Previous studies have demonstrated significant racial differences in incidence, age of onset, outcome and subsequent risk factors of stroke in mixed populations, especially in the USA1-4.
An excess stroke mortality rate among African Americans is known and persists despite dramatic declines in stroke mortality between 1970 and 1990 for both white and African-American men and women. Only a portion of this excess stroke mortality among African Americans can be attributed to the higher prevalence of hypertension and diabetes and to the lower average socioeconomic status5.
Racial differences in risk factors have been documented among the white, black and Hispanic population of the USA1. In an effort to investigate unexplained stroke or transient ischemic attack in both African-Americans and Caucasians, the former were found to have fewer complex thoracic aortic atheroma and fewer combined cardiac sources of embolus than the latter. This suggests that it is doubtful if atherosclerosis accounts for the differences in stroke incidence between them6. In a recent study carried out in the USA, race was not proved to be a predicting factor for future stroke events7.
A study involving Singaporean populations of Chinese, Malay and Indian origin failed to document differences in the prevalence of stroke among them. Nevertheless, it underlined the role of gender because the prevalence of stroke was found to be highest among Chinese men and lowest among Malay women8.
Minority population groups tend to present significant barriers concerning both acute stroke treatment and stroke prevention9. The former may be explained in some minority groups by existing linguistic deficiencies in mainly older people that inhibit case history documentation, whereas the latter may be explained by different application of risk factors4. A recent study demonstrated that black stroke survivors had greater activity limitations than white stroke survivors10.
Studies investigating any powerful relationship between religion and stroke are rare in the literature. An interesting study has shown a significant lack of preventive health care practices, minimal avoidance of dietary cardiovascular risk factors, and a significant difference between men's and women's cardiovascular risk factor status in the old order Mennonite population, who represent cloistered Christian communities whose religious and cultural traditions pervade their dietary and health practices11.
Focusing on either Muslims or Christians, the available literature is even more scarce. In a study investigating the beliefs of caregivers and traditional healers within the South African Indian Muslim community, regarding the etiology and treatment of stroke and the persons likely to be consulted in this regard, the participants expressed disillusionment with referrals to Western healthcare professionals whose treatment was often regarded as culturally inappropriate; they also emphasized the integral role played by family members in the treatment of illness and disease12. Controversially, in a small sample comprising Christian stroke patients, a qualitative approach using a long interview method was employed to expand on spiritual practices expressed through prayer as a way of coping after stroke13.
Little, however, is known about stroke in Muslim populations. In a Turkish study investigating the role of Ramadan fasting in the incidence of stroke, no relationship was documented14. No true comparative study including Muslims has been carried out. However, similar studies analyzing stroke incidence and mortality have been carried out in non-Muslim mixed populations with success15-17.
The aim of the present study was to detect possible differences concerning type, incidence, age of onset, outcome and subsequent risk factors of stroke in the mixed Christian/Muslim population of Xanthi region, Thrace, Greece. These data might be useful for evaluation of present healthcare status and for suggesting further action.
Methods
Setting
This study was performed in the Perfecture of Xanthi, a mainly rural and remote area in northern Greece. The area (Fig. 1) is inhabited by a population of 99 607 (mean true population estimate for the year 2000). Table 1 depicts mean true estimates for the same year according to religion (Christian : Muslim ratio: 52.81% : 47.19%) and gender (men : women ratio: 49.54% : 50.46%)18-19.
Figure 1: Map depicting the Xanthi district, Greece.
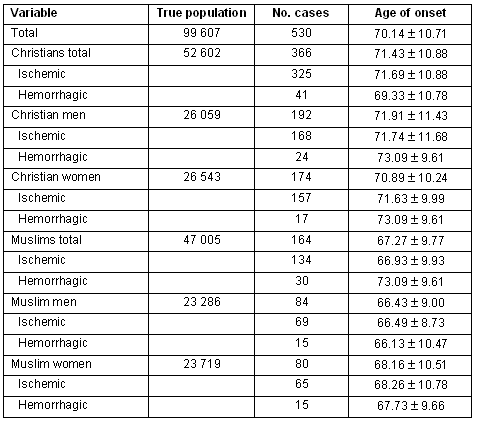
Table 1: Demographics and main descriptive statistics (mean ± SD) of the population of the study
Study population and sample
The study was based on 530 consecutive unselected stroke patients, who suffered from their first documented episode of stroke and were hospitalized under the responsibility of the Internal Medicine Department in the local hospital between 9 February 1998 and 8 February 2002. Data concerning sex, age and religion were collected.
Data collection
For each patient entered in the study, as part of history documentation, based on previous admissions20-26, a detailed medical history was recorded including:
- Hypertension (abnormal systolic and/or diastolic arterial pressure during the period of hospitalization or positive record), diabetes (abnormal fasting glucose and/or glucosylated haemoglobin levels or positive record), and hypercholesterolemia (LDL > 130 mg/dl)
- Tobacco (smoker or non-smoker) and alcohol (more or less than 20 g/day) habits
- Chronic or paroxysmal atrial fibrillation, previous myocardial infarction, heart failure
- Previous stroke
- Obstructive carotid angiopathy, peripheral vascular angiopathy
- Sick sinus syndrome, endocarditis, myocarditis
- Pulmonary embolism, use of contraceptives and polycythemia.
All patients underwent a thorough physical and neurological examination at least three times (on admission, 24 hours later and shortly before leaving the department). Additionally, a routine blood and serum test including hematocrit, hemoglobin and plasma levels of glucose, urea, creatinine, electrolytes and lipids, as well as a 12 lead ECG, chest radiography and CT scan were performed. All laboratory departments were on 24 hour duty and were qualitatively controlled by both internal and external control protocols. CT scan was selectively repeated after a period of 24-48 hours. In cases of unclear differential diagnosis, an MRI was performed. In the case of death, post-mortem findings were used only when it was impossible to document the underlying cause through medical record, physical examination and CT scan findings.
The cerebral infarcts were categorized on the basis of CT scan findings as lacunar when CT scan showed small, deep infarcts measuring 3-15 mm, corresponding to the clinical syndrome (pure motor hemiparesis, pure sensory stroke, hemiparesis-ataxia, dysarthria-clumsy hand, hemichorea-ballismus), non-lacunar (atherothrombotic, cardioembolic, by other causes, of unknown etiology) when the CT scan showed infarcts >15 mm and with negative CT scan. Hemorrhagic strokes were classified as intracranial hemorrhage (ICH), subarachnoid hemorrhage (SAH), or combined.
At the end of the hospitalization period, proposed treatment and the final outcome in terms of a modified Rankin scale were recorded27. Fewer categories than those proposed by the modified Rankin scale were formed to allow statistical performance. In detail, categories 1 and 2, as well as 4 and 5 of the original Rankin Scale were unified in the modified scale used in the present study (as category 2 and 4, respectively). This modified Rankin scale ranged from 1 (no neurological damage) to 5 (death). Unfortunately, the requested one-year follow-up period was not achieved in all cases, especially those concerning the older Muslim population. Thus, risking severe bias, follow-up results were omitted.
Ethical issues
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation and with the Helsinki Declaration of 1975, as revised in 2000. The study was approved by the Ethics Committee of the Xanthi General Hospital.
Data analysis
Student's unpaired t-test used dichotomous variables. Chi-square and, alternatively, Fisher's exact test was used for discrete parameters when expected frequencies fell below 5. A modified c2 test was used for comparison of incidence rates based on the number of cases and the person-time units. Three-dimensional c2 test was used for the comparison of 2 x 2 tables between two groups. Pearson's r was used for correlation analysis. All tests were two-tailed. All mean values were accompanied by 95% confidence intervals. Relative risk was computed based on data from the 2 x 2 tables. The level of statistical significance was set at p <0.05. A multiple logistic regression model (available online at http://members.aol.com/johnp71/logistic.html) was used for the detection of powerful relationships between religion, gender and type of stroke. All p values were given at two digits significance levels. Analysis was performed with the use of an interactive statistical tool (http://members.aol.com/johnp71/javastat.html) and confirmed by the use of SPSS vers. 9.5 (SPSS Inc, Chicago, IL, USA).
Results
Types of stroke
All 530 cases of stroke were classified according to their type as ischemic (459 cases; 86.6%) or hemorrhagic (71 cases; 13.4%). Their distribution according to religion and gender is shown (Table 1). A multiple logistic regression model, which was used for the detection of any powerful relationship between religion and gender and type of stroke, revealed that the Christian religion was a probable risk factor for ischemic stroke (OR = 2.131, 95%CI 1.005-4.521, p = 0.0486). Neither gender was correlated with type (OR=1.062, 95%CI 0.481-2.343, p = 0.883), nor did an interaction exist between religion and gender (OR=0.714, 95%CI=0.255-2.000, p = 0.521).
Ischemic strokes were classified according to CT findings as lacunar (126 of 452 cases; 27.9%), non-lacunar (222 of 452 cases; 49.1%) and having a negative CT (104 of 452 cases; 23.0%).
Hemorrhagic strokes were classified as intracranial (66 of 78 cases; 84.6%), subarachnoid (9 of 78 cases; 11.5%) and combined hemorrhage (3 of 78 cases; 3.8%).
Age of onset
From the medical history of enrolled patients, 17 of 530 (3.2%) had potentially suffered from a previous episode of stroke that had remained unrecognized. Nevertheless, these patients were not omitted from further statistical analysis because the documentation of a previous stroke was insufficient. The mean age of stroke incidence was found to be 70.14 ± 10.71 years. Using Student's unpaired t-test, a difference between Christians (71.43±10.88 years) and Muslims (67.26±9.77 years) was documented (p <0,001), attributed to men (p <0.001), rather than women (p = 0.055), and to ischemic (p <0.001), rather than hemorrhagic (p = 0.346) strokes. Detailed data are included (Table 1).
Incidence rates of stroke
Incidence rates are summarized (Table 2) and are expressed in 100 000 persons*years. The numeric values represent the product of the number of cases (Table 1), the mean true population (Table 1) and the years of the study (n = 4).
Table 2: Incidence rates of stroke among Christian and Muslim population of the present study expressed per 100 000 persons*years
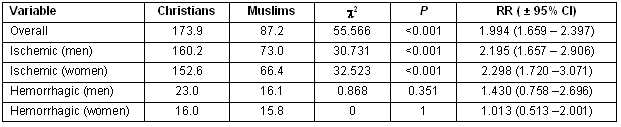
Muslims presented lower incidence rates than Christians as far as total (p <0.001) and ischemic stroke cases were concerned. This difference did not apply to hemorrhagic stroke cases and, thus, the positive correlation they present with the Muslim population is explained.
No difference was found in the distribution of ischemic and hemorrhagic stroke between men and women (p = 0.457; 2 x 2 x 2 c2).
Hospitalization period
There was no difference (p = 0.581; Student's unpaired t-test) in the mean duration of hospitalization between Christians (6.65 ± 3.21 days) and Muslims (6.83 ± 3.97 days).
Outcome
The patients' final outcomes are summarized (Table 3). Sixteen patients were dispatched to other hospitals and, thus, their outcome was not observed. Comparison between Christians and Muslims using the modified Rankin scale did not reveal any difference (p = 0.111; Student's unpaired t-test). A prominent difference was established after comparison between ischemic and hemorrhagic stroke (p <0.001; Student's unpaired t-test).
Table 3: Outcome of the stroke cases in the present study
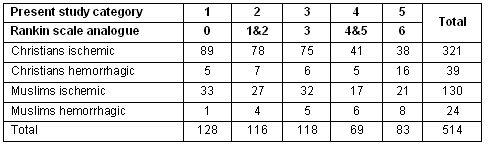
Using Pearson's correlation coefficient, a worse outcome (p <0.001) was correlated with older age, hemorrhagic stroke, diameter of hemorrhagic lesion, diameter of infarct, elevated mean temperature over the first 48 h, elevated mean systolic BP over the first 48 h, elevated mean diastolic pressure over the first 48 h, presence of atrial fibrillation, smoking habits and elevated cholesterol.
Correlation of risk factors and other parameters with religion
The use of Pearson's correlation coefficient r revealed that Muslims suffering from stroke presented greater instances of elevated systolic (p = 0.037) and diastolic (p = 0.025) BP during the first 48 h after admission for stroke than did Christians, despite their similar medical records regarding hypertension (p = 0.806). Controversially, diabetes and atrial fibrillation were less usual in Muslims (p = 0.019 and p <0.001). All other risk factors failed to present statistically significant correlations with religion. Moreover, neither the diameter of infarct or hemorrhage nor the temperature on admission correlated with religion. The statistically significant results were documented after the application of Bonferroni's adjustment (which is used to avoid type I errors in multiple correlations). The modified level of statistical significance was computed to be a = 0.0472.
Discussion and Conclusions
The present study suggests that the Muslims of Thrace, Greece, have a lower incidence of total and ischemic strokes than the Christians. In fact, the overall incidence of stroke in the Muslims of Thrace (87 cases per 100 000 per year) is significantly lower than in other Muslim populations (137 cases per 100 000 per year in Isparta, Turkey)14 and below mean worldwide values28. However, the Christians of the present study presented a similar average age of stroke onset and similar mortality when compared with those of the Athens Registry29. Moreover, the present study concludes that the Muslims of Thrace suffered from stroke at a younger age than the Christians. In fact, the Muslims of Thrace who suffered from stroke were 5 years older than the Muslims of Izmir, Western Turkey, according to the Ege Stroke Registry (62.3 ± 12.0 years)30. Because these two Muslim populations of different origins (mainly Pomaks in Thrace and Turks in Izmir)31 suffered from stroke at a relatively young age, it may be interpreted that a common epigenetic factor is responsible.
What are the major stroke determinants that differ between the Christians and Muslims of Thrace? The data presented suggest that two risk factors differ between the two communities: diabetes mellitus and atrial fibrillation, both favoring Muslims. The Muslims' traditional cuisine, characterized by the consumption of animal fat instead of olive oil, seems to be balanced by their natural way of life, consisting of low calorie intake, plentiful exercise and manual work.
Although the Christians' and Muslims' medical records were similar regarding hypertension, the Muslims' elevated mean systolic and diastolic BP during the first 48 h suggests poor control of hypertension during the acute phase (prejudicial medical care), more severe strokes or a greater degree of hypertension. Because the final outcome is similar in Christians and Muslims, the first two are improbable, and thus a greater degree of hypertension might account for this difference.
Trends in population BP levels have been proposed to explain trends in stroke event rates32. Moreover, it is well documented that hemorrhagic strokes are more closely related to elevated BP than are ischemic strokes33. Thus, the absence of a favorable difference concerning hemorrhagic strokes in Muslims and the lower mean age of onset may reflect a latent situation of uncontrolled hypertension. This potential handicap may be well overcome by the favorable difference in diabetes and atrial fibrillation in case of ischemic strokes.
What could foster hypertension in Muslims? A powerful difference between Muslim and all other subpopulations may be a surprisingly high incidence of depression, especially among women34-36. In a series of 4963 patients hospitalized in our department during the time of the present study, the incidence rates of suicide attempts due to severe depression was 44 per 100 000 per year among Christians and 83 per 100 000 per year among Muslims (V Papadopoulos, unpubl. data, 2005). Depression could be a mechanism that interacts with the effort to control hypertension; people suffering from depression may underestimate their disease and fail to comply with medical recommendations.
Additional differences between the Christians and Muslims of Thrace, was the level of education (a considerable proportion of Muslims remain undereducated), the types of occupation (the majority of Muslims work with agriculture, cattle-breeding and manual tasks) and the income per capita (relatively low in Muslims); these might play a role in stroke development. It has been documented that low socioeconomic status and poor education are negative predictors for stroke incidence and severity5. Moreover, Muslims encounter some restrictive parameters as far as proper use of medical services, due to the harsh landscape of many Muslim villages and the linguistic handicap of mainly older people. Finally, Muslims' strict religious observance of the Ramadan fasting period lead them to omit even medication, although a relevant paper claims that the Ramadan period is not negatively involved in differences concerning stroke incidence14.
Despite the fact that the present study has contributed to stroke epidemiology in Muslims, it has certain limitations. The relatively small sample size, its regional character and an inability to approach the few but existing non-hospitalized cases are some limitations. The number of stroke cases who remain non-hospitalized is believed to be small, because all emergencies reach the local hospital without the intervention of a physician or a GP. However, because there is no obvious reason for religion-related bias in these cases, it may be hypothesized that the present study is a merely a true incidence study that can temporarily substitute for an official stroke registry in the region. Nevertheless, taking into consideration the absence of similar studies, the present conclusions might offer a starting point for future efforts. A field survey targeting patients with previous stroke might be more appropriate in determining the real incidence of stroke and related risk factors in the region, thus providing a clearer view of differences.
In conclusion, the natural way of life (manual work and healthy nutrition) might explain the lower diabetes and atrial fibrillation rates and thus the low stroke incidence rate among the Muslims of Thrace. Thus, all care should be taken to encourage the traditional way of life which seems to exert a prophylactic effect concerning stroke development. Additionally, efforts should be made to clarify confounding factors such as education and occupation, and to investigate the true presence of hypertension among the Muslim population. Clarification should also be attempted regarding the value of targeted cost-effective non-pharmaceutical and pharmaceutical interventions, which may further assist public health status32,37-44.
References
1. McGruder HF, Malarcher AM, Antoine TL, Greenlund KJ, Croft JB. Racial and ethnic disparities in cardiovascular risk factors among stroke survivors: United States 1999 to 2001. Stroke 2004; 35: 1557-1561.
2. Hajat C, Tilling K, Stewart JA, Lemic-Stojcevic N, Wolfe CD. Ethnic differences in risk factors for ischemic stroke: a European case-control study. Stroke 2004; 357: 1562-1567.
3. Sacco RL. Preventing stroke among blacks: the challenges continue. JAMA 2003; 289: 3005-3007.
4. Saposnik G, Caplan LR, Gonzalez LA et al. Differences in stroke subtypes among natives and Caucasians in Boston and Buenos Aires. Stroke 2000; 31: 2385-2389.
5. Howard G, Howard VJ. Reasons for Geographic And Racial Differences in Stroke (REGARDS) investigators. Ethnic disparities in stroke: the scope of the problem. Ethnic Disease 2001; 11: 761-768.
6. Ward RP, Don CW, Furlong KT, Lang RM. Racial differences in aortic atheroma in patients undergoing transesophageal echocardiography for unexplained stroke or transient ischemic attack. American Journal of Cardiology 2004; 94: 1211-1214.
7. Kleindorfer D, Panagos P, Pancioli A et al. Incidence and short-term prognosis of transient ischemic attack in a population-based study. Stroke 2005; 36: 720-723.
8. Venketasubramanian N, Tan LC, Sahadevan S et al. Prevalence of stroke among Chinese, Malay, and Indian Singaporeans: a community-based tri-racial cross-sectional survey. Stroke 2005; 36: 551-556.
9. Morgenstern LB, Steffen-Batey L, Smith MA, Maye LA. Barriers to acute stroke therapy and stroke prevention in Mexican Americans. Stroke 2001; 32: 1360-1364.
10. Centers for Disease Control and Prevention (CDC). Differences in disability among black and white stroke survivors - United States, 2000-2001. MMWR Morbity and Mortality Weekly Report 2005; 54: 3-6.
11. Michel A, Glick M, Rosenthal TC, Crawford M. Cardiovascular risk factor status of an Old Order Mennonite community. Journal of the American Board of Family Practice 1993; 6: 225-231.
12. Bham Z, Ross E. Traditional and western medicine: cultural beliefs and practices of South African Indian Muslims with regard to stroke. Ethnic Diseases 2005; 15: 548-54.
13. Robinson-Smith G. Prayer after stroke. Its relationship to quality of life. Journal of Holistic Nursing 2002; 20: 352-366.
14. Akhan G, Kutluhan S, Koyncuoglu HR. Is there any change of stroke incidence during Ramadan? Acta Neurologica Scandinasia 2000; 101: 259-261.
15. Lawrence ES, Coshall C, Dundas R et al. Estimates of the prevalence of acute stroke impairments and disability in a multiethnic population. Stroke 2001; 32: 1279-1284.
16. Frey JL, Jahnke HK, Bulfinch EW. Differences in stroke between white, hispanic, and native American patients. Stroke 1998; 29: 29-33.
17. Tuhrim S, Godbold JH, Goldman ME, Horowitz DR, Weinberger J. The minorities risk factors and stroke study (MRFASS). Design, methods and baseline characteristics. Neuroepidemiology 1997; 16: 224-233.
18. Greek National Statistical Service. Monthly Statistical Bulletin (Athens). Athens: Greek National Statistical Bureau Bulletin, 2001.
19. Zeginis E. Muslim minority of western Thrace. Kathimerini 1993; 14: 11.
20. Hart CL, Hole DJ, Smith GD. Risk factors and 20-year stroke mortality in men and women in the Renfrew/Paisley study in Scotland. Stroke 1999; 30: 1999-2007.
21. Henrich JB, Horwitz RI. The contribution of individual factors to thromboembolic stroke. Journal of General Internal Medicine 1989; 4: 195-201.
22. Tanizaki Y, Kiyohara Y, Kato I et al. Incidence and risk factors for subtypes of cerebral infarction in a general population, The Hisayama Study. Stroke 2000; 31: 2616-2622.
23. Besson G, Hommel M, Perret J. Risk factors for lacunar infarcts. Cerebrovascular Disease 2000; 10: 387-390.
24. Parnetti L, Gallai V. Atrial fibrillation and stroke. Cerebrovascular Disease 2000; 10: 40-41.
25. Arboix A, Pujades R. Response to: Atrial fibrillation and stroke in patients admitted to a city center hospital serving a multicentre community. International Journal of Cardiology 2000; 75: 285.
26. Yang Z, Wang J, Zheng T, Altura BT, Altura BM. Ethanol-induced contractions in cerebral arteries. Stroke 2001; 32: 249-257.
27. New PW, Buchbinder R. Critical appraisal and review of the Rankin scale and its derivatives. Neuroepidemiology 2006; 26: 4-15.
28. Sarti C, Rastenyte D, Cepaitis Z, Tuomilehto J: International trends in mortality from stroke, 1968 to 1994. Stroke 2000; 31: 1588-1601.
29. Vemmos KN, Takis CE, Georgilis K et al. The Athens stroke registry: results of a five-year hospital-based study. Cerebrovascular Disease 2000; 10: 133-141.
30. Kumral E, Ozkaya B, Sagduyu A, Sirin H, Vardarli E, Pehlivan M. The Ege Stroke Registry: a hospital-based study in the Aegean region, Izmir, Turkey. Analysis of 2,000 stroke patients. Cerebrovascular Disease 1998; 8: 278-288.
31. Papadopoulos V, Dermitzakis E, Konstantinidou D, Petridis D, Xanthopoulidis G, Loukopoulos D. HbO-Arab mutation has originated in the Pomak population of Greek Thrace. Haematologica 2005; 90: 255-257.
32. Tolonen H, Mahonen M, Asplund K et al. Do trends in population levels of blood pressure and other cardiovascular risk factors explain trends in stroke event rates?: Comparison of 15 populations in 9 countries within the WHO MONICA stroke project. Stroke 2002; 33: 2367-2375.
33. Passero S, Ciacci G, Reale F. Potential triggering factors of intracelebral hemorrhage. Cerebrovascular Disease 2001; 12: 220-227.
34. Hassouneh-Phillips D. American Muslim women's experiences of leaving abusive relationships. Health Care Women International 2001; 22: 415-432.
35. Ali A, Toner BB. Self-esteem as a predictor of attitudes toward wife abuse among Muslim women and men in Canada. Journal of Social Psychology 2001; 141: 23-30.
36. Sonuga-Barke EJ, Mistry M, Qureshi S. The mental health of Muslim mothers in extended families in Britain: the impact of intergenerational disagreement on anxiety and depression. British Journal of Clinical Psychology 1998; 37: 399-408.
37. Klungel OH, Heckbert SR, Longstreth WT Jr et al. Antihypertensive drug therapies and the risk of ischemic stroke. Archives of Internal Medicine 2001; 161: 37-43.
38. Klungel OH, Kaplan RC, Heckbert SR et al. Control of blood pressure and risk of stroke among pharmacologically treated hypertensive patients. Stroke 2000; 31: 420-424.
39. Goldstein LB, Adams R, Becker K et al. Primary prevention of ischemic stroke. Stroke 2001; 32: 280-299.
40. Kaste M, Skyhoj Olsen T, Orgogozo J, Bogousslavsky J, Hacke W. Organization of stroke care: education, stroke units and rehabilitation. European Stroke Initiative (EUSI). Cerebrovascular Disease 2000; 10: 1-11.
41. Ohgren B, Weinehall L, Stegmayr B, Boman K, Hallmans G, Wall S. What else adds to hypertension in predicting stroke? An incident case-referent study. Journal of Internal Medicine 2000; 248: 475-482.
42. Ahmed N, Wahlgren G. High initial blood pressure after stroke is associated with poor functional outcome. Journal of Internal Medicine 2001; 249: 467-473.
43. Hajat C, Dundas R, Stewart JA et al. Cerebrovascular risk factors and stroke subtypes: differences between ethnic groups. Stroke 2001; 32: 37-42.
44. Evers SM, Goosens ME, Ament AJ, Maarse JA. Economic evaluation in stroke research. An introduction. Cerebrovascular Disease 2001; 11: 82-91.


