Introduction
Headlines suggest a maternity care crisis in rural Australia, with figures showing a decline in rural general practitioners and specialists practising obstetrics, a decline in rural midwife numbers, and declining rural births1-3. These issues are compounded by increasing role diversity, as midwifery makes up a decreasing portion of rural midwives' work, and yet in small hospitals midwives have an increased likelihood of dealing with an obstetric crisis alone. One important counter to these pressures is Continuing Professional Development (CPD), as both a retention strategy4 and also a method for maintaining competence. All professionals are expected to perform competently, and despite disputes over evidence linking CPD to competence5,6, CPD programs are widely valued as a process for maintaining professional registration, education and practice by Australian and international health professionals.
CPD is a life-long professional development process which augments knowledge, skills and attitudes for the enhancement of professional practice. Involvement in CPD is still largely voluntary and unstructured for Australian midwives, although it is encouraged by organisations such as the Australian Nursing and Midwifery Council, and is implicit in most nursing and midwifery ongoing registration requirements. Frameworks to guide involvement in CPD activities are being developed worldwide because, without structured programs, health professionals can find it difficult to remain up-to-date with knowledge and skills7. It follows that an Australian CPD framework for midwives would assist them to engage in CPD effectively, resulting in an increased ability to maintain competence to practice and assisting retention rates4. This study aimed to inform the development of a CPD framework by exploring rural midwives' experiences and perceptions of CPD in context.
Research into CPD has predominantly focused on process outcomes8 and the levels and benefits of engagement in CPD by midwives and nurses. There are many acknowledged benefits for individuals, including increased confidence, enhanced career opportunities, a sense of achievement, and personal development, as well as collegial benefits of CPD such as the exchange of ideas and enhanced relationships with colleagues9,10. However, there are known access barriers for rural nurses wanting to participate in CPD. The more traditional forms of continuing education, with their focus on attendance at conferences and lectures present the greatest disadvantage to rural midwives because of distance from events, transport difficulties, a lack of funding, and lack of backfill staff11,12. Some of these issues, such as funding, are also matters requiring organisational support, which is an element of the general context of midwives CPD. Ellis13 argues that supportive practice environments are an important aspect of successful CPD.
Globally, there is a shift in focus from formal education to other forms of professional education, as educators realize that formal education does not ensure that individuals learn, and may not address individual learning needs in the context of a learning society14. Other forms of education such as self-education, situated learning, and informal learning15,16 place learning outside formal institutional contexts into a broader social and workplace environment, within communities of practice. By taking a broad view of CPD, a wide range of valuable informal education activities can be supported, such as: clinical attachments, reading journal articles, web-based learning, case debriefing, multi-professional activities, and mentoring. If broader approaches are adopted and the focus moves away from formal CPD education activities, the barriers of distance and cost could be minimized for rural midwives.
Because many existing CPD frameworks place the onus on the individual to meet requirements, it is surprising that there is a lack of information on midwives' views of CPD12,17. Using an individualized approach that does not acknowledge the effect of context or environment is also questionable13. Studies suggest nurses have a positive attitude towards ongoing learning18,19, and one study identified that for the rural nurse, family and supervisor support greatly influenced rates of participation12. However, generally little is known about Australian midwives' perceptions and involvement in CPD within the organisational context. Using a broader situated approach to CPD will require an examination of midwives' perspectives and experiences in context. As Australia moves towards a more defined and monitored CPD process for midwives this type of information is essential for the development of CPD programs and frameworks that allow rural midwives to access the benefits of CPD without long-distance travel to formal education activities.
Methods
A qualitative, inductive approach was used to explore rural midwives' understanding and experiences of CPD. The use of focus groups is particularly useful for gathering opinions, perceptions, attitudes and beliefs20. In addition, a discursive perspective identifies that focus group interactions will provide data that is developed in an interactive environment, and therefore provides a perspective that is negotiated and relevant for that context20,21. The resultant data are therefore the evaluated attitudes and perspectives of individual midwives emerging from group interactions.
Rigor and quality of the results were ensured by maintaining methodological congruence, using experienced moderators, and having two researchers analyse themes. All focus groups were facilitated by the same experienced moderator with the assistance of an experienced midwifery lecturer, and lasted between 90 and 120 min. Member checking was carried out during the focus groups, and the two members of the research team carried out post-session debriefs to discuss impressions, which added to the reliability of the data22.
Ethics approval was granted by the Southern Tasmanian Social Research Ethics Committee at the University of Tasmania. Written consent was obtained from midwives prior to data collection, and anonymity was assured. The focus groups were taped and transcribed; except for one group where technical problems with the tape recorder meant that the investigators had to rely on notes taken during the focus group. The focus group questions were designed to gain understanding of the perspective and involvement of Australian midwives in CPD and were developed from the relevant literature.
Participants
During 2004 a total of 52 midwives attended nine focus groups with a mean of six per group. The focus groups were conducted in three Australian states: Western Australia, Victoria and Tasmania. The study aimed to gather opinions from midwives working in different systems and localities, and therefore a purposive sampling framework identified target healthcare facilities that provided diversity in healthcare context: structures (four midwifery wards, three mixed specialty wards, and one group of independent midwives, public and private hospitals), town sizes (approximate population numbers ranged from 250 000 to 17 000 people), locality (three Australian states), and rurality (groups covered three of the five Accessibility/Remoteness Index of Australia [ARIA] classifications) were important elements of the sampling context. The ARIA23 rates all geographic locations in Australia on the basis of their remoteness by road from 201 service centres. In total, two focus groups were conducted in Very Remote locations, three in Accessible locations, and four in Highly Accessible locations.
Invitations for focus group participation were extended to all midwives at the selected sites, through the clinical educators. The focus groups were conducted in a suitable area within the workplace. Participants were self-selecting, which means it is likely that those most interested in CPD attended, providing some risk of selection bias. Participants were known to each other, which was unavoidable due to the rural locality, but this generally appeared to facilitate, not inhibit discussion. Most of the participant midwives had been practicing for 15-25 years, but a few were recently graduated (two were current students), and they held a diverse range of positions from midwifery students, midwives, ward managers, clinical educators, to site managers.
Data analysis
The data analysis used a two-step inductive approach. Data were coded into overarching themes, then sorted into sub-themes using the assistance of the NVivo (QSR Software, Durham, UK) computer software. Themes are presented in a table format for brevity (Table 1). There were many shared perceptions and concerns among focus group participants, and some issues that were particularly related to rural midwives emerged from the focus groups held in the Accessible and Very Remote locations. Content validity was supported because of the 'emergence of a substantively similar viewpoint on some issues over multiple focus groups ... in geographically dispersed areas'22 p.303.
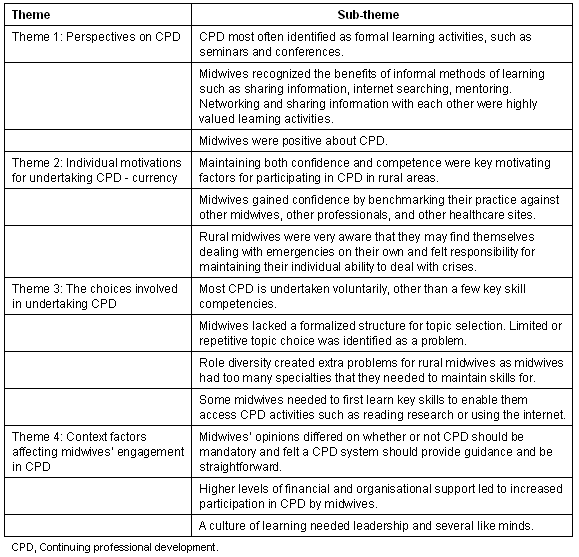
Table 1: Summary of themes and sub-themes from focus groups
Study limitations
While the data value lies in the rich and context specific perspective of rural midwives, it is not generalisable to the broader population. The specific context of the data must be kept in mind when interpreting the data. First, it is likely that, in the main, the views of those already committed to CPD were heard. Second, two groups had a possible power imbalance due to the presence of managers. This did not appear to inhibit participants, with some being quite outspoken. While the focus groups covered a diverse group of midwives with different CPD support structures and many of the findings are supported by literature, further research would be required to assess the generalisability of the results.
Results
The four key themes emerging from the data were: (i) midwives' views of CPD; (ii) their motivations for undertaking CPD; (iii) the choices they make around CPD; and (iv) how context factors facilitate their involvement in CPD (Table 1). These data have implications for the development of a CPD framework.
Most of the participating midwives discussed engagement in a wide-range of effective CPD activities, but most didn't recognize informal activities as CPD. The midwives clearly recognized the value of learning experiences outside the didactic seminar style, and especially valued collegial learning activities, such as networking and sharing information with each other. While the literature identifies a nursing preference for face-to-face learning24, many in this study considered that the opportunity to network was the major benefit of attending formal learning activities. This suggests that if cheaper networking alternatives, such as case debriefing and journal clubs, were resourced and supported at the organizational level, they may provide midwives with valuable learning experiences that could be available regularly and would not be limited by the barriers of distance or roster backfill.
The desire to retain confidence in skills has been previously identified as a major motivation for health professionals undertaking CPD18, and these findings support this. Most of the midwives acknowledged some responsibility for keeping up to date with practice, but the midwives in Very Remote and Accessible locations felt this very strongly. Isolation and limited capacity for back-up support from other health professionals gave rural midwives extra motivation to remain competent and ready for emergencies. The participants desired to provide quality care to birthing mothers, and to be able to cope with untoward events and complicated deliveries. The desire for quality had two aspects because rural midwives in our study worried that isolation could mean they were 'left behind', while many described a strong sense of pride that came from delivering good care. Their confidence in the quality of care was gained partly from informally benchmarking their own practice against that of other midwives, other organizations and other health professionals.
Debates continue about whether CPD should be completely based on individual needs, or more on job or role requirements25. The data from this study suggest that midwives selected CPD topics to meet individual needs and the needs of the job, but that planning was an overlooked aspect of CPD. The increasing diversity of rural midwives' practice created an additional difficulty in choosing CPD topics, and some midwives with multiple roles admitted that other less popular speciality areas, such as gerontology, were neglected due to their own lack of interest. The need for rural nurses to be 'multi-skilled generalists'26 has been noted in a number of studies. Rural midwives seem to be increasingly exposed to a multi-skilling trend. One example given was of a ward that catered for midwifery, paediatrics, level 2 nursery, general/medical/surgical and psychiatry. The diverse role requirements in such a situation suggest that effective planning and support for CPD activities is important in order to ensure that critical knowledge is maintained in all areas.
Despite some polarisation regarding the issue of mandatory CPD, most midwives agreed that a mandatory system should aim to assist 'reluctant CPD participants' to remain competent. In particular, midwives who had trained in the UK and had experienced a mandatory CPD system were strongly in favor of such methods. The same polarisation of opinion is evident in the literature, with some arguing that mandatory requirements may stifle the enjoyment of those who undertake CPD voluntarily27, while others argue that many practitioners need some form of incentive or motivation to undertake sufficient CPD28. These data provide some support for both positions, with midwives suggesting that for a mandatory system to gain wide acceptance it would need to be straightforward and flexible, and not create onerous monitoring and reporting requirements.
Our study noted a difference between university educated nurses and apprenticeship model nurses, who had had no exposure to university study, in their stated capacity to engage in less formal forms of CPD. Because many Australian rural nurses are older apprenticeship-trained nurses29, this suggests key study skills may be a special training need for this group. Assisting midwives to access online computers, and to access and understand recent evidence-based literature, should facilitate the use of cheaper but effective forms of learning.
These data also highlighted that midwives benefit from an environment that is supportive and encouraging of CPD. By being able to compare across three states and eight organisations, we observed that layers of support from the state to the unit level helped participation in CPD. Organisational factors, such as quarantined time, financial assistance, and leadership that demonstrated commitment to CPD were identified by midwives as facilitating their effective engagement in CPD. This finding matches that of other studies which have noted the benefits of organisational support24. Our study also found that some units benefited from strong leadership, peer support and enthusiasm for CPD. This, in hand with more structural support, appeared to generate a climate supportive of CPD, akin to communities of practice. The benefits of leadership support for assisting rural nurses' CPD engagement was also particularly noted by Beatty12. Communities of practice can create an environment where knowledge and skills are gained from everyday work experiences and group communications and conversations. This study supports the suggestion that a strong culture of CPD needs good leadership and peer-support. While in the past a major focus of continuing education has been on the need for individuals to take responsibility for ongoing learning, there is growing awareness in Australia that employers must support a culture of continuing education to retain qualified nursing staff29,30. Facilitating communities of practice, be they local or electronic, may provide new and promising avenues for rural midwives' engagement in CPD.
Conclusion
Within the globally evolving CPD environment it is important to understand how rural midwives view and participate in CPD activities. More importantly, in a climate of workforce shortages, it is critical to understand how midwives in rural areas can be supported to maintain competence. This study suggested that there could be both educational and financial benefits in broadening midwives' understanding of CPD, to emphasise the value of more informal and situated activities, such as support networks and mentoring. Planning forms an important stage in CPD activity, which was largely overlooked by the participants in this study. In a rural environment of increasing role diversity, we suggest that both midwives and health organisations need to systematically identify and prioritise learning needs.
Key skills are considered essential for success in education, employment, lifelong learning and personal development. The term 'key skills' is used within the UK health and education systems to describe six skills in particular that are important for ongoing engagement in CPD and lifelong learning: communication, numeracy, information technology, working with others, improving own learning and performance, and problems solving. Key skills are an important component of CPD because they increase midwives' capacities for undertaking less didactic style CPD activities. In our study, those midwives who had not completed any university level education were less likely to feel they had the skills for understanding evidence-based literature or for accessing electronic methods of CPD. Identifying and developing key skills should form an important part of CPD programs.
Finally, the context of practice is an important aspect of midwives' engagement in CPD. Systematic support for CPD appeared to be beneficial for the participants in this study, as did a supportive culture. Given the likely cost-benefits in terms of retention and quality care, rural health organisations and state level bodies are encouraged to take a bigger role in supporting CPD for rural midwives, particularly in the area of less didactic methods of CPD. Importantly, rural nurse managers need to understand the importance of leadership in facilitating a culture of ongoing learning.
Acknowledgements
The authors would like to thank the Australian Government Department of Health and Ageing for funding this research through the Development Program for Rural and Remote Midwives Extension Project.
References
1. Cole L. Fears obstetric crisis may spell end of bush babies. Medical Observer Weekly 2005; 25 February: 1-2.
2. Australian Medical Workforce Advisory Committee. The Specialist Obstetrics and Gynaecology Workforce - An Update 2003-2013. Report no. 2004.2. Sydney, NSW: AMWAC, 2004.
3. Tracy S, Barclay LPB. Contemporary Issues in the workforce and education of Australian midwives. Australian Health Review 2000; 23: 78-88.
4. Parliament of Australia. The patient profession: time for action. Report on the Inquiry into Nursing. (Online) 2002. Available: http://www.aph.gov.au/senate/committee/clac_ctte/nursing/report/contents.htm (Accessed June 15th).
5. du Boulay C. Continuing professional development: some new perspectives. Journal of Clinical Pathology 1999; 52: 162-164.
6. Grant J. Measurement of learning outcomes in continuing professional development. Journal of Continuing Education in the Health Professions 1999; 19: 214-221.
7. Crampton M, Wilkinson D. The professional development program of the Australian College of Rural and Remote Medicine. Australian Family Physician 2002; 31: 952-956.
8. Smith J, Topping A. Unpacking the 'value added' impact of continuing professional education: a multi-method cast study approach. Nurse Education Today 2001; 21: 341-349.
9. Andersson EP. Continuing education in Sweden-to what purpose? The Journal of Continuing Education in Nursing 2001; 2: 86-93.
10. Nolan M, Owen R, Curran M, Venables A. Reconceptualising the outcomes of continuing professional development. International Journal of Nursing Studies 2000; 37: 457-466.
11. Brodie P. Addressing the barriers to midwifery: Australian midwives speaking out. Australian Journal of Midwifery 2002; 15(3): 5-14.
12. Beatty RM. Continuing professional education, organizational support, and professional competence: dilemmas of rural nurses. The Journal of Continuing Education in Nursing 2001; 32: 203-209.
13. Ellis L, Nolan M. Illuminating continuing professional education: unpacking the black box. International Journal of Nursing Studies 2005; 42: 97-106.
14. Donen N. No to mandatory continuing medical education, yes to mandatory practice auditing and professional educational development. Canadian Medical Association Journal 1998; 158: 1044-1046.
15. Tennant M. Psychology and adult learning. London: Routledge, 1999.
16. Coffield F (Ed.). The necessity of informal learning. Bristol: The Policy Press, 2000.
17. Barriball KL, While AE, Norman IJ. Continuing professional education for qualified nurses: a review of the literature. Journal of Advanced Nursing 1992; 17: 1129-1140.
18. Apgar CJ. Factors that promote or deter trauma care nurses' participation in continuing professional education (Doctor of Education). 2001. Pennsylvania: The Pennsylvania State University.
19. Kersaitis C. Attitudes and participation of registered nurses in continuing professional education in New South Wales, Australia. The Journal of Continuing Education in Nursing 1997; 28: 135-139.
20. Puchta C, Potter J. Focus group practice. London: Sage, 2004.
21. Potter J, Wetherall M. Discourse and social psychology: beyond attitudes and behaviour. Beverly Hills: Sage Publication, 1987.
22. Kidd PS, Parshall MB. Getting the focus and the group: enhancing analytical rigor in focus group research. Qualitative Health Research 2000; 10: 293-308.
23. Department of Health and Aged Care. Measuring remoteness: Accessiblity /Remoteness Index of Australia (ARIA). Occassional Papers: New Series No. 14. Canberra: Commonwealth of Australia, 2001 October 2001.
24. Rosenberg JP, Canning DF. Palliative care by nurses in rural and remote practice. Australian Journal of Rural Health 2004; 12: 166-171.
25. Lawton S, Wimpenny P. Continuing professional development: a review. Nursing Standard 2003; 17(24): 41-44.
26. Kenny A, Duckett S. Educating for rural nursing practice. Journal of Advanced Nursing 2003; 44: 613-622.
27. Henwood S, Edie J, Flinton D, Simpson R. Continuing professional development - a re-examination of the facts. Radiography 1998; 4: 5-8.
28. Blaber C, Jordans R, Weyl E. Comparing the effectiveness of two methods of delivering continuing education to school nurses. Journal of Continuing Education in Nursing 1997; 28: 263-268.
29. Australian Institute Health Welfare. Nursing labour force 2001. (Online) 2001; Available: http://www.aihw.gov.au/publications/index.cfm?type=detail&id=8782 (Accessed 12th June 2005)
30. Heath P. Our duty of care: national review of nursing education. (Online) 2002; Available: http://www.dest.gov.au/highered/nursing/pubs/duty_of_care/default.html#Contents (Accessed 10th June 2005).

