Dear Editor
Orthopedic diseases, such as osteoarthritis and lumbar spine deformation, that are treated with a compress/patch (C/P; called shippu in Japanese) for pain relief are frequently seen in elderly women1,2. Recently (April 2017), the number of C/Ps prescribed by physicians for such diseases has been uniformly restricted (to 70 C/Ps per prescription) in Japan. Given the growing elderly population and the free-access system for visiting all medical institutions in Japan, visiting multiple medical institutions in elderly patients has come to be recognized as a serious problem from the perspective of burden on healthcare costs and adverse drug use3,4. In light of recent restriction for C/P prescriptions, patient behavior (eg multiple physician visits in order to receive additional C/P prescriptions) is a concern of primary care in rural practice3,4.
A preliminary study was conducted using a database (from July 2017 to April 2018) in which female patients (n=68, median age = 82.0 years) were anonymously asked about their behavior after the implementation of restrictions on C/P prescription through a self-reported questionnaire, including questions about the patient’s age, number of C/Ps used daily through April 2017 and additional physician visits. The survey was performed among patients who routinely visited rural medical institutions in Gifu Prefecture for C/P prescriptions. The study was approved by the ethics committee of the Center for Community Medicine in North-Western Gifu prefecture (Approval No. 1). The differences between two groups were analyzed by Mann–Whitney U-test or Fisher’s exact test as appropriate.
As a result, approximately 10% of patients (n=6) reported visiting multiple physicians due to the restriction on C/P prescription. The group with multiple physician visits was significantly older than that without multiple physician visits (Table 1). When the patients were divided by age (≤80 years or >80 years), all patients with multiple physician visits existed in the group of >80 years (with a significant deviation; Table 1). A non-significant difference in the number of C/P prescriptions per day before the restriction was noted between the group with and without multiple physician visits.
More elderly patients may show a new behavior of visiting multiple physicians to obtain multiple C/P prescriptions. This observation was descriptively cross-sectional and did not examine the characteristics of patients’ disease conditions and the change in the daily number of C/P prescriptions before and after the restriction (as the study limitations); therefore, the appropriateness/inappropriateness of existence of multiple physician visits in more elderly patients remained undetermined. As a possible explanation, more elderly patients (who tend to suffer from more than one disease) could have an increased need for C/P treatment, even though there was not a clear difference in the daily number of C/P prescriptions before the restriction between the group with multiple physician visits (more elderly patient group) and the group without multiple physician visits. If so, multiple physician visits might be justified as appropriate behavior. Given the problems of multiple physician visits3,4, the new existence of some problems might be carefully evaluated as inappropriate behavior in such patients. Further, larger scale studies with ample follow-up and more facilities will be planned, as better elderly care is a critical issue to address in clinical practice for rural communities that include elderly patients.
Table 1: Profile of groups with and without multiple physician visits after implementation of restrictions on the prescription of compresses/patches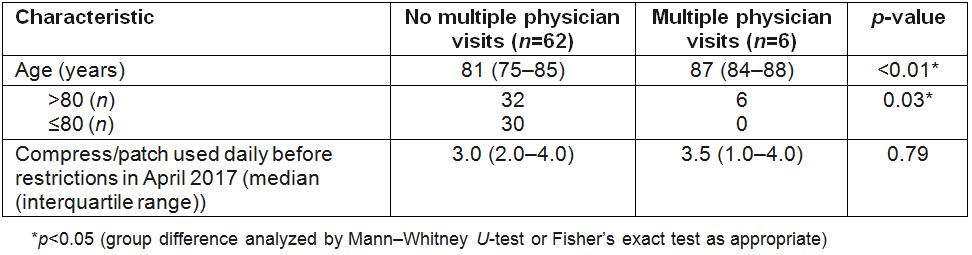
Acknowledgements
The authors thank Gifu Primary Care and Community Medicine Research Net Group for their assistance in conducting the study.
Ban Tetsuaki, National Health Insurance Kukuno Clinic, Gifu, Japan
Hideo Hirose, National Health Insurance Wara Clinic, Gifu, Japan
Hiroyuki Teraura and Kazuhiko Kotani, Division of Community and Family Medicine, Jichi Medical University, Tochigi, Japan
Tadao Gotoh, National Health Insurance Shirotori Hospital, Gifu, Japan
