Introduction
Rabies is one cause of lethal acute encephalitis of viral etiology. The causal virus can be found in saliva and nerve cells1. Transmission of the virus is usually through a bite but it also can occur by exposure to a scratch, abrasion, open wound or mucous membrane, saliva or brain material from rabid animal source/origin. Organ transplant is an exceptionally rare type of transmission. The virus has an extremely high and selective affinity for the central nervous system tissue and moves to the brain along the peripheral nerves. Once the virus is established in brain, the disease is irreversible and fatal. The average incubation period varies from 20 to 90 days after exposure and depends on the following:
- the severity of the bite or laceration
- the location of the bite (incubation periods may be shorter after bites on the head, neck, and fingertips, than bites on the trunk or lower extremities due to the extensive nerve endings in the former areas)
- the age of the victim (children have a faster onset)2.
Two clinical patterns may be manifest and are referred to as 'dumb' or paralytic rabies and furious rabies (prone to bite). The onset of rabies in less then one week is the clearest sign of the deadly evolution of the case. The patient is, theoretically, contagious and very strict isolation is required. The irreversible evolution to death explains why compulsory preventative strategy is prescribed and followed if someone is exposed to a probable rabid animals' aggression.
Our main goal in this study was to assess the burden of exposure to rabies risk factors in the rural population from Cluj County, Romania. We were motivated to start this study because:
- rabies is a fatal disease
- the risk for rabies is still present
- the virus has a large natural reservoir, mostly in wild, but also in domestic, animals.
Methods
The research protocol was initially reviewed and approved by the Cluj-Napoca University of Medicine and Pharmacy Ethics Committee and conducted in accordance with the ethical guidelines legal in Romania.
Case definition
We considered as cases all patients who met the following time/ space/person criteria:
- rural residents of Cluj County
- exposure to wild or domestic animals, with or without a known history of rabies
- exposure that had taken place between April 1998 and December 2004.
Data collection
The source of data regarding the rabies cases in animals was the Cluj County Veterinarian Public Health Department. We collected data on patients from the registry of Vaccination Centre of the Infectious Diseases Teaching Hospital in Cluj-Napoca, with strict confidentiality regarding the patient. The data were entered into an Access 2000 database and were analyzed using Epi Info 3.3.2. The collection variables were as follows:
- age
- gender
- aggressor animals
- exposure date
- contact type (bite or scratch)
- date of contact
- date of starting prophylaxis
- type of prophylaxis (vaccine or specific serum immunoglobulin prophylaxis)
- compliance with prophylactic measures
Statistical analysis
We used Epi Info 3.3.2 to perform the statistical analysis. Odds ratios (OR) and 95% confidence intervals (CI) between men and women were calculated on the crude data.
Results
The natural reservoir of the rabies virus in the Cluj County geographical area was mostly identified in wild animals: 77% (n = 38) in comparison with 23% (n = 11) in domestic species. The species diagnosed with rabies are shown (Table 1).
Table 1: Species diagnosed with rabies between 1998 and 2004 in Cluj County, Romania
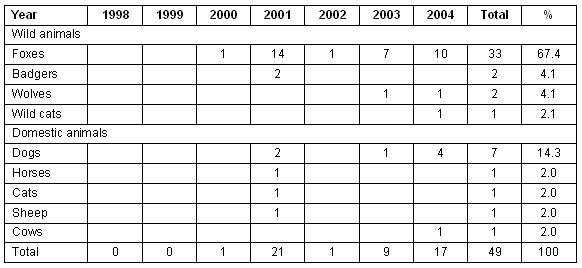
The total population of Cluj County (based on the 2002 General Population and Housing Census) was 702 755 persons, 51.55% female (n = 362,238) and 48.45% male (n = 340 517)3.
The total population living in rural areas of Cluj County was 230 133 (32.8% of the total population). The distribution by sex in this rural population was 50.3% females (n = 115 769) and 49.7% males (n = 114 364).
During the period 1998-2004, 6 cases of human rabies were been diagnosed in Romania (3 cases in 2000, 3 cases in 2002), and none of those cases was in the population of Cluj County.
The demographic characteristics of the exposed rural population studied were an average age of 34 years and a standard deviation of 23.8 years. The youngest person was 6 months old and the oldest person was 87 years, with a median of 30.5 years and a mode of 8 years.
We compared data collected from our patients with data from the population census (Table 2).
Table 2: Age distribution of the population studied and population of Cluj, Romania
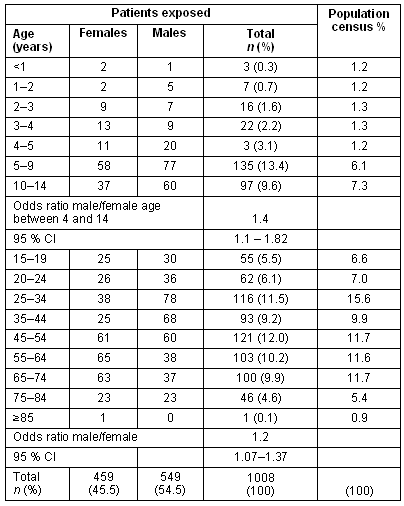
We identified the group at the highest risk of rabies exposure as the group of boys at the ages between 4 and 14 years (Fig 1).
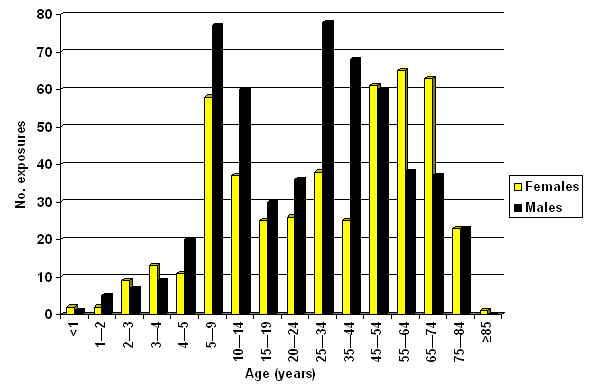
Figure 1: Distribution of exposed individuals by age group and gender.
We found that pets and farm animals were involved in most of the cases of aggression; 91.4% (n = 921) were domestic animals, 7.4% wild animals (n = 75) and 1.2% (n = 12) unidentified animals.
Most of the patients were bitten by the animals 95.4% (n = 962) and only 46 patients were scratched, the animal saliva coming in contact with a fresh scratch on the patient's skin.
From the total number of patients (n = 724), 89.7% (n = 651) were supposed to receive rabies-specific prophylaxis and came to see a doctor in 6 days or less from the day of the aggression. The remainder presented to a doctor in less than one month from the exposure.
None of the patients had pre-exposure prophylaxis against rabies. The necessity of post-exposure prophylaxis for each patient was evaluated by a specialist physician in infectious diseases or epidemiology. The prescribed schedule of immune prophylaxis followed the recommendation of the national health authorities, accordingly to WHO recommendations4-8. Specific serum immune globulin was indicated in almost 9% (n = 90) of cases. Rabies vaccine was indicated in 72% (n = 726). All patients who were recommended for immune globulin prophylaxis were also recommended for vaccination. Rabies immune prophylaxis, either immune globulin prophylaxis or vaccine, was indicated in 726 cases. Only 28% (n = 283) completed the prophylaxis scheme. For 28% (n = 282) of the patients, none of the prophylactic measures were indicated (Table 3).
Table 3: Completion of prophylaxis scheme
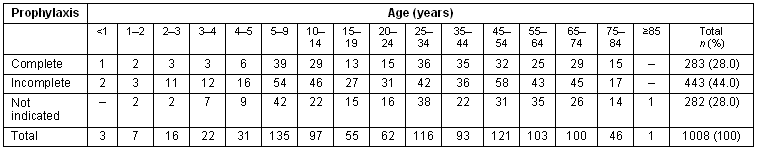
The number of exposures per year remained almost constant (Figure 2).
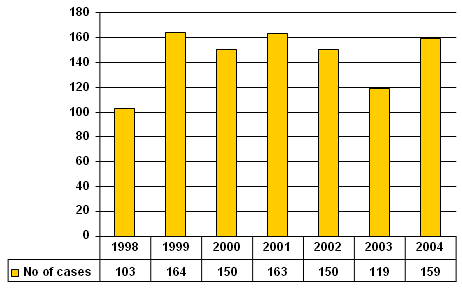
Figure 2: Number of cases (yearly distribution).
Due to the fact that there were no available data for the whole year 1998, the number of exposures counted in that particular year was lowest (n = 103). We did not take into account the number of exposures that occurred in 1998 when we calculated the mean number of exposure per year (mean = 150.8) and the standard deviation (SD = 16.8).
The number of exposures per month constantly increased in the summer and decreased in the winter (November to January, every year but 2001/2002).
Discussion
Rabies is responsible for almost 40 000 deaths per year worldwide9,10. Asia is the continent with the highest number of human deaths due to rabies disease with more than 95% of worldwide cases and approximately 35 000 deaths per year.
The last native case of rabies death in France was in 1924, but between 1970 and 1996, 17 cases were 'imported' into France. Mass vaccination of domestic pets and control of strays is needed11,12. Their close contact with humans introduce risk when rabies immunizations are not kept current. This is especially true in the rural setting where it is not economically feasible to vaccinate livestock13. However, even in an ideal situation, with the right prophylactic measures, rabies cannot always be prevented14.
The main goal of this study was to assess the exposure of the rural population in Cluj County, Romania, to rabies risk factors. We were motivated to conduct the study because of the fatal risk from the disease which is still present in the animal population (the virus has a large reservoir, mostly in wild but also in domestic animals). In addition, we were concerned by the very high number and costly medical care of specific preventative procedures in patients exposed to such animals.
However, we must underline the lack of a formal definition of rurality in Romania; the existing criteria are administrative/geographic, not based on or related to any internationally accepted criteria. This study has demonstrated the burden and dynamic trend of rabies prevention measures in the rural population of Cluj County, in the frame of enzootic persistent potential risk. The presence of the rabies virus in the wild animal population and the relatively close and quite unavoidable contact between wild and domestic animals in rural settings may present a health hazard for the population living in that area.
We identified the highest risk group for rabies exposure as being boys of 4 to 14 years of age. Specific behavioral characteristics of that age group increased the risk of coming into close contact with potentially rabid animals from their environment, while trying to play with them, to catch them or to take care of them.
We found that it was not always possible to identify the animals that came in contact with a given human subject. This also poses a great risk for rabies. 'Domestic' animals were involved in most of the aggressions but a relatively high number of wild animals were responsible for high risk contacts with the rural population15.
We found that it was difficult to assess the number of people who came into contact with possibly sick animals. Compliance for prophylactic measures was relatively low and we assume that a certain number of exposed persons did not even go to a physician. This suggests the importance of specific health education, particularly in the rural population. Rural practitioners may play an important role in educating the public. They must be made aware of this and must also have the appropriate resources to tackle the problem of non-compliance.
In terms of number of aggressions per season, we found that a higher number of exposures took place in spring and at the beginning of summer, and contacts were less likely to occur in the cold season. This may be related to the fact that in spring animals usually give birth to offspring and the mothers are more aggressive with 'intruders'.
A final issue is the cost-benefit of prophylactic treatment for human subjects exposed to rabies. Considering the lethal risk of rabies, counting the individual cost-benefit risk is senseless. The real problem is how to reduce the risk of exposure to infectious contacts with animals whose health status is unknown. This is unsatisfactorily managed in continental countries like Romania. Improved surveillance of the natural reservoir of rabies, vaccination of wild animals and protection of pets and livestock could be a cheaper alternative than immunizing many exposed human subjects. Such surveillance could be managed with the help of veterinarians.
Conclusions
- Similar to data reported in other international papers, our study showed that the risk of being exposed to animal aggression does exist at all ages. Specific behavioral characteristics of boys increases the risk for males between 4 and 14 years of age.
- Foxes represent the main natural reservoir of the rabies virus in the geographical area of Cluj County, among other wild animals.
- Dogs count for most of the incidents.
- Poor access and compliance of patients to medical care may be related to the special conditions in rural areas (larger distances to the nearest medical facility and lack of education).
- The persistence of the rabies virus in this geographic area justifies the recommendation of prophylactic treatment for persons exposed to potentially rabid animals.
- Although the number of positive rabies cases are fewer in domestic animals than in wild animals, dogs, cats and farm animals continue to present a substantial risk to humans.
- There is an obvious need to control the animal reservoir and to educate the public regarding the fatal risk of rabies. Rural practitioners must play a role in educating the public. Adequate resources should be allocated to support this educational effort.
References
1. Rupprecht CE, Hanlon CA, Hemachudha T. Rabies re-examined. Lancet Infectious Diseases 2002; 2: 327-343.
2. Jackson AC, Warrell MJ, Rupprecht CE et al. Management of rabies in humans. Clinical Infectious Diseases 2003; 36: 60-63.
3. National Institute of Statistics, Romania. 2002 General Population and Housing Census. Available: http://www.recensamant.ro/ (Accessed 6 July 2005).
4. WHO. Investing in health research and development: report of the Ad Hoc Committee on Health Research Relating to Future Intervention Options. Geneva: WHO, 1996.
5. WHO. Strategies for the control and elimination of rabies in Asia. Report of a WHO interregional consultation. Geneva: WHO, 2002.
6. WHO. The world health report 2002: reducing risks, promoting healthy life. Geneva: WHO, 2002.
7. WHO. World survey of rabies, no. 32, Year 1996. Geneva: WHO, 1998.
8. WHO. World survey of rabies, no. 27, Year 1991. Geneva: WHO, 1993.
9. Pan American Health Organization. Human rabies in the Americas. Epidemiological Bulletin 1995; 16: 12-13.
10. Taylor LH, Latham SM, Woolhouse MEJ. Risk factors for human disease emergence. Philosophic Transactions Royal Society London, Series B. Biological Science 2001; 356: 983-989.
11. Cleaveland S, Fèvre EM, Kaare M, Coleman PG. Estimating human rabies mortality in the United Republic of Tanzania from dog bite injuries. Bulletin World Health Organization 2002; 80: 304-310.
12. Eng TR, Fishbein DB, Talamante HE et al. Urban epizootic of rabies in Mexico -epidemiology and impact of animal bite injuries.
13. Bögel K, Meslin F-X. Economics of human and canine rabies elimination: guidelines for programme orientation. Bulletin World Health Organization 1990; 68: 281-291.
14. Murray CJL, Lopez AD. The global burden of disease: a comprehensive assessment of mortality and disability from diseases, injuries and risk factors in 1990 and projected to 2020. Cambridge: Harvard University Press; 1996.
15. Kitala PM, McDermott JJ, Kyule MN, Gathuma JM. Community-based active surveillance for rabies in Machakos District, Kenya. Preventative Veterinary Medicine 2000; 44: 73-85.





