Introduction
The epidemic of overweight and obesity in Australia shows no sign of waning, despite extensive public health campaigns designed to raise the awareness of the health risks of overweight and obesity and to encourage healthy eating and physical activity1. The AusDiab study from 2001 estimated that the prevalence of overweight and obesity in urban Australia was 39% and 21%, respectively, a 2.5-fold rise since 19802. While these rates were considered alarming, it was acknowledged that these figures may be an underestimate of true prevalence, particularly for rural and remote areas2,3. Furthermore, studies that have investigated weight change in the Australian population suggest that the obesity epidemic may even be worsening4,5.
The high prevalence of overweight and obesity and its association with diseases such as type 2 diabetes, heart disease, arthritis and some cancers has made overweight and obesity a high priority problem on the agenda of the National Health and Medical Research Council6,7. The question remains whether overweight and obesity is also a high priority problem for the general population. Studies from the USA show that most Americans are not seriously concerned with obesity and express relatively low support for policies to reduce obesity8, despite the fact that obesity is even more prevalent in the USA than in Australia9. This incongruence between views of health authorities and the public also exists in Australia. Studies have shown that many overweight Australians are unconcerned about their weight and have no intention of trying to lose weight10-12.
The lack of action by many Australians to address their weight problems may occur because many overweight Australians do not perceive themselves to be overweight10,13, or do not perceive overweight to be very harmful to health11. While several studies have attempted to explore the reasons for the discrepancies between medical and community views of overweight, there is little current information about the mechanisms that Australians use to assess weight status and their awareness of the specific health risks of overweight. Furthermore, many studies concerned with overweight and obesity have been conducted in urban centres5,14-17 or within the general population4,11,13,18, providing little information about the knowledge base for rural populations. In particular, there is very little information regarding rural Australians' knowledge and perceptions of overweight and the associated health risks. This is of particular concern because studies suggest that rural populations may experience a higher prevalence of overweight and obesity than urban populations19,20, hence increasing their susceptibility to long-term chronic diseases and decreased quality of life. Thus, the aims of this study were to investigate among rural Australians awareness of the specific health risks of overweight, perceptions of individual weight status, individual methods used to assess weight status and the lay understanding of the standard measures used by health professionals to assess overweight.
Methods
Participants and procedure
Formal ethical clearance for this study was granted by The University of Queensland Medical Research Ethics Committee. The study was set in central Queensland. Based on the Rural, Remote and Metropolitan Areas (RRMA) classification scheme21, participants' localities of residence included large rural centres (population 25 000-99 999, RRMA 3), small rural centres (population 10 000-24 999, RRMA 4), other rural areas (population < 10 000, RRMA 5), remote centres (population ≥ 5000, RRMA 6) and other remote areas (population < 5000, RRMA 7).
Participants were sought via direct contact with researchers at five locations: (i) RRMA 3 shopping centre A; (ii) RRMA 3 shopping centre B; (iii) RRMA 4 shopping centre; (iv) RRMA 5 shopping centre; and (v) RRMA 5 annual agricultural show. At each location, researchers approached adults passing through or working in adjacent businesses and offered participation. The questionnaire could be completed at that time and left in a sealed box or completed elsewhere and returned by post. Data collection was conducted on a Thursday and/or a Friday, days considered to have higher foot traffic.
Eligible participants were those who were adult (age ≥ 18 years), lived in the study location, had sufficient language skills to work with the questionnaire and completed the questionnaire. A total of 229 eligible adults completed the questionnaire, representing a response rate of 41.2%. While little is known about non-responders, the length of the questionnaire may have contributed to their decision not to participate.
Measures
A self-completion questionnaire was specifically designed for this study which addressed participants' understanding of healthy weight (available from authors). Participants were asked to provide demographic details and self-report their height and weight. In addition the questionnaire included the following measures.
Self-assessment of weight: Participants were asked, 'How would you assess your own weight?'. The response categories were 'underweight'; 'acceptable or healthy weight'; and 'overweight'. This was followed by the question, 'To answer the question above, how did you assess your weight?'. The response categories were 'comparison to others'; 'clothing size'; 'clothing fit (loose/tight)'; 'body mass index'; 'height/weight charts'; 'how you feel'; 'opinions of others'; or 'other'. Some participants selected more than one option and this was recorded as 'more than one'.
Weight change: Participants were asked, 'Has you weight changed in the last 12 months?' and the response categories were 'increased'; 'decreased'; or 'no change'. Some participants indicated both an increase and a decrease.
Understanding of measures to assess weight: Participants were presented with the following statements: 'body mass index (BMI) is used to determine whether someone is overweight'; 'a BMI between 25 and 30 is considered healthy'; 'BMI is calculated by dividing your weight (in kg) by your waist measurement (in cm) ie weight/waist measurement'; 'BMI is calculated by dividing your weight (in kg) by the square of your height (in m) ie weight/height2'; 'a waist-to-hip ratio (WHR) greater than 1.0 is considered healthy'; 'a high WHR means that you are carrying extra weight around your hips'; and 'being overweight is OK if you are physically active'. The possible responses were: 'true'; 'false'; or 'don't know'.
Understanding of the health risks of overweight: Participants were asked, 'In comparison with "healthy" weight people, overweight people are more likely to get/have:' (with the following diseases listed) 'asthma'; 'arthritis'; 'bowel cancer'; 'breast cancer'; 'diabetes (type 2)'; 'endometrial cancer'; 'fertility problems'; 'heart disease'; 'sleep disorders eg sleep apnoea'; and 'stroke'. The possible responses were: 'true'; 'false'; or 'don't know'.
Additional questions addressing separate issues associated with childhood obesity were asked at the same time and will be reported elsewhere. The questionnaire was trialled on a separate group of potential participants to ensure face validity.
Data analysis
Each participant's self-reported weight and height measurements were translated into kilograms and metres, respectively, if needed and used to calculate a BMI (kg/m2 for each participant. The World Health Organisation classifications of underweight and overweight based on BMI measurements (kg/m2 were used to determine weight status (underweight < 18.5; normal range = 18.5-24.9; overweight ≥ 25.0) and the degree of overweight (grade 1 = 25.0-29.9; grade 2 = 30.0-39.9; grade 3 ≥ 40.0)22.
All data were analysed using the Statistical Package for Social Sciences vers 13.0 (SPSS Inc; Chicago, IL, USA). Simple frequency analyses were used to describe the demographic profile of participants and to report responses. Data are presented as means and mean percentages. Comparative statistics were calculated using c2 analyses or the Mann-Whitney U-test for two independent samples. Correlations were calculated with the Spearman correlation coefficient. The level of statistical significance was defined as p<0.05.
Results
Sample characteristics
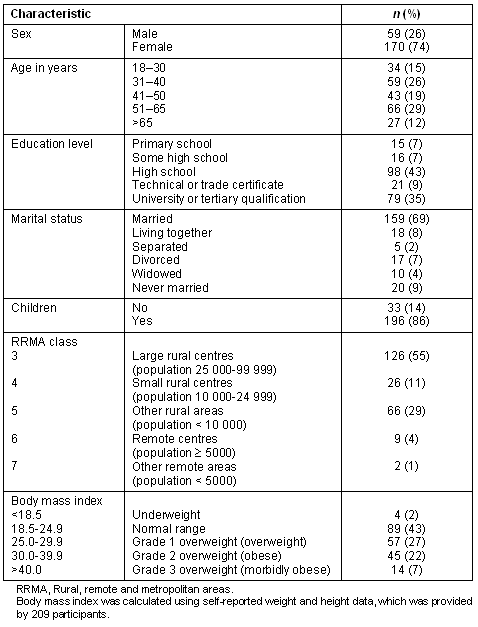
Participant demographics are presented (Table 1). Although the participants were drawn from a convenience sample of shoppers, the survey was completed by a diverse group of people of different ages and educational backgrounds. However, females (74%), parents (88% females, 83% males) and those married (68% females, 75% males) were overrepresented.
Table 1: Distribution of demographic characteristics of participants (n = 229)
Knowledge of risks associated with overweight
The majority of participants were aware that being overweight is a health risk factor regardless of their degree of physical activity (74%), and that overweight is associated with increased risk of arthritis (57%), type 2 diabetes (83%), fertility problems (68%), heart disease (92%), sleep apnoea (69%) and stroke (83%). Fewer participants were aware of other risk factors such as asthma (35%), bowel cancer (32%), breast cancer (18%) and endometrial cancer (14%). As is shown (Fig 1A), significantly more women than men were aware of that overweight is associated with type 2 diabetes (Z = -2.517, p<0.05, Mann-Whitney U-test) and fertility problems (Z = -2.558, p<0.05, Mann-Whitney U-test). The awareness of the disease risks of overweight were not significantly different between participants that were classified overweight or obese based on self-reported data and those that were not (Fig 1B).
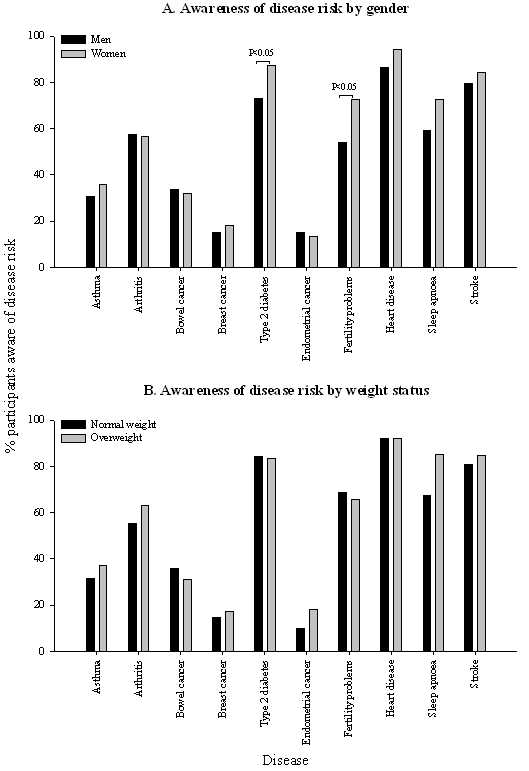
Figure 1: Relationship between gender, weight status and disease risk awareness.
The graph shows the percentage of participants (y-axis) who were aware that overweight is associated with specific disease risks (x-axis). Panel A shows the percentage of men (n = 59) and women (n = 170) who were aware of the disease risks of overweight. Panel B shows the percentage of normal weight (n = 89) and overweight or obese (n = 116) participants who were aware of the disease risks of overweight. P<0.05 (Mann-Whitney U-test) comparisons by gender and weight status.
Differences between perceived and medically defined weight status
Most participants (91.3%) provided self-reported height and weight data, giving a range of BMI values from 17.6 to 54.6 kg/m2 and an average BMI of 27.5 kg/m2. The percentage of overweight men was 71% and overweight women was 50%. The average BMI was 28.7 kg/m2 for men (n = 58) and 27.0 kg/m2 for women (n = 151), with a significantly higher percentage of men overweight compared with women (Z = -2.732, p<0.01, Mann-Whitney U-test). The prevalence of underweight was 2%.
Participants' self-assessment of weight status was compared with their weight status determined from self-reported weight and height (Table 2). There was a significant difference between the number of people that considered themselves overweight and the number that were classified overweight according to BMI (c2 =13.133, p<0.01, Pearson c2 test). Among people classified overweight according to BMI, misperception of weight status was more prevalent among men (59%) than women (28%; c 2 = 4.425, p<0.05, Pearson c2 test. Perception of weight status also differed according to the degree of overweight (c2 = 24.970, p<0.001, Pearson c2 test): 46% of moderately overweight (grade 1 overweight); 84% of obese (grade 2 overweight); and 100% of morbidly obese (grade 3 overweight) participants were aware that they were overweight. Among people with a BMI within the normal range, 6% people incorrectly assessed themselves underweight.
Table 2: Lay perceptions of healthy weight: differences between actual weight status and perceived weight status (n = 209)

Measures used to assess weight
As is shown (Table 3), a range of methods were used by participants to assess their weight status. The majority of participants knew that BMI was used as measure of overweight (61%) but did not know the BMI range for healthy weight (83%) nor how to calculate BMI (69%). No participants indicated that they used WHR to assess weight status, while few (15%) had any understanding of this measure.
Table 3: Lay measures of weight (n = 229)
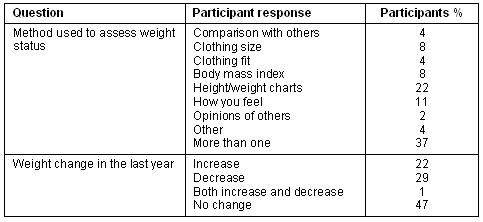
Weight change
The majority of participants (53%) stated that they believed their weight had changed during the previous 12 months either through an increase, decrease or both (Table 3). Compared with women, significantly more men perceived their weight to be more stable over the previous year (59% men vs 43% women, Z = -2.167, p<0.05, Mann-Whitney U-test). Among those participants who classified themselves overweight, 17% of men and 37% of women reported a weight decrease and another 50% of men and 33% of women reported no weight change over the last year.
Discussion
This study has investigated the awareness of the health risks of overweight and understanding of measures of overweight among people in rural communities in Central Queensland. It was found that most people in this study were appropriately aware that, regardless of their degree of physical activity, overweight is associated with increased risk of heart disease, type 2 diabetes and stroke. However this was at odds with participants' apparent inability to determine whether their weight was within the normal or healthy range.
The widespread knowledge among participants that overweight poses a risk to health may reflect the high burden of obesity-related illnesses in these communities. Recent estimates from Queensland Health suggest that the prevalence of coronary heart disease, stroke, diabetes, colorectal cancer, asthma and osteoarthritis in the communities sampled in our study is higher than the rest of Queensland20. The incidence of these diseases is believed to reflect the greater proportion of overweight and obesity in these communities20. While the true prevalence of overweight and obesity in rural and regional communities in central Queensland is unknown, it is estimated to be higher than metropolitan areas of Queensland3,14,23. Our data support these estimations with 71% men and 50% of women classified overweight (grade 1 overweight) or obese (grade 2 and grade 3 overweight) based on self-reported data. These figures are markedly higher than state-wide averages of self-reported data collated for Queensland in the 2001 National Health Survey (56% men, 41% women)24 and are worrying in light of the projection that rates of overweight and obesity will increase in these communities20.
Knowledge of the health risks of overweight were generally consistent across the BMI spectrum, with similar beliefs expressed by those who were classified overweight or obese and those who were not. These findings support previous research that show that awareness of the health risks of overweight is not sufficient to modify behaviour25,26. The apparent inconsistencies between knowledge and behaviour may occur because many overweight people are unaware that they have a weight problem and therefore do not internalise the issue as personally relevant. Consistent with other Australian studies10,11, we found that misperception of weight status was more frequent among men with almost 60% of overweight men believing that their weight was in an 'acceptable' or 'healthy' range. The highest prevalence of misperceived overweight was among participants categorised as grade 1 overweight (moderate overweight). This high prevalence is extremely important given that a greater proportion of the overweight population are in the grade 1 category of overweight and that grade 1 overweight is a risk factor for obesity2,3,27. It should be noted that even among participants who were categorised as obese (ie, grade 2 and grade 3 overweight) and clearly overweight, 16% did not perceive themselves to be overweight. Such underestimation of weight status occurred in all weight classes, with 6% of normal weight participants considering themselves underweight.
The reasons for the failure of participants to recognise overweight in themselves may be due, in part, to the wording of the question. Participants were asked to categorise their weight as 'underweight', 'acceptable' or 'normal', or 'overweight'. It has been argued by other authors that since overweight is 'normal', being moderately overweight is acceptable or not abnormal10. While only 4% of participants in our study indicated that they used comparison to others to assess overweight, many still chose subjective measures to assess overweight such as 'clothing size', 'clothing fit', 'how they feel' and the 'opinions of others'. Nearly one-third of participants indicated that they used objective measures such as height/weight charts and BMI to assess weight status, but when questioned further it became clear that few knew the BMI range considered to be healthy. This suggests that subjective measures of weight status are not adequate to assess weight status and that the population sampled in the study needs to be educated about objective measures to assess healthy weight.
The most appropriate objective measure of overweight and obesity is debatable28,29. Although BMI is commonly used in population surveys of overweight and obesity, as an index of adiposity it has significant shortcomings because it does not take into account body composition. When assessing risks associated with obesity there is substantial evidence that measures of abdominal obesity such as WHR and waist circumference may be more appropriate28,30-39. Abdominal adiposity is associated with greater risk of obesity-related morbidity39 and has been shown to have a stronger positive association with cardiovascular risk than overall adiposity2,30-37,40. Thus, many authors recommend that measurements such as waist circumference or WHR should be a preferred measure of obesity over BMI28-30,33,37-39.
While WHR has been shown to have the strongest correlation with cardiovascular disease risk37,39, none of the participants in our study used WHR to assess weight status. We found that very few even had any understanding of this measure, perhaps due to the need to calculate a ratio from two values. A single measure such as waist circumference may be a more convenient and simple measure for the general population to use41. However, a recent worldwide survey, Shape of the Nations, has found that, in Australia, less than 1% of the general population use waist circumference to assess whether their weight and shape is healthy41. This is despite the fact that 71% of people report that they are aware that abdominal obesity is linked to cardiovascular disease41. In the same study, it was shown that while 70% of primary care practitioners report that they measure waist circumference in some patients, only 8% knew the correct waist circumferences that posed increased cardiovascular risk41.
The focus on absolute weight rather than where weight is carried may be particularly important among women. A range of Australian studies have shown that when waist circumference is used as a measure of obesity, considerably more women are classified obese than when BMI is used as a measure2,37,42. This underestimate of weight status with use of BMI occurs in all weight classes, such that even among women with a normal BMI many will have a high waist circumference that puts them in the overweight class (≥ 80 cm) and at increased risk of disease28,38,43. The insensitivity of BMI as a measure of abdominal adiposity may explain why many Australian women see overweight beginning at a BMI below that currently used to define overweight10. It would also explain why, in this study and other Australian studies10,11, some women considered to be a healthy weight based on BMI assess themselves as overweight.
Women have been shown to be more weight-conscious and more likely to be taking action about their weight than men10,11,15,44. Some authors suggest that this is because women are affected more strongly than men by social pressures to maintain a body image in accordance with the slim ideal16,45. However, an Australian study conducted in a rural community found that the most common reasons among women for trying to lose or maintain weight were related to health, fitness and general wellbeing10. Indeed, we found that women were more aware of some of the specific health risks of overweight than men, such as diabetes and infertility.
The widespread awareness of the association between overweight and increased risk of arthritis, type 2 diabetes, fertility problems, heart disease, sleep apnoea and stroke in our study may evince the success of extensive public health campaigns that have addressed the modifiable risk factors of these chronic diseases. Conversely, the limited awareness of rural men and women regarding the relationship between overweight and increased risk of asthma, bowel cancer, breast cancer and endometrial cancer may be a consequence of the limited attention that has been given to overweight as a potential cause of these diseases. While a 1994 Australian study did show that urban men and women were aware that overweight worsens asthma and lung cancer15, there is considerable variation among the population regarding awareness of overweight as a risk factor for cancer46. Only a few studies have investigated lay knowledge of overweight as a risk factor for bowel, breast and endometrial cancer and these indicate that the general population are unaware that overweight is a risk factor for these diseases46-49. This lack of awareness is not surprising, given that overweight is considered to be a minor risk factor for these diseases and that there is considerable controversy in the medical community regarding the link of overweight with asthma50-52 and cancer53,54.
It must be noted that there are several limitations to this study and these need to be taken into consideration. The method used to assess weight status in this study was based on self-reported weight and height. While self-reported weights and heights correlate highly with measured values and are commonly used in population health research, they have been shown to lead to misclassification of relative weight status, particularly in overweight people, due to underestimation of weight and overestimation of height55-60. Thus, it is probable that the true prevalence of overweight and misperception of overweight among our participants is higher than that reported in our study. As the participants in this study were derived from a convenience sample it is difficult to determine their representativeness of the general population base for this region. It is not possible to provide any information on those who declined to participate, or those sections of the community that may not have been represented. Self-selection predisposes a bias of interest in the topic and willingness to participate, rather than representativeness of the geographical region under study. It is, therefore, not possible to generalise these findings beyond the region of the study and the participants who completed the questionnaire. It is possible that the lack of a statistically significant difference in many of the questions, such as gender differences, and differences between rural centres, may be because of the small sample size. A larger sample size may have had more power to detect differences across the multiple questions.
Conclusion
Despite apparent knowledge of the major health risks of overweight, many participants were unaware that they were at risk. The inability of individuals to identify overweight in themselves may explain the high prevalence of overweight and obesity in central Queensland. This study highlights the need to educate people in these communities about accurate and objective measures to assess overweight and obesity.
The findings of this exploratory study provide a basis for larger studies to test hypotheses about contributors to overweight in rural communities throughout Australia. It also suggests that national estimates of the prevalence of overweight may grossly underestimate the true prevalence of overweight in some rural communities, and that further data are needed to accurately gauge the seriousness of the obesity problem in rural Australia.
References
1. Eckersley RM. Losing the battle of the bulge: causes and consequences of increasing obesity. Medical Journal of Australia 2001: 174: 590-592.
2. Cameron AJ, Welborn TA, Zimmet PZ, Dunstan DW, Owen N, Salmon J et al. Overweight and obesity in Australia: the 1999-2000 Australian Diabetes, Obesity and Lifestyle Study (AusDiab). Medical Journal of Australia 2003: 178: 427-32.
3. Dunstan D, Cameron A, de Courten M, Coyne T, D'Embden M, Welborn T et al. The Australian Diabetes, Obesity and Lifestyle Study (AusDiab). Data report: Brisbane. Melbourne: International Diabetes Institute, 2001.
4. Jackson M, Ball K, Crawford D. Beliefs about the causes of weight change in the Australian population. International Journal of Obesity and Related Metabolic Disorders 2001: 25: 1512-1516.
5. Ball K, Crawford D, Ireland P, Hodge A. Patterns and demographic predictors of 5-year weight change in a multi-ethnic cohort of men and women in Australia. Public Health and Nutrition 2003: 6: 269-281.
6. National Health and Medical Research Council. Acting on Australia's weight. Canberra: Australian Government Publishing Service, 1997.
7. National Health and Medical Research Council. Clinical practice guidelines for the management of overweight and obesity in adults. Canberra: Australian Government Publishing Service, 2003.
8. Oliver JE, Lee T. Public opinion and the politics of America's obesity epidemic. KSG Working Paper No. RWP02-017. Cambridge: John F Kennedy School of Government, 2002.
9. Australasian Society for the Study of Obesity. Obesity prevalence in several countries worldwide. (Online) 2005. Available: http://www.asso.org.au/home/obesityinfo/stats/worldwide/prevtable (Accessed: 25 February 2005).
10. Crawford D, Campbell K. Lay definitions of ideal weight and overweight. International Journal of Obesity and Related Metabolic Disorders 1999: 23: 738-745.
11. Timperio A, Cameron-Smith D, Burns C, Crawford D. The public's response to the obesity epidemic in Australia: weight concerns and weight control practices of men and women. Public Health and Nutrition 2000: 3: 417-424.
12. Crawford D, Owen N, Broom D, Worcester M, Oliver G. Weight-control practices of adults in a rural community. Australian and New Zealand Journal of Public Health 1998: 22: 73-79.
13. Donath SM. Who's overweight? Comparison of the medical definition and community views. Medical Journal of Australia 2000: 172: 375-377.
14. Coyne TJ, Findlay MG, Firman DW, Ibiebele TI. Overweight and obesity in Australia: an underestimate of the true prevalence? Medical Journal of Australia 2004: 180: 93-94.
15. Paxton SJ, Sculthorpe A, Gibbons K. Weight-loss strategies and beliefs in high and low socioeconomic areas of Melbourne. Australian Journal of Public Health 1994: 18: 412-417.
16. Craig PL, Caterson ID. Weight and perceptions of body image in women and men in a Sydney sample. Community Health Studies 1990: 14: 373-383.
17. Crawford DA, Baghurst KI. Diet and health: a national survey of beliefs, behaviours and barriers to change in the community. Australian Journal of Nutrition and Dietetics 1990: 47: 97-104.
18. Crawford D, Worsley A, Syrette J. Victorian adults' nutrition opinions and concerns: results of a statewide survey. Journal of Food and Nutrition 1987: 44: 36-40.
19. Strong K, Trickett P, Titulaer I, Bhatia K. Health in rural and remote Australia. AIHW Cat no PHE 6. Canberra: Australian Institute of Health and Welfare, 1998.
20. Harper C, Cardona M, Bright M, Neill A, McClintock C, McCulloch B et al. Health Determinants Queensland 2004. Brisbane, QLD: Public Health Services, Queensland Health, 2004.
21. Australian Institute of Health and Welfare. Rural, regional and remote health: a guide to remoteness classifications. AIHW Cat no PHE 53. Canberra, ACT: AIHW, 2004.
22. WHO Expert Committee. Physical status: the use and interpretation of anthropometry. WHO Technical Report Series 854. Geneva: WHO, 1995.
23. Australian Bureau of Statistics. Health risk factors. 4812.0. Canberra: Australian Bureau of Statistics, 2001.
24. Australian Bureau of Statistics. Australian Social Trends 2005. Canberra: Australian Bureau of Statistics, 2005.
25. Avis NE, McKinlay JB, Smith KW. Is cardiovascular risk factor knowledge sufficient to influence behavior? American Journal of Preventive Medicine 1990: 6: 137-144.
26. Kupper B, Krause P, Glaesmer H, Wittchen HU. [How do risk patients with overweight/obesity differ in their health knowledge and behaviour from patients with normal weight? A study in primary medical care]. Gesundheitswesen 2004: 66: 361-369. (In German)
27. Thorburn AW. Prevalence of obesity in Australia. Obesity Review 2005: 6: 187-189.
28. Booth ML, Hunter C, Gore CJ, Bauman A, Owen N. The relationship between body mass index and waist circumference: implications for estimates of the population prevalence of overweight. International Journal of Obesity and Related Metabolic Disorders 2000: 24: 1058-1061.
29. Kragelund C, Omland T. A farewell to body-mass index? Lancet 2005: 366: 1589-1591.
30. Yusuf S, Hawken S, Ounpuu S, Bautista L, Franzosi MG, Commerford P et al. Obesity and the risk of myocardial infarction in 27,000 participants from 52 countries: a case-control study. Lancet 2005: 366: 1640-1649.
31. Hartz AJ, Rupley DC, Rimm AA. The association of girth measurements with disease in 32,856 women. American Journal of Epidemiology 1984: 119: 71-80.
32. Ohlson LO, Larsson B, Svardsudd K, Welin L, Eriksson H, Wilhelmsen L et al. The influence of body fat distribution on the incidence of diabetes mellitus. 13.5 years of follow-up of the participants in the study of men born in 1913. Diabetes 1985: 34: 1055-1058.
33. Pouliot MC, Despres JP, Lemieux S, Moorjani S, Bouchard C, Tremblay A, Nadeau A, Lupien PJ. Waist circumference and abdominal sagittal diameter: best simple anthropometric indexes of abdominal visceral adipose tissue accumulation and related cardiovascular risk in men and women. American Journal of Cardiology 1994: 73: 460-468.
34. Richelsen B, Pedersen SB. Associations between different anthropometric measurements of fatness and metabolic risk parameters in non-obese, healthy, middle-aged men. International Journal of Obesity and Related Metabolic Disorders 1995: 19: 169-174.
35. Han TS, van Leer EM, Seidell JC, Lean ME. Waist circumference action levels in the identification of cardiovascular risk factors: prevalence study in a random sample. BMJ 1995: 311: 1401-1405.
36. Zhu S, Wang Z, Heshka S, Heo M, Faith MS, Heymsfield SB. Waist circumference and obesity-associated risk factors among whites in the third National Health and Nutrition Examination Survey: clinical action thresholds. American Journal of Clinical Nutrition 2002: 76: 743-749.
37. Dalton M, Cameron AJ, Zimmet PZ, Shaw JE, Jolley D, Dunstan DW et al. Waist circumference, waist-hip ratio and body mass index and their correlation with cardiovascular disease risk factors in Australian adults. Journal of Internal Medicine 2003: 254: 555-563.
38. Bigaard J, Frederiksen K, Tjonneland A, Thomsen BL, Overvad K, Heitmann BL, Sorensen TI. Waist circumference and body composition in relation to all-cause mortality in middle-aged men and women. International Journal of Obesity 2005: 29: 778-784.
39. Welborn TA, Dhaliwal SS, Bennett SA. Waist-hip ratio is the dominant risk factor predicting cardiovascular death in Australia. Medical Journal of Australia 2003: 179: 580-585.
40. Haffner SM, Mitchell BD, Stern MP, Hazuda HP, Patterson JK. Public health significance of upper body adiposity for non-insulin dependent diabetes mellitus in Mexican Americans. International Journal of Obesity and Related Metabolic Disorders 1992: 16: 177-184.
41. IFOP- Canada Market Research. Shape of the Nation - Australia Country Report. Sydney, NSW: Sanofi Aventis, 2006.
42. Dixon T, Waters AM. A growing problem: trends and patterns in overweight and obesity among adults in Australia, 1980-2001. Bulletin No 8 Cat No AUS 36. Canberra: Australian Institute of Health and Welfare, 2003.
43. Gill T, Chittleborough C, Taylor A, Ruffin R, Wilson D, Phillips P. Body mass index, waist hip ratio, and waist circumference: which measure to classify obesity? Soz Praventivmed 2003: 48: 191-200.
44. Neumark-Sztainer D, Sherwood NE, French SA, Jeffery RW. Weight control behaviors among adult men and women: cause for concern? Obesity Research 1999: 7: 179-188.
45. Bowen DJ, Tomoyasu N, Cauce AM. The triple threat: a discussion of gender, class, and race differences in weight. Women Health 1991: 17: 123-143.
46. Reeder A, Trevena J. Adults' perceptions of the causes and primary prevention of common fatal cancers in New Zealand. New Zealand Medical Journal 2003: 116: U600.
47. Waller J, McCaffery K, Wardle J. Measuring cancer knowledge: comparing prompted and unprompted recall. British Journal of Psychology 2004: 95: 219-234.
48. Wardle J, Waller J, Brunswick N, Jarvis MJ. Awareness of risk factors for cancer among British adults. Public Health 2001: 115: 173-174.
49. Consedine NS, Magai C, Conway F, Neugut AI. Obesity and awareness of obesity as risk factors for breast cancer in six ethnic groups. Obesity Research 2004: 12: 1680-1689.
50. Lavoie KL, Bacon SL, Labrecque M, Cartier A, Ditto B. Higher BMI is associated with worse asthma control and quality of life but not asthma severity. Respiratory Medicine 2006; 100: 648-657.
51. Braback L, Hjern A, Rasmussen F. Body mass index, asthma and allergic rhinoconjunctivitis in Swedish conscripts - a national cohort study over three decades. Respiratory Medicine 2005: 99: 1010-1014.
52. Schaub B, von Mutius E. Obesity and asthma, what are the links? Current Opinion in Allergy and Clinical Immunology 2005: 5: 185-193.
53. Calle EE, Kaaks R. Overweight, obesity and cancer: epidemiological evidence and proposed mechanisms. National Review of Cancer 2004: 4: 579-591.
54. Pi-Sunyer FX. Comorbidities of overweight and obesity: current evidence and research issues. Medical Science of Sports and Exercise 1999: 31: S602-S608.
55. Wang Z, Patterson CM, Hills AP. A comparison of self-reported and measured height, weight and BMI in Australian adolescents. Australian and New Zealand Journal of Public Health 2002: 26: 473-478.
56. Flood V, Webb K, Lazarus R, Pang G. Use of self-report to monitor overweight and obesity in populations: some issues for consideration. Australian and New Zealand Journal of Public Health 2000: 24: 96-99.
57. Bostrom G, Diderichsen F. Socioeconomic differentials in misclassification of height, weight and body mass index based on questionnaire data. International Journal of Epidemiology 1997: 26: 860-866.
58. Australian Bureau of Statistics. How Australians measure up. ABS Cat. No. 4359.0. Canberra, Australian Government Publishing Service, 1998.
59. Spencer EA, Appleby PN, Davey GK, Key TJ. Validity of self-reported height and weight in 4808 EPIC-Oxford participants. Public Health and Nutrition 2002: 5: 561-565.
60. Waters AM. Assessment of self-reported height and weight and their use in the determination of body mass index. AIHW Cat No AIHW-023. Canberra: Australian Institute of Health and Welfare, 1993.


