Recent studies in developing countries suggest that household resources (eg electricity, toilet facilities, source of drinking water, type of fuel for cooking, roofing and flooring materials) are associated with lower risk of child mortality1-5. In these studies, the economic status of the household was operationalized as having possession of assets such as electricity2 or toilet facilities5 or access to clean drinking water4,5 or sound roofing and finished flooring3; these were found to significantly increase under-age-5 survival. One study that focused on capital cities of East Africa found that mortality was highest among children of mothers residing in households with no toilet facilities compared to those with flush toilets; furthermore, pipe-borne water was associated with lower odds of child mortality compared to well water6.
The role of household assets as predictors of child mortality over and above other measures of socioeconomic status (SES) has not been well studied in developing nations. Most of the studies that investigated the influence of SES on child mortality tended to use the more traditional measures such as education and income7-9. For example, Blakely and colleagues (2003) examined maternal education in relation to child mortality and found that maternal education level is significantly associated with lower odds of child mortality7. However, not all studies10 have found a significant association between maternal education and lower child mortality. Of these studies, few6,9 accounted for both household assets and maternal education with assets showing significant associations with child mortality when education was controlled.
Several Ghanaian studies have suggested that child mortality is higher among women with low SES, for first order births compared with second and third order births and among children who live in rural areas versus urban areas5,8,11-13. However, none of these studies examined child mortality in relation to household resources, although such resources are shown to be important determinants in studies of mortality in other countries1-3. The present study was designed to test associations between household resources and child mortality in Ghana, controlling for maternal education as a measure of SES. Because the child mortality risk is 36% lower for children living in urban areas compared to children in rural areas of Ghana5, urban versus rural residence was tested as a potential effect modifier of associations between household resource possession and child mortality. Findings from this study could be used to inform public health interventions expected to address the indirect causes of child mortality in the general population and within sociodemographic subgroups. For example in 2015, the World Health Organization called on community health workers in low resource settings to conduct assessment of household resources among families with children to guide counseling and education to address the identified needs. Understanding the prevalence and role of specific household resources in child mortality by rurality would support Ghana and similar sub-Saharan African countries to move toward achieving the child mortality targets specified in the Sustainable Development Goals to reduce under-5 mortality to at least as low as 25 per 1000 live births14.
Methods
Setting, design and data source
This cross-sectional descriptive study used a secondary analysis based on data collected from the 2007 Ghana Maternal Health Survey (GMHS), the first and the only maternal health survey conducted in Ghana15. Phase I was a short household questionnaire administered to some 240 000 households which were divided into 1600 clusters to identify deaths to women aged 12-49 years. Phase II of the GMHS survey was fielded in 400 clusters selected randomly from 1600 clusters identified in Phase I, yielding interviews with 10 370 women aged 15-45 years and selected from 10 858 households in both rural and urban areas.
Sample and study variables
For this analysis, women who reported giving birth prior to the interview in the Phase II survey were selected (n=7183).
Child mortality: The dependent variable was measured for each woman included in the survey and was a binary (yes/no) measure of report of any child death before the age of 5 years (hereafter referred to as child mortality).
Household resources: The independent variable was household resources. The GMHS survey included the following 16 household resources items (each measured as a binary yes or no): electricity, radio, refrigerator, toilet facility, clock, pipe or sachet water, television, polished floor, freezer, car or truck, mobile phone, liquefied petroleum gas (LPG) cooker, having one to 3 bedrooms, kerosene lantern, bed and computer. An index representing the total number of resources in the house was created by counting the number of items each woman responded to with 'yes'. The overall household resource index ranged from 0 to 16; a higher score was reflective of more resources.
Consistent with prior work by Godson and Nnamdi3, factor analysis16 was employed to reduce the set of household resources given correlations up to 0.49 between these variables and to eliminate potential problems of multicollinearity. Both oblique and varimax rotations were used for the factor analysis. Also examined was the correlation between each of the obliquely and varimax rotated factors as per the suggestion of Pedhazur and Schmelkin16. However, the result of obliquely rotated factors showed a weak correlation, with effect size less than 0.3 between the factors. Therefore, the authors resolved to stay with the varimax rotated result. To determine the number of factors to be selected, the authors followed prior work by Godson and Nnamdi3 and retained those factors with eigenvalues greater than 1.0. Eigenvalues measure the variance in all the resources accounted for by a given factor, and any factor having eigenvalue greater than or equal to 1.0 explains more variance than any single observed variable16. On food preparation and storage (factor 1), kerosene lantern, computer, refrigerator, LPG cooker, car/truck and freezer loaded highest. On electronics items (factor 2), mobile telephone, bed, clock, radio and flush toilet loaded highest. On water, sanitation and basic amenities (factor 3), natural floor, water pump, electricity, piped or bottled water, and three or more rooms loaded highest. Factor 1 primarily represents items that could affect food preparation and storage. Factor 2 primarily represents ownership of electronics items in the household and factor 3 primarily represents items related to water and sanitation and basic amenities (ie electricity). These three uncorrelated factors were added to a regression model in lieu of the individual household resources.
Covariates included maternal education, region of residence, number of pregnancies and maternal religion. Maternal age was categorized as 'less than 29 years' (reference group), '30-39 years', and 'greater than 39 years'. Maternal education was categorized as 'none' (reference group), 'primary school', 'middle school' and 'secondary school or above'. From Ghana's 10 geographical regions, a four-level categorical variable was developed to categorize region of residence: Western/Central, Ashanti/Eastern, Northern/Brong Ahafo/Upper East/Upper West and Greater Accra/Volta (reference group). These regions were included in the analysis as there is a wide SES gap across these regions in Ghana. Like most countries in Africa, Ghana is a multi-ethnic and multicultural society that consists of a vast mosaic of large and small ethnic groups. The major groups are the Akan, the Mole Dagbani, the Ewe, the Ga Adangbe, the Guan, the Gurma, the Grusi and the Mande-Busanga, which constitute the regions15. There is also collinearity between region of residence and ethnicity; therefore, region was controlled and ethnicity was omitted from the multivariate models. The number of pregnancies each woman had at the time of the interview was categorized as 'one only' (reference group), 'two or three', 'four' and 'five or more'. Maternal religion was categorized as 'Protestant' (reference group) 'Catholic', 'other Christian', 'Moslem', 'traditional', or 'other beliefs'.
Statistical analysis
Data were analyzed using STATA v13 (StataCorp; http://www.stata.com). Descriptive statistics was used to summarize the means of continuous variables and proportions of categorical variables and to cross-tabulate each variable, including the household resources by child mortality in the full sample. Means were compared statistically with t-tests, and proportions were tested using χ2 analysis. Logistic regression analysis was used to examine the association between the household resources - modeled first as factors and second as counts - and child mortality, controlling for the covariates. In all models, effect modification by urban versus rural residence was tested with partial F-tests, and, if significant, stratified models were reported. In all of the analyses, survey weights were applied to adjust the standard errors for the complex survey design. In exploratory analysis, each household's resources were examined using a regression model.
Ethics approval
This study was approved by the University of California, Davis Institutional Review Board (approval number 613626-1).
Results
Table 1 compares the health and demographic characteristics of the study sample by child mortality. Most of the variables differed significantly between the groups. Specifically, the results show that women were more likely to report child mortality if they were older, had no education, lived in the Northern/Brong Ahafo/Upper East/Upper West region, had traditional or other religious beliefs, lived in rural areas, or had five or more pregnancies. With respect to the overall household resource index, women in the highest quartile, with most household resources, reported child mortality with less frequency. Results from the multivariate regression model, which assessed the relationship between household resources and child mortality, are presented in Table 2. The overall household resources count was significantly associated with child mortality in analyses for the entire sample (adjusted odds ratio (AOR)=0.95; 95% confidence interval (CI): 0.92, 0.98). Analyses stratified by place of residence showed the household resources count was significantly associated with the death of one or more child in both rural (AOR 0.98; 95%CI: 0.92, 0.98; p<0.01) and urban (AOR 0.97; 95%CI: 0.90, 1.36; p< 0.01) residences.
With respect to the three household resource domains created using factor analysis (Table 2), factor 1, which represented items for food preparation and storage, was significantly associated with child mortality in analyses including the entire sample. Households that reported more factor 1 resources had a lower odds of child mortality (AOR=0.86; 95%CI: 0.78, 0.94) than households that reported fewer. In stratified analyses, factor 1 was significantly associated with lower odds of child mortality in urban areas (AOR=0.82; 95%CI: 0.73, 0.93), but only marginally in rural areas (AOR=0.92; 95%CI: 0.78, 1.09). Household resource factor 2, which represented electronic items (AOR=0.95; 95%CI: 0.88, 1.02), and factor 3, which represented shared water and sanitation items (AOR=0.96; 95%CI: 0.90, 1.02), were only marginally associated with child mortality in the entire sample. In stratified analyses, factor 2 and factor 3 were marginally associated with a lower odds of child mortality in urban area, but in rural areas neither were associated with the odds of child mortality.
Results from the exploratory analysis assessing the relationship between each of the household resources and child mortality are in tables 3 and 4. In unadjusted regression analyses, women who reported possession of each of the household resources were less likely to report child mortality. The one exception was the number of sleeping rooms, for which there was no significant difference in the proportion of women reporting child mortality. Results from the multivariate regression model of child mortality, including each of the household resources as separate variables, showed that none of the household resources were statistically significant except a refrigerator. Specifically, women who reported having a refrigerator had lower odds of reporting child mortality (AOR=0.67; 95%CI: 0.54, 0.84).
In the model restricted to women living in rural areas, none of the household resources were associated with child mortality. In contrast, in the model restricted to women who lived in urban areas, having a refrigerator at the time of interview was associated with lower odds of reporting child mortality (AOR=0.63; 95%CI: 0.48, 0.83). Those who had a kerosene lantern (AOR=1.40; 95%CI: 1.06, 1.85) or flush toilet (AOR=1.84; 95%CI: 1.23, 2.75) were associated with higher odds of reporting child mortality. In both stratified models, the significance of covariates associated with child mortality was similar to the pooled (urban + rural residence) model, with two exceptions. First, in the rural model, residence in the Ashanti/Eastern, Western/Central, Northern/Brong Ahafo/Upper East/Upper West regions was associated with higher child mortality compared to the Greater Accra/Volta region; in the urban/town model, only residence in the Ashanti/Eastern region was significantly associated with higher child mortality. Second, primary school and middle school education compared to no education was associated with lower child morality in the rural model; only secondary school education relative to no education was associated with lower child mortality in the model restricted to women living in urban areas and towns.
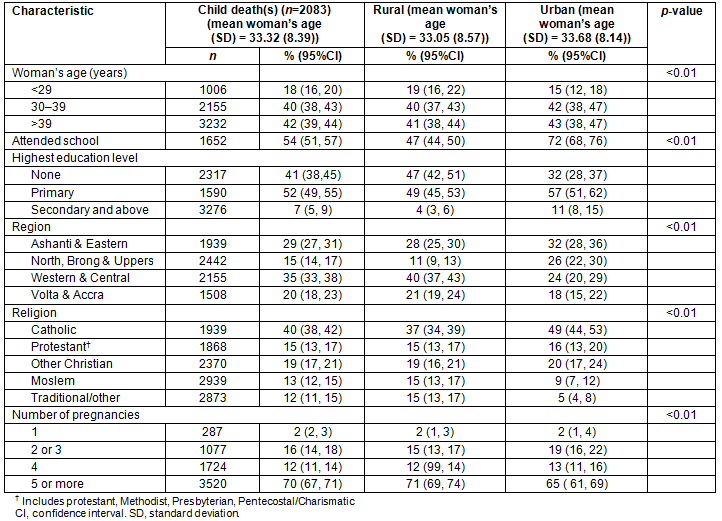
Table 2: Odds ratios for child mortality by place of residence?
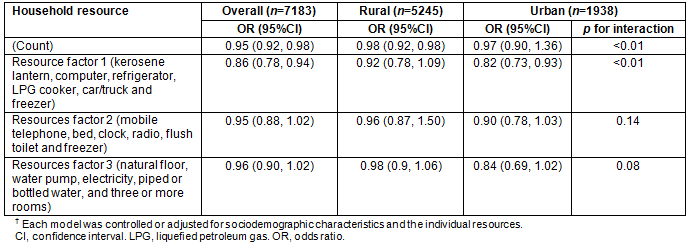
Table 3: Household resources among Ghanaian women by residence (n=7183)
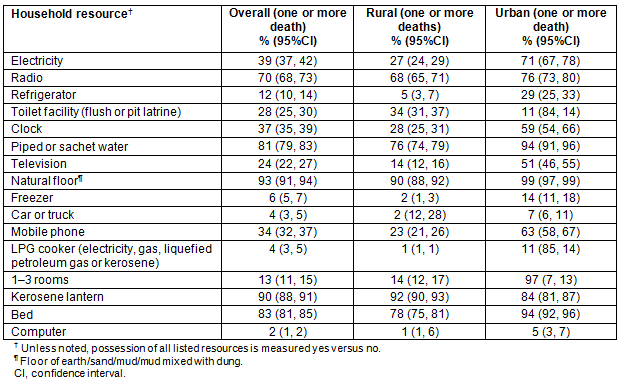
Table 4: Logistic regression of household resources among Ghanaian women by residence (n=7183)
Discussion
To the authors' knowledge, this is the first study to simultaneously examine associations of household resources and socioeconomic factors with child mortality in Ghana. It was found out that 29% of the parous Ghanaian women who were surveyed reported at least one child death. Because the measure of child mortality included maternal reports of any child death under age 5 years within the 5 years preceding the survey, the rate reported here is much higher than typical annual reports of child mortality in Ghana; In 2010, WHO reported 72 deaths per 1000 live births14. Despite this difference, the findings provide a community-based snapshot of factors associated with child mortality in Ghana.
Prior work has demonstrated that household resources significantly contribute to the survival of a child17. This study has added to the previous work by simultaneously examining the contribution of household resources and maternal education (as a measure of socioeconomic status) to childhood mortality in both rural and urban areas of Ghana. In unadjusted analysis, each of the household resources examined was associated with lower odds of reporting child mortality. However, in the adjusted regression, only possession of a refrigerator was significant. Prior studies have considered the contribution of possession of household resources to child mortality; however, to the authors' knowledge none have specifically evaluated possession of a refrigerator.
The association of possessing a refrigerator with lower child mortality has at least three possible explanations. First, in Ghana, buying a refrigerator is an expensive purchase, and only the most affluent members of society can afford such a purchase. Therefore, possession of a refrigerator could reflect unmeasured socioeconomic status in terms of wealth or income; furthermore, the present study's findings are consistent with prior work finding that higher socioeconomic status is associated with lower child mortality4,13. Second, Ghana is located in the tropics, and refrigeration is recommended to maintain the potency and efficacy of many syrups, mixtures, and suspensions given to treat common childhood conditions including malaria, diarrhea and infections18.
Third, access to a refrigerator minimizes contamination of food and drinks from bacteria and other disease-causing organisms, particularly in the tropics, and households with a refrigerator have the means to preserve food and drink and prevent such contamination. This pathway is consistent with findings of a review that found the major cause of diarrheal diseases and malnutrition in children leading to child mortality to be contamination of their foods with pathogens19.
Studies conducted in sub-Saharan African countries have found lower mortality rates among children who live in households with toilets attached to the dwelling5,9,20. Similarly, Kabubo-Mariara, et al. in their study in Kenya found that having a toilet facility in the residence reduces the risk of mortality by 48%; moreover, having a flush toilet reduces the risk of child mortality by 25% more relative to latrines4. In contrast, in a study conducted in rural India, Chakrabarti found that SES of a household, discussed in terms of possession of certain assets such as toilet facilities, has no significant impact on morbidity leading to child mortality in children10. The present study's results show that having a flush toilet or pit latrine compared to having no toilet facility is associated with higher odds of reporting child mortality in the urban/town analysis; however, this association was not significant in the rural subgroup. The lack of significant association in the rural areas is consistent with the findings of Chakrabarti conducted in rural India. In the models restricted to respondents in rural areas, toilet facility was not associated with child mortality. This may be due to insufficient heterogeneity in the type of toilet facilities in these areas; also, similar to Chakrabarti's findings in rural India, most rural households in Ghana do not have a toilet facility. The association of higher child mortality associated with the present study's measure of toilet facility may be due to most of those preferring this measure having pit latrines and far fewer having flush toilets. Dashtseren12 and Rutaremwa6 found that having a flush toilet, used as a measure of affluence, was associated with lower child mortality.
In rural areas, possession of a kerosene lantern was associated with higher child mortality. This finding could reflect mechanisms for child mortality associated with low SES. In Ghana, those most likely to report possession of a kerosene lantern are of low SES and unable to afford electricity connection fees or monthly bills or they reside in rural areas without access to electricity. This result is consistent with results reported in Kyei's South African study where socioeconomic variables of a household were found to be important determinants of child mortality9. Other studies have reported that child mortality is higher among households that do not use electricity1. It was hypothesized that households with more than three rooms for sleeping would report higher rates of child mortality because, in Ghana, poorer people live in compound houses, which provide more rooms for sleeping. However, consistent with Blakely, et al.7, no association was found between the number of sleeping rooms and child mortality. The relationship between household resources and child mortality has been demonstrated in a number of studies in other parts of the world. For instance in two separate studies, Andoh, et al21 and Blakely, et al7 conducted in Cote d'Ivoire and New Zealand, respectively, the authors argued that the root cause of child mortality is the uneven distribution or lack of household resources. Households that experienced lower child mortality rates were found to use low polluting fuels as their main sources of cooking3,22, have access to electricity1,3 and have a car7. None of these variables, however, were significant in the present study's models. The differences in the present study's findings compared to prior work may be explained by inconsistent use of measures to control for potential confounding by SES across the studies.
It is well established that the socioeconomic conditions of the population, whether measured at the individual, household, or community level, are major determinants of childhood mortality in developing countries. Several studies12,20,22 have described the relationship between child mortality and SES in sub-Saharan Africa. These studies have concluded that child mortality rates in sub-Saharan African countries have been high due to the lower SES of most women12,21,23.
Consistent with other work worldwide, the present study found maternal education to be inversely associated with child mortality in a dose-response relationship. Maternal education has been identified as one of the most important socioeconomic determinants of child mortality with decreasing mortality as maternal educational level increases5,7-9. Maternal education and place of residence show positive relationships with use of prenatal care, place of delivery (either hospital or home), breastfeeding and receipt of recommended childhood vaccinations8,10. The current study also found that primary and middle school education was associated with lower child morality compared to no education for women in rural areas, whereas only secondary school education relative to no education was associated with lower child mortality among women living in urban areas and towns. This difference may be explained by universally low levels of educational attainment among women in rural areas in contrast to the variation in the educational status of women in the urban areas and towns5,8. Efforts to promote opportunities for education among Ghanaian girls, particularly in rural areas, could yield improvements in household socioeconomic conditions as well as childhood mortality rates.
Similar to the findings of Andoh, et al21, the present study found that number of prior pregnancies and advanced maternal age were associated with child mortality. This finding supports efforts currently under way to improve access to family planning and reproductive services in Ghana and other sub-Sahara African countries. Some sub-Saharan African countries such as Burkina Faso, Cote d'Ivoire, Ethiopia, Nigeria, Uganda and Zambia are currently implementing these measures to improve family planning and reproductive services24.
These results have suggested higher child mortality rates in rural compared to urban areas in Ghana as well as differences in some predictors of child mortality by urban and rural areas. Similarly, others have reported higher child mortality rates in rural areas5,8,21. Most rural dwellers are poor and possess the same types of household resources due to their similar SES5. This lack of variability in household resources could explain why these factors were largely not significant in the present study's models. Income inequality is greater in urban areas of Ghana, with some extremely rich and extremely poor households, while the majority of households are middle class. Similar inequality is apparent between regions in Ghana; for example, it was found that residents of Greater Accra/Volta, Ashanti/Eastern and Western/Central had relatively higher incomes than residents of the Northern/Brong Ahafo/Upper East/Upper West region. Not surprisingly, these lower income regions also had higher child mortality. Gyimah reported that the higher income regions in Ghana also tended to include more urban areas, while the lower income regions included more rural areas5. The findings associated with the measures of region may reflect unmeasured SES as well as regional policies and access to resources.
Study strengths and limitations
The 2007 GMHS reflects the most recently available data describing child and maternal health-related issues pertaining to pregnancies, live births, abortions, miscarriages and related health services use in Ghana. As such, it is an important resource for studies of child mortality. A decade later, these data may not reflect the current environment in Ghana because there have been significant changes in maternal and child health access and policies. Child mortality rates in Ghana have seen consistent decline since 1990 (119 deaths per 1000 live births) to 60 deaths per 1000 live births in 201425. At the same time, socioeconomic conditions have improved; however, this improvement has lagged in rural areas relative to urban areas25. These temporal changes underscore the importance of the present study's findings regarding rural resources and child mortality. As in any secondary analysis, these results may be due to unmeasured confounding. For example, important variables to measure community attributes such as wealth or income were omitted. Future studies that include these variables would make an important contribution to the understanding of child mortality in Ghana.
Households were asked to report events as far back as 5 years before the Phase II GMHS, raising the question of recall bias (where respondents are unable to remember). It is likely that respondents would be able to remember a child's date of birth or the age of a child at death26. However, other variables such as the conditions leading to child death may be subject to recall bias or misclassification. Ideally, such errors occur randomly across households and are not related to any of the independent variables26. As respondents reported possession of household resources at the time of the survey, there is also the possibility of temporal mismatch of the reported resources and child mortality.
Conclusions
Using the 2007 GMHS, the association between child mortality and household resources in Ghana were examined. In an unadjusted analysis, each of the household resources examined was associated with child mortality. However, in the adjusted regression, only possession of a refrigerator was significant. Other covariates, such as maternal education, maternal age, place of residence and number of pregnancies, at the time of the survey were all found to be significantly associated with child mortality. Women who had no or only primary education, were of advanced age, resided in a rural area, or had multiple pregnancies reported higher child mortality. Further studies should focus on understanding the association of household resources and child mortality in rural areas and the contribution of these community socioeconomic attributes to child mortality.
References
