Introduction
In vision and mission statements within the public health sector in South Africa, the aspiration to practise holistically is either stated or implied1. However, moving from the goal and strategy to changes on the ground is difficult, and this often remains the realm of the ideal, particularly in a developing country. The limitations to implementing holistic practice were explored as part of a larger process of attempting to understand holistic practice in a rural primary healthcare setting of a sub-district in the public sector of the KwaZulu-Natal province in South Africa.
Context: healthcare system in South Africa
Over the past decade a concerted effort has gone into developing a unified public healthcare system in South Africa, based on the principles of primary healthcare, and using the district health system, as advocated by WHO. As a result, each of the nine provinces in South Africa is divided into districts, which function as units of healthcare delivery. Within each of the districts, the health service may be further divided into smaller functional units (called sub-districts) usually formed around a district hospital, depending on the local resources and population needs. Each district hospital relates to a number of primary healthcare clinics and mobile teams, which are both supported by the hospital and refer to the district hospital.
The sub-district where the study reported on was performed has a population of approximately 150 000 people, who are served by one district hospital, five residential primary healthcare clinics and three mobile primary healthcare teams. This sub-district is situated in the foothills of the Drakensberg in the KwaZulu-Natal province, with high rates of poverty, unemployment and migrant labour characterizing the community. KwaZulu-Natal also has one of the highest HIV prevalence rates in the world. The study reported on was conducted within the public sector, which mostly treats the indigent population.
Background: what is 'holistic'?
The term 'holistic' is often used loosely, having a range of meanings for different people. Smuts2 coined the word 'holism' in his work entitled 'Holism and Evolution' where he described it as a unifying principle of the whole, which is greater than the sum of its parts. Since then it has been incorporated into a number of scientific disciplines, particularly in the areas of biology and ecology, as a way of explaining the organisation of systems at complex levels. Work in areas as diverse as quantum physics, human geography and anthropology have borrowed from the concept. Over the past two decades the term holism has increasingly entered other fields of study, such as organisational development and management as well as popular culture3. Many critiques of the biomedical approach to health advocate a more holistic perspective4,5, where mind-body-spirit unity is part of the diagnostic and therapeutic approach6. In a number of health-related disciplines, such as nursing and community health7,8, ideas of holism have been incorporated into theoretical approaches.
Central to the holistic approach is recognising the person's experience and its interrelatedness with the environment. The disease is no longer the centre of attention9. The unique experience and history of the person is honoured and worked with, rather than reducing a symptom to how it relates to the average or the norm. In this way the cultural context, individual development and experiences, current relationships and the familial context play a strong role in understanding and therefore managing the illness that the person presents with to the healthcare worker.
Within the public sector of South Africa the term 'holistic' is used loosely and no local operational definition could be found. In the study on which this article is based, the research group agreed on an operational definition of what is considered to be holistic practice. The definition came from the Canadian Holistic Medicine Association10:
Holistic medicine is a system of health care which fosters a cooperative relationship among all those involved, leading towards optimal attainment of the physical, mental, emotional, social and spiritual aspects of health.
It emphasises the need to look at the whole person, including analysis of physical, nutritional, environmental, emotional, social, spiritual and lifestyle values. It encompasses all stated modalities of diagnosis and treatment including drugs and surgery if no safe alternative exists. Holistic medicine focuses on education and responsibility for personal efforts to achieve balance and well-being.
Methodology
A participatory action research (PAR) design was used to explore how we could practice holistically in a sub-district. The PAR process allows front-line workers to reflect on their practice, deepen understanding of the issues involved, and plan action around their understanding. A research group of four primary healthcare nurses and one medical practitioner formed and reflected on the definition of holistic care, current holistic care in the public sector, as well as the limitations to holistic practice.
The primary healthcare nurses were aged between 42 and 53 years, while the age of the medical practitioner was 37 years. The average work experience in primary care for the primary healthcare nurses was 12 years (range 8-17 years) and the medical practitioner had 9 years work experience at district level. The nurses' first language was Zulu, while the first language of the medical doctor was English. None of the participants had any experience working in formal holistic care settings. All the participants volunteered for the study and were not reimbursed for their participation. The study had the support of district management and took place during working hours.
Data were generated from four facilitated meetings, the researcher's notes from participant observations as well as semi-structured interviews with the participants. The interview questions were developed in discussion with the research team to address the key issues the study was attempting to explore. The questions covered:
- how were current practices seen to be holistic
- what were the limitations to practicing holistically
- what actions needed to be taken to implement holistic care in the sub-district?
The meetings and interviews were audio-taped and transcribed by the researcher and then checked by another member of the research team.
An initial thematic analysis of the data was performed, using a cut-and-paste method. This thematic analysis was then presented to the whole group where a iterative process of grouping and relating themes generated a deeper level of analysis took place. Graphical mapping of the themes produced network diagrams of the interrelationships of the themes. The process allowed for maximum participation in the group to generate new meaning from and understanding of the collected data. A separate analysis was performed for each of the key questions of the research study; however, this article only reports on findings regarding the limitations of practicing holistically in the sub-district.
Relating the themes back to the original data, as well as reaching consensus in the group that generated the data, further validated the findings. The findings of the research process were then shared with the staff working in the sub-district, as well as with the district office.
An important aspect of PAR is that the generation of new knowledge should lead to action. The process of implementation of these findings was mostly in changes occurring in the individual consultations due to knowledge and attitude changes from the research process. The presentation of the research findings to the sub-district and district level put the issue of holistic care on the agenda of health service planning, but concrete outcomes have not been assessed as resulting directly from the study.
Results
The results presented are primarily of the data collected in relation to the limitations to practising holistically, and not of the research project as a whole. A graphic representation constructed out of the thematic analysis demonstrated the major limitations to practising holistically in the primary healthcare sector (Fig 1). Working as clinicians, the patient-healthcare relationship is the terrain in which holistic care is being delivered. Therefore the limitations were considered to be those impacting negatively on the patient-healthcare worker relationship. These limitations were broadly divided into aspects of the healthcare system and the wider context.
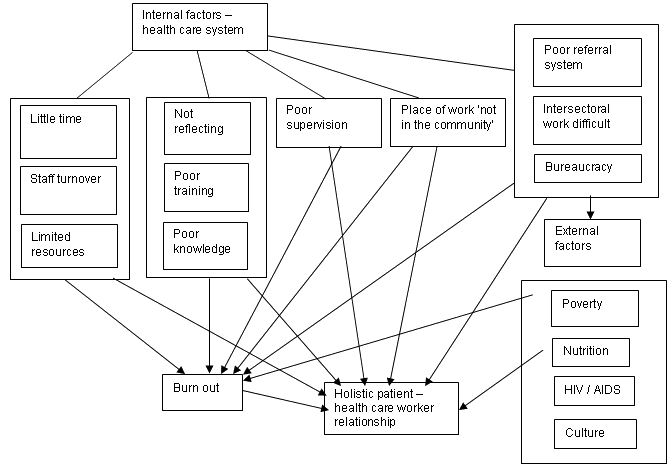
Figure 1: Limitations to holistic care - network of themes.
Within the healthcare sector the main groups of themes of limitations to the holistic patient-healthcare worker relationship were:
- Limited resources: working in a resource-constrained setting limits the possibilities to spend sufficient time and energy on individual patients and to get beyond the purely physical dimension.
- Poor training in and knowledge of holistic care: holistic approaches are not part of the training curriculum; general knowledge of what holism means is poor among healthcare workers. Holistic remains a vague concept in vision statements that is not explained or taught about regarding implementation.
- Poor supervision: staff in the healthcare system are not supervised or supported well, leading to inconsistent performance.
- Distance from the community: many communities are geographically far from services. Also, in terms of the relationship of communities with government services, many people feel alienated and separate from public health care.
- Referral system, intersectoral work and bureaucracy: the ability of the healthcare system to provide a seamless service across service levels (from community-level interventions to hospital and back), as well as among different government departments, is limited by poor referral systems, poor collaboration among different levels and sections in the service, as well as a cumbersome bureaucracy.
In the external context, the following groups were seen to be closely inter-linked:
- poverty
- poor nutrition
- HIV/AIDS
- cultural context.
These themes had very similar reasons for posing a challenge to practising holistically in the clinical context of a primary healthcare clinic. Poverty, poor nutrition and HIV/AIDS were seen as not only local problems, but also to have their roots in historical, social and political dynamics - and significantly within the local cultural context. While these factors need to be addressed within a holistic approach, the capacity to do so within the confines of a clinical consultation was felt to be limited.
When trying to provide a holistic service, the extent of the challenges faced may feel overwhelming and lead to an increased risk of burnout for the practitioner. Being burnt-out and frustrated within the service also limits the capacity to care for patients adequately, and therefore limits the ability to work holistically.
Discussion
As is already established, the term 'holistic practice' is used loosely and seems to be poorly understood in the public sector. Little in terms of local definitions or local literature on holistic practice was found to assist in clarifying the practical meaning, even though it is often held up as an ideal. Despite the lack of clarity, the idea of exploring the implementation of holistic care in the public sector generated considerable enthusiasm and interest among the research group.
Our results indicate that the majority of factors identified related to the structure and functioning of the healthcare system. The orientation of the whole healthcare system seems not to be towards holistic health, and provision of holistic services seems to depend on the individual clinician's commitment. The context, therefore, is not conducive to practising holistically.
The centrality of the patient-healthcare worker relationship
Placing the patient-healthcare worker relationship at the centre of the diagram is evidence of a vital perspective among the group who explored the question. By not placing community health outcomes or the healthcare service at the centre, the primacy of the individual is indicated in holistic care in the larger context. The same perspective is not often evident in public health approaches to healthcare service planning, where population-level indicators drive resource allocation and service development.
Resource limitation and training in a developing world context
Clearly the lack of resources within a specific context has an impact on the capacity to practise holistically in the public sector, and is related primarily to too few health-care workers and facilities. The shortage of suitably qualified staff pressurises clinicians to spend little time with patients due to the number of patients needing to be seen. The poor skill-mix in primary health care further limits the provision of a holistic service. In the current South African primary health model, the burden of the healthcare service falls on nursing staff11. Yet nurses working in these settings often have little training in clinical medicine, not to mention holistic approaches in primary care.
However the limitations to practising holistically go beyond the issue of lack of training and resources within the primary healthcare clinic. In a social context that is characterised by high levels of poverty, many healthcare interventions make a limited impact on basic socioeconomic issues that lie outside the formal healthcare sector. With diseases such as tuberculosis and HIV/AIDS, socioeconomic, cultural and motivational dimensions are powerful determinants of the disease process. However, it is difficult to address high levels of unemployment or lack of food-security within the processes of the current healthcare system in South Africa. The focus on clinical medicine limits the ability of clinicians to address apparent social issues. While it may not be seen as the province of the healthcare service, the poor integration of service delivery between different government and non-government agencies are obstacles to delivering integrated, holistic care to people. Our study has noted difficulty in working intersectorally, together with the problems of bureaucracy and a poor referral system. In a holistic approach it would be imperative to address issues of poverty, disempowerment, lack of food security and structural violence.
High expectations and burnout
Within the representation of the network of themes, the centrality of burnout as a limitation to practising holistically was an important finding. Vulnerability to burnout was related to practitioners wanting to practice holistically having high ideals12. Such high ideals lead to stress in the presence of the work-load expectation of primary care workers (allowing only a few minutes for each consultation). The recognition and prevention management of burnout is therefore an important strategy in supporting healthcare workers to practice more holistically.
It is implicit in this research that the healthcare system does not support people to practise holistically. The lack of support of primary care clinicians is also reflected in the finding of lack of adequate supervision, and that management feels distant from the clinical setting. This gap is reflected in what motivated the study - that the vision statement of many institutions does not seem to be implemented in the clinical setting. It is important to explore the gap between policy and practice further because it is the stated vision of many institutions to practice holistically.
Paradigms of care
Throughout the study a tension was evident between the biomedical approach of focussing on disease processes and a much more integrated and person-centred, holistic approach. Much healthcare delivery is still primarily structured towards a disease-management process and a pharmaceutical delivery system11. Aspects of care that are neglected - such as mental, emotional, social and spiritual aspects - are poorly integrated into a coherent approach. Lack of involvement of non-allopathic traditions (such as traditional healers or alternative medicine) in the formal healthcare system in South Africa is an indication of the current biomedical bias. Within the research team, there was tension relating to what holistic actually meant. The majority of participants viewed holistic as synonymous with 'comprehensive' (and therefore a method of practice), rather than a concept that would transform the way of practice. The exclusion of non-allopathic approaches of care therefore indicates the dominant worldview within the healthcare service.
Underlying issues of paradigms that inform policy development and health service planning need to be clarified and communicated throughout the healthcare system. A careful consideration of the implications of a change in paradigm also needs to accompany such a shift, in order for the change to be transformative, rather than an 'add-on' to already unsustainable workloads.
Conclusion
This exploration demonstrates that limitations to practising holistically in the public sector in South Africa are greater than merely resource allocation issues, as is often claimed. The resource limitations in terms of both number of healthcare workers and their skills are real. However, many of the limitations lie with organizational reorientation and the management of a paradigmatic change, rather than just adding greater numbers of healthcare workers. Aspects of the implementation of more holistic practice may be addressed with modest increases in resource allocation, by the management of the more fundamental paradigm shift (eg in improving intersectoral collaboration).
This exploration of the topic is specific to the context of the public sector in a particular sub-district in KwaZulu-Natal in South Africa and cannot be considered to be representative of any other context. There may well be primary care clinicians in South Africa practicing holistically in the public sector, not suffering from burnout and not feeling the pinch of resource constrains. However, the findings may generate discussion and reflection in other areas of the public sector in South Africa, and indeed in diverse settings throughout the world, and stimulate debate and further research into how holistic practices can be developed.
References
1. Department of Health KwaZulu Natal. Vision statement. Pietermaritzburg: Department of Health KwaZulu Natal, 1996.
2. Smuts JC. Holism and evolution. (First published 1926). Cape Town: N&S Press, 1987: 89-102.
3. Bloom W (Ed.). The Penguin book of new age and holistic writing. Harmondsworth: Penguin Books, 2000.
4. Capra F. Turning point. London: Flamingo, 1983.
5. Kriel J. Matter, mind, and medicine. Transforming the clinical method. Amsterdam: Rodopi, 2000.
6. Kent-Smith C, Kleinman A. Beyond the biomedical model: integration of psychosocial and cultural orientations. In: RB Taylor (Ed.). Fundamentals of family medicine. New York: Springer-Veckey, 1988: 88-97.
7. Neuman BM. The Neuman systems model, 3rd edn. Stamford: Appleton & Lange, 1995: 3-61.
8. Labonte R. Community and public health: an international perspective. Health Visitor 1997; 70: 64-67.
9. Whittaker D. Illness, the patient and the family. In: B Mash (Ed.). Handbook of family medicine. Cape Town: Oxford University Press, 2000.
10. Canadian Holistic Medical Association. What is holistic medicine? (Online) no date. Available: www.holisticmed.com/whatis.html (Accessed 29 November 2006).
11. Petersen I. Comprehensive integrated primary mental health care for South Africa. Pipedream of possibility? Social Science & Medicine 2000; 51: 321-334.
12. Couper ID. Approaching Burnout. South African Family Practice 2005; 47: 5-8.



