Introduction and background
Human resources have been described as 'the heart of the health system in any country', 'the most important aspect of health care systems', and 'a critical component in health policies'1. Despite their importance to rural health systems, rural health workers, and doctors in particular, are scarce all over the world. In an international survey of fourteen countries, it was found that rural doctors made up only 8% to 22% of the population of doctors, while serving between 25% and 70% of the population of these countries2. Similarly in South Africa, fewer doctors work in rural areas, where the majority of the population resides (Table 1).
Table 1: Distribution of population and health professionals in provinces in South Africa3,4
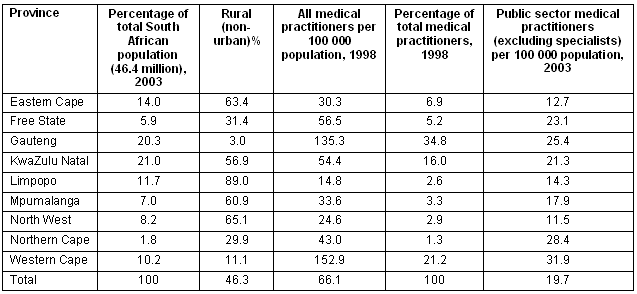
This lack of rural healthcare personnel has a significant impact on health care, and health systems cannot function adequately or effectively without them5. Investing in human resources is therefore a vital component of developing countries' strategies to improve health outcomes, such as the Millennium Development Goals (MDG), and if not urgently addressed could form a constraint that renders these MDG unattainable6.
Post-apartheid South Africa faces an enormous health challenge and a number of human resource related achievements have been made post-1994. These include the amalgamation of historically fragmented former national, provincial and homeland governments with their civil services; the introduction of the District Health System; the transformation of statutory health councils regulating health professionals; the founding of training schools; and the deliberate shift in emphasis towards primary health care with concomitant downsizing of sophisticated curative and tertiary care3.
Internationally countries have tried various interventions to increase their numbers of rural doctors. These are ideally packaged in a Rural Health Care Strategy to oversee all planned activities and their implementation7,8. An important component is also the establishment of policies regarding Human Resources Planning9.
Various policies for the deployment and retention of public health personnel are mentioned in the literature but results have been mixed10. These include decentralization of the location of training institutions; the introduction of recruitment quotas to ensure that the most peripheral areas are represented among medical students; and making rural field experience during medical training compulsory.
Policies for reducing migration out of developing countries, especially Africa, are much debated. Various codes of practice such as the Commonwealth code of practice for international recruitment of health workers11 and the Melbourne Manifesto adopted at the 5th WONCA World Rural Health conference12, have been developed to address recruitment from under-developed countries. These address important issues raised such as the need for developed nations to train more doctors, to select more rural origin students, to pay compensation for doctors recruited at a government-to-government level, not to advertise in the journals of developing countries, and to ensure that recruiters do not make recruitment visits to developing countries13.
Other attempts to provide more doctors in rural areas include the recruitment of foreign doctors14, either on an individual basis or as part of government-to-government cooperation agreements, such as the deployment of Cuban doctors in a number of African countries, including South Africa15.
Another strategy has been the implementation of programs of compulsory community service lasting for one to two years after graduation for medical doctors16,17. The South African government introduced a system of community service for doctors18 that has improved the staffing situation in some provinces, but it is limited as a recruitment and retention strategy19.
Recognition of health qualifications and substitution of skills has been used in some countries to reduce migration, where qualifications meet the needs of the source country but are not internationally recognized. Developed countries such as the United States20 and a number of countries in Africa, including South Africa21,22, have implemented mid-level worker or similar programs.
Successful strategies to increase the numbers of doctors willing to work in rural areas include the selection of more rural background medical students23-27, providing positive training opportunities in rural areas during medical training28-31, providing bursary schemes32, and bringing specialist services to rural communities32. Improving the salaries of rural doctors is often mentioned as an intervention to attract and retain rural doctors, but how health workers respond to different reimbursement structures is largely unknown1.
Little research has been done in South Africa to determine what rural doctors' feel will encourage them to stay on in rural areas. The aim of this study was to identify interventions that will lead to improved retention of South African qualified doctors in rural hospital service in the Limpopo province of South Africa.
Methods
This study utilised a descriptive survey design. A semi-structured questionnaire was used for the project to collect data.
The population under study consisted of post-community service (a one-year period of compulsory public hospital service after completion of internship), non-specialist South African qualified doctors working in Limpopo public hospitals during 2005. After these doctors were identified with the help of the Limpopo Department of Health (DoH), they were contacted to obtain more details regarding their background information and at the same time were asked if they would be willing to be interviewed, if selected.
Doctors were then purposively selected to maximise variability. The variables taken into consideration were race, sex, age, district (location of hospital), university where undergraduate training was undertaken, and duration of service in rural hospitals. It was ensured that doctors were selected so that the greatest diversity of these variables was included. The selected doctors were then interviewed until saturation point was reached. Saturation point was determined as being reached when no new major themes were identified after three consecutive interviews. This was achieved after 10 interviews.
A semi-structured questionnaire consisting of a main question and five follow-up questions was developed by the researchers in consultations with a number of experts in the rural health field (Fig 1). The questions related to demographics, salary scales, career structure, rural allowances, other incentives, and factors that make doctors want to leave rural practice. Piloting of the questionnaire was conducted prior to commencement of the study.

Figure 1: Research questions explored in this study.
The main question was distributed to participants one week before the interview, to allow time for reflection on the topic. One researcher (TJK) personally interviewed each participant. The interviews were arranged at a convenient time for both interviewer and interviewee. All interviews were conducted at the hospitals where the doctors were employed, and in a setting that provided maximum privacy. The interviews lasted between 15 and 50 min. The initial exploratory question was asked and respondents were encouraged to respond fully by the use of active listening techniques, clarification, reflective summaries and repetition of the question when necessary. Once the main question was fully explored, the follow-up questions were posed and each of these questions was then further discussed. Interviews were audiotaped and field notes were recorded. Saturation was reached after 10 doctors were interviewed.
The audio-taped interviews and field notes were transcribed in full by the author. Each transcribed interview was individually analysed to identify all themes. Analysis was performed using the approach of namely familiarization with the data, identifying a thematic framework (major and minor themes) and interpretation33. After analysis of each successive transcription it was then combined to present major and minor themes from all 10 interviews.
Credibility, dependability and conformability
Respondent validation was used to improve the credibility of the research. Analysed data were returned to all 10 participants and the researcher used their comments and further clarifications to make adjustments. The submission of the questionnaire to experts in rural health and piloting of the questionnaire improved its quality and validity. Original audio recordings as well as transcripts of these interviews and field notes form part of the research record. A notebook was kept detailing how the transcripts were made and verified. It includes notes by the researcher about how the research progressed, describes what occurred, how long the interviews lasted, when and where they took place etc. No co-researchers formed part of the study to further enhance dependability.
Based on the above-mentioned criteria, data generated in this research could be regarded as transferable to situations that are similar in setting so far as the population studied is concerned. To further ensure the transferability, the sampling strategy ensured that a diverse range of individuals and settings were included.
Ethical considerations
Each potential participant was informed about the project and invited to participate. Those who agreed and who were then sampled were approached and the project was explained in depth. If they agreed to be interviewed, written consent was requested. The standard consent form of the Medical University of Southern Africa (Medunsa), adapted for this study, was used and completed by each participant. Ethical clearance was given by the Medunsa Research, Ethics and Publications Committee and the Limpopo Department of Health gave permission to interview the participants.
Results
The demographics of the doctors interviewed are presented first and thereafter the themes identified in response to the main question. This is followed by the themes identified from the follow-up questions.
The diversity of the interviewed doctors is reflected (Table 2). The majority of the doctors had a rural upbringing, and undergraduate training was completed at a number of universities from all over South Africa. Most of the doctors completed their community service in rural hospitals and had spent from 4 to 9 years in rural practice.
Table 2: Demographic characteristics of rural doctors working in Limpopo province
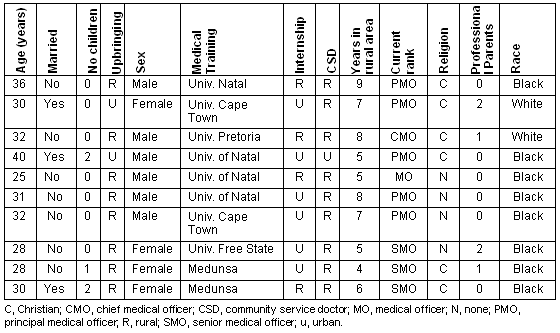
Table 3: Main question: What interventions do you think will retain South African doctors in rural hospital service in Limpopo province?
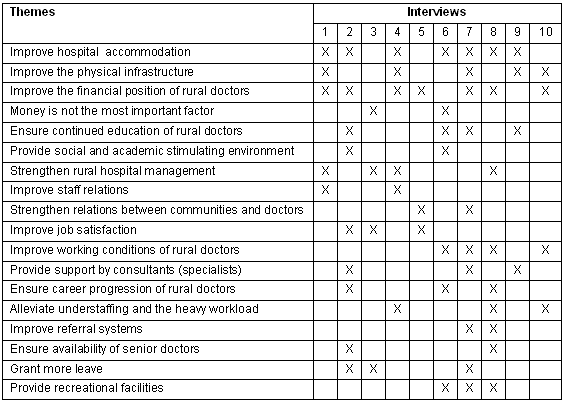
Several interventions are recommended in response to the main question (Table 3). The most common themes that emerged follow.
Improving the financial situation of rural doctors
Improving the financial situation of rural doctors was one of the most common themes, usually as part of a broader strategy. Some doctors felt that money was the most important factor to retain them in rural hospitals, while others stated that issues other than money were more important.
I think the most important thing for me to stay on is that money is not the most important factor for any clinician to be working in a rural setting...what is more important is job satisfaction.
One doctor mentioned that the recent increases in public doctor salaries have already attracted a number of private practitioners back to government hospitals.
Improving the physical hospital infrastructure
In addition to 'old' mission hospitals being in poor condition, doctors mentioned the lack of basic infrastructure, such as adequate access roads and telephone connections. Many doctors mentioned the lack of appropriate facilities and medical equipment in some of the hospitals. Several doctors tired of this and left rural hospitals.
Yes it's [the hospital] not really good for really working, like the wards are hot, it's also the suspicion of the patients who start looking at you [the doctor] thinking this one is not really a good one.
...the cleanliness of the hospital... the tidiness of the place. Yes I know because I follow people [new doctors] around and some people [new doctors] get tired of it and many leave.
Poor hospital accommodation
The impact of poor accommodation on retaining doctors was clearly stated, and it was mentioned that many doctors leave as soon as they finish their year of compulsory community service because their houses are falling apart. However, some doctors who had good accommodation mentioned that this was one of the more important reasons for them to stay on at a particular hospital.
...the other most important thing is good accommodation; if anybody is going to struggle with accommodation they are not going to enjoy working there... you don't want to wake up in the morning and know that you are going to share your bathroom with four other people and stuff like that.
Interventions to improve the current housing situation included the recommendation that hospital management, in addition to upgrading current accommodation inside hospitals, should explore accommodation options outside of rural hospitals. These options could include public private partnerships with game farms, lodges and reserves.
Improve the working conditions in rural hospitals
Doctors felt that their current working conditions were poor and this contributed to the 'stress' of working in rural hospitals. A number of doctors stated that the working conditions were one of the most important factors contributing to good job satisfaction.
Okay firstly ... our casualty... there is virtually nothing you know related to emergency... if you want to attend to an emergency patient there isn't much you can use except maybe things like...IV lines...maybe a drip stand; since I came here we didn't have simple things like glucometers. So every time a patient comes and you want to do the glucose level you have to wait for the lab to do it. Recently they have introduced some glucometers but they only work for a few months ... maybe there is one BP machine, which is used by two or three different wards. They have to wait until the other ward is done so they can go and borrow so it is - yeah - it is a problem.
Improvements in continuing medical education
The lack of academic stimulation in rural hospitals was mentioned by a number of doctors. Many doctors reportedly leave rural hospitals to further their academic careers and to specialize. Interventions mentioned included accrediting rural hospitals for post-graduate Masters in Medicine programs. In addition, time spent working in rural hospitals could form part of the accreditation towards attaining post-graduate specialist degrees. Other recommendations included accrediting more rural hospitals for diploma courses, arranging more short courses for rural doctors, and providing internet access for the purposes of distance based education.
Provide specialist support in rural hospitals
Doctors believed that the quality of their work and job satisfaction was improved by consultant visits. It was felt that visits by consultants from certain specialities would be more appropriate than others. Visiting consultants could assist rural doctors by attending to complicated patients and by teaching.
...what has helped keep me stimulated is even though we are in a rural area there are so many visiting consultants coming from Wits and Garankuwa and Polokwane... Just knowing that there's people coming every month or so that are interested in what you're doing; that can support you and you can always ask them; it definitely improves the quality of your work and the job satisfaction and you feel less out of touch and that you're doing the right thing, some times you need a bit of reassurance that you are doing the right things under the circumstances.
Ensure career progression for rural doctors
Difficulties with promotions were a commonly stated problem that led to doctors leaving for 'greener pastures'. Interventions recommended include improving career options by creating more senior post in rural hospitals. Providing access to further training programs such as postgraduate Masters in Medicine degrees and diploma courses, as sated above, may also lead to more career development opportunities.
...making a lot of post, senior specialists of level 12 available you know there is something to aim for umm so potentially you can get to level 12 in a rural area.
Improving rural hospital management
Managers were not seen as supportive and it was felt they did not treat rural doctors satisfactorily. Personnel departments were identified as a specific problem area. Doctors faced difficulties with promotions, and vacant posts were not advertised.
They are difficult, very, very difficult here with promotions. They don't advertise posts that are available, they'll tell you in human resources that the posts are there but even if you qualify for the post they tell you that because it hasn't been advertised, you can't get into [it].
In addition, doctors felt that they should be treated as professionals and felt frustrated by bureaucracy and protocols. They felt that non-clinical managers should not interfere with clinical work, and that hospitals with chief executive officers (CEOs) who understand clinical medicine do better.
Leave
A number of recommendations regarding leave for rural doctors were mentioned. It was felt that a lack of opportunity to utilise annual leave led to 'burnt out', and the granting of unpaid leave and study leave led to doctors staying on in rural hospitals. Interventions mentioned included granting more annual leave, study leave, unpaid leave and sabbatical leave.
...certainly in a rural area study leave is important for those who want it, some people are not interested that's fine, but people that are craving it and not getting it they then leave.
...I was able to take unpaid leave for two months to justify the diploma to gain experience overseas.
Strengthening relationships
Another theme was strengthening relationships among rural doctors, and between doctors and the communities they served.
...for me definitely the relationship between staff, if there is no friction between staff people are more likely to stay on.
I think the thing that makes me stay here is the things are like; the interaction with the community.
Responses to the follow-up questions
Responses to the follow-up questions included the following.
Current salary scales and career structure: Responses to the importance of current salary scales and career structure varied considerably. Most of the doctors regarded the current salary scale and career structure as insufficient but some doctors felt it was adequate. Some doctors felt that the salary was the most important factor, while others felt that other factors were more important.
I believe that the increase in the rural allowance, the fact that doctor's salaries have been upgraded and the scarce skills allowances has to some degree at least created a scenario that doctors are coming to the hospital with the evidence that I am seeing now with general practitioners coming to us now. But as I said initially the salary is not the most important of all the objections.
Rural allowance: While there was no consensus on whether the rural allowance was beneficial, it was regarded by all interviewees as being insufficient (Table 4). Suggestions of the amount that would make a significant difference ranged from R2000 (approximately US$330/month) after tax, to R10 000 (approximately US$1600/month, with an average of approximately R4700 (approximately US$750/month) after tax.
I actually think that it [rural allowance] needs to be individualized and there needs to be a scale of how rural a hospital is; in fact it needs to be individualized but I do believe that there is still some room for improvement. I think realistically speaking if it could be increased, then maybe it would attract more people.
Other incentives: Other incentives mentioned included providing subsidies for items such as housing, motor vehicles, telephones, electricity, schooling for children, flexibility with bursary work back commitments, and recreational facilities (Table 5).
Factors that make doctors want to leave rural hospital practice: Factors that made doctors want to leave rural hospital practice included the factors already mentioned, such as insufficient salary, heavy work load and understaffing, poor housing, poor hospital management, lack of basic medical equipment, personal relationships, no recreational facilities and specialisation. A number of other factors were also mentioned. including the lack of managerial input as a doctor, poor relationship with colleagues, lack of transport and lack of good schooling for children. Last, some doctors found living in a rural area 'just dull' and preferred an urban lifestyle
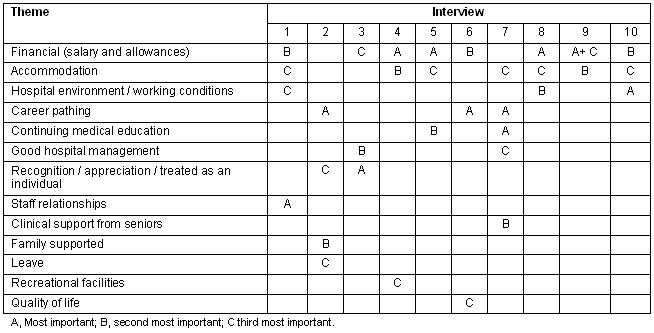
The most important interventions: The most important interventions as mentioned by the participants (Fig 2; Table 6) included improving salaries, proving adequate career pathing, improving hospital accommodation, providing continuing medical education, better working conditions and improving the hospital environment in rural hospitals. Other factors included receiving recognition and appreciation for ones work as a rural doctor, receiving adequate support from senior doctors, facilitating good relationship between staff, supporting rural doctors families, providing more leave and recreational facilities in rural hospitals.
Currently the rural allowance for medical officers is 22% of basic salary. For senior and principal medical officers this is approximately R2700 (US$450) - R4000 (US$670) per month after tax.

Figure 2: Incentive package to attract and retain doctors in rural hospitals.
Table 4. Do you think the current rural allowance leads to the retention of doctors, and is it sufficient? If not what would you suggest it should be?
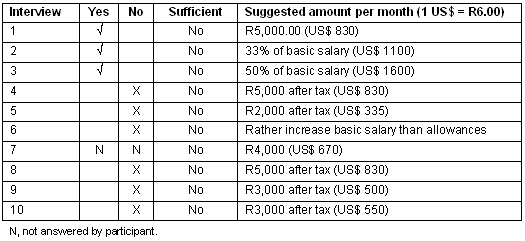
Table 5. What other incentives would you want to see instituted for permanent staff in rural hospitals?
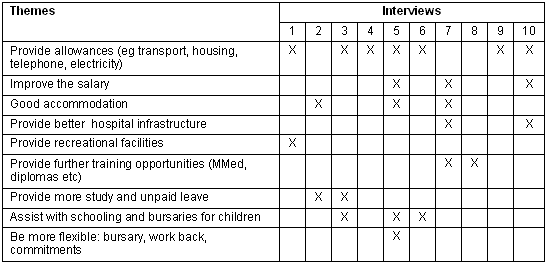
Table 6. Of all the intervention we talked about, which are the most important interventions to retain rural doctors?
Discussion
Almost all the doctors participating in this study stated that improving their salary was one of the three most important factors in retaining doctors in rural practice and almost half mentioned it as the most important factor. Around the world, dissatisfaction with income is one of the major causes of doctors leaving public service34, and improving salaries is often mentioned as an intervention to attract and retain rural doctors35-38. It was reported that recent increases in the salaries of doctors in the public sector in South Africa are already leading to a number of private general practitioners returning to public service. Anecdotal reports in the literature also report that salary increases lead to increases in the number of doctors in the public sector35,39. However, despite the importance of salaries, many doctors stated that other factors, such as job satisfaction and working conditions, were more important and the salary on its own would not retain them.
A few of the doctors interviewed in this study felt the current rural allowance was making a significant difference. However, all 10 doctors felt that the amount was not enough.
Targeted financial support is recommended as a strategy to retain doctors in rural areas40. In South Africa, the outcome of the introduction of rural and scarce skills allowances in 2003 still needs to be determined. The results of preliminary research by Reid et al41 indicate that approximately one-third of health professionals working in rural hospitals were influenced to remain in the rural area by this rural allowance.
The majority of the doctors in the study mentioned better accommodation as one of the three most important factors that would influence them to remain in rural areas. Other authors have also reported accommodation to be one of the factors in attracting and retaining rural doctors42,43. Hospital accommodation is often the only realistic option for rural doctors because many hospitals are situated in extremely underdeveloped areas with inadequate accommodation available in communities outside the hospital. Many of the hospitals in rural Limpopo are old mission hospitals built in the early and mid 1900s and the quality of the hospital accommodation is often inadequate. Attempts by the provincial Department of Health, such as the capital works program, should therefore be prioritised as a matter of urgency. This capital works program is a provincial program to build new clinics and hospitals and to improve the physical infrastructure of existing health care institutions.
Due to the limited budget allocation and the magnitude of the problem, many healthcare institutions have not been upgraded yet. To provide short-term improvements, local hospital management should also look for innovative ways to involve local communities and resources outside the hospital. Many doctors might accept rural service more easily if they and their families are offered the option of a more diverse range of long-term accommodation in and around hospitals. Alternative accommodation options outside hospitals could include public-private partnerships with lodges, farms, and nature and game reserves.
Ensuring career progression has been suggested to be an important factor in retaining rural doctors38,43,44. The creation of more senior posts in rural hospitals is offered as a potential retention mechanism. In this study, a number of doctors mentioned career progression as the most important factor in retaining them in rural hospitals. Rural doctors often face difficulties in the promotion process and personnel departments are specifically identified as a problem area. It was felt that there were delays with promotions, and that vacant posts were not advertised. Doctors often leave because of lack of or delays in rectifying problems with salaries, promotions and annual leave. Lack of the use of basic personnel management tools by hospital managers, such as exit interviews with doctors when they leave rural hospitals, are missed opportunities to identify and correct problems.
Related to this, a number of doctors mentioned strengthening rural hospital management as one of the three most important interventions that would lead to retaining doctors. Poor rural hospital management seemed to add to the frustration and dissatisfaction of rural doctors42,43,45. Doctors felt unsupported by hospital managers and felt that they were not being treated satisfactorily. CEOs who understand clinical medicine were seen to manage hospitals better than CEOs who did not have a medical background.
*Rural doctors were frustrated by bureaucracy, protocols and procedures and often did not have enough time to deal with this adequately due to the heavy workload and understaffing. Establishing proper communication channels between rural doctors and their local hospital management is critical. This could lead to problem areas being identified and resolved where possible. This has been identified as a key to successful management of rural hospitals46. Clinical managers should regularly conduct one-to-one interviews with doctors. This should include entry, follow up, and exit interviews. This could help to identify concerns and lead to their resolution. It would also encourage a culture of problem solving among hospital doctors and alleviate the negative criticism expressed by many who do not feel they have any role in improving their current situation. In addition, good human resource management would minimise conflict between rural doctors. Managing interpersonal relationships was also found to be an important factor, as mentioned in previous research43.
Improving the poor working conditions, hospital infrastructure and lack of medical equipment were mentioned by a number of doctors as among the three most important interventions to retain rural doctors. All of these could be the result of poor management. Lack of basic hospital equipment frustrated many doctors and caused them to leave. Other studies also report on the frustration of rural doctors because they were unable to perform their duties satisfactorily, due to lack of equipment and drugs43,47. A survey conducted in Zimbabwe in 1998 showed that a common cause of health workers resigning from the public sector was the inability to offer effective care to patients due to inadequate resources in health facilities48.
Old mission hospitals are dilapidated and difficult to work in. Basic infrastructure such as hospital access roads and telephone lines should be upgraded. Rural doctors should also be provided with inter-access and recreational facilities. Other authors also found the lack of social amenities at rural hospitals to be a problem47.
Granting more annual, study leave and unpaid leave is mentioned as an important intervention that would retain some doctors. This could be offered as an incentive to rural doctors that have completed a specified time in a rural hospital. Sabbatical leave could be a benefit that would attract rural doctors43,44. Clinical managers should ensure that all doctors have the opportunity to utilize their annual leave. This could reduce burn-out and ensure that doctors are well motivated and positive in the daily provision of duties. Organised vacations by the Department were mentioned as a possible incentive to rural doctors.
Using part time private practitioners in district hospitals to reduce after-hours duties for rural hospital doctors was mentioned as a recommendation to reduce the workload of rural doctors. Researchers from other rural areas in South Africa also recommend private-public collaboration as an untapped resource42,43. Doctors referred to the heavy work load and specifically to the fact that many patients were unnecessarily seen in hospital casualties during after-hours overtime work. This led to insufficient time to attend to 'real' emergencies and made overtime work extremely demanding. De Villiers and De Villiers43, also recommended addressing the inappropriate primary health care load at district hospitals with better functional integration of district health services.
Providing assistance to the families of rural doctors was mentioned in this study and is presented as an intervention to retain doctors in various articles40,49,50.
Limitations of the study
A qualitative research design was chosen to ensure that new themes that were relevant to rural Limpopo were identified. The limitations of qualitative research have to be considered when interpreting the findings of this study. An alternative sampling strategy could be to interview South African qualified doctors who have left rural hospitals. A future study including these doctors may identify valuable additional interventions not raised by the doctors selected in this study.
Three of the 10 interviewed doctors are currently family medicine registrars at the University of Limpopo. This may have led to a bias towards Family Medicine and the University of Limpopo, but it may also reflect that there are a growing number of South African doctors in rural Limpopo who are completing this degree. This study formed part of a Family Medicine Masters' degree research project; researcher bias towards Family Medicine could potentially prejudice the results of this study. An attempt to reduce this bias was made by submitting the research questionnaire to a number of experts in the rural health field and by piloting it before starting the research project. All of the above helped ensure that the questions were not solely devised by the researchers and should, therefore, enhance the validity of the research.
To improve the transferability of the results to situations of a similar population, the sampling strategy helped to ensure that a diverse range of doctors and settings were included. This is reflected in the demographics of the interviewed doctors.
Conclusion and Recommendations
Human resources are finally being recognized as the most important aspect of healthcare systems but, despite this recognition, health personnel continue to be scarce in services where they are most needed. The reasons for this are the numerous 'push and pull' factors that combine to form a serious challenge to rural health care systems.
The resolution of one individual factor, for example increasing rural doctors' salaries, is unlikely to lead to significant long-term improvements in the retention of rural doctors. The challenge to health systems is to identify the most pressing needs of rural doctors and to address them appropriately within the restrictions of available resources.
The interventions proposed by the participating doctors in this study will assist in prioritising the multitude of factors impacting on the retention of rural doctors. The next step will be for health managers to develop interventions based on these and other recommendations. In addition to the multiple health system and policy recommendations discussed in detail in previous sections, the introduction of an incentive package could provide recognition for time spent in rural hospital practice, as measured in years spent in service at a particular hospital (Figure 2).
References
1. Hongoro C, McPake B. How to bridge the gap in human resources for health. Lancet 2004; 364: 1451-1456.
2. Chaytors RG. International Survey of Distribution of Rural Doctors'. Proceedings, First International Conference on Rural Medicine, Shangai, 1996.
3. Health Systems Trust. South African Health Review 2003/04. Durban: Health Systems Trust, 2004.
4. Van Rensburg HCJ. The Health Professions and Human Resources for Health - Status, Trends and Core Issues. In: HCJ van Rensburg (Ed.). Health and Health Care in South Africa. Pretoria: Van Schaik, 2004.
5. Padarath A, Chamberlain C, McCoy D, Ntuli A, Rowson M, Loewenson R. Health personnel in Southern Africa: confronting maldistribution and brain drain, Circulation or convection? Following the flow of health workers along the hierarchy of wealth. Harhare: EQUINET: Network for Equity in Health in Southern Africa, 2003.
6. Sudhir A. A joint learning initiative: Human resources for health and development: Human Resources and Health Outcomes. JLI working paper 7-26. (No town): University of Oxford, Harvard University, Global Equity Initiative Till Baernighausen, Harvard School of Public Health, Department of Population and International Health, 2003.
7. Couper I. The rocky road to rural health. South African Family Practice 2003; 45: 6-8.
8. Australian Government Department of Health and Ageing. A continuing commitment to rural, regional and remote Australians. (Online) 2004. Available: http://www.health.gov.au/internet/wcms/publishing.nsf/Content/health-budget2004-hbudget-hfact4-cnt.htm/$FILE/hfact4.pdf (Accessed 29 August 2004).
9. South African Department of Health. Draft strategic framework for human resources South Africa. (Online) 2005. Available: http://www.doh.gov.za/docs/discuss-f.html (Accessed 15 September 2005).
10. Ferdinand WA. Healthcare in Rural Areas of Sri Lanka. Presidential address by President of the College of General Practitioners of Sri Lanka. (Online) 2002. www.medinet.lk/colleges/slcgp/topstory/health.htm (Accessed 1 January 2005).
11. Commonwealth Secretariat. Commonwealth Code of Practice for the International Recruitment of Health Workers. London: Commonwealth Secretariat, 2002.
12. WONCA. The Melbourne Manifesto: A Code of Practice for the international recruitment of Health Care Professionals. Proceedings: 5th WONCA World Rural Health Conference. WONCA Working Party on Rural Practice. 30 April-3 May 2001,Melbourne, Australia: WONCA, 2001.
13. Couper I, Worley P. The ethics of International recruitment. Rural and Remote Health 2: 196. (Online) 2002. Available: http:rrh.org.au (Accessed 1 February 2005)
14. Martineau T, Decker K, Bundred P. Briefing note on international migration of health professionals: Levelling the playing field for developing health systems. International Health Division School of Tropical Medicine. (Online) 2002. Available: www.liv.ac.uk/lstm/research/documents/InternationalMigrationBriefNote.pdf (Accessed 1 November 2004).
15. South Africa info reporter. Cuban skills in SA. (Online) 2004. Available from: http://www.southafrica.info/public_services/foreigners/immigration/cuban-doctors.htm (Accessed 1 August 2005).
16. Fadayomi TO, Oyenene OY. The demographic factor in the provision of health facilities in developing countries: the case of Nigeria. Social Sciences Medicine 1984; 19: 793-797.
17. Reid S J, Conco D. Monitoring the implementation of community doctors in South Africa: a qualitative study in three provinces. Durban: Centre for Health and Social Studies University of Natal, 1999.
18. Reid S (Ed.). Community service for health professionals. In: South African Health Review. Durban: Health Systems Trust, 2002.
19. RuDASA. Position paper: January 2001 crisis in staffing of rural hospitals. (Online) 2001. Available: www.rudasa.org.za (Accessed 24 October 2001).
20. Health Systems Trust. Program to address shortage of doctors. (Online) 2004. Available: http://www.hst.org.za/news/20040330 (Accessed 1 November 2004).
21. Huddart J, Picazo O. The Health Sector Human Resource Crisis in Africa: an issues paper. Washington, DC: United States Agency for International Development, Bureau for Africa, Office of Sustainable Development, 2003.
22. Freeman C. SA to train 'medical assistants'. (Online) 2004. Available from: http://www.southafrica.info/ess_info/sa_glance/health/update/medical-assistants.htm (Accessed 29 August 2004).
23. Bowman R. More rural doctors through partnerships between rural and academic communities. (Online) 2003. Available: http://www.unmc.edu/Community/ruralmeded/fedstloc/impacting.htm (Accessed 1 November 2003).
24. Wilkinson D, Beilby J, Thomson D, Laven G, Chamberlain L, Laurence C. Associations between background and where South African general practitioners work. Medical Journal of Australia 2000; 173: 137-140.
25. Cooper J, Heald A, Samuels M. Affecting the supply of rural physicians. American Journal of Public Health 1977; 67: 756-759.
26. Rabinowitz H. Relationship between US medical school admission policies and graduates entering rural practice. Family Practice 1985; 5: 142-144.
27. Rosenblatt R A, Whitcomb M E, Cullen T J, Lishner D M, Hart L G. Which students become rural physicians? JAMA 1992; 268: 1559-1565.
28. Inoue K, Hirayama Y, Igarashi M. A medical school for rural areas. Journal of Medical Education 1997; 31: 430-434.
29. Magnus J, Tollan A. Rural doctor recruitment: does medical education in rural districts recruit doctors to rural areas? Journal of Medical Education 1993; 27: 250-253.
30. Chaytors RG, Spooner G R., Training for rural family medicine: a cooperative venture of government, university and community in Alberta. Academic Medicine 1998; 73: 739-742.
31. Easterbrook M, Godwin MA, Wison R. Rural background and clinical rotations during medical training: effect on practice location. Canada Medical Association Journal 1999; 160: 1159-1163.
32. Rural Doctors Association of Australia, Australian Local Government Association, Country Women's Association of Australia, Health Consumers of rural and remote Australia, National Farmers Federation. Good health to rural communities - a 10-point plan. (Online) 2004. Available: http://www.rdaa.com.au/uploaded_documents/GOOD%20HEALTH%20TO%20RURAL%20COMMUNITIES_final.pdf (Accessed 30 March 2005).
33. Pope C, Ziebland S, Mays N. Analysing qualitative data. London: BMJ Publishing Group, 2000.
34. Bundred P, Levitt C. Medical Migration: Who are the real losers? Lancet 2000; 356: 245-246.
35. Physicians for Human Rights. Brain drain: The exodus of doctors and nurses from the AIDS-affected countries of sub-Saharan Africa to wealthier nations. Bangkok: Physicians for Human Rights, 2004.
36. Dovlo D. Retention and Deployment of Health Workers and Professionals in Africa. Addis Ababa: Consultative Meeting on Improving Collaboration between Health Professionals and Governments in Policy Formulation and Implementation of Health Sector Reform, 2002.
37. Jones J, Humphreys J, Adena M. Rural GPs' ratings of initiatives designed to improve rural medical workforce recruitment and retention. Rural and Remote Health 4: 314. (Online) 2004. Available: http:rrh.org.au (Accessed 3 February 2005).
38. Muula A, Mfutso-Bengo J, Makoza J, Chatipwa E. Is it ethical for industrialised nations to recruit nurses from a developing country? The case of Malawi. Blantyre: Department of Community Health, University of Malawi College of Medicine and Nurses and Midwives Council of Malawi, 2002.
39. EQUINET. Equity in the distribution of health personnel regional research review meeting report. Johannesburg, South Africa: Southern African Regional Network on Equity in Health (EQUINET) in co-operation with Health Systems Trust South Africa, 2004.
40. WONCA Working Party on Training for Rural Practice. Policy on training for rural practice. Hong Kong: WONCA, 1995.
41. Reid S. Monitoring the effect of the new rural allowance for health professionals. Durban: Health Systems Trust, 2004.
42. Couper ID. Rural hospital focus: staffing. Rural and Remote Health 3: 201. (Online) 2003. Available: http:rrh.org.au (Accessed 5 February 2005).
43. De Villiers M, De Villiers P. Doctors' views of working conditions in the rural hospitals in the Western Cape. South African Family Practice 2004; 46(3): 21-26.
44. Jacques P. Recruitment and retainment of staff in Rural Areas. South African Family Practice 1994; 15(7): 398-400.
45. Couper I. The rocky road to rural health. South African Family Practice 2003; 45(5): 6-8.
46. Couper ID, Hugo JFM. Management of district hospitals - exploring success. Rural and Remote Health 5: 433. (Online) 2005. Available: http:rrh.org.au (Accessed 20 March 2006).
47. Maseka DN, Ogunbanjo GA, Malete NH. The perceptions and experiences of community service doctors about compulsory community service at Shongwe Hospital, Mpumalanga Province, Republic of South Africa. Proceedings: World Rural Health Conference 2002, 30 April-3 May, 2002; Melbourne; WONCA, 2002.
48. Huddart J, Picazo O. The health sector human resource crisis in Africa. Washington, DC: Bureau for Africa, Office of Sustainable Development, United States Agency for International Development, 2003.
49. Wilkinson D, Beilby J, Thomson D, Laven G, Chamberlain L, Laurence C. Associations between background and where South African general practitioners work. Medical Journal of Australia 2000; 173: 137-140.
50. Strasser R. Rural Medicine in Australia. South African Family Practice 1997; 18(5): 23.


