Introduction
The University of Queensland (UQ), Australia, runs a 4 year graduate medical program, the final 2 years of which comprise the clinical component. During their third year, students undertake 8 week rotations in medicine, surgery, mental health, general practice and rural medicine, respectively.
Although students can elect to study in one of three Clinical Divisions, namely Southern, Central or Rural, all students undertake their Rural Medicine Rotations (RMR) within the Rural Division. The first week is spent at the Rural Clinical School in Toowoomba or Rockhampton, Queensland, gaining an understanding of rural health issues, including the role of other health professionals in patient management, and learning a number of procedural skills. The following 6 weeks, as two 3 week attachments, are spent at rural practices and regional hospitals, mainly in Southern and Central Queensland. The final week consists of assessments and further educational sessions, in Toowoomba or Rockhampton.
The aim of the RMR is to give all third year medical students exposure to, and an understanding of, clinical practice in rural or remote locations. Given, however, that the primary role of Rural Clinical School is to improve medical recruitment and retention in rural areas, the provision of positive student learning experiences and subsequent ability to make properly informed rural career choices is also regarded as a priority. One of the difficulties in enabling students to gain sufficient knowledge of the spectrum of rural medicine is the relatively short period of clinical attachment, in only one or two rural or remote locations.
Placements are organised in accordance with a number of factors, including student preferences, practice availability, and specific student limitations, such as illness or family issues. This necessary flexibility results in offering placements that are very different in character, ranging from remote sites, such as Central Australian Aboriginal communities or Thursday Island, to near-metropolitan placements, such as Caloundra or Beaudesert.
Therefore, one of the major challenges for the RMR is to enable students to obtain an adequate understanding of the depth and breadth of Australian rural medical practice from a limited rural environment.
A web-based Clinical Discussion Board (CDB) has been introduced to address this problem by allowing students at all locations to discuss their rural experiences and clinical issues with each other. The rationale behind the CDB is to encourage an enhanced understanding of rural medicine through peer-based learning. Likewise, we anticipate that students will achieve deeper learning through discussion and reflection1.
An initial trial of this concept on a voluntary basis proved a failure, with only two contributions from a single student in a 3 month period. On the basis that assessment drives learning and should be an integral part of the educational process2, the decision was made to allot 10% of rural medicine summative assessment marks to the CDB. This decision coincided with a move by the UQ School of Medicine from Web CT to Blackboard eLearning system, enabling the system to be readily accessed through its website as a threaded archival discussion of individual issues. Further clear guidelines for student contributions and evaluation were established. This included preclusion of social discussion within the CDB topic threads. This was because feedback from the first rotation indicated students thought this wasted time in downloading comments that were not relevant to the RMR, and it was not regarded as appropriate to the educational focus of the CDB.
Information and communications technology (ICT) is widely used to support educational programs across disciplines. Entire courses are delivered via the World Wide Web using course management systems3,4, particularly in distance education. In other cases, specific instructional tools such as discussion boards are used to supplement traditional methods5,6. Discussion or bulletin boards enable asynchronous communication between students and teachers, and studies suggest that this enhances learning by promoting reflection, critical thinking and encouraging collaboration and peer learning7,8. Recent research shows that students who actively used a discussion or bulletin board by posting messages achieved better results than those who did not use the board or were passive users9.
Discussion boards have been used to bring together geographically dispersed students, including those undertaking full time distance education, or on temporary placement in rural or remote areas. Providing a forum to discuss course concepts or share experiences assists students to overcome rural isolation and increases their overall exposure to the discipline4,10,11.
In medical undergraduate education, discussion boards have been used in conjunction with streaming video to teach the cognitive basis of interviewing skills8. In Australia and Canada, discussion boards provide a forum for students undertaking rural attachments, allowing them to share experiences with fellow students and preceptors10,11.
This article presents the results of the CDB from the first two RMR of 2005.
Method
Ethical clearance for this project was obtained through the UQ Behavioural and Social Science Ethical Review Committee.
All third year RMR students are required to participate in the CDB. Instructions on access and use of the CDB plus clear guidelines relating to course requirements and evaluation are provided, both orally and included in the 2005 RMR manual, to all third year medical undergraduates prior to the start of each rotation. Students were required to submit a minimum of two original contributions and two replies to other submissions on the CDB. Access was password limited to students undertaking the RMR and academic staff of the Rural Clinical School.
Training of staff and students in the use of the CDB was undertaken by the UQ librarian at Toowoomba and Rockhampton, and an orientation session was given by academic staff in week one of the RMR. IT management and support of 'Blackboard' was provided through the School of Medicine.
The students were asked to evaluate the CDB by responding to a five question survey, plus a comments section that focused on three main issues:
- Was it easy to access and use? (questions 1 and 2; 'was easy to use' and 'was easy to access')
- Was it educationally valuable? (questions 3 and 4: 'increased my knowledge of rural medicine' and 'was useful to my clinical education')
- Was it an enjoyable way to learn? (question 5; 'was an enjoyable way to learn')
Students were asked to respond to each statement on a Likert scale of 1 (strongly disagree) to 4 (strongly agree).
A final question was asked relating to the RMR as a whole, in which they indicated 'how this program had altered their desire to pursue a medical career in rural or remote locations'. This question was presented on a scale of -5 (discouraged my desire) to +5 (encouraged my desire) with a nil effect option of 0 at midpoint.
In addition to an evaluation by the students regarding their opinions of the CDB, the CDB transcripts were also analysed for type of article posted, relevant broad medical category, and specific topic under discussion.
Results
Eighty-three students participated in the CDB during the two RMR (40 students in Rotation 1; 42 students in Rotation 2) and 82 completed the survey. One student did not complete the survey due to an erroneous assumption that local internet access was unavailable. The survey results from the first two RMR are presented (Table 1).
Table 1: Responses to clinical discussion board survey questions
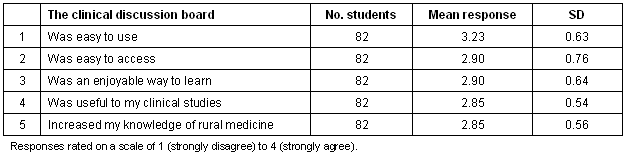
The first five questions were rated on a Likert scale of 1 to 4 (where 1 = strongly disagree and 4 = strongly agree). Students agreed most highly with the statements that the CDB was 'easy to use', 'easy to access' and 'an enjoyable way to learn'. The two questions relating to the 'usefulness of the CDB to their clinical studies' and its potential to 'increase their knowledge of rural medicine' were rated next highest and still above the mid-way rating on the four-point scale.
The final question asked, 'how did the RMR alter your desire to pursue a career in a rural or remote location'? The mean response to this question on a scale of -5 to -1 (discouraged) to +1 to +5 (encouraged), with a mid-point of zero (nil effect) was +2.43 (SD = 2.25) with 23% of respondents giving the question a +3 rating.
A total of 819 CDB website responses (Rotation 1 = 461; Rotation 2 = 403) were collated for type of article posted, relevant clinical category ,and specific topic under discussion. This resulted in 217 individual articles or topics discussed (Rotation 1 = 111; Rotation 2 = 106) within 12 broad categories. The categories and breakdown of topics within them are shown (Table 2).
Table 2: Number and category of topics discussed on the clinical discussion board
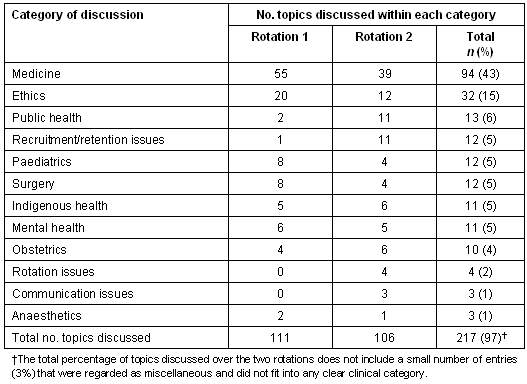
Discussions on medicine were by far the dominant category (43%) with topics that included: dengue fever, opportunistic screening, when sterile technique is needed, snakebite management, and managing a stroke in a rural setting. Ethics was the next most discussed category (15%) with topics that included: chronic illness in visa seekers, use and abuse of hospital facilities in rural areas, where to place an abused child, drug seekers and difficult patients in a rural setting, and safe working hours for rural health workers.
Of the total submissions, a small percentage (less than 2%) revealed significant student distress following a clinical incident or situation. This revealed an unexpected benefit of the CDB in its ability to assist in the early identification of students experiencing difficulties during their rural placement. Because each submission included email contact details, senior academic staff were able to discreetly contact students immediately to address their concerns, thus providing a degree of pastoral care.
Analysis of student participation showed that 36% (n = 35) of the students contributed the minimum requirement of four postings, with the remaining 64% (n = 61) contributing more than five. Further breakdown of this participation showed that 47% (n = 45) submitted more than six postings, 21% (n = 20) contributed more than eight and 14% (n = 13) submitted more than 10 postings.
The students were also invited to provide qualitative feedback on the best and worst features of the CDB, to which the majority of students responded (Table 3). A total of 129 comments were provided, 76% of which were positive and highlighted the best features of the CDB. The remaining 24% of comments focussed primarily on the slow access of the CDB and length of time it took to display discussion threads. This was due to the limited internet dial-up facilities in some rural areas. Any student who had difficulty in CDB access was instructed to contact the Head of Division with their complaint and, if deemed necessary, special consideration was given to these students regarding their assessment on the CDB.
Table 3: Comments on the best and worst features of the clinical discussion board
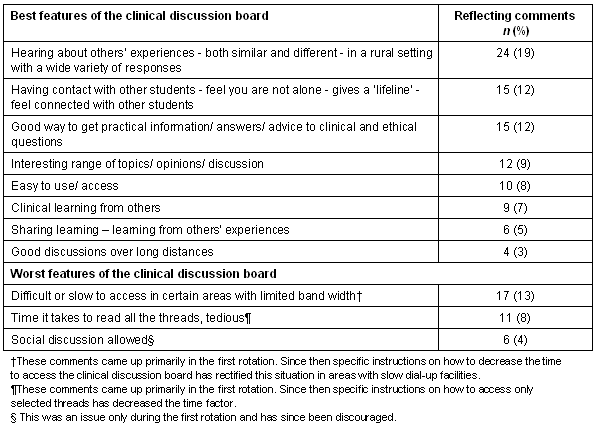
Difficulties with access primarily affected students in the first rotation, in areas restricted to 56 k modem dial-up connections instead of broadband. The problem was readily rectified by advising the second group of students to configure the CDB to view new submissions only, rather than the default setting of all discussion threads. This considerably sped up display and response times and no further major problems were encountered in this area.
Discussion
These data, although preliminary, demonstrate a high level of interest and enthusiasm by these students in the use of the CDB as part of their RMR. This was evident in that the majority of students (64%) submitted more than the mandatory posting requirement. This interest translates to a new approach to learning for students. It provides a method of expanding their clinical experience through contact with peers in other rural areas and sharing their experiences and strategies.
The results of the survey indicated that the students found the CDB 'easy to use' and 'easy to access'. This finding is especially important with respect to the rural rotation because internet facilities in a rural or remote area may sometimes be limited or problematic. The ease of use of the CDB is encouraging also in terms of future use by students, no matter where they may be undertaking their rural placement. Early comments relating to slow internet response times by a number of students using dial-up facilities enabled a configuration modification to be rapidly introduced to rectify the problem. This allowed students at all locations to access the Board in a satisfactory manner and is regarded as crucially important in terms of learning opportunities and educational equity within the Rural Medicine Program.
Students were high in their agreement that the CDB was 'an enjoyable way to learn'. This response was particularly encouraging, given the importance of student engagement with educational activities in obtaining good learning outcomes. Innovative strategies to impart information to students effectively are widely recognised as necessary in 21st century medical education if it is to keep pace with the exponential expansion of new knowledge and information in health science12,13. The CDB appears to hold significant potential as an innovative means of supporting clinical teaching across widely dispersed student groups in a cost-effective manner.
The two questions regarding the 'usefulness' of the CDB to clinical studies and the CDB 'increasing rural knowledge' both received very positive student ratings. These responses provide good support for the strategy of using the CDB as an additional educational resource to increase the breadth and depth of medical undergraduate rural health experiences and knowledge.
The final global question, which asked medical students how the RMR encouraged or discouraged their desire to undertake rural medical practice, was rated very favourably towards encouraging students to choose this as a future career. Considering the well publicised disincentives to becoming a rural doctor in Australia, such as professional isolation and heavy workloads, these findings are very encouraging. The potential ability of positive undergraduate rural clinical experiences to reverse negative perceptions or enhance positive views is a major advantage of the RMR. The CDB as part of that rotation experience may have contributed to this positive response.
The breadth of topics discussed during these first two rotations was remarkable (Table 2). It was interesting to note the number of responses on the CDB that pertained to ethical issues. This highlights the importance of this area to students and may point to the need for more attention devoted to ethical issues during their training. Future research will focus on this dialogue and demonstrate how the students interacted with each other, sharing experiences and ideas on interesting, puzzling and challenging encounters, of which a significant proportion were unique to rural and remote environments. It is particularly interesting to observe that discussions entailing the management of uncertainty generated high levels of student input, often over a period of several days or, occasionally, weeks. High level thinking and acquisition of novel ideas or views is very evident.
Regarding the students' evaluation of the CDB it is encouraging that the majority (76%) of comments provided were positive. In particular they corroborated the peer-based learning aspect of the CDB. Discussion boards have been shown to encourage reflection, collaboration and peer-learning by providing a forum for peer-to-peer dialogue. The exchange of experiences and opinions is enhanced as responses may be more considered14,15. Discussion boards facilitate peer support which is of particular benefit to geographically dispersed groups11,16. Certainly for many students, the CDB serves as a point of contact with and support from their colleagues, and a way to share learning and interesting experiences with each other. This is further proof that the CDB provides the opportunity for all RMR students to gain exposure to a wide range of rural clinical encounters, even though they themselves may not get a chance to experience these or anything similar in their particular placement.
In contrast to this positive feedback, the negative comments were primarily centred on the slow access of the CDB in some rural placement areas. A certain degree of this problem was expected and limited internet dial-up and broadband-width facilities are well documented in more rural and remote areas. The problem was fully realised after the first rotation and steps were immediately taken to rectify this by providing specific instructions for decreasing internet access time. No student was disadvantaged by the initial teething problems. This aspect of the CDB highlights a reality of rural life. Although inconvenient for some students, it provided them with another challenge in their RMR placement and a rural fact of life that needed to be recognised and dealt with.
In summary, the major strengths of the CDB were its ability to expose all students to a rich and diverse variety of Australian rural practice settings and offer students the opportunity to share each other's experiences. Students were able to contribute to diagnosis or management and deal with a greatly increased range of situations or issues in a manner conducive to the development of deep reflective patterns of learning through a peer-based process. The CDB was also seen as having important potential for building professional networks, interpersonal relationships and collegial support systems.
These networks and relationships are essential for rural medicine to help alleviate the possible isolation well recognised in rural life. The CDB also gave students with no current intention of choosing a career in rural medicine the opportunity to develop a much greater understanding of its breadth and depth - its unique character, challenges and, perhaps most importantly, opportunities.
Conclusions
The CDB is a tool, like other web-based systems17, that may prove helpful to ensure that all RMR students receive the maximum benefit and learning experience during their rural rotation. In particular, the CDB assists students in gaining exposure to a wide variety of rural health issues and encounters that, given the short duration of the RMR, they would not have access to. Furthermore it encourages teamwork and collaboration among students which could prove a valuable source of support in future careers. Anecdotal accounts suggest that building professional networks early in their medical education is a particular advantage to rural doctors who often work in isolation with limited support available. Finally, this report has shown that the CDB increases clinical knowledge and understanding through a peer-based learning process.
The CDB offers a unique way to understand the concerns and interests of third year medical students immersed in their RMR. It highlights the issues they need to discuss or share with their peers, provides insights into the ways in which students learn medicine or deal with medical problems of the modern-day world and assists with student support, including pastoral care. Such information may afford medical educators valuable guidance in relation to future curriculum changes or educational support to better prepare undergraduates for their medical careers. The results obtained in these first two rotations of students may also be useful in helping educators identify areas of rural interest. Once identified, these areas of interest can be considered for inclusion in the rural undergraduate teaching programs to encourage interest in rural medicine among their students.
Limitations
A major limitation of this study is that participation in the CDB is mandatory for students and, as such, presents the possibility of participation bias. However the breakdown of the number of responses posted over the two 6 week periods showed there was far greater participation in the CDB than the mandatory requirement. The data presented in this study represent only two rural rotations of third year RMR students. Forthcoming rotations will provide more information on which to further evaluate the educational potential of the CDB.
Acknowledgements
The authors wish of acknowledge the assistance of Yasmin Childs and staff at the UQ School of Medicine IT support service.
References
1. Bunker A, Ellis R. Using bulletin boards for learning: What do staff and students need to know in order to use boards effectively? In: A Hermann and MM Kulski (Eds). Expanding Horizons in Teaching and Learning. Proceedings, 10th Annual Teaching Learning Forum, 7-9 February 2001. Perth: Curtin University of Technology. Available: http://lsn.curtin.edu.au/tlf/tlf2001/bunker.html (Accessed 28 February 2005).
2. Ramsden P. Learning to teach in higher education. Assessing for Understanding. London: Routledge, 1992; 181-213.
3. Witham SA, Krockover GH, Ridgway KD, Zinsmeister WJ. Lessons online: Educational technology for the undergraduate geology classroom. Journal of College Science Teaching 2002; 32: 264-269.
4. Fyfe S. Collaborative learning at a distance: The Human Biology experience. In: A Herrmann and MM Kulski (Eds), Flexible Futures in Tertiary Teaching. Proceedings of the 9th Annual Teaching Learning Forum, 2-4 February 2000. Perth: Curtin University of Technology. Available: http://lsn.curtin.edu.au/tlf/tlf2000/fyfes.html (Accessed 15 April 2005).
5. Land SM, Dornisch MM. A case study of student use of asynchronous bulletin board systems (BBS) to support reflection and evaluation. Journal of Educational Technology Systems 2002; 30: 365-377.
6. Sheard J, Ceddia J, Hurst J, Tuovinen J. Inferring student learning behaviour from website interactions; a usage analysis. Education and Information Technologies 2003; 8: 245-266.
7. Barker S. Introducing group work and communication skills for external students: an analysis of the use of asynchronous online tools. In, G Crisp, D Thiele, I Scholten, S Barker and J Baron (Eds). Interact, Integrate, Impact. Proceedings, 20th Annual Conference of the Australasian Society for Computers in Learning in Tertiary Education; 7-10 December 2003; Adelaide, South Australia.
8. Wiecha JM, Gramling R, Joachim P, Vanderschmidt H. Collaborative e-learning using streaming video and asynchronous discussion boards to teach the cognitive foundation of medical interviewing: a case study. Journal of Medical Internet Research 2003; 5: e13.
9. Hoskins SL, van Hooff JC. Motivation and ability: which students use online learning and what influence does it have on their achievement? British Journal of Educational Technology 2005; 36: 177-192.
10. Broudo M, Walsh C. MEDICOL: online learning in medicine and dentistry. Academic Medicine: Journal of the Association of American Medical Colleges 2002; 77: 926-927.
11. Walker J, Thomson A, Smith, P. Maximising the world wide web for high quality educational and clinical support to health and medical professionals in rural areas. International Journal of Medical Informatics 1998; 50: 287-291.
12. Armstrong EG, MacKey M, Spear SJ. Medical education as a process management problem. Academic Medicine: Journal of the Association of American Medical Colleges 2004; 79: 721-728.
13. Lawson KA, Chew M, Van Der Weyden MB. The new Australian medical schools: daring to be different. Medical Journal of Australia 2004; 181: 662-666.
14. Lindsay-North JL. Incorporating a course website into teaching: a promising practice, especially for teacher education. 2000. (ERIC ED447077). Available: http://www.eric.ed.gov/ (Accessed 21 November 2005).
15. Luca J, McLoughlin C. Peers supporting peers through structured bulletin boards. In: N Smythe (Ed.). Digital voyages. Proceedings, Apple University Consortium Conference, 23 September -1 October 2003. Canberra: Apple Computer Australia.
16. Breen L, Drew N, Pike L, Pooley JA, Young A. Evaluation of the School of Psychology Peer Mentoring Program - Semester 1, 2000. In: A Herrmann and MM Kulski (Eds). Expanding Horizons in Teaching and Learning. Proceedings, 10th Annual Teaching Learning Forum; 7-9 February 2001. Perth: Curtin University of Technology. Available: http://lsn.curtin.edu.au/tlf/tlf2001/breen.html (Accessed 28 September 2005).
17. Crouch M, Richardson G, Reid S. Enhancing patient-based learning: introducing STRAC and the reflective history template. Rural and Remote Health 5: 368. (Online) 2005. Available: http://rrh.org.au (Accessed 13 June 2005).


