Although 20% of Canadians live in rural or remote areas1, and, disproportionately, half of Canadian emergency care is delivered in rural or small urban centers2, assuring the availability of emergency medical expertise has been difficult. Canadian rural emergency departments have limited access to medical consultants, surgeons, and intensive care support3,4, and these deficiencies vary dramatically between provinces5,6. Furthermore, physicians in rural hospitals may not have formal emergency training7, and nurses in remote or isolated communities may not have the necessary training or supports available for critically ill patients8.
The inherent differences of rural emergency medicine may also present challenges to maintain medical competency9. Lower patient volumes, lower rates of procedures, and infrequent exposure to critically ill patients may present difficulties for rural physicians in maintaining skills and knowledge10,11. Nevertheless, patients presenting to rural departments are still triaged in urgent categories, and they represent a very wide breadth of emergent presentations12. Some of these presentations may be different than those in urban contexts13, suggesting subtleties unique to urban contexts that need to be appreciated.
Innovative continuing medical educational support for Canadian rural physicians14, nurses15,16 and other healthcare providers is required to deliver effective team emergency care. Gaining access to quality professional development, however, may be onerous. Simulation may be part of the solution, but the cost, lack of simulation expertise, and potentially weaker ties or distance to tertiary centers may deter health professionals from seeking such experiences17,18. Mobile emergency simulation may mitigate these issues - programs for obstetrics18, surgical procedures19, and war trauma20 have been reported. These initiatives appear to be feasible and practical18,19 and may enable training and assessment over a 1-week trauma course20. However, to the authors' knowledge, no studies have addressed rural mobile emergency simulation programs. This article reports an evaluation of Canadian rural healthcare providers' satisfaction related to emergency simulation training using a mobile education unit (MEU).
Methods
Rural centers
Data were collected during 14 educational sessions held in nine different communities in southern Manitoba, between 4 June and 3 November 2015. Catchment populations for the rural centers of the communities ranged from <5000 to >20 000 people. Emergency department hours varied from <12 h to 24 h a day, and the departments were staffed with either a registered nurse only or a registered nurse and two or more physicians.
Mobile education unit
The Shock Trauma Air Rescue Service (STARS) MEU (Fig1) is a motorhome that has been converted to a medical simulation lab. 'Stan', the high fidelity mannequin (CAE Healthcare, Saint-Laurent, Quebec) in the MEU, speaks, breathes, blinks, and has reactive pulses and pupils. It mirrors patient responses to such procedures as CPR, intravenous medications, intubation, and ventilation.
The goals of the MEU sessions are to enhance critical care skills and crisis resource management (CRM) for rural healthcare providers who have barriers of distance and difficulties leaving their own communities regularly to train. CRM addresses the skills necessary for effective teamwork during a crisis, including communication, leadership, resource utilization, situational awareness, and problem solving21-23.
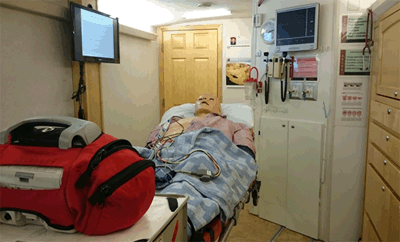
Figure 1: Case room of the mobile education unit simulation lab.
Simulation sessions
The host rural clinical educator initiated over 85% of simulation outreaches by first contacting STARS. The MEU simulation cases were a combination of polytrauma, severe sepsis, and inferior myocardial infarction with right ventricular involvement, or others suggested by rural clinical educators. Each group participated in a 90-minute session that allowed up to five rural healthcare providers to participate in one simulation case, followed by observing another case. A preliminary thread was presented to the team before they managed the 20-minute case to its conclusion. Each session comprised an introduction and pre-brief (10 minutes), simulated case 1 and debrief (20 minutes each), then simulated case 2 and debrief (20 minutes each).
Approximately half of each group were active participants in a case while the other half observed. For the second case, the groups traded roles so that each had a chance to actively participate in one case. Both learner participants and learner observers were invited to take part in the debriefing sessions. The sessions were facilitated by STARS transport physicians, flight nurses and/or flight paramedics, using the PEARLS (Promoting Excellence And Reflective Learning in Simulation) debriefing framework24. Debriefs conformed to an advocacy-inquiry model, with the goals of creating a safe context for learners to engage learning objectives, examining ideas and thought processes (cognitive 'frames') that lead to a learner's behavior, assisting the learner to identify ways to improve his/her performance, and inviting active reflection on the experience and learning attained25. One author (BB) facilitated simulations and led debriefs for a subsection of rural healthcare providers.
Simulation feedback form
The authors searched PubMed using the keywords 'simulation training', 'personal satisfaction' and 'program evaluation'. Original studies were retrieved, and the reference list reviewed. Relevant articles were reviewed, two studies were prioritized26,27, and a feedback form was created. To ensure ease of completion, face validity, and clarity, three healthcare providers with extensive simulation experience were interviewed to address potential redundancy and/or omissions, and to determine if the stated outcomes were addressed. A few modifications ensued, and the feedback form was finalized. Eleven questions were answered on a five-point Likert scale (1 ('disagree' or 'unacceptable') to 5 ('agree' or 'excellent')), followed by six short-answer questions. Participants were enumerated with an attendance sheet, and asked to complete an anonymous feedback form at the conclusion of session.
Ethics approval
The University of Manitoba granted ethics approval for this study (HS19433(H2016:051)).
Results
Data from 131 respondents were analyzed, for a response rate of 75.6%. Respondents included nurses (27.5%), medical residents (26.7%), medical first responders (16.0%), and physicians (12.2%). Other professions or training streams represented included paramedics, physician assistants, air ambulance pilots, medical students, and medical first responder students.
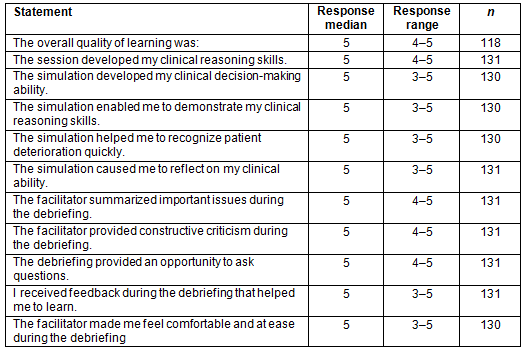
Not all subjects responded to every item on the feedback from, thus sample size varies for each question. The median for all 11 questions was 5 on the Likert scale, with a range of 4-5 on five questions (Table 1).
Respondents reported that the overall quality of learning was excellent, and that the simulation developed clinical reasoning skills and decision-making ability, helped in recognizing patient deterioration quickly, and allowed for self-reflection. The debrief summarized important issues, provided constructive criticism, and the feedback helped participants to learn.
In selected short answers, respondents reported that the MEU provided a believable working environment (87.0%, n=114), they had limited or no previous access to high fidelity mannequins (82.7%, n=107), and they had no specific training in CRM or were unfamiliar with the term (92%, n=118).
Discussion
The purpose of this article is to summarize satisfaction feedback from a wide scope of Canadian rural health providers on the high fidelity simulation of emergency cases. The feedback form responses indicated that the MEU was perceived to be clinically useful, and that the facilitator-led debrief was a safe and positive educational experience. Furthermore, the MEU was thought to provide a believable working environment for providers who have not been trained in CRM and have very limited access to high fidelity mannequins.
The MEU was able to provide an emergency educational session to rural healthcare providers from a minimum of nine different professions and/or training streams, ranging from student medical first responders to emergency trained physicians. While such a wide scope of experiences may present unique challenges to the learning environment, the diversity reported may also be very beneficial. First, it builds upon the collaborative efforts of multiple and heterogeneous providers involved in rural emergency care. Second, the paucity of physicians (~12% of respondents) in the simulations may accurately reflect rural health centers where patients are managed by nurses, and not physicians9. Third, it may address some limitations of training streams that lack educational resources or ties to larger institutions17,18. More than 80% of respondents in this study had very limited access to high fidelity simulation, suggesting growth areas for rural education.
The MEU was perceived to be clinically useful in developing reasoning skills and decision-making abilities, and in recognizing patient deterioration. This is consistent with review articles that concluded simulation sessions purportedly facilitate learning28,29. To optimize the experience, the authors of the present study were often able customize cases at a rural center's request, mimicking past difficult cases or addressing an area of need. Furthermore, over 87% of respondents found the cases believable. This likely has clinical relevance, as other studies have reported that realistic simulations provide opportunities to practice skills, increase confidence and promote critical reflection30,31. However, it remains uncertain whether the MEU educational experience will transfer to the bedside.
The respondents also reported that the debriefing promoted introspection and learning. This has been described as the most important aspect of simulation training - the 'heart and soul' of the program32 - and MEU facilitators were instrumental in the process. Debriefers must encourage positive transformative changes, while potentially navigating through learner anxieties, perceived poor performance, or negative emotions33. They also facilitate discussions about CRM. Particularly in the diverse and mixed groups of the present study, simulation training was a means to address CRM goals by 'facilitating cultural changes needed for a collaborative team environment with effective communication styles that extend to all workplace interactions'33. Interestingly, most respondents were not familiar with CRM, suggesting areas to enhance self-awareness and personal growth.
The major limitation of the present study was the reliance on self-reporting. Self-reporting may be biased, unreliable and prone to error. The authors note that median Likert scoring clustered around 'excellent' with a narrow interquartile range. However, the feedback form was based on a validated peer-reviewed evaluation tool developed for nursing and paramedic students for simulation training27, and the results are based on the feedback from 131 respondents. The authors also recognize that the study was not structured to assess changes of bedside competency following the simulation training. The assessment of high satisfaction is nevertheless important, as this is a crucial element for meaningful learning34.
Conclusions
A high level of satisfaction was reported in rural health providers after emergency simulation training using an MEU. Access to a comprehensive simulation program and knowledge about CRM was limited, suggesting potential educational growth areas.
Statement of conflict of interest
Dr Douglas Martin (Medical Director) is a contractor to STARS. Brent Bekiaris (mobile education leader) is an employee of STARS. Neither has received funding nor financial incentives for this study.
References:
