'Telehealth' is a term that refers to the electronic delivery of clinical and educational health resources to remote regions1 . Telehealth has been used extensively in recent years in developed countries for both clinical and educational purposes2-5. Linking patients in rural and underserved areas to remote physicians may address the lack of access to quality care6,7 and poor health outcomes8, which are common in these regions. In addition to connecting distant providers with international specialists for clinical support, telehealth could also increase communication between regional healthcare facilities, thereby strengthening local professional interactions and mitigating the sociocultural differences that intercountry interactions typically entail9,10. In addition to providing clinical support, telehealth offers a means for distance learning and training. Continuing medical education (CME) opportunities through telehealth may encourage providers to remain in or return to remote and underserved areas11,12. Telehealth programs have been found to be cost effective for certain patient populations13,14 and cost neutral for others3, and are well received by patients and providers alike15,16. Certain barriers exist that make the implementation of telehealth programs challenging. Limited Internet connectivity, unreliable electrical power, low bandwidth, lack of technical experience, and cultural and language barriers are often cited reasons that telemedicine programs are slow to succeed17.
Honduras in particular lacks adequate access to health services, with a coverage rate of nine physicians per 10 000 population in 200818. Approximately 50% of the population lives in rural areas, which are especially deficient in access to health care and basic health infrastructure. In 2013, the infant mortality rate in Honduras was 18 deaths per 1000 live births and the under-five mortality rate was 19 per 1000 live births, significantly higher than the regional average19. These statistics suggest that Honduras would greatly benefit from the establishment of a telehealth network, particularly one that aims to improve regional professional communication. Little data exist regarding telehealth in Honduras, particularly networks that connect providers within the country.
The purpose of this study was to assess the feasibility of establishing a telehealth network between underserved sites in Honduras and the Medical University of South Carolina (MUSC). The ultimate goals of the telehealth network are to facilitate a bidirectional education exchange, and to improve access to primary and specialty care for underserved pediatric patients in Honduras.
Establishment of a telehealth network
In February 2015, investigators from MUSC established network connectivity at Cliníca de Especialidades y Neurocentro, an inner city neurology clinic in Tegucigalpa, and Clínica el Buen Pastor, a rural community health clinic in Santa María del Real, Olancho. The Honduran co-investigator identified both sites as clinics that are committed to caring for underserved populations. Investigators delivered a computer and monitor, a medical examination camera with lens and a Logitech BCC950 web camera (Logitech; http://www.logitech.com/en-au/product/conferencecam-bcc950) to both of the participating sites. VidyoDesktop v3.4.0 videoconferencing software (Vidyo, Inc.; https://www.vidyo.com/video-conference-systems/vidyodesktop) was installed on the computers at both Honduran sites and at MUSC. MUSC IT personnel trained at least two Honduran providers from each site to use the network equipment.
Educational conferences
Physicians and physicians in training at the Honduran sites were invited to remotely connect and present patients at morning and noon pediatric educational conferences over a period of 5 months. Educational conferences are held regularly in the Pediatrics Department at MUSC for medical students, residents, fellows and faculty, and typically consist of either an interactive case presentation followed by a brief lecture on a pertinent topic, or a didactic session focusing on a specialty topic within pediatrics such as pediatric neurology or rheumatology. All patient information was de-identified. Honduran providers were asked to complete satisfaction surveys immediately following the conferences, which assessed the ease of connectivity, connection quality and technical difficulties, as well as overall satisfaction with the conference. An IT specialist from MUSC was available during the conferences to assist sites with any technical problems. All educational conferences were conducted in English.
Physician consults
General pediatric and subspecialty consultations were conducted for the Honduran sites by a general pediatrician and a pediatric neurologist at MUSC using the telehealth equipment. These consults were primarily for general pediatric ailments, as well as chronic pediatric neurological conditions. No emergency consultations were performed. The Honduran sites were also instructed to hold teleconsults between each other in the absence of the MUSC providers (referred to as intracountry consults going forward). Physicians and physicians in training at the Honduran sites were asked to complete a survey immediately following each consult assessing the ease of connectivity, connection quality and technical difficulties, as well as satisfaction with the consultation. All physician consults were conducted in English, with the exception of the intracountry consults, which were conducted in Spanish.
Data collection and analysis
Satisfaction surveys for the educational activities and pediatric consults were adapted from existing MUSC telemedicine satisfaction surveys and translated into Spanish, and asked providers to assess connection quality and technical difficulties using a five-point Likert scale. A section for comments was also available. Respondents completed the surveys electronically through the RedCap study database. Descriptive analyses were performed.
Ethics approval
This study was reviewed and approved by the Institutional Review Board of MUSC and the National Autonomous University of Honduras (Pro00034887).
Educational conferences
Seven educational conferences were included in the study period. For each of these conferences, two to nine providers attended the session and completed the satisfaction surveys (Table 1). Overall satisfaction with the conferences was positive, with 100% of the respondents stating that they would utilize telemedicine again as an education exchange. Poor image quality, volume level, Internet connection problems and low voltage posed issues for some of the respondents (Table 2).
MUSC physician consults
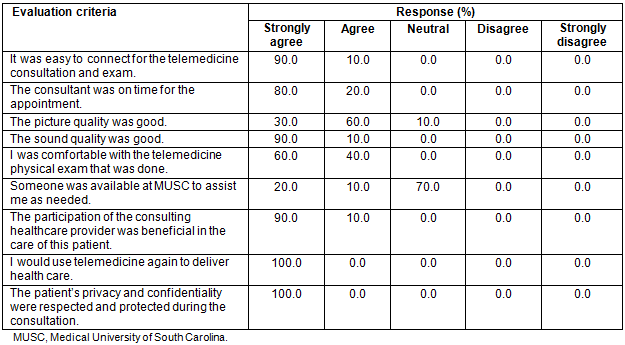
MUSC providers completed a total of eight consults, and eight Honduran providers completed satisfaction surveys. Responses were overwhelmingly positive, as 100% of respondents completely agreed that they would utilize telemedicine in the future. A few subjective complaints were made regarding the image quality (Table 2).
Intracountry consults
A total of three consults were conducted between the two Honduran sites, and three to six providers completed the satisfaction surveys after each consultation (Table 3). Overall responses were positive, with 100% of respondents reporting that they would utilize telemedicine in the future to improve patient health.
Table 1: Pooled provider responses from educational conference surveys (n=41)
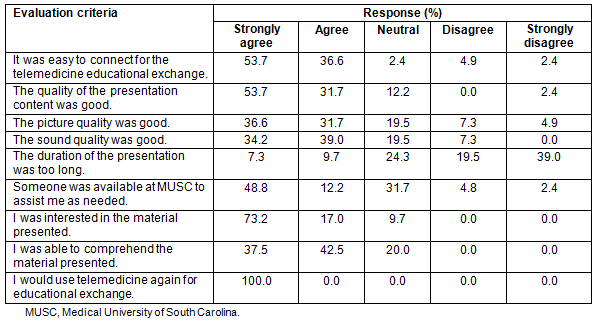
Table 2: Provider survey comments following educational activities and consults
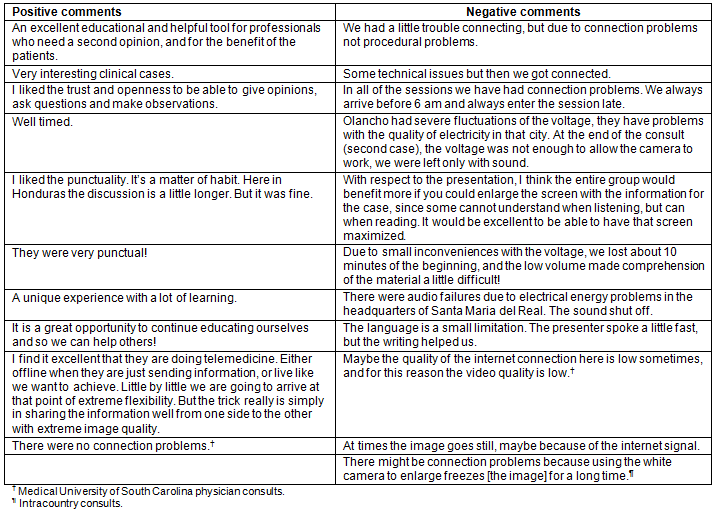
Table 3: Pooled provider responses from satisfaction surveys (intracountry consults; n=10)
Discussion
The Likert scale data from both the educational conferences and the telemedicine consults suggest that the use of telehealth is well received by providers working in underserved facilities in Honduras. Of particular significance were survey responses from consults that occurred between the two Honduran sites. These consultations demonstrated that internal networking and communication between local health facilities could be established in Honduras. Using telehealth to reach underserved practitioners for learning opportunities in the USA has been done successfully4,5. The advantage of extending these types of telehealth activities to other countries is the opportunity for two-way learning.
The data generated by this project provided valuable insight into establishing a telehealth network in Honduras. The primary challenges encountered were poor Internet connectivity and low bandwidth, which are likely to improve as technology progresses in Honduras. The positive responses from the Honduran providers were encouraging, since user satisfaction is essential to the success of any telehealth program. The most significant limitation to this study was the small number of facilities and providers that participated. While the results of this study may not be generalizable to the country as a whole, they provide ample qualitative support for future exploration of telehealth in Honduras. The long-term goal of this project is to expand telehealth capabilities to other underserved areas in Honduras by integrating this technology into existing infrastructure to support routine in-country collaboration for clinical care, learning and professional development.
Acknowledgements
The authors thank their clinical collaborators Dr Nestor Salavarría, Dr Gabriela Guifarro, and Dr Allan Oliva at Clínica el Buen Pastor, and Dr Glenda Oliva at Clínica de Especialidades y Neurocentro. This project was supported by the Medical University of South Carolina's Center for Global Health.
References
1. American Telemedicine Association. ATA telemedicine/telehealth terminology. Internet (2016). Available: http://thesource.americantelemed.org/resources/telemedicine-glossary (Accessed 22 May 2016).
2. Duncan C, Dorrian C, Crowley P, Coleman R, Patterson V. Safety and effectiveness of telemedicine for neurology outpatients. Scottish Medical Journal 2010; 55(1): 3-5. https://doi.org/10.1258/rsmsmj.55.1.3
3. Franzini L, Sail KR, Thomas EJ, Wueste L. Costs and cost-effectiveness of a telemedicine intensive care unit program in 6 intensive care units in a large health care system. Journal of Critical Care 2011; 26(3): 329e1-6.
4. Monteiro AM, Correa DG, Santos AA, Cavalcanti SA, Sakuno T, Filgueiras T, et al. Telemedicine and pediatric radiology: a new environment for training, learning, and interactive discussions. Telemedicine Journal and e-Health 2011; 17(10): 753-756. https://doi.org/10.1089/tmj.2011.0049
5. Gonzalez-Espada WJ, Hall-Barrow J, Hall RW, Burke BL, Smith CE. Achieving success connecting academic and practicing clinicians through telemedicine. Pediatrics 2009; 123(3): e476-e483. https://doi.org/10.1542/peds.2008-2193
6. Chanussot-Deprez C, Contreras-Ruiz J. Telemedicine in wound care: a review. Advances in Skin and Wound Care 2013; 26(2): 78-82. https://doi.org/10.1097/01.ASW.0000426717.59326.5f
7. Sekar P, Vilvanathan V. Telecardiology: effective means of delivering cardiac care to rural children. Asian Cardiovascular and Thoracic Annals 2007; 15(4): 320-323. https://doi.org/10.1177/021849230701500411
8. Lopez-Magallon AJ, Otero AV, Welchering N, Bermon A, Castillo V, Duran A, et al. Patient outcomes of an international telepediatric cardiac critical care program. Telemedicine Journal and E-health 2015; 21(8): 601-610.
9. Vassallo DJ, Hoque F, Roberts MF, Patterson V, Swinfen P, Swinfen R. An evaluation of the first year's experience with a low-cost telemedicine link in Bangladesh. Journal of Telemedicine and Telecare 2001; 7(3): 125-138. https://doi.org/10.1258/1357633011936273
10. Geissbuhler A, Ly O, Lovis C, L'Haire JF. Telemedicine in Western Africa: lessons learned from a pilot project in Mali, perspectives and recommendations. AMIA Annual Symposium Proceedings 2003: 249-53.
11. Pradeep PV, Mishra A, Mohanty BN, Mohapatra KC, Agarwal G, Mishra SK. Reinforcement of endocrine surgery training: impact of telemedicine technology in a developing country context. World Journal of Surgery 2007; 31(8): 1665-1671. https://doi.org/10.1007/s00268-007-9108-1
12. Agrawal S, Maurya AK, Shrivastava K, Kumar S, Pant MC, Mishra SK. Training the trainees in radiation oncology with telemedicine as a tool in a developing country: a two-year audit. International Journal of Telemedicine and Applications 2011; 2011: 230670.
13. Ho YL, Yu JY, Lin YH, Chen YH, Huang CC, Hsu TP, et al. Assessment of the cost-effectiveness and clinical outcomes of a fourth-generation synchronous telehealth program for the management of chronic cardiovascular disease. Journal of Medical Internet Research 2014; 16(6): e145. https://doi.org/10.2196/jmir.3346
14. Crow SJ, Mitchell JE, Crosby RD, Swanson SA, Wonderlich S, Lancanster K. The cost effectiveness of cognitive behavioral therapy for bulimia nervosa delivered via telemedicine versus face-to-face. Behavioral Research Therapy 2009; 47(6): 451-453. https://doi.org/10.1016/j.brat.2009.02.006
15. Glaser M, Winchell T, Plant P, Wilbright W, Kaiser M, Butler MK, et al. Provider satisfaction and patient outcomes associated with a statewide prison telemedicine program in Louisiana. Telemedicine Journal and e-Health.2010; 16(4): 472-479.
16. World Health Organization. Telemedicine opportunities and developments in member states: report on the second global survey on ehealth. Geneva: World Health Organization, 2010.
17. Vassallo DJ, Hoque F, Roberts MF, Patterson V, Swinfen P, Swinfen R. An evaluation of the first year's experience with a low-cost telemedicine link in Bangladesh. Journal of Telemedicine and Telecare 2001; 7(3): 125-138. https://doi.org/10.1258/1357633011936273
18. Pan America Health Organization, Regional Office for the World Health Organization. Health in the Americas: Honduras. (Internet) 2013. Available: http://new.paho.org/saludenlasamericas/index.php?option=com_content&view=article&id=43&Itemid=50&lang=en (Accessed 8 April 2013).
19. World Health Organization. Honduras: health profile. (Internet) 2015. Available: http://www.who.int/gho/countries/hnd.pdf (Accessed 5 January 2016).