Introduction
Seventy-five percent of all deaths can be expected; this is when a person with an incurable life-limiting disease is likely to die within the next year1. Such people benefit from palliative care, which improves their quality of life and experience of dying through early identification, assessment and treatment of physical, psychological, social, cultural and spiritual symptoms and needs, respecting their care preferences, and supporting their carers and family in bereavement2,3. Palliative and end-of-life care is provided by general practitioners, primary healthcare teams, palliative care specialists and others, but access to quality care is limited across Australia and the need for such care is predicted to double in the next 25 years2,4-8.
The palliative care landscape is changing across Australia, informed by national and state-based strategies. Australia’s National Palliative Care Strategy advocates for the provision of appropriate and quality palliative care in a suitable setting from providers with capacity and capability2. While not every dying person requires input or care from specialist palliative care services (SPCSs), everyone should have ‘equitable access to quality care based on assessed need as they approach and reach the end-of-life’, thereby making palliative and end-of-life care everyone’s business (p.5)9. Meeting this growing demand for care will challenge health systems, particularly where there are known gaps, such as a lack of clearly defined roles and coordination of care across provider groups, and in rural and remote communities where access is limited due to distance as well as workforce and resource shortages4,6-8,10,11.
The Far West Local Health District (FWLHD, District) in New South Wales (NSW), Australia, serves a remote region with approximately 30 000 people living across 200 000 km212. An SPCS has been operating throughout the FWLHD since 1989; the service had 5.5 full-time equivalent nursing staff and a 0.5 full-time equivalent palliative physician at the time of the mapping study. They provide access to 24-hour palliative and end-of-life care and they work in collaboration with generalist providers (including those working in hospital, primary healthcare, residential aged care facilities (RACF) and community-based services). The SPCS care for approximately half of the people in the FWLHD whose deaths are expected; however, little has been documented about the palliative care provided to the other 50%. What does their palliative and end-of-life care look like and who provides it?
In 2007, a study in the district investigated how well-equipped nurses working in remote health service facilities felt to provide palliative care13. A key recommendation from that study was that a formal model was needed to guide the delivery of quality palliative and end-of-life care across the District. The Far West NSW Palliative and End-of-Life Model of Care has now been developed to offer the first whole-of-system response for a palliative approach to care in a remote region (Fig1). The model was adapted from a best practice model used in the UK14. It provides a simple structure for the last year of life that applies the recognisable palliative care phases (stable, unstable, deteriorating, terminal, bereavement)15. The model is applicable for both generalist and specialist services, thereby ensuring a consistent and quality palliative approach to care for everyone from an appropriate provider, at the right time, and in the place of the person’s choosing, regardless of age or diagnosis. A palliative approach to care can be cost effective and improve patient outcomes such as effective pain management, fewer hospital admissions, and dying in the place of one’s choosing4,16,17.
Prior to implementation of the model, the delivery of palliative and end-of-life care in the FWLHD was mapped, with objectives to:
- identify who was involved in providing such care in the FWLHD, how they connect, and any gaps in the network
- describe what care was provided and identify any challenges to care provision.
This article reports on the outcomes of a mapping study.
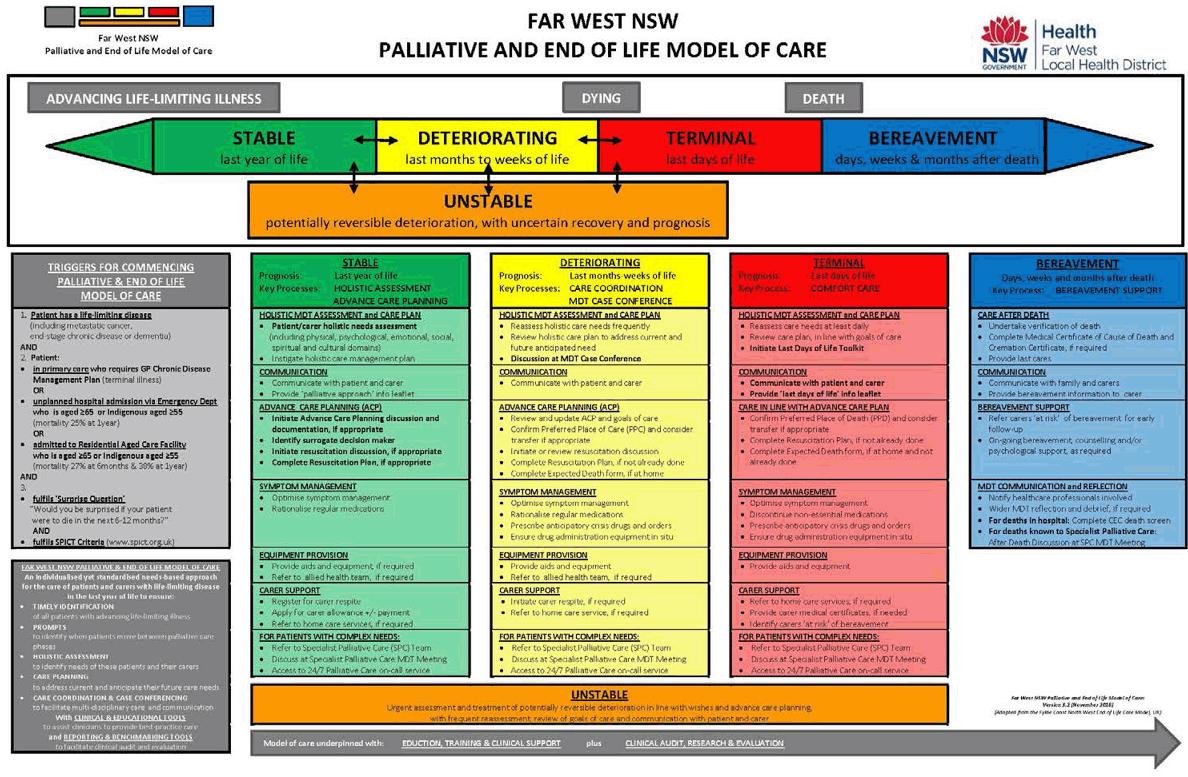 Figure 1: Far West NSW Palliative and End of Life Model of Care.
Figure 1: Far West NSW Palliative and End of Life Model of Care.
Method
A social network methodology was applied for this mapping study. In-depth, semi-structured interviews were conducted with SPCS and generalist healthcare providers within the FWLHD (Table 1). The SPCS were invited to participate, and interviewed first. A one-tiered snowball technique was then used to identify, invite and interview generalist providers from the identified provider settings.
Fifteen interviews were conducted over 7 months (December 2014 to June 2015) in each respective workplace or at the university, audio-recorded and transcribed. The interviews were grouped by provider and setting, identified as specialist (S) or generalist (G), and numbered for referencing and confidentiality. The transcripts were analysed within a social network analysis methodology using both inductive and deductive content analyses18. They were deductively analysed to identify who provided palliative care along with patterns and connections between providers (Table 2). This, along with a second deductive analysis, identified unidirectional connections in order to map the services and providers involved in providing palliative and end-of-life care in context19. The resulting network map was created using NodeXL v2014, a free network analysis program for Microsoft Excel (Social Media Research Foundation; https://nodexl.codeplex.com/2014) (Fig2). An inductive analysis of the transcripts examined processes of and challenges for providers and the provision of palliative care along with suggested improvements for care.
Authors ES and DL are independent researchers working with the SPCS. ES conducted all interviews and initial analyses, approaching the study as a blank slate. Initial and progressive codes, analyses and findings were reviewed and final interpretations reliability-checked with DL. Co-authors SW and MC assisted the study design and confirmed interpretations but, as members of the SPCS, they did not collect, analyse or interpret any project data.
Table 1: Invited and consenting interview participants, identified by group and setting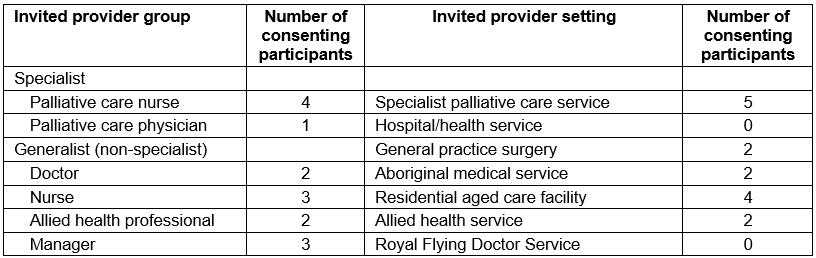
Table 2: Communication lines identified from interviews by provider settings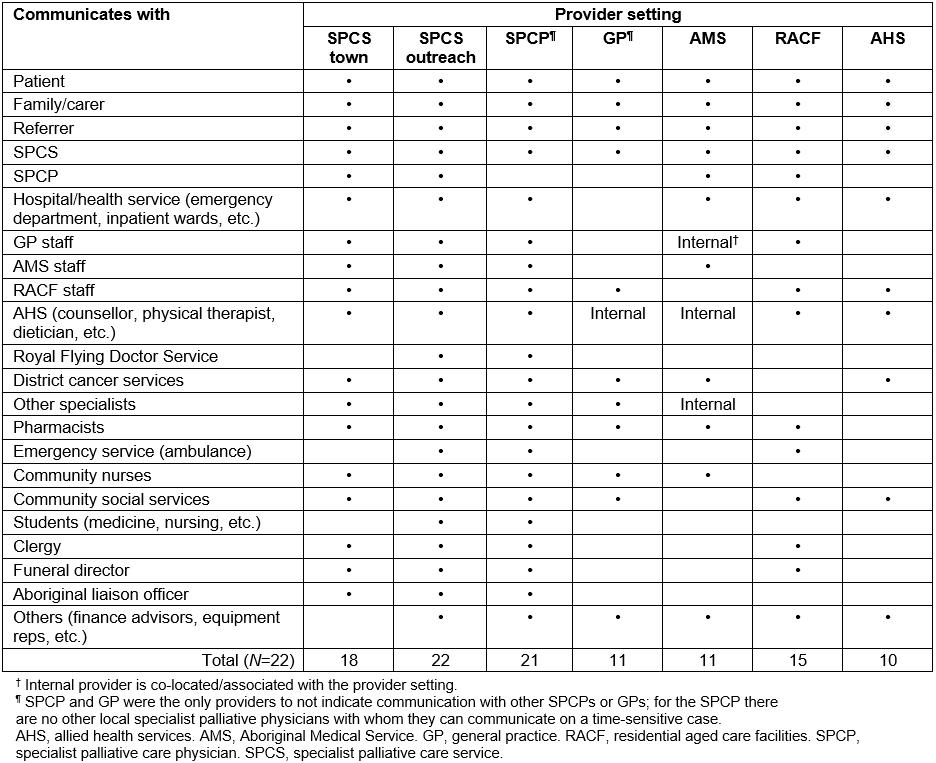
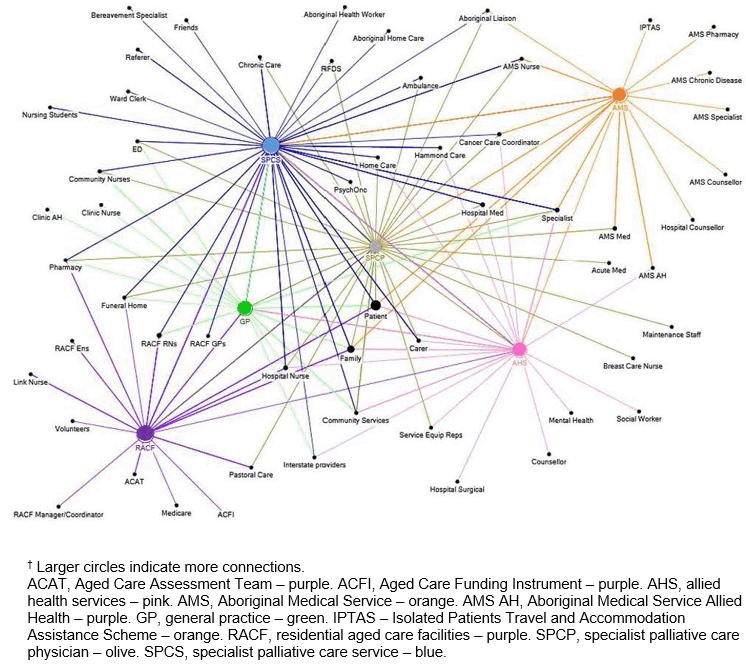 Figure 2: Network map of unidirectional connections associated with the provision of palliative and end-of-life care in the Far West Local Health District (at 2015).†
Figure 2: Network map of unidirectional connections associated with the provision of palliative and end-of-life care in the Far West Local Health District (at 2015).†
Limitations
Two provider settings did not respond to participate. While it was not possible to ascertain their unique perspective, experience and position, this study was able to indirectly map their involvement through the other participants’ accounts. The majority of participants were based in the district’s regional hub, thereby reflecting a particular experience. While small participant numbers may limit the range of experiences reported, commonalities were identified to support the transferability of results.
Ethics approval
Ethics approval was granted by the Greater Western Human Research Ethics Committee (LNR-14-GWAHS-94).
Results
Who is involved in providing a palliative approach to care?
It is known that palliative care is provided by specialists, generalists, and even supported by lay carers and volunteers2. This palliative care network map demonstrated the extent of multiple connections within the district prior to implementing the new model (Fig2). Everyone interviewed said that they knew their community and patients well and that they had good communication with their patients, families and other providers associated with palliative care – from hospital staff and allied health professionals to pharmacists and volunteers (Table 2). Often the pronoun ‘we’ was used when discussing care provision, and one specialist explained:
It is ‘we’ because it’s not just one, it can’t be one person … for most patients it’s ‘we’. … [‘we’ is] whoever has been required to provide service to that patient. So it’s a team, it’s a service, ‘we’ are the service and the team. (S4)
The SPCS had the most connections within this network, in part as they were the first to be interviewed, but this was also commensurate with their central role in palliative care across the region and reflected the high referral rate for specialist care (Table 2). They have provided 24-hour palliative and end-of-life care to far west NSW for almost 30 years and were well integrated into the palliative mindset of the district.
The RACFs care for many people with life-limiting illnesses and were the most connected generalist setting in the network; this was followed by general practice and the Aboriginal Medical Services. The allied health services had the least connections within this network; their involvement was defined by their discipline and in response to particular needs (Table 2). Although half of the people who die an expected death in the FWLHD are referred for specialist care, the generalist providers felt responsible for the management and care of each dying person and their family:
We’re doing the same thing; we’re doing … the best by the patient. (G4)
The network demonstrated connections and opportunities for communication between the services and providers involved in palliative care. Mapping and knowing the network is a vital step for achieving effective and integrated care by incorporating and enhancing current referral pathways, respecting existing relationships and enabling new connections as needed. Mapping can also inform the adoption of the model, which provides a clear structure, along with key processes, to support person-centred and integrated care.
What care is provided?
As specialists, the SPCS are trained to provide timely support for complex needs and long-term care along the person’s palliative journey, through death, and into bereavement using regular assessment and management of holistic needs, care planning, equipment provision and family support. They were the only provider to discuss active and routine support for bereavement. The care they provided was described by others as consistent, high quality, and equitable. They were:
… sensitive with every patient. I think that helps and it’s a part of their everyday practice … they’re actually sensitive to every patient that they see. (G4)
For the generalists, identifying patients needing a palliative approach, and the provision of such care, was less clear:
No one necessarily asks the question as to whether or not the patient is dying. (G10)
While each of the generalist participants considered palliative care to be part of their usual role, they had different views and definitions of ‘palliative care’ and what it involved. ‘Palliative care’ was commonly linked with ‘comfort care’ and short timeframes (no more than a few months), deterioration due to a life-limiting illness, no expected recovery, particular pain management strategies or the diagnosis. Patients with incurable cancers had a clear referral pathway to the district’s cancer services and SPCS. This reflects the established history and association between oncology and palliative care. However, identification, provision and referral options for those with chronic, non-malignant, life-limiting diseases were less clear. This may be related to the trajectory and unpredictability of end-stage chronic disease, as prognostication and palliative needs can be difficult to determine and identify4. Delayed identification for a palliative approach, or even referral to specialist palliative care, was noted by the participants as an issue because need may be masked with familiarity, not recognised or not considered significant.
The network mapping highlighted an opportunity within local networks to consolidate and integrate systems and care practice. Identifying someone in need of, and providing, palliative care may be confronting and could pose challenges for timely care. The gaps in the provision of care highlighted the need for a model that provides a consistent definition of and process for palliative care which incorporates universal triggers, along with locally adaptable tools, to enable earlier identification for a needs-based approach to care, independent of diagnosis, during the last year of life.
Challenges to providing palliative care
Challenges of communication and coordination were identified, and within this palliative network there were opportunities for new and integrated connections to enhance the provision of care. Each person interviewed reflected that better communication, coordination and integration would minimise problems and misunderstandings, and improve patient care. Improving collaboration and coordination will require agreement and engagement across provider groups and settings to enable a needs-based palliative approach for everyone. Challenges of communication and coordination are not new or unique to the district nor health care13,20.
Referral indicators and processes were also identified as a challenge and gap by each provider within the network. The SPCS receive referrals across the district, but highlighted that the reason and timing for these referrals were variable:
We need something there right at the start so that referrals are made appropriately. (S1)
Timely identification provides ‘opportunities to establish goals of care and to plan for changing care demands into the future. [It] also allows for earlier consideration of approaches to care that focus on improved quality of life. … [and] increases capacity to improve support to carers and families, especially where the patient’s goals of care include remaining at home’9. Incorporating ‘triggers’ to help identify and initiate a palliative approach earlier, along with indicators for referral, could guide the appropriate assessment and provision of care no matter the provider, location, age or diagnosis. This could also guide pre-emptive planning by following the palliative phases and key processes such as recording advance care plans and conducting multidisciplinary case conferences.
Care planning needs to be proactive, and medication orders were a particular planning challenge for each of the provider groups:
Planning is really important thing in palliative care and we know that, but if you can’t get a doctor to give you any [medication] orders, and then all of a sudden someone crashes or deteriorates rapidly and you’ve got no orders, then that’s the really difficult time for us. (G5)
This was further compounded by the fact that some doctors were uncomfortable prescribing certain end-of-life medications before they were needed along with challenges of prescribing authority and the cost of particular palliative medications when used in community settings. Additional challenges included managing patient transfers and negotiating interstate and jurisdictional care. Tools (such as medication guidelines) may be applied within the model to aid familiarity and confidence with standard palliative processes and to guide provider practice.
Everyone identified a need for continuing education and training to enhance their knowledge and improve confidence. This may include knowledge about patient identification, understanding the different services available and their referral pathways, the confidence to manage a person’s care in the home, or the means for self-care. The National Palliative Care Strategy and the NSW Health Agency for Clinical Innovation’s Blueprint for Palliative and End-of-Life Care each identify the importance of enhanced awareness and understanding of providers regarding ‘dying, death, grief, and bereavement’2,9. Self-care, while important for all clinicians, was considered to be particularly important when caring for dying patients and their families:
Your client’s dying to begin with. Even though you go into the job knowing full well that’s going to happen, that is still confronting … (G9)
Self-care was essential when working in rural and remote communities because the patients and their families may be relatives, friends or colleagues, and negotiating that familiarity and grief is challenging21.
The Far West NSW Palliative and End-of-Life Model of Care
The mapping study was used to inform the implementation of this new model of care to support a patient-centred palliative approach to care in the region (Fig1). Before implementing the model, it was necessary to document the current connections between providers and identify where the model might build on the strength of existing networks and respond to gaps to improve capacity and capability for the consistent provision of a palliative approach across different providers and contexts.
While this is not the first model to endorse collaborative or integrated care, this is the first to explicitly include all generalist care providers within a region in order to establish a consistent palliative approach to care for anyone in need. The collaborative or integrated care with other known models is limited by provider, diagnosis, even age7,8,11. The model offers a consistent definition of palliative care and enables earlier identification for the effective application of a palliative approach in all healthcare settings, yet it is adaptable for the local context. Mapping the existing networks, resources and relationships proved invaluable to guide the implementation of the model, ensuring it was acceptable, fit for purpose and regionally responsive.
Conclusion
The implementation of a palliative approach, as with any service model, requires agreement and engagement across relevant healthcare organisations, services, and providers. Mapping and understanding the network of providers (and organisations) that support healthcare delivery before implementing new models of care will identify the existing strengths and gaps in the network. This knowledge will then support new and integrated connections that enhance the provision of care so that it is acceptable, fit for purpose and regionally responsive.
Acknowledgements
The authors thank and acknowledge the study participants and the Far West NSW Palliative and End-of-Life Care Steering Committee. The Broken Hill University Department of Rural Health is funded by the Australian Government Department of Health.


