In the USA, an estimated 26% of adults and 13-20% of children experience a diagnosable mental disorder in a given year1,2. Mental health is an important public health issue as it is associated with chronic diseases as well as morbidity and mortality3. In 2003, the economic cost (including loss of productivity, disability benefits, and health expenditures) attributed to mental health disorders was estimated at US$300 billion4. The shortage and poor distribution of mental health professionals is a concern nationally, as it creates access to care issues for individuals in need of health care5,6. In 2004, the Annapolis Coalition on the Behavioral Health Workforce, with support from the Substance Abuse and Mental Health Services Administration, called for workforce development initiatives to expand mental health services and treatment for psychiatric disorders at the national level7.
Rural areas have complex challenges, and continue to show a gap between rural and urban health disparities, especially in unmet mental health needs8-10. A review found that non-metropolitan individuals with more severe psychiatric disorders achieve worse outcomes over time than their metropolitan counterparts10. However, it is unknown what is attributing to the differences in mental health in metropolitan and non-metropolitan areas. Specific attention is needed to improve mental health outcomes in rural communities. Quantifying workforce supply and shortages can aid in identifying areas in need of the recruitment, training, licensure, and retention of behavioral health professionals. However, workforce analyses have presented a challenge as comprehensive workforce data is limited. In 2009, a study used county-level data from certification counts from credentialing organizations as well as membership counts from professional associations to estimate the supply of groups of mental health professionals11. While the study provided a national picture of the supply of mental health professions, the data sources had limitations to provide accurate estimates. Mainly, licensing, credentialing, and membership counts do not accurately reflect the number of actively practicing providers. Furthermore, studies have highlighted the need for data that includes specific practice information, such as location and specialty11,12.
Nebraska is ahead of most states in terms of workforce data collection, and rural and frontier counties cover the majority of the state. The University of Nebraska Medical Center's (UNMC) Health Professions Tracking Service (HPTS) has been tracking actively practicing health professionals in Nebraska since 1995 through annual surveys. Additionally, practice locations for physicians, advanced practice registered nurses (APRNs), and physician assistants are surveyed semi-annually to update the current status of their practice. HPTS maintains a rich repository of continuously updated information on healthcare providers, including demographic characteristics, education and training, expertise, languages spoken fluently, retirement plans, primary practice locations, and satellite offices.
In 2004, Nebraska's behavioral health system underwent a major reform with the passage of legislative bill (LB) 1083. LB 1083 required a transition from institutionalized care to community-based care resulting in a significant increase in the number of people with mental illness receiving care close to their home in both rural and urban communities13,14. In order to address the significant changes in Nebraska, it is crucial to facilitate the collection, analysis, and dissemination of behavioral health workforce data as it aids in planning efforts, such as prioritizing the training and recruitment of behavioral health professionals.
This study provides a snapshot of the county-level supply of licensed and certified behavioral health professionals (psychiatrists, nurse practitioners, physician assistants, psychologists, licensed independent mental health practitioners, licensed mental health practitioners, and addiction counselors) actively practicing in Nebraska in 2012, using data obtained from the HPTS annual survey database. This study also examines the relationship between the supply of behavioral health professionals and county characteristics.
Study population
The study population included all 93 counties in Nebraska. Using the 2003 Federal Office of Management and Budget designation of metropolitan counties and the 2008 Department of Health and Human Services definition of 'frontier' (ie less than or equal to 6 persons/mi2; 2.3 persons/km2), there were 9 metropolitan, 49 rural, and 35 frontier counties in Nebraska in 2012 (Fig1). Nebraska also has six behavioral health regions as defined by LB 1083, where every county belongs to one of the six regions.
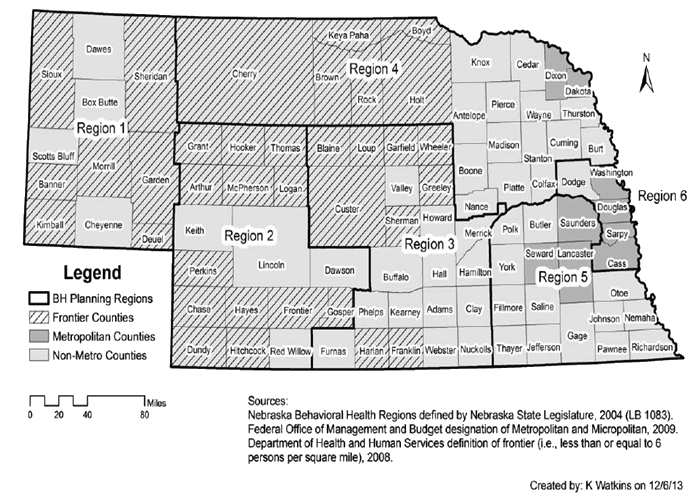
Figure 1: Nebraska counties and behavioral health regions, 2012.
Data source
This study used UNMC's HPTS data for 2012. HPTS maintains a database of Nebraska's licensed healthcare professionals including behavioral health professionals. HPTS surveys health professionals annually using the Nebraska licensure database as the sampling frame. In addition, practice locations for physicians, APRNs, and physician assistants are surveyed semi-annually. The surveys are pre-populated with previously identified practice information for professionals, and provide professionals the opportunity to update their information with each survey. The response rate of the survey was 50%. Non-respondents may have included individuals that are still practicing in the state but did not respond, individuals that relocated to practice outside of the state, individuals not actively practicing, or individuals that have retired. HPTS also contacts the healthcare facilities to verify and document the practice locations and contact information of non-respondents for psychiatric prescribers. Of the psychiatric prescribers that did not respond, 86% were verified by contacting their practice location. Professionals' current status and historical cumulative responses are documented in the HPTS tracking system. This additional data from the surveys provide data more comprehensive and information more current than what is available through the Nebraska licensure bi-annual licensure renewal process.
This study consisted of the following categories of behavioral health professionals: psychiatric prescribers, independent behavioral professionals, and other behavioral health professionals (Fig2). Behavioral health professionals who had an active license to practice in Nebraska in 2012 and who had a primary and/or satellite practice location in Nebraska were included in this study. Behavioral health professionals who had provisional licenses in 2012 were excluded from this study.
Actively practicing psychiatrists consisted of board-certified (by the American Allopathic Board of Neurology and Psychiatry or the American Osteopathic Board of Neurology and Psychiatry) or board-eligible allopathic or osteopathic physicians. The definition of 'psychiatrist' was consistent with the federal mental health professional shortage area (HPSA) designated by the Health Services and Resources Administration's definition. Actively practicing APRNs and physician assistants practicing psychiatric mental health consisted of those who self-identified psychiatry as their primary or secondary practice specialty. Thus, APRNs practicing psychiatric mental health included both those who were and were not board-certified in psychiatry. APRNs who were board certified in psychiatric mental health nursing held a national board certification from the American Nurses Association.
Independent behavioral professionals and other behavioral professionals may hold more than one license. Psychologists included those who held a license to practice psychology and were actively practicing psychology. Independent mental health practitioners included those who were licensed and actively practicing as an independent mental health practitioner. Mental health practitioners included those who were licensed and actively practicing as a mental health practitioner. Addiction counselors consisted of licensed and actively practicing alcohol and drug counselors and/or certified compulsive gambling counselors.
Other secondary databases used to obtain county-level population and demographic characteristics for Nebraska included the US Census Bureau's 2012 Population Estimates, the 2012 American Community Survey, and the 2011 Small Area Income and Poverty Estimates data.
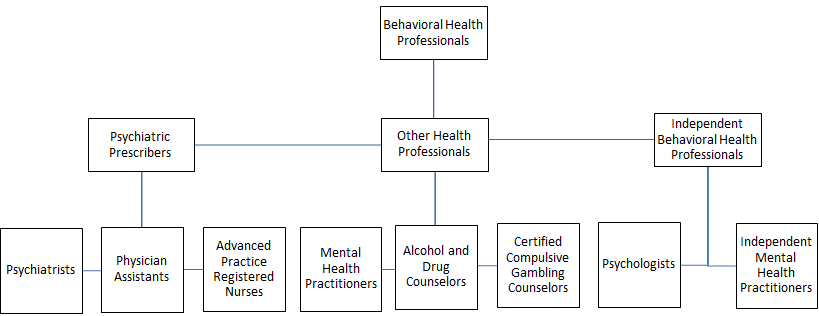
Figure 2: Behavioral health professionals included in the study.
Data analysis
The unit of analysis was the county. The geographic (ie metropolitan/rural/frontier) distribution of each group of behavioral health professionals was examined using descriptive statistics. Multivariate Poisson regression analyses, with the log of the county population size, were used to examine the relationship between the supply of behavioral health professionals and county-level characteristics (including whether or not in a metropolitan statistical area), behavioral health planning region, percentage of individuals in poverty, percentage of individuals aged ≥65 years, and percentage of individuals <18 years). The supply of behavioral health professionals was measured as a count variable. Poisson regression analyses estimated the scale parameter by the square root of deviance divided by the degrees of freedom to allow for over-dispersion. A sensitivity analysis was conducted using median household income to measure levels of poverty; however, the results did not change. All data were analyzed using SAS software v9.2 (SAS Institute Inc.; http://www.sas.com).
Ethics approval
The study received approval from the University of Nebraska Medical Center Institutional Review Board.
Table 1 shows the supply of behavioral health professionals by geographic location and profession. In 2012, there were 2468 behavioral health professionals actively practicing in Nebraska. A total of 243 (9.8% of the total behavioral health professionals) were categorized as psychiatric prescribers, 1038 (42.1%) as independent behavioral health professionals, and 1187 (48.1%) as mental health practitioners or addiction counselors. The overall ratio of actively practicing psychiatrists to 100 000 population was estimated to be 8.4 in 2012, which indicates that the supply is greater than the federal mental HPSA shortage designation ratio of 3.3 psychiatrists to 100 000 population15.
The majority (71.2%) of behavioral professionals in Nebraska were actively practicing in metropolitan areas as compared to 27.3% in rural areas and 1.5% in frontier areas. In metropolitan areas, there were 159.7 behavioral health professionals per 100 000 population (Table 1). Of the total actively practicing behavioral professionals in metropolitan areas, there were 181 (10.3%) psychiatric prescribers, 263 (15.0%) psychologists, 493 (28.0%) licensed independent mental health practitioners, 725 (41.2%) licensed mental health practitioners, and 96 (5.5%) addiction counselors. The overall ratio of actively practicing psychiatrists to 100 000 population in Nebraska's metropolitan areas was 11.7, which was greater than the federal mental HPSA shortage designation ratio15 (Table 1). The ratio of actively practicing psychologists to 100 000 population in metropolitan areas was 23.9 in 2012, which was greater than the average national supply of 1.9 psychologists per 100 000 population in metropolitan areas in 200611.
In rural and frontier areas, there were 94.0 behavioral health professionals per 100 000 population (Table 1). Of the total actively practicing behavioral health professionals in rural and frontier areas, 62 (8.7%) were psychiatric prescribers, 72 (10.1%) psychologists, 210 (29.6%) licensed independent mental health practitioners, 306 (43.1%) licensed mental health practitioners, and 60 (8.5%) addiction counselors. The overall ratio of actively practicing psychiatrists to 100 000 population in Nebraska's rural areas was 3.8, and that for frontier counties was 2.2 (Table 1). The supply of psychiatrists in Nebraska's frontier areas was less than the federal mental HPSA shortage designation ratio15.
For all categories of professions, except physician assistants actively practicing psychiatric mental health, Nebraska's metropolitan areas had the highest ratio of provider to 100 000 population as compared to rural and frontier areas. Rural areas had a slightly higher ratio of 0.9 physician assistants to 100 000 population as compared to 0.5 physician assistants to 100 000 population in metropolitan areas (Table 1).
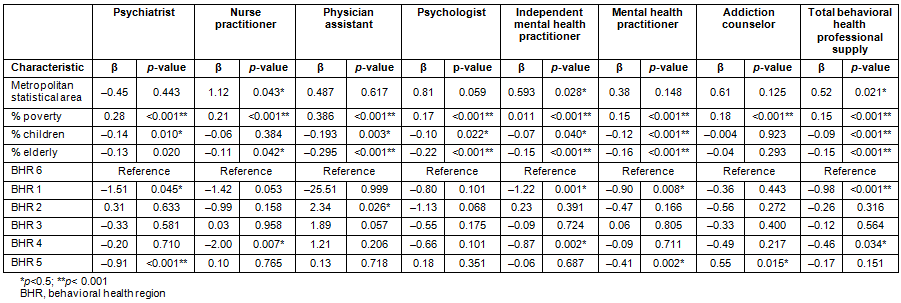
Table 2 shows the association between county characteristics and the total supply of behavioral health professionals. There was a significant positive association between the total supply of behavioral health professionals and metropolitan counties as well as the percentage of the population in poverty. On the other hand, there were significant negative associations between the total supply of behavioral health professionals and the percentage of children aged less than 18 years and the percentage of elderly people aged 65 years or older. The negative associations found between the total supply and behavioral health regions 1 and 4 suggest that behavioral health professionals were less likely to be actively practicing in regions 1 and 4 as compared to region 6.
Table 2 also shows the associations between county characteristics and specific behavioral health profession categories. Psychiatrists were less likely to be practicing in counties with a higher percentage of children aged less than 18 years and elderly people aged 65 years or more. There were geographical differences, where psychiatrists were also less likely to be practicing in behavioral health regions 1 and 5, as compared to region 6. Nurse practitioners actively practicing in psychiatric mental health were more likely to be found in metropolitan counties and less likely to be found in counties with a higher percentage of elderly population. Psychologists were less likely to be practicing in counties with higher proportions of children and elderly individuals. Across all categories of behavioral health professionals, there was a significant positive association between the supply of actively practicing professionals and the percentage of the population in poverty.
Table 1: Association between behavioral health professional supply and county characteristics
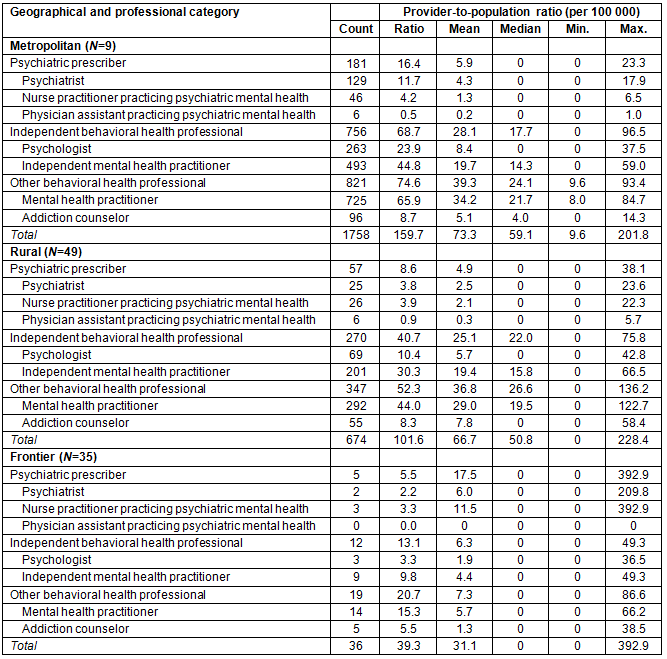
Table 2: Geographic distribution of behavioral health professionals, Nebraska 2012
Discussion
The findings from this study indicate that Nebraska suffers from a poor geographic distribution in the supply of behavioral health professionals. For almost all categories of behavioral health profession, urban counties had a higher supply of providers as compared to rural and frontier counties, which is consistent with findings from other studies11,12,16. Urban counties in Nebraska had almost three times the number of actively practicing psychiatric prescribers and 2.5 times the number of non-prescribing behavioral health professionals than rural and frontier counties. A poor geographic distribution in the supply of behavioral health professionals is of particular concern as a significant proportion (40.6%) of Nebraska's residents live in rural or frontier areas. However, 28.8% of the total number of behavioral health professionals in Nebraska are actively practicing in these areas.
The ratio of actively practicing psychiatrists to 100 000 population in Nebraska's metropolitan counties was 11.7, which was greater than the federal mental HPSA shortage designation ratio15. This ratio also compared well with the national average supply of 10 psychiatrists per 100 000 population in metropolitan counties in 200511. The ratio of actively practicing psychiatrists to 100 000 population in Nebraska's rural counties was much lower than metropolitan counties at 3.9. The ratio was slightly greater than the federal mental HPSA shortage designation ratio15, and it compared well with the 2005 national average supply of four psychiatrists per 100 000 population in rural areas that were adjacent to metropolitan areas11. In Nebraska's frontier counties, the ratio was two psychiatrists per 100 000 population, which was less than the federal mental HPSA shortage designation ratio as well as the 2005 national average supply of providers in rural counties not adjacent to metropolitan areas11,15. These findings not only further highlight the poor geographic distribution of providers in Nebraska, but they also show that access-to-care issues are magnified in remote areas of Nebraska. Rural areas face other complexities that attribute to limited access to care for populations. Rural populations are more likely to be uninsured, less likely to have private insurance, more likely to have Medicaid or other public insurance, more likely to be in fair or poor health, and more likely to have a chronic condition17. Thirty-five of Nebraska's 93 counties are considered frontier counties, and more than 91 000 residents reside in frontier areas, which are scattered across the entire state of Nebraska.
The significant associations found between the supply of behavioral health professionals and county-level characteristics indicate that there may be some unmet mental healthcare needs among Nebraska's rural populations as well as child and elderly populations. While rural and urban residents have a comparable prevalence of mental health illnesses and disorders, rural residents have an increased risk for poorer mental health outcomes, likely due to the inadequate access to care, and limited social and community support18,19. In the USA, mental health has been identified as a top rural health priority20,21. Most mental health disorders also begin at the adolescence or youth stages of development22. There are high rates of self-harm, and suicide is the leading cause of death among young populations22. Older adults are also at an increased risk for experiencing mental health disorders, particularly depression23.
Future policy and program interventions should focus on recruitment and retention of the rural workforce in order to develop an adequate rural health workforce. Research suggests that students from rural areas are four times more likely to return to rural areas to practice24, and this may provide a direction for policy-makers and stakeholders to develop behavioral health career programs targeting rural students. Overall, the present study's findings suggest that rural and frontier areas as well as areas with a high proportion of children and elderly residents in Nebraska may be appropriate targets for behavioral health workforce interventions, such as the provision of incentives to recruit or retain behavioral health professionals or the exploration of alternative modes of mental and behavioral health services delivery (eg telehealth). On the other hand, the positive association found between the supply of behavioral health professionals and the percentage of populations in poverty suggests that Nebraska may be appropriately meeting the demand for care among low-income populations. Low-income individuals are more likely to be affected by and have more mental disorders than those with more resources25.
The study findings also highlight the poor regional distribution in the supply of behavioral health professionals in Nebraska. In general, behavioral health professionals were more likely to be actively practicing in behavioral health region 6 as compared to regions 1 and 4 in Nebraska. This is not surprising as region 6 has highest population density, of 144 persons/km2 (373 persons/mi2). Four of its total five counties are metropolitan counties. These findings have implications for prioritizing central Nebraska and the western panhandle of Nebraska as areas in need of appropriate interventions to increase access to care.
There are several limitations to this study. The supply of behavioral health professionals is considered in the absence of information about the demand, utilization, or quality of services. All of these are important factors in workforce planning. Despite these limitations, the study served the purpose of broadly describing the relationship between supply and county characteristics. Previous studies have highlighted the need for data that includes specific practice information such as location and specialty to better quantify the supply of professionals11,12,26. Thus, this study has been able to more accurately quantify the supply of actively practicing behavioral health professionals by using HPTS data. Previous studies have overestimated the supply by using licensing, credentialing, and membership counts, which do not provide an accurate depiction of actively practicing professionals11. Overall, the data used in this study has implications for other states in terms of workforce data collection.
Based on the study findings, it is clear that Nebraska faces a significant geographical and regional maldistribution of the behavioral health workforce. Rural counties and areas with high proportions of children and aging populations in Nebraska face significant challenges in recruiting and retaining behavioral healthcare professionals. The study findings have implications for quantifying the need and demand for behavioral healthcare professionals in workforce planning and policy analysis. The study findings suggest that proactive steps need to be taken to address the needs of rural and frontier populations, as well as the shortages due to the geographic and regional maldistribution of supply.
Acknowledgements
The support for this study was provided by the Nebraska Behavioral Health Education Center at the University of Nebraska Medical Center.
References
1. Kessler RC, Demler O, Frank RG, Olfson M, Pincus HA, Walters EE, et al. Prevalence and treatment of mental disorders, 1990 to 2003. New England Journal of Medicine 2005; 352(24): 2515-2523.
2. Perou R, Bitsko RH, Blumberg SJ, Pastor P, Ghandour RM, Gfroerer JC, et al. Mental health surveillance among children - United States, 2005-2011. Morbidity and Mortality Weekly Report Surveillance Summaries 2013; 62(Suppl 2): 21-35.
3. Chapman D, Perry G, Strine T. The vital link between chronic disease and depressive disorders. Preventing Chronic Disease 2005; 2(1): A14.
4. Mark TL, Levit KR, Buck JA, Coffey RM, Vandivort-Warren R. Mental health treatment expenditure trends, 1986-2003. Psychiatric Services 2007; 58(8): 1041-1048.
5. Thomas KC, Ellis AR, Konrad TR, Holzer CE, Morrissey JP. County-level estimates of mental health professional shortage in the United States. Psychiatric Services 2009; 60(10): 1323-1328.
6. Hanrahan N. Analysis of the psychiatric-mental health nurse workforce in the United States. Journal of Psychosocial Nursing and Mental Health Services 2009; 47(5): 34-42.
7. Hoge MA, Morris JA, Stuart GW, Huey LY, Bergeson S, Flaherty MT, et al. A national action plan for workforce development in behavioral health. Psychiatric Services 2009; 60(7): 883-887.
8. DeLeon PH, Wakefield M, Hagglund KJ. The behavioral health care needs of rural communities. In: BH Stamm (Ed). Rural behavioral health care: an interdisciplinary guide. Washington, DC: American Psychological Association, 2003; 23-31.
9. Wang PS, Lane M, Olfson M, Pincus HA, Wells KB, Kessler RC. Twelve-month use of mental health services in the United States: results from the National Comorbidity Survey Replication. Archives of General Psychiatry 2005; 62(6): 629-640.
10. Rost K, Fortney J, Fischer E, Smith J. Use, quality, and outcomes of care for mental health: the rural perspective. Medical Care Research and Review 2002; 59(3): 231-265.
11. Ellis AR, Konrad TR, Thomas KC, Morrissey JP. County-level estimates of mental health professional supply in the United States. Psychiatric Services 2009; 60(10): 1315-1322.
12. Baldwin LM, Patanian MM, Larson EH, Lishner DM, Mauksch LB, Katon WJ, et al. Modeling the mental health workforce in Washington State: using state licensing data to examine provider supply in rural and urban areas. Journal of Rural Health 2006; 22(1): 50-58.
13. Substance Abuse and Mental Health Services Administration, Center for Mental Health Services. 2010 CMHS uniform reporting system output tables. (Online) 2011. Available: http://www.samhsa.gov/dataoutcomes/urs/urs2010.aspx (Accessed 19 November 2013).
14. Substance Abuse and Mental Health Services Administration, Center for Mental Health Services. SAMHSA 2007 uniform reporting system (URS) output tables. (Online) 2008. Available: http://www.samhsa.gov/dataoutcomes/urs/urs2007.aspx (Accessed 19 November 2013).
15. Health Resources and Services Administration. Mental health HPSA designation overview. (Online). Available: http://bhpr.hrsa.gov/shortage/hpsas/designationcriteria/mentalhealthhpsaoverview.html (Accessed 19 November 2013).
16. Merwin E, Hinton I, Dembling B, Stern S. Shortages of rural mental health professionals. Archives of Psychiatric Nursing 2003; 17(1): 42-51.
17. Hoffman C, Damico A, Garfield R. Research brief: insurance coverage and access to care in primary care shortage areas. Washington, DC: Henry J. Kaiser Family Foundation, 2011.
18. Searles VB, Valley MA, Hedegaard H, Betz ME. Suicides in urban and rural counties in the United States, 2006-2008. Crisis 2014; 35(1): 18-26.
19. Inder K, Lewin T, Kelly B. Factors impacting on the well-being of older residents in rural communities. Perspectives in Public Health 2012; 132(4): 182-191.
20. Gamm L, Hutchison L. Rural health priorities in America: where you stand depends on where you sit. Journal of Rural Health 2003; 19(3): 209-213.
21. Mechanic D. More people than ever before are receiving behavioral health care in the United States, but gaps and challenges remain. Health Affairs 2014; 33(8): 1416-1424.
22. Patel V, Flisher A, McGorry P. Mental health of young people: a global public health challenge. Lancet 2007; 369: 1302-1313.
23. Sarró-Maluquer M, Ferrer-Feliu A, Rando-Matos Y, Formiga F, Rojas-Farreras S. [Depression in the elderly: Prevalence and associated factors]. [In Spanish] Semergen/Sociedad Española De Medicina Rural Y Generalista 2013; 39(7): 354-360.
24. Rabinowitz HK, Diamond JJ, Markham FW, Paynter NP. Critical factors for designing programs to increase the supply and retention of rural primary care physicians. JAMA 2001; 286(9): 1041-1048.
25. Miranda J, Green BL. The need for mental health services research focusing on poor young women. Journal of Mental Health Policy and Economics 1999; 2(2): 73-80.
26. Weil TP. Insufficient dollars and qualified personnel to meet United States mental health needs. Journal of Nervous and Mental Disease 2015; 203(4): 233-240.

