Introduction
Drug therapy is the most commonly used method of any disease treatment in general practice. However, the patterns of drug prescribing are often inappropriate1,2 and the need for registration of these patterns is essential in an effort to improve prescribing standards3.
General practice databases have been used as an effective method for pharmacoepidemiological research4. Sales statistics also provide useful information, but have some limitations, such as the absence of information for age, sex and the disease of the patient5.
There are only a few publications on the subject of the use of drugs available in Greece6,7, a country where general practice is seeking academic recognition8. Searching the literature, we found only a few publications for studies in rural areas over the last 10 years9-11. Differences between rural and urban areas have previously been reported10,11. Research on pharmacoepidemiology that helps the development of quality control programs in general practice and makes a substantial contribution to the formulation of guidelines for the proper use of drugs5,12 seems to be an obvious need and challenge for Greek rural practitioners. Thus, it was important to carry out a study on prescribing patterns in a rural primary health care area in Crete, Greece. This study reports on the prescribing patterns in a rural Primary Health Care (PHC) area and discusses the findings with the broad aim of identifying areas for practice improvement.
Methods
Setting
The project, which was known as the Anogia Prescription Study (APS), was carried out in the Anogia Health Centre in rural Crete. The catchment area is a mountainous district consisting of 11 villages with a population of approximately 9000 inhabitants. Children comprised 24.1% of the total population and seniors 19.0%13. Eight physicians served the population.
Design
The APS was a prospective study, with a pre-selected sample of 1000 prescriptions. It was initiated in January 1999 and was completed in December 1999.
Data recorded
For each prescription, the participating physicians were invited to make a copy and to fill out a pre-tested questionnaire with supplementary information about the prescription. The selected information included first, information from the prescription (name, diagnosis, date, drugs, dosage) and second, supplementary information from the questionnaire (age, sex, prescription through a third person's intervention, renewal of an old prescription etc). The total number of prescriptions issued in the studied year was approximately 20 000. The first out of twenty consecutive issued prescriptions per physician was pre-selected (total number 1000 prescriptions included). Drugs were classified according to the International Classification of Primary Health Care-drugs (ICPC-drugs)14. Diagnoses were coded according to the International Classification of Primary Health Care (ICPC-2)14.
Statistical analysis
The Mann-Whitney-U test was used for comparison of the patients' average age. Because the population's age profile was clearly skewed, the 95% Confidence Interval (CI) was estimated for the median value of patients' ages15. Statistical analysis was undertaken using MedCalc, ver. 7.3.0.1 (MedCalc Software; Belgium).
Results
The sample consisted of 1000 subjects (384 male and 616 female patients; Fig 1). The age distribution of the population of patients was as follows: age group 0-14 years: 5.7%, age group 15-64 years: 30.7% and age group 65+ years: 63.6%. The median age of the patients was 71.0 (95% CI: 70.0-72.0) years. The median age of male patients was 72.0 (95% CI: 69.0-74.0) years, while for female patients the median age was 70.0 (95% CI: 69.0-72.0) years. Male and female patients did not differ statistically significantly in terms of average age (p = 0.401).
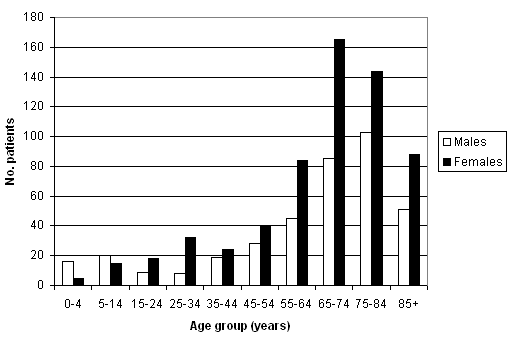
Figure 1: Age and sex distribution of the patients in the Anogia Prescription Study.
Table 1 shows the diagnoses related to the prescriptions after coding according to the ICPC-2. The total number of diagnoses was 1095 because some prescriptions had more than one diagnosis. Diseases of the circulatory, respiratory and musculoskeletal systems were the most commonly recorded, with 605 (55.2% of the total) diagnoses being recorded on the prescriptions of the study. Table 2 shows the ten most commonly recorded diagnoses for male and female patients. These constituted approximately 54.2% of all diagnoses for male and 47% for female patients. Hypertension, infections of the respiratory tract, and ischaemic heart disease were the most commonly recorded diseases for both males and females, which accounted for 32.7% of male and 23.1% of female diagnoses. Table 3 shows the 10 most frequently prescribed substances. Paracetamol, furosemide, and some antibiotics were the most commonly prescribed drugs for both sexes.
Table 1: The registered diagnoses (ICPC-2 coding)
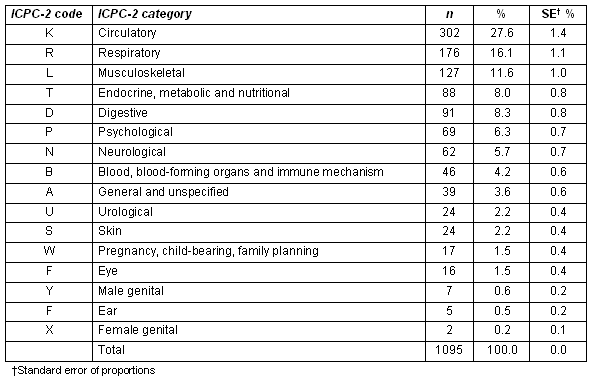
Table 2: The 10 most frequently recorded diagnoses for males and females (ICPC-2 coding)
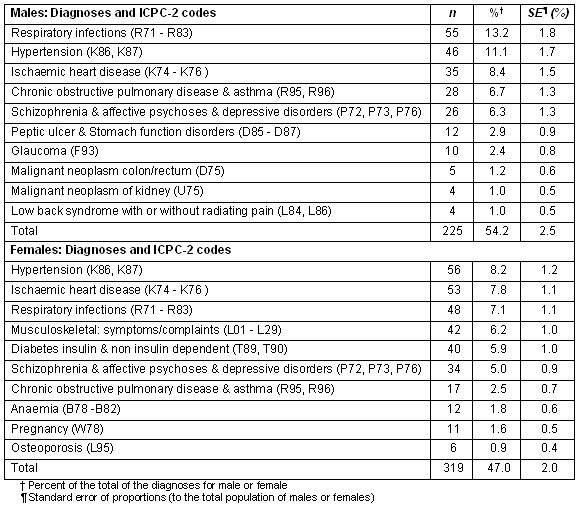
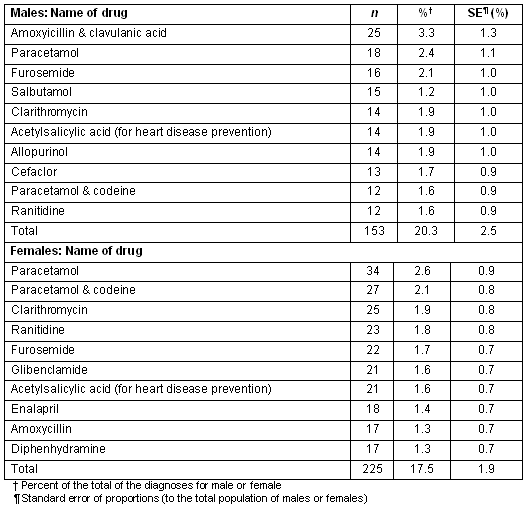
Table 3: The 10 most frequently prescribed drugs for males and females
Analysis of the questionnaires revealed that, for more than 51% of cases, patients were visiting their physicians only to ask for a prescription. Prescriptions were requested through a third person's intervention in 354 (35.4%) cases. Males were 120 (33.9%) and females 234 (66.1%). The most common diagnoses of these patients were those of cardiovascular system diseases (26.5%), respiratory system diseases (13.1%) and metabolic disorders (11.1%). The average age of patients who requested prescriptions through the intervention of a third person was significantly higher than the patients who requested directly from the health centre, when median values were compared (74.0 with 95% CI 73.0 to 75.0, against 69.0 with 95% CI 67.0 to 71.0, p<0.001).
The number of drugs per prescription was close to 2 (1.96 for males and 2 for females). The distribution of the drugs in 'ICPC-drug' categories is presented (Fig 2). All patients with more than four drugs on a single prescription were older than 50 years. Figure 3 shows an increase of drug numbers per prescription for older patients. This increase concerns the total of the patients and each gender separately. Prescriptions that were a renewal of a previous one were 68.9% of the same total.
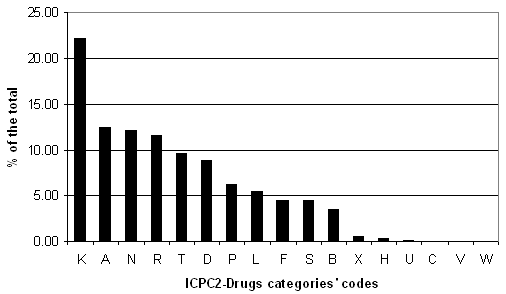
Figure 2: The distribution of the prescribing drugs of APS (ICPC-Drug coding). K: Cardiovascular system; A: general anti-infectives systemic; N: central nervous system; R: respiratory system; T: metabolism; D: alimentary tract; P: psychopharmaceuticals; L: musculoskeletal system; F: ophthalmologicals; S: dermatologicals; B: blood and blood-forming organs; X: gynaecological and sex hormones (excl. contraceptives: W1); H: otologicals; U: urologicals; C: antitumoral therapy; V: various; W: contraceptives and sex hormones.
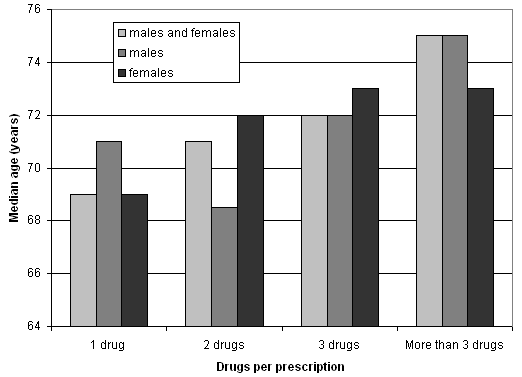
Figure 3. Patients' ages and drugs per prescription
Discussion
Some methodological considerations should be discussed prior to the interpretation of the findings. Potentially, a selection bias may have been introduced. However, the selection was made from the whole area of the health center and from the general population. We may assume that the study sample reflects the prescribing patterns in the area, because it was selected from the total of all prescriptions from that year16. The structure of the studied population differed from the rural population of Greece. The aging ratio (the ratio of the population 65+ to 0-14 population) in Anogia region was lower than in Greece as a total (0.97 against 1.10) and even lower than the aging rate in rural Greece (0.97 against 1.39)13. Therefore, some of our findings, for example prescribing through the intervention of a third person, may possibly be different from other Greek areas.
Some findings of this study may offer new information when researchers look for evidence in explaining national and regional differences in prescribing and drugs consumption. An important finding of the study is the high number of drugs per prescription. It was higher than others previously reported5,17. The advanced age of our study sample may explain this finding, while different attitudes towards drug therapy, both among doctors and patients, may contribute to it. The high prevalence of prescribing for the elderly and particularly among females is in agreement with the findings of other authors5,17,18. The possible reason for such findings may well reside in the fact that the female population visits their GP more frequently than the male18,19. The fact that the number of drugs per single prescription has increased proportionally with each age group corresponds well with the findings of previous reports20,21. It can be ascribed to multiple morbidity and the severity of disease, more than to irresponsible prescribing22.
The finding that the half of the subjects were visiting their physician only for a prescription has been reported in other Greek studies and it deserves further discussion23 when quality of care is at the top of health authorities' agenda24.
Hypertension was the most common diagnosis for drug prescribing for females, and the second most common diagnosis in males. This is in agreement with the reports of other studies that have shown that the most common diseases in PHC in Europe are similar to those in the APS14. Insomnia was not included in the ten most frequently recorded diagnoses of our study, while it is reported that insomnia is the most common diagnosis for drug prescribing in Norway5,25. The cause for this may be the difference in climates. It also may be the use of simple guidelines for the management of the insomnia in the Anogia's area. Studies with similar methodology are not available in the literature, thus we were not able to discuss these findings within the southern European setting. However, it seems that the prevalence of insomnia in Italy is also lower in comparison with Scandinavian countries26.
Hypertension, respiratory infections, ischaemic heart disease, chronic obstructive pulmonary disease, asthma, and mental disorders were the most common recorded diagnoses in both the APS and a Norwegian study5. We would like to point out that diabetes mellitus was the fifth most common diagnosis in APS and a high prevalence of diabetes mellitus has been previously reported in rural Crete27. In the APS, the diagnoses 'pregnancy' was very common (Table 2), in contrast with the Norwegian study in which this diagnosis was absent5. In addition, the diagnosis 'oral contraceptive' was absent from the APS, but in Norway, the Netherlands, and Belgium these drugs were of the most commonly prescribed14. The finding of the high prevalence of the diagnoses 'pregnancy' may be explained by the high birthrate of the Anogia Health Centre area13. The absence of oral contraceptives from APS may be due to the fact that only a small number of women in Greece use contraceptive drugs28, and because the prescribing is performed by gynecologists and not by GPs.
Another interesting finding of our study was that benzodiazepines were absent from the ten most frequently prescribed drugs for males and females, while diazepam was found to be the most common drug prescribed for females, and the third highest for males in the Norwegian study5. The lower prevalence of the diagnoses of anxiety, depression, and insomnia in prescriptions of the APS, may have an impact on the absence of benzodiazepine prescribing from the commonly used drugs in this study.
The large consumption of antibiotics in Greece is a well known public health problem29, and the results of this have already been highlighted30. Amoxicillin with clavulanic acid, and clarithromycin were used very frequently in the Anogia Health Centre area (Table 3). Most Mediterranean countries report similar patterns for antibiotic prescribing, and it is supported that the number of daily doses strongly influences the prescription of these medications31.
Our study findings may help in identifying some areas of potentially non-rationally prescribed drugs. Furosemide is a good example. Furosemide was in the 10 most frequently prescribed drugs in the APS and in the top 20 most frequently prescribed drugs of the Norwegian study5. We found that in most prescriptions for furosemide (92.4%) the diagnosis was, indeed, heart failure. Further study of these patients' medical histories showed that, in some cases, the use of furosemide was not necessary (first stage of heart failure, oedema from venous insufficiency etc). An algorithm for the use of furosemide in our area may be helpful.
Another finding was the high proportion of patients who sought a prescription through the intervention of a third person (usually their neighbour or the receptionist of the health center). In the APS, more than one in every three prescriptions was prescribed through third-person contact. In another Norwegian study, 48.1% of contacts with GPs for prescriptions were made by a third party on behalf of the patient32. This unusual finding certainly needs further investigation. Although aging and geographical remoteness may partly explain this, it is uncertain, based on the results of this study, to what extent cultural and sub-cultural characteristics have a potential impact on patient's behavior. We found that patients who were requesting prescriptions through a third person were older in comparison with patients who were presenting directly to the Anogia Health Centre.
Conclusion
This is the first published study of prescribing patterns in this rural region of Greece. Although there were some similarities with other studies, the differences showed that region-specific data is crucial for practitioners and policy-makers in rural health services. In conjunction with the permanent registration of the prescription patterns, the formulation of practical guidelines on the drugs most often prescribed, and the use of medical audit procedures, are anticipated to improve the primary-care physicians' practices and quality of care in rural primary care.
References
1. Stanton LA, Peterson GM, Rumble RH, Cooper GM, Polack AE. Drug-related admissions to an Australian hospital. Journal of Clinical Pharmacy and Therapeutics 1994; 19: 341-347.
2. Lesar TS, Briceland L, Stein DS. Factors related to errors in medication prescribing. JAMA 1997; 277: 341-342.
3. Figueiras A, Sastre I, Tato F et al. One-to-one versus group sessions to improve prescription in primary care: a pragmatic randomized controlled trial. Medical Care 2001; 2: 158-167.
4. Skegg DC. Pitfalls on pharmacoepidemiology. BMJ 2000; 321: 1171-1172.
5. Rokstad K, Straand J, Fugelli P. General practitioners' drug prescribing practice and diagnoses for Prescribing: The Mre & Romsdal prescription study. Journal of Clinical Epidemiology 1997; 50: 485-494.
6. Kafatos A. Prescribed medication and nutrition of social care patients in Crete, Greece. Public Health 1996; 110: 361-367.
7. Tzimis L, Katsantonis N, Leledaki A, Vasilomanolakis K, Kafatos A. Antibiotics prescriptions for indigent patients in primary care. Journal of Clinical Pharmacy and Therapeutics 1997; 22: 227-235.
8. Lionis C, Carelli F, Soler JK. Developing academic careers in family medicine within the Mediterranean setting. Family Practice 2004; 21: 477-478.
9. Bernardez M, Puche E, Martinez B, Garcia Morillas M, Luna JD. A long-term pharmacoepidemiological study on drug dispensing by the pharmacy office in rural primary care. The influence of age and sex. Atencion Primaria 1997; 19: 7-11.
10. Craig D, Passmore AP, Fullerton KJ et al. Factors influencing prescription of CNS medications in different elderly populations. Pharmacoepidemiology and Drug Safety 2003; 12: 383-387.
11. Dineshkumar B, Raghuram TC, Radhaiah G, Krishnaswamy K. Profile of drug use in urban and rural India. PharmacoEconomics 1995; 7: 332-346.
12. Dukes G, Lunde PKM, Melander A et al. Clinical pharmacology and primary health care in Europe - A gap to bridge. European Journal of Clinical Pharmacology 1990; 38: 315-318.
13. Census 2001. General secretarial of national statistical service of Greece. (Online) 2001. Available: http://www.statistics.gr/Main_eng.asp (Accessed 25 January 2006).
14. Lamberts H, Wood M, Hofmans-Okkes I. The International Classification of Primary Care in the European community. London: Oxford University Press, 1993.
15. Bland M. Confidence interval should be used in reporting trials. BMJ 2000; 321: 1321.
16. Beaglehole R, Bonita R, Kjelleström T. Types of studies. In: Basic Epidemiology. Geneva: World Health Organization, 1993; 31-53.
17. Montanaro N, Margini N, Vaccheri A, Battilana M. Drug utilization in general practice: prescribing habits of national formulary drugs by GPs of Emilia Romagna (Italy) in 1988 and 1989. European Journal of Clinical Pharmacology 1992; 42: 401-408.
18. Svarstad B, Cleary P, Mechanic D, Robers P. Gender differences in the acquisition of prescribed drugs: An epidemiological study. Medical Care 1987; 25: 1089-1098.
19. Koutis A, Isakson Ǻ, Lindholm L, Lionis C, Svenninger K, Fiotetos M. Use of primary care in Spili, Crete, and in Dably, Sweden. Scandinavian Journal of Primary Health Care 1991; 9: 297-302.
20. Nolan L, O'Malley K. Age related prescribing pattern in general practice. Comprehensive Gerontology 1987; 1: 97-101.
21. Free C. Study of medicine prescribing for elderly patients. BMJ 1985; 290: 1113-1115.
22. Hallas J, Nissen A. Individualized drug utilization statistics. Analyzing a population's drug use from the perspective of individual users. European Journal of Clinical Pharmacology 1994; 47: 367-372.
23. Batikas A, Antonakis N, Liapis K et al. Repeat prescription as an indicator of poor clinical care: room for improvement in rural general practice in Greece. Primary Health Care 2001; 13: 121-126 in Greek.
24. Lionis C, Tsiraki M, Bardis V, Philalithis A. Seeking quality improvement in primary care in Crete, Greece: the first actions. Croatian Medical Journal 2004; 45: 599-603.
25. Rokstad J, Straand J, Fugelli P. Can drug treatment be improved by feedback on prescribing profiles combined with therapeutic recommendations? A prospective, controlled trial in general practice. Journal of Clinical Epidemiology 1995; 48: 1061-1068.
26. Ohayon MM, Partinen M. Insomnia and global sleep dissatisfaction in Finland. Journal of Sleep Research 2002; 11: 339-346.
27. Lionis CM, Bathianaki N, Antonakis S, Papavasiliou T, Philalithis A. High prevalence of diabetes mellitus in a municipality of rural Crete, Greece. Some threatening results from a primary care study. Diabetic Medicine 2002; 18: 768-769.
28. Tsamandouraki K, Alamanos Y, Tountas Y. Knowledge of and attitudes towards family planning and early detection of breast and cervical cancer in two female populations in Greece. Sozial- und Praventivmedizin 1992; 37: 136-141.
29. Zogas D, Elefthaeriou S, Zoga B, Eleftheriou M, Liakos M. Antimicrobial drugs in primary health care: use and abuse. Primary Health Care 1998; 10: 58-67 in Greek.
30. Syrogiannopoulos G, Grivea I, Katopodis G, Geslin P, Jacobs M, Beratis N. Carriage of antibiotic-resistant Streptococcus pneumoniae in Greek infants and toddlers. European Journal of Clinical Microbiology & Infectious Disease 2000; 19: 288-293.
31. Esposito S, Noviello S, Boccazzi A, Tonelli P. Management of upper respiratory tract infections in primary care in Italy: a national survey. International Journal of Antimicrobial Agents 2001; 17: 189-194.
32. Straand J, Rokstad K. General practitioner's prescribing patterns of benzodiazepine hypnotics: are elderly patients at particular risk for overprescribing? Scandinavian Journal of Primary Health Care 1997; 15: 16-21.




