Physician shortage in rural areas is a major concern in many societies1. Less than 25% of the total physician workforce serve rural areas, home to approximately half of the world's population2. To improve this situation, many countries have implemented interventions from the medical school to the government level.
Special local quotas constitute one intervention for ameliorating the shortage of physicians in rural areas3,4. For example, Jefferson Medical College in the United States has a Physician Shortage Area Program5, and Flinders University in Australia established the Northern Territory Clinical School and uses a local quota program6. They have had moderate success in increasing the number of doctors who practice in medically underserved areas (MUAs)4,5,7-10. Similar approaches related to admission systems have successfully increased the number of rural physicians11,12.
Physician shortage in rural areas is a major health policy issue in Japan13. To address this issue, the Japanese government began a policy to increase a special quota at medical schools to alleviate the physician shortage in MUAs14,15. This expanded quota is called chiikiwaku. There are variations in how chiikiwaku is implemented across medical schools; however, for most chiikiwaku students, medical education is followed by obligatory medical practice of approximately 6-9 years in an MUA. The practice location is determined by the medical school or the local government of the student's home prefecture. Most chiikiwaku students are required to take out a student loan but are exempted from repayment after fulfilling this obligation. As of 2013, more than 1400 of 9000 medical students each year were chiikiwaku students, and 80% of medical schools in Japan have introduced the chiikiwaku system14. Eighty-five percent of chiikiwaku graduates from 25 medical schools were working in their home prefectures during the obligatory period in 201314.
Most chiikiwaku graduates are still under obligatory rural dispatch; it is unclear whether they will remain in MUAs after meeting their obligation. Well-experienced doctors who have completed the obligatory period play a key role in sustaining rural health care. To address physician shortages in rural areas, retention of doctors who started their careers in rural areas is important16. To make the chiikiwaku system an effective intervention for addressing physician shortages in MUAs, it is important to investigate the motivation of chiikiwaku students to remain in MUAs and associated factors after obligatory practice5,17,18. By clarifying the motives of chiikiwaku students and the factors associated with their willingness to stay, medical schools can improve admission processes and develop effective curricula or support systems to maintain motivation. The motives of chiikiwaku students have not been well characterized to date on a national level.
Previous studies have suggested that rural home town, male gender and career plans during the first year of medical school (family practice or rural practice location) are predictors of rural primary care practice3,19,20. In addition, reasonable workload requirements or on-call schedules21 and financial sustainability19 are important factors associated with physician retention in MUAs. Family issues such as employment opportunities for spouses22 or parenting young children23 also affect physician retention in rural areas.
Jichi Medical University (JMU) was established in 1972 to train doctors that will serve in MUAs24. All JMU students receive monetary support from their home prefecture in the form of a loan. Two or three high school graduates are recruited each year from each prefecture across Japan. Medical graduates can be exempted from repayment if they complete 9 years of obligatory postgraduate medical practice. Studies of JMU students revealed that physician retention in MUAs is associated with male sex, rural upbringing, early-career experience with rural service, and primary care practice4,9,25,26. Most of these factors were identified in retrospective surveys of rural doctors, so it is unclear whether these factors are also associated with the willingness of chiikiwaku students to remain in MUAs in the future. In addition, it may be more difficult for chiikiwaku students to remain willing to stay than other JMU students because they constitute a minority of the medical student population. It has not been long since the chiikiwaku system was started, and there have been no national-scale surveys of chiikiwaku students.
In this study, the objective was to assess the motivation of chiikiwaku students to remain in MUAs after fulfilling their obligations and to identify factors associated with their willingness to stay.
Study participants
This was a nationwide cross-sectional survey. The study population consisted of all first-year chiikiwaku students at medical schools in Japan whose deans agreed to participate in the survey. Since the conditions of the chiikiwaku system vary across medical schools, it was defined as a special quota with obligatory medical practice in MUAs after graduation, regardless of the length of the obligation or student loan dollar amount.
Data collection
The authors asked for the cooperation of representatives of rural medicine at each medical school with a chiikiwaku quota. The survey consisted of an original self-administered questionnaire. The questionnaire was developed with reference to previous studies about selective admission systems for MUAs in Japan as well as other countries4,5,9,21,27. Questionnaires were sent to the staff of each medical school, who were asked to distribute the questionnaires to students. Medical school staff were also asked to collect completed questionnaires in sealed envelopes, to prevent information bias, and return them to the researchers. The questionnaire collected demographic information such as gender, hometown type (metropolis, suburb of metropolis, city, town or village, and remote area), high school type (private or public), occupational experience (yes or no), and marital status (single or married). Hometown was defined as the location where the student had lived the longest before admission to medical school, which was described in the questionnaire. Hometown type was based on self-report.
The primary outcome, willingness to remain in MUAs after fulfilling the obligation, was assessed using a five-point Likert scale ('very willing', 'somewhat willing', 'fair', 'somewhat unwilling' and 'completely unwilling'). Subjects were also asked whether they felt belonging to chiikiwaku was encouraging and whether they felt obligatory practice and/or loan repayment was stressful using a five-point Likert scale. In addition, students were asked about their primary reason for applying for chiikiwaku: passion for contributing to MUAs, financial support, higher medical school acceptance rate and 'other'. Regarding factors influencing future work preferences, the questionnaire asked about preferred location type (urban or rural), length of duty hours, call frequency, adequate number of holidays, work-life balance, experiences during clinical clerkships, influence of patients, personal medial history, role models, ease in running a private practice, succession of parent's work, recommendations from seniors or friends, academic attraction, novels or TV shows, and taking out a loan for which repayment is not required after serving in a rural community. The influence of these factors on work preferences was assessed using a five-point Likert scale.
Statistical analysis
For the primary outcome, students were categorized into the willing group ('very willing' or 'somewhat willing' to remain in MUAs after obligation) or the unwilling group ('fair,' 'somewhat unwilling,' or 'completely unwilling').
In the univariate analyses, independent variables included demographic characteristics, stress and supports related to chiikiwaku status, primary reason for applying for chiikiwaku, and factors influencing work preferences. These variables were all categorical, and participants were dichotomized for each variable. Regarding hometown, 'metropolis', 'suburb of metropolis' and 'city' were classified as urban, and 'town or village' and 'remote area' were classified as rural. The cutoff for stress from obligation or repayment was between 'sometimes stressful' and 'not very often.' The cutoff for feeling that chiikiwaku was encouraging was between 'somewhat agree' and 'neither agree nor disagree.' Primary reason for applying for chiikiwaku other than passion for contributing to MUAs was collapsed into one category because such reasons were not essential to a student's eagerness to contribute to MUAs. Regarding the influence of factors on work preferences, the cutoff for each factor was between 'large influence' and 'small influence.' The χ2 test was used for the univariate analyses.
Multivariate logistic regression analysis included variables with p<0.1 in the univariate analyses. Gender was also included in the multivariate analysis because it is a fundamental characteristic. In addition, the authors conducted factor analysis on factors associated with work preference. The factor with the lowest p value in the χ2 test from each domain was included in the multivariate analysis.
For both univariate and multivariate analyses, the significance level was set at p<0.05. Statistical analysis was performed using the Statistical Package for the Social Sciences v21 (IBM; http://www.spss.com).
Ethics approval
The cover sheet of the questionnaire stated that information collected through this survey had no influence on the student's academic record. Students were asked to submit completed questionnaires in sealed envelopes that were provided by the researchers. This study was approved by the Ethics Committee of the Faculty of Medicine of the University of Tsukuba. The approval number was 21-413.
Of 63 medical schools that had a chiikiwaku quota system in Japan at the time of this survey, 38 schools participated in this study. Between September 2010 and February 2011, the authors surveyed 542 first-year chiikiwaku students at these schools, of whom 440 students answered the questionnaire. There were 405 valid responses (response rate, 74.7%).
There were 233 male students (58%), and 172 female students (42%). There were 128 students who came from rural areas (31.6%). Few students had work experience or were married. The average age of the subjects was 19.7 years (standard deviation, 2.3) .
There were 95 (23%) students who were very willing to remain in MUAs, 117 (29%) somewhat willing, 157 (39%) fair, 31 (8%) somewhat unwilling, and 5 (1%) completely unwilling (Fig1). Table 1 shows the characteristics of the subjects by willingness to remain in MUAs. In the univariate analysis, student home town, stress from obligation or repayment, encouragement from belonging to chiikiwaku and primary reason for applying for chiikiwaku were significantly associated with willingness to remain in MUAs after fulfilling the obligation.
Factors influencing work preferences are shown separately in Table 2 due to the large number of factors. Among these factors, call frequency and student loans were significantly associated with willingness to remain in MUAs. In the factor analysis, six domains emerged: work-life balance, future vision as a doctor, role models, private practice, influence from others, and student loans that will not require repayment after service in a rural community .
In the multivariate analysis, home town type (odds ratio (OR), 1.8; 95% confidence interval (CI), 1.1-2.9), encouragement from belonging to chiikiwaku (OR, 3.6; 95%CI, 2.3-5.8), passion for contributing to MUAs as the primary reason for applying for chiikiwaku (OR, 4.4; 95%CI, 2.5-7.5) and influence of student loans on work preferences (OR, 1.7; 95%CI, 1.0-2.7) were significantly associated with willingness to remain in MUAs after fulfilling the obligation (Table 3).
Table 1: Characteristics of participants by willingness to remain in medically underserved areas (n=405)
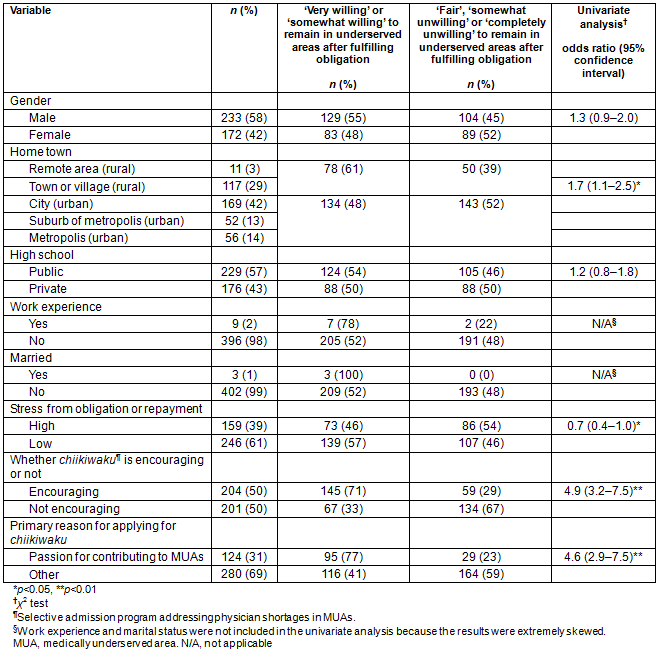
Table 2: Factors influencing work preferences by willingness to remain in medically underserved areas
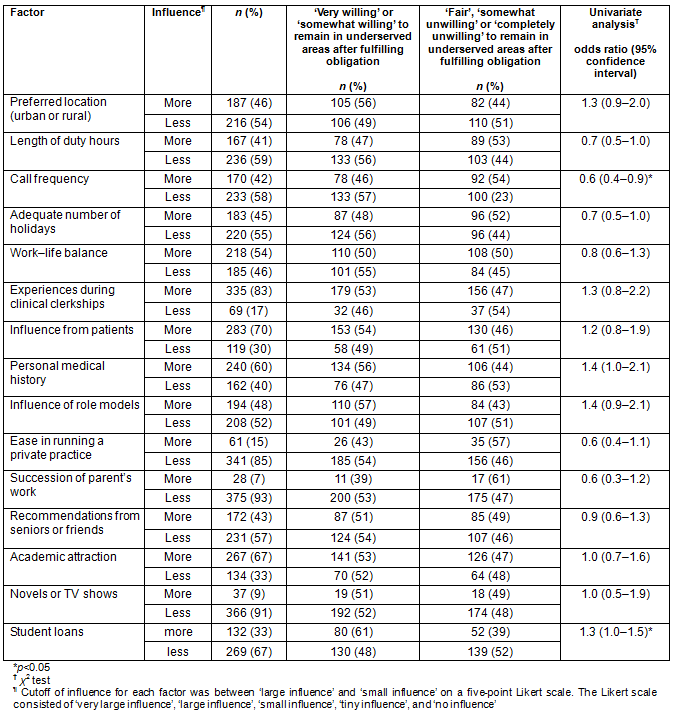
Table 3: Multivariate analysis? of factors associated with willingness to remain in medically underserved areas (n=398)
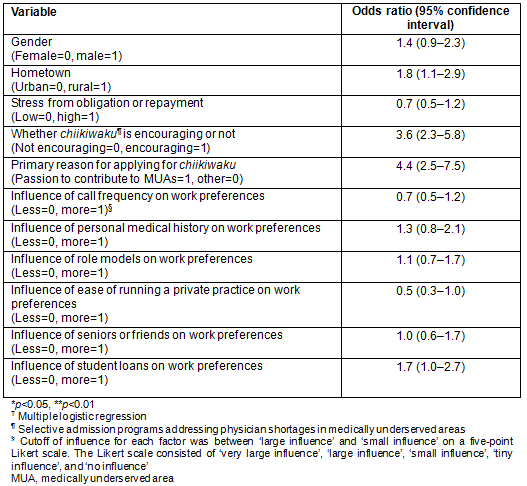
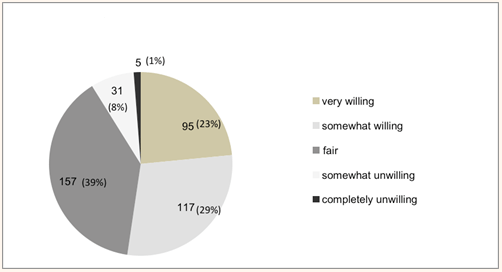
Figure 1: Students' willingness to remain in medically underserved areas (n=405)
Discussion
Fifty-two percent of chiikiwaku students were 'very' or 'somewhat' willing to remain in MUAs after obligatory practice. The authors found several factors associated with willingness to remain in MUAs. Regarding pre-medical school factors, rural hometown and passion for contributing to MUAs as a primary reason for applying for chiikiwaku were associated with willingness to stay. After admission to medical schools, students who felt encouraged by being in a chiikiwaku program and students whose work preferences were influenced by loans (medical school factors) were more willing to remain in MUAs.
In previous studies, both pre-medical school factors such as rural upbringing5,18,19 and medical school factors such as rural preceptorship5 or clinical rotation experience18 were associated with working in rural areas. However, these factors were not associated with remaining in rural areas5,27. In the present study, subjects were all first-year medical students, who have a long time (approximately 15 years) to fulfill their obligations. Therefore, first-year medical students may not perceive much difference between working and remaining in MUAs.
Students who felt encouraged because of their chiikiwaku status were willing to remain in MUAs. It has been hypothesized that chiikiwaku itself can be as a positive incentive for students to remain motivated to work in MUAs. It is possible that the special curriculum on rural medicine, including early rural exposure, encourages students to remain eager to contribute to MUAs28,29.
Physician work preferences such as work-life balance, after-hours workload and ease in running a private practice are said to affect the willingness to remain in MUAs21,27,30. However, these factors had no significant association with the willingness to remain in MUAs in this study, possibly because this study focused on first-year students who could not easily imagine future working or family conditions, including the education of their own children.
Although male doctors have been reported to work in rural areas or MUAs in higher proportions than female doctors5,9, gender was not associated with willingness in this study. During the first year of medical school, female students might have difficulty imagining work-life balance after marriage or childbirth, factors that are considered to be barriers to retention in MUAs31. Surveys involving senior medical students might show differences between male and female students.
For the first-year chiikiwaku medical students, predisposing factors such as home town type or passion for contributing to MUAs as the primary reason for applying for chiikiwaku were associated with willingness to remain in MUAs. Adequate selection of students on admission may be important for increasing the number of doctors who will serve in MUAs8,17,32. The present study showed that approximately 30% of students applied for chiikiwaku because of a passion for contributing to MUAs, so it may be necessary to improve the chiikiwaku admissions process. For example, multiple interviews may be needed to assess their real motivation to apply for the chiikiwaku quota. Furthermore, encouragement from belonging to chiikiwaku was relevant to the willingness to remain in MUAs. Educational interventions that provide encouragement to chiikiwaku students could be useful in maintaining students' willingness or motivation to serve in MUAs. For example, development of a community-oriented curriculum33 or mentoring system5 might be effective.
This study has several limitations. First, this study was cross-sectional, and thus cannot identify causal relationships between willingness to stay in MUAs and explanatory variables such as stress or encouragement received by chiikiwaku students. Second, differences in how the chiikiwaku quota system works among medical schools affected the homogeneity of the sample. As mentioned in the introduction, the admission or education system of chiikiwaku is different among medical schools, but the authors did not collect these information. There may be a difference of characteristics between the sample of this study and students who did not participate in this study because deans of their medical schools did not consent to this study. Third, the authors did not include future career preferences in this study, although some previous studies have indicated that primary care physicians tend to remain in rural areas or MUAs more than other specialists4,9,18,34. It was assumed that it was difficult to identify feelings about specific specialties in this study population because most first-year medical students in Japan have not had clinical experiences such as clinical clerkships; thus, they do not have a precise image of each discipline. Consequently, the authors did not include career preference as an explanatory variable. Fourth, five-point Likert scales were converted to dichotomous variables for willingness to remain in MUAs and influence of work preferences because the number of responses was low. Factors significantly associated with willingness to remain in MUAs with dichotomization will remain so in the five-point format, but dichotomization may have affected the results of this study. Although this study has these limitations, the results of this nationwide study would be useful for improving the selection and support system for chiikiwaku students at many medical schools.
The career plans and considerations of chiikiwaku students may change as they progress through medical school and begin to practice. Willingness could also change during senior year or residency. Identifying factors associated with maintaining levels of willingness from junior to senior year may be helpful for increasing the number of doctors who consider remaining in MUAs for a long period of time.
Approximately half of the chiikiwaku students in Japan are very or somewhat willing to remain in MUAs after fulfilling their obligations. Factors associated with willingness to remain include rural upbringing, primary reason for applying for medical school, passion to contribute to MUAs, encouragement during medical school and perceiving loans as having a strong influence on their work preferences.
References
1. Zurn P, Dal Poz MR, Stilwell B, Adams O. Imbalance in the health workforce. Human Resources for Health 2004; 2(1): 13.
2. Dolea C, Stormont L, Braichet JM. Evaluated strategies to increase attraction and retention of health workers in remote and rural areas. Bulletin of the World Health Organization 2010; 88(5): 379-385.
3. Brooks RG, Walsh M, Mardon RE, Lewis M, Clawson A. The roles of nature and nurture in the recruitment and retention of primary care physicians in rural areas: a review of the literature. Academic Medicine 2002; 77(8): 790-798.
4. Matsumoto M, Inoue K, Kajii E. A contract-based training system for rural physicians: follow-up of Jichi Medical University graduates (1978-2006). Journal of Rural Health 2008; 24(4): 360-368.
5. Rabinowitz HK, Diamond JJ, Markham FW, Paynter NP. Critical factors for designing programs to increase the supply and retention of rural primary care physicians. Journal of the American Medical Association 2001; 286(9): 1041-1048.
6. Worley P, Martin A, Prideaux D, Woodman R, Worley E, Lowe M. Vocational career paths of graduate entry medical students at Flinders University: a comparison of rural, remote and tertiary tracks. Medical Journal of Australia 2008; 188(3): 177-178.
7. Barnighausen T, Bloom DE. Financial incentives for return of service in underserved areas: a systematic review. BMC Health Services Research 2009; 9: 86.
8. Curran V, Rourke J. The role of medical education in the recruitment and retention of rural physicians. Medical Teacher 2004; 26(3): 265-272.
9. Matsumoto M, Inoue K, Kajii E. Long-term effect of the Home Prefecture Recruiting Scheme of Jichi Medical University, Japan. Rural and Remote Health (Internet) 2008; 8(3): 930. Available: www.rrh.org.au (Accessed 10 May 2015).
10. Rabinowitz HK, Diamond JJ, Markham FW, Wortman JR. Medical school programs to increase the rural physician supply: a systematic review and projected impact of widespread replication. Academic Medicine 2008; 83(3): 235-243.
11. Hart LG, Salsberg E, Phillips DM, Lishner DM. Rural health care providers in the United States. Journal of Rural Health 2002; 18(Suppl): 211-232.
12. Royston PJ, Mathieson K, Leafman J, Ojan-Sheehan O. Medical student characteristics predictive of intent for rural practice. Rural and Remote Health (Internet) 2012; 12: 2107. Available: www.rrh.org.au (Accessed 10 May 2015).
13. Tanihara S, Kobayashi Y, Une H, Kawachi I. Urbanization and physician maldistribution: a longitudinal study in Japan. BMC Health Services Research 2011; 11: 260.
14. Ministry of Education, Culture, Sports, Science and Technology. Investigation into community medicine. (Internet) 2013. Available: http://www.mext.go.jp/a_menu/koutou/iryou/1324090.htm (Accessed 12 August 2015).
15. Matsumoto M, Inoue K, Kajii E, Takeuchi K. Retention of physicians in rural Japan: concerted efforts of the government, prefectures, municipalities and medical schools. Rural and Remote Health (Internet) 2010; 10(2): 1432. Available: www.rrh.org.au (Accessed 10 May 2015).
16. Pathman DE, Konrad TR, Agnew CR. Studying the retention of rural physicians. Journal of Rural Health 1994; 10(3): 183-192.
17. Matsumoto M, Inoue K, Takeuchi K. Evidence-based reform of rural medical education. Literature review and political application. Iryo To Shakai (Japanese) 2012; 22(1): 103-112.
18. Kawamoto R, Uemoto A, Ninomiya D, Hasegawa Y, Ohtsuka N, Kusunoki T, et al. Characteristics of Japanese medical students associated with their intention for rural practice. Rural and Remote Health (Internet) 2015; 15: 3112. Available: www.rrh.org.au (Accessed 20 September 2015).
19. Rabinowitz HK, Diamond JJ, Hojat M, Hazelwood CE. Demographic, educational and economic factors related to recruitment and retention of physicians in rural Pennsylvania. Journal of Rural Health 1999; 15(2): 212-218.
20. Wilkinson D. Selected demographic, social and work characteristics of the Australian general medical practitioner workforce: comparing capital cities with regional areas. Australian Journal of Rural Health 2000; 8(6): 327-334.
21. Cutchin MP, Norton JC, Quan MM, Bolt D, Hughes S, Lindeman B. To stay or not to stay: issues in rural primary care physician retention in eastern Kentucky. Journal of Rural Health 1994; 10(4): 273-278.
22. Mitka M. What lures women physicians to practice medicine in rural areas? Journal of the American Medical Association 2001; 285(24): 3078-3079.
23. Pathman DE, Konrad TR, Dann R, Koch G. Retention of primary care physicians in rural health professional shortage areas. American Journal of Public Health 2004; 94(10): 1723-1729.
24. Inoue K, Hirayama Y, Igarashi M. A medical school for rural areas. Medical Education 1997; 31(6): 430-434.
25. Matsumoto M, Inoue K, Kajii E. Policy implications of a financial incentive programme to retain a physician workforce in underserved Japanese rural areas. Social Science and Medicine 2010; 71(4): 667-671.
26. Matsumoto M, Inoue K, Kajii E. Characteristics of medical students with rural origin: implications for selective admission policies. Health Policy 2008; 87(2): 194-202.
27. Hancock C, Steinbach A, Nesbitt TS, Adler SR, Auerswald CL. Why doctors choose small towns: a developmental model of rural physician recruitment and retention. Social Science & Medicine (1982) 2009; 69(9): 1368-1376.
28. Ranmuthugala G, Humphreys J, Solarsh B, Walters L, Worley P, Wakerman J, et al. Where is the evidence that rural exposure increases uptake of rural medical practice? Australian Journal of Rural Health 2007; 15(5): 285-288.
29. Rabinowitz HK, Diamond JJ, Markham FW, Hazelwood CE. A program to increase the number of family physicians in rural and underserved areas: impact after 22 years. Journal of the American Medical Association 1999; 281(3): 255-260.
30. Matsumoto M, Okayama M, Kajii E. Rural doctors' satisfaction in Japan: a nationwide survey. Australian Journal of Rural Health 2004; 12(2): 40-48.
31. Allen I. Women doctors and their careers: what now? British Medical Journal (Clinical Research Ed) 2005; 331(7516): 569-572.
32. Wilson NW, Couper ID, De Vries E, Reid S, Fish T, Marais BJ. A critical review of interventions to redress the inequitable distribution of healthcare professionals to rural and remote areas. Rural and Remote Health (Internet) 2009; 9(2): 1060. Available: www.rrh.org.au (Accessed 14 May 2015).
33. Okayama M, Kajii E. Educational effects of a standardized program for community-based clinical clerkships. Igaku Kyoiku/Medical Education (Japan) 2004; 35(3): 197-202.
34. Matsumoto M, Okayama M, Inoue K, Kajii E. Factors associated with rural doctors' intention to continue a rural career: a survey of 3072 doctors in Japan. Australian Journal of Rural Health 2005; 13(4): 219-225.



