Introduction
Issues related to rural and remote medicine are widely distributed in medical science. A search of the Medline database reveals that there are 23 scientific journals related to various aspects of rural and remote health. The majority of articles from those journals come from large countries with isolated human settlements, for example Australia1, Canada2, and USA3, or from countries facing problems in the provision of health care in rural and remote areas.
A smaller number of published articles deal with the reverse phenomenon, the arrival of students from rural and remote backgrounds at medical schools in urbanised surrounding. Such students experience a number of novel and specific problems. Separation from family and friends, introduction of new cultural norms and financial issues are among the most commonly reported issues4. All these negative issues could hypothetically have a powerful effect on students' performance in highly demanding educational systems, such as medicine.
Students coming from rural settings are very valuable to the health system, because they are most likely to be employed in underserved geographic areas5. Other than rural upbringing, a crucial element for rural and remote workforce development is a positive educational experience as part of undergraduate medical education6, confirming the importance of the education system in recruiting to the rural and remote workforce7,8. Some medical schools have developed tailored programs to assist students from rural and remote backgrounds in managing various problems9, further contributing to the development of positive attitudes towards rural and remote placement10.
The aim of this study was to compare the academic performance and research involvement of medical students coming from rural and urban backgrounds in Croatia.
Methods
Subjects
We analysed the final (sixth) year Zagreb University Medical School students' academic performance and scientific involvement. Students were surveyed during the academic year 2004/2005, several months prior to their graduation. Surveys that contained insufficient information or intentionally misleading answers were excluded from the study (n = 7).
Students were divided into three groups, based on their background: (i) those coming from highly urbanised background (cities and towns with more than 35 000 inhabitants); (ii) mid-urban (towns with 15 000 to 35 000 inhabitants); and (iii) rural and remote background (rural settlements and remote towns with less than 15 000 inhabitants).
Survey questions
Survey questions were grouped into five sections: (i) general data; gender, age and place of origin; (ii) academic performance; grade point average and failed study year(s); (iii) research involvement, measured through involvement in research projects, number of published articles, and interest in career supplemented with research activities; (iv) extracurricular activities, with information related to student organization membership and hobbies; and (v) workplace preferences.
Statistical analyses
Several questions regarding research involvement had open-ended answers, which were categorized. Data were analysed in three-by-two contingency tables with c2 test. Fisher's exact test was used in contingency tables with too few cases for a c2-square to be used (less than five). We used the Kruskal-Wallis test in the analysis of grade point average and age, due to non-normal data distribution. Statistical analyses were performed with SPSS software, vers. 12.0.0 (SPPS Inc, Chicago, IL, USA), with significance set at p <0.05.
Results
The final sample consisted of 204 respondents (out of 240 enrolled students; response rate 85%). Most students were from highly urbanised background (n = 100, 49.0%), and least students were from rural and remote backgrounds (n = 29, 14.2%). There was no indication of gender gap or age difference among the groups (Table 1).
Table 1: Comparison of the three groups of students in relation to their background
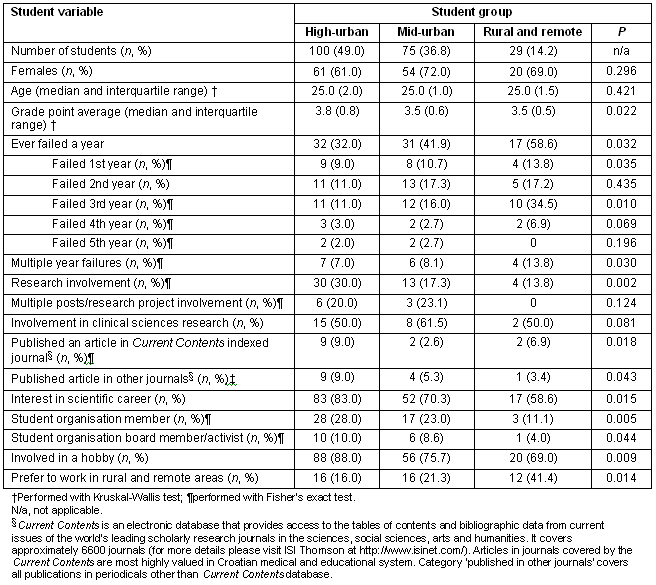
Students from a highly urbanised background reported the best grade-point average (Table 1). Rural and remote students were the most likely to experience failure in any study year. Multiple year failures were also commonest among rural and remote students (Table 1). Analysis of failures per each study year showed significant differences in the first and third study year. Most students from the entire sample reported failure in the third study year (33 students, 16.2%).
Students from a highly urbanised background were most commonly involved in research projects. Rural and remote students reported the lowest interest for scientific work in their future careers, and also the least involvement in extracurricular activities (Table 1). However, students from rural and remote backgrounds most commonly reported interest in employment in rural and remote areas (Table 1).
Discussion
The results presented in this study reveal substantial differences in self-reported academic performance and research involvement among the three groups of students coming from various urbanisation backgrounds. Students from a highly urbanised background reported the best academic and research indicators, closely followed by the mid-urban students.
This study exhibited rather homogenous student population in Zagreb University Medical School, with no age difference or gender gap among the three groups investigated. Such findings are unusual, because some studies exhibited significant age differences between rural and urban students3, and a higher interest for employment in rural areas among women11. Lack of a gender gap is even more interesting knowing that women predominate at the Medical School, University of Zagreb, being almost two-thirds of the entire student population12,13.
Grade-point average is the single most important academic performance indicator in Croatia. It is used in various situations, such as in scholarship awards and for internship and residency contests. Students from highly urbanised background reported the highest grade-point average in this study. However, grade-point average does not always reflect the student's knowledge14, nor accurately reflect clinical skills. Some studies even suggest that rural students exhibited better performance in clinical skills than their urban colleagues15.
Rural students were the most likely to fail a study year, and also experience multiple years' failing. Differences in failing the first study year could possibly be explained by the effect of rural and remote students adaptation to a new lifestyle, although without supporting data this assumption remains hypothetical. The differences in the third year failure might be a reflection of increased curricular encumbrance (third year consists of four major subjects: pathology, pathophysiology, pharmacology and microbiology), which seems to have mostly affected rural and remote students. The finding that most students in the entire sample failed the third study year might support the hypothesis of increased curricular encumbrance during the third study year. The impact of rural and remote background did not cease even in the extracurricular activities, with urban students more commonly reporting involvement in student organizations and various hobbies.
Students from highly urbanised backgrounds most commonly reported involvement in research projects, while those from rural and remote background were least often involved in such projects. A similar outcome was recorded in students' attitudes to research involvement in their career. A previous study reported that students who do not plan a research career are more likely to choose family medicine and obtain employment in rural and remote areas16. The current study indeed identified rural and remote students as the most likely to pursue long-term careers in rural and remote areas. This makes them a highly valuable resource for programs aiming at development of the health workforce in underserved areas of Croatia. Such areas include counties affected by the 1991-1995 war in Croatia, isolated and underdeveloped geographical areas, and remote Adriatic islands. The scientific literature abounds with examples of studies that reported a positive correlation of rural and remote background with employment in similar areas5,16-18. Various programs have been developed which increase support to rural students, aiming to reduce the gap between rural and urban workforce demand. One of the simplest solutions has been increasing the number of students from rural and remote backgrounds, with some of the first examples set in motion as far back as 197419. The results of this approach, combined with a special education program, were later evaluated, indicating the positive impact of a program on physician retention in underserved areas20. Opening a specialized medical school, such as Jichi Medical School, provides an additional example that a unique approach to undergraduate education can provide an effective way of yielding more physicians with increased interest in employment in rural and remote areas21.
However, programs dealing with the rural and remote physician shortage require interdisciplinary approaches22, preferably on a national level17. One approach in solving this problem is providing tailored scholarships that attract people to underserved areas23. The Croatian Ministry of Science, Education and Sports developed a program of state scholarships in areas of special state interest24. A total of 150 scholarships are awarded yearly in all schools within the university. Students who accept these scholarships are obliged to work in areas of special state interest after graduation, for a period of time defined in the award conditions (usually of equal length to the scholarship duration). However, evaluation of these scholarships has not been publicly available.
A shortcoming of the present study is the use of self-reported data, and possibly recall-biased survey data. Due to the lack of strict definitions of rurality, some group miss-classification may have occurred. To overcome this problem, we divided students into three groups, gradually increasing the urbanisation level. Additionally, the results reported here may vary yearly. A continuation of the survey in forthcoming cohorts might confirm the finding of the unfavourable effect of rural and remote background on students' academic and research performance at Zagreb University Medical School.
Conclusion
Overall, this study suggested that students from urban backgrounds had significantly better academic and research indicators than those from rural and remote backgrounds. With more than half the students from rural and remote backgrounds failing at least one study year, faculty offices must give special attention to suppressing this negative effect. Students coming from a rural and remote background must be encouraged and given additional support in areas they recognize as most problematic, because they represent highly valuable future personnel for health-care provision in underserved rural areas.
Acknowledgements
OP was supported by a PhD scholarship from the University of Edinburgh, UK, and a Postgraduate International Scholarship from the Ministry of Science, Education and Sports, Republic of Croatia.
References
1. Humphreys J, Hegney D, Lipscombe J, Gregory G, Chater B. Whither rural health? Reviewing a decade of progress in rural health. Australian Journal of Rural Health 2002; 10: 2-14.
2. Kwong JC, Dhalla IA, Streiner DL, Baddour RE, Waddell AE, Johnson IL. A comparison of Canadian medical students from rural and non-rural backgrounds. Canadian Journal of Rural Medicine 2005; 10: 36-42.
3. Whitcomb ME. The challenge of providing doctors for rural America. Academic Medicine 2005; 80: 715-716.
4. Durkin SR, Bascomb A, Turnbull D, Marley J. Rural origin medical students: how do they cope with the medical school environment? Australian Journal of Rural Health 2003; 11: 89-95.
5. Pacheco M, Weiss D, Vaillant K, Bachofer S, Garrett B, Dodson WH 3rd et al. The impact on rural New Mexico of a family medicine residency. Academic Medicine 2005; 80: 739-744.
6. Strasser R. Rural medical education comes of age. Australian Journal of Rural Health 2005; 13: 263-264.
7. Rabinowitz HK, Diamond JJ, Markham FW, Rabinowitz C. Long-term retention of graduates from a program to increase the supply of rural family physicians. Academic Medicine 2005; 80: 728-732.
8. Curran V, Rourke J. The role of medical education in the recruitment and retention of rural physicians. Medical Teacher 2004; 26: 265-272.
9. Kamien M. Rural student clubs and the social responsibility of medical schools. Australian Journal of Rural Health 1996; 4: 237-241.
10. Shapiro J, Longenecker R. Country doctors in literature: helping medical students understand what rural practice is all about. Academic Medicine 2005; 80: 724-727.
11. Wainer J. Gender and the medical curriculum: a rural case study. Women Health 2003; 37: 67-87.
12. Danic A, Hadzibegovic I, Loparic M. Status of women in small academic medical communities: case study of the Zagreb University School of Medicine. Croatian Medical Journal 2003; 44: 32-35.
13. Kolcic I, Polasek O, Mihalj H, Gombac E, Kraljevic V, Kraljevic I et al. Research involvement, specialty choice, and emigration preferences of final year medical students in Croatia. Croatian Medical Journal 2005; 46: 88-95.
14. Golubic R, Golubic K. What do grades in clinical subjects depend on? Case study of the Zagreb University School of Medicine. Croatian Medical Journal 2004; 45: 67-71.
15. Levy BT, Merchant ML. Factors associated with higher clinical skills experience of medical students on a family medicine preceptorship. Family Medicine 2005; 37: 332-340.
16. Senf JH, Campos-Outcalt D, Kutob R. Factors related to the choice of family medicine: a reassessment and literature review. Journal of American Board of Family Practice 2003; 16: 502-512.
17. Brooks RG, Mardon R, Clawson A. The rural physician workforce in Florida: a survey of US- and foreign-born primary care physicians. Journal of Rural Health 2003; 19: 484-491.
18. Ward AM, Kamien M, Lopez DG. Medical career choice and practice location: early factors predicting course completion, career choice and practice location. Medical Education 2004; 38: 239-248.
19. Rabinowitz HK. Evaluation of a selective medical school admissions policy to increase the number of family physicians in rural and underserved areas. New England Journal of Medicine 1988; 319: 480-486.
20. Rabinowitz HK, Diamond JJ, Markham FW, Hazelwood CE. A program to increase the number of family physicians in rural and underserved areas: impact after 22 years. Journal of American Medical Association 1999; 281: 255-260.
21. Inoue K, Hirayama Y, Igarashi M. A medical school for rural areas. Medical Education 1997; 31: 430-434.
22. Glasser M, Holt N, Hall K, Mueller B, Norem J, Pickering J et al. Meeting the needs of rural populations through interdisciplinary partnerships. Family and Community Health 2003; 26: 230-245.
23. Pathman DE, Konrad TR, King TS, Taylor DH Jr, Koch GG. Outcomes of states' scholarship, loan repayment, and related programs for physicians. Medical Care 2004; 42: 560-568.
24. Ministry of Science, Education and Sports of Republic of Croatia. State Scholarships. Available at: http://public.mzos.hr/default.asp?ru=301&gl=&sid=&jezik=2 (Accessed 12 April 2006) (in Croatian).

