To deliver the rural health training, university academic and administrative staff are required to live and work locally in a range of rural 'campuses' across Australia. Students learn from and work with local health professionals and the broader community in these rural settings1. In 2016, the federal government committed further funds in support of quality rural health education to improve the health and wellbeing of rural and remote communities in Australia6. The resulting RHMT program aims to make a measurable impact on addressing the maldistribution of the rural health workforce. Depending on the education programs they offer, Australian universities accepting RHMT funds are required to place greater emphasis on improving recruitment and retention of professionals from nursing, dentistry, allied health and/or medicine in rural and remote Australia. The stated funding requirement for longer rural placements in all disciplines is an exciting opportunity for greater investment in interprofessional education to foster collaborative practice, a global health system imperative for care that is centred around the patient7.
A decade or so of higher funding support and targets (25% of Australian Commonwealth-supported students) for year-long rural medical placements has resulted in more longitudinal placements in medicine than for other disciplines. Now, with rural health professional education evolving to reflect the greater requirement for recruitment of rural origin students and long-term rural placements for all health disciplines, new educational possibilities unfold. Increased numbers of students from a range of disciplines, living, socialising and learning together over longer time periods, creates the ideal conditions to prepare students for future collaborative practice. We share insights into how to maximise this opportunity at rural education centres and suggest questions for ongoing reflection on how best to capitalise on these conditions.
Like others in Australia, our rural educational centre, with its extended placements for many health disciplines and its multiprofessional learning environment, has great potential for interprofessional education. Each student is supported by one or more academics from their own profession, and these academics support each other and all students during interprofessional learning activities. Administrative staff provide support for the program, including managing accommodation, coordinating social activities and assisting with preparation of educational activities. Commitment from managerial staff over many years has been crucial to the interprofessional nature of the centre.
At the centre of the insights shared in this perspective is our centre's relationship-focused research finding that rapport is core to 'how students in a co-located area learn to work with other health professions'8. The components of rapport that enabled students to learn to work together were identified in relation to interpersonal capabilities (being interested, being inclusive, developing interpersonal bonds, bringing a sense of own discipline, giving and receiving respect, and being patient-centred) and core contextual conditions for interprofessional-rapport-building opportunities (shared space, adequate time and balance of disciplines). While recognising the importance of an individual's interpersonal capabilities, this perspective focuses on the core contextual conditions.
Using a framework of core contextual interprofessional-rapport-building opportunities8, a cross-section of multidisciplinary academic and professional staff at the centre asked and/or were asked a series of questions to informally explore how the research findings had impacted on the centre's practice. They were encouraged to make explicit their current operational process behind ensuring that students were offered sufficient shared space, adequate time and balance of disciplines to ensure rapport-building between members of different professions. Key aspects of these core contextual conditions were iteratively discussed. The questions that arose from, and were part of, these discussions are shared in Table 1 as an illustration of how the model can be operationalised in a rural education context. By highlighting opportunities and challenges integral to facilitating students' development of interprofessional rapport on long-term rural placements, we invite international readers to reflect on the issues these questions raise, to encourage rapport-building between students in their educational contexts. Through such reflection, additional questions may be raised that are specific to readers' particular situations and experiences.
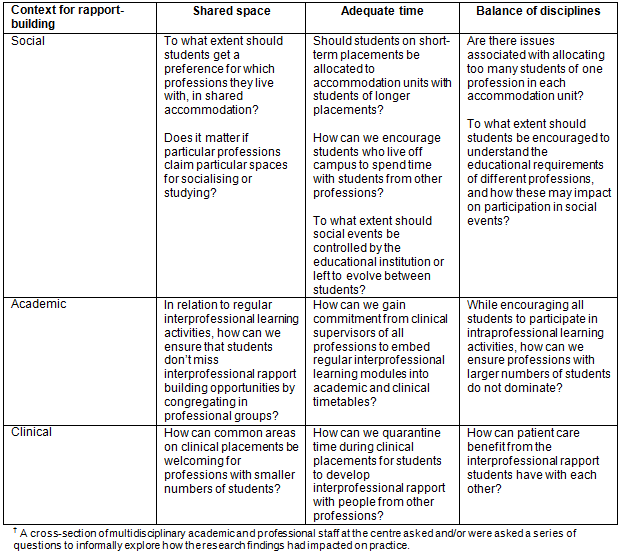
To build rapport between rural co-located students from many disciplines, the following issues are important: (i) congruence between core contextual conditions across a range of rapport-building opportunities and (ii) sensitivity for which aspects of rapport-building need to be explicitly controlled and which need to evolve organically. Key to the successful operationalisation of the interprofessional-rapport-building model is continuing to seek and maintain this congruence and sensitivity in relation to decisions made about shared space, adequate time, and balance of disciplines, for students to get to know each other and learn to work together for collaborative patient-centred practice. Readers can consider the relevance of these, and the balance and clarity between them, in their own educational settings.
Importantly the same issues need to be considered for educators and clinicians9; for example, what spaces do educators and clinicians of different professions share, and is there adequate time for them to 'get to know each other'? Academic program directors need to enable and support interprofessional-rapport-building opportunities for their staff as well as their students, and healthcare managers/leaders should reflect on the same contextual conditions to enable rapport-building between their health professionals.
Although the contextual issues have been foregrounded, clearly it is important to note that the behaviours of people within the spaces, time and professions are important for rapport10. Facilitating the development of these behaviours by exploring interprofessional "rapport-building moments" in clinical situations is currently being further researched by Croker and colleagues8-10 with findings potentially having utility for interprofessional education and collaborative practice. Translating interprofessional education in to collaborative practice is one of the challenges for health professional education11. Australian health policy-makers, by increasing the RHMT funding for longer term rural placements for all health professional students, have enhanced opportunity to co-locate rural learners and build interprofessional rapport. These early steps towards collaborative practice are usually more difficult to achieve in urban settings due to the logistics of staging interprofessional educationactivities for larger student numbers, and the reduced occurrence of interprofessional groups of students living together over time.
Educational leaders and academics globally should recognise that offering health professional students opportunity to live and work together in extended placements in rural settings has potential benefits for interprofessional education. Governance structures then need to facilitate time and space for interprofessional learning. Understanding the contextual conditions for building rapport between health professional learners, and reflecting on these, potentially will lay the foundation for collaborative practice when these learners become health professionals. Policy-makers, health managers and clinical leaders from medicine and all health disciplines must build on this foundation by considering the interpersonal capabilities and contextual conditions for rapport-building in the health workforce. This should foster a collaborative practice environment for graduates to embrace when they enter the health workplace.
Judith Hudson, University of Adelaide
Anne Croker, University of Newcastle
References:


