Rural communities across Australia continue to experience significant challenges recruiting and retaining general practitioners (GPs)1-3. A number of policy responses have made gains; however, inadequate recruitment and retention of GPs remains problematic and impacts health outcomes among rural and remote populations1-3.
Attributes of a community and challenges within a health facility play key roles in the recruitment and retention of GPs4-8. Issues may include long working hours, poor employment opportunities for spouses, insufficient educational opportunities for children, or geographic and social isolation5,7,9. Prior workforce studies have investigated GP characteristics, employment satisfaction, psychosocial needs and challenges encountered by rural GPs5-7,10.
An alternative perspective was conceived to address GP recruitment and retention challenges experienced in rural Idaho in the USA. This led to the development of the Community Apgar Questionnaire (CAQ)4,8,11,12. Apgar testing is used to quantify the resources, capabilities and current functioning of newborns13; similarly, the CAQ is used to quantify resources and capabilities of a community to recruit and retain GPs11,12. It differentially diagnoses a community's relative strengths and challenges in recruiting and retaining GPs, while supporting health facilities to prioritise achievable goals to improve long-term retention strategies4,8,11,12.
The CAQ contains 50 factors that are scored as being advantages or challenges and then scored on how important the factor is to GP recruitment and retention. These factors are classified into five classes: geographic, economic, scope of practice, medical support and hospital and community support. In addition, three qualitative open-ended questions allow key factors to be validated, while identifying site-specific factors11,12.
Since its inception, the CAQ has been successfully used in the US states of Idaho, Wyoming, North Dakota, Wisconsin, Alaska, Maine, Utah, Montana, Indiana and Iowa4,8,11,12. However, the CAQ's value and efficacy have not been examined internationally.
The aim of the study was to pilot the CAQ across communities in the Hume region of rural Victoria, evaluate its usability and develop a greater understanding of the community factors that impact GP recruitment and retention.
The Hume region has more than 300 000 people across 12 local government areas and encompasses 27 health facilities that consist of three public and three private hospitals in major centres, 19 district health services (which include three private health services) and two bush nursing services14.
In the study, district health facilities and bush nursing services in the Hume region of Victoria were specifically targeted for this project, of which 14 (76%) participated in this study. The target population were chief executive officers (CEOs) and directors of clinical services (DCSs) who had responsibilities for recruitment and retention activities. Each CEO and DCS that provided informed consent underwent an individual face-to-face structured interview using the CAQ, which lasted 45-60 minutes.
Once collected, data were cleaned, checked, analysed using the Statistical Package for the Social Sciences v22.0 (IBM, http://www.ibm.com) and scored by assigning quantitative values to the four-point Likert scale of community advantages or challenges for each factor (major advantage = 2, minor advantage = 1, minor challenge = -1, major challenge = -2). The factors were then weighted according to perceived importance on a four-point Likert scale (very important = 4, important = 3, unimportant = 2, very unimportant = 1), as outlined in the following algorithm:
(community advantage/challenge score) x (community importance score) = CAQ score
This algorithm created a community asset and capability measure that ranges from -8 to 8 with a higher score indicating a more developed community asset and capability related to recruitment and retention of GPs. Scores were then added to provide a cumulative CAQ score.
Once all data were collected and calculated, site-specific data were fed back to CEOs and this provided opportunity to discuss the strengths of their health facility or how the identified challenges may or have been overcome.
Ethics approval
Ethics approval for the study was obtained by Albury Wodonga (HRECAW409/15/4), Northeast Health Wangaratta (HRECNHW160), and the Goulburn Valley Health (GVH09-15) human research ethics committees.
Among the 21 identified district health and bush nursing services, 14 (76%) sites chose to participate, with 14 CEOs and 14 DCSs as the final sample of 28 respondents. Each provided responses to the 50 factors within the CAQ and the three open-ended questions. The reliability of the CAQ was assessed using Cronbach's alpha coefficients, a standard measurement of reliability. The overall Cronbach's alpha was 0.814, which was above 0.7 and considered acceptable. Mean CAQ scores were then calculated for the 50 factors and five classes of the CAQ. The average scores for factors within and across each class were rank ordered and the top 10 CAQ scores and bottom 10 CAQ scores across all 50 factors were identified for the Hume region.
Advantages and challenges
Medical support was identified as the highest community advantage class across the Hume region, followed by hospital/community support and then economic class. The top 10 individual advantages were transfer arrangements, nursing workforce, perception of quality, hospital leadership, community need/GP support, ancillary staff (allied health, pathology and X-ray), GP workforce stability, part-time opportunities, inpatient care and income guarantee.
The top 10 challenges were spousal satisfaction, schools, shopping and other services, religious/cultural opportunities, call/practice coverage, social networking, electronic medical records, caesarean section, emergency room coverage and obstetrics.
Importance
Again, medical support was identified as the highest importance class among the communities followed by the geographic class, hospital/community support and the economic class. The top 10 important factors across all 50 factors were spousal satisfaction, call/practice coverage, hospital leadership, perception of quality, adequacy of schools, employment status, nursing workforce, internet access, GP workforce stability and physical plant and equipment.
Overall community Apgar scores
The community Apgar algorithm, derived from the community advantage/challenge score weighted by its relative importance, was calculated. The medical support class was identified as the highest community asset and capability followed by hospital/community support, the economic class, scope of practice and the geographic class. The top 10 CAQ factors were perception of quality, hospital leadership, nursing workforce, transfer arrangements, community need/GP support, GP workforce stability, part-time opportunities, inpatient care, ancillary staff workforce and specialist availability.
The bottom 10 CAQ factors were spousal satisfaction, schools, shopping and other services, religious/cultural opportunities, call/practice coverage, electronic medical records, social networking, caesarean section, emergency room coverage and obstetrics (Table 1).
The cumulative CAQ scores for each of the participating health facilities was derived by adding all CAQ scores of each of the 50 factors for both the CEOs and the DCSs. The cumulative CAQ scores range from 387 to 61. Higher scores indicate greater community assets and capabilities for a particular health facility as they relate to GP recruitment and retention (Table 2). The overall Apgar score distribution indicates that the tool was sensitive enough to differentiate between communities that were high and low performers in terms of physician recruitment, as shown in the USA15 (Fig1).
Table 1: Advantages/challenges, importance and overall community Apgar scores (n=28)
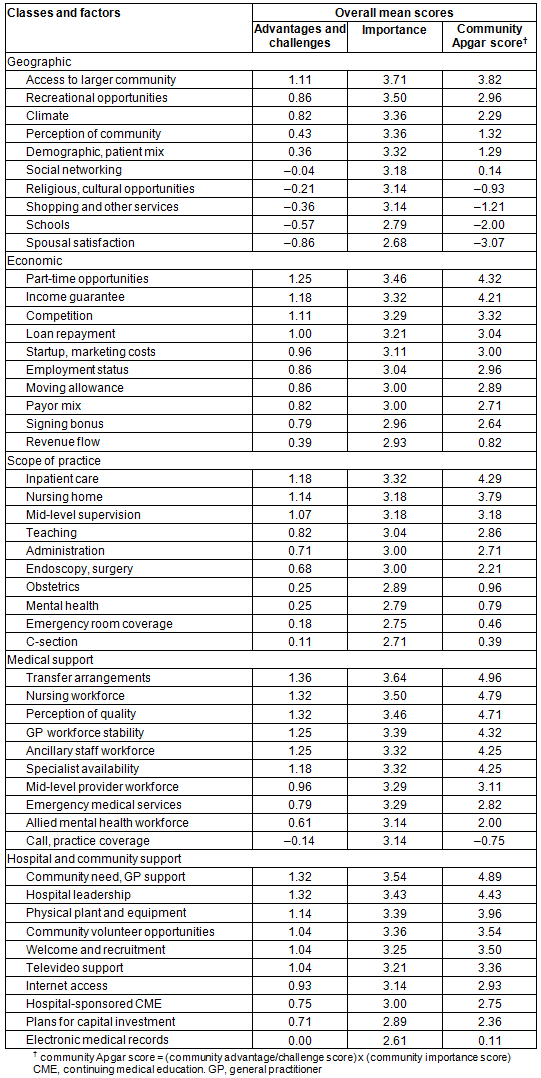
Table 2: Community Apgar scores by cumulative score (n=28)
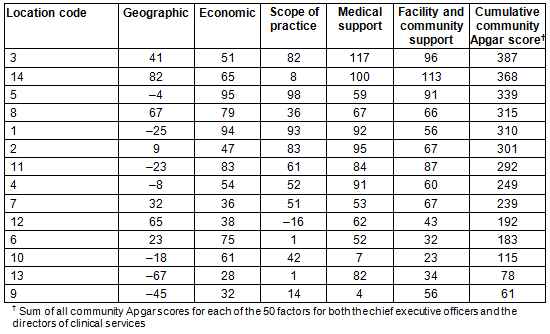
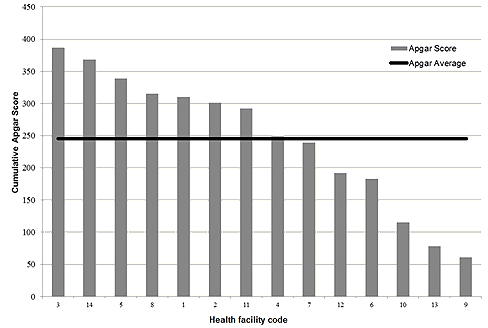
Figure 1: Cumulative mean community Apgar scores according to location.
Reliability and validity of chief executive officer and director of clinical services results
To ensure reliability and validity of the results, three additional CAQs were administered to general practices and then compared to scores obtained from CEOs and DCSs from the same communities. The three selected sites were sites 3, 4 and 9, as these were the top, bottom and middle scoring communities in the region. The CAQ was administered to either the principal GP or the practice manager in charge of practice operations and recruitment.
After CAQs were conducted with GP practices it was evident that individual advantages/challenges and importance scores among GP practices were relatively similar to scores from CEO and DCS; however, they were more likely to be consistent with CEO scores. Analysis was achieved by using intra-class correlation coefficient (ICC) to determine the inter-rater reliability of the CAQ scores between the CEOs, DCSs and GP practices at the three sites.
The analysis confirmed all respondents were reliably and consistently scoring factors in the same way. The reliability scores, produced under the two-way mixed effects model, demonstrated that all respondents from all three sites were consistently scoring the CAQ similar to one another (ICC = 0.683 (95% confidence interval (CI)=0.616-0.750), F(99,792)=20.423, p=0.000). This suggests the inter-rater reliability of the CAQ among each respondent, whether CEO, DCS or GP practice, has a moderate level of agreement between CAQ scores across the three sites. This finding was indicated to be similar if GP practice scores were excluded (ICC=0.701 (95%CI=0.631-0.767), F(99,495)=15.040, p=0.000).
Overall, including GP practices as part of the CAQ would provide similar scores to either CEOs or DCSs. However, including GPs and practice manages within future programs would also provide greater insight beyond the healthcare setting itself. They would present a richer contextual meaning regarding the advantages/challenges and relative importance of recruitment and retention of GPs within rural settings.
Additional barriers
The most noted barrier to recruitment and retention from the open-ended questions was work-life balance, while managing on-call responsibilities. The amount of on-call duty that was required of local GPs either made a service attractive or less attractive. In smaller towns, with only one or two smaller practices, local doctors found maintaining a good work-life balance challenging, whereas the larger towns had what some participants termed a 'critical mass' of doctors, allowing less on-call responsibility. On-call requirements varied between towns from 1 in 4 to 1 in 13 weekends each year. These issues were further confirmed by the three GP practices that were included in the study.
Access to greater procedural medicine, anaesthetics and surgery with a greater complexity of practice was the second greatest barrier, highlighted in the open-ended questions, to recruiting and retaining GPs. In many cases, services were unable to offer these opportunities, which they felt made the service less attractive or less competitive. By contrast, some health facilities did not provide obstetrics, caesarean section, or emergency room services. Both health facilities and GP practices felt this was an advantage as it meant less on-call duty and the better work-life balance that physicians were seeking.
Solutions to challenges
A number of recruitment and retention solutions were highlighted by the various health facilities and GP practices, particularly among those with high CAQ scores. One example is including the spouse as part of the recruitment process or supporting the spouse and family in other ways. Health facilities with lower CAQ scores aimed to build better relationships with GPs, related to contract negotiation and engaging the spouse more through workplace and social activities. For some health services, providing employment or working with local employment agencies was one achievable goal.
Those communities with good school bus services were those where GPs were more satisfied with school options for children. The challenge of schools within the Hume region is that there are a small number of GP-preferred private schools in larger towns. In many cases school bus services were provided through most communities; however, school zoning precluded some children from attending certain schools. Those health facilities in communities with poorer bus services or school zoning issues indicated they would engage schools and local government to look at viable options.
Among some health facilities, good relationships had been developed with the larger tertiary hospitals in the region, which allowed for greater complexity of practice for GPs, while increasing the use of televideo for emergency coverage and reducing GP on-call obligation. In other facilities, rural and isolated practice endorsed registered nurses were trained to alleviate GP on-call duties. Some health facilities had upskilled all staff with regular emergency simulation training and X-ray operator courses. Many health services that had challenges with on-call duties were planning or had planned to address this issue either through additional training of staff or increasing the use of tele-video support, while further developing partnerships with ambulance services and larger hospitals.
Overall there was an emphasis on 'finding the right fit' for GP recruitment to rural communities. Factors most commonly discussed included providing greater opportunities for medical students and those requiring further training; directly employing medical staff rather than subcontracting private providers, which was felt to be what younger doctors wanted; providing greater professional and social support for GPs and whole families; and providing attractive leasing agreements for practice and/or personal accommodation.
Discussion
Community Apgar factors that were considered to have the most impact on GP recruitment and retention were perception of quality, hospital leadership, nursing workforce, transfer arrangements and community need/GP support. In the Hume region, the reputation of a health facility providing quality of medical care was suggested to be strongly supported by the community and vital to attract and retain GPs11,16,17. Many participants indicated that strong and open communication between GPs and leadership was paramount and that open communication ensured GPs working in private practices felt valued and empowered4,8,12,16.
The adequacy of nursing workforce for both quantity and quality was indicated to be as essential as the relationship between the GPs and nurses18,19. A GP-nurse relationship that is built on trust, support and reciprocity has been shown to 'protect' GPs from burnout and leaving a community19. Transfer arrangements may be a vital factor due to limited subspecialist availability among many rural health facilities20. In these situations, it is advantageous to ensure GP stressors are reduced by having procedures in place when critically ill patients require greater care. Community need/GP support is also central within the Hume region, as community support and appreciation of GPs has an impact on retention, particularly if services were to be reduced7.
The lowest individual factor CAQ scores were spousal satisfaction, and schools, shopping and other services. Each of these factors may be related to the perceived isolation or remoteness of the various communities with the Hume region5,7. For example, spousal satisfaction may be related to poor employment opportunities, while schools may be related to access to particular types of school. Possible solutions were to ensure recruitment of the GP also considered what social, employment and school opportunities are available for spouses and children5,7.
Limitations
Differences between Australian and US-based community Apgar research relate to the structure of health facilities and GP recruitment. For example, in Australia contract agreements are between health facilities and private general practice providers to service the facility. Relatively few health services directly recruited GPs. As such, health facilities did not always have direct recruitment and retention responsibilities. Despite this, researchers actively investigated and continue to investigate whether the results reflect the views and perceptions of GPs across many practices across the Hume region.
Hume was the first site to implement the CAQ internationally, and its reliability and validity as a tool was indicated to be moderate to high. The CAQ provided an analysis of the comparative strengths and challenges that each community encountered, while establishing the uniqueness of each community. The process identified what each community had to offer physicians, and who might be the best match for their community. Participation in the program was reported to be useful as it helped health services ascertain how they were performing and highlighted areas for improvement in terms of recruitment and retention.
The implementation of the CAQ has offered health services and GP practices the opportunity to develop strategic plans that are specifically tailored to their service and community in terms of who to recruit and what key strategies may assist retention. It has also provided an opportunity to confidentially share best practices and obstacle elimination from services that were performing well. Lastly, it has encouraged greater networking opportunities between services to address issues of recruitment and retention. The CAQ has commenced identifying trends and overarching themes, and it directly impacts rural communities. Its use in Australia has begun to develop an evidence-based platform for the advocacy of key issues at community, state and national levels.
Acknowledgements
This research has been supported by the Australian Government Department of Health and Ageing through the Rural Health Multidisciplinary Training Programme. Original development and ongoing funding has been provided by Idaho Bureau of Rural Health and Primary Care, Family Medicine Residency of Idaho, and Center for Health Policy, Boise State University. The authors also acknowledge Mary Sheridan, Bureau Chief, Idaho Bureau of Rural Health and Primary Care and the research assistance of Lisa MacKenzie.
References
1. National Competition Council. National Competition Policy Melbourne. (Internet) 2012. Available: http://ncp.ncc.gov.au/pages/about (Accessed 26 March 2012).
2. National Competition Policy Review Committee. National competition policy. Canberra: Australian Government, 1993.
3. Humphreys J, Jones J, Jones M, Hugo G, Bamford E, Taylor D. A critical review of rural medical workforce retention in Australia. Australian Health Review 2001; 4(4): 91-102. https://doi.org/10.1071/AH010091a
4. Baker E, Schmitz D, Epperly T, Nukui A, Miller CM. Rural Idaho family physicians' scope of practice. The Journal of Rural Health 2010; 26(1): 85-89. https://doi.org/10.1111/j.1748-0361.2009.00269.x
5. Terry DR, Lê Q. International medical graduates: a cohort study of key informant perspectives. Universal Journal of Public Health 2013; 1(4): 151-165.
6. Kamalakanthan A, Jackson S. A qualitative analysis of the retention and recruitment of rural general practitioners in Australia. Brisbane: University of Queensland, School of Economics, 2008.
7. McGrail M. 'Rurality' and community amenity: how they relate to rural primary care supply and workforce retention. Canberra: Australian Primary Health Care Research Institute, 2015.
8. Schmitz D, Baker E, MacKenzie L, Kinney L, Epperly T. Assessing Idaho rural family physician scope of practice over time. The Journal of Rural Health 2015; 31(3): 292-299. https://doi.org/10.1111/jrh.12107
9. McGrail MR, Humphreys JS, Joyce CM, Scott A. International medical graduates mandated to practise in rural Australia are highly unsatisfied: results from a national survey of doctors. Health Policy 2012; 108(2-3): 133-139. https://doi.org/10.1016/j.healthpol.2012.10.003
10. Reed AJ, Schmitz D, Baker E, Nukui A, Epperly T. Association of 'grit' and satisfaction in rural and nonrural doctors. The Journal of the American Board of Family Medicine 2012; 5(6): 832-839. https://doi.org/10.3122/jabfm.2012.06.110044
11. Schmitz D, Baker E, Nukui A, Epperly T, Schmitz D. Idaho rural family physician workforce study: the community Apgar questionnaire. Rural and Remote Health (Internet) 2011; 11: 1769. Available: www.rrh.org.au (Accessed 13 November 2014).
12. Baker E, Schmitz D, Wasden S, MacKenzie L, Epperly T. Assessing Community Health Center (CHC) assets and capabilities for recruiting physicians: the CHC Community Apgar Questionnaire. Rural and Remote Health 2012; 12: 2179. Available: www.rrh.org.au (Accessed 13 November 2014).
13. Apgar V. The newborn (Apgar) scoring system. Pediatric Clinics of North America 1966; 13(3): 645-650. https://doi.org/10.1016/S0031-3955(16)31874-0
14. Regional Development Victoria. Victoria's Hume Region Melbourne. (Internet) 2016. Available: http://www.rdv.vic.gov.au/victorian-regions/hume (Accessed 28 January 2016).
15. Baker E, Schmitz D, MacKenzie L, Morris B, Epperly T. Rural community variation in physician recruitment readiness. Journal of Health Sciences 2014; 2(8): 393-401.
16. Szafran O, Crutcher RA, Chaytors RG. Location of family medicine graduates' practices. What factors influence Albertans' choices? Canadian Family Physician 2001; 47(11): 2279-2285.
17. Backer EL, McIlvain HE, Paulman PM, Ramaekers RC. The characteristics of successful family physicians in rural Nebraska: a qualitative study of physician interviews. The Journal of Rural Health 2006; 22(2): 189-191. https://doi.org/10.1111/j.1748-0361.2006.00030.x
18. Tang CJ, Chan SW, Zhou WT, Liaw SY. Collaboration between hospital physicians and nurses: an integrated literature review. International Nursing Review 2013; 60(3): 291-302. https://doi.org/10.1111/inr.12034
19. Blue I, Fitzgerald M. Interprofessional relations: case studies of working relationships between registered nurses and general practitioners in rural Australia. Journal of Clinical Nursing 2002; 11(3): 314-321. https://doi.org/10.1046/j.1365-2702.2002.00591.x
20. Wong K, Levy RD. Interhospital transfers of patients with surgical emergencies: areas for improvement. Australian Journal of Rural Health 2005; 13(5): 290-294. https://doi.org/10.1111/j.1440-1584.2005.00719.x



