Introduction
Seven million people live in rural and remote Australia, constituting 29% of the Australian population1. These communities face significant healthcare disparities when compared to their metropolitan counterparts, with reduced life expectancy and an increased burden of disease2. Physiotherapists are known to contribute to health care in this community; however, there are several barriers to the recruitment and retention of rural physiotherapists. For example, rural physiotherapists report stress associated with managing large caseloads3, having limited support4 and providing care across wider clinical areas to more culturally diverse populations than their metropolitan counterparts4.
Rural and remote physiotherapy in Australia has evolved to be regarded by some as a discipline in its own right5. A 2009 literature review by the Centre for Allied Health Evidence defined additional competencies and skills required of allied health professionals in rural and remote health practice to bridge the gap from metropolitan practice6. The domains recognised by the review were clinical, organisational, professional, cultural, team practice, and attitudinal, and are all considered to contribute to effective rural practice6. The postgraduate Allied Health Rural Generalist Pathway7,8 emerged in response to a need for additional training pathways within the discipline. Such qualifications aim to provide the knowledge, skills and attributes needed of practitioners who best meet the needs of the community7. At the graduate level, Beattie and colleagues created an entry to practice framework titled Developing rural and remote allied health competencies9, which addressed three broad domains of practice: generic, professional and technical. Therefore, although great work has already been done to understand competencies required for effective allied health practice in rural and remote contexts, as well as development of training frameworks to support best practice health care for these communities, work specific to the physiotherapy context is yet to be performed.
To enter the physiotherapy profession, practitioners are required to meet the competencies outlined in the physiotherapy practice thresholds in Australia and Aotearoa New Zealand10. These competencies encompass knowledge, skills and attributes such as ‘plan and implement an efficient, effective, culturally responsive and client-centred physiotherapy assessment’ and ‘advocate for clients and their rights to health care’10. Competencies can provide credibility and accountability to a profession, by streamlining the expectations of all stakeholders and providing an objective measure of outcomes11. Competencies can also be utilised to create frameworks for pre-professional training and professional development, and can underpin role descriptions.
Employers and education providers advocate for training in preparation for entering and succeeding in the rural workforce6,12,13, and competencies similar to those above may be considered the first step to inform the creation of physiotherapy support. With acknowledgement of the work of Beattie and colleagues regarding competencies for rural allied health practitioners9, the work underpinning the postgraduate Rural Allied Health Generalist Pathway8, and the physiotherapy practice thresholds in Australia and Aotearoa New Zealand 201510, there has been no investigation into the physiotherapy-specific skills that contribute to effective entry-level practice in rural and remote settings. The exploration of competencies that contribute to effective physiotherapy practice in rural settings may inform strategies aimed to enhance the transition from student to clinician in this challenging context. Therefore, this study aimed to identify a set of competencies that contribute to effective physiotherapy practice in rural Australia.
Methods
Study design
The Delphi method aims to reach consensus of opinion of a group of identified experts by providing organised feedback between ‘rounds’ where experts collate their ideas14,15. The experts independently complete several rounds of a survey, through which they are asked to consider and refine their own opinions and the de-identified opinions of the other panel members until consensus is reached16. The Delphi method allows for asynchronous contribution from geographically dispersed experts in rural and remote physiotherapy practice, without the need to have all contributors in the same location and also avoiding potentially destructive group dynamics17. This method has also been used to define and clarify roles and performance competencies across health care and education17,18.
Participants
Three rounds of online questionnaires were used (detailed below), which exceeds the required two rounds considered adequate for collation of varied and comprehensive expert opinions17. Agreement between 80% of the panel members was the benchmark selected a-priori to indicate that consensus had been reached17.
In this study, experts in rural and remote physiotherapy were selected in agreement with expert criteria defined by Jensen et al19. These criteria include:
(a) a dynamic, multidimensional knowledge base that is patient-centred and evolves through therapist reflection,
(b) a clinical reasoning process that is embedded in a collaborative, problem-solving venture with the patient,
(c) a central focus on movement assessment linked to patient function, and
(d) consistent virtues seen in caring and commitment to patients19.
In addition to these criteria, experts were required to have worked full-time in a rural or remote workplace for a minimum of 5 years over the previous 10-year period. This aimed to ensure sufficient experience as well as recency of rural and remote practice. The Modified Monash Model (MMM) was chosen to classify rural and remote areas20.
The usefulness of findings from the Delphi method depends on the breadth of perspectives obtained17. The publicly accessible Australian Physiotherapy Association database21 was used to access the contact details of 222 physiotherapists working in rural and remote locations across all Australian states and territories. Physiotherapists were contacted by email and asked to consider the criteria above and nominate themselves or their peers to participate. Physiotherapists were encouraged to consider nominating peers outside of their setting of practice to promote diversity of the sample. A minimum of 15 members for the initial panel14 was determined, with a first-to-consent approach applied to the purposive sampling. Eligible participants were sent the round one survey from the lead researcher by email. Participants were assured that their responses would remain de-identified.
Data collection
The Delphi question was designed following a review of the literature and through collaboration with the research team including a panel of expert academics, researchers and physiotherapists working in rural and remote locations. This question aimed to elicit detailed and specific responses that would allow for thematic analysis in combination with other participants’ responses, for the generation of competencies17. Round one was piloted by a convenience sample of physiotherapists (n=28) who were contacted through the initial recruitment, but did not meet the inclusion criteria of the study. This was undertaken to refine the structure and content of the Delphi question. No changes were required as a result.
The initial round of the Delphi was created in an online survey program and sent as a link to consenting panel members. Round one contained both demographic questions and the open response question of the Delphi:
What unique knowledge, skills, abilities, attributes or other characteristics do physiotherapists need to possess, or learn in order to provide effective physiotherapy specifically in a rural or remote setting?
Data analysis
The responses from round one were thematically analysed22 as per Delphi protocol14, with the assistance of NVivo v10 (QSR International; https://www.qsrinternational.com/nvivo-qualitative-data-analysis-software/support-services/nvivo-downloads) to review and categorise the data. The lead researcher (RM) undertook training in qualitative analysis and the use of NVivo prior to immersing in the raw data, with the aim of identifying possible competencies suggested by the expert panel. All data were read several times to ascertain the intended meaning of the participants, and then coded with initial themes and subthemes. This step was repeated independently by another researcher (RF) to ensure the creditability of the findings. To ensure the validity of the results, an experienced rural physiotherapist (AL), not involved as a participant, reviewed the data, codes and themes to aid in the verification of findings. All potential themes were then reviewed and discussed by the research team.
Delphi process
A total of 127 items were provided by the panel in round one, which resulted in 22 competencies following data analysis (Fig1). The 22 competencies derived from round one were presented to the expert panel in round two in a table format. Participants were invited to consider each competency and indicate whether they felt that it was ‘important for most rural and remote physiotherapists’, ‘important for only some rural and remote physiotherapists’ or ‘not important for rural and remote physiotherapists’. Questionnaires were individualised to each participant to include their answers from round one along with the 22 competency items. Each survey also included an open text space for participants to raise concerns or provide additional information regarding the competencies. Each round of the Delphi was open for 3 weeks, with prompting emails sent to non-responding participants 1 week prior to closure.
A total of seven panel members provided additional responses in the open text space during round two. This resulted in two new competencies being presented to the expert panel in round three (totalling 24 competencies for panel consideration). Round three followed identical procedures to round two. At the completion of round three, no additional free text comments were provided by the respondents, signalling the completion of the survey rounds.
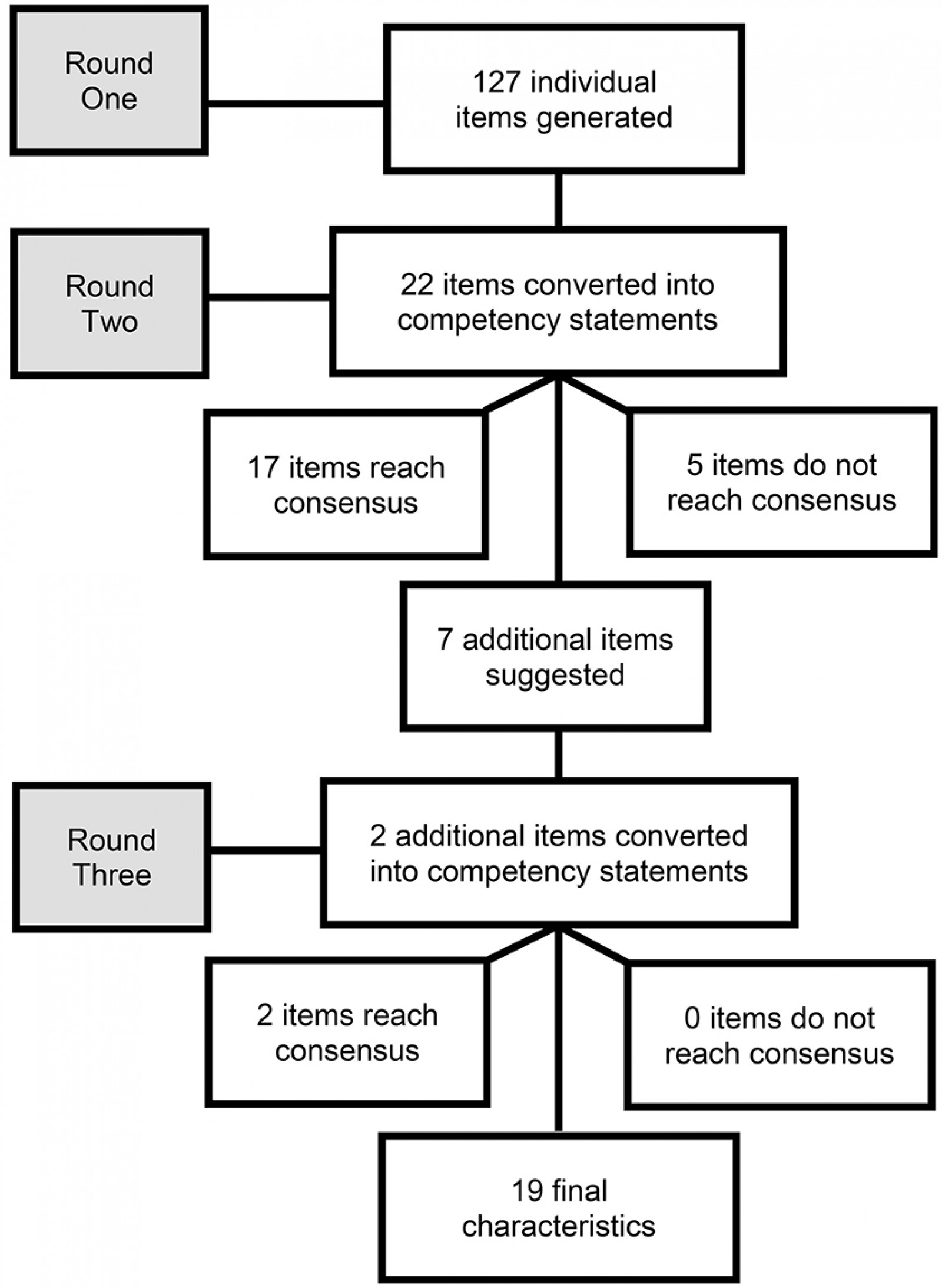 Figure 1: Data analysis rounds one, two and three.
Figure 1: Data analysis rounds one, two and three.
Ethics approval
Ethics clearance was obtained from the University of Queensland Human Research Ethics Committee (approval number 2019002084).
Results
A purposive sample of 17 expert physiotherapists agreed to participate. All 17 panel members completed the first round (100% response rate), 16/17 completed the second round (94.1% response rate), and 15/16 competed the third round (93.8% response rate). The responses from participants who completed rounds one and two were not removed if they did not respond in subsequent rounds, as consistent with the Delphi approach16. Reported reasons for attrition included participants taking periods of annual leave and failing to complete the survey within the required timeframe.
Rural experience among the panel had a range of 5–36 years, with an average of 17.5 years. Over half of the participants were female (10/17, 58.8%) with most participants (8/17, 47.1%) based in large rural towns (MM 3), followed by medium rural towns (MM 4) (4/17, 23.5%), small rural towns (MM 5) (3/17, 17.7%), and remote communities (MM 6) (2/17, 11.8%). Additional demographic information is outlined in Table 1. Most participants (13/17, 76.5%) identified as working in a ‘musculoskeletal and/or sports private practice’ setting, with four other settings identified. The Health Workforce Australia classification system was used to define the respondents’ physical setting of work; however, the ‘musculoskeletal and/or sports private practice’ category does not reflect their clinical practice. The respondents worked across a broad range of clinical areas within their identified settings of practice, and a breakdown of their clinical expertise across the seven major disciplines of physiotherapy is presented in Table 2.
Of the 24 competencies presented to the panel, consensus was reached on a total of 19. These were considered by a consensus of 80% of the panel as ‘important for most rural and remote physiotherapists’. Five competencies did not achieve consensus (Table 3). No competencies achieved consensus as being ‘important for only some rural and remote physiotherapists’ or ‘not important for rural and remote physiotherapists’. Of the final set of 19 competencies, five achieved 100% agreement by the panel. The final set of competencies is outlined in Table 4 alongside the levels of consensus that were achieved for each competency.
Table 1: Demographic characteristics of the Delphi panel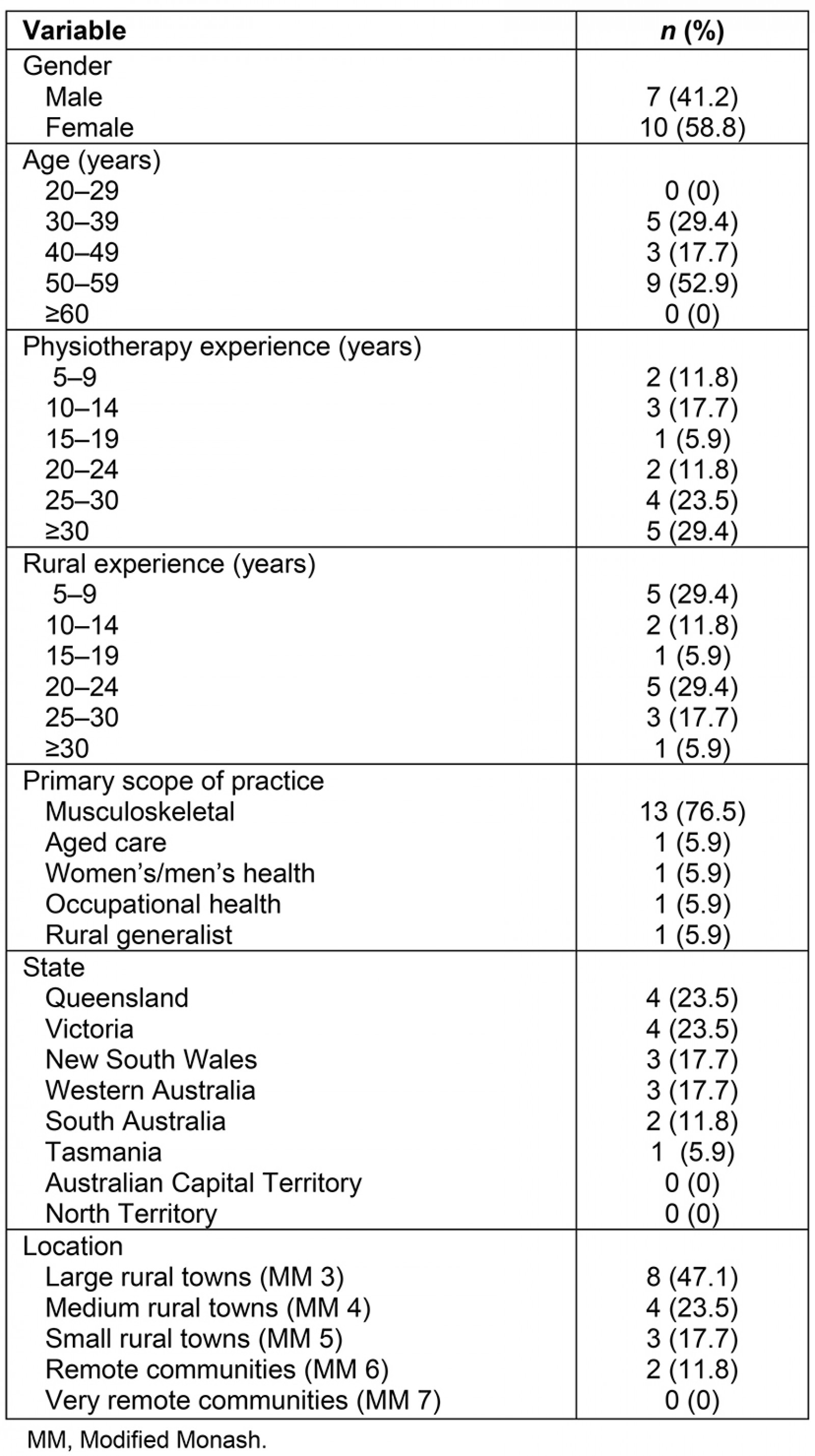
Table 2: De-identified panel member details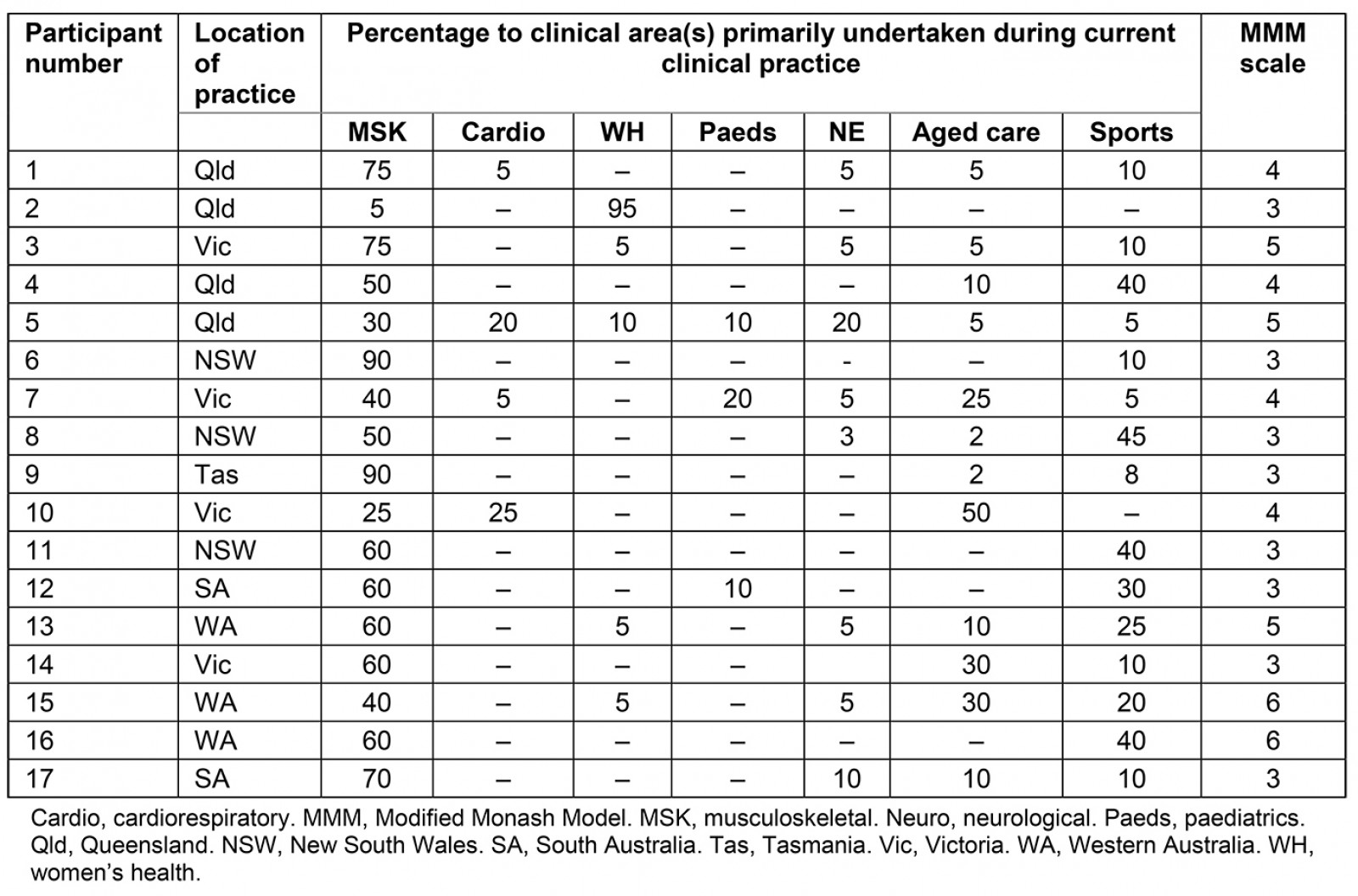
Table 3: Rural and remote physiotherapy competencies that did not reach consensus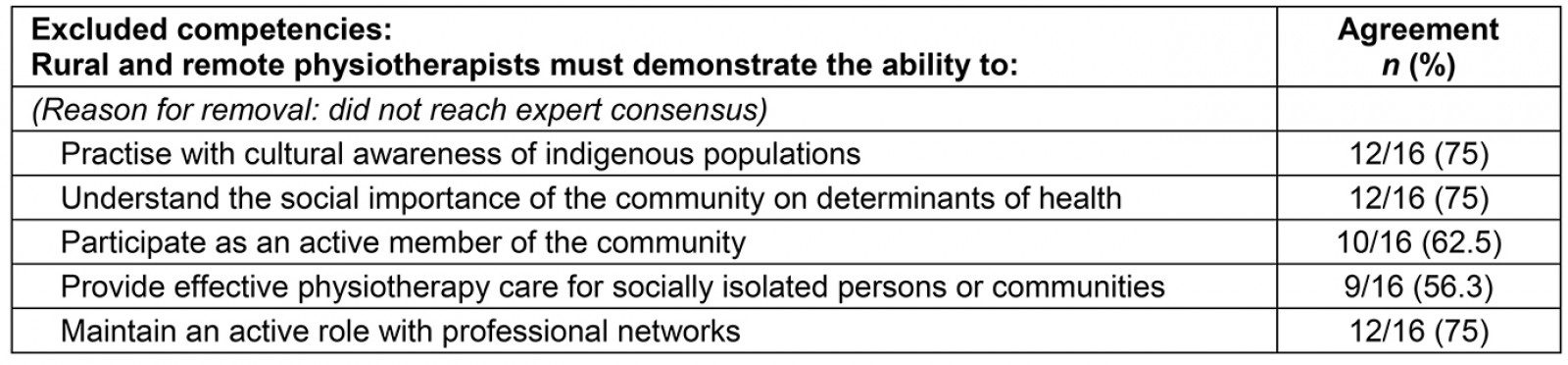
Table 4: Entry-level rural and remote physiotherapy competencies list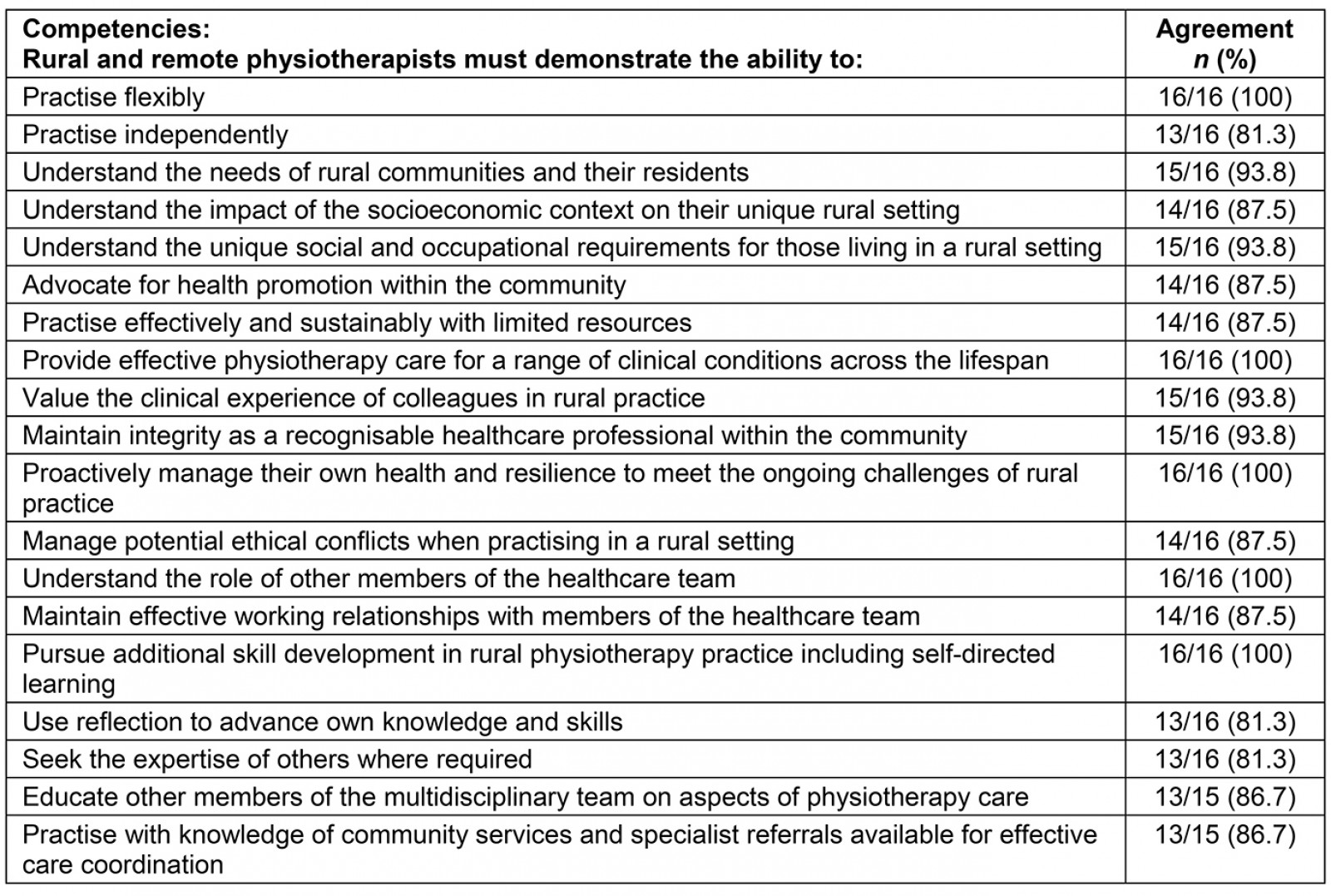
Discussion
This study has explored the attributes that contribute to effective physiotherapy practice in rural Australia. The attributes are presented as a set of 19 competencies and reflect the complexity of rural physiotherapy practice. The competencies also emphasise the importance of providing health care that is responsive to rurality and considers broader constructs such as isolation, resource limitations and the social determinants of health. These competencies add to the body of work that explores effective practice in rural Australia, furthering the literature in the scope of entry-level physiotherapy practice. The competencies are a preliminary step in providing a common language for physiotherapists and their employers, and may be used to guide mentorship and training in this setting. In outlining attributes that contribute to effective practice, these competencies may also have a role in ensuring positive experiences in rural settings and may contribute to discussions around recruitment and retention.
The knowledge, skills and attributes represented by these competencies reflect the factors that add complexity to rural and remote practice, for example the ability to ‘understand the needs of rural communities and their residents’, ‘understand the impact of the socioeconomic context on their unique rural setting’ and ‘understand the unique social and occupational requirements for those living in a rural setting’. The Allied Health Rural Generalist Pathway competencies encourage the deliberate fostering of these skills to overcome the challenges presented by rural practice, for example recommending ‘appropriate and relevant community engagement mechanisms in rural and remote settings’7. The Allied Health Rural Generalist Pathway, combined with the findings of this study, encourage physiotherapy education providers to consider the inclusion of such awareness and skills in pre-professional training.
Several competencies generated concern the intrinsic skills of physiotherapists to problem solve in response to challenges to practising in rural and remote locations, including the ability to ‘practise flexibly’, ‘practise independently’, and ‘practise effectively and sustainably with limited resources’. The inclusion of independence and sustainability competencies by the expert panel was not surprising, given that professional isolation and resource limitations are considered significant challenges for rural and remote health practitioners6. These skills further reflect the clinical adjustments required of physiotherapists working in a rural and remote health care model23. Similar skills relating to adaptation and initiative in the face of scarcity have been identified as strengths of health practitioners working in this area24. Beattie et al’s framework also advocates for the acquisition of generic competence such as leadership and management, on entry to the rural workforce9. The additional skills that contribute to effective practice in the rural setting may highlight the disparity between rural and metropolitan practice. This study presents the competencies that contribute to responsive practice in rural settings, and may encourage new graduates to consciously foster these skills when working rurally.
The competencies developed within the present study are particularly relevant to the retention challenges faced in rural and remote physiotherapy settings. Warburton and colleagues (2014) identified that, in rural and remote settings, workplace support was a strong extrinsic factor that contributed to retention of healthcare practitioners25. The final set of competencies featured skills valuing the resources and supports available; for example the ability to ‘value the clinical experience of colleagues in rural practice’. A literature review conducted by Campbell and colleagues identified that the intrinsic qualities of rural and remote work, such as the ability to be flexible and autonomous, were viewed as beneficial to working in the setting3. Attainment of these competencies in addition to the Physiotherapy Practice Thresholds in Australia and Aotearoa New Zealand (2015)10 may create positive steps towards actions that may enhance retention. The competencies highlight the knowledge, skills and attributes required for effective practice in rural and remote settings; supporting entry-level physiotherapists to attain these may improve the sustainability of their practice, and subsequently their retention in this workforce.
The concept of independence as a competency was not unexpected considering the recognition of the ability to work autonomously as a key requirement for other health professionals working in rural and remote settings26, and the first-contact practitioner role of physiotherapists. It is known that practitioners who are able to develop a sense of professional autonomy may find rural and remote practice more satisfying and rewarding6, supporting the inclusion of a competency addressing independence. The opportunity to practice with autonomy must be considered in the context of current literature, which suggests that what are viewed as incentives by some may be viewed as disincentives by others27.
The literature reviewed by the Centre for Allied Health Evidence highlighted the many non-clinical domains of competence required of rural and remote practitioners6. In the present study, several competencies representing non-clinical domains were included in the final set, such as the ability to ‘maintain integrity as a recognisable healthcare professional within the community’, and ‘proactively manage their own health and resilience to meet the ongoing challenges of rural practice’. Existing literature that considers all domains must be prioritised when referring to professional development and career progression, as opposed to effective entry-level practice.
Two competencies that did not reach expert consensus were ‘practice with cultural awareness of indigenous populations’ and ‘understand the social importance of the community on determinants of health’. These potential competencies were identified in the rural practice literature review undertaken prior to data collection. It is hypothesised that although these are fundamental to all physiotherapy practice, they did not reach consensus because they may not be applicable exclusively to all rural settings across Australia.
The creation of specific competencies for rural and remote physiotherapy practice may serve several purposes. Primarily, this set of competencies provides insight and a common language for individuals interested in the requirements of entry-level physiotherapists working specifically in rural or remote locations. This may facilitate a shared approach between educators regarding the requirements for professional development in this context. This study may also have relevance for guiding current curriculum or the potential for refining pre-professional training related to rural and remote physiotherapy education. Further inquiry into the feasibility of including specific rural and remote training into existing preprofessional programs or through individual approaches holds merit. As demonstrated by Strasser and Neusy, positive clinical and educational experiences in rural health during pre-professional training are strongly associated with entering the rural workforce12, which in turn informs curriculum design. Also, these entry-level competencies identify the knowledge, skills and attributes required of physiotherapists who are transitioning from student to clinician in the rural setting. As the competencies reflect the skills required to be effective, their use to guide new-graduate training may contribute to positive experiences in the rural setting. Ensuring that new graduates are appropriately prepared to deliver effective care may contribute to their retention to the rural workforce. Given the common challenges of rural and remote practice, these competencies may be potentially modified to suit other health disciplines. This article presents an introductory exploration of competencies for effective entry-level practice in rural and remote settings. Further research is required to gain a deeper understanding of the opinions of physiotherapists working in specific rural and remote settings (such as hospitals and aged care), as well as further research to establish the need for competencies that detail the unique skills of rural physiotherapy practice.
Limitations
This study has only considered rural and remote physiotherapy practice in Australia, and the generality of the findings may be limited as other nations were not represented. This is reinforced by the geographic challenges and cultural variables that may be considered unique to the Australian context. Attrition occurred from the expert panel in round two (n=1) and round three (n=1), and the effect of this missing data is unknown. Over three-quarters of the panel identified as working most of their time in a ‘musculoskeletal and/or sports private practice’ setting. Despite this representing the respondent’s location of practice rather than their clinical caseload, the skewed representation may have biased the final set of competencies toward musculoskeletal practice. All seven of the major disciplines of physiotherapy in Australia were represented within the panel members’ workloads. Furthermore, a previously established consensus threshold of 80% was selected to achieve the aims of the study; however, if the panel had been required to achieve 100% agreement the ongoing deliberation may have altered the final set of competencies.
Conclusion
This study has introduced competencies that detail the attributes contributing to effective physiotherapy practice in rural Australia. These competencies support the understanding of rural and remote physiotherapy as an area of practice with unique challenges and may inform pre-professional preparation and new-graduate support.
