The terms 'rural health' and 'remote health' are often used without explicit definitions of either term. There is a frequent assumption of a shared language in rural and remote health policy, practice, research and education. Yet rural health and remote health engage professionals from a broad range of disciplinary backgrounds and may have quite different goals, training, practice standards, ways of working and underlying understandings of rural health and remote health1. Some authors view rural and remote health as distinctive in terms of context, practice and research2,3. Others discount geographical influence and suggest that health differentials are explained by socioeconomic status or the social determinants of health4,5. Postmodern perspectives suggest that hybrid forms of 'rural' have dissolved previous rigid categories6,7. The lack of common meaning is rarely addressed. There is a range of possible explanations for these variations. These include the multidisciplinary and generalist nature of practice in remote and rural settings and the fact that relatively few health professionals or academics are specifically trained in rural health or remote health.
Until recently, little was published addressing the distinct features of remote health3 or remote medicine8. A comprehensive literature review described remote health within a geographical context characterised by relatively higher mortality and morbidity, higher proportion of the population that is Indigenous, and a more dispersed population than in rural areas3. Service delivery in 'remote' areas is characterised by an undersupply of health workforce, significantly poorer access to services, a very strong multidisciplinary team approach with overlapping roles, and a greater reliance on visiting service models. Other distinct features of remote health practice include generally non-procedural medical practice and a high degree of general practitioner substitution, especially utilising remote area nurses (RANs) and Aboriginal health workers (AHWs). Based on an alternative method of expert consensus, Smith et al. described remote medical practice as characterised by nine distinct attributes, including a cross-cultural context, isolation, the use of telehealth, the need for increased clinical acumen, extended practice, a strong multidisciplinary approach, public health and security considerations, and predominantly non-private employment8.
However, empirical evidence that describes the nature and distinct features of remote health, and what makes it different to rural health, is lacking. The aim of this article is to contribute to this literature by reporting on findings from a major national study that sought to better understand what is meant by 'rural health' and 'remote health'1. Specifically, this article seeks to build the evidence base about the key distinctive characteristics of remote health. Identification of key characteristics of remote health can be used to guide the education of health workers, increase the understanding of important differences between rural health and remote health for policymakers, and for health authorities who govern the nature and quality of practice.
A total of 59 rural health experts from across Australia were identified by the research team (based on experience, tenure, reputation and at least 5 years work in rural health and/or remote health) and approached for an interview. Selection was purposive to ensure coverage of four key domains of practice: academic, policy, practitioner and advocate, as well as to ensure geographical diversity. Within each category were professionals who were active or had experience in remote areas and in Aboriginal health.
Each of the 59 potential respondents was contacted via email or telephone and sent an information statement. Eight refused, one did not attend and two agreed to participate but a mutually feasible appointment time could not be organised. The remaining 48 people were interviewed. An information statement, consent form, brief questionnaire and a long and summary version of a draft conceptual framework for rural and remote health were sent to each interviewee9. Three respondents would agree only to be interviewed together. Because group dynamics may alter response, this interview was not included in the final analysis. Thus 45 participants completed a useable, individual, face-to-face interview.
Respondents were also asked to complete a short questionnaire before or at the beginning of the interview. This questionnaire asked respondents to rate a set of 16 characteristics, derived from the extant literature2,3,8,10 , on the basis of whether each differed between remote health and rural health on a scale of 1 ('not different') to 5 ('extremely different'). Demographic questions sought age, gender, predominant employment type and Indigenous status. Respondents were also asked if they worked predominantly in rural health, in both rural and remote health or predominantly in remote health, and in another question if they worked predominantly in Aboriginal health.
Data from the questionnaire were coded and analysed utilising the Statistical Package for the Social Sciences v19.0 (SPSS; http://www.spss.com). Descriptive statistics were used along with t-test, ANOVA and Pearson's r to test for statistically significant correlations between characteristics perceived to be different in remote practice and demographic characteristics of participants. All interviews were recorded, transcribed and a content analysis conducted with the assistance of NVivo v9 (QSR International; http://www.qsrinternational.com).
Ethics approval
The study was approved by the University of Melbourne School of Rural Health Human Ethics Advisory Group (1033251.1).
Questionnaire data
A total of 41 questionnaires were completed. This was a diverse sample; the characteristics of these respondents are presented in Table 1. Of the 41 survey participants, 21 were female and three were Aboriginal or Torres Strait Islander. Ten were aged less than 50 years, a little more than half (23) were aged between 51 years and 60 years, and eight were older. Half (21) identified themselves as working predominantly as academics while nine, six and five indicated that they worked as practitioners, in policy and in advocacy, respectively. Most, however, listed more than one of these, and sometimes all of these categories. Thirteen stated they worked in rural health, 10 in remote health and 18 in both. Twenty-three participants indicated that they worked in Aboriginal and/or Torres Strait Islander health, with eight predominantly in this area. Respondents had worked in rural health and/or remote health for up to 36 years, with means of 13 years and 8 years, respectively.
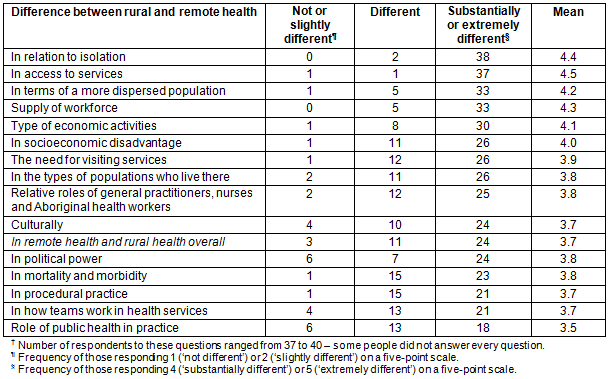
The respondent group perceived each of the nominated characteristics as different in remote health compared to rural health. Table 2 summarises the responses about the distinguishing characteristics. Means for each of these items ranged from 3.5 to 4.5 ('different' = 3, 'substantially different' = 4 and 'extremely different' = 5). Almost all participants indicated that isolation and access to services are substantially or extremely different in remote health, and the majority reported that a more dispersed population, the supply of workforce and the type of economic activities were substantially or extremely different. More than half indicated that overall remote health was substantially or extremely different, and specifically in relation to the need for visiting services, the types of populations who live there, the relative roles of general practitioners, nurses and Aboriginal health workers, culturally, in political power, mortality and morbidity. Fewer, but approximately half, suggested that procedural practice, how teams work in a health service and the role of public health in practice were also substantially different.
Responses exhibited a high degree of consistency. Together, all 16 items had an inter-reliability coefficient of 0.87 using Cronbach's alpha. Compared to men, women indicated that how teams work in remote health was more different, but were otherwise similar to men in their responses. Age was not associated with perceiving more differences between remote health and rural health. Compared to those working in rural health, those working in remote health perceived that there were more differences in mortality and morbidity. Those working in Aboriginal health reported more extreme differences in a dispersed population, type of population, mortality and morbidity, economic activities, socioeconomic disadvantage, political power and overall differences between remote health and rural health. This suggests that experience in remote and especially Aboriginal health leads to stronger identification of remote health as distinct from rural health.
Table 1: Characteristics of the sample
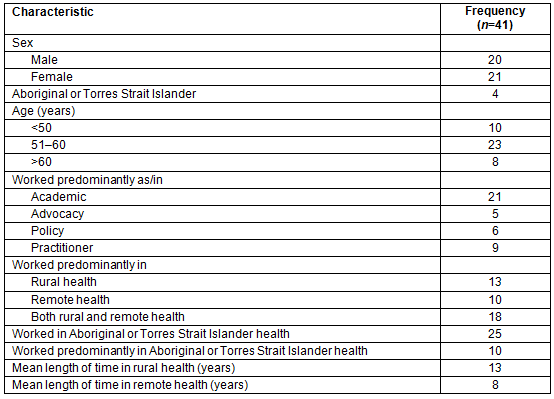
Table 2: Frequencies and means of questions asking about specific differences between remote health and rural health (n=41)?
Interview data
Respondents were also asked in the interview if remote health differs from rural health, and, if so, how the two differ from each other. All but four indicated that they differed, with one stating they were the same; the remaining three talked about them being similar.
For some interviewees, rural health and remote health were part of a continuum wherein '... the nature of remote health ... is magnification of all those [rural] problems - distances are further, number of staff is smaller, expectations remain the same'. They talked about remote health having more of the features that distinguished rural from urban, including being more isolated, further from other services, more of a 'gold fish bowl' with poorer health outcomes, fewer services and less workforce.
More respondents suggested that 'rural health and remote health are two different things, and I think they are as distinctly different as rural and metropolitan'. These respondents spoke about remote health in terms of remoteness, isolation, population size, proportion of the population who were Aboriginal, health outcomes, mortality and morbidity rates, economic opportunities, social life and different models of health care (fly-in fly-out services and more focus on prevention). Being completely different was a result of a smaller, more dispersed population more distant from other places and services that resulted in very different healthcare models and practices and created 'different societies'. Several interviewees indicated that remote residents were different, with different attitudes, cultures and relationships.
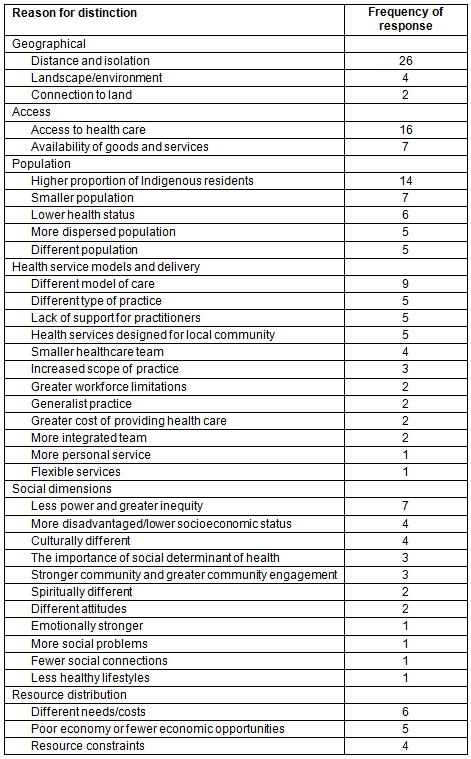
Despite these differences, understandings of remote health commonly focused on distance and isolation (26); access to services (16), particularly specialist and emergency medical services; a higher proportion of Aboriginal and Torres Strait Islander residents (14); a different model of health care (9); a range of factors that influenced healthcare delivery including a smaller team, a more integrated team, a broad scope of practice and more responsibility; a smaller, more dispersed population; and a range of terms to describe power, inequity and disadvantage (Table 3). Interviewees working predominantly in the policy area tended to make less of a distinction between them compared to practitioners. Those arguing most strongly about the distinctive nature of remote health were the practitioners and academics working in remote health: 'remote is ... not well understood unless you've actually been there, worked there and are passionate about Indigenous health, especially in Australia'.
Regardless of how respondents viewed rural health and remote health, all indicated that both rural and remote environments exhibited significant heterogeneity. For example, most identified distinctions between remote Indigenous communities, remote mining towns and residents on remote stations, acknowledging the different health outcomes and services required for different types of remote settlement. Furthermore, the sorts of places respondents classified as remote differed. Some respondents identified rural and remote places based on settlement types and activities; hence 'rural' was described as the typical farming area community with its own small health service, while 'remote' was equated to remote Indigenous communities with fly-in fly-out services. While a few participants spoke of small towns 45 minutes driving distance from a regional centre as remote, others indicated that towns with services 1200 km from a regional centre were not remote. Some Tasmanian respondents spoke about island cultures and the isolation of small islands off the mainland, which tend to be forgotten. Despite this considerable diversity, proximity to other places and access to services underpinned many answers.
Table 3: Reasons given at interview for why remote health differs from rural health, and frequency of response
A large majority of leading Australian experts perceived that remote health is different to rural health. Whilst there are marked differences in practice and experience between frontline clinicians, academics and policymakers, typically most experts in this study had broad experience across multiple domains of clinical practice, policy, advocacy and the academy. Many were in senior positions and were key decision makers. Importantly, those working in remote and particularly Aboriginal health identified greater distinctions, suggesting that experience of working 'remote' highlights these differences.
In summary, rural and remote health experts considered that remote populations are smaller, more isolated and more highly dispersed. Political power is less in remote areas; the nature of economic activity varies between rural and remote areas; and socioeconomic disadvantage is higher, especially in Aboriginal and Torres Strait Islander communities. As a result, morbidity and mortality are generally worse in remote areas. There are also workforce supply problems (particularly in relation to staff turnover and retention) and decreased access to health services in remote areas. Different models of service delivery have developed in response to these conditions. Remote areas rely more heavily on visiting services, with differences in the relative roles of health professionals. In remote areas, practice is characterised by smaller integrated teams, less procedural activity than in rural areas and a stronger emphasis on public health approaches. Interview data confirmed these differences and suggested that remoteness, population and resultant access characteristics underpinned them.
Do these distinctive features mean that remote health is a distinct discipline? A number of authors have referred to criteria for recognition of a distinct discipline11,12. They relate to the formation of an academic body representing the discipline, presence of an intellectually rigorous training program, emergence of a unique literature, and recognition from outside the discipline. The Australian College of Rural and Remote Medicine recognises a specific discipline of remote medicine, and accordingly offers specific vocational training in this area. Flinders University offers postgraduate awards in remote health practice. There is a small but growing literature specifically around remote health. There has been an acute recent recognition of issues specific to remote Australia generally13. This study provides solid evidence that some of Australia's leading rural health experts understand the distinctive nature of remote health, characterised by issues relating to geographical, demographic and socioeconomic context, services and workforce.
More importantly, a definition and description of the specific characteristics and raison d'etre of the discipline of remote health, as distinct from rural health, is potentially very useful for policymakers, health planners, health professionals and for teachers and researchers. For teachers, a better and more detailed understanding of the distinct characteristics of remote health assists in the appropriate education of the remote health medical and allied health workforce. Researchers benefit from understanding this complex environment accurately in order to ensure that the design, implementation and translation of research are appropriate and effective. For health professionals, one very effective example that accounts for these differences is the CARPA standard treatment manua14. For two decades, these clinical protocols have been developed in appreciation of the nature of the population and epidemiology in remote areas, especially Indigenous communities, the multidisciplinary and often unstable workforce, and difficulties with service access generally15,16. Policymakers and planners are mandated to direct resources and programs to address the health needs of populations in these areas. They need to account for the distinctive features of this challenging environment, including the costs of delivering services and attendant infrastructure, appropriate workforce planning and relevant workforce preparation. This knowledge will assist in guiding the monitoring and evaluation of the effectiveness of policies, programs and practices in remote areas in order to appropriately meet population health needs. It is through better understanding of the remote context and through timely and commensurate response to health need that we will ensure a more equitable distribution of resources and health outcomes across this large and imposing continent.
References
1. Bourke L, Taylor J, Humphreys JS, Wakerman J. Rural health is subjective, everyone sees it differently: understandings of rural health among Australian stakeholders. Health and Place 2013; 24: 65-72.
2. Bourke L, Sheridan C, Russell U, Jones G, DeWitt D, Liaw ST. Developing a conceptual understanding of rural health practice. Australian Journal of Rural Health 2004; 12: 181-186.F
3. Wakerman J. Defining remote health. Australian Journal of Rural Health 2004; 12: 210-214.
4. Beard JR, Tomaska N, Earnest A, Summerhayes R, Morgan G. Influence of socioeconomic and cultural factors on rural health. Australian Journal of Rural Health 2009; 17(1): 10-15.
5. Dixon J, Welch N. Researching the rural-metropolitan health differential using the 'social determinants of health'. Australian Journal of Rural Health 2000; 8: 254-260.
6. Heley J, Jones L. Relational rurals: some thoughts on relating things and theory in rural studies. Journal of Rural Studies 2012; 28: 208-217.
7. Woods M. Rural geography: blurring boundaries and making connections. Progress in Human Geography 2009; 33(6): 849-858.
8. Smith JD, Margolis SA, Ayton J, Ross V, Chalmers E, Giddings P, et al. Defining remote medical practice: a consensus viewpoint of medical practitioners working and teaching in remote practice. Medical Journal of Australia 2009; 188: 159-161.
9. Bourke L, Humphreys JS, Wakerman J, Taylor J. Understanding rural and remote health: a framework for analysis in Australia. Health and Place 2012; 18(3): 496-503.
10. Kulig JC, Andrews ME, Stewart NL, Pitblado R, MacLeod ML, Bentham D, et al. How do registered nurses define rurality? Australian Journal of Rural Health 2008; 16: 28-32.
11. Smith J, Hays R. Is rural medicine a separate discipline? Australian Journal of Rural Health 2004; 12: 67-72.
12. Strasser R. Rural general practice: is it a distinct discipline? Australian Family Physician 1995; 24: 870-876.
13. Walker BW, Porter DJ, Marsh I. Fixing the hole in Australia's heartland: how government needs to work in remote Australia. Alice Springs: Desert Knowledge Australia, 2012.
14. Central Australian Rural Practitioners Association. CARPA standard treatment manual. (6th Edn). Alice Springs, NT: Centre for Remote Health, 2014.
15. Reddy S, Herring SE. Can Australia's clinical practice guidelines be trusted? Medical Journal of Australia 2015; 202(9): 475.
16. Wakerman J, Skov S, Williams N. Time to move beyond clinical practice guidelines. [Letter] Medical Journal of Australia 2001; 175: 287-288.



