Rural and remote medical practitioner shortage in Australia has been a critical issue for many decades1. It has led to considerable research into effective strategies for recruiting and retaining rural doctors. Rural origin is a predictor for rural practice2,3. An association between rural exposure during medical school and increased likelihood of working rurally has been postulated2,3. As a consequence, the Australian Government has invested heavily in strategies aimed at providing medical students with rural placements during their studies4. These strategies include the Rural Undergraduate Support Program, the John Flynn Placement Program and the Rural Clinical School (RCS) Program5,6.
Through RCSs, Australian medical students are able to undertake a year or more of their clinical training in regional and rural areas. Although there remains some conjecture, positive rural student placement experience is increasingly recognised to promote careers in rural practice7-9. Social and financial supports may be important to students' experience of these placements, in addition to factors such as the quality of the medical education provided, the quality of the clinical experience, and greater exposure to patients. Little is known about the interaction between perceptions on financial supports and intentions to work rurally.
Rural placements remove students from their social context support structures, often during difficult study periods10. Furthermore, recent medical student wellbeing studies have demonstrated that whilst medical students are similar to the general population when commencing medical school, as they progress in their courses they begin to exhibit lower psychological wellbeing than age-matched peers11. As such, equity in accessibility, education and support is essential to ensure that students undertaking rural clinical placements are not disadvantaged financially, academically or psychologically10.
RCSs provide a diverse range of supports to students undertaking rural clinical placements10. Support offered to students differs between each RCS but may include access to counsellors, mentoring programs, free or cheap accommodation, travel allowances or reimbursements, face-to-face teaching days and teleconferencing facilities. In addition to student supports, access to resources such as library services can be compromised in rural and remote locations due to external factors such as logistics. In this study, uncompromised access to learning resources and services are also considered to support RCS students. The aim of this study is to gain insight into how students perceive the supports they receive through their RCSs and identify potential associations between these supports and intentions to work rurally.
Australian RCSs and regional medical schools (RMSs) have collaborated through the Federation of Australian Medical Educators (FRAME) to develop an annual national questionnaire collecting demographic, educational, experiential and intentional data from students completing their rural clinical school experience12. The aims of the FRAME survey are to support RCSs/RMSs to report to the RCS Commonwealth parameters, to progress knowledge creation regarding rural medical education and to provide external groups with opportunity to commission research12.
The survey tool includes quantitative and qualitative data such as demographics, experience of rural placement, intentions to work rurally and clinical school preferencing. Intention to practise in rural areas was measured through two questions. First, a five-point Likert scale ('strongly disagree' to 'strongly agree') was included for the statement 'I intend to do my internship in a rural/remote area'. Second, participants were asked about their preferred geographical practice location within Australia on completing their training by utilising the Remoteness Areas (RA) classification system (ie major city, inner regional area or large town (25 000-100 000), small rural town (10 000-24 999), small rural or remote community (<10 000) or very remote centre/area)13. Additional questions were integrated into the 2012 FRAME survey by the Australian Medical Students' Association. These questions aimed to investigate students' opinions about perceived support during their rural placements using five-point Likert scales. Questions asked students to rate their cost of living for specific items such as accommodation with the costs in the previous year (rated from 1='significantly worse off' to 5='significantly better off'), and also to indicate their agreement with statements indicating that they felt well supported financially (rated from 1='strongly disagree' to 5='strongly agree').
Australian medical students enrolled in RCSs in 2012 were invited to complete the survey between September 2012 and January 2013 as they left their RCS placement, using either a paper-based survey in their study groups, or an online survey via a standardised email sent by an administrative staff member from their university. The survey took approximately 20 minutes to complete. De-identified data from the survey were provided to the research group for statistical analysis.
Analyses were conducted using Stata v13.1 (StataCorp; http://www.stata.com). Correlations are reported as Spearman rank correlations as the underlying variables are not normal. Ordinal logistic regression was used to identify associations between the outcomes 'intention to complete a rural internship' and 'intention to practice in a rural setting' and predictors. The proportional odds assumption for both models was validated (using Stata's brant command) and no evidence of model violation was found (p>0.37). Results are presented as odds ratios (ORs) with 95% confidence intervals (CIs). A p value of less than 0.05 (two-tailed) is considered statistically significant.
Ethics approval
Ethics approval for the 12 RCS/RMSs participating in the study was granted through each relevant university ethics committee, led by Flinders University Social and Behavioural Research Ethics Committee (project number 4098).
From the medical students who completed a RCS placement in 2012, 454 of a potential 701 students participated in the survey, producing a response rate of 64.8%. Of these, 41.5% were male. The circumstances of the participants are shown in Table 1.
When asked to take into account financial and other supports provided by the RCS and then indicate relative status compared to remaining at the same site as the previous year, 56.4% of RCS students reported that they were better off with regards to accommodation costs and 25.6% reported no change (Table 2). The cost of utilities (after reimbursement) followed a similar pattern, with 47.1% feeling that they were better off, and 35.9% (n=156) reporting no change. High proportions of students also reported being equal or better off than the previous year when considering access to prescribed texts (77.5%), counselling services (75.9%), internet access at home (74%), clinical training labs (73%) and relocation costs (71.6%). Somewhat lower proportions of students described being equally or better off in relation to access to library resources (67%) and course-related travel costs (60.7%).
The majority of students felt financially well supported (60.5%) (Table 3). This variable correlated well with accommodation costs (rho=0.50). There was no correlation between accommodation costs and perceived academic support (rho=0.09). The majority of students (79.2%) felt well supported academically by their RCS, despite 29.6% experiencing some degree of academic isolation during their rural clinical placement (Table 3). Results show that 79.1% of respondents felt well supported overall by their RCS. However, only 42.4% of students agreed that the RCS informed them of health and counselling services, despite 37.1% of students describing feeling socially isolated during their RCS placement and 19.2% of students indicating the RCS placement did not impact positively on their wellbeing.
Ordinal multivariate logistic regression showed that students with a positive effect on wellbeing placement (OR=1.38 (95%CI:1.07-1.80)) or considered themselves to be rural (OR=1.64 (95%CI:1.13-2.38)) or who had a fee-paying position in medical school (OR=2.16 (95%CI:1.18-3.96)) were more likely to express interest a rural internship (Table 4). Those who perceived themselves as socially isolated during rural clinical training were less likely to express interest in a rural internship (OR=0.82 (95%CI:0.70-0.97)).
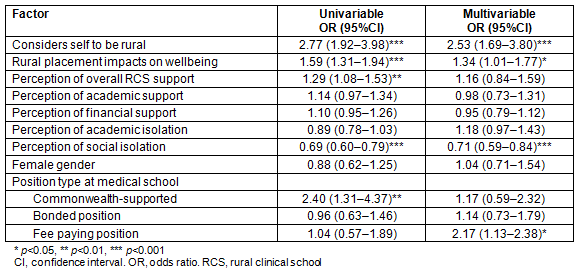
Similarly, ordinal multivariate logistic regression showed that students with a positive effect on wellbeing placement (OR=1.34 (95%CI:1.02-1.77)), or who considered themselves to be rural (OR=1.63 (95%CI:1.13-2.33)), or who had a fee-paying position in medical school (OR=2.17 (95%CI:1.13-2.38)) were more likely to express interest in working in rural and remote areas on completion of training (Table 5). Those who perceived themselves as socially isolated during rural clinical placement were less likely to express interest in working in rural and remote areas on completion of training (OR=0.71 (95%CI:0.96-0.88)). There is a moderate correlation between intention to complete a rural internship and preference for more rural practice on completion of training (rho=0.33). Further analysis showed a strong negative correlation between perceived academic support and reported academic isolation (rho= -0.50), and between perceived impact of rural placement on wellbeing and social isolation (rho= -0.49).
Table 1: Types of medical school place of survey participants
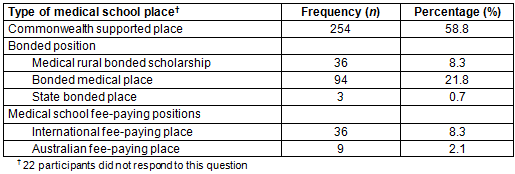
Table 2: Perceptions on relative status at rural clinical school compared with previous university campus after any university reimbursement
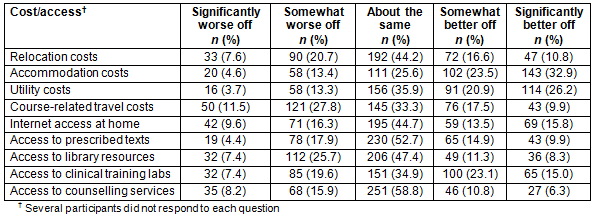
Table 3: Perceptions on supports offered by rural clinical schools
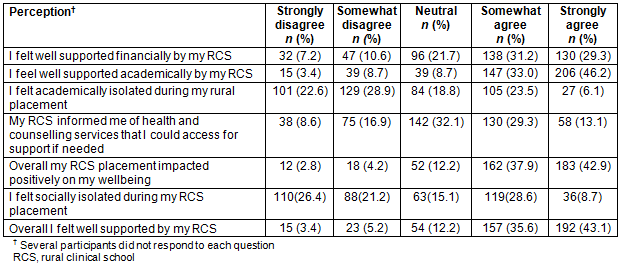
Table 4: Factors associated with intention to complete a rural internship
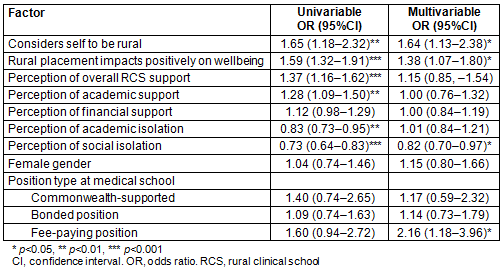
Table 5: Factors associated with preference for practice in a small rural, remote or very remote area within Australia
Discussion
This study demonstrates that students' perceptions of RCS supports are generally positive; however, positive perceptions of financial, educational and psychological supports do not translate to rural career intent. In contrast, self-perceptions of improved wellbeing during RCS placements is a key contributor influencing intentions to undertake a rural internship (OR=1.38 (95%CI:1.07-1.80)) or to practise rurally after vocational training (OR=1.34 (95%CI:1.01-1.77)).
A positive perception of student wellbeing was also associated with a decreased likelihood of social isolation (rho= -0.49). Previous studies have found that social isolation is an important concern for students considering rural placements14. Shared student accommodation may be a useful strategy in reducing students' perceptions of social isolation15. The negative association between perceived social isolation and intentions to complete a rural internship (OR=0.82 (95%CI:0.70-0.97)) or work rurally after vocational training (OR=0.71 (95%CI:0.59-0.84)) supports the value of investing in community engagement strategies for RCS students. RCSs have developed multi-level community engagement strategies that see students bonding to their communities through personal relationships, individual formal connections, facilitated collective structured activities and strategic regional engagement functions16. Recognising recent beyondblue findings that medical students and doctors situated in rural areas have lower levels of mental wellbeing than their city peers17, the authors recommend universal provision of information regarding health and counselling services by RCSs to improve on the current reported 42.4% of students who feel informed. Further work is required to build on medical student clinical resilience during medical school18.
Financial factors have been identified as a perceived barrier for students considering undertaking RCS training10. Evidence that medical students are well supported financially is reassuring for rural clinical school leaders and policy makers as it is an Australian Government requirement that RCS experiences are made universally accessible to domestic students by negating undue financial burdens19. Student feedback indicating adequate support to facilitate equivalent academic achievement meets both Australian Government and Australian Medical Council expectations20. For example, it is now commonplace in medical schools across Australia to access clinical skills training in simulation laboratories from early in pre-clinical and throughout the medical course. Health Workforce Australia has invested considerably in clinical simulation infrastructure and equipment for health professional student training in recent years21. The results of this study are indicative that this investment has led to reasonable access to clinical simulation facilities for medical students based in rural Australia.
The effect of student support variables on internship preference appears to be comparable to the effect on preference of practice location on completion of training. Although there is moderate correlation between these variables (rho=0.33), it may be possible that internship preferences and final practice location preference are different outcomes since medical students have previously indicated concern that rural internship will negatively influence their chances of entering specialty training18. Another factor influencing interest in a rural internship includes students' social circumstances including the availability of social supports14.
Self-reported rural background was associated with preferencing a rural internship (OR 1.64, 95%CI:1.13-2.38) and final practice location (OR 1.63, 95%CI:1.13-2.33). This finding is consistent with previous research and highlights the importance of RCS key performance indicators which seek to ensure equity of admission to medical school for rural-origin students2,8. This has been achieved in Australian medical schools through systems including both quotas and weighting of rural student academic performance22.
Facilitation of positive experiences in rural locations by RCSs has been seen as a key strategy in addressing rural health workforce shortages. Strengths of this research include representation from 14 medical schools across Australia. It is envisaged that this data will contribute to a growing body of research on RCS experiences and understanding of the effect of rural exposure whilst at medical school and rural career uptake. Although a response rate of 64.8% is reasonable, a little over one-third of the students did not complete the survey. Another possible limitation of this study is that data are collected immediately following RCS placements, so no account was made of the impact of follow-on urban placement experiences. Further, this study did not adjust for students (if any) who may have been attending an RCS in the previous year. Even if one or a few more students would have attended an RCS in the previous year, it is unlikely that this would have made a significant impact on the results of this study. Additionally, due to the anonymity of participants we were unable to access the extent of financial support provided by different universities and correlate this with the results.
Maximising students' wellbeing whilst on rural placements may improve future rural career intentions. Further research should investigate the factors influencing student wellbeing and whether there are differences in how rural- and urban-origin students develop and maintain resilience23. This would shed light on strategies RCSs should adopt to strengthen social supports for students, taking into consideration the diversity of the geography and communities in which they are placed.
This study provides information for universities and policy-makers on students' perceptions of RCS supports and their relationship to rural practice intentions.
Generally students perceived the supports offered positively, and in this study perceived financial support did not correlate with intent to practise rurally following graduation. However, providing medical students with appropriate financial supports so that all interested students can access the RCS program remains an important philosophy of the program. For the purpose of recruitment to rural practice, this study demonstrated that student wellbeing is an important factor.
References
1. Health Workforce Australia. Health Workforce 2025 volume 1. Doctors, nurses and midwives. Adelaide: Health Workforce Australia, 2012.
2. Jones M, Humphreys J, Prideaux D. Predicting medical students' intentions to take up rural practice after graduation. Medical Education 2009; 43(10): 1001-1009.
3. Dunbabin J, Levitt L. Rural origin and rural medical exposure: their impact on the rural and remote medical workforce in Australia. Rural and Remote Health (Internet) 2003; 3(1): 212. Available: www.rrh.org.au (Accessed 12 October 2014).
4. Strasser R. Advances in rural medical education in three countries: Canada, the United States and Australia. Education for Health 2005; 18(3): 405-415.
5. Department of Health and Ageing. Workforce education and training - rural clinical schools. (Internet) 2014. Available: http://www.health.gov.au/internet/main/publishing.nsf/Content/work-st-rcs (Accessed October 2014).
6. Young L, Kent L, Walters L. The John Flynn Placement Program: evidence for repeated rural exposure for medical students. Australian Journal of Rural Health 2011; 19(3): 147-153.
7. Kondalsamy-Chennakesavan S, Eley D, Ranmuthugala G, Chater A, Toombs M, Darshan D, et al. Determinants of rural practice: positive interaction between rural background and rural undergraduate training. Medical Journal of Australia 2015; 202(1): 41-45.
8. Walker J, DeWitt D, Pallant J, Cunningham C. Rural origin plus rural clinical school placement is a significant predictor of medical students' intention to practice rurally: a multi-university study. Rural and Remote Health (Internet) 2012; 12: 1908. Available: www.rrh.org.au (Accessed October 2014).
9. Barrett F, Lipsky M, Lutfiyya M. The impact of rural training experiences on medical students: a critical review. Academic Medicine 2011; 86(2): 259-263.
10. Australian Medical Students' Association. Rural Clinical Schools Policy. (Internet) 2012. Available: http://media.amsa.org.au.s3.amazonaws.com/policy/2012/201210_rural_clinical_schools_policy.pdf. (Accessed 12 October 2014).
11. Hillis J, Perry W, Carroll E, Hibble B, Davies M, Yousef J. Painting the picture: Australasian medical student views on wellbeing teaching and support services. Medical Journal of Australia 2010; 192(4): 188.
12. Federation of Rural Australian Medical Educators (FRAME). Frame survey study. (Internet) 2012. Available: http://www.ausframe.org/index.php/2012-06-15-05-28-07/national-rcs-project-secure-data-linkage. (Accessed 12 October 2014).
13. McGrail M, Humphreys J. Geographical classifications to guide rural health policy in Australia. Australia and New Zealand Health Policy 2009; 6(1): 28.
14. Deaville J, Grant A. Overcoming the pull factor of convenient urban living - perceptions of rural general practice placements. Medical Teacher 2011; 33(4): e211-e217.
15. Health Workforce Australia. A framework for effective clinical placements in rural and remote primary care settings. Adelaide: Australian Health Workforce Institute, 2013.
16. Walters L, Stagg P, Conradie H, Halsey J, Campbell D, D'Amore A. Community engagement by two Australian Rural Clinical Schools. Australasian Journal of University-Community Engagement 2011; 6(2): 27-56.
17. Beyondblue. National mental health survey of doctors and medical students. (Internet) 2013. Available: http://www.beyondblue.org.au/docs/default-source/research-project-files/bl1132-report---nmhdmss-full-report_web (Accessed 5 April 2016).
18. Greenhill J, Fielke K, Richards J, Walker L Walters L. Towards an understanding of medical student resilience in longitudinal integrated clerkships. BMC Medical Education 2015; 15: 137.
19. Department of Health and Ageing. Regional Health Strategy: funding parameters for rural clinical schools. Canberra: Commonwealth Government, 2001.
20. Australian Medical Council Limited. Standards for assessment and accreditation of primary medical programs by the Australian Medical Council. (Internet) 2012. Available: http://www.amc.org.au/images/Accreditation/FINAL-Standards-and-Graduate-Outcome-Statements-20-December-2012.pdf (Accessed June 2015).
21. Health Workforce Australia. Simulated learning: expanding simulation capacity. (Internet) 2013. Available: http://www.hwa.gov.au/our-work/build-capacity/simulated-learning-environments-program (Accessed 15 June 2014).
22. Stagg P. Medical School Admissions policies targeting rural students. Wonca Rural Medical Education Guidebook. (Internet) 2014. Available: http://www.globalfamilydoctor.com (Accessed 15 June 2015).
23. Eley D, Cloninger R, Walters L, Laurence C, Synnott R, Wilkinson D. The relationship between resilience and personality traits in doctors: implications for enhancing wellbeing. PeerJ Computer Science 2013; 1: e216.



