Introduction
In rural areas the issue of access to, and quality of, health services has been a major cause for concern among rural dwellers1. Various strategies have been introduced by governments to assist in the development of health services and to solve access issues, one of the main strategies in recent times being the introduction of overseas trained doctors into rural communities. Yet it would seem that policy and political discourse concerning rural health, at least in the Australian context, relies on the disease model and fails to take adequate account of gender or the social experiences of rural women2,3.
This article presents data from a national survey of Australian rural women undertaken in 2004 to assess various quality-of-life indicators and issues relating to health service access. We argue that a feminist perspective is essential to understanding the health of rural women because it centralises the concerns of women. Without this, women's issues disappear into a more general overview of rural health disadvantage and a focus on individual pathology and the medical model.
Background
Why gender is important
Feminist theorising has enabled a focus on women and their experiences. Drawing on the distinction between sex and gender, feminists argue that while sex is biologically determined, gender identity is socially constructed through the societal expectations placed on men and women in a relational context4,5. The way rural women and men live their lives is shaped by gender constructions and discourses6-8 and, consequently, gender is a key determinant of health status2. Not only are women the most frequent users of health services, their often broader conceptualisation of health and wellbeing is framed by their biological role (for example in pregnancy), and their social or gendered roles (for example in caring)9,10. At the same time, women are more likely to take responsibility for the health of those closest to them, in the process often ignoring their own health status1. While a feminist perspective allows an exposure of these issues, it also enables a focus on the way health care and provision of health services is gendered. Thus, a feminist perspective provides a challenge to both medical discourse and the premises on which it is based10.
The women's health movement developed as a response to the 'ideological and practical deficiencies within the medical approach to women's health care'10, and pointed to ways the medical model has acted to reduce women's power around health decision-making11. The women's health movement allows an analysis of the way women's health is affected by social factors such as limited job opportunities, lack of public transport and other services, family transience and social isolation12. A failure to address these issues in relation to health results in a lack of attention to women's own health priorities. As Hunt11 notes, mainstream health servicing 'rarely addresses quality of life issues and seldom accounts for difference in opportunity deriving from the social context of people's lives'. When we consider the Australian rural condition, this failure is a significant one1.
Rural health
Rural Australia is as diverse geographically, economically and socially as urban Australia12. Nonetheless it is clear that health inequalities between rural and urban areas are significant - rural Australians have poorer health and less access to services than urban Australians, and lower life expectancies and higher disability rates13. Further, because socio-economic measures such as education, employment and the quality of the physical and social environment determine health status14, rural people in general are particularly disadvantaged. In fact, the Australian Institute of Health and Welfare notes that health status decreases as distance from metropolitan areas increases15. Indigenous Australians living in rural Australia have the poorest health of any rural dwellers, indicated by lower life expectancies, higher rates of hospital admissions, and higher rates of health problems such as diabetes and ear infections16.
Health risk factors such as smoking, drinking and environmental dangers are more prevalent in rural areas2 with the result that there are some health problems, including injury (incorporating farm accidents), asthma and diabetes that are more prevalent in rural areas15. Additionally, the poor quality of roads, lack of public transport and length of time to get to treatment compromises treatment options.
Despite the clear evidence of reduced rates of health and wellbeing in rural areas, services are clearly lacking to meet the need, and those that are available are often inadequately funded2,17. Areas that are relatively inaccessible and have small populations are more likely to have limited services and a poor standard of facilities14. Problems with rural health service delivery include limited funds for services, a lack of access to specialist services, and, where travel to services is the only alternative, a lack of access to public transport or affordable private transport12,17. While access to specialists is a critical issue for most rural Australians, access to GPs is also problematic18. Australian Bureau of Statistics figures reveal that the number of doctors per head of population varies from 308 per 100 000 in major cities to 77 per 100 000 in very remote areas, creating further problems related to access and transport19. In addition, access is complicated by cost, with GPs far less likely to bulk bill in rural areas making out of pocket expenses higher for rural people20. (Bulk-billing refers to the Australian practice of doctors providing a medical service at no cost to the patient).
Further complications for rural health provision arise from the imposition of corporate values on funding allocations, a lack of revenue from smaller populations, a lack of consensus on what is adequate health servicing, the application of urban strategies to rural health provision, and a lack of research on rural health17,21.
Rural women's health
We have demonstrated that there is widespread evidence that rural Australians suffer disadvantage in relation to health and infirmity. Adopting a feminist perspective, where women are centralised and gender is a key analytical construct, may allow a more searching appraisal of rural health disadvantage and a broader understanding of the emotional, social and spiritual wellbeing of rural Australian women.
Masculine hegemony is dominant in small town rural Australia with men controlling significant sites of power as well as the resources on which rural industries are based7,22. The stereotypical view of rural women is that they are stoical, used to adversity and self-reliant2. As overseers of the family's finances, education and general wellbeing, women see themselves as responsible for caring for those family members who are ill or in need of care, often to the detriment of their own health1,2,9,23. Rural women's health status is likely to differ depending on where they live and according to their environment, and their ability to access support, information and services24. Further, women are more likely to discuss broader issues relating to health such as isolation, availability of transport, child care and counselling1.
Women's health status may vary by age. For example, the ageing of the rural population, and the dominance of women in the older rural age groups, suggests that specific aged care needs of this group will become problematic in future25. Additional issues surround mid-life women who are often too busy to travel to access services for their own health and wellbeing1,26, while younger women needing access to ante- and post-natal health services, and adolescent women with an unplanned pregnancy face their own particular health issues27.
Drought
During much of the 2000s, vast areas of rural landscape have been devastated by drought conditions28. For those rural Australians dependent on agriculture, the resulting stresses have been significant1. Women report their wellbeing is compromised by the additional stresses associated with loss of income, increased workloads both on and off farms, issues relating to the health and welfare of family members, caring for others who are themselves stressed, a lack of income thereby reducing options to get away, and barriers to health service access including transport difficulties, a lack of bulk-billing and the need to travel1. For many women in rural areas, the drought has come on top of existing problems of health service availability and access. It is in this context that the study on which this article is based took place.
Methods
Members of the Gender, Women and Social Policy Community of Scholars (COS) undertook to assess issues of importance to rural women in areas served by Charles Sturt University (CSU) (the Central West and Riverina areas of New South Wales). The rationale was to develop a research agenda for the group that was grounded in local area issues. A series of qualitative focus groups were held in Wagga Wagga, Bathurst and Cowra with women in key service or representative positions. These focus groups generated similar but extensive issues, many of which related to health and wellbeing indicators and service access. So strong was the feeling in the groups about declining access to health care services that the COS group felt the need to test these issues more widely.
Initially a small CSU grant was obtained to conduct a quantitative survey through randomised telephone surveys in the CSU catchment area, testing wellbeing and access issues. Members of the group who conducted the telephone interviews were overwhelmed with the response by women about their lack of access to critical services, including basic maternity and aged care. After 70 telephone interviews were completed, the group sought further funding to extend the survey.
The National Rural Women's Coalition (NRWC) was successfully approached for additional funding. The member organisations of the NRWC include the Local Government Women's Association, Australian Women in Agriculture, Country Women's Association, the Foundation for Australian Agricultural Women, the National Rural Health Alliance, the Rural Doctor's Association - Female Doctor's Group, Women's Industry Network Seafood Community and an Indigenous Women's representative. Because of budgetary constraints a decision was made to conduct the national survey by mail. The survey (Appendix I) sought information on personal factors such as age, marital and work status, whether services are difficult to access and whether they are adequate. Over 1500 paper-based surveys were distributed through the women's groups represented by the NRWC and two of the groups put the survey on their members-only websites. It is difficult to assess a response rate because of the web-based element of the survey, however 820 returned surveys were received by the cut-off date in October (and several more trickled in for an additional 3 months) suggesting a response rate of 50%. This article reports on the national mailed survey only.
Limitations
There is no claim that this group is representative of all rural women, and the survey results reflect this with a bias to women over 40 years who are married and working. There is also a bias to women in organisations, women who are literate and women with internet access. The survey administration method also made determination of a precise response rate difficult. These factors reduce the generalisability of this study. There is also no comparative urban data, nor comparison with the views of rural men. These could be opportunities for further study. Nonetheless, it was apparent that the issue of rural health service access touched a nerve with rural women and the responses often included extensive hand-written comments.
Results
Demographics
Eight hundred and twenty women responded to the survey, 98% (790) of whom had English as their first language, and less than 2% of whom identified as Indigenous (1.1% [9] Aboriginal, 0.2% [2] Torres Strait Islander and 0.4% [3] both). Most respondents were living with their husband (73% or 585) or a male partner (6% or 45), 0.5% (4) were living with their female partner, 4% (32) were divorced, 5% (42) widowed, 3% (26) separated and 8% (67) were single. Figure 1 illustrates the states where respondents resided indicating that while NSW respondents dominated, the survey was completed by a significant number of people across the other states. Figure 2 indicates age levels of respondents suggesting a bias to mid-life women.
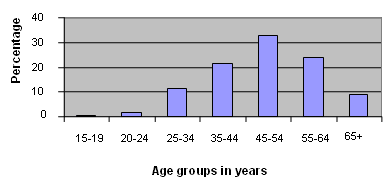
Figure 1: Australian home states of respondents.
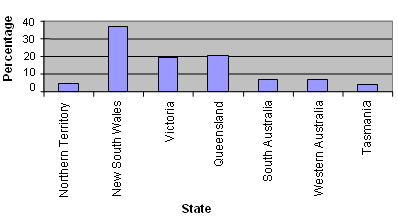
Figure 2: Age of respondents.
Indicating that rural women are entering the workforce in large numbers, 79% of our respondents were in paid work (51% of these full-time). A further 10% were looking for work at the time they completed the survey.
Level of general wellbeing
Respondents were asked to comment on their level of wellbeing and on things that would improve, or have hindered, their wellbeing. Fifty-five percent of respondents felt their level of wellbeing was excellent while 25% felt it was poor. Things that would improve levels of wellbeing can be summarised into the following categories: less stress and more time; better working conditions; better financial circumstances; a breaking of the drought; greater access to health, mental health, welfare and telecommunications services; more access to leisure facilities and time; better relationships and a holiday. A significant number noted the drought conditions caused stress, relationship difficulties and an increased need for women to work.
Things that hindered wellbeing fall into the following categories: family relationship problems; health factors; high costs/low income; the drought; being tired; having no time for leisure; being overworked; losing services; distance to facilities; being overweight/having poor diet; lack of exercise; having no time. Asked to comment on what might make the biggest difference to wellbeing right now, 33% nominated money, 23% health, 27% less work and 2% more work.
Access to services
Respondents were asked to comment on access to a range of listed services. Table 1 shows the percentages of respondents who had difficulty accessing the listed services.
Table 1: Access to services
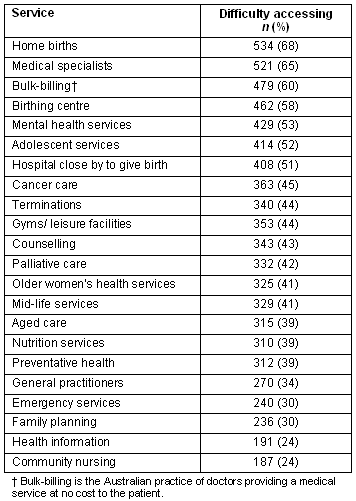
Respondents were also asked for open-ended qualitative responses on the most available, and the least available health services in their area. Respondents were given the option of nominating four services in each category. Tables 2 and 3 summarise these responses. Note that not all respondents chose to nominate four options so percentages listed in the tables are based on the respondents who did choose to address the particular question not the total sample.
Table 2: Most available services
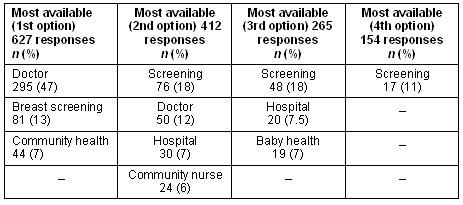
Table 3: Least available services

These qualitative responses indicate that the main focus of health care for respondents is general practitioner basic medical services. By contrast, women noted in their qualitative responses that the least available services are in areas of birthing, mental health, women's health, and counselling. Women also noted the lack of aged care, women's health services and domestic violence services.
Service adequacy
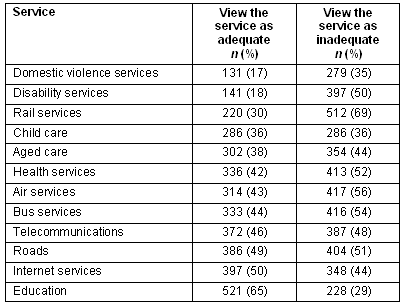
While service access was difficult for many women, service adequacy was also problematic. Table 4 indicates the percentages of women who view their services as adequate and inadequate. Not all women responded to this question and the authors are unsure whether they did not know or chose not to respond to these questions.
Table 4: Adequacy of services available in local area
Private health insurance
Respondents were asked to comment on the cost-effectiveness of their holding private health insurance and 52% (405) felt that private health insurance is not cost effective in rural areas because, as they indicated, of a lack of services.
Travelling for health service access
Two-thirds (66% or 525) of respondents noted that they needed to travel to a regional centre for health services, and yet 84% (664) noted that public transport was not available to travel to this centre. Asked to comment on the issues this raises, 65% (349) noted the additional costs associated with travel, accommodation and loss of work time, 15% (79) noted the problems associated with child care and 82% (435) noted the additional burden of travel. A further 37% (194) noted other issues, including the need to find accommodation, needing to take leave, being away from home, the time factor involved and tiredness.
Caring and support
Respondents were asked to nominate their caring roles. A significant percentage of the respondents were carers with 38% (306) caring for a child/children, 16% (131) for an aged person, 10% (78) for someone with a disability and 6% (52) for someone with other special needs. Despite their caring roles, 31% (95) of carers noted it was not easy to gain information on caring, 50% (154) that it was not easy finding resources to assist with caring, 48% (149) that it was not easy to find emergency assistance and 51% (153) that they could not access respite.
Respondents were asked to comment on personal support available to them in their areas. Half (50% or 386) noted that they had extended family in their local area. Nonetheless, only 32% (246) felt there was adequate support for mothers in their area, and only 40% (311) noted that they had assistance with housework from someone in their household.
Discussion
While there is no claim that this study reflects the views of all rural women, it does extend our understanding of health service access for rural Australians. The women who responded were from across Australia, suggesting that rural health disadvantage and a lack of attention to rural women's health is endemic. Using a feminist analysis to expose issues of relevance to women, this study suggests that rural health service provision is focused on the medical model of care in its approach to rural health disadvantage. First, it is clear that there is a general paucity of health and wellbeing services; second, women respondents see health servicing as extending far beyond the primary health care provided by doctors; third, women responding to this survey note the lack of support for women/mothers/carers in rural Australia; and services dealing with issues relating specifically to women's health and wellbeing, such as maternity services, mental health services, care and respite services and domestic violence services are clearly lacking.
There is no doubt that both women and men receive inadequate service support, and this article is not attempting to overshadow this obvious fact. However, in undertaking an analysis focused on women's concerns, we note that the rural services that are available are focused on primary health care and not on the services needed to ensure the health and wellbeing of women. Our analysis revealed that there are not enough critical services for women - there are few birthing services, no model that supports homebirths and no attempt to address the issue of distance so that women do not have to travel so much for services. Following publicity of our results in media interviews, women have come forward in the media revealing horror stories about their experiences in childbirth - long trips in labour on dangerous roads, being turned away by local hospitals or being forced to leave their communities and families for several weeks around the time of their labour (see, for example, Daily Telegraph, 6 October 2004, p.1). Fifty-one percent of our respondents noted there was no hospital in their local area where women can give birth. Yet even in the area of primary care, it would appear that services are lacking with 34% noting they have limited access to GPs, 65% limited access to specialists, and 60% not having access to bulk-billing.
By focusing on primary health care as the sole issue relating to rural health disadvantage, policy makers may be overlooking the problems arising in relation to service access including limited attempts to develop new models of care that provide women with safe, affordable and adequate access to a variety of care services.
Conclusion
This study revealed that a focus on primary health care servicing to rural areas may be overshadowing the needs of women for a variety of additional services. The lack of safe, affordable and adequate services in a variety of areas continues to put women's health, and that of their families, at risk in rural areas. This study revealed the need for a wider conceptualisation of health care in rural areas and the need to consider the health concerns of rural women.
References
1. Alston M, Kent J. The social impacts of drought. Wagga Wagga, NSW: Centre for Rural Social Research, Charles Sturt University, 2004.
2. Smith JD. Australia's rural and remote health: a social justice perspective. Melbourne: Tertiary Press, 2004.
3. Allan J. Rural Women's Health Project: Health Women, Healthy Communities. A review of literature. In: M Alston. Gender, women and social policy community of scholars. Report to the National Rural Women's Coalition. Wagga Wagga, NSW: Centre for Rural Social Research, 2004.
4. Wharton A. The sociology of gender: an introduction to theory and research. Boston, MA: Blackwell Publishing, 2005.
5. Wearing B. The pain and pleasure of difference. Melbourne: Longman Australia, 1996.
6. Alston M. Women on the land: the hidden heart of rural Australia. Sydney: University of NSW Press, 1995.
7. Alston M. Breaking through the grass ceiling: women, power and leadership in rural organisations. Amsterdam: Harwood Publishers, 2000.
8. Leipins R. Making men: the construction and representation of agriculture-based masculinities in Australia and New Zealand. Rural Sociology 2000; 65: 605-619.
9. Lee C. What Women's Health Australia can tell us about women's well-being in the bush. Proceedings, The art and science of healthy community - sharing the country know-how. 7th National Rural Health Conference, 3-4 March 2003 Hobart, Tas. (Online) 2003. National Rural Health Alliance. Available: http://www.nrha.net.au/nrhapublic/publicdocs/conferences/7thNRHC/Papers.htm (Accessed 23 August 2005).
10. Rogers-Clark C. Women and health. In: A Smith, C Rogers-Clark (Eds). Women's health: a primary health care approach. Sydney: MacLennan & Petty, 1998; 1-18.
11. Hunt, L. Primary health care for women: An evolving speciality. In: A Smith, C Rogers-Clark (Eds). Women's health: a primary health care approach. Sydney: MacLennan & Petty, 1998; 278-291.
12. Warner-Smith P. and Brown P. It's time to play a bit: mid-age rural women's leisure and well-being. In: Proceedings, The art and science of healthy community - sharing the country know-how. 7th National Rural Health Conference, 3-4 March 2003, Hobart, Tas: (Online) 2003. National Rural Health Alliance. Available: http://www.nrha.net.au/nrhapublic/publicdocs/conferences/7thNRHC/Papers.htm (accessed 23 August 2005).
13. Brown M. Health-care choices - the right of all Australians. Rural and Remote Health 2: 162. (Online) 2002. Available: http://rrh.org.au(Accessed 23 August 2005).
14. Ryan-Nicholls KD. Health and sustainability of rural communities. Rural and Remote Health 4: 242. (Online) 2004 http://rrh.org.au (Accessed 23 August 2005).
15. Welch N. Understanding of the determinants of rural health (Online) 2000. Available: http://www.ruralhealth.org.au/nrhapublic/publicdocs/others/03_welch_00.pdf (Accessed 23 August 2005).
16. SCRGSP (Steering Committee for the Review of Government Service Provision). Overcoming Indigenous disadvantage: key indicators 2003. Canberra: Productivity Commission, 2003.
17. Worley PS. Good health to rural communities? Rural and Remote Health 4: 292. (Online) 2004. Available: http://rrh.org.au (Accessed 2005 August).
18. Boffa J. Is there a doctor in the house?. Australian and New Zealand Journal of Public Health 2000; 26: 301-304.
19. Australian Bureau of Statistics. Australian social trends. Canberra: Commonwealth of Australia, 2003.
20. Young AF, Dobson AJ. The decline in bulk-billing and increase in out-of-pocket costs for general practice consultations in rural areas of Australia, 1995-2001. Medical Journal of Australia 2003; 178: 122-126.
21. Rankin SL, Hughes-Anderson W, House J et al. Rural residents' utilisation of health and visiting specialist health services. Rural and Remote Health 2: 119. (Online) 2002. http://rrh.org.au (Accessed 23 August 2005).
22. Campbell H. The glass phallus: pub(lic) masculinity and drinking in rural New Zealand. Rural Sociology 2000; 4: 562-581.
23. Heron, C. Working with carers. London: Jessica Kingsley, 1998.
24. Stehlik, D. 'Out there': places, spaces and border crossings. In: S Lockie, L Bourke (Eds). Rurality bites: the social and environmental transformation of rural Australia. Sydney: Pluto Press, 2001; 30-41.
25. de la Rue M. and Coulson I. The meaning of health and well-being: voices from older rural women. Rural and Remote Health 3: 192. (Online) 2003. Available: http://rrh.org.au (Accessed 23 August 2005).
26. Brown WJ, Young AF, Byles, JE. Tyranny of distance? The health of mid-age women living in five geographical areas of Australia. Australian Journal of Rural Health 1999; 7: 148-154.
27. Thomson J. The health of rural and remote area women. In: A Smith, C Rogers-Clark (Eds). Women's health: a primary health care approach. Sydney: MacLennan & Petty, 1998; 110-119.
28. Botterill L, Fisher M (Eds). Beyond drought: people, policy and perspectives Melbourne: CSIRO, 2003.
Abstract
Access to health services in rural Australia has been particularly problematic because of the vast geographical areas and the sparse population distribution across the inland. The focus on health servicing has been very much on primary health care with most attention being giving to the distribution of doctors in rural Australia. This study takes a closer look at rural health servicing through the eyes of women in rural Australia. Drawing on a survey of 820 women, the study revealed that a focus on primary health care may be resulting in a lack of attention to women's health in areas, such as maternity models of care, domestic violence and mental health. The study also reveals the disquiet of Australian rural women at the poor state of health services.
Key words: access, women's health.





