Colorectal cancer (CRC) is the second-leading cause of death in the USA1. The US Preventive Services Task Force recommends that adults aged between 50 and 75 years have a CRC screening, including fecal occult blood testing annually, sigmoidoscopy every 5 years, or colonoscopy every 10 years2. Despite the significant health benefits of routine CRC screening2-7, previous studies well documented the disparities between urban and rural communities in CRC screenings8-11. Primary care providers (PCPs) in rural clinics can play a critical role in improving CRC screening, by educating patients, providing accurate information, and recommending screening12. For rural patients, PCPs can be major source of information as 'physician recommendation' has been found to be the strongest predictor of rural patients' adherence to CRC screening13-16.
However, rural practitioners face many 'practice or delivery system-level' challenges in promoting CRC screening. Physicians report that lack of time is one of the most common barriers, especially for those who see high numbers of patients per day17. In addition, many rural patients visit the clinic on a non-routine basis, only visiting when they have acute health problems. Even for their routine visit, rural patients typically have other priority health issues (eg multiple chronic conditions) to be addressed first17,18. This may make it even more difficult for practitioners to recommend CRC screening within the limited time, or they may forget to mention it in the face of other, more pressing concerns. Electronic Health Records (EHR) system is a digital system for storing and managing patients' medical history, and includes key administrative clinical data relevant to patients' care. For many rural clinics, however, EHR functionalities, such as computer-aided automated flags or reminder systems, are not in place or are under-utilized19,20. The American Cancer Society suggests four essential strategies to improve CRC screening in primary care practice: provider recommendation, an office policy, an office reminder system for patients and physicians, and an effective communication system21. Despite the potential role of rural primary care practice in improving CRC screening, these practice-based, provider-oriented approaches have not been effectively developed and implemented in rural primary care settings.
An accountable care organization (ACO) is a healthcare delivery reform model that focuses on changes in the method of delivery and payment22. Unlike traditional methods of delivery, this new model allows healthcare providers from different settings (eg hospitals, physicians, post-acute providers, or others) to form an alliance to collectively manage and be responsible for the quality, cost, and overall care of a patient population22,23. The key features include an aligned provider network, implementation of quality measures, improved IT infrastructure, transformed clinical operations (eg standardized care pathways, primary care focus, care transition, and patient activation), and partnerships with payers24,25.
Theoretically, the principles and key features of ACO coincide with the elements required to promote CRC screening. For example, cancer screenings are one of the quality measures that ACO has to report to the payer, Center for Medicare and Medicaid Services (CMS), to receive group savings. Other features, such as improved health IT and primary care focus, may have positive impacts on the increase in CRC screenings. However, there is limited evidence on how an ACO impacts the CRC screening rate, especially in rural areas. To address this gap, this study aims to explore how rural healthcare professionals perceive the opportunities or challenges of an ACO for promoting CRC screening. The study discusses how the key features and components of a primary ACO promote evidence-based CRC screening practice in rural Nebraska. The findings of this study provide practical information that helps identify primary-focused, rural population-oriented programs based on alternative care delivery models (eg ACO) to effectively improve CRC screening.
Research design
The study is a qualitative case study to examine opportunities and challenges to promote CRC screening grounded in data collected from individual healthcare professionals in a rural primary care ACO26.
Study setting
The study setting is a physician-led primary care ACO in Nebraska, a Midwestern state in the USA. The ACO was participating in the group shared savings model based on fee-for-service reimbursement, called Medicare Shared Savings Program (MSSP), with 15 group-practice primary care clinics. These clinics are responsible for taking care of more than 21 000 people enrolled in Medicare, a national social insurance program administered by the US federal government. These clinics are located mostly in rural counties and range in size from 4 to 12 PCPs. All of the participating clinics have received or are working on completing patient-centered medical home (PCMH) certification and have adopted an EHR system. The core members of the ACO, including the executive director, chief medical officer, and a clinic integration specialist, have actively engaged in this study from the planning to execution stage by helping conceptualize the study, providing relevant data and feedback, and helping recruit interview participants. The participating ACO was ranked seventh in the nation among all MSSP ACOs by quality performance ratings in 201427.
Study sample
A convenience sampling approach was used with a referral strategy for recruiting individual participants26. Subjects were eligible for the study if they had at least 1 year of work experience in the participating ACO clinic and had been involved with CRC screening directly or indirectly. The study recruited PCPs (physician, nurse practitioner, or physician assistant), nurse coordinators, and IT/administration staff.
Data collection procedures
To recruit participants, the research team worked closely with the ACO leadership team. The participating ACO provided lists of potential participants, who were then invited to the study via email and follow-up phone calls by the research team. A cover letter explaining the research goals and procedures, and confidentiality statements, was attached to the email invitation. Verbal consent was obtained from each participant prior to the interview. The two researchers (first and third author) completed a total of 21 semi-structured individual interviews from June through November of 2015. Interviews were conducted face-to-face or by phone, depending on the interviewees' schedules and resources. The interview guide was developed by the research team and modified as the interview process continued. The duration of each interview was about an hour and was audio-recorded, transcribed, and independently coded by two of the study authors.
Data analysis
This study followed the basic principles of grounded theory data analysis28. An independent coder reviewed all transcribed quotes iteratively to ensure that no important ideas or constructs were overlooked. Codes were created for each new idea and themes were grouped together if they were conceptually similar or related in meaning. A second researcher reviewed the coded data for an informal consensus. Disagreements were discussed until a consensus was reached. NVivo v10 (QSR International; http://www.qsrinternational.com) was used for qualitative analysis.
Ethics approval
This research was approved by the Institutional Review Board by the University of Nebraska Medical Center (# 352-15-EP).
Table 1 displays characteristics of individual interviewees (n=21). Final participants included 10 PCPs (48%), 9 nurse coordinators (43%), and 2 IT/administrative personnel (10%). More than half (57%) of the interview participants were female. Participants had a median of 16 years of experience, from a minimum of 1 year to a maximum of 40 years. All the participating clinics are located in rural areas, as defined by the US Department of Agriculture Economic Research Service29. Nine are from rural areas with population of 20 000 or more, while 10 are from rural areas with populations between 2500 and 19 999. Two participants are from a completely rural area according to the Rural-Urban Continuum Code. The participating clinics' annual CRC screening rate for Medicare beneficiaries ranged from 65.7% to 79.2% in 2015 (Table 1).
Table 1: Participant characteristics (n=21)

Opportunities to promote colorectal cancer screening
Six themes emerged as the main opportunities for promoting CRC screening through a rural primary care ACO: enhanced EHR use, information sharing and learning within the ACO network, performance reporting and feedback, a shift to preventive/comprehensive care, an adoption of team-based care, and empowered care coordinators (Table 2).
Table 2: Themes: opportunities to promote colorectal cancer screening by rural practitioners in an accountable care organization context
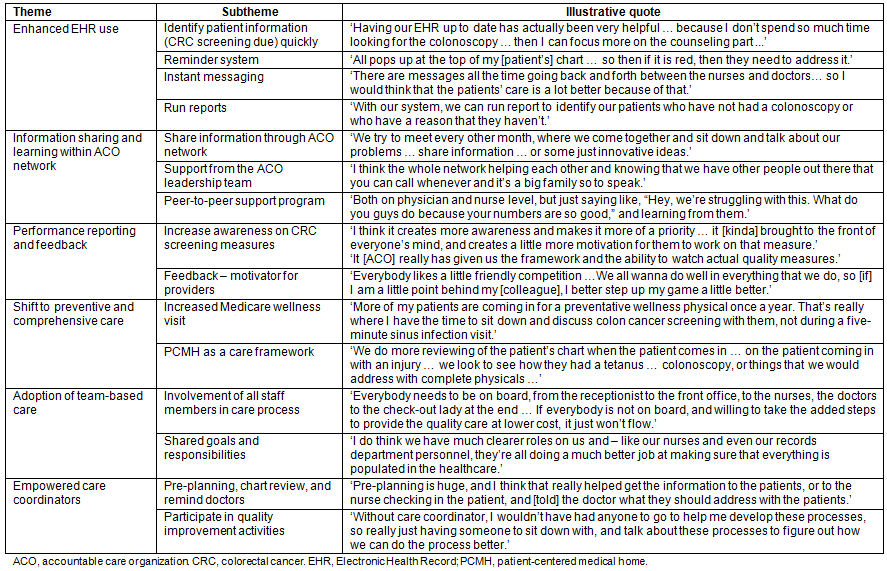
Enhanced electronic health record use: Rural practitioners perceived that enhanced use of EHR had been a great help for recommending CRC screening in several ways. First, the care process becomes more efficient because of the reduced time for searching and retrieving patient information about CRC screenings due. One physician said:
Having our EHR up to date has actually been very helpful for me, because I don't spend so much time looking for the colonoscopy ... then I can focus more on the counseling part rather than the patient trying to remember. (female, family physician, 4 years of experience)
Second, most providers reported that a 'computer-aided reminder' helped them initiate discussion about CRC screening with patients, regardless of the purpose of the visit (wellness or acute). According to a female registered nurse (RN) care coordinator, with 32 years of experience, '[Screening information] all pops up at the top of my [patient's] chart ... so then if it is red, then they need to address it.' Third, rural providers also use an instant 'messaging' function in the EHR system. This enhances communication between nurses and doctors by instantly sending short messages regarding a patient's screening due date or by immediate scheduling a next appointment. Fourth, rural clinics were able to use the 'create report' function from the EHR system. They could pull out the lists of patients who are due for CRC screening but have not done it yet and have staff members send out reminder letters or postcards to these patients. A female director of nurse with 10 years of career said, 'With our system, we can run reports to identify our patients who have not had a colonoscopy or who have a reason that they haven't.'
Information sharing and collaborative learning: The second theme emerging from this study's analysis was the role of the ACO network as an information sharing and learning collaborative in the rural setting. Learning takes place within an ACO network through regular meetings or communication among members. A female RN care coordinator, who started to work in this position a year ago said, 'We do try to meet, probably every other month, where we come together and sit down and talk about our problems ... share information ... or some innovative ideas.'
The ACO leadership team, consisting of experienced physicians, nurses, and the clinical data integration specialist, facilitate and coordinate ACO meetings, and provide technical support for clinics to set up programs or retrieve information. A health IT manager said:
So she [data specialist] came out and worked with us on where she was going to pull it from and stuff, so that we could figure out how to make the [reports]. (female, 33 years of experience)
Rural providers were reportedly highly positive about the ACO's peer support program. When members of a newly joined clinic were not sure how to launch a new program or set up protocols, existing members helped them by sharing tips or resources. This 'culture of helping' was particularly strong in the ACO.
Performance measures and feedback: The study participants appeared to have a broad consensus regarding the positive impact of using standardized measures required by CMS. They noted increased awareness among all the staff of the need to pay attention to those measures (eg percentage of patients who are up to date with CRC screening). The standardized quality measures gives them a structured framework of 'what' quality they need to focus on. Feedback mechanism was perceived to be of great value under the ACO model. Use of standardized measures and reporting these measures also enabled an ACO to receive feedback about their performance at a group level and at a clinic level. Group-level feedback is provided by the CMS when CMS compares performance scores of a certain ACO to their benchmarks. Clinic level feedback is provided by the ACO leadership team by comparing each clinic's performance to that of other clinics within the same ACO group. Most clinics have the capacity to retrieve their own charts and compare their numbers to other clinics or other providers. An RN care coordinator said:
Everybody likes a little friendly competition [laughs] ... We all wanna do well in everything that we do, so [if] I am a little point behind my [colleague], I better step up my game a little better, something like that. (female, 2 years of experience as RN coordinator)
Shift to preventive/comprehensive care: Rural providers mentioned that 'a shift to preventive care', such as Medicare wellness visits, was a big opportunity to introduce and initiate CRC screening to patients. Compared to other types of visit (eg acute or follow-up on hospital discharges), wellness visits allow providers more time to review various kinds of preventative measures. In addition, ACO and the mandated 33 quality measures were the main drivers for increasing extra attention on CRC screening. According to a physician:
More of my patients are coming in for a preventative wellness physical once a year. That's really where I have the time to sit down and discuss colon cancer screening with them, not during a five-minute sinus infection visit ... ACO helps promote more wellness exams, which is where we really catch our people. (male, 12 years of experience)
The participating ACO takes the PCMH model as its care framework, thus placing the emphasis on providing holistic care. This approach made providers check preventive screenings for patients, even for episodic visits.
Adoption of team-based care: Participants felt strongly that adoption of a team-based care was necessary for promoting cancer screening under this new model of care delivery system. Four subthemes emerged: involvement of all-clinic staff in the screening processes, clear roles and shared responsibilities, team meetings, and shared goals and objectives. One physician interviewee said:
Everybody needs to be on board, from the receptionist to the front office, to the nurses, the doctors to the check-out lady at the end ... If everybody is not on board, and willing to take the added steps to provide the quality care at lower cost, it just won't flow ... I do think we have much clearer roles on us and - like our nurses and even our records department personnel, they're all doing a much better job at making sure that everything is populated in the health care [setting]. (male, 12 years of experience)
Empowered care coordinator: The care coordinator role was perceived to be important in rural clinics. However, their roles have changed over time, due to the increasing amount of coordinating work and reduced staffing. While they used to do pre-planning, review patient charts before the patient visit, and remind doctors about CRC screening dues, now more clinics have transitioned care coordinator roles to post-discharge care, medication reconciliation, and management of high-risk patients. Still, care coordinators actively participated in the quality improvement activities (eg developing care-process maps). A physician said:
Without [the] care coordinator, I wouldn't have had anyone to go to help me develop these processes, so [it is] really just having someone to sit down with and talk about these processes to figure out how we can do the process better. (male, 5 years of experience)
Challenges to promote colorectal cancer screening
Despite all the opportunities for promoting CRC screening, operational and system-level challenges associated with this new delivery care model were found: financial instabilities, staff workload, lack of training or education opportunities, and lack of resources in rural areas. Table 3 shows four themes and related subthemes, as well as illustrative quotes regarding perceived challenges of the ACO model.
Table 3: Themes: challenges to promote colorectal cancer screening by rural practitioners in an accountable care organization context
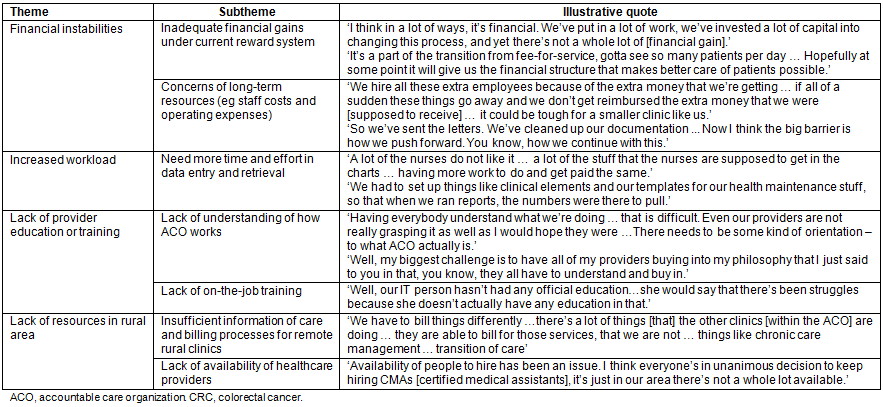
Financial instabilities: Rural providers expressed frustrations about their inability to generate financial savings from the current reimbursement plan (eg MSSP) in spite of their high performance rankings. A male physician in a rural clinic said:
I think in a lot of ways, it's financial. We've put in a lot of work, we've invested a lot of capital into changing this process, and yet there's not a whole lot of [financial gain]. (male, 5 years of experience)
They felt that they needed long-term financial resources to cover their staff costs and operating expenses. Another physician said:
We hire all these extra employees because of the extra money that we're getting ... if all of a sudden these things go away and we don't get reimbursed the extra money that we were [supposed to receive] ... it could be tough for a smaller clinic like us. (male, 5 years of experience)
A nurse director commented about long-term sustainability of the current program:
So we've sent the letters. We've cleaned up our documentation ... Now I think the big barrier is how we push forward. You know, how we continue with this. (female, 10 years of experience)
Increased workload: Throughout the interviews, the rural providers strongly felt that 'being a member of the ACO' means more 'work' for all staff members, including nurses, coordinators, PCPs, receptionists, and IT and administration staff. Even though they appreciated and were proud of quality improvement results that ACO brought, they still acknowledged that they needed to spend extra time and labor for good performance. The biggest area is to do a more rigorous data entry and retrieval. An RN care coordinator said:
A lot of the nurses do not like it ... a lot of the stuff that the nurses are supposed to get in the charts ... having more work to do and get paid the same. (female, 25 years of experience)
Lack of provider education or training: Most participants did not seem to fully understand what the ACO meant and how the ACO worked. Some lead physicians expressed difficulty motivating other providers in their clinics, who were not accepting the ACO or PCMH philosophy:
Well, my biggest challenge is to have all of my providers buying into my philosophy that I just said to you in that, you know, they all have to understand and buy in. (male, 17 years of experience)
In addition, care coordinators and IT/administrative staff perceived the immediate need for well-organized and practical on-the-job training. A female RN care coordinator commented:
Initially [the challenge was] not really knowing what my job was. What all I should be doing ... it took a while [to learn] and I think that was frustrating for me. (female, 30 years of experience)
Another participant made similar comments in terms of IT staff education: 'Well, our IT person hasn't had any official education ... she would say that there's been struggles because she doesn't actually have any education in that.'
Lack of resources in rural areas: Clinics located in a remote rural area had dissimilar care and billing processes, so they could not derive benefits from sharing information within the ACO network. One RN care coordinator at a remote rural clinic said:
We have to bill things differently ... there's a lot of things [that] the other clinics [within the ACO] are doing ... they are able to bill for those services, that we are not ... things like chronic care management ... transition of care. (female, 6 years of experience)
The lack of an available healthcare provider workforce was another challenge that the rural clinics reported facing. As explained by one family physician:
Availability of people to hire has been an issue. I think everyone's in unanimous decision to keep hiring CMAs [certified medical assistants], it's just in our area there's not a whole lot available. (male, 5 years of experience)
Discussion
Rural primary care providers play a critical role in improving CRC screening and reduce disparities between urban and rural communities. However, they encounter many challenges, which have not been effectively improved thus far17-21,30,31. This study added evidence about the role of a new healthcare delivery model, the ACO, in the improvement of CRC screening rates from a rural provider point of view. Consistent with findings from previous studies32-35, the present study's findings suggest that the ACO-affiliated primary care clinics could improve CRC screening by utilizing fully functioning EHR systems, including computer-aided reminders, electronic messaging, receiving timely feedback, and generating data for quality improvement projects. However, there were great variabilities between clinics in degree of capacity and advanced use of the EHR system due to the variations of health IT system support. Future interventions need to consider the different levels of EHR system capacities of each clinic.
In addition, ACO based rural primary care providers perceived that CRC screening rates could be enhanced by 'information sharing and collaborative learning' within the ACO network. The term 'learning collaborative' is derived from the quality improvement literature, meaning that multidisciplinary teams from various organizations or units come together regularly to learn about methods to improve their provision of care36,37. For example, healthcare team members from different units, departments, or practices can meet regularly to learn new quality improvement methods, share information, and generate innovative ideas. Facilitators or content experts could be included as additional features to guide the implementation and change process and to help create collaborative environments through periodic instructions. The theoretical rationale is that health teams, which typically hold ideas or information internally and are slow to innovate, are likely to be more effective in generating ideas or implementing change when working together with other teams than when working alone.
Learning collaboratives have been used as an effective tool to disseminate medical and healthcare innovations through enhanced strategies for learning and change38. In a previous study, learning collaboratives were used as a part of interventions to increase CRC screening36. Physicians and other representatives from each practice attended in the 2-day learning collaborative session to learn and discuss effective modalities of CRC screening, general cancer screening and cancer survivorship, and organizational change. The present study's qualitative findings revealed that the learning collaborative model is particularly effective for a primary care ACO in a rural setting, where resources and access for networking opportunities are often limited. Participants seemed highly satisfied with their bimonthly and quarterly ACO meetings, where they could learn and share quality improvement ideas, including CRC screening (eg patient reminder strategies, system set-up know-how, and process analysis tips). However, empirical evidence about the use of a learning collaborative in the promotion of CRC screenings is very limited38. Future research can further examine the scope and impacts of collaborative learning on the promotion of CRC screening in rural primary ACO settings.
Another mechanism by which ACO assisted rural providers to increase CRC screening rates is to hold rural providers accountable through mandatory reporting. ACO-based providers are mandated to report 33 quality measures in five domains: patient and caregiver experience, care coordination, patient safety, preventive health care and at-risk populations. CRC screening is one of the required quality measures to report. In the process of integrating and calculating clinical data for reporting purposes, rural providers can do some self-assessment by comparing their current quality scores to those in ACO benchmarks, other clinics within their ACO network, or other individual providers within their clinics. This process may increase rural providers' intrinsic and extrinsic motivation to improve their quality score in CRC screenings. This data-driven, provider-oriented assessment and feedback approach has been supported by previous literature as the evidence-based interventions for increasing CRC screening rates, although previous studies have focused on less invasive techniques (eg fecal occult blood test)39,40. For developing future intervention, one should consider data accuracy and completeness, advanced methodology for longitudinal comparison, and education/training of providers in data management and analysis.
The team-based care approach was perceived as an effective strategy to promote CRC screening41-46. The present study's findings showed that ACO-based primary care practices were more likely to use the multidisciplinary team to perform CRC screening. For instance, a common strategy for a team-based approach is to empower non-physician delegates (eg behavioral educator, nurse coordinator, or data person) to educate patients, track overdue appointments, facilitate test ordering, and manage patient records. It was also found that limited financial (eg lack of funding to hire new personnel) and system support (eg lack of human resources in rural areas) might hinder team-based strategy from being fully effective in rural settings47. Future intervention should be designed in a way that will overcome those barriers.
Study strengths and limitations
By examining healthcare professionals' perspectives, this study helps understanding of the real-world mechanisms to promote CRC screening in the new US delivery system of healthcare reform. Despite the suboptimal level of screening rates nationally and in rural areas, research is lacking on uncovering effective, data-driven, but financially feasible intervention ideas for improving CRC screening in rural primary care settings. Rather than creating a whole new multilevel intervention, care providers and managers could start identifying and understanding what contributes to successful CRC screening interventions that fit well in their current practice setting (ACO or non-ACO primary care setting).
This study has some limitations. First, sample size (n=21) is small. However, the qualitative nature of the study provides rich information about health professionals' views about opportunities and challenges in promoting CRC screening. Second, the study findings have limited generalizability because the study participants are from primary care clinics in rural Nebraska, a Midwestern state in the USA. Nevertheless, the study findings can be useful for rural primary care practitioners who are already a member of an ACO or who are considering adopting this new alternative delivery system. Third, the study lacks the patient view on mechanisms to improve CRC screening, such as increasing awareness or education, removing cost and transportation barriers, and changing fatalistic cultures in rural areas. Despite these limitations, the findings of this study could inform efforts to promote CRC screenings among rural primary care ACOs.
Based on in-depth interviews with 21 healthcare professionals, this study identified themes that may be useful for existing and planned ACOs for promoting CRC screening in rural areas. Features of ACOs, such as meaningful use of EHR, performance reporting with feedback, aligned provider network, and a team-based care coordination, were perceived to be opportunities for promoting CRC screenings in rural areas. The findings may help ACO or non-ACO based primary care practices design and implement effective, data-driven, but financially feasible interventions using real-world evidence to promote CRC screening.
Acknowledgement
We would like to express our deepest appreciations to all the members and leadership team of the South-Eastern Rural Physician Alliance - Accountable Care Organization (SERPA-ACO) for their generous support for data collection and recruitment for the study.
References
1. American Cancer Society. Cancer facts and figures 2015. Atlanta: American Cancer Society, 2015.
2. Whitlock EP, Lin JS, Liles E, Beil TL, Fu R. Screening for colorectal cancer: a targeted, updated systematic review for the U.S. Preventive Services Task Force. Annals of Internal Medicine 2008; 149(9): 638-658. https://doi.org/10.7326/0003-4819-149-9-200811040-00245
3. He J, Efron JE. Screening for colorectal cancer. Advances in Surgery 2011; 45: 31-44. https://doi.org/10.1016/j.yasu.2011.03.006
4. Meester RG, Doubeni CA, Zauber AG, Goede SL, Levin TR, Corley DA, et al. Public health impact of achieving 80% colorectal cancer screening rates in the United States by 2018. Cancer 2015; 121(13): 2281-2285. https://doi.org/10.1002/cncr.29336
5. Levin B, Lieberman DA, McFarland B, Smith RA, Brooks D, Andrews KS, et al. Screening and surveillance for the early detection of colorectal cancer and adenomatous polyps, 2008: a joint guideline from the American Cancer Society, the US Multi-Society Task Force on Colorectal Cancer, and the American College of Radiology. CA: a Cancer Journal for Clinicians 2008; 58(3): 130-160. https://doi.org/10.3322/ca.2007.0018
6. Smith RA, Cokkinides V, Brawley OW. Cancer screening in the United States, 2012: a review of current American Cancer Society guidelines and current issues in cancer screening. CA: a Cancer Journal for Clinicians 2012; 62(2): 129-142. https://doi.org/10.3322/caac.20143
7. Centers for Disease Control and Prevention (CDC). Vital signs: colorectal cancer screening test use - United States, 2012. Morbidity and Mortality Weekly Report 2013; 62(44): 881-888. https://doi.org/10.3322/caac.20143
8. Cole AM, Jackson JE, Doescher M. Urban-rural disparities in colorectal cancer screening: cross-sectional analysis of 1998-2005 data from the Centers for Disease Control's Behavioral Risk Factor Surveillance Study. Cancer Medicine 2012; 1(3): 350-356. https://doi.org/10.1002/cam4.40
9. Fan L, Mohile S, Zhang N, Fiscella K, Noyes K. Self-reported cancer screening among elderly Medicare beneficiaries: a rural-urban comparison. Journal of Rural Health 2012; 28(3): 312-319. https://doi.org/10.1111/j.1748-0361.2012.00405.x
10. Hughes AG, Watanabe-Galloway S, Schnell P, Soliman AS. Rural-urban differences in colorectal cancer screening barriers in Nebraska. Journal of Community Health 2015; 40(6): 1065-1074. https://doi.org/10.1007/s10900-015-0032-2
11. Ojinnaka CO, Choi Y, Kum HC, Bolin JN. Predictors of colorectal cancer screening: does rurality play a role? Journal of Rural Health 2015; 31(3): 254-268. https://doi.org/10.1111/jrh.12104
12. Greiner KA, Engelman KK, Hall MA, Ellerbeck EF. Barriers to colorectal cancer screening in rural primary care. Preventive Medicine 2004; 38(3): 269-275. https://doi.org/10.1016/j.ypmed.2003.11.001
13. Jilcott Pitts SB, Lea CS, May CL, Stowe C, Hamill DJ, Walker KT, et al. 'Fault-line of an earthquake': a qualitative examination of barriers and facilitators to colorectal cancer screening in rural, Eastern North Carolina. Journal of Rural Health 2013; 29(1): 78-87. https://doi.org/10.1111/j.1748-0361.2012.00424.x
14. Atassi K, Nemeth L, Edlund B, Mueller M, Tessaro I. Adapting the PPRNet TRIP QI Model to increase colorectal cancer screening in primary care. Journal of Cancer Therapy 2012; 3(6A): 866-873. https://doi.org/10.4236/jct.2012.326111
15. Coughlin SS, Thompson T. Physician recommendation for colorectal cancer screening by race, ethnicity, and health insurance status among men and women in the United States, 2000. Health Promotion Practice 2005; 6(4): 369-378. https://doi.org/10.1177/1524839905278742
16. Coughlin SS, Costanza ME, Fernandez ME, Glanz K, Lee JW, Smith SA, et al. CDC-funded intervention research aimed at promoting colorectal cancer screening in communities. Cancer 2006; 107(5 Suppl): 1196-1204. https://doi.org/10.1002/cncr.22017
17. Shell R, Tudiver F. Barriers to cancer screening by rural Appalachian primary care providers. Journal of Rural Health 2004; 20(4): 368-373. https://doi.org/10.1111/j.1748-0361.2004.tb00051.x
18. Hatcher J, Dignan MB, Schoenberg N. How do rural health care providers and patients view barriers to colorectal cancer screening? Insights from Appalachian Kentucky. Nursing Clinics of North America 2011; 46(2): 181-192, vi. https://doi.org/10.1016/j.cnur.2011.02.001
19. Ellerbeck EF, Engelman KK, Gladden J, Mosier MC, Raju GS, Ahluwalia JS. Direct observation of counseling on colorectal cancer in rural primary care practices. Journal of General Internal Medicine 2001; 16(10): 697-700.
20. Rosenwasser LA, McCall-Hosenfeld JS, Weisman CS, Hillemeier MM, Perry AN, Chuang CH. Barriers to colorectal cancer screening among women in rural central Pennsylvania: primary care physicians' perspective. Rural Remote Health (Internet) 2013; 13(4): 2504. Available: www.rrh.org.au (Accessed 5 August 2016).
21. Sarfaty M. How to increase colorectal cancer screening rates in practice: a primary care clinician's evidence-based toolbox and guide. Atlanta: American Cancer Society, National Colorectal Cancer Roundtable and Thomas Jefferson University, 2008.
22. Helfgott AW. The patient-centered medical home and accountable care organizations: an overview. Current Opinion Obstetrics Gynecology 2012; 24(6): 458-464. https://doi.org/10.1097/GCO.0b013e32835998ae
23. Meyers D, Peikes D, Genevro J, Peterson G, Taylor EF, Lake T, et al. The roles of patient-centered medical homes and accountable care organizations in coordinating patient care. Rockville, MD: Agency for Healthcare Research and Quality, 2010.
24. O'Hara S. The care transformation alphabet: what's the difference between CI, ACO, and PCMH? (Internet) 2014. Available: https://www.advisory.com/research/care-transformation-center/care-transformation-center-blog/2014/09/deciphering-the-reform-alphabet (Accessed 5 August 2016).
25. Rundall TG, Wu FM, Lewis VA, Schoenherr KE, Shortell SM. Contributions of relational coordination to care management in accountable care organizations: views of managerial and clinical leaders. Health Care Management Review 2016; 41(2): 88-100. https://doi.org/10.1097/HMR.0000000000000064
26. Creswell JW. Qualitative inquiry and research design: choosing among five approaches. Thousand Oaks, CA: Sage, 2012.
27. Rappleye E. 20 Medicare ACOs with the highest quality scores in 2014. Becker's Hospital Review. (Internet) 2015. Available: http://www.beckershospitalreview.com/accountable-care-organizations/20-medicare-acos-with-the-highest-quality-scores-in-2014.html (Accessed 18 May 2016).
28. Tong A, Sainsbury P, Craig J. Consolidated criteria for reporting qualitative research (COREQ): a 32-item checklist for interviews and focus groups. International Journal for Quality in Health Care. 2007; 19(6): 349-357. https://doi.org/10.1093/intqhc/mzm042
29. United States Department of Agriculture Economic Research Service. Rural classifications. (Internet) 2013. Available: http://www.ers.usda.gov/topics/rural-economy-population/rural-classifications.aspx. (Accessed 24 April 2016).
30. Levy BT, Dawson J, Hartz AJ, James PA. Colorectal cancer testing among patients cared for by Iowa family physicians. American Journal of Preventive Medicine 2006; 31(3): 193-201. https://doi.org/10.1016/j.amepre.2006.04.008
31. Levy BT, Nordin T, Sinift S, Rosenbaum M, James PA. Why hasn't this patient been screened for colon cancer? An Iowa Research Network study. Journal of the American Board of Family Medicine 2007; 20(5): 458-468. https://doi.org/10.3122/jabfm.2007.05.070058
32. Klabunde CN, Lanier D, Breslau ES, Zapka JG, Fletcher RH, Ransohoff DF, et al. Improving colorectal cancer screening in primary care practice: innovative strategies and future directions. Journal of General Internal Medicine 2007; 22(8): 1195-1205. https://doi.org/10.1007/s11606-007-0231-3
33. Nease DE, Jr, Ruffin MT, 4th, Klinkman MS, Jimbo M, Braun TM, Underwood JM. Impact of a generalizable reminder system on colorectal cancer screening in diverse primary care practices: a report from the prompting and reminding at encounters for prevention project. Medical Care 2008; 46(9 Suppl 1): S68-S73. https://doi.org/10.1097/MLR.0b013e31817c60d7
34. Stone EG, Morton SC, Hulscher ME, Maglione MA, Roth EA, Grimshaw JM, et al. Interventions that increase use of adult immunization and cancer screening services: a meta-analysis. Annals of Internal Medicine 2002; 136(9): 641-651. https://doi.org/10.7326/0003-4819-136-9-200205070-00006
35. Wilkinson C, Champion JD, Sabharwal K. Promoting preventive health screening through the use of a clinical reminder tool: an accountable care organization quality improvement initiative. Journal for Healthcare Quality 2013; 35(5): 7-19. https://doi.org/10.1111/jhq.12024
36. Shaw EK, Ohman-Strickland PA, Piasecki A, Hudson SV, Ferrante JM, McDaniel RR, Jr, et al. Effects of facilitated team meetings and learning collaboratives on colorectal cancer screening rates in primary care practices: a cluster randomized trial. Annals of Family Medicine 2013; 11(3): 220-228, S1-S8.
37. Nadeem E, Olin SS, Hill LC, Hoagwood KE, Horwitz SM. Understanding the components of quality improvement collaboratives: a systematic literature review. Milbank Quarterly 2013; 91(2): 354-394. https://doi.org/10.1111/milq.12016
38. Shaw EK, Chase SM, Howard J, Nutting PA, Crabtree BF. More black box to explore: how quality improvement collaboratives shape practice change. Journal of the American Board of Family Medicine 2012; 25(2): 149-157. https://doi.org/10.3122/jabfm.2012.02.110090
39. Sabatino SA, Lawrence B, Elder R, Mercer SL, Wilson KM, DeVinney B, et al. Effectiveness of interventions to increase screening for breast, cervical, and colorectal cancers: nine updated systematic reviews for the guide to community preventive services. American Journal of Preventive Medicine 2012; 43(1): 97-118. https://doi.org/10.1016/j.amepre.2012.04.009
40. Curry WJ, Lengerich EJ, Kluhsman BC, Graybill MA, Liao JZ, Schaefer EW, et al. Academic detailing to increase colorectal cancer screening by primary care practices in Appalachian Pennsylvania. BMC Health Services Research 11: 112. https://doi.org/10.1186/1472-6963-11-112
41. Shaw EK, Ohman-Strickland PA, Piasecki A, Hudson SV, Ferrante JM, McDaniel RR, Jr, et al. Effects of facilitated team meetings and learning collaboratives on colorectal cancer screening rates in primary care practices: a cluster randomized trial. Annals of Family Medicine 2013; 11(3): 220-8, S1-S8.
42. Kiran T, Kopp A, Moineddin R, Glazier RH. Longitudinal evaluation of physician payment reform and team-based care for chronic disease management and prevention. Canadian Medical Association Journal 2015; 187(17): E494-502. https://doi.org/10.1503/cmaj.150579
43. Klabunde CN, Lanier D, Nadel MR, McLeod C, Yuan G, Vernon SW. Colorectal cancer screening by primary care physicians: recommendations and practices, 2006-2007. American Journal of Preventive Medicine 2009; 37(1): 8-16. https://doi.org/10.1016/j.amepre.2009.03.008
44. Hudson SV, Ohman-Strickland P, Cunningham R, Ferrante JM, Hahn K, Crabtree BF. The effects of teamwork and system support on colorectal cancer screening in primary care practices. Cancer Detection and Prevention 2007; 31(5): 417-423. https://doi.org/10.1016/j.cdp.2007.08.004
45. Clouston K, Katz A, Martens PJ, Sisler J, Turner D, Lobchuk M, et al. Does access to a colorectal cancer screening website and/or a nurse-managed telephone help line provided to patients by their family physician increase fecal occult blood test uptake?: A pragmatic cluster randomized controlled trial study protocol. BMC Cancer 12: 182. https://doi.org/10.1186/1471-2407-12-182
46. Dietrich AJ, Tobin JN, Cassells A, Robinson CM, Greene MA, Sox CH, et al. Telephone care management to improve cancer screening among low-income women: a randomized, controlled trial. Annals of Internal Medicine 2006; 144(8): 563-571. https://doi.org/10.7326/0003-4819-144-8-200604180-00006
47. Toliver Z. Rural ACO leaders speak: What have been the biggest challenges and the biggest advantages to creating your ACO? The Rural Monitor. (Internet) 2016. Available: www.ruralhealthinfo.org/rural-monitor/rural-aco-leaders-speak/ (Accessed 1 April 2016).


