Introduction
Leptospirosis is a globally important zoonotic disease that affects humans on all continents, in both urban and rural contexts, and in temperate and tropical climates. However, rural areas of tropical countries are the present endemic areas for leptospirosis. Leptospirosis is a disease of the environment; transmission depends on interaction between humans and mammalian reservoir hosts1. The disease is spread by ingestion of contaminated animal urine1. If leptospirosis is untreated, severe complications including renal failure and death can result.
Leptospirosis has a high prevalence in the northeastern area of Thailand2,3. The annual number of reported leptospirosis cases increased to 14 285 cases in 2000, and the peak endemic areas are Buriram, Nakornratchasrima and Surin provinces in the northeast region4. It is locally known as 'Rhok-Chee-Nhu' or 'rat urine disease'. The etiology of the disease is pathogenic Leptospira species, locally known as 'Lep-to'. The main risk factor of this disease is bare-footed human activity during daily work in the rice fields. Other risk factors include accidental exposures to contaminated swamp and water sources. Presenting symptoms vary with age, with children displaying primarily fever, vomiting, headache, abdominal and generalized muscle pain and diarrhea; whereas adults present with fever, headache, anorexia, muscle pain and constipation5.
To control outbreaks of leptospirosis, which have occurred repeatedly in Thailand for many years, preventive actions are necessary. Presently the Thai Ministry of Public Health is active in its interventions against the disease, including using the primary health-care system in rural communities. Interventions include control programs and health education of the local community. Due to a recent Thai Ministry of Public Health analysis, educational efforts on basic knowledge of the disease were enhanced in areas where leptospirosis is endemic to encourage the use of protective clothing. In addition, wound management and the avoidance of potentially contaminated water when skin wounds are present was included in health education programs6. Indeed, health education on basic knowledge of the disease is the core of successful prevention of leptospirosis, as indicated in many international reports7,8.
In Thailand, although control programs have been launched in the endemic areas for many years, an annual outbreak of leptospirosis still occurs. In addition, there are only a few reports of the successful evaluation of heath education programs in the endemic areas. Good practice is based on good knowledge; therefore, a knowledge survey of villagers in the endemic area was planned. In addition, such a survey can provide an indicator of the success of interventions. This cross-sectional descriptive study was conducted among a sample of rural villagers in the highly endemic area of leptospirosis in Thailand, to assess their knowledge of leptospirosis.
Methods
Setting
This cross-sectional descriptive study was designed as a pilot study. The study focused on Kok Yang Subdistrict, Buriram Province, where the prevalence of leptospirosis was reported as 1% (Office of Rural Development, Prakhonchai District, unpubl. data, 1999). The location is approximately 400 km from Bangkok, the capital of Thailand. Most villagers in this district are farmers, a high risk group for leptospirosis. The studied village is under the control efforts of the Thai Ministry of Public Health. This survey was performed during May 2001 at the beginning of the rainy season, the season with the highest prevalence of leptospirosis2,5.
Knowledge survey
A total of 300 villagers (approximately 20% of the total population in this subdistrict) were sampled by simple randomization. A self-administered questionnaire interview on aspects of knowledge about leptospirosis was used as the data collection tool. The questionnaire was produced after a review of the specific literature on leptospirosis in Thailand and also of tropical infectious diseases9,10. All questions were selected according to identified common misguided knowledge among Thais. In addition, this questionnaire was tested by the Kuder-Richardson method and gave a reliability of equal to 0.83.
The questionnaire was composed of 10 true or false questions (Fig 1). One point was given for each correct answer and zero for each incorrect answer. The answer 'do not know' was classified as an incorrect answer. The total score per subject was calculated as a percentage and graded according to the modification evaluation criteria for knowledge of the Thai Ministry of Education: good >79%, fair 50-79%, poor 0-49%.

Figure 1: Questionnaire used in this study.
Data analysis
All data collected from interviewing were analyzed using descriptive statistics. A correlation analysis was also applied in order to determine the relationship between two variables. Descriptive statistical analysis was applied where appropriate. Chi-squared at a significance level of 0.05 was used to test for independence. All statistical analysis in this study was performed using SPSS for Windows (SPSS Inc; Chicago, IL, USA).
Results
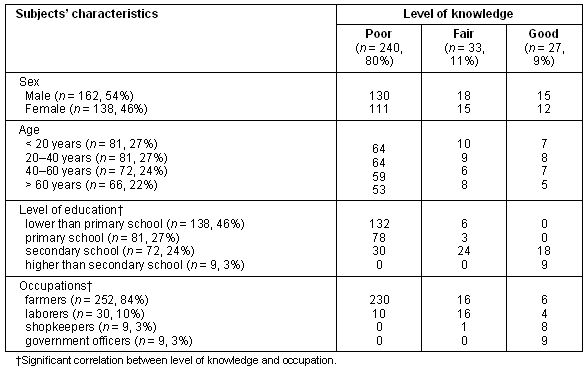
The response rate from the 300 subjects was 100% (Table 1). It was found that 80% of the subjects had an overall poor knowledge, 11% had fair knowledge and 9% had good knowledge of the disease. There was no significant correlation of sex and age of the subjects to the level of knowledge (c2, p > 0.05); however, there was significant correlation of the level of education and occupation of the subjects to the level of knowledge of the disease (c2, p < 0.05) (Table 1).
Table 1: Knowledge of the subjects in this study
Discussion
To stop repeated outbreaks of leptospirosis in Thailand, the Thai Ministry of Public Health has set control programs, focusing on promotion of knowledge about the leptospirosis via the mass media. However, there appear to be some gaps in knowledge between rural and urban people, due to the different opportunities to gain such knowledge, with rural people being less knowledgeable11. Because the endemic area of leptospirosis is the rural area, the disease is still prevalent in Thailand3,12.
At rural village level there are repeated leptospirosis outbreaks. Although this disease is well known among the rural Thais, the average knowledge scores of the villagers about leptospirosis was poor or fair. Of interest, almost all subjects (270/300; 90%) held the false belief that eating and drinking contaminated food results in leptospirosis infection. This may imply that the villagers know the disease relates to rat urine but that they have no knowledge of the mode of transmission. This may contribute to poor disease control. In addition, although the study setting was in an area of high disease prevalence, some subjects held incorrect knowledge about it, such as 'screaming like a rat' being the main symptom of the disease. Some also indicated their belief that leptospirosis was caused by contamination of their food by insecticide.
Similar to a previous study focusing on the health knowledge of the Thai rural population12, we found that education level was a significant parameter relating to knowledge of the subject. The finding of the relationship between the subjects' occupation and knowledge is typified by the fact that a government officer who had the overall highest knowledge had the highest educational level. Although previous studies identify the potential of environment (surroundings) and travel factors to increase knowledge of leptospirosis control12-14, the effect of awareness campaigns should not be overlooked. In addition, poor knowledge of leptospirosis implied the need for repeated health education for villagers, especially for those with low education, as control efforts.
Conclusions
The results of the present pilot study reflect an interesting pattern in the knowledge of villagers in this endemic area, and hint at the shortcomings of the control program. It implies that the present leptospirosis control program does not succeed fully, and that the main problem is the lack of knowledge of the people in endemic areas. A program to improve the basic knowledge of leptospirosis of rural villagers in the endemic areas is called for. This could be done by adding to the current broadcasting via the mass media to the targeted population. Based on a recent report8, the role of village health volunteers in knowledge promotion should also be encouraged.
Acknowledgements
The author thanks all the official workers and villagers of Kok Yang Subdistrict, Prakhonchai District, Buriram Province who participated in this study. The author would also like to thank the staff and students of the Mulitdisciplinary Study Project, Chulalongkorn University, for their help in and support of this study.
References
1. Vinetz JM. Leptospirosis. Current Opinion of Infectious Diseases 2001; 14: 527-538.
1. Sundharagiati B, Harinasuta C, Photha U. Human leptospirosis in Thailand. Transcripts of the Royal Society of Tropical Medicine and Hygiene 1966; 60: 361-365.
3. Tangkanakul W, Tharmaphornpil P, Plikaytis BD et al. Risk factors associated with leptospirosis in northeastern Thailand, 1998. American Journal of Tropical Medicine and Hygiene 2000; 63: 204-208.
4. Tangkanakul W, Smits HL, Jatanasen S et al. Leptospirosis: an emerging health problem in Thailand. Southeast Asian Journal of Tropical Medicine and Public Health 2005; 36: 281-288.
5. Heisey GB, Nimmanitya S, Karnchanachetanee C et al. Epidemiology and characterization of leptospirosis at an urban and provincial site in Thailand. Southeast Asian Journal of Tropical Medicine and Public Health 1988; 19: 317-322.
6. Phraisuwan P, Whitney EA, Tharmaphornpilas P et al. Leptospirosis: skin wounds and control strategies, Thailand, 1999. Emerging Infectious Diseases 2002; 8: 1455-1459.
7. John TJ. The prevention and control of human leptospirosis. Journal of Postgraduate Medicine 2005; 51: 205-209.
8. Cachay ER, Vinetz JM. A global research agenda for leptospirosis. Journal of Postgraduate Medicine 2005; 51: 174-178.
9. Ettinger SJ, Feldman EC (Eds). Texbook of veterinary internal medicine - diseases of the dog and cat, 4th edn. Philadelphia: WB Saunders, 1995.
10. Charoonves N (Ed.). Tropical diseases, 2nd edn. Bangkok: Reun Kaew, 1991.
11. Rakue Y, Panasoponkul C, Suthienkul O, Radomyos P. Overview reflection of primary health care in Thailand supported from 1976 to 1996 by Japan-Thailand partnership. Southeast Asian Journal of Tropical Medicine and Public Health 1998; 29: 622-627.
12. Tangkanakul W, Siriarayaporn P, Pool T, Ungchusak K, Chunsuttiwat S. Environmental and travel factors related to leptospirosis in Thailand. Journal of the Medical Association of Thailand 2001; 84: 1674-1680.
13. Wiwanitkit V. A study on attitude towards blood donation among people in a rural district, Thailand. Southeast Asian Journal of Tropical Medicine and Public Health 2000; 31: 609-611.
14. Kauffman KS, Myers DH. The changing role of village health volunteers in northeast Thailand: an ethnographic field study. International Journal of Nursing Studies 1997; 34: 249-255.
Abstract
Introduction: The main purpose of this pilot study was to assess knowledge of leptospirosis among a sample of rural villagers in the highly endemic area, Thailand.
Method: This cross-sectional descriptive study was conducted among a sample of 300 rural villagers in the highly endemic area of leptospirosis, Buriram Province in Thailand. A self-administered questionnaire on some knowledge aspects of leptospirosis was used.
Results: The response rate was 100%. Most participants (80%) had a poor knowledge of leptospirosis. There was no significant correlation of sex and age of the subjects as to the level of knowledge (c2, p 0.05); however, there was significant correlation of level of education and occupation of the subjects to the level of their knowledge (c2, p < 0.05).
Conclusions: Although this was a limited pilot study, the results imply that the present leptospirosis control program is not successful, and that the main problem is the knowledge level of people in endemic areas. A program to improve the basic knowledge of leptospirosis of rural villagers in endemic areas must be initiated.
Key words: leptospirosis, Thailand.
You might also be interested in:
2015 - Re-orienting a remote acute care model towards a primary health care approach: key enablers
