Introduction
On a range of measures, rural populations experience poorer health than those in capital cities1. Demographic and distribution patterns reveal Australia's health workforce is poorly placed to respond, with significant shortages in many areas2.
Population growth and 'baby boomer' ageing will increase demand on health services at a time when the health workforce is also ageing, with more than half the current nursing workforce expected to retire within the next 15 years3. Providers of health services, particularly those with existing workforce shortages, require accurate knowledge of current and projected work patterns for effective workforce planning and for development of appropriate recruitment and retention strategies.
This article uses a special extract from Australian Bureau of Statistics (ABS) census surveys to compare changes in the work practices and retirement patterns of rural and city GPs and nurses. These historical data can help us predict future rural and city workforce attrition, and inform our workforce planning.
Methods
The ABS provided an extract of data for GPs (including trainees) and registered nurses from the ABS Census of Population and Housing for the years 1986, 1991, 1995 and 2001. The variables included were occupation, age, sex, hours worked and region.
When defining generational cohort boundaries we chose boundaries which best matched the five-year age groups of the census (Table 1). The data were then used to examine ageing, changes in hours worked and gender, and to calculate attrition rates, or the net decline in the workforce as 5 year cohorts were followed as a group from one census to the next. While these attrition rates include GPs and nurses leaving the workforce for a variety of reasons, including retirement, illness, death, change of career or family reasons, it is expected that the majority of workforce attrition in the older age groups is related to retirement from the workforce3.
Attrition rates were derived by following cohorts through each of the 1986, 1991, 1996 and 2001 censuses and calculating the net loss from each cohort every 5 years. The formula is expressed as:
CAR = 1 - Nti/Nt1
where CAR = Cumulative attrition rate, N = number of people, ti = census date and t1 = first census in series (1986).
Table 1: Definition and size of GP and nurse cohorts in Australia for the years 1986 and 2001
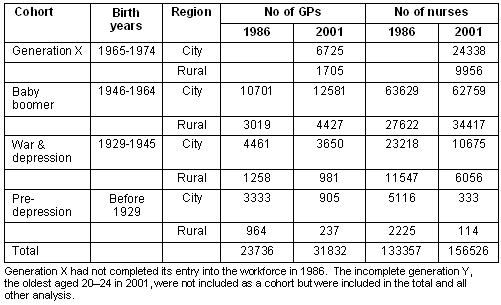
In this article 'city' refers to major capital city and 'rural' to the remainder of Australia. Rural and remote data were combined due to low numbers in remote areas. Data analysis was undertaken using SAS (vers 9.1; SAS Institute Inc; Cary, NC, USA). Tests of association used Pearson's χ2 tests and all tests were undertaken at the 5% level of significance.
Results
Twenty years ago rural GPs were younger than city GPs but that is no longer the case. Between 1986 and 2001 both the rural and city GP workforce aged with the rural GPs being significantly older than city GPS by 2001 (p<0.001) (Fig 1). During this period, the percentage of rural GPs aged over 40 years rose from 40% to 60%, compared with 43% to 57% for city GPs. In 2001, baby boomers made up 52% of the city GP workforce and 59% of the rural GP workforce.
The rural nursing workforce is slightly but significantly older than that in the city (p<0.001). In 1986, 31% of city nurses were 40 or more years of age compared with 33% in the country. But by 2001 this proportion had increased to 58% for city nurses and 60% for the country (Fig 2).
Baby boomer nurses made up 61% of the city nursing workforce and 63% of the rural nursing workforce in 2001.
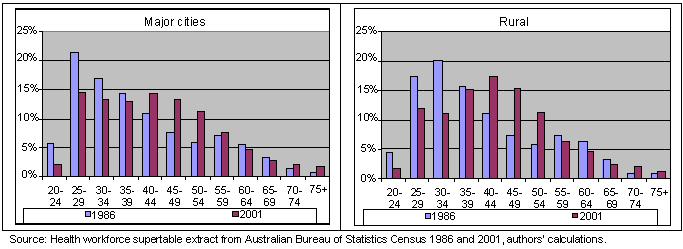
Figure 1: Age distribution of GPs, 1986 - 2001
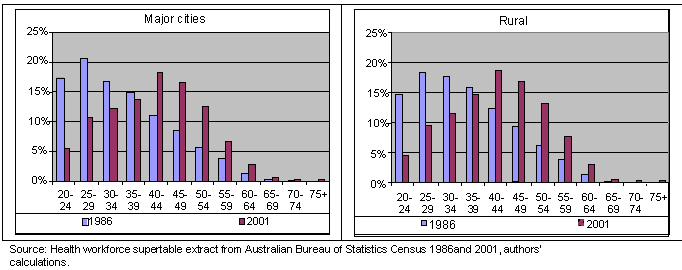
Figure 2: Age distribution of registered nurses 1986 - 2001
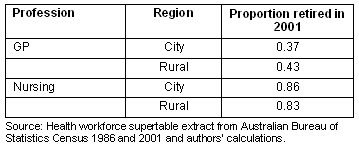
As the health workforce ages, patterns of attrition are important for understanding the workforce age structure. Attrition rates for the cohort of rural and city GPs and nurses aged 50-55 in 1986 and then aged 65-69 in 2001 were calculated. Most notable was that rural GPs in this age group retired significantly earlier than those in the city (p<0.001) (Table 2).
However, rural nurses retired significantly later than city nurses (p<0.001). Regardless of location, a much lower proportion of GPs retire by traditional retirement age than nurses.
Table 2: Attrition rates of 50-55 year old GPs and registered nurses, 1986 - 2001
Traditionally the rural GP workforce has compensated for shortages by working longer hours, however this is changing in the transition from baby boomers to generation X.
In 1986, a significantly higher proportion of all rural GP cohorts worked more than 41 hours per week than city GPs (p<0.05). However, by 2001 only the older baby boomer and the pre-depression cohorts worked significantly longer in rural areas than in the city. These younger rural generation X GPs were no more likely to work long hours than their city peers (Table 3).
Table 3: Proportion of GPs working more than 41 hours per week
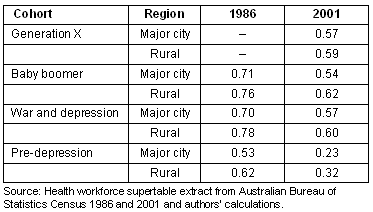
Compared with GPs, few nurses worked more than 41 hours per week. There was little difference between city and rural nurses with the only significant difference in 2001 being that a higher proportion of city nurses worked long hours (12%) than rural nurses (10%) (p<0.001) (Table 4).
Table 4: Proportion of nurses working more than 41 hours per week
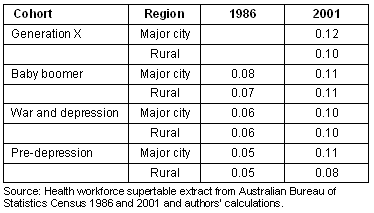
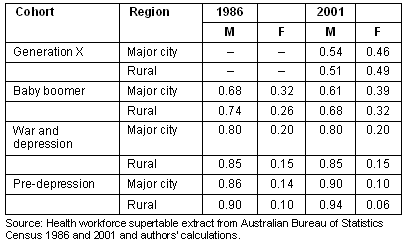
In 1986 there were more male than female GPs in each cohort with rural GPs more likely to be male than those in the city (Table 5). With each successive cohort the proportion of women increased in both the city and rural areas. By 2001, the split between men and women was almost even for generation X, with rural Australia having a slightly higher proportion of women than the city. However, in the older cohorts, rural Australia still had a lower proportion of women than in the city.
There was no change in the gender of nurses. Nursing remained a predominantly female profession in both city and country Australia with less than 10% of nurses being male in 1986 and in 2001.
Table 5: Proportion of GPs, by cohort and gender, 1986 and 2001
Discussion
There are doubts that younger doctors are entering the workforce in sufficient numbers to replace the baby boomers as they retire3. Geographic shortages of GPs are significant2, with remote areas having half the workforce of capital cities per capita, and with GP registrars tending to opt for training with urban-based regional training providers4.
Analysis of census data indicates that rural GPs are older than city GPs, and they cease work earlier, so the impact of baby boomer generation retirement will be felt sooner in the country. But what are the reasons for their early departure? We need to turn to other data to find answers to this question. Other studies suggest that some rural doctors are not necessarily retiring from the workforce when they are older, but are moving to other areas. Exit interviews such as those by the Rural Workforce Agency of Victoria5 reveal that rural GP workforce attrition due to retirement constitutes just 7.5% to 25% of the total, while relocation to urban or overseas areas constitutes 36% to 49%. This may relate to reduced opportunities for variety of clinical practice6 due to the combined effects of workforce shortages, closure of procedural units and personal medical litigation concerns7. Significantly, non-procedural GPs are less likely to stay in rural locations for periods longer than 5 years than are their procedural colleagues (45.9% compared with 63.8%)8 who reflect this greater retention by being, on average, older. Significantly, 75% of all procedural GPs practice in rural towns of 5000 to 25 000 population (ie, RRMA 4&5)9.
Morale is implicated in retention because contented doctors stay in rural practice longer - women by 3.5 years and men 5.2 years - than discontented ones, and while there are differences with gender including the need for flexible and family-friendly working and training conditions10, rural GPs overall are negatively influenced by poor on-call arrangements, restricted variety of practice, and by levels of local professional support, availability of services and geographic attractiveness (rather than distance from population centres)11.
Older GPs work fewer hours than when they were younger. This is expected as their children may have grown up and they may have fewer financial commitments such as a mortgage, children's education and other child-raising costs.
Whereas older country GPs once were more likely to work longer hours than city GPs, this is no longer the case for generation X. How might this be explained?
The rising participation of female GPs in the country is a major factor. Women make up only one-third of rural baby boomer GPs (and even fewer for older generations) but half of the generation X cohort working in the country, and 55% of domestic undergraduate medical students in 20059. Changing the 'super doc' rhetoric is associated with retention of female GPs10 and this, combined with increases in the number of group practices offering flexible work options and protection from the burden of business management12, may explain why rural areas showed the largest growth in the proportion of female GPs between 1995 and 2001 nationally4.
Another aspect of feminisation of the rural GP workforce is childcare responsibilities. Forty-two per cent of female GPs compared with just 29% of male GPs are married to other doctors, and the majority retain childcare responsibilities that limit their rural workforce participation13.
Education is an issue for all rural professionals with school-age children - families tend to relocate to major centres as their children move on to secondary school14. Nurses in general retire earlier than GPs. This may in part be because GPs are self-employed and have greater flexibility to manage their work arrangements than nurses3. Also, partly because professional women balance their work and professional identity with family roles/obligations, social contacts, and community involvement15; and achieving work/life balance plays a role in their workforce participation and retention16. Nursing retirement behaviour is heavily influenced by household finances and family factors17. The female baby boomer generation in general had their children later in their career, while increased overall life expectancy means they may now also have elderly relatives to care for. Consequently, one-third of nurses in the 50+ age group employed by the National Health Service (NHS) in the United Kingdom report caring responsibilities that impact on their work engagement18.
But why do rural nurses retire later than city nurses? In rural areas, nurses are unlikely to leave employment for alternative careers, making retirement the most likely reason for cessation19. Nursing may be one of the few reliable sources of income in rural communities, where unemployment is higher and average weekly earnings (AWE) substantially less than in metropolitan regions20. Economic downturns in rural industry, combined with changes in rural banking practice such as rapid managerial staff turnover that limit the ease of loan approvals, have created a focus on short-term finances that may delay the desire for retirement21. This is particularly relevant in an occupation predominantly of women, who on average accumulate half the superannuation benefits of men20.
The rural working environment may also deliver greater job satisfaction for nurses and thereby reduce turnover22. Rural health facilities provide individual nurses with more varied case-mix and the opportunity for less regulated models of advanced nursing practice within integrated clinical teams, including remote area nursing. This more visible role in clinical care is associated with increased patient satisfaction23 and may in turn lead to a higher social status within the rural community and make early retirement less attractive. It is also possible that the smaller clinical teams in rural areas create closer collegiate relationships that may be protective against occupational bullying, which has been associated with as much as 20% of nursing attrition in other settings24.
In addition, greater acuity and complexity of hospital case-mix, especially in the city, relating to changes in clinical practice and advances in health technology have increased the nursing workload. These changes have been identified as a source of stress for the senior nurses in particular who also act as unit managers and staff preceptors25. Nursing workforce per capita is greater in rural and regional areas2 and rural hospitals lack much of the technological infrastructure to manage high acuity cases. The comparative reduction in workload in rural areas might also reduce the incidence of musculoskeletal injury allowing longer participation in the workforce26.
Conclusion
In conclusion, the rural workforce is ageing faster than the urban workforce. Current GP workforce shortages are being partially mitigated by a declining cohort of older rural GPs willing to work long hours. Younger GPs are no longer prepared to work longer hours than their city counterparts.
New policies such as bonded rural places and rural clinical schools27 may improve the geographic distribution of younger GPs, but need to be matched with effective strategies to delay their retirement. Retention of older nurses could provide a significant human resource in terms of both numbers and expertise, however, the needs of an ageing nursing workforce will require the development of a new approach to this sector28.
With rural GPs retiring faster than city GPs, policies to attract and retain GPs in the country have immediate import to ensure ongoing access to medical care in the bush.
References
1. Australian Institute of Health and Welfare. Rural, regional and remote health-Indicators of health. Canberra: AIHW, 2005.
2. Joyce C, Wolfe R. Geographic distribution of the Australian primary health workforce in 1996 and 2001. Australian and New Zealand Journal of Public Health 2005; 29: 129-135.
3. Schofield D, Beard, J. Baby boomer doctors and nurses: demographic change and transitions to retirement. Medical Journal of Australia 2005; 183: 80-83.
4. AMWAC. The general practice workforce in Australia - supply and requirements to 2013. AMWAC Report 2005.2. Sydney: AMWAC, 2005.
5. Rural Workforce Agency of Victoria. Report on Interviews with General Practitioners and Spouses who left practice in rural Victoria. Melbourne, VIC: RWAV, 2002.
6. Dunbabin J. Procedural Medicine in rural and remote NSW. Newcastle: NSW Rural Doctors' Network, 2002.
7. Australian College of Rural and Remote Medicine. Barriers to the maintenance of procedural skills in rural and remote medicine and factors influencing the relocation of rural proceduralists. In: Medicine TACoRaR. Brisbane, QLD: ACRRM, 2002; 1-47.
8. Australian Rural and Remote Workforce Agencies Group. Minimum data set report as at 30th November 2003. Canberra: ARRWAG, 2003.
9. Committee of Deans of Australian Medical Schools (CDAMS). Medical Student Statistics 2005 CDAMS. (Online) 2005. Available: http://www.cdams.org.au/projects.html#topic7 (Accessed: 19 October 2005).
10. Wainer J. Sustainable rural practice: successful strategies from male and female rural doctors. Melbourne, VIC: Monash University, 2004.
11. Humphreys JS, Jones MP, Jones JA, Mara PR. Workforce retention in rural and remote Australia: determining the factors that influence length of practice. Medical Journal of Australia 2002; 176: 472-476.
12. Doyle S. Women doctors in rural Australia: workforce support strategies. In: Australian Rural Workforce Agencies. National report on the findings from surveys of rural and remote female GPs conducted by the Australian Rural Workforce Agencies 2000-2003. Sydney: Australian Rural Workforce Agencies, 2003; 1-72.
13. McEwin K. Wanted: New Rural Workforce Strategies for female Doctors - Findings from a Survey of Women in rural practice. Newcastle, NSW: NSW Rural Doctors Network, 2001.
14. Miles B, Marshall C, Rolfe J, Noonan S. Attraction and retention of professional services in regional, rural and remote Queensland. Institute for Sustainable Regional Development Central Queensland University Rockhampton (Online) 2004. Available: http://www.isrd.cqu.edu.au/about/Publications/ISRD%20Attr%20Reten%20Report_Final_March2004.doc (Accessed 19 October 2006).
15. Price C. Retirement for Women: The Impact of Employment. Women and Aging 2002; 14(3-4): 41-57.
16. Allen I. Women doctors and their careers: what now? BMJ 2005; 331(7516): 569-572.
17. Minnick AF. Retirement, the nursing workforce, and the year 2005. Nursing Outlook 2000; 48: 212-217.
18. Buchan J. The 'greying' of the United Kingdom nursing workforce: implications for employment policy and practice. Journal of Advanced Nursing 1999; 30: 818-826.
19. Australian Health Workforce Advisory Committee. The Australian Nursing Workforce - and overview of workforce planning 2001-2004. Sydney: AHWAC, 2004.
20. The Office for Women. Women and Superannuation. Information Paper 3. Brisbane, QLD: The Office for Women, 2005; 1-5.
21. Shrapnel MDJ. Impediments to rural prosperity: a social perspective. In: Proceedings, 24th ANZRSAI Annual Conference, 2000. 3-6th December 2000; Hobart, TAS; 1-13.
22. HSM Group L. Acute care hospital survey of RN vacancy and turnover rates in 2000. Journal of Nursing Administration 2002; 32(9): 437-439.
23. Buchan JC. Skill-mix and policy change in the health workforce: Nurses in advanced roles. Paris: Organisaion for Economic Co-operation and Development, 2004.
24. Hadikin R. The bullying culture: cause, effect, harm reduction. Oxford: Butterworth-Heinemann, 2000.
25. O'Brien-Pallas L, Duffield C, Alksnis C. Who will be there to nurse? Retention of nurses nearing retirement. Journal of Nursing Administration 2004; 34: 298-302.
26. Bongers PM, DeWinter CR, Kompier MAJ, Hildebrandt VH. Psychological factors at work and musculoskeletal disease. Scandinavian Journal of Work, Environment and Health 1993; 19: 297-312.
27. Department of Health and Ageing. Health Workforce - Rural Clinical Schools. (Online) 2005. Available: www.health.gov.au/internet/wcms/publishing.nsf/Content/health-workforce-new-rurclinical.htm (Accessed 8 August 2005).
28. O'Brien-Pallas L, Duffield C, Alksnis C. Who will be there to nurse? Retention of nurses nearing retirement. Journal of Nursing Administration 2004; 34: 298-302.
Abstract
Introduction: Objective: To compare the impact of ageing on the GP and nursing rural and city workforce.
Method: Cohort analysis of Australian Bureau of Statistics census data. The data was used to examine the age distribution of the city and rural GP and nursing workforce; patterns of attrition for those 50 years and over; and the impact of changes in working hours.
Results: The rural GP and nursing workforce is significantly older than their city counterparts (p<0.001) with the 'baby boomer' generation making up 52% of city GPs but 59% of rural GPs in 2001. While a large proportion of city and rural GPs continued to work past the age of 65 years, rural GPs left the workforce at a significantly younger age than city doctors (p<0.001). Rural nurses are older than their city peers (p<0.001) but retire at an older age than city nurses (p<0.001). In 1986, a significantly higher proportion of rural GPs in all age cohorts worked more than 41 hours per week compared with their city counterparts (p<0.001). By 2001, rural 'generation X' GPs were no more likely to work long hours than those in the city (p<0.001). However, significantly more rural than city 'baby boomers' continued to work long hours.
Conclusions: Rural GPs are retiring faster than city GPs and strategies to attract rural GPs and nurses will be critical to ensure adequate rural health care and that current rural workforce shortage do not worsen.
Key words: demographic, doctor, nurse, retirement ageing, workforce.




