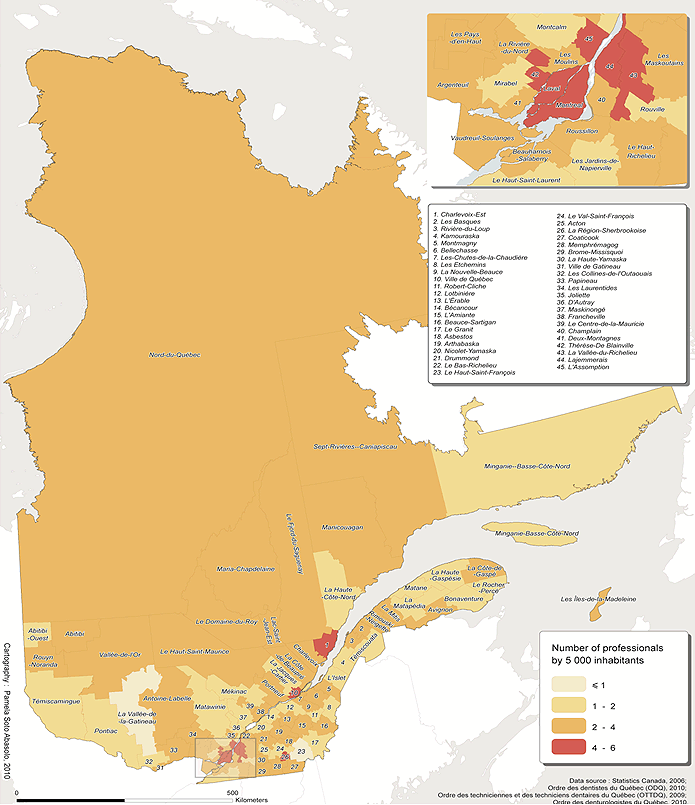
Figure 1: Dental workforce availability by 5000 inhabitants in Quebec's census divisions.
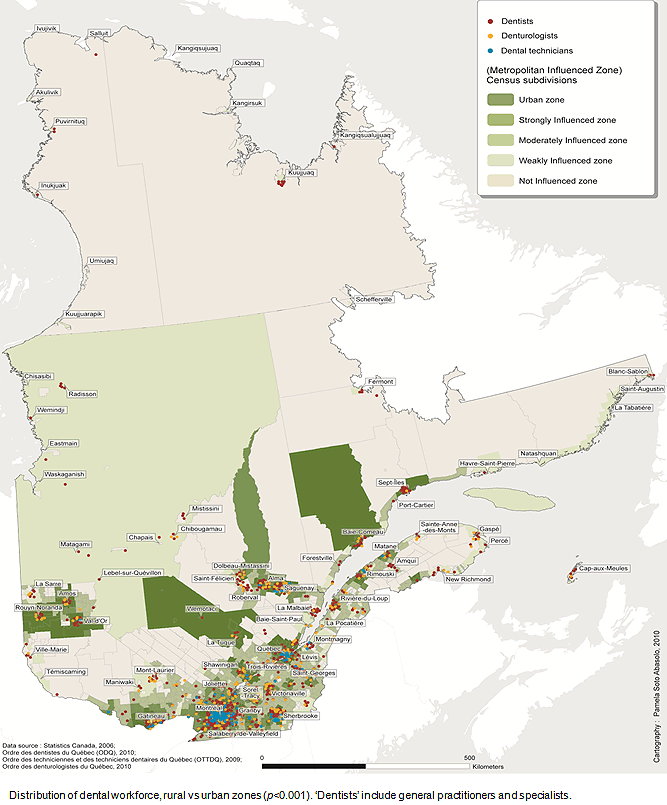
Figure 2: Geographic distribution of Quebec dental workforce according to metropolitan-influenced zones.
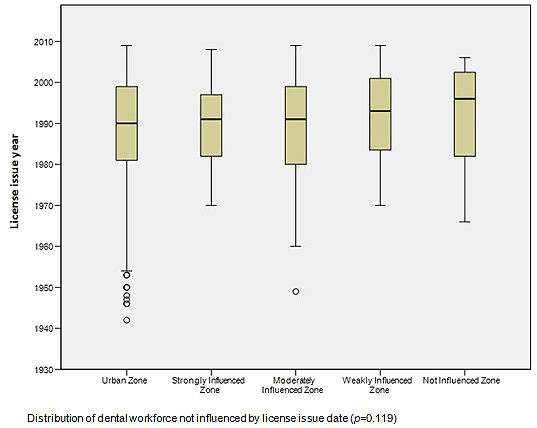
Figure 3: Distribution of general dentists and specialists by metropolitan-influenced zones according to license issue year.
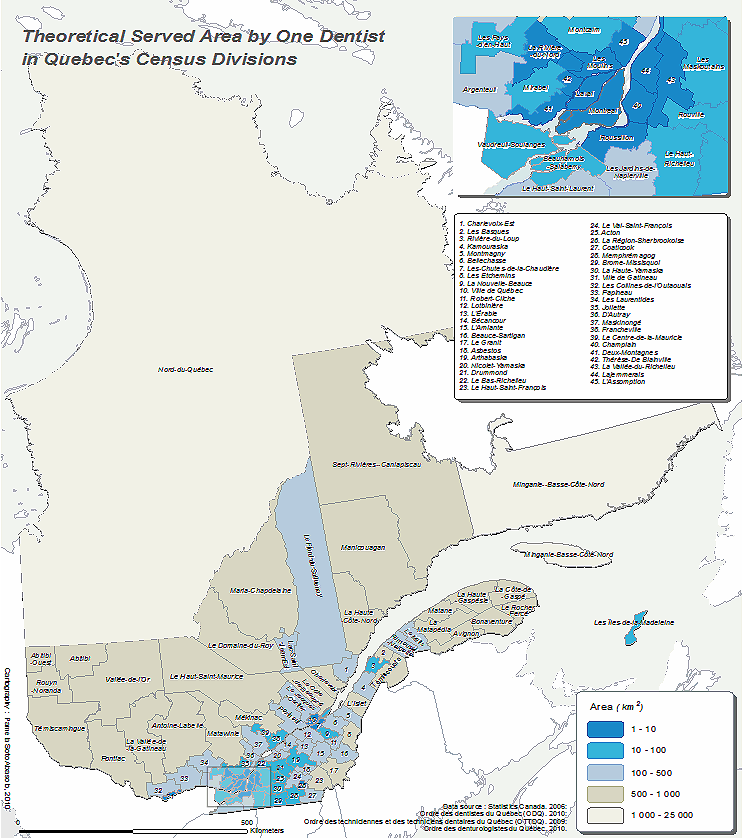
Figure 4: Theoretical served area by one dentist in Quebec's census divisions.
Discussion
The present findings are consistent with previous studies on the shortage of dental professionals in rural areas27,28. Unequal distribution of oral health services and distance barriers may negatively influence health perception and health behaviors in rural areas because of a lack of ease of access and unavailability of adequate education and information provided by oral health professionals10,18,29. It is observed that most of the dental workforce prefer to practice in urban areas like Montreal, Quebec and Sherbrooke. Factors that may contribute to these professional preferences might be related to demanding working conditions, substandard facilities, inadequate remuneration and fewer career enhancement opportunities in rural areas30. Similar patterns were also observed comparing general dentists and specialists. This professional predicament is the result of a higher diversification of clinical cases, exploitable interprofessional communication and opportunities for professional growth in urban cities31. Consequently, the area covered by a dentist in rural areas is 1000-25 000 km2, in contrast to 1-10 km2 in urban regions as seen in Figure 4.
The inhabitants of strong MIZ areas are closer to urban zones and can seek oral healthcare services more easily than those in weak or non-MIZ areas. In weak or non-MIZ areas, access to dental care may be challenging due to population dispersion and long travelling distances. Despite these barriers, some of the rural regions in weak MIZ areas had a higher ratio of dentists/5000 residents than those lying close to strong MIZ zones. This unusual observation could be best associated with professional motivation to practice in cities, where the demand for services is greater. However, on a larger scale only 0.3% of the dental workforce was found to be located in non-metropolitan-influenced zones, posing a great challenge to the oral healthcare system. The results highlight the need for a larger dental workforce to be scattered throughout the territory, even in the absence of a high-density population. The theoretical served area by one dental professional in Quebec's census divisions substantiates the MIZ distribution of oral healthcare professionals whilst supporting this lack of dental workforce in rural areas.
In Quebec, a male dental workforce is more common, perhaps due to past perceptions of dentistry as a male-dominated career. However, the perception of a male dental workforce is changing. Even though the results suggest that the distribution of dental workforce was not influenced by sex or license issue date, popularization of the dental field among women may cause change. According to the literature, on average female practitioners work fewer clinical hours, are less entrepreneurial, and are more likely to work in urban zones32,33, thus not significantly contributing to improvement of the dental workforce-to-population ratio in rural areas. Policy makers and health planners need to implement strategies that encourage dental workforce to benefit from the advantages of living and working in rural areas, thus improving access to care for rural residents10. Furthermore, there is a need for academic policies to educate and facilitate the process to increase the knowledge and motivation of dental students in regard to community-based and patient-centered practice in rural areas34,35.
In order to improve rural oral health it is important to examine and understand how rural environment and dental workforce shortage impact the healthcare needs of the population. GIS and related spatial analysis methods provide a useful tool for exploring the delivery of health care along with understanding the relationship between access and oral health outcomes36. This study generalizes the location of workforce and may be less accurate than six-character postal codes. Nevertheless, the methodology employed reports the spatial distribution of professionals throughout Quebec with better accuracy than previously reported. Based on the available data and the methodology used, it is difficult to ascertain the shortage of dental workforce and services in rural Quebec. The data needs to be analyzed with a finer division of territory (perhaps using subdivisions) to get more accurate results. Figures 2 and 4 were not created with these divisions due to missing and incompatible data. Further analysis of professional distribution variables is required to identify the needs of dental care in rural Quebec.
The study, at the time of being conducted in 2010, utilized the most up-to-date data available for the years 2009-2010. It is therefore difficult to ascertain how the distribution of the dental workforce has changed over the course of last few years. Monitoring the distribution of healthcare workforce has the potential to assist policy makers in planning effective healthcare strategies to improve access to dental care. Future research aimed at utilizing a spatial approach to explore and understand population characteristics and barriers to access to care is needed.
This study concludes that there is a lack of oral healthcare workforce in rural Quebec, particularly a shortage of specialists. Indeed, there is a strong relationship between the degree of urbanization and the highest concentration of dental professionals. However, further in-depth research is needed to examine how this distribution pattern might contribute to poorer oral health outcomes.
Acknowledgements
The authors acknowledge Mrs Pamela Abasolo for her significant role in the methodological aspects of the maps produced. This study was supported by a grant from the Network for Oral and Bone Health Research and Fonds de recherche du Québec - Santé. Dr Emami is supported by the Canadian Institutes of Health Research Clinician Scientist Salary Award, entitled Investigating urban-rural disparities in oral health and oral health services: a Quebec profile.
References
1. Locker D, Ford J. Using area-based measures of socioeconomic status in dental health services research. Journal of Public Health Dentistry 1996; 56(2): 69-75.
2. Knapp KK, Hardwick K. The availability and distribution of dentists in rural ZIP codes and primary care health professional shortage areas (PC-HPSA) ZIP codes: comparison with primary care providers. Journal of Public Health Dentistry 2000; 60(1): 43-48.
3. Kulig JC, Williams AM. Health in rural Canada. Vancouver: UBC Press, 2011.
4. Sibley LM, Weiner JP. An evaluation of access to health care services along the rural-urban continuum in Canada. BMC Health Services Research 2011; 11: 20.
5. Epp J. Achieving health for all: a framework for health. Ottawa, ON: Health and Welfare Canada, 1986.
6. National Collaborating Centre for Aboriginal Health. Access to health services as a social determinant of First Nations, Inuit and Métis Health. Prince George, BC: National Collaborating Centre for Aboriginal Health, 2011.
7. Bowen S. Access to health services for underserved populations in Canada. In 'Certain circumstances': issues in equity and responsiveness in access to health care in Canada. A collection of papers and reports prepared for Health Canada. Ottawa, ON: Health Canada, 2000.
8. Pong RW, DesMeules M, Heng D, Lagacé C, Guernsey JR, Kazanjian A. Patterns of health services utilization in rural Canada. Chronic Diseases and Injuries in Canada 2011; 31(Suppl 1): 1-36.
9. Emami E, Feine JS. Focusing on oral health for the Canadian rural population. Canadian Journal of Rural Medicine 2008; 13(1): 36-38.
10. Emami E, Wootton J, Galarneau C, Bedos C. Oral health and access to dental care: a qualitative exploration in rural Quebec. Canadian Journal of Rural Medicine 2014; 19(2): 63-70.
11. McDonald JT, Conde H. Does geography matter? The health service use and unmet health care needs of older Canadians. Canadian Journal of Aging 2010; 29(1): 23-37.
12. Canadian Dental Association. Position paper on access to oral health care for Canadians. Ottawa, ON: Canadian Dental Association, 2010.
13. Goodman DC, Fisher E, Stukel TA, Chang C. The distance to community medical care and the likelihood of hospitalization: is closer always better? American Journal of Public Health 1997; 87(7): 1144-1150.
14. Edelman MA, Menz BL. Selected comparisons and implications of a national rural and urban survey on health care access, demographics, and policy issues. Journal of Rural Health 1996; 12(3): 197-205.
15. Brustrom JE, Hunter DC. Going the distance: how far will women travel to undergo free mammography? Military Medicine 2001; 166(4): 347-349.
16. Chan L, Hart LG, Goodman DC. Geographic access to health care for rural Medicare beneficiaries. Journal of Rural Health 2006; 22(2): 140-146.
17. Bushy A. Needed: quality improvement in rural health care. Australian Journal of Rural Health 2005; 13(5): 261-262.
18. Statistics Canada. Canada's rural population since 1851: population and dwelling counts, 2011 Census. Ottawa, ON: Statistics Canada, 2012.
19. Susi L, Mascarenhas AK. Using a geographical information system to map the distribution of dentists in Ohio. Journal of American Dental Association 2002; 133(5): 636-642.
20. Paez A, Mercado RG, Farber S, Morency C, Roorda M. Accessibility to health care facilities in Montreal Island: an application of relative accessibility indicators from the perspective of senior and non-senior residents. International Journal of Health Geographics 2010; 9: 52.
21. Penchansky R, Thomas JW. The concept of access: definition and relationship to consumer satisfaction. Medical Care 1981; 19(2): 127-140.
22. Delamater PL, Messina JP, Shortridge AM, Grady SC. Measuring geographic access to health care: raster and network-based methods. International Journal of Health Geographics 2012; 11(1): 15.
23. Gulliford M, Figueroa-Munoz J, Morgan M, Hughes D, Gibson B, Beech R. What does 'access to health care' mean? Journal of Health Services Research and Policy 2002; 7(3): 186-188.
24. Statistics Canada. CMA and CA: detailed definition. (Internet) 2013. Available: http://www.statcan.gc.ca/pub/92-195-x/2011001/geo/cma-rmr/def-eng.htm (Accessed 21 November 2014).
25. du Plessis V, Beshiri R, Bollman RD, Clemenson H. Definitions of 'rural' (Internet) 2002. Available: http://EconPapers.repec.org/RePEc:ags:scarwp:28031 (Accessed 21 November 2014).
26. Canada Post Corporation. Canada Post addressing guidelines. (Internet) 2013. Available: http://www.canadapost.ca/tools/pg/manual/pgaddresse.asp (Accessed 24 July 2013).
27. Research RiFo. What can the census tell us about Canada's dental workforce? Sudbury, ON: Centre for Rural and Northern Health Research, 2008.
28. Cane R, Walker J. Rural public dental practice in Australia: perspectives of Tasmanian government-employed dentists. Australian Journal of Rural Health 2007; 15(4): 257-263.
29. Macintyre S, Ellaway A, Cummins S. Place effects on health: how can we conceptualise, operationalise and measure them? Social Science and Medicine 2002; 55(1): 125-139.
30. Grobler L, Marais BJ, Mabunda SA. Interventions for increasing the proportion of health professionals practising in rural and other underserved areas. Cochrane Database of Systematic Reviews 2009; (1): CD005314.
31. Drugan CS, Chestnutt IG, Boyles JR. The current working patterns and future career aspirations of specialist trainees in dentistry. British Dental Journal 2004; 196(12): 761-765; discussion 759.
32. McKay JC, Quinonez CR. The feminization of dentistry: implications for the profession. Journal of Canadian Dental Association 2012; 78: c1.
33. McKernan SC, Kuthy RA, Kavand G. General dentist characteristics associated with rural practice location. Journal of Rural Health 2013; 29(Suppl 1): s89-95.
34. McAndrew M. Community-based dental education and the importance of faculty development. Journal of Dental Education 2010; 74(9): 980-985.
35. Bailit HL, Beazoglou TJ, Formicola AJ, Tedesco LA. Financing clinical dental education. Journal of Dental Education 2008; 72(Suppl 2): 128-136.
36. Graves BA. Integrative literature review: a review of literature related to geographical information systems, healthcare access, and health outcomes. Perspectives in Health Information Management 2008; 5: 11.
