Changes to medical education
Since the 1990s, the methods used for the training and teaching of medical students have undergone change1-4. Pressure for a move away from the centuries old pathways of training5 has resulted in gradual changes occurring in medical schools worldwide6,7. In a traditional medical education framework, students typically learn through didactic teaching methods within curricula that focus on conceptual knowledge and understandings, and the acquisition of large amounts of factual knowledge5,8,9. The process of change has given rise to innovative and radical restructurings of medical curricula across the globe. Vertical and horizontal integration of the medical curricula has been part of the restructuring evident in many medical schools. Horizontal integration occurs through the integration of knowledge and skills between the basic clinical science subjects through a multi-disciplinary approach, while vertical integration places emphasis on the integration of basic science with clinical science within the clinical context5,10. Approaches to medical education based on a problem-solving model provide a framework to apply principles of horizontal and vertical integration10,11.
Concurrent changes in the tertiary level hospital system, traditionally a key-learning site for the medical student, has also affected medical training2,12,13. As hospitals increasingly become short-stay institutions with a focus on same-day treatments and early discharge, only the more critically ill patients remain for a longer time2,5,14,15. Therefore, medical students no longer always have access to a full range of educational experiences, having less opportunity to observe and assess patients with a wide variety of diseases, illnesses and physical signs/symptoms15-18.
The transference of theoretical knowledge to the diagnosis and management of acutely ill patients has long been a major challenge for medical students and their teachers. Traditionally the acquisition and ongoing improvement of higher level psychomotor skills required to be a clinician took place in an apprentice-style model of 'see one, do one, teach one' typically occurring during the intern and registrar years in a tertiary hospital setting8,9,19. However, this apprentice-style learning approach is no longer considered viable or acceptable20,21. Numerous researchers have indicated increasing concern for patient care and safety8,9,19,22-24, particularly in light of the landmark report issued by the US Institute of Medicine in 1999, To Err is Human, which highlighted the role of human error and organisational issues in compromising patient safety25. There exists a 'gap' between the need for medical students to acquire the necessary skills, obtain sufficient practice to develop proficiency, and the safety and wellbeing of the patient8,26. Relying on exposure to hospital patients during training years may result in an ad hoc method of learning clinical skills, as it is dependent upon case presentations possibly leading to less than optimal development and performance of clinical skills26.
The changing role of hospitals is of particular import to those Australian medical students who are undertaking a component of their medical training in rural and regional areas of Australia. As part of a national strategy to alleviate the shortage of doctors in rural Australia, a number of medical schools have developed programs in which medical students spend varying amounts of time in rural and regional locations27-29. This raises concerns regarding whether rural and regionally based medical students have similar opportunities to access the diversity of clinical and educational experiences to their urban counterparts learning in tertiary teaching hospitals. Rural and regional hospitals cannot always offer the same range of healthcare services available in urban and metropolitan areas.
The dynamic, uncertain and high-pressured environments of emergency departments and intensive care units where critically ill patients are managed, present challenging environments for students to learn core psychomotor and clinical reasoning skills. In order to integrate basic and clinical sciences, experience is critical; however, medical students are usually excluded from the primary management of acutely ill patients24. In such dynamic environments there is often no opportunity for students to receive constructive feedback when they are able to participate, and little opportunity for reflection8.
Current societal and medical concerns for patient safety have led to calls for alternative teaching modalities that include non-patient based training for the acquisition and maintenance of clinical skills9,22. One method of providing medical students with the psychomotor skills necessary for their education, which is risk free to patients while simultaneously providing a realistic clinical experience, is through simulation experiences that use a variety of clinical simulators. Simulation has been defined as: 'a generic term that refers to the artificial representation of a real-world process to achieve educational goals via experiential learning'8, and cover a wide range of clinical simulators, from part-task trainers through to computer activated full-scale human simulators.
History of simulation training
Modern simulator training had its beginnings in the aviation industry when Edward Link developed flight simulators to train pilots in the 1920s. This method of training proved to be efficient and cost-effective and has remained a standard tool for initial and ongoing training of pilots30. In the early 1970s, simulation training was further developed in the field of aviation to teach crisis management, as well as fostering teamwork and leadership31-33.
Applications of simulation technology in medicine, however, were less frequent than in other fields, and have only emerged in the last two decades34. The development of simulators for use in medical training was first established in the field of anaesthetics and took on the conceptual framework developed by the aviation industry for managing clinical crisis and promoting teamwork, commonly known as crisis resource management24,25,32,33,35. The need for effective, non-human based training methods for medical personnel36 merging of computer technology and medical science24, as well as advances in bioengineering and learning and behavioural sciences37, contributed towards the development of sophisticated computer driven, life-sized mannequins. These mannequins model human anatomy and physiology and can be used in a variety of simulated clinical settings, from standard hospital wards to intensive care units, as well as outside scenarios24,36,37.
The specialities of anaesthetics, cardiology, critical care and surgery have led the way in using simulators for teaching clinical skills38; however, it is only recently that the implications of using simulators in medical education have been considered24. There are numerous articles that provide detailed descriptions of simulators, ranging from computer-based programs and part-task simulators to full-scale human patient simulators (HPS)22,24,25,39-41.
Clinical simulators as a learning tool
Clinical simulators have become established as an accepted teaching tool and are considered powerful learning aids that provide a mechanism to integrate basic and clinical sciences8,21,24. Learning experiences that use simulation technology do not intend to supplant the necessity of learning in a clinical setting. Rather, these experiences provide participants with the chance to learn and practice in a controlled environment, and through such improved preparation, enhance clinical experiences as well as patient care and outcomes22,40. As such, simulation imitates, but does not duplicate reality - it is a controlled 'real-world-like' medical setting34. Because the simulation replicates the cognitive and behavioural responses that would occur in real settings, the environment in which it takes place must fashion a sense of realism34. The re-creation of 'reality' or 'fidelity' is important for the success of the simulation and for the participant32.
Educational processes underpinning the use of simulation as a teaching tool are the opportunity for deliberate practice, reflection and feedback22. Simulation technology is believed to improve the acquisition and retention of knowledge in comparison with other more traditional educational approaches35. Benefits of simulation include:22,24,30,35,38,42
- practising 'hands on' and invasive procedures
- exposure to rare and complex clinical situations
- the ability to allow errors to continue to their natural conclusion
- the opportunity for the same scenario to be accessed by multiple students providing similar learning opportunities
- planning clinical cases based on student need, rather than patient availability
- immediate feedback
- continuing practice
- the use of real medical equipment
- learning in a risk free environment.
Another important feature of simulation-based education is that it can teach aspects of medical care not always readily or easily taught: teamwork, leadership, interpersonal communication skills, stress management, decision-making and the ability to prioritise tasks under pressure8. Participants are encouraged to take an active role in the management of crisis, helping to teach these other skills9. The traditional apprentice-style model of learning is replaced with an experiential learning experience in which participants interact in 'real' time, with authentic equipment, yet also have the opportunity to reflect, rehearse and repeat scenarios to maximise learning outcomes38.
One of the key learning tools associated with the use of clinical simulators, in particular scenarios using the HPS, is the ability to videotape the scenario, providing accurate and immediate feedback to participants. This process of debriefing is an integral part of any experiential learning process. In a number of studies, participants have reported gaining substantial benefit from the debriefing process, in addition to the benefits of working through a problem-based scenario25,38. Viewing the videotape as part of the debriefing process helps participants focus on the cognitive processes of problem recognition, decision-making and management issues. Additionally, the non-technical skills of teamwork and interpersonal communication can be considered25. A recent study by Nilsen and Baerheim explored medical students' experiences of receiving feedback from their videotaped consultations43. It found that while students felt the videotaped feedback 'acceptable, useful and inspiring', they also experienced anxiety and apprehension about being videotaped. While videotaping has been shown to enhance communication skills and be more effective long term than other teaching and feedback methods, few training programs use this method43.
Clinical skills centres
Clinical skills centres featuring a variety of clinical simulators have been established to provide a safe, non-threatening environment for skill acquisition and maintenance at all levels of medical education17. There are an increasing number of simulation centres worldwide. A 2002 study by Weller stated that at the end of 2001 the Bristol Medical Simulation Centre had identified 207 centres worldwide41; however, a 2004 article30 estimated that there were more than 1000 simulation centres globally, demonstrating the rapid expansion of the use of simulators in medical education and training17,30.
The use of clinical skills centres has the potential to confer benefits at all stages of medical education, from early undergraduate years to the provision of ongoing education for a diversity of healthcare professionals. Continuing medical education (CME) provides a crucial role in the maintenance and upgrading of skills and knowledge for practising clinicians and other healthcare professionals. This is essential to remain up to date with the continually changing body of knowledge within medicine and associated specialities and to improve patient outcomes44,45. The use of full-scale clinical simulators for crisis management has proved a popular and effective CME workshop for medical specialists46. Simulation can be used in the training of multidisciplinary teams in high-risk areas such as trauma, operating rooms, critical care, obstetrics and disaster management21.
Development of a regional clinical simulation centre
The Rockhampton Clinical Skills Learning Centre (CSLC) utilises modern clinical simulator technology and was established as a joint venture between the University of Queensland Rural Clinical School (RCS), and Mercy Health and Aged Care (MHAC), based in Rockhampton, central Queensland, Australia. The RCS was funded by a project grant from the Federal Department of Health and Ageing, with recurrent funds used to purchase the equipment. MHAC provided the building, funded the required renovations and provided ongoing building maintenance and other technical support. To the best of our knowledge, in 2005 the Rockhampton CLSC was the only fully equipped clinical simulation centre established outside a capital city in Australia.
The aim of a clinical skills centre is to replicate fully functioning medical settings, for example, emergency departments, operating rooms, intensive care units or patient rooms37. The CSLC followed this aim and was housed in a purpose-designed room, adjacent to the other facilities of the RCS that are based at the MHAC. The teaching area was 6.2 m2, with an adjacent storage, preparation and wet area 6 x 3 m in size. The hospital bed, HPS, standard emergency resuscitation trolley, defibrillator, monitors, oxygen and suction occupied most of the teaching area. The desk for the computer and operator and video equipment was to the side in the remainder of the room. Enough space was available for participants and facilitators to sit comfortably and observe the projected videotape of the scenario, PowerPoint presentations from an overhead mounted data projector or utilise the whiteboard.
Equipment
The CSLC utilised a variety of medical simulation technologies from part task trainers, to computer-based simulations and full-scale HPS. The core HPS of the CSLC were SimMan©, MegaCode Kid VitalSim? and Laerdal ALS Baby?. Specific part-task trainers that replicate sections of the anatomy and designed for training psychomotor skills in specific areas supplemented the HPS (Table 1).
Table 1: Human patient simulators used in the Clinical Simulation Learning Centre
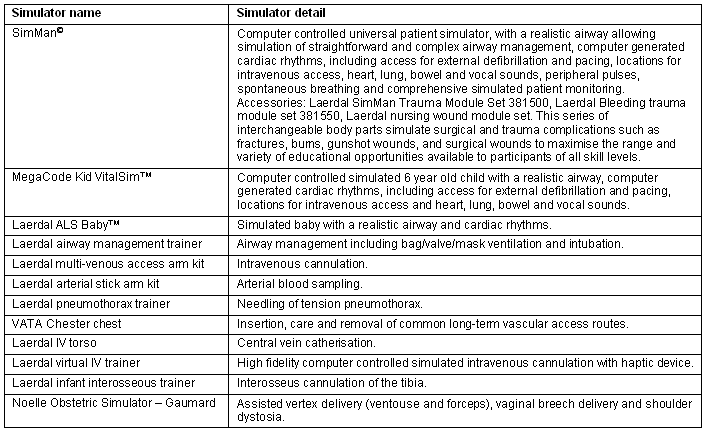
Both a Lifepak® 12 defibrillator monitor and a Heartstart® FR2 automatic defibrillator were utilised. Wall oxygen and suction, as well as a simulated emergency alarm were installed. A standard emergency room trolley was stocked with routine disposable equipment for airway management, circulation management, simulated medications, urethral catheterisation and bandages.
The use of multiple simulators enhances the opportunities for maximal educational benefit through the provision of a range of learning opportunities, from the early training of clinical skills to advanced CME of high-fidelity scenarios of an ICU, emergency department or other settings.
Use of a clinical simulation centre: an example of a CSLC program for University of Queensland medical students
As the aim of the CSLC program was for students to be actively engaged, acquire new knowledge in 'real' clinical settings and then be able to determine the relevance of the learning through the scenario and feedback process41 educational experiences were constructed around two distinct modes; core skills training and simulation based scenarios. Cores skills training utilised a hands-on approach with a series of part-task trainers to develop the psychomotor skills required for managing the airway, access to the circulation and cardiac dysrhythmias. This was taught in small groups with high staff : student ratios (usually 1:2) utilising guided experiential learning, allowing each learner to advance their personal skills at their own pace within the context of prior knowledge. The tasks acted as triggers for more detailed discussions about associated aspects of clinical management.
On completion of core skill training, learners progressed to the HPS based scenarios. The introductory session was designed to equip participants with both the special rules for safe practice of the HPS (eg use of lubrication for intubation) and a clear understanding of the strengths and weaknesses of the HPS. Simulation sessions were conducted in a standardised format that was clearly explained to all participants. The simulation exercise was performed in groups of four learners, with one selected by the group to be the team leader. The team leader initially entered the CSLC and was provided with a brief verbal outline of the problem at hand by an experienced facilitator. The simulated emergency alarm system was then used to summon the team waiting outside, who were subsequently briefed on the situation and assigned tasks by the team leader. The team leader was encouraged to use written flow sheet to record events.
The facilitators observed the process and verbally described clinical findings for key events that the simulation process was unable to provide, such as pupil size and responsiveness to light, but no other comments were supplied. The predetermined end point of the scenario was typically completion of handing over the patient to a senior colleague, retrieval team or other personnel. The 'patient' never 'died' in the scenario, to avoid negative learning experiences, with the exception of a learning session for year 4 students, specifically designed to explore the psychosocial issues associated with unsuccessful resuscitation of a child. This session was conducted with a psychiatrist as one of the facilitators and a simulated patient acting as the parent, demonstrating the integration of multiple disciplines.
On completion of the simulation, participants and facilitators viewed the videotape together. The primary mode of learning was self-assessment and reflection, with the facilitators assisting as required especially with factual gaps in knowledge. Utilising a constructive, non-judgemental and supportive approach, learners were encouraged to identify both the positive and negative aspects of their performance and to assist in identifying gaps in knowledge and technique. The core topics considered in the debriefing session included leadership and teamwork, psychomotor skills, clinical judgement, choice of management, safety of the team members and planning, anticipation and preparation for (un)expected events. No permanent video recordings were kept.
The participants then repeated the scenario performing the same roles, providing an opportunity to reinforce new learning, and a second debriefing was performed. One major difference between this program and other reported curricula was the participants' second attempt at the scenario. This process has not been commonly mentioned in the educational literature regarding the use of HPS, yet anecdotal evidence from the participants at the Rockhampton CSLC found this to be a highly valued learning opportunity.
Applications for rural clinicians
Rural practitioners are often more involved in higher level assessment, emergency care due to the high incidence of trauma in rural areas, procedural based work, obstetrics, anaesthetics, surgery and community-based care than their urban counterparts47,48. While they do not deal with trauma on a daily basis, they are often responsible for the evaluation and management of the patient directly after injury49. In addition, rural practitioners are considered to have different needs in terms of knowledge and skills from clinicians practicing in urban regions. Smith and Hays found that the scope of knowledge and skills required by rural practitioners, outside their core knowledge base, increases with remoteness47. Hence, there is a critical need for ongoing CME in trauma care and other ongoing skills training relevant to the specificities of rural practice.
However, gaining access to CME is a challenge faced by many rural and regional healthcare professionals, due to their geographical isolation and distance from tertiary teaching hospitals44,50. Indeed, it has been argued that lack of access to regular CME is implicated in the difficulty incurred in recruiting and retaining a rural medical workforce44,48. Another factor for rural medicine is that it typically involves a multidisciplinary team approach47. The use of simulation technologies provides an innovative mechanism to enhance knowledge and skills involved in crisis resource management, vertical integration and collaborative up-skilling among rural healthcare professionals within a multidisciplinary approach.
Two recent studies by von Lubitz et al.20 and Treloar51 explored the use of HPS as distance education tools through the application of enhanced telecommunication networks and HPS technology. These studies considered in particular the application for rural and remote practitioners. The von Lubitz study was conducted among the USA, France and Italy with two HPS sites, one in the USA and one in France. The Italian site was remote access only. Von Lubitz and colleagues argued that:
...training based on advanced technologies transcends barriers of distance, time and national medical guidelines. Hence, international simulation-based distance training may ultimately provide the most realistic platform for a large-scale training of emergency medical personnel in less developed countries and in rural/remote regions of the globe20.
The potential of this technology for providing relevant and timely CME programs to rural and remote Australian practitioners appears boundless.
Discussion
The CSLC was primarily established as an integrated learning facility for developing psychomotor skills in tandem with building effective teamwork, communication and task management skills. Use of the SimMan© simulator is a significantly less expensive option than other HPS and has been shown to be an effective tool41. The lower cost may make it a more viable option for RCS that may not necessarily have the same opportunities and access to clinical skills training as schools in larger metropolitan areas.
The use of clinical simulation has broad clinical applications in diverse fields of medicine, including emergency medicine, anaesthesia, critical care, paediatrics, obstetrics, family medicine and surgery35. The range of educational possibilities arising from use of the patient simulator as well as other part-task trainers, makes it an ideal learning tool not only for medical students, but also for multiple healthcare professionals. In accordance with the spirit and letter of Federal Government funding, the CSLC was viewed from the outset as both an educational resource for medical students and the wider healthcare community of central Queensland. To this end, the CSLC has already catered for ongoing professional development of both medical and nursing staff of the Royal Flying Doctor Service, an organisation whose staff provides retrieval and inter-hospital transfers of critically ill patients. Table 2 details the intended usage of the CSLC and demonstrates the potential applications of the CSLC as centre for training and retraining clinical skills, teamwork, crisis resource management, communication and task management skills. The CSLC has also provided an opportunity for a paediatrician to teach the use of oropharyngeal airways to the mother of a child with significant neurological problems, another example of the diverse applications of a clinical simulation centre.
Table 2: Learners utilising the Clinical Simulation Learning Centre, 2005
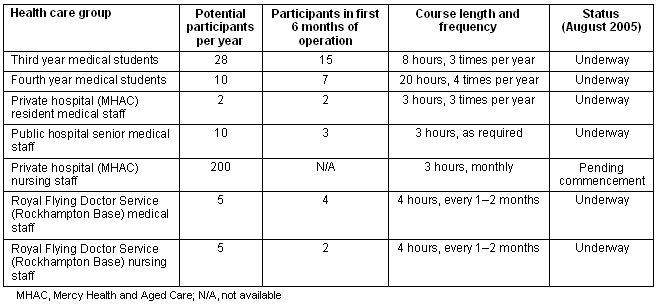
However, despite the growing number of simulation centres, there remains a dearth of information concerning the use and effectiveness of clinical simulators in undergraduate medical education. A 2005 systematic review of 670 articles on high-fidelity simulations in medical education, conducted under the auspices of the Best Evidence Medical Education collaborative, found that over 55% of these articles had been published in journals of surgery and biomedical engineering, with just over 5% published in medical education journals. Typically, the studies were small, with the number of participants being less than 30, and the modal participant was a postgraduate student in a medical speciality17.
Alongside this is the paucity of research that evaluates the effectiveness of clinical simulators in the education process at all levels, and its usefulness as an assessment tool. Many of the articles reviewed reported on medical participants' self-perceptions of the usefulness and effectiveness of clinical simulation training, rather than as a measurement tool to accurately assess skill acquisition and retention. There is a need for further research into the use of clinical simulators both in terms of quantitative measurable effectiveness and as a tool for assessment purposes.
Very few examples of the distance education applications of HPS and CME via enhanced telecommunication networks exist, yet there appears to be tremendous scope in the application of this technology to meet the needs of rural clinicians in Australia. If one of the barriers to retaining a rural medical workforce is lack of access to CME, this technology has the potential to address such obstacles. There exists the potential to conduct research in this area by further developing the capabilities of the Rockhampton CSLC to incorporate a distance based CME component that could involve rural healthcare workers in central Queensland in CME programs. Such collaborative ventures between the university, public and private hospitals, and healthcare providers, afford opportunities to maximise vertical integration in healthcare delivery in rural settings.
In conclusion, the CSLC has been a major capital investment in a relatively under-resourced part of regional/rural Australia, best justified by opening its doors to all healthcare professionals in the community; a process already underway.
Acknowledgements
The authors gratefully acknowledge the support of Professor Ken Donald, University of Queensland, School of Medicine, in the establishment of the Rockhampton Clinical Skills Learning Centre.
References
1. Oswald N, Alderson T, Jones S. Evaluating primary care as a base for medical education: the report of the Cambridge community-based clinical course. Medical Education 2001; 35: 782-788.
2. Murray E, Todd C, Modell M. Can general internal medicine be taught in general practice? An evaluation of the University College London model. Medical Education 1997; 31: 369-374.
3. Howe A. Patient-centred medicine through student-centred teaching: a student perspective on the key impacts of community-based learning in undergraduate medical education. Medical Education 2001; 35: 666-672.
4. Littlewood S, Ypinazar V, Margolis SA, Scherpbier A, Spencer J, Dornan T. Early practical experience and the social responsiveness of clinical education: systematic review. BMJ 2005; 331(7513): 387-391.
5. Elliott M. Are we going in the right direction? A survey of the undergraduate medical education in Canada, Australia and the United Kingdom from a general practice perspective. Medical Teacher 1999; 21: 53-60.
6. Flanagan B, Nestel D, Joseph M. Making patient safety the focus: crisis resource management in the undergraduate curriculum. Medical Education 2004; 38: 56-66.
7. Nargozian C. Teaching consultants airway management skills. Paediatric Anaesthesia 2004; 14: 24-27.
8. Flanagan B, Nestel D, Joseph M. Making patient safety the focus: crisis resource management in the undergraduate curriculum. Medical Education 2004; 38: 56-66.
9. Nargozian C. Teaching consultants airway management skills. Paediatric Anaesthesia 2004; 14: 24-27.
10. Snyman WD, Kroon J. Vertical and horizontal integration of knowledge and skills - a working model. European Journal of Dental Education 2005; 9: 26-31.
11. Dahle LO, Brynhildsen J, Behrbohm Fallsberg M, Rundquist I, Hammar M. Pros and cons of vertical integration between clinical medicine and basic science within a problem-based undergraduate medical curriculum: examples and experiences from Linkoping, Sweden. Medical Teacher 2002; 24: 280-285.
12. Howe A. Patient-centred medicine through student-centred teaching: a student perspective on the key impacts of community-based learning in undergraduate medical education. Medical Education 2001; 35: 666-672.
13. Oswald NT, Alderson TSJ, Jones S. Evaluating primary care as a base for medical education: the report of the Cambridge Community-based Clinical Course. Medical Education 2001; 35: 782-788.
14. Grant J, Ramsay A, Bain J. Community hospitals and general practice: extended attachments for medical students. Medical Education 1997; 31: 364-368.
15. Sturmberg J, Reid A, Khadra M. Medical education based in a rural area: a new direction in undergraduate training. Australian Journal of Rural Health 2001; 9: S14-S18.
16. Worley P, Silagy C, Prideaux D, Newble D, Jones A. The Parallel Rural Community Curriculum: an integrated clinical curriculum based in rural general practice. Medical Education 2000; 34: 558-565.
17. Issenberg SB, McGaghie WC, Petrusa ER, Gordon DL, Scalese RJ. Features and uses of high-fidelity medical simulations that lead to effective learning: a BEME systematic review. Medical Teacher 2005; 27: 10-28.
18. O'Sullivan M, Martin J, Murray E. Students' perceptions of the relative advantages and disadvantages of community-based and hospital-based teaching: a qualitative study. Medical Education 2000; 34: 648-655.
19. Nackman GB, Bermann M, Hammond J. Effective use of human simulators in surgical education. Journal of Surgical Research 2003; 115: 214-218.
20. von Lubitz DK, Carrasco B, Gabbrielli F, Ludwig T, Levine H, Patricelli F et al. Transatlantic medical education: preliminary data on distance-based high-fidelity human patient simulation training. Studies in Health Technology and Information 2003; 94: 379-385.
21. Morgan PJ, Cleave-Hogg D. Simulation technology in training students, residents and faculty. Current Opinions in Anaesthesiology 2005; 18: 199-203.
22. Maran NJ, Glavin RJ. Low- to high-fidelity simulation - a continuum of medical education? Medical Education 2003; 37(Suppl 1): 22-28.
23. Morgan PJ, Cleave-Hogg D. Evaluation of medical students' performance using the anaesthesia simulator. Medical Education 2000; 34: 42-45.
24. Gordon JA, Wilkerson WM, Shaffer DW, Armstrong EG. "Practicing" medicine without risk: students' and educators' responses to high-fidelity patient simulation. Academic Medicine 2001; 76: 469-472.
25. Gaba DM, Howard SK, Fish KJ, Smith BE, Sowb YA. Simulation-based training in anesthesia crisis resource management (ACRM): A decade of experience. Simulation and Gaming 2001; 32: 175-193.
26. Bradley P, Postlethwaite K. Setting up a clinical skills learning facility. Medical Education 2003; 37(Suppl 1): 6-13.
27. Worley P, Silagy C, Prideaux D, Newble D, Jones A. The parallel rural community curriculum: an integrated clinical curriculum based in rural general practice. Medical Education 2000; 34: 558-565.
28. Margolis SA, Davies LM, Ypinazar V. Isolated rural general practice as the focus for teaching core clinical rotations to pre-registration medical students. BioMed Central Medical Education 2005; 5: 22.
29. Sturnberg J, Reid A, Khadra M. Medical education based in a rural area: A new direction in undergraduate training. Australian Journal of Rural Health 2001; 9: S14-S18.
30. Grenvik A, Schaefer JJ 3rd, DeVita MA, Rogers P. New aspects on critical care medicine training. Current Opinion in Critical Care 2004; 10: 233-237.
31. Howard SK, Gaba DM, Fish KJ, Yang G, Sarnquist FH. Anesthesia crisis resource management training: teaching anesthesiologists to handle critical incidents. Aviation Space and Environmental Medicine 1992; 63: 763-770.
32. Zirkle M, Blum R, Raemer DB, Healy G, Robertson DW. Teaching emergency airway management using medical simulation: a pilot program. Laryngoscope 2005; 115: 495-500.
33. Reznek M, Smith-Coggins R, Howard S, Kiran K, Harter P, Sowb Y et al. Emergency medicine crisis resource management (EMCRM): pilot study of a simulation-based crisis management course for emergency medicine. Academic Emergency Medicine 2003; 10: 386-389.
34. Streufert S, Satish U, Barach P. Improving medical care: The use of simulation technology. Simulation and Gaming 2001; 32: 164-174.
35. McLaughlin SA, Doezema D, Sklar DP. Human simulation in emergency medicine training: a model curriculum. Academic Emergency Medicine 2002; 9: 1310-1318.
36. Tsai TC, Harasym PH, Nijssen-Jordan C, Jennett P, Powell G. The quality of a simulation examination using a high-fidelity child manikin. Medical Education 2003; 37(Suppl 1): 72-78.
37. Lane JL, Slavin S, Ziv A. Simulation in medical education: A review. Simulation and Gaming 2001; 32: 297-314.
38. Hammond J. Simulation in critical care and trauma education and training. Current Opinion in Critical Care 2004; 10: 325-329.
39. Wantman A, Chin C. Use of simulation in paediatric anaesthesia training. Paediatric Anaesthesia 2003; 13: 749-53.
40. Schaefer JJ 3rd. Simulators and difficult airway management skills. Paediatric Anaesthesia 2004; 14: 28-37.
41. Weller JM. Simulation in undergraduate medical education: bridging the gap between theory and practice. Medical Education 2004; 38: 32-38.
42. Good ML. Patient simulation for training basic and advanced clinical skills. Medical Education 2003; 37(Suppl 1): 14-21.
43. Nilsen S, Baerheim A. Feedback on video recorded consultations in medical teaching: why students loathe and love it - a focus-group based qualitative study. BioMed Central Medical Education 2005; 5: 28.
44. Curran VR, Fleet L, Kirby F. Factors influencing rural health care professionals' access to continuing professional education. Australian Journal of Rural Health 2006; 14: 51-55.
45. Weller J, Wilson L, Robinson B. Survey of change in practice following simulation-based training in crisis management. Anaesthesia 2003; 58: 471-473.
46. Weller JM. Simulation in undergraduate medical education: bridging the gap between theory and practice. Medical Education 2004; 38: 32-38.
47. Smith J, Hays R. Is rural medicine a separate discipline? Australian Journal of Rural Health 2004; 12: 67-72.
48. Allan JA, Schaefer D. Do the learning needs of rural and urban general practitioners differ? Australian Journal of Rural Health 2005; 13: 337-342.
49. Royal Australasian College of Surgeons. Introduction. In: EMST Handbook (a Supplement to the ATLS Course Manual). Melbourne: Royal Australasian College of Surgeons, 2004; 3-6.
50. Strasser RP, Hays RB, Kamien M, Carson D. Is Australian rural practice changing? Findings from the National Rural General Practice Study. Australian Journal of Rural Health 2000; 8: 222-226.
51. Treloar D, Hawayek J, Montgomery JR, Russell W. On-site and distance education of emergency medicine personnel with a human patient simulator. Military Medicine 2001; 166: 1003-1006.

