Context
A recent Australian National Rural Health Alliance discussion paper outlined the role of advanced rural and remote nurses and the benefits of an expanded practice scope for rural and remote communities1. Studies have concluded advanced nursing roles deliver high quality effective health care; however, it is recognised that measuring the impacts on health outcomes is difficult2,3. What remains to be debated is how an advanced nursing role contributes to quality care.
Monash University School of Rural Health recently completed two studies exploring the role and practice of remote area nurses (RANs) working autonomously in bush nursing centres (BNC) in East Gippsland, Victoria4,5. Consistent with measures for advanced nursing competencies in Australia6, the studies confirmed the remote nursing role as advanced and expanded, and the care effective and of high quality. However, the studies also revealed the contribution of the nursing role to quality care involved more than demonstrating clinical expertise. The context of practice emerged as an important indicator of quality care4,5. The influence of economic structures and community characteristics on remote nursing practice and service delivery is overlooked.
The studies identified four core drivers creating the context: the system, the organisation, the community and the individual. These drivers have shaped current remote nursing practice, and the advanced role has established a standard of quality care to rival large health agencies. This article presents an alternative approach to evaluate the contribution of an advanced RAN role that involves a 360 degree view of the practice environment. The four drivers form the model's framework; interactions between the drivers determine the context and capture the RANs' efforts to sustain high service standards.
Issue
What is 'quality care'?
The quest to define 'quality care' has occupied theorists and academics for many years. Debates concede the concept of quality is multidimensional, and time and context specific7,8. In Australia there is need to measure performance to demonstrate service effectiveness and the provision of quality care7. However, there are limitations to and gaps in performance measurement in Australia, especially outside the acute hospital system, related to assessment model design and performance indicator development7. The validity of measuring health service performance is reliant on the appropriateness and reliability of the indicators7.
Attree8 suggests the following elements are central to a model of quality care: observable attributes; structure, process and outcomes criteria; professional and managerial perspectives; context/environment; and time/era. The latter two elements indicate quality is context and time specific, influenced by various environmental factors. Attree8 supports the view that individual and societal expectations are influenced by the context of the service; however, adds that the prevailing opinion of the day will influence the organisational culture of the healthcare system and determine quality.
Sidani et al.9 apply a theory-driven approach to evaluating quality, and identify five factors influencing outcomes: the person receiving care; the professional providing care; the context; the type of care provided; and the timing of outcomes expected from the care provided. The authors conclude that realistic evaluation of quality care requires attending to the factors that affect outcomes. Current Australian health service and professional competency standards fail to combine external structural and organisational factors and the social and economic situation of a given remote community. Professional nursing attributes such as social leadership, community advocacy and capacity building are also ineffectively captured. In the remote context, if quality care is to be assessed, a comprehensive understanding of the relationship between contextual variables, service provision and advanced nursing roles is required.
The role of context
Until recently rural health experts have circumvented the significance of context; however, the importance of location is included as the environment that constructs reality10. There is a growing body of literature exploring the role of context and its relationship to health. Curtis and Jones11 consider an individual's health experience to be partly dependent on the physical and social environment. Thurston and Meadows12 discuss the role of place and influence of the rural context on health. Ryan-Nicholls13 suggest health strategies have centred on the symptoms, rather than the causes of rural health and sustainability problems, indicating health strategy models need to reflect the rural context. Australian rural researchers exploring mental health and wellbeing in rural Australia believe 'place' influences health variables and health outcomes, with the risk of illness connected to the community and environmental context in which the individual lives10,14. The 'vulnerable populations' conceptual model15 encapsulates the experience of context and focuses on the interrelationships between available resources, relative risk and health status15.
It is this inclusive view of context that frames RAN practice in Australia and determines the delivery of quality care. Consequently measures of service performance and the delivery of quality health care should be placed within a contextual framework.
Australian remote area nurses: In Australia, RANs generally work and live in small isolated communities. The nurses provide the first point of contact for a range of primary-care functions normally provided by medical practitioners and allied health professionals in urban and large regional centres1. Remote area nurses act as sole providers of primary and urgent health care, and frequently extend their skills due to community demand and a lack of any other form of health professional support. In remote areas of Australia, nurse-led health services provide care across the lifespan catering for acute and chronic illnesses, and population-based preventative programs. The role also requires health service management and demands a high level of knowledge and skill1. In addition, fundamental activities to identify health needs, coordinate care and evaluate services include collaboration with health colleagues and partnership development. The nurses also facilitate communication among the community, government and non-government organisations. Critical strategies to promote positive health outcomes include advocacy and empowerment1. To effect quality care and health outcomes it is essential for the RAN to collaborate within and among health professionals, services and other sectors that impact on health1.
Victorian remote area nurses: Until 2005 in the Australian state of Victoria, RANs were historically called 'bush nurses', and the nurse-led clinics referred to as 'bush nursing centres'. The nurses are now classified as RANs; however, the clinics remain known as bush nursing centres. In the East Gippsland region of Victoria, there are five BNC operating as single nurse-led clinics.
The East Gippsland region is dominated by forest and mountain ranges with numerous small communities scattered across the area. The communities range in size from under 200 people to a maximum of 500 people, and are serviced by a limited network of sealed, winding roads. The East Gippsland RAN model is context specific and operates in an environment without a local medical practitioner, hospital or pharmacist. Geographically isolated from any other health services and reliant on telephone support, five single nurse-led clinics provide a range of primary health, acute, chronic and emergency care, and population-based preventative programs.
Recent studies by Monash University School of Rural Health, Victoria, explored the role and practice of RANs working autonomously in the East Gippsland BNC. The studies confirmed the role as advanced and expanded, consistent with definitions of RAN practice in other isolated areas of Australia1. The care provided was evaluated as effective and of high quality; however, the studies also revealed that the contribution of the nursing role to quality care involved more than demonstrating clinical expertise. The context of practice emerged as an important indicator of quality care4,5. The findings from these studies form the basis of this article and the development of a quality evaluation model, citing the East Gippsland RAN as an example.
Lessons learned
The core drivers
The core drivers - the system, the organisation, the community and the individual - are critical elements to understanding the professional role and evaluating the contribution of RANs to quality health care. The 'core drivers' concept has emerged from integration of the Monash studies4,5 with the contribution of Sidani et al.9, who identify five factors influencing outcomes, and the 'clinical value compass' quality improvement model developed by Nelson et al.16. Each core driver is important and provides us with areas of significance known to influence dimensions of quality16. When core driver factors are considered in addition to the currently used quality measures of financial and usage data, the model provides a more reflective view of the individual situation.
The following is a brief outline of key factors within each driver that have shaped the current context.
The system: Factors considered in 'the system' included:
- the political party in power, their policies, programs and preferences
- legislation related to health-service delivery, practice and evaluation
- credentialling/registration of health service practitioners and providers
- workforce issues
- regional governance and health service priorities.
The organisation: Factors considered in 'the organisation' include:
- strategic plan
- health services alliances: local, regional and metropolitan
- health-service provision model/s such as: main organization, additional campuses, community health centres or clinics
- organizational policies and procedures.
The community: Factors considered in 'the community' include:
- service access
- community cohesiveness and connectedness
- socio-economic status
- transport and environment.
The individual (either client or significant other): Factors considered in 'the individual' include:
- experience with illness/ill people
- personal beliefs, preferences and expectations
- ability to be a 'partner' in care decisions
- availability of support network.
Healthcare professional (centre diamond): Factors considered in relation to the 'healthcare professional' include:
- experience
- knowledge, attitude and skills
- understanding of client/community
- qualifications
- authorisation, designation or registration.
The interrelatedness of the four core drivers also demonstrates a particular focus. The system and organisation have a very strong task focus due to their need to meet reporting deadlines, target numbers for service provision and budget targets. The community and the individual conversely focus on relationships and the need to work/pull together to support, sustain and maintain their health services, health-service providers or community members needing support. The health service provider, in the centre of the model, is the link between all four core drivers and has a direct influence on the quality of care outcomes for the client, community, organisation or the system. Quality of care is the outcome of the interactions and interrelationships of all components in the 'core driver' model. As with any system, a change in one factor has the potential to create change in another.
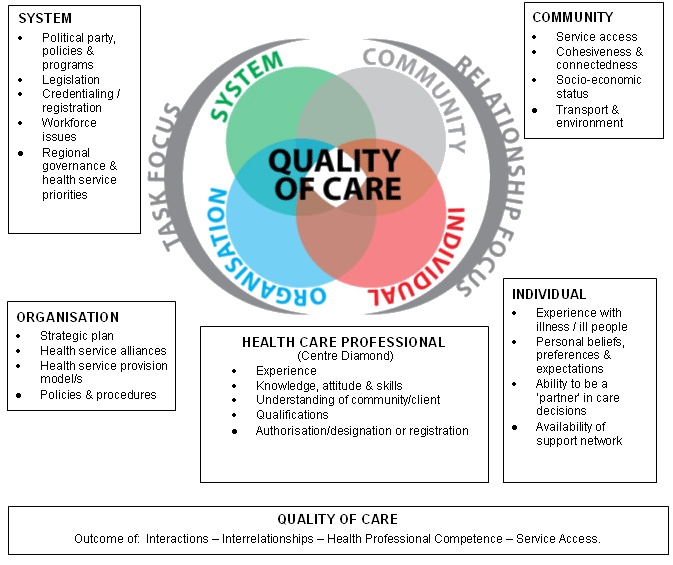
Figure 1: Integrated contextual model - four drivers of quality health care.
The proposed model represents the core attributes inherent in the concept of 'quality care' in a remote context. The interconnecting circles allow the attributes to be considered separately in context, time and place and in relation to each other. The attributes influence the process of care and achievement of outcomes. The model offered includes these factors and shows the relationship between elements. The model (Fig1) is transferable to other remote nursing contexts; however, the influence of the core drivers will vary according to the context.
How remote area nurses contribute to the quality of care: a remote Australian example
Using the 'core driver' model this next section will outline how we applied the model to explore the quality of care in a small isolated community serviced by RANs.
To effectively measure the quality and role contribution of RANs to the health of rural communities, and in an attempt to crystallise the role of context as it contributes quality rural health care, we undertook a 360 degree view of the RANs' practice context using the core drivers model.
The system: The previous Victorian Government introduced health system reform and massive funding cuts, affecting staff retention and backfill, and service delivery. In remote health services, access to relieving staff and allied health professionals became increasingly difficult, and increased financial competition made it harder for small health agencies to attract funding4,17. Isolated communities are difficult to serve due to small population numbers and are able to sustain only basic services13. The size of health services impacts on remote area nursing, influenced by a lack of on-site medical and allied health professionals18. In East Gippsland, limited resources and cuts to services resulted in the RANs carrying out non-nursing activities within their practice, and undertaking the roles of multiple health disciplines5. In essence the RANs have had to 'fill in the gaps' due to the unavailability of other cost-effective services18 p.26. This has meant developing strong networks with health professionals and agencies across the region to ensure remote communities have access to multiple health resources5. Maintaining these relationships is vital to protecting the viability and sustainability of nursing services.
The current health services provided by RANs are not adequately funded because the client population does not match the allocated funding model17. Classified and funded as Home and Community Care (HACC) agencies, the majority of service users do not fit the classification (people aged over 65 years or with a disability). Consequently many of the services provided fall outside of the scope of HACC programs and are ineligible for growth funding17. One reason for mismatched funding is an historical budgeting process that does not reflect actual need19. Wakerman suggested adapting resource benchmarks to local conditions, factoring level of need and costs associated with providing remote services19. Accessing additional money is necessary for some health services to be sustained. Minimal financial assistance is provided from other sources, including an annual subscription system and donations, although these extra community generated resources do not adequately cover the cost of these services4. Access to some local services was reviewed due to financial constraints and lack of available health professionals, including after-hours nursing assistance, visiting maternal and child health nurses, physiotherapists and occupational therapists5. Remote are nurses are now involved in grant applications and managing multilevel funding arrangements. Increasingly complex funding arrangements are considered an impediment to the implementation of sustainable and equitable health-service models20. Current financing arrangements limit the ability of remote health services to effectively respond to local needs20. Despite arguments of financial inequity, the studies by Monash University determined the various services provided by the East Gippsland RANs met the needs of the local community4,5. Recognising and supporting health-service costs particular to remote areas remains an issue for government funding policies21.
The organisation: In 1999 the BNC auspicing body the Victorian Bush Nursing Association amalgamated with Aged Care Victoria to form the Victorian Aged Health and Extended Care Association which has since been renamed Aged and Community Care Victoria (ACCV). This merger dissolved the structures and processes for addressing RAN issues. A senior nursing position that provided clinical support and governance became redundant, impeding access to appropriate professional development and peer-support systems4. With the loss of a formal clinical supervisor position, the RANs provided each other with informal support. However this strategy failed to meet professional development and ongoing clinical training needs.
In 2003 the removal of the 'designation status', permitting Victorian RANs to use specific emergency guidelines in the absence of a medical officer, left them without legal practice parameters for managing emergencies without medical support. This, however, did not deter the nurses from continuing to provide emergency and trauma care. Following a review of 'designation' status and a training needs analysis, a new partnership with Rural Ambulance Victoria (RAV) was formed, and appropriate RAN emergency training was developed and implemented in 2005. This new program provides 'accreditation' for RANs who achieve the required competencies, and authorisation to use specific emergency clinical guidelines when a medical officer cannot be contacted22. This initiative is an excellent example of innovative collaborative training and practice models designed to meet the needs of the practitioners and remote communities21. This successful collaboration is due to proactive action by the RANs and the culture of RAV to share knowledge and skills and develop roles that will provide better patient outcomes and more efficient and sustainable services.
The East Gippsland BNC are non-profit organisations governed by a local voluntary committee of management. Voluntary committees must comply with expanded government requirements ensuring accountability and transparency (J Lawrence, pers. comm., 2004)23. The BNC committees of management have expressed concern over the level of expertise required to fulfil governance responsibilities17; mainly the need to undertake formal governance training resulting in difficulties attracting the 12 volunteers with appropriate knowledge, skills and dedication required to manage these public facilities. Contextual barriers affecting volunteering include government policy and legislation, funding limitations and service priorities24, and community change has reduced the number of people willing to volunteer25. A declining and ageing population has impacted on the recruitment of committee of management volunteers and the availability of other community resources. The RANs have assumed some responsibilities for accountability and administration requirements within their role, and actively participate in governance training programs to contribute to the sustainability of delivering responsible quality remote health services. The creation of a paid administrative role has alleviated the nurses and committees of management of the responsibility of daily administrative functions. Unfortunately the hours and funding bases for the position are not consistent across the BNC despite similar management situations. This has placed pressure on some committees of management to secure annual funding to ensure the administrative position can be sustained. Hegney et al.18 point out that nurses working in small health services spend more time on management issues than in larger organisations.
Through the support of the RANs, committees of management, VACC and Department of Human Services Victoria (DHSV), the East Gippsland Bush Nursing Network was formed. There is a complementary group in western Victoria to support the BNC in that area of the state, which are larger and not single nurse-led clinics. A recent review of Victorian BNC highlighted and emphasised the role of VACC in supporting the BNC and management committees17. Improved collaboration between DHSV, VACC and the BNC have resulted in the development of strategic plans, enhanced linkages with other health services, exploring new service and funding approaches, establishing funded administrative support and the development of common financial reporting requirements17. The BNC are now included in the Victorian Government's framework for human service delivery for rural and remote regions21.
The community and the individual: Since 1996, the five isolated East Gippsland BNC communities have experienced negative population shifts resulting from social, industrial and environmental influences17. Environmentally the area has recently experienced drought, flood and bushfire. Socially and economically these remote communities experience above average levels of disadvantage with restricted accessibility to goods, services and opportunities for social interaction26. Services within the communities have gradually been withdrawn and businesses have closed. The unemployment rate in all five communities is above the rural Victorian and Victorian averages17. The prevalence of mental health issues across East Gippsland is rising26; however, the rise in mental health issues has not been matched by primary mental health services across the region. The population of these remote communities is ageing, with increasingly complex health needs. Individuals are now expected to be more involved in their health care and need to be more informed of psychological and physical health risks, and chronic disease self-management. The focus has moved from sharing disease knowledge and treatments to equipping patients with the skills and confidence to manage their condition27. Appropriate local management of chronic disease necessitates effective case coordination across the care continuum, and linkages with complementary community resources27.
Attending to the needs of the total community includes aiming for a quality of life for all who live there. This includes addressing the health and social problems encountered in daily living. Significant industrial and environmental challenges have impacted on the socio-economic situation and mental wellbeing of East Gippsland's remote communities26. Limited educational, employment and recreational opportunities, alongside economic and infrastructure decline, have been identified as contributing factors linked to depression and suicide in young rural Australians28. The influence of these events on the health of individuals and communities is difficult to quantify; however, the link between economic hardship and increasing mental health issues cannot be dismissed. This is well supported by social capital and social justice commentators who argue that health is partly dependent on the level of economic inequality29-33.
As a cornerstone of primary and public health, the concepts of social and economic justice appear to strongly inform remote nursing practice34. The RANs consider health as part of the total community, and participate in advocacy and change, while building on existing strengths of their communities. Remote nurses frequently advocate for individuals and communities on issues of concern, consistent with Averill's findings34. Predominantly, RAN practice is patient-centred; however, the focus on community activities is less easily identifiable. Strengthening social capital through voluntary participation and leading by example are unaccounted attributes.
The remote area nurse
Advanced knowledge and skills: Political movements and changing needs of individuals and communities have influenced the development of new roles and responsibilities35. In practice, new demands and reduced resources call for a higher level of clinical autonomy2. Central to an advanced nursing role is the continued development of service and care standards, with an holistic rather than technical focus35. The studies demonstrated the RANs provide an advanced level of clinical care and implement practice changes according to client need and service demands4. This necessitates awareness of local health and social demographics in order to provide appropriate primary health services matched to broader community needs. The assimilation of local knowledge and resident experiences into service planning is essential to strengthen health outcomes34. Forged partnerships, for example with RAV, have resulted in a contextually relevant professional training program. Partnership developments and targeted education are integral to maintaining the delivery of quality emergency and advanced clinical care for the remote communities.
Expanding practice scope: Restructuring of local government public health programs and reduced access to health professionals have led the RANs to 'pick up' some programs affected by resource constraints, for example immunisation programs. Other specific services provided to their local communities include womens' health, first-aid training, trauma management and palliative care4,5. Cognizant that effective and safe practice is founded not only on clinical competence, but also on education35, the RANs have undertaken additional education to support role expansion, and the legal and professional issues surrounding these changes5. Mental health has become a significant part of the nurses' scope of practice. Counselling, support, mental health first-aid training programs, mental health assessments and referrals are some of the new knowledge and skills developed.
Care coordination: Nurses practising at an advanced level have demonstrated excellent care outcomes attributable to their roles as case managers36. As the only health service providers, the RANs administer and coordinate most of the health care. The remote residents are provided with ready access to skills and expertise to support and assist care management. The nurses also have the advantage of patient familiarity and local social and health agency networks to anticipate care needs. Effective collaboration with allied health colleagues maximises care planning and resources for residents with long-term needs34. In this respect, the RANs contribute to high quality remote health care by providing regular assessments, treatment support, professional collaboration and follow up along the care continuum5.
Collaboration and partnerships: Long before government policy stipulated funded health agencies engage in collaborative care activities, the RANs actively sought outside professional assistance37. Recognising a single nurse-led primary health service is unable to meet the total needs of a community, the nurses have developed strong linkages with medical and allied health professionals, and acute health and community services. Although the nature of isolated practice requires autonomous decision-making, the nurses frequently communicate with health colleagues4,5. The RANs collaborate with health professionals, social services and government departments to maximise opportunities for equitable health care for remote individuals and communities5. The mix of advanced skills, expanded roles and collaborative activities contributes to health enhancement by improving the use of and access to the local health services4.
Preventative health: A primary health care approach has reformed areas of the Australian healthcare system, redirecting care approaches back to the community21. Access to medical and health information have added to greater public expectations of medical care and health promotion36 p.65. Alongside an increase in community responsibility for health care there is an expectation of health professionals to integrate health promotion into practice21. The RANs have incorporated preventative health strategies into their practice based on national trends and local needs5. Farm related injuries and specific injury areas including suicide and self-harm remain high in rural areas38. Implementing effective local injury prevention strategies, like other population-based initiatives, is restricted by geography, local infrastructure, a shortage of rural health services, and appropriate education and training to manage specific injury areas. In their daily practice the RANs act as role models for the community, and work with community groups to provide health promotion activities5. The demand for RANs to manoeuvre their practice between individual, primary and public approaches is due in part to the size of the health service, community needs, limited resources and a role that includes an active public interface5. This advocacy role extends from the individual to the health and social needs of the total community.
The contribution of RANs to quality remote health care is multifaceted with many role attributes outside formal organisational and nursing quality measures. As a group RANs, committees of management, communities and the auspicing body were successful in achieving accreditation through the Quality Improvement and Community Services accreditation39. This achievement demonstrates that the services, facilities and staff maintain a standard that equals that of larger health institutions and community agencies.
Conclusion
Providing quality care is challenging in a remote practice environment dominated by few resources, professional isolation and the culture of the individual community. As this article has attempted to illustrate, demonstrating quality care in the remote context requires more than measuring clinical and service performance indicators.
Political ideologies and escalating health costs have led to changes in health care delivery. Funding cuts, the application of health outcome indicators, and increased community-based health care are also to blame. Primary healthcare and chronic disease-management models have highlighted the responsibility of the health consumer and grounded the role of remote primary-care providers. Changes in government policy and approaches to health care have directly increased the responsibilities of sole RANs. Remote area nurses are now expected to manage and coordinate the health needs of the chronically ill, provide advanced clinical care for acute and urgent presentations, and conduct population-based health preventative programs. These activities occur alongside a growing management role.
Delivering efficient healthcare and demonstrating service effectiveness requires adequate resources. However, current funding arrangements do not adequately support the broad range of activities as demonstrated in our remote nursing example. In an era of measuring performance a 'whole of system' review is needed. The core drivers - the system, the organisation, the community and the individual - form a contextual matrix. It is the interaction of the core drivers that shape practice and benchmark the quality of the health care delivered. Context, therefore, forms the overarching framework for evaluating performance, and highlights the contribution of RANs to quality care.
References
1. National Rural Health Alliance. Advanced nursing practice in rural and remote areas. Canberra, ACT: NRHA, 2005; 25.
2. Daly W, Carnwell R. Nursing roles and levels of practice: a framework for differentiating between elementary, specialist and advancing nursing practice. Journal of Clinical Nursing 2003; 12: 158-167.
3. Furlong E, Smith R. Advanced nursing practice: policy, education and role development. Journal of Clinical Nursing 2005; 14: 1059-1066.
4. Burley M, Duffy E, McGrail M, Siegloff L. VRNP2: Victorian Rural Nurse Project - part 2; advanced nursing practice: bush nursing perspective. Traralgon, VIC: Monash University School of Rural Health, 2002; 104.
5. Greene P, Duffy E. Victorian Nurse Practitioner Project - phase 2: nurse practitioner models of practice: quality care in the bush. Traralgon, VIC: Monash University School of Rural Health, 2003.
6. Royal College of Nursing Australia. Position statement: advanced practice nursing. Canberra, ACT: RCNA, 2005.
7. National Health Performance Committee. Measuring performance in the Australian health system: toward a national performance assessment framework - discussion paper. Canberra, ACT: Australian Government.
8. Attree M. Towards a conceptual model of 'quality care'. International Journal of Nursing Studies 1996; 33: 13-28.
9. Sidani S, Doran DM, Mitchell PH. A theory-driven approach to evaluating quality of nursing care. Journal of Nursing Scholarship 2004; (First quarter): 60-65.
10. Judd F, Murray G, Fraser C, Humphreys J, Hodgins G, Jackson H. The mental health of rural Australians: developing a framework for strategic research. Australian Journal of Rural Health 2002; 10: 296-301.
11. Curtis S, Jones I. Is there a place for geography in the analysis of health inequity? In: M Bartley, D Blane, G Smith (Eds). The Sociology of Health Inequities. Oxford: Blackwell, 1998; 87-88.
12. Thurston W, Meadows L. Rurality and health: perspectives of mid-life women. Rural and Remote Health 3: 219. (Online) 2003. Available: www.rrh.org.au (Accessed 13 July 2007).
13. Ryan-Nicholls K. Health and sustainability of rural communities. Rural and Remote Health 4: 242. (Online) 2004. Available: www.rrh.org.au (Accessed 13 July 2007).
14. Fraser C, Judd F, Jackson H, Murray G, Humphreys J, Hodgins GA. Does one size really fit all? Why the mental health of rural Australians requires further research. Australian Journal of Rural Health 2002; 10: 288-295.
15. Leight S. The application of a vulnerable populations conceptual model to rural health. Public Health Nursing 2003; 20: 440-448.
16. Nelson E, Mohr J, Batalden P, Plume S. Improving health care part 1: the clinical value compass. Journal on Quality Improvement 1996; 22: 243-258.
17. Bleeser J, Hallis J. Bush nursing centres report. Melbourne, VIC: Department of Human Services Victoria, 2003; 147.
18. Hegney D, McCarthy A, Pearson A. Effects of size of health service on scope of rural nursing practice. Collegian 1999; 6: 21-42.
19. Wakerman J. Access to health-care services in remote areas. In: Regional Australia summit. 27-29 October 1999. Canberra, ACT: Australian Government Department of Transport and Regional Services, 1999.
20. Humphreys J. Health service models in rural and remote Australia. In: D Wilkinson, I Blue (Eds). The new rural health. Melbourne, VIC: Oxford University Press, 2002.
21. Department of Human Services Victoria, Rural and Regional Health Services Branch. Rural directions for a better state of health. Melbourne, VIC: State Government of Victoria, 2005.
22. Department of Human Services Victoria, Gippsland Region. Remote area nurse statement of completion. Trarlagon, VIC: DHSV Gippsland, 2005.
23. Victorian Association of Health and Extended Care. Community care and bush nursing issues paper. Melbourne, VIC: VAHEC, October 2002.
24. Seith F, Purton R. Is bureaucracy interfering or helpful to volunteering? In: Proceedings, The heart beat of the nation. 6 August 2001; Adelaide, South Australia. Adelaide, Department of Human Services South Australia, 2001.
25. Reinholdt S. Managing change within the emergency services to ensure the long-term viability of volunteerism. Australian Journal of Emergency Management 1999-2000; 14: 6-9.
26. Department of Human Services Victoria. Gippsland Region Health, wellbeing and demographic profile. Melbourne, VIC: Rural and Remote and Community Services, 2002.
27. Wagner E, Austin BT, Davis C, Hindmarsh M, Schaefer J, Bonomi A. Improving chronic illness care: Translating evidence into action. Health Affairs 2001; 20: 64.
28. Quine S, Bernard D, Booth M. Health and access issues among Australian adolescents: a rural-urban comparison. Rural and Remote Health 3: 245. (Online) 2003. Available: www.rrh.org.au (Accessed 13 July 2007).
29. Dade Smith J. Australia's rural and remote health: a social justice perspective. Melbourne, VIC: Tertiary Press, 2004.
30. Kawachi I. Social capital as public health. The American Prospect 1997; 8: 56-59.
31. Leeder S. Social capital and its relevance to health and family policy, in health and family services policy forum. Sydney, NSW: University of Sydney, 1998.
32. Wilkinson D, Marmott M. Social determinants of health: the solid facts, 2nd edn. Geneva: World Health Organisation, 2003.
33. Wilkinson R, Pickett K. Income inequality and population health: A review and explanation of the evidence. Social Science and Medicine 2006; 62: 1768-1784.
34. Averill J. Keys to the puzzle: recognising strengths in a rural community. Public Health Nursing 2003; 20: 449-455.
35. Wilson-Barnett J, Barriball KL, Reynolds H, Jowett S, Ryrie I. Recognising advancing nursing practice: evidence from two observational studies. International Journal of Nursing Studies 2000; 37: 389-400.
36. Aiken L. Achieving an interdisciplinary workforce in health care. New England Journal of Medicine 2003; 348: 164-166.
37. Priestley S. Bush nursing in Victoria: 1910-1985 - The first 75 years. Melbourne, VIC: Victorian Bush Nursing Association and Lothian Publishing,1986.
38. Pointer S, Harrison J, Bradley C. National injury prevention plan priorities for 2004 and beyond: discussion paper. Canberra, ACT: Australian Institute of Health and Welfare, 2003.
39. East Gippsland Bush Nursing Network. quality improvement community standards Australia (QICSA) report: East Gippsland Bush Nursing Network. Melbourne, VIC: LaTrobe University. 2003

