Introduction
In accordance with Thailand's Healthcare Reform policy, the universal coverage healthcare scheme, which facilitates a more accessible and standard quality of health care for underprivileged groups, was launched in 2001. Universal health care coverage, or the 30-Baht Scheme (US$1 = 40 Baht), emphasizes the establishment and utilization of primary care units (PCU), which were health centers at the sub-district level that were upgraded to provide front-line healthcare services for communities by health officers, including primary treatment, health promotion, disease control and prevention, and rehabilitation1. The development of PCU aimed to standardize services across the country. Emphasis was placed on proactive community service, the establishment of a self-reliant community and the facilitation of health promotion among all age groups.
The concept of supervision is widely used in public health, community health care and the nursing discipline in general. However, supervision is not a well-defined concept and there is a lack of consensus with regard to a definition2. Supervision is very important for process and service quality control, which is the main goal of the universal coverage healthcare scheme1. In the present study, supervision was defined as the processes of monitoring, problem analysis, identifying the causes of problems, investigating to improve operations, explaining guidelines and providing suggestions and directions to improve operations regarding service system management, treatment, patient safety and health promotion of PCU. The definition covered management supervision and clinical supervision. Strengthening supervisors' capabilities is an important mechanism influencing the success of service delivery. Previous studies have revealed that community involvement helps the community to identify problems itself, formulate alternatives to meet community needs, and may lead to establishing a network for community health promotion, and help sustain physical exercise and sporting clubs in the community3-5. The purpose of this study was to compare and identify the strengths and challenges of two different supervisory models in building the health promotion capabilities of PCU health officers and the community, based on the concept of community participation in management and health service systems development, in two PCUs in Chiang Mai Province, Thailand.
Methods
A quasi-experimental study was utilized with two different supervisory models over the six-month period, September 2003 to February 2004. In the first model, supervision was conducted by supervisors from district level with the full participation of health officers at tambon (sub-district) level. The second model was designed with the additional involvement of the community in the supervisory process. Prior to implementing the models, district supervisors attended a re-training course to enhance their supervisory knowledge and ability. This participatory training course was based on the existing literature as well as information obtained from interviews with 18 selected district level supervisors and supervisees. Participatory training referred to a continuous learning process, starting from experience or current activities, followed by analysis and conclusion, leading to operative planning implementation. This training consisted of two phases. The objectives of Phase 1 were to improve the knowledge and abilities of district level supervisors, to set plans for supervision in the PCU, and to develop supervisory instruments and documents (6 months). Phase 2 aimed to compare the results of the two supervisory models (6 months). The conceptual framework for the study is shown (Fig 1).
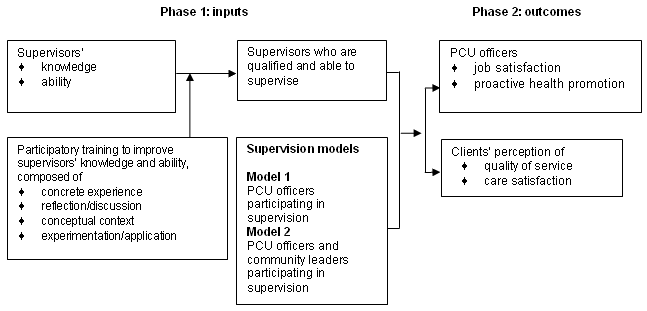
Figure 1: Conceptual framework for the participatory supervisory model of a primary care unit (PCU) in Chiang Mai Province.
Settings
Mae Oon semi-district is 27 km east of the city of Chiang Mai, a northern province of Thailand, where there were six tambons (sub-districts) and 48 villages. Two PCU were recruited into this study, with the following inclusion criteria, to: (i) be in the Mae Oon Hospital Network under the Ministry of Public Health; (ii) have a clear scope of responsibility for the people; (iii) be open at least 56 hours per week for all primary medical treatment and provide rehabilitation and healthcare education services; (iv) employ community health officers and provide equivalent public health technologies; (v) have personnel working in the PCU who are responsible, enthusiastic, understand the universal healthcare scheme, and have cultivated a good relationship with supervisors and community leaders; (vi) have no epidemic diseases in the area, such as dengue hemorrhagic fever or leptospirosis. PCU with doctors from the Ministry of Public Health providing services were excluded. PCU 1 is located approximately 75 km from Chiang Mai city and 80% of its responsible area is valleys. There were 1367 families, and the households were scattered. The total population was 4921 persons, with 2511 male and 2410 female. PCU 2 is situated on the west of Mae Oon semi-district business center. There were 659 families and the total population was 2524 persons, of whom 1284 were male and 1240 female. The locations of the two PCU are shown (Fig 2).
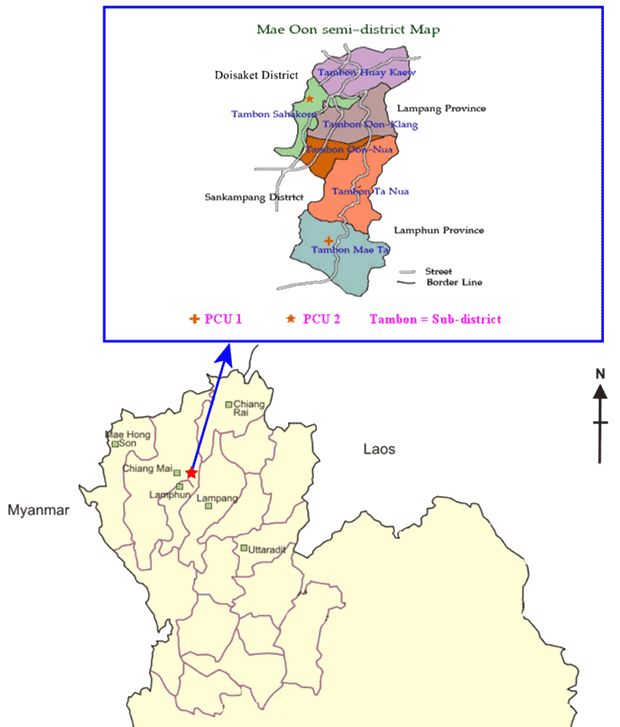
Figure 2: Location of two selected PCU in the study area, Mae Oon semi-district, Chiang Mai Province, northern Thailand.
Participants
Three sample groups participated in the supervisory trial and service satisfaction survey.
Group 1: Group 1 consisted of 18 district-level supervisors who were chosen to attend a supervision-retraining course. Five of these participants were selected to be supervisors of the two supervision models: four graduate nurses and one technical officer. All passed the post-retraining test on supervisory knowledge and ability with at least 80% of the total possible scores, as well as having good work performance, based on researcher observation.
Group 2: Group 2 consisted of three health officers from each PCU, Ban Huay Sai (PCU 1) and Ban Sahakorn (PCU 2) in Mae Oon semi-district. They were included based on observation of their work performance, which met the minimum requirements for the PCU target indicators, such as family planning practices and immunization in the community.
Group 3: Group 3 consisted of clients who utilized the two participating PCU during the study period: 195 clients before and 195 after implementing supervision in each PCU. The sample size was estimated based on the single proportion formula, with a 95% confidence interval. A sample of 195 clients was calculated based on a rate of 42% 'good' satisfaction in the pilot study at a nearby PCU in Mae Oon semi-district. The cut-off point for 'good' satisfaction was defined as ≥80% of the total possible score, and precision was set at 7%. Convenience sampling was used and the inclusion criteria were clients aged 15-60 years who utilized the PCU service during the study period and had at least one experience using PCU health services in the previous year. The research protocol was approved by the Committee on Human Rights Related to Human Experimentation, Mahidol University, Thailand.
Participatory supervision process
Supervision is a complex activity, occurring in a variety of settings, and having various definitions, functions, and modes of delivery6. Kadushin7 defined the functions of supervision as administration or management, education and support. This idea of supervision is reflected across professionals; for example, medicine8, nursing9 and social work7. The intervention is called 'participatory supervision' because supervisors, health officers, and the communities shared the building of health-promotion capacity. The supervisory model referred to guidelines, methods, and tools used for supervision, according to the following models.
Supervisory model 1: Supervisory model 1 included health officers' participation in PCU 1. The district level supervisors and PCU officers had equal voices and input into identifying problems, planning, decision-making and evaluation. The supervisors' main goals were improved treatment, health promotion services, and client satisfaction. The processes of the health officers' participatory supervision were as follows:
- Step 1: established treatment and health promotion service criteria.
- Step 2: supervisors collected and examined monthly health status and unit performance data in each area under the responsibility of their PCU.
- Step 3: the supervisors and health officers in the participating PCU analyzed work performance, comparing outcomes with targets, and identifying problems.
- Step 4: the supervisors and health officers in the participating PCU analyzed the causes of problems or obstacles together and provided advice.
- Step 5: the supervisors and health officers in the PCU participated in identifying problem-solving methods.
- Step 6: summarized supervision outcomes.
Supervisory model 2: Supervisory model 2 was similar to model 1 with the additional of community involvement in the supervision process, with supervisors and health officers in PCU 2. This supervisory model was divided into two periods. The first period was supervision with participation of the PCU health officers and community leaders, who consisted of a teacher, a village headman, representatives from the Tambon or sub-district Administrative Organization (TAO), representatives from the group of elders, representatives of housewives, representatives from village health volunteer groups and the village development sub-committee. The working steps were:
- Step 1: established an action plan for treatment and health promotion services.
- Step 2: established outcome expectations for the health services.
- Step 3: collected data.
- Step 4: the health officers presented the working results.
- Step 5: the supervisors, health officers, and community leaders participated in finding alternative methods to solve problems related to service system management and proactive health promotion.
- Step 6: summarized the supervision outcomes.
The second period was the supervisory model with the participation of PCU health officers only. This supervisory model aimed to enhance the capability of PCU health officers in providing primary treatment, drug administration, and other health services. The supervisory process included collecting data, summarizing the problems by supervisors and PCU health officers, and finding ways to provide better health services.
Measures
Quantitative measurement: To measure the health officers' job satisfaction, all health officers completed a 33 item questionnaire with a 5 point rating format (1 = very dissatisfied, 2 = dissatisfied, 3 = moderately satisfied, 4 = satisfied, 5 = very satisfied). The dimensions of health officers' satisfaction included satisfaction with policy, working conditions, work itself, responsibility, security, achievement, recognition, team work, welfare and remuneration and advancement. Possible scores ranged from 33 to 165. Cronbach's alpha was 0.87.
Clients' perception of service quality consisted of 19 items with a 5 point rating scale (1 = strongly disagree, 2 = disagree, 3 = moderately agree, 4 = agree, 5 = strongly agree). Possible scores ranged from 19 to 95. Cronbach's alpha was 0.94.
Clients' care satisfaction consisted of 18 items with a 5 point rating scale (1 = very dissatisfied, 2 = dissatisfied, 3 = moderately satisfied, 4 = satisfied, 5 = very satisfied). Possible scores ranged from 18 to 90. Cronbach's alpha was 0.94.
Qualitative aspects: Proactive health promotion services were assessed by semi-structured interviews, reviews of monthly health reports and use of an observational checklist while the investigator attended meetings for proactive health promotion services preparation. Semi-structured interviews and participant observations were also used to explore the health officers and community involvement, the strengths and challenges of each supervisory model (for details of all instruments see Sennun10).
Data analysis
For the quantitative analysis, descriptive statistics (ie, mean and standard deviation) were used describe all research variables. An independent t-test was used to compare clients' perceived service quality and care satisfaction before and after supervision between and within the two supervisory models. The level of significance was p <0.05.
For the qualitative analysis, all interviews were transcribed for thematic analysis11. The first and third researcher read and re-read the transcribed texts to construct codes and identify emergent issues and themes, to discern the principal themes related to the reasons for involvement of health officers and the community, and identify the strength and challenges of each supervisory model. Data were also triangulated across data-collection methods12: observation, reviews of monthly health reports, and semi-structured interviews looking for structure, meaning, and checking the validity of the data.
Results
Baseline for PCU health officers
Of the three health officers at PCU 1, two were female. All had completed bachelor degrees, had a mean age of 40 years and mean working experience of 20.7 years. At PCU 2, one health officer was female and two were male. All had completed bachelor degrees and their mean age was 34.7 years. The mean working experience was 14.3 years.
PCU health officers' job satisfaction
After the intervention, the overall job satisfaction mean score for model 1 increased from 105.3 to 113.7, and for model 2 from 109.7 to 126.3. Both before and after, the PCU health officers appeared to have good and comparable job satisfaction levels. Due to the small population sizes (three per group), the health officers' survey data were not analyzed statistically.
Clients' perceived service quality and satisfaction with care in the PCU
A total of 195 clients who were seeking care at each PCU during the study period completed the questionnaire before and after the intervention. The general characteristics of all participants are shown (Table 1). After supervision, the mean score for clients' perceived service quality among PCU 1 (model 1) decreased significantly (80.5 vs 77.8; p = 0.001). Similarly, the mean score for client satisfaction decreased significantly (74.0 vs 71.5; p = 0.006). PCU 2 (model 2), after supervision, the mean scores for clients' perceived service quality before and after supervision were almost the same (80.8 vs 80.9; p >0.05). In contrast, after supervision, the mean score for client satisfaction had increased statistically (72.7 vs 75.0; p = 0.013).
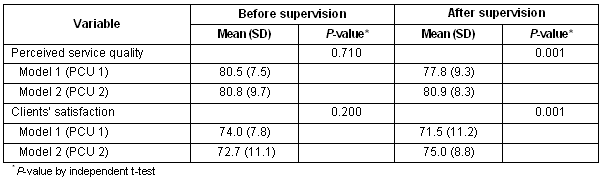
Clients' perceived service quality and care satisfaction mean scores were compared between models 1 and 2. Before supervision the mean scores for both variables in models 1 and 2 were not statistically different (p >0.05). However, after supervision, the mean scores for both variables in model 2 were significantly higher than for model 1 (p <0.001) (Table 2).
Table 1: General characteristics of 195 clients before and after the health officers received participatory supervision in each model
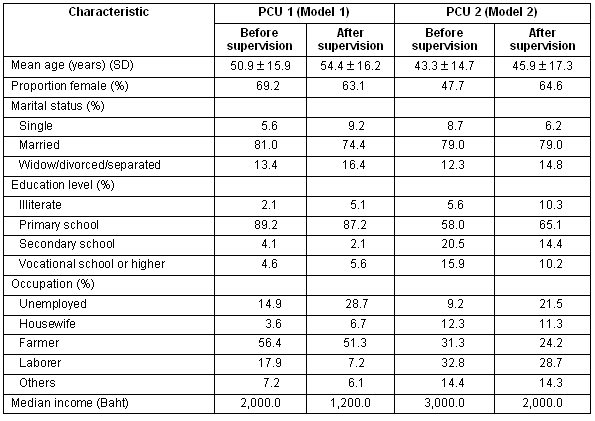
Table 2: Comparison of clients' perceived service quality and care satisfaction between 2 supervisory models among 195 clients before and after the health officers received participatory supervision
Qualitative findings
Differences in health promotion activities between the two supervisory models: The comparative health promotion activities of the two PCU were assessed by semi-structured interview, reviews of monthly reports, and an observational checklist, to ascertain whether the health officers followed the core health promotion activities package.
Supervisory model 1 The health promotion activities of the health officers in PCU 1 were prenatal care, such as teaching pregnant women, assessment of nutritional status, assessment of mental condition, promoting nutrition for children to solve malnutrition problems, assessment of development in pre-school age and autistic children, assessment of nutritional status in school-age children, health education for various community groups, and an annual physical check-up campaign for people ≥21 years. Establishment of an exercise club in the village was a community health promotion activity.
Supervisory model 2 The health promotion activities of the health officers in PCU 2 were the same as for model 1. Additional activities comprised coordinating and supporting the community committee for health and quality of life development through organizing community activities, for example, by providing a training program to enhance consumer and food vendors' knowledge of food safety, clean food/good taste, providing social support for specific patient groups such as diabetes, hypertension, and obesity self-care. Before supervision, the PCU 2 community already had a health promotion and quality of life development club. The major activities were providing health education for pre-school parents on National Children's Day; organizing a training camp for teenagers and parents; setting up information boards for an accident prevention campaign, and setting up activities and responsibilities for sanitation and environmental health improvements in the village.
Opinions of community leaders, PCU officers and supervisors about the supervisory models: All community leaders said that they were very pleased about the opportunity to participate in the supervision because it was very useful and exactly what they needed. Participatory supervision made it possible for them to learn the problems of the community and to help solve them. They were proud to be part of the community development team with people with differing areas of expertise.
The PCU officers felt that participatory supervision for community leaders was very useful. It made them feel that they were not alone in providing health services, but that there were people in the community giving them support, particularly with community health promotion. In addition, the community leaders could provide opinions from their own perspectives regarding problems in the health center and help to promote health in the community. However, they felt participatory supervision should be more open to community leaders regarding health issues, to gain greater input, comments and suggestions for their health operations.
The supervisors felt that the participation of the PCU officers and community leaders provided better community health promotion outcomes than the other supervisory model. It accounted for more community activities, greater participation, and a sense of belonging. They expected participatory supervision from the PCU officers to have a greater effect on improving the PCU than supervision with only PCU health-worker participation.
Strengths and challenges of the PCU officers' participatory supervision (model 1)
Strengths: First, after supervisory model 1 was implemented some changes occurred in the administration of medical supplies and family folder use in the PCU. (The family folder is a folder that contains brief health information of all family members, a genogram, family members' general characteristics, major health problems of each and progress notes on treatment). The records for health promotion services and annual physical examinations were completed. The second strength was its democratic characteristic. When the health officers collected the working results, analyzed the problems' causes and alternatives, and decided on the correct methods, they also gained the ability to analyze problems, and the skills to find solutions, acquiring wider perspectives and diversity in problem solving. Problem solving teamwork helped brainstorming, it involved acceptance and respect between the supervisors and the health officers. In addition, the work in the PCU had become systematic, and the health officers had increased working knowledge regarding advising clients and writing up health reports correctly. The feedback data were used for healthcare service development.
Challenges: The health officers had an increased workload due to collecting work results, preparing problem analysis and problem solving for presentation to their supervisor. Moreover, the participation required had the potential to cause conceptual arguments among the team that could lead to conflict. From the standpoint of the participants, the officers' participatory supervision did not always proceed well, and not all health officers could participate in every step of the supervision process, due to their client service obligations.
Strengths and challenges of PCU officer and community leader participatory supervision (model 2)
Strengths: First, as a result of implementing supervision, changes occurred in the administration of the medical supplies and healthcare practices in the PCU. Regarding health promotion, the health officers were able to work with the community health improvement and quality of life development committee in PCU 2 and the community leaders in order to solve problems. Second, community leaders felt authorized to give feedback to the PCU regarding community problems. Third, in this supervisory model, community health promotion by the community itself worked best. This was because of community empowerment from the process of building the knowledge, skills and experiences to enable increased community self-development. The process of equal participation, without discrimination according to social status, strengthened the community and promoted greater participation. Therefore, the benefits of participation decreased reaction to change. Fourth, the participation of a wide variety of people assisted in rapid development of the community.
Fifth, from observation of participatory supervisory model 2, community leaders demonstrated cooperation and participated in sharing their opinions, presenting problems and giving advice to the health officers. Every officer in the PCU attended every supervision session. In this supervision model, the roles of both PCU health officers and community leaders changed from previous styles. Previously, the community leaders received supervision from the health officers. In contrast, with this supervision model, the community leaders played roles as supervisors while the PCU officers were supervised. They could express their demands, identify health problems and suggest solutions based on local wisdom focusing on health promotion activities. The roles of the supervisors at the district level were to control the operation according to the PCU standards and ensure that there was active participation among the partners. This new model of supervision focused on the supervisor's role, and thus the results of supervision in the first two sessions were unsatisfactory. In the third session, the officers and community leaders started to adapt, so that supervision was more constructive. Consequently, the supervisor had a clearer role in providing knowledge to the officers, similar to being a teacher.
Challenges: The challenges are similar to those of model 1, with increasing workload and conflict between the PCU health officers and community leaders during discussions. In addition, community leaders had to allocate their time to participate in the supervision.
Discussion
The success of both participatory supervisory models in this study may be due to the strong support of the supervisors at Chiang Mai provincial level, and the mutual benefits to the staff and the research team. In the present study, supervisory model 2 appeared more successful than model 1. There may be several explanations for this. In model 2, the community had the opportunity to give critical advice to health officers that had never been offered before. The participation of the community was empowering13. By enhancing knowledge, skills and experiences, the community became more responsible for its own development14-16. The process of equal participation, without discrimination according to social status, strengthened the community and promoted greater participation17. The benefits of participation decreased reaction against change18. The participation of a wide variety of people assisted in rapid development of the community. Model 2 communities had a common goal, focusing on pre-existing health promotion and the development of quality of life. This may have made the community more proactive in health promotion than in model 1. Some examples of health promotion activities include nutrition, accident prevention, taking care of teenagers, and sports racing. Model 1's health promotion was less self-generated and people did not have an opportunity to identify community problems. Participatory supervision in the community created an awareness of community health. Community leaders identified community health problems, determined solutions in relation to the community's demands, and introduced health promotion activities to health personnel based on local wisdom. Guidelines for improving the services had been made by the three partners. This satisfied the community and gained their cooperation. The enthusiasm of the health officers created relationships between the officers and the community. However the different sizes of the two communities may have had an effect. PCU 2 was smaller, and this may have resulted in better community involvement and collaboration. After supervision, model 2 clients rated service quality and care satisfaction as significantly higher than those in model 1, possibly due to the participation of the community leaders.
Limitations
One potential source of bias in this study was selection bias, because we only included supervisors with a good knowledge of, and enthusiasm for, supervision, and only health officers whose work performance achieved the minimum requirements of the PCU target indicators in the study. This was likely to partially affect the positive outcomes of the participatory supervision model. Other major limitations of this study were: first, the 'Hawthorn effect', in which the officers felt that they and their practices were being observed and, thus, changes occurred. Second, during the study period, some influential incidents occurred that affected the study results and the performance of the officers. There were many distracting events, such as the SARS epidemic, a new policy on narcotics suppression, a call for public health officers to set up a camp to treat drug addicts, the 'avian flu' epidemic, and a TAO committee election. These events consumed a large amount of health personnel working time. Third, PCU health officers had other responsibilities apart from providing common health services. These included monthly meetings with the public health officers and meetings with the TAO committee. All these affected the service system development in the PCU and the arrangement of health service activities in both nursing care and health promotion. Fourth, the client sample groups before and after implementing supervision were different, which may have affected measurement of clients' perceived service quality and care satisfaction. In addition, PCU 2 was of a smaller size and had pre-existing health promotion in the form of a quality of life development club. Thus, it is difficult to decide conclusively that the significant improvement in client scores for perceived service quality and care satisfaction was solely due to the effects of implementing the participatory supervision model.
Conclusion
This study showed positive outcomes for two forms of participatory supervision in a rural setting. There appear to be additional positive outcomes for the model that involved community participation. The proposed supervisory model might be useful as a guide for further supervision in the future. Relationships among community leaders, health officers and supervisors, as well as the supervision evaluation process, should be improved in a participatory manner.
Acknowledgements
The authors would like to thank the district supervisors and health officers in Ban Huay Sai and Ban Sahakorn PCU in Mae-Oon Semi-district, Chiang Mai, Thailand, and the clients who participated in this study. This study was partially supported by a research grant from the Faculty of Graduate Studies, Mahidol University and Payap University.
References
1. Thai Ministry of Public Health. [Standard of primary care service system.] (Online) 2002. Available: http://www.moph.go.th (Accessed 20 April 2002). [In Thai]
2. Hyrkäs K, Koivula M, Paunonen M. Clinical supervision in nursing in the 1990s - current state of concepts, theory and research. Journal of Nursing Management 1999; 7: 177-187.
3. Chaoniyom W, Suwannapong N, Howteerakul N, Pacheun O. Strengthening capability of family health leaders on sustainable community-based health promotion. Southeast Asian Journal of Tropical Medical Public Health 2005, 36: 1039-1047.
4. Boswell C, Cannon S. New horizons for collaborative partnerships. (Online) 2005. Journal of Issues in Nursing 2005; 10. Available from: http://nursingworld.org/ojin/topic26/tpc26_2.htm (Accessed 8 April 2005).
5. Townsend M, Moore J, Mahoney M. Playing their part: the role of physical activity and sport in sustaining the health and well being of small rural communities. Rural and Remote Health 2: 109. (Online) 2002. Available from: http://rrh.org.au (Accessed 16 May 2005).
6. Kilminster SM, Jolly BC. Effective supervision in clinical practice setting: a literature review. Medical Education 2000; 34: 827-840.
7. Kadushin A. Supervision in social work. New York: Columbia University Press, 1976.
8. Coles C, Peyton JWR (Eds). The educational supervisor's role in medicine. Teaching, learning in medical practice. Heronsgate: Medicare Europe, 1998.
9. Brocklehurst N. Clinical supervision in nursing homes. Nursing Times 1997; 93: 48-49.
10. Sennun P. Supervisory model of community health center in Chiang Mai Province (PhD Thesis). Nakhon Pathom: Mahidol University, 2004.
11. Boyatzis R. Transforming qualitative information: thematic analysis and code development. Thousand Oaks, CA: Sage, 1998
12. Patton MQ. Qualitative research and evaluation methods, 3rd edn. Thousand Oaks, CA: Sage, 2002.
13. World Health Organization. Community involvement in health development: challenging health services. Report series 809, Geneva: WHO, 1991.
14. Chavis D, Florin P. Community development, community participation, and substance abuse prevention. San Jose, CA: Santa Clara County Department of Health, 1990.
15. Labonte R. Health promotion and empowerment: practice frameworks. Toronto: Center for Health Promotion and Participation, 1993.
16. Labonte R. Health promotion and empowerment: reflections on professional practice. Health Education Q 1994; 21: 253-68.
17. Suwannapong N. [Unit 10 Community participation in health development in Health and Development, 1st edn]. Nonthaburi: Sukhothaithammathirat Universtiy, Department of Health Sciences, 2003; 47-122. [in Thai].
18. Reber RW, Gilder GV. Behavioral insights for supervision, 2nd edn. New Jersey: Prentice-Hall, 1982.



