Introduction
Interprofessional practice and education (IPE) is critically important to the future of healthcare delivery. The benefits of IPE are well documented and include clear patient identified goals and a mutual trust among the healthcare team1. Furthermore, IPE provides opportunities to strengthen communication and collaboration skills while learning innovative patient care delivery2. While many institutions are implementing IPE into their didactic curriculum, fewer have taken the next step of putting IPE theory into practice by pairing students from different disciplines on concurrent clinical rotations with supporting IPE activities. Moving IPE from the classroom to the clinic is important so students can 'learn by doing', with the ultimate goal being future clinicians better trained for team-based care.
There are challenges inherent in placing clinical learners from different training programs into a concurrent interprofessional clinical experience. Competing curricular requirements, uneven clinical modeling of interprofessional care and differing learner clinical expectations can confound efforts to provide robust interprofessional experiences to interprofessional learners on a clinical rotation. These challenges can be exacerbated when learners are on an away clinical rotation where there is little control of the learning environment and the interprofessional standards of care may vary. These challenges may be why the majority of IPE programs currently take place in the academic rather than clinical learning settings3.
The Combined Medical-Physician Assistant Student Rural Rotation (Med-PARR) pilot program at the Oregon Health and Science University addresses the challenges of placing two clinical learners concurrently in a rural clinical location. The program uses student-driven curricular activities that overlay, or 'float', on top of the clinical experience, giving students the opportunity to critically reflect on their interprofessional roles while participating in their rural clinical settings.
Program description
The Med-PARR was developed jointly by PA and MD program faculty members at the university in 2013. Separate pairs of third-year MD students and second-year PA students spend a 5-week rural, primary-care-focused clinical rotation together in the same location. During the rotation, students share a living environment as well as common IPE activities. Clinical learning environments vary by site: some student pairs practice in the same clinic in a team-based model while other sites have learners in the same clinical location but with little interaction with one another. In some cases, pairs will practice in the same rural location but in different clinical sites. As clinical environments vary, Med-PARR students rely on shared educational activities that 'float' on top of their clinical experiences to address IPE objectives. These activities foster critical reflection on the interprofessional experience as well as real-world application of interprofessional teamwork through a rural community project.
'Floating' interprofessional education activities
Obstacles such as scheduling conflicts and concurrent, conflicting curricular programming specific to each profession can challenge efforts to implement IPE curricular activities in clinical settings. Too many additional IPE curricular requirements can overload students with busy clinical obligations and program-specific curricular requirements, many of which may be necessary for accreditation purposes. Conversely, too few IPE-specific requirements may downplay the importance of the IPE experience and miss opportunities for critical student reflection. The Med-PARR's IPE activities address these issues by 'floating' on top of the relative curricular requirements of each student's program and, in some cases, by capitalizing on existing elements. Students spend the majority of their rotation participating in their individual clinical requirements.
The amount of clinical integration between the MD and PA student varies by rural clinical site, with some students working together and others not at all. While less than ideal, this variability is largely out of the control of the academic program. The Med-PARR IPE activities serve as the curricular overlay to overcome this variability and compel the students to critically reflect on their IPE experience and one another in a manner that complements their relative programmatic and clinical requirements. Students may have variable integration in their clinical experiences at their rural site, but the activities that 'float' on top of their clinical experiences give them the opportunities for interprofessional collaboration they often lack in clinic. Efforts are also made to match MD and PA student rotation start and stop times, permitting maximized IPE time and easier scheduling.
Goals and reflections
There are two Med-PARR floating IPE activities: goals and reflection and the community project. At the beginning of the rotation students identify three interprofessional-focused goals they would like to achieve from the IPE experience. At the end of the rotation, students reflect on those goals and how successful they were in meeting each. Faculty members provide students with feedback on their goals and reflections.
Community project
The community project is a combined educational activity that MD and PA students must work on together throughout their 5-week rotation. Students must submit a questionnaire early in their rotation that addresses the project's subject, goals, and plan for dissemination to an audience in their rural location. The project should relate to a healthcare issue appropriate to the students' rural context and should have a value-added effect on the rural community. The project culminates in a 15-minute presentation to university School of Medicine faculty at the conclusion of the rotation.
Experiences of an MD-PA pair
Since its inception, 24 MD and PA students have participated in the Med-PARR. The program has been well received by students in course evaluations and informal feedback. This section presents the experiences of one MD-PA pair as an example of the program. The students in the MD-PA pair gave permission for their work to be included in this article.
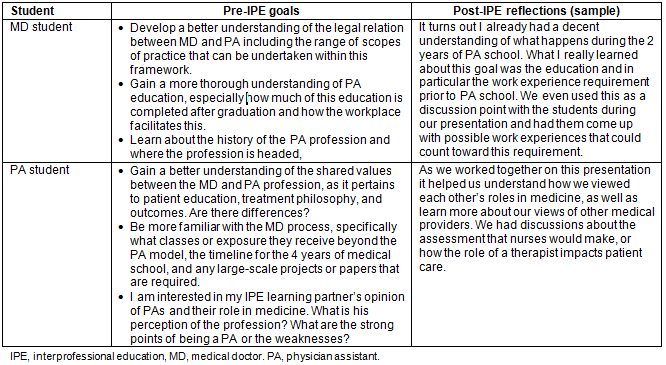
The MD student and the PA student participated in the Med-PARR in June 2015 at a rural family practice clinic in Oregon. The goals for each student are shown in Table 1. For their community projects these students decided to do a health professions career day at a local secondary school that entailed co-presenting to secondary school students about what each of their respective professions and other healthcare professionals (eg nurse, medical assistant) did and how they worked together in the clinical setting. They concluded their session with a suture workshop where both the MD and PA students demonstrated suturing techniques, using pig's feet, and coached the secondary school students to practice their own sutures.
The community project was well received by the secondary school students, and the school plans to continue the program with future MD and PA students. The Med-PARR students' post-experience reflections illustrate the positive impact of the program (Table 1).
Table 1: Comparison of Combined Medical-Physician Assistant Student Rural Rotation pre-experience goals and post-experience reflections
Discussion
This Med-PARR program description highlights how a 'floating' IPE activity approach can support interprofessional learning in variable rural clinical learning environments. These activities complement the already existing MD or PA program curricular and clinical requirements for learners of different specialties, thus alleviating common barriers to applied IPE clinical experiences. Furthermore, the 'floating' approach of the Med-PARR works in contrast to standalone IPE initiatives that rely heavily on multiple, planned activities with additive curricular requirements. In other words, less may be more in applied IPE.
A post-experience survey is currently being administered to gather additional data on the impact of Med-PARR. Application of the 'floating' IPE approach at other institutions either planning on or currently doing concurrent rural clinical placements of interprofessional learners will help to better understand how effective this approach may be in alleviating programmatic barriers and encouraging increased interprofessional clinical programming.
Ideally, the clinical site will model the interprofessional, team-based care necessary for a robust interprofessional learning environment. The reality is that clinical sites vary in their level of interprofessional care delivery. Site development is needed to grow all clinical learner sites into robust interprofessional learning environments for students. Until this happens, academic leaders can address variable interprofessional clinical sites through curricular efforts. Reflective, student-driven educational activities that 'float' on the clinical experience as exemplified by Med-PARR may serve as a model for other institutions with similar IPE initiatives.
Acknowledgements
The authors thank Michael-Hunter Clement (MD, class of 2016) and Joe Buck (PA, class of 2015) for allowing their student project to be highlighted in this article. The authors also thank LeNeva Spires, Publications Manager, Department of Family Medicine, Oregon Health and Science University, for her editing assistance and help with preparing this manuscript for publication.
References
1. Golden A, Miller KP. Championing truly collaborative team-based care. Annals of Internal Medicine 2013; 159(9): 640-642. https://doi.org/10.7326/0003-4819-159-9-201311050-00714
2. Spencer J, Woodroffe J, Cross M, Allen P. 'A golden opportunity': exploring interprofessional learning and practice in rural clinical settings. Journal of Interprofessional Care 2015; 29(4): 389-391. https://doi.org/10.3109/13561820.2014.970250
3. West C, Graham L, Palmer RT, Miller MF, Thayer EK, Stuber ML, et al. Implementation of interprofessional education (IPE) in 16 U.S. medical schools: common practices, barriers and facilitators. Journal of Interprofessional Education & Practice 2016; 4: 41-49. https://doi.org/10.1016/j.xjep.2016.05.002
