How best to provide and sustain adequate primary healthcare (PHC) services in the many small communities scattered across the vast reaches of rural and remote Australia has been a major challenge facing governments for several decades1,2. Over the past 40 years, numerous demographic and economic changes have impacted significantly on these communities, resulting in widespread rural population decline, ageing and outmigration; agricultural restructuring and vertical integration of industry; and significant loss of locally available services. At the same time, the health needs of Australians remaining in rural and remote areas increased, yet their accessibility to PHC services often remained at risk3.
Faced with this scenario, health authorities encouraged innovative models of PHC service delivery with a view to maximising the local availability of appropriate health care4-6. These models ranged from discrete GP or nurse service providers (such as the Easy Entry, Gracious Exit model facilitating GP recruitment, and the Central Australian Nurse (CAN) Management model, which supports the remote area nurse workforce and sole nurse practitioners), through integrated models (such as multi-purpose services, shared-care, coordinated care models), and comprehensive care models (such as Aboriginal community-controlled health services), to a wide variety of outreach models (such as hub-and-spoke; fly-in, fly-out; virtual clinics and numerous telehealth models), with the Royal Flying Doctor Service arguably the best known7-10. More recently, various forms of 'corporate' models have emerged in rural areas11. The various models seek to deliver services to small numbers of people scattered over vast areas. In these circumstances, population size can fail to meet the critical mass necessary to support traditional health services or hospitals and the service models may vary in their provision of care and sustainability. Part of the reason for this varied success can be attributed to the lack of a comprehensive understanding of the processes and factors that enable and inhibit PHC services to successfully expand into communities that are either inadequately serviced or at high risk of becoming inadequately serviced. Given the dearth of contextually relevant research investigating enablers and inhibitors of rural PHC service expansion, this study primarily adopts an exploratory, qualitative approach to investigating this issue.
A detailed analysis is provided of how one small rural PHC service transitioned from a comprehensive PHC service model (Elmore Primary Health Service (EPHS)) providing multidisciplinary PHC via a single-entry point within a single rural community (Elmore)12,13, to a regionally networked PHC service model. Whilst continuing to evolve, the regionally networked model is currently providing PHC services in six small rural communities within the Loddon-Campaspe region of northern Victoria (Elmore, Rochester, Boort, Heathcote, Rushworth, Lockington) and in one large regional centre (Strathfieldsaye, an outlying suburb of Bendigo) (Fig1). Previous discrete models of PHC service delivery in these small rural centres were frequently associated with isolated practice and a high risk of discontinuity of services when existing GPs left12-15 . The regionally networked model has, in contrast, been able to provide continuity of PHC services and improved access to appropriate, integrated and comprehensive PHC for the rural (and regional) populations in the communities and catchments serviced12,13,16,17 .
The specific objectives of this article are twofold: first, to better understand the factors and processes enabling and impeding the expansion of EPHS into these small rural communities and, second, to outline lessons for other rural health services seeking to expand the provision of effective and sustainable PHC to neighbouring small rural communities.
Primary health care: what's known?
- Many small rural and remote communities struggle to sustain comprehensive PHC services.
- Recent research has identified some of the key requirements associated with the provision of high-quality PHC services.
- With the possible exception of corporate models, little is known about how best to expand the provision of core high-quality PHC services to the many small and diverse non-metropolitan communities that currently lack them.
Primary health care: what's new?
- This evaluation of a 'networked' model of PHC in rural areas identifies the factors and processes underpinning service expansion and demonstrates how risks are managed.
- The importance of 'community-driven' as opposed to 'provider-led' service expansion is highlighted.
- 'Networked' service delivery models sustain themselves well in small rural communities because network linkages assist individual services to effectively manage change and meet essential service requirements in rapidly changing circumstances.
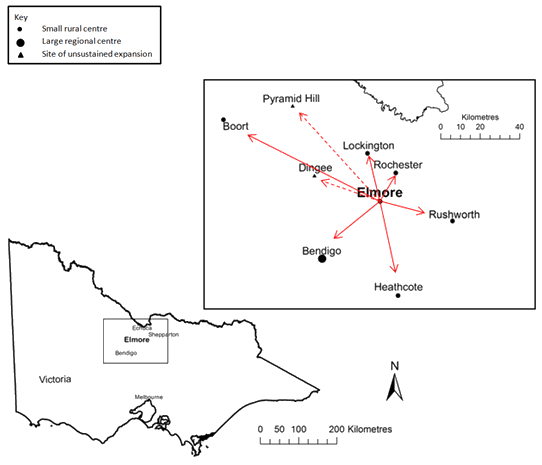
Figure 1: Map showing communities to which Elmore Primary Health Service has expanded.
Individual face-to-face interviews were held with 11 purposively selected staff members of EPHS and its associated business entity, St Anthony Family Medical Practice (hereafter referred to as EPHS) between February and June 2015. Two investigators were present at each interview. Purposive sampling aimed to capture data from key practice decision makers, most notably the practice principal and the practice manager. Data were also collected from primary care clinicians (including seven general practitioners and two practice nurses) working at each of the currently operational sites within the regional network (including Elmore, Lockington, Boort, Rochester, Heathcote, Rushworth and Strathfieldsaye) and from administrative staff members, all of whom had substantial knowledge and experience of the service expansion. Interviews were conducted at the various health service sites, for the convenience and comfort of the participants. All interviewees provided their informed consent. Only one GP declined to be interviewed.
A comprehensive semi-structured interview schedule was developed to guide in-depth interviews with the practice principal and practice manager. A more concise interview schedule was subsequently developed to guide interviews with all other staff members (it was not necessary to collect detailed factual data relating to the services from every stakeholder). The interview schedules were informed by the literature and by the researchers' first-hand knowledge of the EPHS expansion gained through previous joint research13,17.
Following the semi-structured interviews, respondents were requested to indicate the importance of 16 different factors (and any other factor they wished to add) to the expansion of EPHS. Questions were structured to capture the importance of each of three environment enablers of rural PHC (supportive policies, Commonwealth/state relations and community readiness), five essential service requirements (workforce; funding; governance, management and leadership; linkages; and infrastructure) and the past success of EPHS10. A four-point scale ('very important', 'important', 'somewhat important', and 'not important') with the additional option of 'don't know' was used to measure the importance of each factor. The practice principal and practice manager were approached by telephone for their participation in this study. In accord with ethics requirements, the EPHS practice manager subsequently approached other potential participants contracted to or employed by EPHS.
Interviews, with an average duration of 41 minutes, were recorded and audio files transcribed verbatim, with participant quotes made anonymous in order to maintain confidentiality. Transcribed interviews were imported into QSR NVivo v10 (QSR International; http://www.qsrinternational.com) for coding and thematic analysis by the researchers, with analysis guided by the methods outlined by Braun and Clarke18. The transcripts were independently analysed by two investigators using an inductive approach, with the researchers reading and re-reading the transcripts to identify important patterns in the data, and meeting frequently to discuss emerging themes and to resolve any discrepancies. Analysis occurred concurrently with interviewing.
Ethics approval
Ethics approval was received from the Monash University Human Research Ethics Committee (Ref. CF14/3468-2014001803).
Although only 55% of participants indicated that they considered the environmental enabler - supportive policies - to be very important for the expansion of EPHS, almost all participants (91%) considered community engagement to be a very important environmental enabler of successful expansion (Table 1). A number of aspects of the five essential service requirements were also identified by almost all participants to be very important to expansion. Three aspects of workforce - improving residents' access to PHC (100%), broadening the range of care provided (91%), and professional satisfaction (91%) - were considered as making very important contributions to EPHS expansion. Funding opportunities (82%), vision and leadership (91%), and linkages with other health services (91%) were also considered by most participants to be very important. Several participants identified three additional aspects of linkages (relationships with universities and health student vocational training organisations as well as with hospitals) as having either very important or important associations with expansion. Availability of community and health service infrastructure and the past successes of EPHS were each considered to be either important or very important by the majority of participants.
Thematic analysis of the data revealed five stages in the evolution and expansion of the EPHS comprehensive PHC service model (Fig2): initiative, consultation, roll-out, evaluation and consolidation. Because new sites were progressively added to the developing regionally networked PHC service model, at any given time EPHS comprised multiple health service sites at different developmental stages.
Table 1: Importance of essential service requirements and environmental enablers for expansion of Elmore Primary Health Service
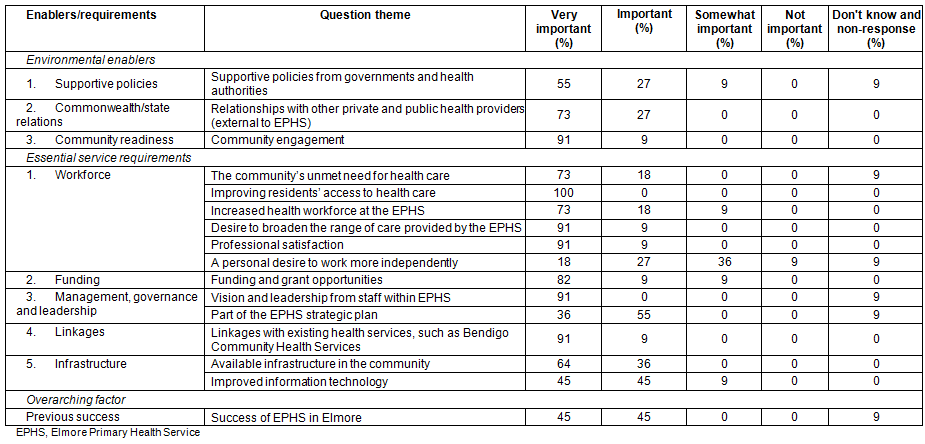
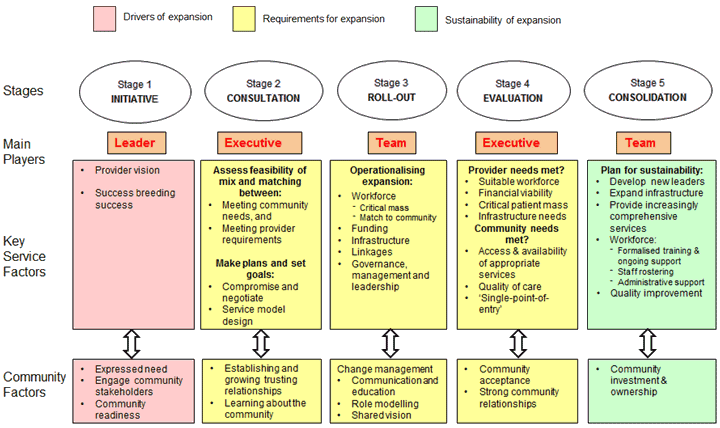
Figure 2: Conceptual model of the stages of primary healthcare service expansion.
Stage 1: Initiative
Expansion beyond Elmore was, in most instances, primarily initiated by the expressed need of other small rural communities within the region for a doctor:
... [They] were left without a doctor and they had ... a nursing home, hostel, hospital and (the hospital board members were) really afraid that they were going to lose all that.
The dire situation galvanised community stakeholders to seek solutions, and to approach leaders at EPHS for help, as they knew of EPHS's success in transforming Elmore from a doctorless town with minimal health services to one having high-quality and comprehensive PHC services. The leaders at EPHS understood the gravity of the situation and sought ways in which they could help:
We were thinking how can we help them? ... we decided ... we could roster our doctors and send them up to help them out in the beginning ...
At this stage the leader's altruistic motivation and vision to provide much-needed PHC to these small rural communities was critical:
... [He's] really passionate and driving it and ... as you know, he's the visionary with all of those things ... So he's the driving force really.
Stage 2: Consultation
The next stage of EPHS expansion required extensive internal consultation with an 'inner executive' of senior GP partners and their immediate families, to ascertain and further develop support. Concurrently, the inner executive invested considerable time and energy into developing strong and trusting relationships with community stakeholders, in some instances over prolonged time periods, aware that:
It wouldn't work if the community weren't supporting ...
It was during the consultation stage of EPHS's initial expansion beyond Elmore that a networked service model was initially conceived, and its advantages over the stand-alone single-entry point comprehensive PHC model providing PHC services to only one small rural community were evaluated:
... we looked at it and we thought that the ideas were good, that ... if you wanted a practice to work in these rural areas this was how you needed to run it.
During the consultation stage, the inner executive also assessed the feasibility of delivering PHC services at each new site, deliberating on what they could reasonably offer and how this matched the needs and expectations of the community and its stakeholders. Considerable negotiation and compromise was a feature, both within the inner executive and also with community stakeholders
We have to sit down and talk together and there's a lot of give and take.
Whilst the inner executive also considered the financial feasibility of expansion to new sites, financial considerations were not primary motivators of expansion, and did not feature strongly in the consultation stage:
... It [profit] will come.
Stage 3: Roll-out
The roll-out of each new service involved considerable teamwork, largely orchestrated by the EPHS practice manager and overseen by a coordinator at the new site. This required meticulous attention to all aspects of workforce, funding, infrastructure, linkage and governance factors, the crucial importance of which has been outlined elsewhere10,16,19,20.
During the initial roll-out, senior GP partners provided GP services at each new site until the 'right' doctor was recruited for that community. From a workforce perspective, establishing a new doctor frequently required a period of orientation and initial supervision at the new site by senior GPs, as most recruits were either EPHS-sponsored international medical graduates or GP registrars. A key benefit of the networked model, seen especially at this stage, was that the critical workforce mass within EPHS could 'cover' the senior doctors' regular patients in their absence from their usual practice. Recruitment of new doctors comprised a careful assessment of the 'mix' of professional and social needs of a prospective doctor and their 'match' with the needs of the community, the new practice and the EPHS group.
During the roll-out phase, an initial lack of short-term financial viability was accepted by the partners, due in part to their shared expectation that in the middle and longer term a local, high-quality and comprehensive PHC practice would attain financial viability. This approach was supported by the generally healthy financial position of EPHS, which provided capacity to support practices that weren't yet financially viable:
... sometimes in the beginning [the services] will struggle ... until they become established and until they build up ... if someone's struggling [financially] the other [EPHS] can support as we go.
The initial roll-out phase focused on establishing basic medical and nursing services, using existing infrastructure at each new site:
There's still not - at some of them [the sites], not as comprehensive a service as what there is in Elmore, but we're working on it ...
During the roll-out phase, linkages with the small rural community hospitals were especially important and supported by co-location or proximate location of clinics with hospitals:
Most of the clinics (are) either inside the hospital or close to the hospital ... we have an extremely good relation or strong relationship with the local hospital.
Successful roll-out was associated with highly skilled management who communicated regularly, both with team members and patients within the organisation, and also with external stakeholders. Management also showed an acute awareness of the need to manage community expectations and adjustments to change.
Roll-out was also characterised by strong role-modelling by the leadership team, and the creation of increased opportunities for other members of the team to step up into leadership roles:
... [it's about] letting other people take on responsibility, to make them feel as though they have ownership ...
These factors inspired team members to develop a shared vision of providing accessible PHC of outstanding quality to another community. In short, during roll-out, all the requirements for an effective, high-performing PHC service were incorporated as part of a strategic approach to implementation.
Stage 4: Evaluation
Following roll-out, PHC operations at the new site were evaluated to determine the extent to which both community and provider needs and expectations were being adequately met. An important aspect was an assessment of financial viability, as reflected by the volume or critical mass of patients seen:
[We did] ... a spreadsheet on the amount of months we were there, how many visits he did ...
Evaluation also examined a range of key factors underpinning health service sustainability, including succession planning, ongoing community engagement, and infrastructure needed for service development. In some instances a lack of community acceptance, combined with a lack of external community health infrastructure, threatened sustainability and contributed to service closure:
... the community just didn't accept having a doctor there ... they used to travel down to Bendigo ... they already had doctors established in [Bendigo] ... There was no pharmacy there so if they were seen [in their community] by the doctor they still had to travel to get medications as well.
In other instances, strong relationships with community stakeholders, particularly with hospitals, were identified as supporting PHC service sustainability:
... one of the main [reasons] for our model [being successful] is working [closely] together [with the hospital].
Unsupportive relationships, on the other hand, were found to contribute to failed expansion:
I felt they were not supportive - but even went against us.
Workforce issues, too, were integral to the evaluation stage, as was an assessment of the extent to which the service was providing accessible and high-quality PHC though a single point of entry.
Stage 5: Consolidation
During consolidation, some of the key advantages of the networked model of PHC service delivery come to the fore. First, having a critical mass of PHC providers supports succession planning. Providers are identified at an early stage and trained across a range of settings as future leaders. Second, having a critical workforce mass across multiple sites provides substantial professional support. For example, the increased workforce flexibility enables GPs and nurses to take leave more easily - including for external formal training purposes - as others can be rostered to provide services in their absence. Third, having multiple sites with central administrative support facilitates good induction and orientation of new recruits to rural Australian practice:
I did some mentorship, observership, in Rochester, in Elmore, and Strathfieldsaye and in Heathcote ... And it was actually pretty good, because you saw the different ways in which all the different bosses work ... And you sort of got it and you merged it and it works! So it's very good.
Fourth, the availability of supervision and regular internal continuing professional development is particularly attractive to international medical graduates and GP registrars striving to gain their fellowship and nurses transitioning from hospital-based care to PHC:
... once a month they also have a clinical meeting so that's also helpful for us and we bring whatever's happening there ... to our meeting as well to try and improve the level of quality of care.
During consolidation the organisation continued to strive to achieve and maintain high-quality PHC services, through ongoing quality improvement processes. These activities, in turn, support workforce development, as 'success breeds success':
It's quite amazing really how many people want to work here because they hear it's a good practice ... I think it comes down to reputation.
Furthermore, individual sites matured from providing mainly GP and nursing PHC to providing more comprehensive PHC. This often required sourcing specific funding for additional infrastructure to accommodate multidisciplinary PHC team members:
... we've been a little bit stuck because of space ... we just literally couldn't employ more staff because we had nowhere to put them and so [with funding for a bigger new practice[ the community over there is now going to have this really state of the art fantastic service.
It is at this stage that community investment in service development is realised as a sense of community ownership of the PHC service:
So you get that belonging ... there's community involvement. [That's] important, very important to see that the community involved, be part of it.
Discussion
This unique investigation of PHC service expansion revealed key interrelated processes that operate to achieve a successful outcome, and provide several salient lessons for other health service providers and policy-makers. While each community has unique health needs, culture and context, some common requirements underpin the successful expansion and delivery of appropriate PHC services.
First and most notable of these is the importance of working closely with communities and with community stakeholders at all stages of the development - a point emphasised in Figure 1 by separate boxes for community factors at each stage.
Second, while each site within the EPHS networked model operates with a degree of autonomy within its community, its links within a large network provide crucial benefits that help meet the requirements for sustainability, including workforce relief, supervision and mentorship, relevant ongoing continuing professional development, and shared management and administrative expertise. These benefits are especially realised in stage 3 (roll-out) and stage 5 (consolidation).
Third, the importance of fulfilling each of the environmental enablers and essential service requirements shown in Table 1, and outlined in detail elsewhere, was validated10. What additionally emerged from this analysis, however, is that their role and importance come into play at different stages of the expansion and evolution of the PHC service. For example, without the championing vision of leadership at the formative stage, it is possible that community need and readiness will not necessarily result in the most appropriate service model or delivery of services required by the community.
Fourth, the successful expansion of EPHS into small rural communities demonstrated an ability to grow and adapt - to changes at not only the micro level in the needs and circumstances of the communities served and in neighbouring communities, but also the macro level in health policies that guide the nation's funding of PHC and how these resources are distributed. Adapting to take advantage of government policies that enhance access to a rural medical PHC workforce - particularly through limiting provider number access for international medical graduates, but also through requiring a large proportion of GP vocational training positions to be located in rural areas - has required EPHS to build GP supervisory capacity within its workforce. Growth and expansion of EPHS has been led by principals and managers who keep up to date with rural health policy developments, and who ensure that data are collected and analysed so that the PHC service's performance is closely monitored. These features are integral to both service quality and sustainability, and not some discretionary 'add-on' that is only undertaken at times of accreditation or review.
The findings of this research are consistent with and complement existing literature in this field. A developing body of international evidence indicates that community participation in the planning and implementation of their PHC is associated with improved service accessibility, utilisation, quality and responsiveness and with improved health outcomes21. Of note, in instances where community participation is not accompanied by fulfilment of essential service requirements, such as adequate funding, infrastructure and workforce supply, improvements in PHC access and health outcomes have not been observed22. The Canadian experience and literature on transformative change in PHC, too, suggests that group practices and networks of family physicians are key to achieving health system goals such as improved access to PHC by geographically dispersed populations23 . Greenhalgh and colleagues' study of the sustainability of innovations in health service delivery shows, in keeping with the present study's findings, that organisations that are able to keep up to date by identifying, capturing, interpreting, sharing, reframing and recodifying new knowledge, and assess it in the light of their existing knowledge, are better able to sustain themselves24 .
Whilst this qualitative study has extended understanding of rural PHC service expansion, it is not without its limitations. Foremost among these is the generalisability of the findings to other rural and to remote contexts. In areas more sparsely settled than the Elmore region, distances between settlements and settlement population sizes may result in inefficiencies that limit the sustainability of networked models of PHC delivery. That said, however, there are many wheat/sheep belt regions with similar settlement patterns where the lessons from this study are particularly relevant. The expansion of EPHS also largely comprised growth into communities within the catchment for Bendigo Health. It is not clear from this research whether networked models, as exemplified by EPHS, would be equally successful if operating across multiple health service catchments or in multiple jurisdictions. The initial difficulties experienced with expanding into the catchment of an adjacent health service region (Goulburn Valley Health), however, suggest that greater investment in developing strong relationships with stakeholders may be necessary in such circumstances. With the exception of these potential limitations, however, the findings of this study - including the conceptual model of the stages of service expansion that has been developed - are readily generalisable to other rural PHC settings.
A final limitation of this study was related to the last-minute decision by one GP not to take part in the study, reflecting the demands of being a busy rural clinician. Nonetheless, stakeholders from all sites - including sites that were no longer sustained - participated in the study.
This research captured a richness of data, analysis of which revealed a staged process in the successful expansion of PHC services. A range of key environmental enablers and essential service requirements were found to come in to play at different stages of expansion. Critically important at all stages, however, was community engagement.
Acknowledgements
The research reported in this article is a project of the Australian Primary Health Care Research Institute, which is supported by a grant from the Australian Government Department of Health and Ageing. The information and opinions contained in it do not necessarily reflect the views or policy of the Australian Primary Health Care Research Institute or the Australian Government Department of Health and Ageing. The authors would also like to acknowledge the support and generosity of participants who made their time available for interviews, and the assistance of Dr Matthew McGrail with preparation of the map.
References
1. NSW Ministerial Advisory Committee on health services in smaller towns. A framework for change. Sydney: NSW Government, 2000.
2. McLean R. Small rural hospitals and casemix funding: Victoria, 1993-94. Australian Journal of Rural Health 1994; 2: 33-36.
3. Australian Institute of Health and Welfare. Review and evaluation of Australian information about primary health care: a focus on general practice. Canberra: AIHW, 2008.
4. Humphreys J, Dixon J. Access and equity in Australian rural health services. In: J Healy, M McKee (Eds). Accessing health care: responding to diversity. Oxford: Oxford University Press, 2004; 89-107.
5. Humphreys JS, Mathews-Cowey S, Rolley F. Health service frameworks for small rural and remote communities - issues and options. Armidale: University of New England, 1996.
6. Humphreys JS. Health service models in rural and remote Australia. In: D Wilkinson D, I Blue (Eds). The new rural health: an Australian text. New York: Oxford University Press, 2002; 273-296.
7. Snowball K. Multipurpose services - a potential solution for rural health and aged care. Australian Journal of Rural Health 1994; 2: 37-40.
8. New South Wales Rural Doctors Network. Easy Entry, Gracious Exit. Newcastle: NSW RDN, 2003.
9. van Haaren M, Williams G. Central Australian nurse management model (CAN Model): a strategic approach to the recruitment and retention of remote-area nurses. Australian Journal of Rural Health 2000; 8: 1-5.
10. Wakerman J, Humphreys JS. Sustainable primary health care services in rural and remote areas: innovation and evidence. Australian Journal of Rural Health 2011; 19: 118-124.
11. Department of Health and Ageing. State of corporatisation: a report on the corporatisation of general practices in Australia. Canberra: DoHA Medicare financing and analysis branch, 2012.
12. Asaid A, Riley K. From solo practice to partnering - the evolution of the Elmore Model of Primary Health. Australian Family Physician 2007; 36: 167-169.
13. Buykx P, Humphreys JS, Tham R, Kinsman L, Wakerman J, Asaid A, et al. How do small rural primary health care services sustain themselves in a constantly changing health system environment? BMC Health Services Research 2012; 12: 81.
14. Rural Doctors Association of Victoria. Submission re: RDAA application for collective negotiation A 91078. (Internet) 2008. Available: http://www.rdav.com.au/sites/default/files/public/2008%2520RDAV%2520submission%2520to%2520ACCC%2520for%2520RDAA%2520Authorisation_20140811105503.pdf (Accessed 1 February 2016).
15. Humphreys JS, Fraser M. The trialing and evaluation of alternative models of health services in small rural and remote communities. Bendigo: LaTrobe University, 2001.
16. Tham R, Humphreys J, Kinsman L, Buykx P, Asaid A, Tuohey K, et al. Evaluating the impact of sustainable comprehensive primary health care on rural health. Australian Journal of Rural Health 2010; 18: 166-172.
17. Ward BM, Buykx PF, Tham R, Kinsman L, Humphreys JS. Investing in longitudinal studies of primary healthcare: what can we learn about service performance, sustainability and quality? Rural and Remote Health (Internet) 2014; 14: 3059 (Accessed 26 February 2016).
18. Braun V, Clarke V. Using thematic analysis in psychology. Qualitative Research in Psychology 2006; 3: 77-101.
19. Wakerman J, Humphreys JS, Wells R, Kuipers P, Entwistle P, Jones J. Primary health care delivery models in rural and remote Australia: a systematic review. BMC Health Services Research 2008; 8: 276.
20. Wakerman J, Humphreys JS, Wells R, Kuipers P, Jones JA, Entwistle P, et al. Features of effective primary health care models in rural and remote Australia: a case-study analysis. Medical Journal of Australia 2009; 191: 88-91.
21. Bath J, Wakerman J. Impact of community participation in primary health care: what is the evidence? Australian Journal of Primary Health 2015; 21: 2-8.
22. Chilaka MA. Ascribing quantitative value to community participation: a case study of the Roll Back Malaria (RBM) initiative in five African countries. Public Health 2005; 119: 987-994.
23. Hutchison B, Levesque JF, Strumpf E, Coyle N. Primary health care in Canada: systems in motion. Milbank Quarterly 2011; 89: 256-288.
24. Greenhalgh T, Robert G, Macfarlane F, Bate P, Kyriakidou O. Diffusion of innovations in service organizations: systematic review and recommendations. Milbank Quarterly 2004; 82: 581-629.

