Between 21 and 23 September 2005, over 200 delegates from 8 countries gathered in Tromsö, within the Arctic Circle, to discuss challenges and solutions to rural health issues. The conference was jointly organised by Helse Nord, from Northern Norway, and NHS Highland and NHS Grampian from Scotland, whose catchment areas (Fig 1) share aspects of demography, geography, economy and social development.
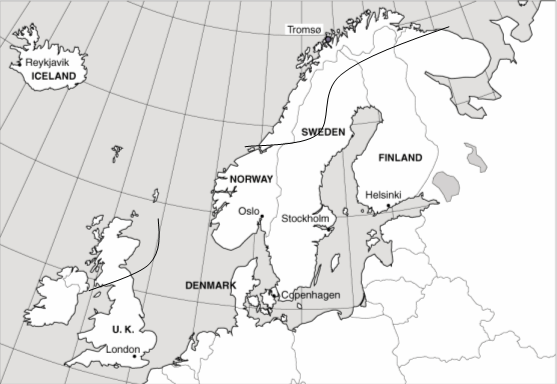
Figure 1: Helse Nord (North Norway) and NHS Highland and Grampian (Scotland) catchment areas.
This conference was a sequel to a previous event entitled 'Making it Work', held in Scotland in 2003, in which it was identified that service delivery in remote and rural areas needed to be innovative to ensure equity. A major aim of this event was to move the debate forward to describe specific examples of practice that could be adopted in participating countries.
The conference recognised that health and delivery of care in rural and remote areas are closely intertwined with many other aspects of rural society. Thus, the delegates (mainly from Norway and Scotland) included clinicians, managers and administrators, senior policymakers and educationalists, elected local and national politicians, patients and their representatives. International experts from countries with advanced thinking about rural health policy were also present.
The virtual community
In pre-conference meetings held in both organising countries, it was recognised that although the output from the first conference provided a broad range of opinion and information on rural health issues, it was important for this follow-up event to identify practical strategic approaches to rural health issues, where possible. In order to focus the debate, the organisers provided a description of a virtual remote community ('Hope'). This fictitious community was designed to include geographic and demographic features that would be recognisable to those providing services in rural and remote Scotland and Norway. In addition, four case studies of individual health problems faced by residents of the community were developed. The conference organisers created a short film which was shown during the introductory session of the conference and featured the 'residents' of this community introducing delegates to the specific problems they faced. Throughout the conference, delegates and session leaders were asked to reflect back to how any recommendations made might apply to particular clinical scenarios described for Hope. A brief description of Hope is as follows.
Hope has a population of 18 000, including two villages: Hope Springs, population 7000; and Hope Falls population 2000. In addition, there is an offshore island, Isolation Island, with 2000 inhabitants (Fig 2). A university teaching hospital is located at Destiny, 120 miles distant from Hope Springs, across a mountain range. The community of Hope has a largely traditional rural economy with significant deprivation and unemployment. The clinical scenarios presented included: (i) a 37 year old pregnant woman in labour during adverse weather conditions; (ii) a 17 year old island resident with acute psychosis who attempts suicide; (iii) an 80 year old woman living alone who suffers a stroke; and (iv) a family of four with a complex range of chronic health issues, including smoking, alcoholism, diabetes, teenage pregnancy, asthma and depression, on a background of deprivation and unemployment.
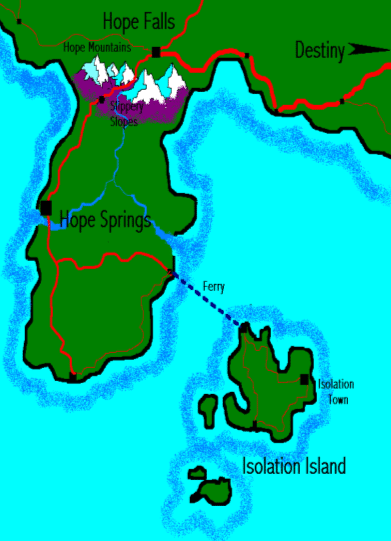
Figure 2: Map of the virtual community 'Hope'
Themes addressed
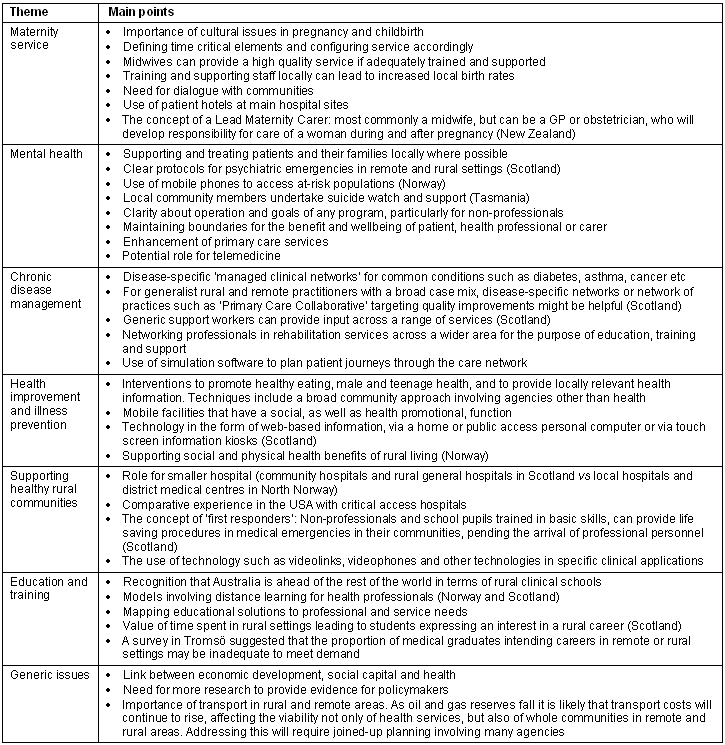
For parallel discussions and workshops, a number of key themes were chosen, linked to the examples highlighted in the 'Hope' scenario. These included: maternity services; mental health; chronic disease management; health improvement and illness prevention; supporting healthy rural communities; and education for rural health staff. Delegates were free to choose which sessions to attend. Inevitably, in some cases, time conflicts meant that delegates had to prioritise their attendance at particular sessions. Where parallel sessions took place, plenary sessions were used to allow a rapporteur to describe the main features of each session to all delegates. Feedback from delegates was collected by a number of routes. During each session, a scribe noted key points for discussion, including any discussion of how that session's content might apply to the clinical scenarios in 'Hope'. A 'knowledge bank' was employed where delegates could deposit suggestions, comment or opinions in writing at any time during the conference. Content of presentations was also available for analysis. All data from each of these sources were available for the creation of this report.
Table 1: Lists the main points identified from that feedback in relation to each theme
Implications for the virtual community (Hope)
Drawing from the wide range of expertise and discussion at this conference, delegates could structure healthcare plans that address the issues facing the community of Hope.
Scenario 1: Consider the 37 year-old pregnant woman in labour during adverse weather conditions. We might expect that the community and the health authorities will have developed a dialogue about the safe and effective provision of services, that takes account of the cultural context. From the early stages of pregnancy, the woman will have had an identifiable professional who takes lead responsibility for her care, most likely, but not necessarily, a midwife. The midwife will have had education and training that makes her competent in risk assessment and determination of time critical elements. Ideally, the pregnancy will be entirely managed in the local community, using a facility appropriately configured. This could be located in a community hospital or district medical centre. If she is required to travel to the teaching hospital because a level of risk has been identified that renders local delivery inappropriate, then suitable transport facilities will be in place, a patient hotel may be located at the major hospital centre, and local support will allow an early transfer home after delivery.
Scenario 2: For the 17 year old island resident with acute psychosis who attempts suicide, again the aim would be to provide a care package in his home community. Clearly, if he has sustained physical injuries in his suicide attempt, these may require medical or surgical intervention that might necessitate transfer off the island. There may be a need for a local 'safe house' where he can be managed during the most acute phase of his disturbance. This need not necessarily be located within a hospital facility. If he does require transfer off the island, available guidelines should be followed to effect the transfer. With effective multi-agency working, support in the community for the family, proactive intervention from a service that has been developed locally, possibly making use of new technologies, he should receive quality care.
Scenario 3: The elderly woman who suffered the stroke could be cared for within the context of a managed clinical network. At the acute episode of collapse in the shop, first responder type skills may be invaluable, delivered by local residents. For the health-care professional, a key early clinical decision would relate to the need for imaging of the brain, which might necessitate transfer out of the community. However, time spent out of the community should ideally be as brief as possible. In a community of this size, rehabilitation services could be provided by an appropriately trained and supported team, including social care as well as physiotherapy, occupational therapy etc. In such a setting, the use of home telecare might have a role.
Scenario 4: For the family with multiple health-related risk factors, a variety of inputs might be beneficial. Outreach services, in which health promotion activities are linked with a social aspect would be appropriate, delivered via mobile facilities and/or use of technology (eg web-based programs or information kiosks). This family's problems might be ameliorated if the socioeconomic situation in Hope can be improved. Closer involvement with the community could potentially increase this family's feeling of self worth and value. For example, the school resuscitation project described from Scotland can provide young people with an important role in society.
Generic issues
Planning and integrating the services for this community will require some key decisions. Developing a 'first responder' scheme may, as well as its specific role, serve to engage the community in health and social care planning. The basis of most services for the community will be in primary care, which will require support and development, and will be sensitive to the local culture. A community hospital may provide a hub for services, staffed by a team of appropriately trained and supported individuals. Relationships with the distant teaching centre and its specialist services will be explicit, based on mutual trust and understanding of individual and shared responsibilities and working practices. Technology will be used as appropriate, recognising that it is a tool and not a substitute for personal connections and face-to-face interactions. Services will be provided within a national framework that takes account of appropriate clinical and governance standards, but allows for the local context to influence the precise mode of delivery of services. Finally, the broader efforts of elected officials and economic development agencies will be needed to ensure that the community thrives, recognising the integral linkages between health and social capital.
Conclusions
The use of the virtual community at this conference helped to focus discussion on the realities of providing health services to remote rural communities. Some of the issues raised and the potential solutions feature in the recently published report on the future of health services in Scotland1 and in the strategy document arising from that2. In a Norwegian report, national strategies for decentralised cooperation between specialist and generalist are outlined3. Many challenges of implementation remain, but a clear articulation of the characteristics of remote and rural communities and their health needs provides a basis for meaningful discussion between policymakers, clinicians, and community leaders.
Further details of the Conference, including conference presentations are available4.
Acknowledgements
The conference was organised by Helse Nord (Norway) and NHS Highland and Grampian (Scotland).
References
1. Scottish Executive. Building a Health Service Fit for the Future (the Kerr Report). (Online) May 2005. Available: http://www.scotland.gov.uk/Resource/Doc/924/0012113.pdf (Accessed 27 April 2006).
2. Scottish Executive. Delivering for Health. (Online) November 2005. Available: http://www.scotland.gov.uk/Publications/2005/11/02102635/26356 (Accessed 27 April 2006).
3. Norway: Rapport fra regionale helseforetak. Samhandling og desentralisering. Available: http://odin.dep.no/hod/norsk/sykehus/politikkensinnhold/042031-990088/dok-bn.html (Accessed 27 April 2006; in Norwegian)
4. Helse Nord. Making it work. (Online) 2005. Available: http://www.helse-nord.no/makingitwork (Accessed 27 April 2006).
Abstract
Between 21 and 23 September 2005, over 200 delegates from eight countries gathered in Tromsö, within the Arctic Circle, to discuss challenges and solutions to rural health issues. This conference was a sequel to a previous event entitled 'Making it Work', held in Scotland in 2003, in which it was identified that service delivery in remote and rural areas needed to be innovative to ensure equity. A major aim of this event was to move the debate forward to describe specific examples of practice that could be adopted in participating countries. The delegates included clinicians, managers and administrators, senior policymakers and educationalists, elected local and national politicians, patients and their representatives. In order to focus debate, the organisers provided an outline of a virtual remote community ('Hope'), including some geographic and demographic information, together with four case studies of individual health problems faced by residents of the community. During the introductory session, a short film was shown featuring the 'residents' of this community, introducing delegates to the specific problems they faced. Throughout the conference, delegates were asked to reflect back to how any recommendations made might apply to the citizens of Hope. The clinical scenarios presented included: (1) a 37 year old pregnant woman in labour during adverse weather conditions; (2) a 17 year old island resident with acute psychosis who attempts suicide; (3) an 80 year old woman living alone who suffers a stroke; and (4) a family of four with a complex range of chronic health issues including smoking, alcoholism, diabetes, teenage pregnancy, asthma and depression on a background of deprivation and unemployment. Parallel discussions and workshops focussed on a number of key themes linked to the examples highlighted in the 'Hope' scenario. These included: maternity services; mental health; chronic disease management; health improvement and illness prevention; supporting healthy rural communities; and education for rural health staff. This approach to targeting discussion is valuable in rural health conferences where the participants may be from diverse backgrounds and the issues discussed are multi-faceted.
Keywords: conference, scenarios, virtual community.

