Cell phones and personal computers have become increasingly popular as a medium for health education and promotion and as a mechanism to support healthy lifestyle behaviors1. Cellphone and smartphone ownership is proliferating worldwide, and while most pervasive in industrialized and higher income countries and populations, ownership in emerging nations and lower income populations is also increasing2. In 2015, 92% of the US population had cell phones, 88% had cell phone coverage with unlimited texting, and 68% of adults had smart phones with Internet access3,4. Undergraduate college students are among the most 'connected' demographic groups in the USA, as 98% report internet access of some kind and 92% report internet access through a personal laptop or cell phone5. Given the widespread availability of these devices, mobile applications have proliferated, and health promotion efforts increasingly rely on messaging, social media and other internet access to deliver health information and behavioral interventions.
Text messaging has been demonstrated to positively impact tobacco cessation efforts in studies conducted worldwide. A 2016 Cochrane review reported on 12 text-message-based tobacco cessation studies conducted in Australia, New Zealand, Switzerland, the UK and the USA. The meta-analysis of the studies' data revealed that smokers in the intervention groups were approximately 1.7 times more likely to be tobacco abstinent at 6 months after their quit date than those in the control groups6. Another recent systematic review of tobacco cessation text messaging programs included four studies implemented with young adults or college students. This review reported that text messaging was effective as either a standalone or adjunct mechanism, and that the intervention was well accepted by participants7.
Tobacco smoking is prevalent among American Indians (AIs) and Alaska Natives (ANs). According to findings from the National Health Interview Survey in 2014, 26% of AI/AN men and 33% of women aged 18 years or more reported current smoking, compared to 19% and 17%, respectively, of their white counterparts and 22% and 14% of black counterparts8. Smoking is even more prevalent in Northern Plains AI populations, with 42% of men and women reporting current smoking9. Despite the high prevalence of cigarette smoking in the AI population, there is a dearth of published research on smoking cessation interventions focused on this population. It is notable that only one randomized controlled trial focusing on AI populations was included in a 2012 Cochrane review of smoking cessation interventions for indigenous populations10. In that study, Johnson and associates examined tobacco abstinence rates among 601 AI clients at four urban clinics, including two sites that offered the 'Giving American Indians No-smoking Strategies' (GAINS) program and two that did not. No significant differences in abstinence rates were detected at 1 year post-intervention11. Another small randomized controlled trial published in 2014 reported the effects of culturally tailored versus generic smoking cessation counseling combined with pharmacotherapy (varenicline) on 103 adult AI participants' smoking abstinence. The authors reported no statistically significant differences between the participants receiving culturally tailored and standard counseling12. Other non or quasi-experimental studies examined the effects of smoking cessation counseling and pharmacotherapy on AI youth (n=79) and adults (n=317)13,14. Both studies reported non-significant changes in abstinence rates between intervention and control groups at follow-up, but both also indicated that community and participant interest and need warranted further study. Other studies document the tobacco smoking prevalence15, the importance of culturally relevant programs16,17, and special challenges in AI populations and their efforts to abstain from tobacco18. The authors are aware of no published studies that use culturally tailored text messaging to support tobacco cessation in AI populations.
In New Zealand, a randomized controlled trial using text messaging to promote smoking cessation among young adults found that 28% of intervention participants successfully quit smoking, as measured 6 weeks after the designated quit date, compared to 13% of controls19. A secondary analysis revealed that the intervention was as effective with Maori participants as it was with non-indigenous participants20. Therefore, the authors proposed to adapt this intervention for implementation in AI/AN populations, on the hypothesis that an approach with success in one indigenous group might be suitable for another with a broadly similar history of colonization and marginalization.
For rural AI/ANs, as with other marginalized groups in the U.S. and other countries, , limited data are available on ownership or access to cell phones and other technologies, or on the populations' preferences regarding the use of electronic media for health promotion. The aim of this study was to address this gap in the literature by surveying tribal college students in rural settings regarding their access to and use of electronic technologies and their preferences regarding the use of these technologies for health promotion purposes. The study also assessed participants' smoking prevalence and interest in participating in tobacco research studies.
Setting
Tribal colleges and universities are institutions of higher education that preserve and support Native ways and are located on or near AI reservations21. Sites for the present study were two tribal colleges in Montana, a Northern Plains state. Fort Peck Community College, on the Fort Peck Reservation in north-eastern Montana, home to the Assiniboine and Sioux tribes, has an enrollment of about 450 students, of whom 82% are AI/AN. Little Big Horn College, on the Crow Reservation in south-eastern Montana, has an enrollment of about 400 students, of whom 95% are AI/AN22. The rurality of each community was measured by using Rural-Urban Commuting Area designations, which apply US Census Bureau definitions and data on commuting to characterize rurality and urbanicity of geographic locations in the USA23. According to these designations, Fort Peck Community College is located in a 'small rural town' and Little Big Horn College is located in an 'isolated small rural town'. These designations are based on zip codes rather than county-level data, making them appropriate for Montana, which has counties the size of Rhode Island, and includes both urban and very rural areas.
Eligibility and enrollment
Study participants were recruited at both campuses in December 2013. Eligibility criteria included age 18 years or greater and enrollment at the local tribal college. Student assistants were hired, and after completing human subjects training were instructed on recruitment procedures, and helped to administer the project survey to participants. These student assistants visited classrooms and common spaces and, along with researchers, informed potential participants about the intent of the project and encouraged them to participate. Interested students completed a pencil and paper survey; per the exemption granted by ethical review, survey completion was considered implied consent. Respondents were compensated $10 for their time. Budgetary considerations limited the number of respondents to 200.
Data collection and measures
The study measure was a 22-item survey administered with paper and pencil, requiring about 10 minutes to complete. Some survey items were modified from the Canadian Internet Use Survey for Individuals or the American Indian Adult Tobacco Survey24,25 and others were developed specifically for the purposes of this study. Reliability and validity measures are available for those items adopted from previous studies; measures developed for the study were assessed by the research team which included AI researchers familiar with the topic and environment. A copy of the survey is available on request from the corresponding author. Items assessed computer access; computer availability (every day, all day, or only for a few hours); cell phone ownership; type of service plan (pre-paid versus monthly, limited versus unlimited text messaging); ability to access the internet by cell phone; average number of text messages sent daily (10 or more, 1-9, not every day, none); daily time spent on the internet by computer and phone combined (10 or more hours, 5-9 hours, 1-4 hours, less than 1 hour, no internet access); frequency of email use (daily, less than daily, not at all); interest in using the internet to schedule appointments, respond to health questionnaires, and find health information (frequently, sometimes, rarely, or never); and preferred media for reminders of vaccinations, health screening, and medical appointments (US mail, cell phone, email, text messaging, or Facebook).
Items on cigarette smoking and health status included current cigarette use (none or number of cigarettes or packs per day), age at smoking initiation, number of quit attempts (free response), and self-reported health status (five-point Likert scale with 1='poor' and 5='excellent'). Respondents also reported their age, gender, and race (AI/AN, White, Other) and indicated their interest in participating in the larger intervention study (Yes/No).
Statistical analysis
Frequencies to describe sample demographics, tobacco use, and ownership or access to a cell phone or computer were calculated. t-tests were used to examine group differences with regard to tribal college location, age, and gender. Data analysis was performed with the Statistical Package for the Social Sciences v22 (IBM; http://www.spss.com). An alpha error rate of 0.05 was considered the threshold for statistical significance in group comparisons.
Ethics approval
The institutional review boards of Washington State University, the University of Washington, Fort Peck Community College, and Little Big Horn College determined that the project was exempt from institutional review board review.
Descriptive findings
Despite verbal screening efforts, 32 out of 200 respondents did not meet inclusion criteria, with 30 reporting that they were not tribal college students, and two ineligible due to age (one aged less than 18 years, and one with no age reported). Compared to eligible respondents, the 32 respondents who were ineligible were older, more likely to be male, and less likely to have access to computers or cell phones. Students were not required to declare their race prior to completing the survey; 12 of the 168 eligible respondents reported their race as white and three reported 'other'. The results reported here are findings from analyses of the data obtained from the remaining 153 students aged 18 years or older who reported they identified as AI/AN.
Participant demographics and smoking behaviors
The mean age of eligible respondents was 29 years (range 18-64 years), and 85 (56%) were female. Eighty four (55%) studied at Little Big Horn College and 45% at Fort Peck Community College. One hundred and thirty four (88%) reported good to excellent health, 12% reported fair health and none reported poor health. The prevalence of self-reported current smoking was 40%. The mean age at smoking initiation was 16 years, with 90% of current smokers reporting initiation by the age of 18 years. Ninety six or 63% of all respondents responded to the 'age of initiation', indicating they had tried cigarettes at some point in their lives. Approximately two-thirds of smokers indicated that they smoked less than half a pack of cigarettes per day. The average number of quit attempts was four (range 0-50 attempts). Participant demographics and tobacco use are summarized in Table 1.
Cell phone use and computer access
Across both sites, 131 respondents (86%) owned a cell phone, 98 (75%) of those had monthly plans, and 33 (25%) had prepaid plans. A total of 104 (80%) of cell phone owners reported having internet access on their phone. However, about 38% of those 104 individuals reported that internet access was either too slow to use easily or available only at certain locations in their community. A total of 122 (93%) of cell phone owners had unlimited text messaging, and the same proportion also reported at least occasional text messaging, with 65% texting 10 or more times per day.
Most respondents (146 or 95%) reported having access to a computer, although one-third of those did not have daily access. Eighty-five (about 60%) of the 146 with computer access reported the ability to use a computer at any time. About 84% of all respondents reported spending 1 hour or more on the internet per day, and 93% reported using email, although two-thirds of those did not check email daily. Computer and cell phone access is summarized in Table 2.
About half (49%) of respondents with cell phones reported they would either frequently or sometimes use online health appointment scheduling. Two-thirds would frequently or sometimes respond to online health questionnaires, and one-third would frequently or sometimes use websites to view or update their personal health information. t-tests indicated no significant differences in these variables by gender or smoking status (data not shown). Internet access and use patterns are summarized in Table 3.
Interest in participating in tobacco cessation research and frequency of messages
Respondents with cell phones were asked about their interest in a health research project that used text messaging to stop smoking and their preferred frequency for messaging. Among the 131 respondents with cell phones, 70 (53%) indicated they were interested, and 60 (46%) indicated they were not. Responses of the 49 cell phone owners who were also smokers were of particular import; 29 (59%) reported being interested in participating in the research, 19 (39%) were not, and 1 (2%) did not respond. Cell phone owners who were smokers reported their preferred frequencies of messaging for health behavior education as once or twice per week (45%) and once or twice per month (41%). Few respondents (8%) preferred receiving messages once or twice per day.
Inferential statistics
No significant differences were observed in cigarette use whether by tribal college site (t(151)=1.16, p=0.250), age (<23 years vs ≥23 years) (t(151)= -0.829, p=0.408), or gender (t(150)=0.959, p=0.339). These results are inconsistent with previous studies reporting a higher prevalence of smoking in males than females26-28. In general, nonetheless, self-reported health status in the study sample was consistent with recent research among AI/AN college students29.
There were significant differences in cell phone ownership and internet capability on cell phones by site, with the more remote site reporting lower levels of both ownership and access to internet through their phones (t(151)=-2.87, p=0.005; and t(128)= -2.55, p=0.012, respectively) (Table 4).
Table 1: Participant demographics and tobacco use (n=153)
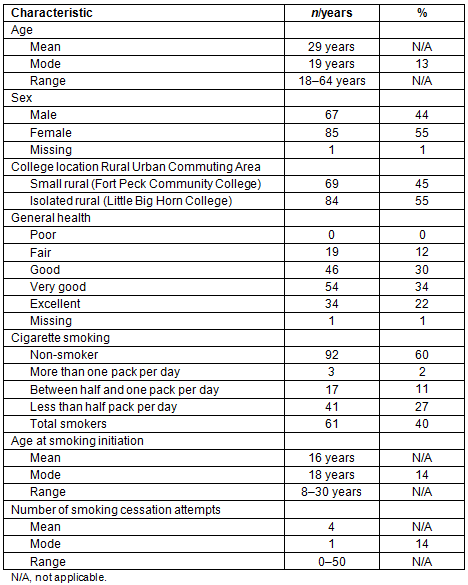
Table 2: Access to computers and cell phones (n=153)
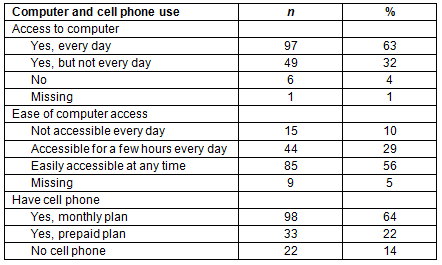
Table 3: Internet access and use (n=131)
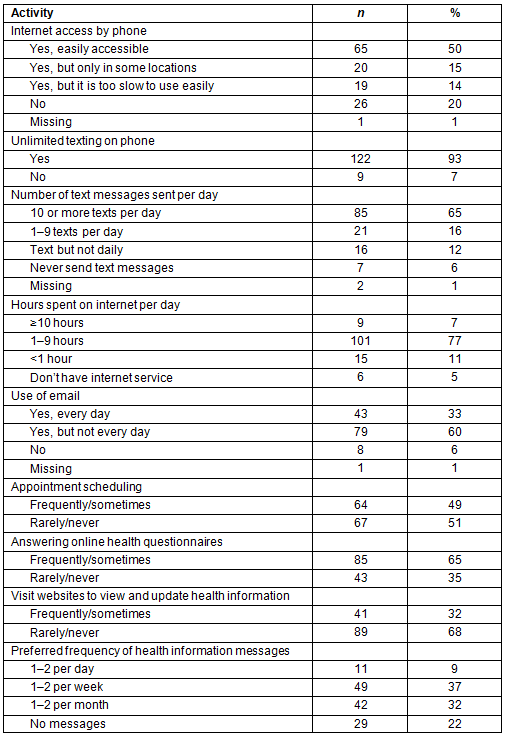
Table 4: t-tests access to computers and cell phones by campus (n=153)
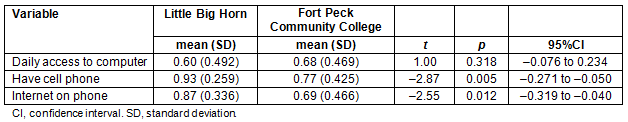
Discussion
Forty percent of study participants reported being current smokers, similar to the 37.0% reported for 18-25-year-old AI/ANs on the 2013 National Survey on Drug Use and Health30. This proportion is consistent with recent research on self-reported health behaviors by AI/AN college students, in which 44% of Northern Plains students reported smoking tobacco 'now'31. The mean age at smoking initiation (16 years) was similar to that reported in previous studies among AIs in the Northern Plains32.
About 63% of respondents reported daily computer access, a much smaller proportion than the 92% for non-students and 100% for college students reported for the all-races population in a survey on internet use in 20115. A total of 104 (80%) of those with cell phones reported having access to the internet on their phones, however, only 65 (50%) of those with phones had consistent internet, with the other 39 (30%) reporting inconsistent access due to location or low signal. These proportions are lower than a 2014 Pew Foundation survey which reported that 85% of young adults (aged 20-29 years) had smart phones (with internet access)33. The authors note that internet access and cell phone use vary widely in rural communities, with limiting factors including location of service towers, efficiency of service providers, and income and resources of users.
Limitations of this study include a small sample size and recruitment of participants at only two sites. This limited size and scope preclude generalization of results to other tribal communities or student populations. Approximately 300 students were enrolled at each of the colleges during the data collection period; therefore, the sample represented approximately one-third of the colleges' populations. Also, it should be noted that because recruitment for survey participation was largely by word of mouth, and was conducted during a limited time frame, in person, on campus, the authors may have obtained a sample that was more able to travel to campus, or be in classes on the given days, thus potentially excluding otherwise eligible students with less access to transportation or other resources.
These results guided the recruitment plan and research design for the authors' larger intervention study. They can also help to remedy the general lack of information on cell phone access and internet use among AI/ANs, while offering insight into the preferences of AI/AN college students regarding the use of digital media for health information34. Younger participants in the study were especially likely to own cell phones and to use digital media. The well-known 'digital divide' in access to technology disproportionately affects rural and low-income people in the USA, including many AI/ANs35,36. Even though access to the internet and other technologies is now an expected feature of everyday life and important in college settings, such access is often restricted for Native people37,38. Limiting factors include individual and family income, both of which tend to be low in AI/AN communities, as well as available infrastructure, which is generally less than optimal in rural areas, where most AI reservations are located39,40.
Effective smoking cessation programs in tribal communities, especially interventions using text messaging and other technology-dependent delivery systems, must be designed and implemented with a thorough understanding of resources and access. More research is needed to assess the impact of the digital divide on health and health services in rural Native and other marginalized communities, and to identify realistic, responsive interventions in partnership with community leaders.
References
1. Evers KE. eHealth promotion: the use of the internet for health promotion. American Journal of Health Promotion 2006; 20(4): 1-7.
2. Pew Research Center. Emerging nations embrace internet, mobile technology. Washington, DC: Pew Research Center, 2014.
3. Anderson M. Technology device ownership: 2015. (Internet) 2015. Available: http://instantcensus.com/blog/almost-90-of-americans-have-unlimited-texting (Accessed 16 November 2016).
4. Zagorsky J. U.S. cellphones with unlimited texting. December 7, 2015 ed. Boston, MA: Instant Census; 2015.
5. Smith A, Rainie L, Zickuhr K. College students and technology. Pew Research Internet Project. (Internet) 2011. Available: http://www.pewinternet.org/2011/07/19/college-students-and-technology/. (Accessed 14 December 2014).
6. Whittaker R, McRobbie H, Bullen C, Rodgers A, Gu Y. Mobile phone-based interventions for smoking cessation. Cochrane Database Of Systematic Reviews 2016; 4: CD006611.
7. Sampson A, Bhochhibhoya A, Digeralamo D, Branscum P. The use of text messaging for smoking cessation and relapse prevention: a systematic review of evidence. Journal of Smoking Cessation 2015; 10(1): 50-58.
8. Jamal A, Homa D, O'Connor E, Babb S, Caraballo R, Singh T, et al. Current cigarette smoking among adults - United States, 2005-2014. Morbidity and Mortality Weekly Report 2015; 64(44): 1233-1240.
9. Cobb N, Espey D, King J. Health behaviors and risk factors among American Indians and Alaska Natives, 2000-2010. American Journal of Public Health 2014 (Suppl.3): S481-S489.
10. Carson KV, Brinn MP, Peters M, Veale A, Esterman AJ, Smith BJ. Interventions for smoking cessation in Indigenous populations. Cochrane Database of Systematic Reviews 2012 (1).
11. Johnson KM, Lando HA, Schmid LS, Solberg LI. The GAINS project: outcome of smoking cessation strategies in four urban Native American clinics. Giving American Indians no-smoking strategies. Addictive Behaviors 1997; 22(2): 207-218.
12. Smith SS, Rouse LM, Caskey M, Fossum J, Strickland R, Culhane J, et al. Culturally tailored smoking cessation for adult American Indian smokers: a clinical trial. Counseling Psychologist 2014; 42(6): 852-886.
13. D'Silva J, Schillo BA, Sandman NR, Leonard TL, Boyle RG. Evaluation of a tailored approach for tobacco dependence treatment for American Indians. American Journal of Health Promotion 2011; 25(S5): S66-S69.
14. Horn K, McGloin T, Dino G, Manzo K, McCracken L, Shorty L, et al. Quit and reduction rates for a pilot study of the American Indian Not On Tobacco (N-O-T) program. Preventing Chronic Disease 2005; 2(4): A13-A13.
15. Horn K, Noerachmanto N, Dino G, Manzo K, Brayboy M. Who wants to quit? Characteristics of American Indian youth who seek smoking cessation intervention. Journal of Community Health. 2009; 34(2): 153-163.
16. Fu SS, Rhodes KL, Robert C, Widome R, Forster JL, Joseph AM. Designing and evaluating culturally specific smoking cessation interventions for American Indian communities. Nicotine & Tobacco Research 2014; 16(1): 42-49.
17. Gryczynski J, Feldman R, Carter-Pokras O, Kanamori M, Chen L, Roth S. Contexts of tobacco use and perspectives on smoking cessation among a sample of urban American Indians. Journal of Health Care for the Poor & Underserved 2010; 21(2): 544-558.
18. Hendricks PS, Westmaas JL, Ta Park VM, Thorne C, Wood S, Baker M, et al. Smoking abstinence-related expectancies among American Indians, African Americans, and women: potential mechanisms of tobacco-related disparities. Psychology of Addictive Behaviors 2014; 28(1): 193-205.
19. Rodgers A, Corbett T, Bramley D, et al. Do u smoke after txt? Results of a randomised trial of smoking cessation using mobile phone text messaging. Tobacco Control 2005; 14(4): 255-261.
20. Bramley D, Riddell T, Whittaker R, Corbett T, Lin RB, Wills M, et al. Smoking cessation using mobile phone text messaging is as effective in Maori as non-Maori. New Zealand Medical Journal 2005; 118(1216): U1494-U1494.
21. American Indian Higher Education Consortium. Tribal colleges and universities. (Internet) 2014. Available: http://www.aihec.org/our-stories/TCUmovement.cfm. (Accessed 17 October 2014).
22. American Indian College Fund. Tribal college listing. (Internet) 2015. Available: http://www.collegefund.org/tribal_colleges_listing (Accessed 26 June 2015).
23. Rural Health Research Center. Rural-Urban Commuting Areas (RUCA) data. (Internet) 2011. Available: http://depts.washington.edu/uwruca/ruca-codes.php. (Accessed 14 November 2014).
24. Statistics Canada. Canadian internet use survey (individual). Ottowa: Statistics Canada, 2012.
25. Weber J, Thorne J. American Indian adult tobacco survey implementation manual. Atlanta: US Department of Health and Human Services, Centers for Disease Control and Prevention, 2008.
26. Jamal A, Agaku IT, O'Connor E, King BA, Kenemer JB, Neff L. Current cigarette smoking among adults - United States, 2005-2013. Morbidity and Mortality Weekly Report. 2014; 63(47): 1108-1112.
27. Henderson PN, Kanekar S, Wen Y. Patterns of cigarette smoking initiation in two culturally distinct American Indian tribes. American Journal of Public Health 2009; 99(11): 2020-2025.
28. Spear S, Longshore D, McCaffrey D, Ellickson P. Prevalence of substance use among White and American Indian young adolescents in a Northern Plains State. Journal of Psychoactive Drugs 2005; 37(1): 1-6.
29. Patterson-Silver Wolf D, VanZile-Tamsen C, Black J, Billiot S, Tovar M. A comparison of self-reported physical health and health conditions of American Indian/Alaskan Natives to other college students. Journal of Community Health 2013; 38(6): 1090-1097.
30. Substance Abuse and Mental Health Services Administration and Center for Behavioral Health Statistics and Quality. Results from the 2013 National Survey on Drug Use and Health: detailed tables. (Internet) 2014. Available: http://www.samhsa.gov/data/sites/default/files/NSDUH-DetTabs2013/NSDUH-DetTabs2013.htm. (Accessed 16 September 2016).
31. Choi WS, Nazir N, Pacheco CM, Filippi M, Pacheco J, Bull J, et al. Recruitment and baseline characteristics of American Indian tribal college students participating in a tribal college tobacco and behavioral survey. Nicotine & Tobacco Research 2016; 18(6): 1488-1493.
32. Nez Henderson P, Kanekar S, Wen Y, Buchwald D, Goldberg J, Choi, W, et al. Patterns of cigarette smoking initiation in two culturally distinct American Indian tribes. American Journal of Public Health 2009; 99(11): 2020-2025.
33. Pew Research Center. Smartphone ownership highest among young adults, those with high income/education levels. (Internet) 2015. Available: http://www.pewinternet.org/2015/04/01/us-smartphone-use-in-2015/pi_2015-04-01_smartphones_07 (Accessed 6 March 2017)
34. Filippi M, McCloskey C, Williams C, Bull J, Choi W, Allen G, et al. Perceptions, barriers, and suggestions for creation of a tobacco and health website among American Indian/Alaska Native college students. Journal of Community Health 2013; 38(3): 486-491.
35. Goode J. Mind the gap: the digital dimension of college access. Journal of Higher Education 2010; 81(5): 583-618.
36. Bissell T. The digital divide dilemma: preserving Native American culture while increasing access to information technology on reservations. Journal of Law, Technology & Policy 2004; spring: 129-152.
37. Salpeter J. Inside the divide: despite progress, it's still a tale of missed connections. Technology & Learning 2006; 26(8): 22.
38. Access to telecommunications technology: bridging the digital divide in the United States. Congressional Digest 2013; 92(4): 2-5.
39. Maccartney S, Bishaw A, Fontenot K. Poverty rates for selected detailed race and hispanic groups by state and place: 2007-2011. Washington, DC: U.S. Census Bureau, 2013.
40. Wolff RS, Andrews E. Broadband access, citizen enfranchisement, and telecommunications services in rural and remote areas: a report from the American frontier. IEEE Communications Magazine 2010; 48(5): 128-135.
